1 2 Classification of Ischemic Heart Disease Chronic







































































- Slides: 86

1

2

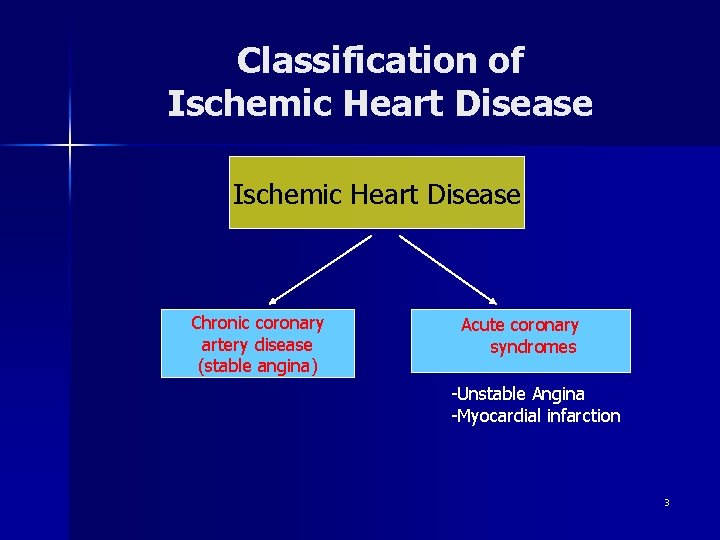
Classification of Ischemic Heart Disease Chronic coronary artery disease (stable angina) Acute coronary syndromes -Unstable Angina -Myocardial infarction 3

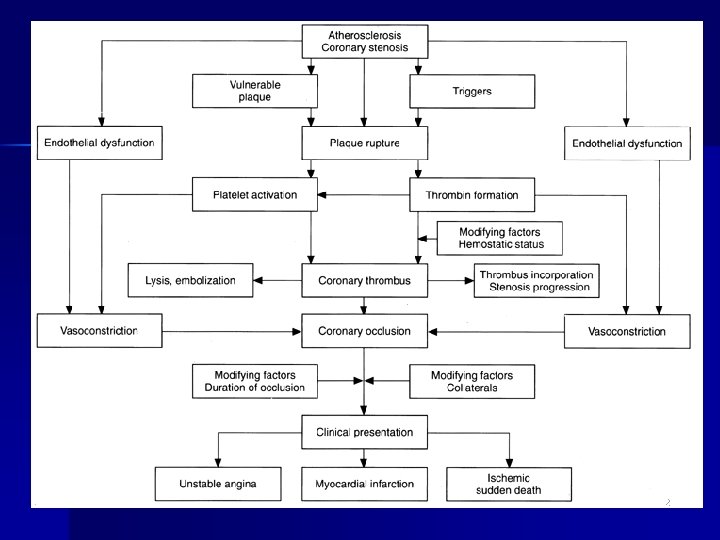
1) Drugs that Affect Blood Coagulation n Used in the prevention and management of thrombotic and thromboembolic disorders 4

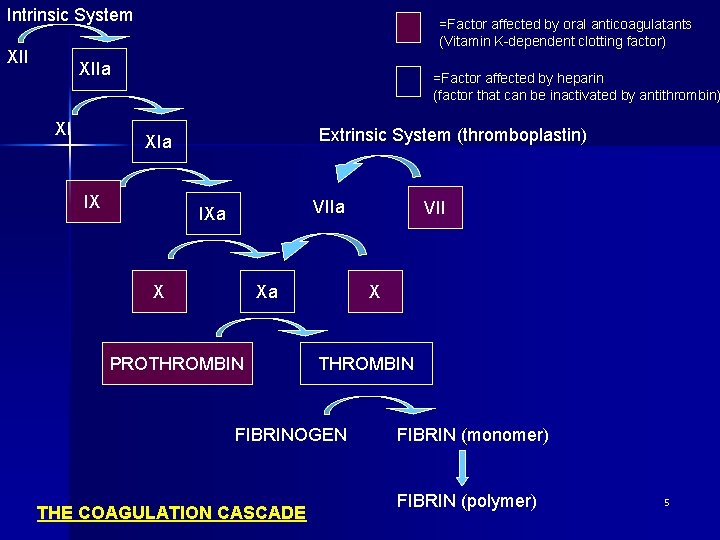
Intrinsic System XII =Factor affected by oral anticoagulatants (Vitamin K-dependent clotting factor) XIIa XI =Factor affected by heparin (factor that can be inactivated by antithrombin) Extrinsic System (thromboplastin) XIa IX VIIa IXa X Xa PROTHROMBIN X THROMBIN FIBRINOGEN THE COAGULATION CASCADE VII FIBRIN (monomer) FIBRIN (polymer) 5

