Coronary Artery Disease and Acute Coronary Syndrome Description




































- Slides: 41

Coronary Artery Disease and Acute Coronary Syndrome

Description • Coronary Artery Disease (CAD) – A type of blood vessel disorder that is included in the general category of atherosclerosis

Description • Atherosclerosis – Can occur in any artery in the body – Atheromas (fatty deposits) • Preference for the coronary arteries

Description • Atherosclerosis – Terms to describe the disease process: • Arteriosclerotic heart disease (ASHD) • Cardiovascular heart disease (CHD) • Ischemic heart disease (IHD) • CAD

Description • Cardiovascular diseases are the major cause of death in the US and Canada • Heart attacks are still the leading cause of all cardiovascular disease deaths and deaths in general

Etiology and Pathophysiology • Atherosclerosis is the major cause of CAD – Characterized by a focal deposit of cholesterol and lipids, primarily within the intimal wall of the artery

Etiology and Pathophysiology • Endothelial lining altered as a result of chemical injuries – Hyperlipidemia – Hypertension

Etiology and Pathophysiology • Bacteria and/or viruses may have role in damaging endothelium by causing local inflammation • C-reactive protein (CRP) – Nonspecific marker of inflammation – Increased in many patients with CAD – Chronic exposure to CRP triggers the rupture of plaques

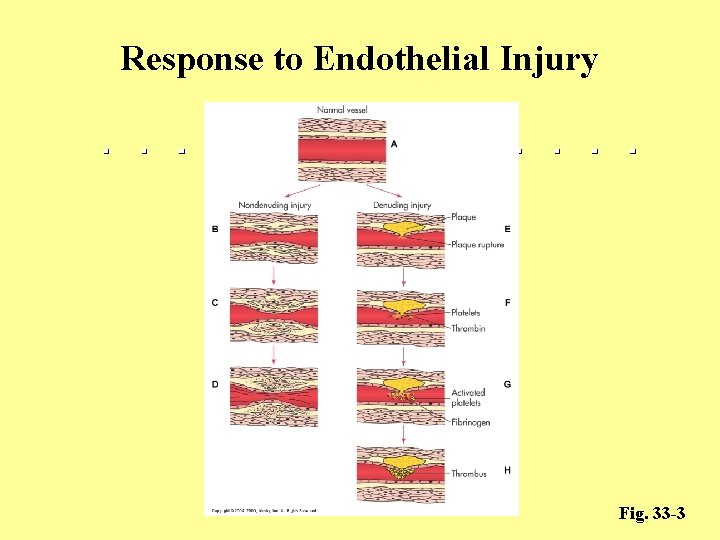
Etiology and Pathophysiology • Endothelial alteration – Platelets are activated – Growth factor stimulates smooth muscle proliferation – Cell proliferation entraps lipids, which calcify over time and form an irritant to the endothelium on which platelets adhere and aggregate

Etiology and Pathophysiology • Endothelial alteration – Thrombin is generated – Fibrin formation and thrombi occur

Response to Endothelial Injury Fig. 33 -3

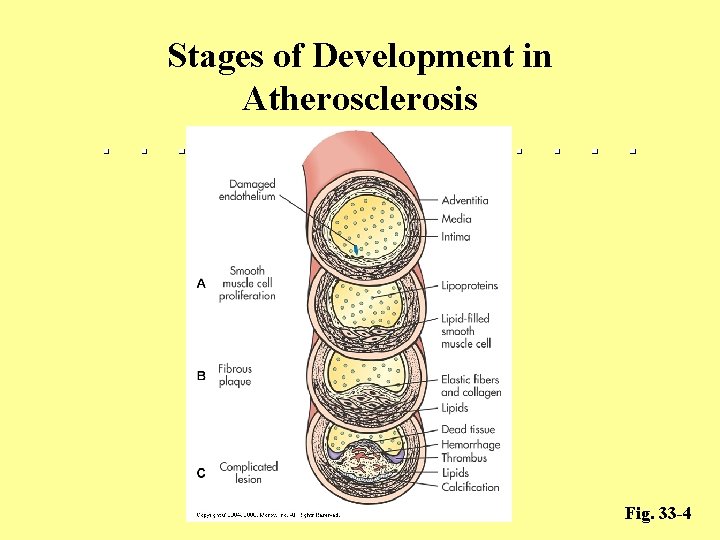
Stages of Development in Atherosclerosis Fig. 33 -4