1) Drugs that Affect Blood Coagulation (Cont’d) n (i) Anticoagulant drugs – Drugs that disrupt the coagulation cascade, & thereby suppress production of fibrin – Prevention of thrombosis in veins – Heparin n n Suppresses coagulation by helping antithrombin III inactivate thrombin, factor Xa and other clotting factors Used in: – Prevention and treatment of pulmonary embolism, stroke, deep vein thrombosis (DVT) – Prevent coagulation in devices in open heart surgery and renal dialysis – Treatment of disseminated intravascular coagulation – Adjunct to thrombolytic therapy of acute myocardial infarction 6

1) Drugs that Affect Blood Coagulation (Cont’d) n Dosage – Based on body weights of the patients & their indications n Adverse effects – Hemorrhage – Thrombocytopenia n Decrease platelet count – Hypersensitivity reactions n Since commercial heparin is extracted from animal tissue 7

1) Drugs that Affect Blood Coagulation (Cont’d) – Warfarin n Suppress coagulation by acting as an antagonist of vitamin K n 4 clotting factors (VII, IX, X & prothrombin) require vitamin K for their synthesis n Indications: – Prevention of venous thrombosis & associated pulmonary embolism – prevention of thromboembolism in patients with prosthetic heart valves – Prevention of thrombosis during atrial fibrillation – Reduce risk of recurrent transient ischemic attacks (TIAs) & recurrent MI 8

1) Drugs that Affect Blood Coagulation (Cont’d) n Daily dose – usually 3 to 9 mg but it should be based on the INR values. – INR targeted values are different indications, usually within 2 to 3. 5 n Adverse effects: – Hemorrhage – Teratogenic 9

1) Drugs that Affect Blood Coagulation (Cont’d) n (ii) Antiplatelet drugs – Suppress platelet aggregation – Indicated for prevention of thrombosis in arteries 10

11) Drugs that Affect Blood Coagulation (Cont’d) n Clopidogrel (Plavix) – Adenosine diphosphate receptor (ADP) antagonist – Irreversible blocking of ADP receptors on the platelet surface – Prevent ADP-stimulated aggregation – Indicated for prevention of stroke, vascular death & MI – The combination of aspirin and clopidogrel appears to be the most effective and safest therapy for secondary prevention of stroke. 11

11) Drugs that Affect Blood Coagulation (Cont’d) n Clopidogrel (Plavix) – Dose n 75 mg po daily with or without food – Adverse effects: n Hemorrhage (GI & Intracranial) n GI side effects 12

1) Drugs that Affect Blood Coagulation (Cont’d) n Aspirin – Suppress platelet aggregation by causing irreversible inhibition of cyclooxygenase, an enzyme required by platelets to synthesize thromboxane A 2 (TXA 2) 13

1) Drugs that Affect Blood Coagulation (Cont’d) n Aspirin – Indicated in : n Primary prophylaxsis of MI n Prevention of reinfarction patients who have experienced an acute MI n Prevention of stroke in patients with a history of TIAs – Dose n Maintenance treatment 75 -150 mg daily po – Adverse effects n GI hemorrhage & also other hemorrhage n Bronchospasm 14

1) Drugs that Affect Blood Coagulation (Cont’d) n (iii) Thrombolytic drugs – Promote lysis of fibrin, thereby cause dissolution of thrombi n Streptokinase – First bind to plasminogen to form an active complex – The streptokinase-plasminogen complex then catalyzes the conversion of other plasminogen molecules into plasmin, an enzyme that digests the fibrin meshwork of clots 15

1) Drugs that Affect Blood Coagulation (Cont’d) n Alteplase (t. PA) – Also known as tissue plasminogen activator (t. PA) – Is produced commercially by recombinant DNA technology – Human t. PA is an enzyme that promotes conversion of plasminogen to plasmin, an enzyme that digests the fibrin matrix of clots n Adverse effects: – Nausea & vomiting – Bleeding 16

1) Drugs that Affect Blood Coagulation (Cont’d) n Nursing Alerts: – Monitor signs of hemorrhage n Lowering of blood pressure, elevation of heart rate, discoloration of urine or stools, bruises, petechiae, etc. – Monitor INR, APTT, PT regularly – Warfarin is contraindicated in pregnancy & breast-feeding 17

2) Cardiotonics & other Inotropic Drugs n The cardiotonics are drugs used to increase the efficiency & improve the contraction of the heart muscle, which leads to improved blood flow to all tissues of the body 18

2) Cardiotonics & other Inotropic Drugs (Cont’d) n Digoxin – Inhibits the enzyme Na, K-adenosine triphosphatase (Na, K-ATPase), increases the movement of Na out of myocardial cells after contraction – As a result, Ca enters the cell in exchange for Na, causing additional Ca to be released from intracellular binding sites – With the increase in intracellular concentration of free Ca ions, more Ca is available to activate the contractile proteins, actin & myosin, & increase myocardial 19 contractility

2) Cardiotonics & other Inotropic Drugs (Cont’d) n Side effects: – Usually associated with excessive dose – Digoxin toxicity: n anorexia, nausea, vomiting, diarrhoea, visual disturbance, confusion & mental disturbance, arrthythmia, heart block n Dosage: – Maintenance: 62. 5 -500 mcg daily 20

2) Cardiotonics & other Inotropic Drugs (Cont’d) n Milrinone (Primacor) – Increase levels of cyclic adenosine monophosphate (c. AMP) in myocardial cells by inhibiting phosphodiesterase (PDE) – Relax vascular smooth muscle to produce vasodilation & decrease preload & afterload – Used in short term management of acute severe heart failure that is not controlled by digoxin, diuretics & vasodilators 21

2) Cardiotonics & other Inotropic Drugs (Cont’d) n Side effects: – Arrhythmias, headache, hypotension n Dosage: – Maximum dose: 1. 13 mg/kg daily 22

2) Cardiotonics & other Inotropic Drugs (Cont’d) n Nursing Alerts: – Withhold the drug & contact the physician if there any signs of digoxin toxicity or marked changes in the pulse rate/rhythm – Monitor digoxin levels closely: should be smaller than 2 ng/ml – Older adults are particularly prone to digoxin toxicity – Hypokalemia makes the heart muscle more sensitive to digoxin, thereby increasing the possibility of developing digoxin toxicity 23