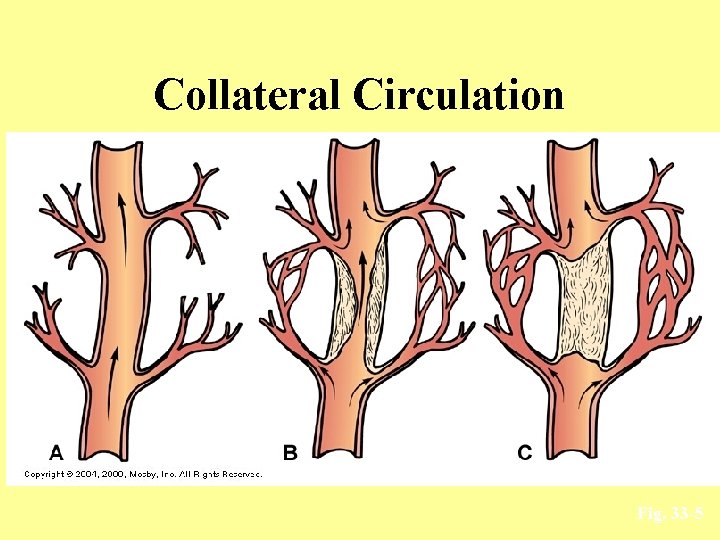
Etiology and Pathophysiology Collateral Circulation • Analogous to “detours” around atherosclerotic plaques • Occur normally in coronary circulation • But collaterals increase in the presence of chronic ischemia • When occlusion occurs slowly over a long period, there is a greater chance of adequate collateral circulation developing

Collateral Circulation Fig. 33 -5

Risk Factors for Coronary Artery Disease • Risk factors can be divided: – Unmodifiable risk factors – Modifiable risk factors

Risk Factors for Coronary Artery Disease • Unmodifiable risk factors: – Age – Gender – Ethnicity – Genetic predisposition

Risk Factors for Coronary Artery Disease • Modifiable risk factors: – Elevated serum lipids – Hypertension – Smoking – Obesity – Physical inactivity – Diabetes mellitus – Stressful lifestyle

Risk Factors for Coronary Artery Disease • Health Promotion – Identification of high-risk persons – Management of high-risk persons • Risk factor modification – Physical fitness – Health education in schools – Nutrition (weight control, ↓ fat, ↓ chol intake) – Cholesterol-lowering medications

Types of Angina • Results when the lack of oxygen supply is temporary and reversible • Types of Angina – Stable Angina – Prinzmetal Angina – Unstable Angina

Stable Angina Pectoris • Chest pain occurs intermittently over a long period with the same pattern of onset, duration, and intensity of symptoms • Can be controlled with medications on an outpatient basis • Pain usually lasts 3 to 5 minutes – Subsides when the precipitating factor is relieved – Pain at rest is unusual

Silent Ischemia

Prinzmetal’s Angina • Occurs at rest usually d/t spasm of major coronary artery • Spasm may occur in the absence of CAD

Unstable Angina • Angina that is: – New in onset – Occurs at rest – Has a worsening pattern – Unpredictable – Considered to be an acute coronary syndrome – Associated with deterioration of a once stable atherosclerotic plaque

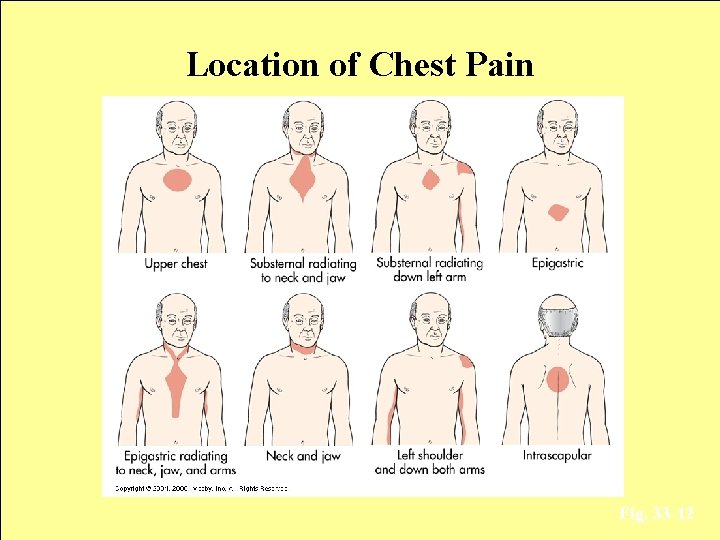
Clinical Manifestations Angina • Chest pain or discomfort (d/t ischemia) – A strange feeling, pressure, or ache in the chest – Constrictive, squeezing, heaving, choking, or suffocating sensation – Indigestion, burning