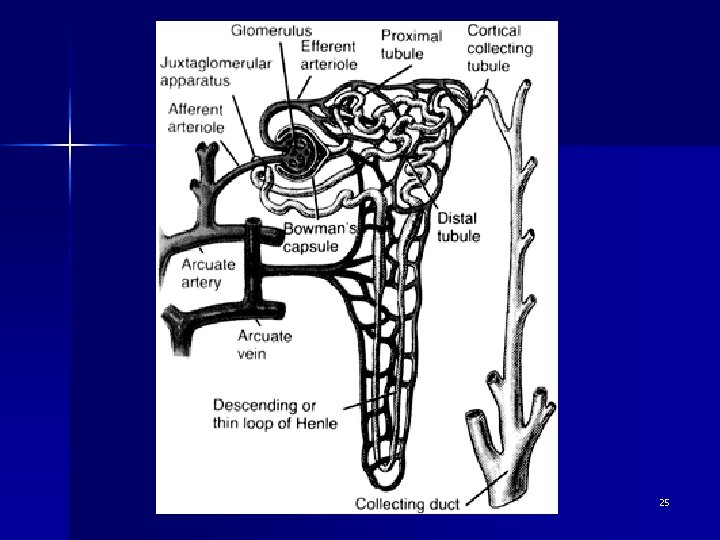
3) Antihypertensive Drugs – (i) Diuretics n Diuretics are drugs that increase renal excretion of water, sodium & other electrolytes, thereby increasing urine formation & output n Used in the management of heart failure, renal & hepatic disease, hypertension, ophthalmic surgery 24

25

3) Antihypertensive Drugs (Cont’d) – Thiazide diuretics: n Decrease reabsorption of Na, water, Cl & bicarbonate in the distal convoluted tubule n Hydrocholorothiazide – 25 -100 mg daily or BD po n Indapamide (Natrilix) – 2. 5 mg/1. 5 mg(S. R. ) daily po 26

3) Antihypertensive Drugs (Cont’d) – Loop Diuretics: n Inhibit Na & Cl reabsorption in the ascending loop of Henle n Frusemide – 20 -80 mg daily po n Bumetanide (Burinex) – 0. 5 -2 mg daily po 27

3) Antihypertensive Drugs (Cont’d) – Potassium-Sparing Diuretics: n Act directly on the distal tubule to decrease the exchange of Na for K – Amiloride : 5 -20 mg daily po – Triamterene: 100 -300 mg daily in divided dose po n Spironolactone – Block the Na-retaining effects of aldosterone in the distal tubule – 25 -200 mg daily po 28

3) Antihypertensive Drugs (Cont’d) – Combination Products n Thiazide & related diuretics are available in numerous fixed-dose combination with nondiuretic antihypertensive agents & with Ksparing diuretics. This can increase patient compliance & prevent K imbalances: – Dyazide (Hydrochlorothiazide 25 mg+Triamterene 50 mg) – Moduretic (Hydrochlorothiazide 50 mg+Amiloride 5 mg) – Hyzaar (Losartan 50 mg+Hydrochlorothiazide 12. 5 mg) 29

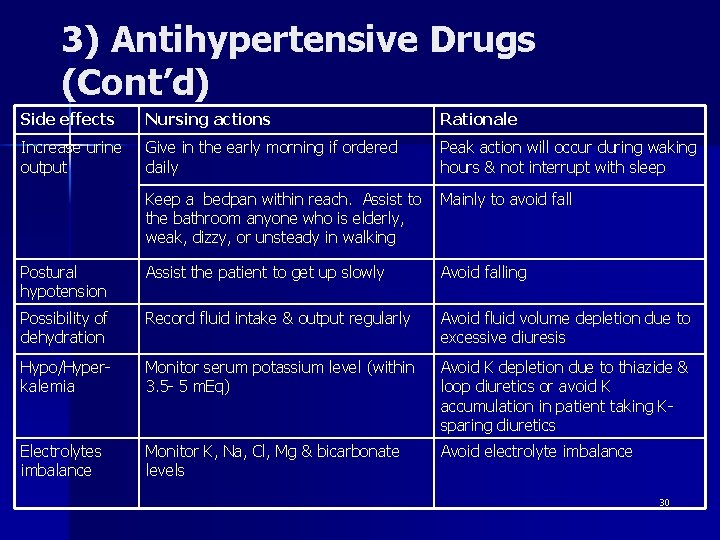
3) Antihypertensive Drugs (Cont’d) Side effects Nursing actions Rationale Increase urine output Give in the early morning if ordered daily Peak action will occur during waking hours & not interrupt with sleep Keep a bedpan within reach. Assist to the bathroom anyone who is elderly, weak, dizzy, or unsteady in walking Mainly to avoid fall Postural hypotension Assist the patient to get up slowly Avoid falling Possibility of dehydration Record fluid intake & output regularly Avoid fluid volume depletion due to excessive diuresis Hypo/Hyperkalemia Monitor serum potassium level (within 3. 5 - 5 m. Eq) Avoid K depletion due to thiazide & loop diuretics or avoid K accumulation in patient taking Ksparing diuretics Electrolytes imbalance Monitor K, Na, Cl, Mg & bicarbonate levels Avoid electrolyte imbalance 30

3) Antihypertensive Drugs (Cont’d) n (ii) Beta Blockers – Block beta-1 receptors in the heart – Hence: n Reduce heart rate n Reduce force of contraction n Reduced velocity impulse conduction through the AV node 31

3) Antihypertensive Drugs (Cont’d) – Used in: n Hypertension n Angina pectoris n Arrhythmias n Myocardial Infarction n Heart Failure 32

3) Antihypertensive Drugs (Cont’d) – Differ in: n n Receptor selectivity Intrinsic sympathomimetic activity (partial agonist activity), e. g. Oxprenolol. Pindolol, acebutolol Lipid solubility (Atenolol, nadolol, Sotalol are the most watersoluble) Duration of action, e. g. Esmolol 33

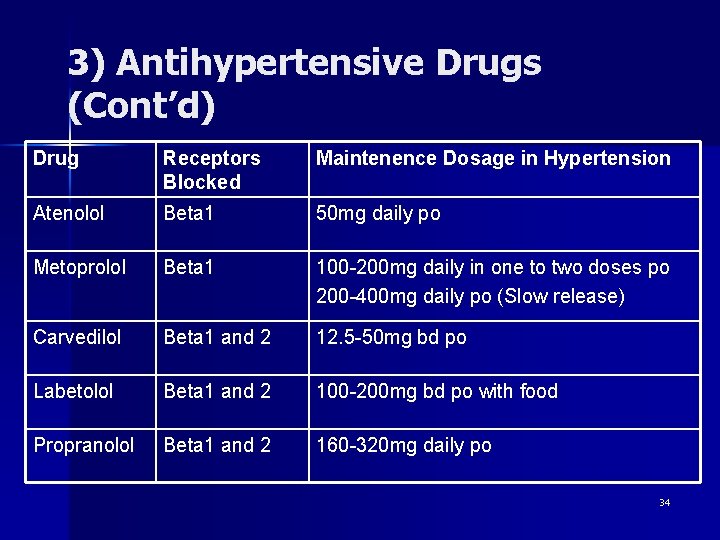
3) Antihypertensive Drugs (Cont’d) Drug Receptors Blocked Maintenence Dosage in Hypertension Atenolol Beta 1 50 mg daily po Metoprolol Beta 1 100 -200 mg daily in one to two doses po 200 -400 mg daily po (Slow release) Carvedilol Beta 1 and 2 12. 5 -50 mg bd po Labetolol Beta 1 and 2 100 -200 mg bd po with food Propranolol Beta 1 and 2 160 -320 mg daily po 34

3) Antihypertensive Drugs (Cont’d) Receptor Subtype Tissue Effects Alpha 1, 2 Vascular smooth muscle Contraction Beta 1 Heart Inc. Heart Rate Inc. Force of Contraction Beta 2 Smooth muscle Relaxation 35

3) Antihypertensive Drugs (Cont’d) – Adverse Effects n n n Bradycardia Hypotension Brochospasms GI disturbances Heart failure Fatigue n Nursing Alert – Check blood pressure & pulse frequently, especially when dosage is being increased 36