However • Up to 80% of patients with myocardial ischemia are asymptomatic • Associated with diabetes mellitus and hypertension

Location of Chest Pain Fig. 33 -12

Diagnostic Studies Angina • • ECG Coronary angiography Cardiac markers (CK MB, Troponin) Treadmill exercise testing (stress test) Serum lipid levels C-reactive protein (CRP) Nuclear imaging

Collaborative Care Angina • Treatment for stable angina: – oxygen demand and/or oxygen supply – Nitrate therapy – Stent placement

Collaborative Care Angina • Treatment for stable angina: – Percutaneous coronary intervention – Atherectomy – Laser angioplasty – Myocardial revascularization (CABG)

Collaborative Care Angina • Drug Therapy – Antiplatelet aggregation therapy • Aspirin: drug of choice (for MI prevention) • First line of treatment for angina

Collaborative Care Angina • Drug Therapy – Nitrates • 1 st line therapy for treatment of acute anginal symptoms • Dilation of vessels

Collaborative Care Angina • Drug Therapy – -Adrenergic blockers – Calcium channel blockers

Collaborative Care Angina • Percutaneous coronary intervention – Surgical intervention alternative – Performed with local anesthesia – Ambulatory 24 hours after the procedure

Collaborative Care Angina • Stent placement – Used to treat abrupt or threatened abrupt closure and restenosis following PCI

Collaborative Care Angina • Atherectomy – The plaque is shaved off using a type of rotational blade – Decreases the incidence of abrupt closure as compared with PCI

Collaborative Care Angina • Laser angioplasty – Performed with a catheter containing fibers that carry laser energy – Used to precisely dissolve the blockage

Collaborative Care Angina • Myocardial revascularization (CABG) – Primary surgical treatment for CAD – Patient with CAD who has failed medical management or has advanced disease is considered a candidate

Clinical Manifestations Myocardial Infarction • Pain – Severe, immobilizing chest pain not relieved by rest, position change, or nitrate administration • The hallmark of an MI

Clinical Manifestations • Acute Coronary Syndrome (ACS) – Develops when the oxygen supply is prolonged and not immediately reversible

Clinical Manifestations • ACS encompasses: – Unstable angina – Myocardial infarction (MI)

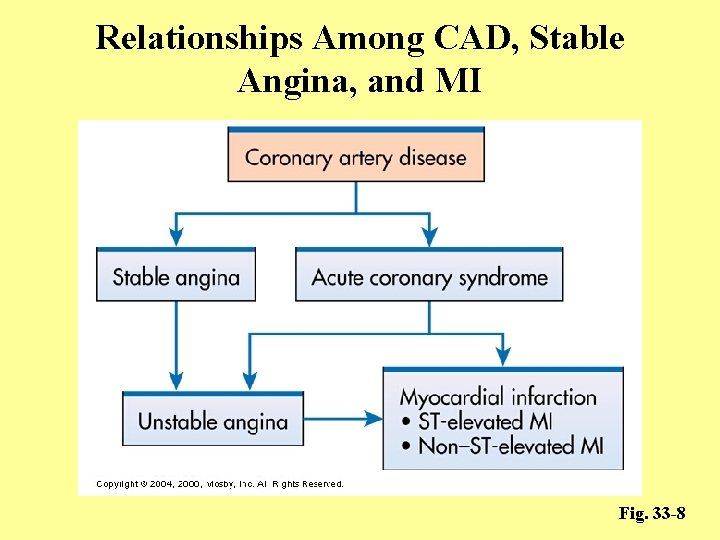
Relationships Among CAD, Stable Angina, and MI Fig. 33 -8