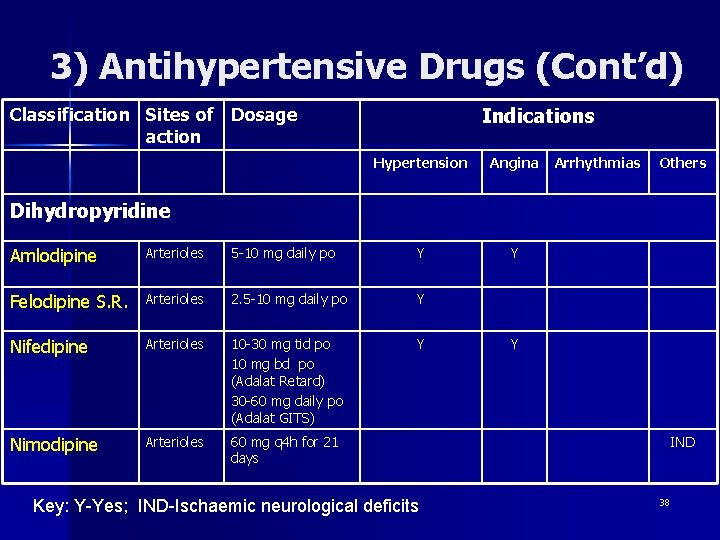
3) Antihypertensive Drugs (Cont’d) n (iii) Calcium Channel Blockers (CCB) – Drugs that prevent calcium ions from entering cells. – Have the greatest effect on the heart and blood vessels. – Widely used to treat hypertension, angina pectoris and cardiac dysrhythmias 37

3) Antihypertensive Drugs (Cont’d) Indications Classification Sites of Dosage action Hypertension Angina Y Arrhythmias Others Dihydropyridine Amlodipine Arterioles 5 -10 mg daily po Y Felodipine S. R. Arterioles 2. 5 -10 mg daily po Y Nifedipine Arterioles 10 -30 mg tid po 10 mg bd po (Adalat Retard) 30 -60 mg daily po (Adalat GITS) Y Nimodipine Arterioles 60 mg q 4 h for 21 days Key: Y-Yes; IND-Ischaemic neurological deficits Y IND 38

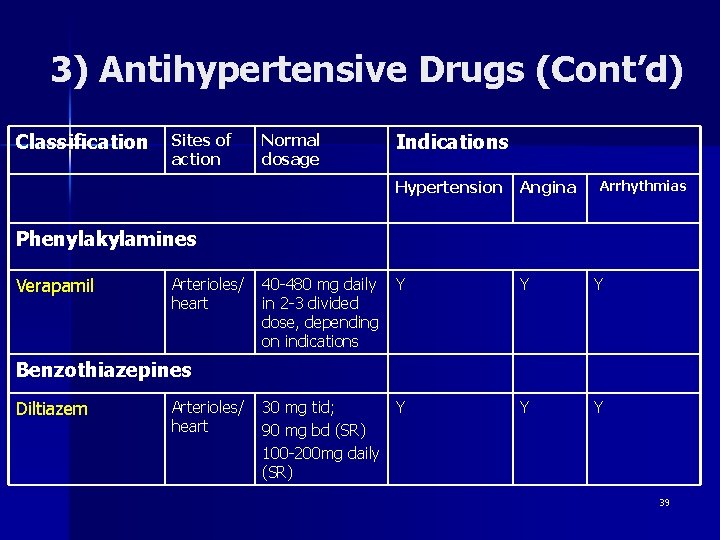
3) Antihypertensive Drugs (Cont’d) Classification Sites of action Normal dosage Indications Hypertension Angina Arrhythmias Phenylakylamines Verapamil Arterioles/ heart 40 -480 mg daily Y in 2 -3 divided dose, depending on indications Y Y 30 mg tid; Y 90 mg bd (SR) 100 -200 mg daily (SR) Y Y Benzothiazepines Diltiazem Arterioles/ heart 39

3) Antihypertensive Drugs (Cont’d) – Side effects: n Hypotension, dizziness, weakness, peripheral edema, headache, heart failure, pulmonary edema, nausea, constipation n Bradycardia (Verpamil, Diltiazem) n Tachycardia (Nifedipdine & other dihydropyridines) 40

3) Antihypertensive Drugs (Cont’d) n Nursing Alerts: – The older may have a greater hypotensive effect after taking CCB’s than younger adults. The nurse must monitor them closely during dosage adjustments – Make position changes slowly to minimize hypotensive effects – Some patients may experience dizziness and light-headedness, especially during early therapy. The nurse should assist the patient with all ambulatory activities and instructs the patients to ask for help when getting out of bed or ambulating 41

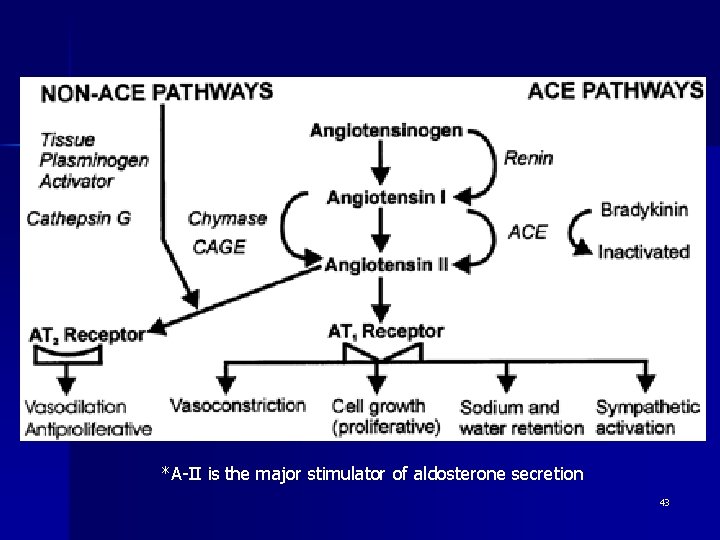
3) Antihypertensive Drugs (Cont’d) n (iv) Drug Acting on Renin-Angiotensin System – There are 2 families of drugs: n Angiotensin-converting inhibitors enzyme (ACE) – Block the enzyme (ACE) that normally converts angiotensin I to the potent vasoconstrictor angiotensin II – Decrease vasoconstriction & decrease aldosterone production, reducing retention of Na and water 42

*A-II is the major stimulator of aldosterone secretion 43

3) Antihypertensive Drugs (Cont’d) n (iv) Drug Acting on Renin-Angiotensin System – There are 2 families of drugs: n Angiotensin-converting inhibitors enzyme (ACE) – Block the enzyme (ACE) that normally converts angiotensin I to the potent vasoconstrictor angiotensin II – Decrease vasoconstriction & decrease aldosterone production, reducing retention of Na and water 44

3) Antihypertensive Drugs (Cont’d) n Used to treat hypertension, heart failure, myocardial infarction, and nephropathy – – Enalapril 10 -40 mg/day in 1 or 2 doses Lisinopril 10 -40 mg once daily Perindopril 2 -8 mg daily Ramipril 1. 25 -10 mg once daily n Side – – – Effects: Can produce serious first-dose hypotension Cough, due to accumulation of bradykinin Hyperkalaemia, due to inhibition of aldosterone release 45

3) Antihypertensive Drugs (Cont’d) n Angiotensin II receptor blockers (ARBs) – Compete with angiotensin II for tissue binding sites & prevent angiotensin II from combining with its receptors in body tissues – Used for hypertension, may be used as an alternative to ACE inhibitors in the management of heart failure and diabetic nephropathy. n n n Irbesartan 150 -300 mg once daily Losartan 25 -100 mg once daily Valsartan 80 -160 mg once daily 46

3) Antihypertensive Drugs (Cont’d) n Side-effects – Hypotension – Less likely to cause cough and hyperkalaemia than ACE inhibitors 47

3) Antihypertensive Drugs (Cont’d) n Nursing Alerts Potential Adverse Effects Nursing Actions ACE inhbitors and Angiotensin II receptor antagonists may cause first dose hypotension Instruct the patient to lie down if hypotension develops ACE inhibitors may produce cough Warn patients about the possibility of cough. Consult the doctor if the cough is bothersome to the patient 48

3) Antihypertensive Drugs (Cont’d) n Nursing Alerts (cont’d) Potential Adverse Effects Nursing Actions ACE inhibitors may cause hyperkalaemia Avoid potassium supplements, potassium containing salt substitutes and potassiumsparing diuretics ACE inhibitors and Angiotensin II receptor antagonists are contra-indicated in pregnancy Avoid these dugs in pregnancy 49

4) Antianginal Drugs n Organic Nitrates – Used to treat or prevent angina – Mechanism: Ø Nitrates are converted to NO in vascular smooth muscle Ø NO activates guanylate cyclase Ø Increase formation of c. GMP so that the intracellular calcium levels decrease Ø Vasodilation 50

4) Antianginal Drugs(Cont’d) – Relieves anginal pain by relaxing smooth muscles in the blood vessels (vasodilation) by several mechanisms n Dilate veins n Dilate coronary arteries n Dilate arterioles 51

4) Antianginal Drugs (Cont’d) – Most widely used nitrate is nitroglycerin (Glyceryl trinitrate) n Since it is highly lipid soluble, it can be administered by sublingual and transdermal route, as well as oral and intravenous routes 52

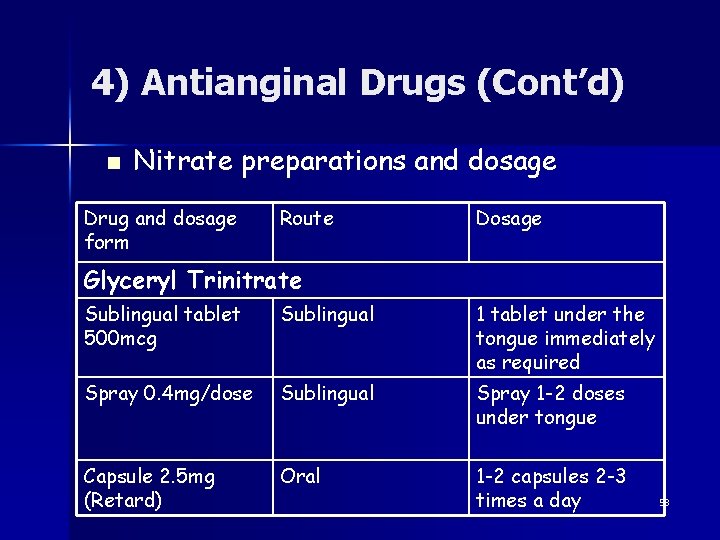
4) Antianginal Drugs (Cont’d) n Nitrate preparations and dosage Drug and dosage form Route Dosage Glyceryl Trinitrate Sublingual tablet 500 mcg Sublingual 1 tablet under the tongue immediately as required Spray 0. 4 mg/dose Sublingual Spray 1 -2 doses under tongue Capsule 2. 5 mg (Retard) Oral 1 -2 capsules 2 -3 times a day 53

4) Antianginal Drugs (Cont’d) Drug and dosage form Route Dosage Glyceryl Trinitrate (Cont’d) Transdermal patches 5 mg / 10 mg Transdermal 1 patch every 24 hours Isosorbide Mononitrate Tablet 20 mg Oral 20 mg bd to tid / 40 mg bd Tablet 60 mg (controlled release) Oral 30 -120 mg in the morning Capsule 50 mg (sustained release) Oral 1 -2 capsules in the 54 morning

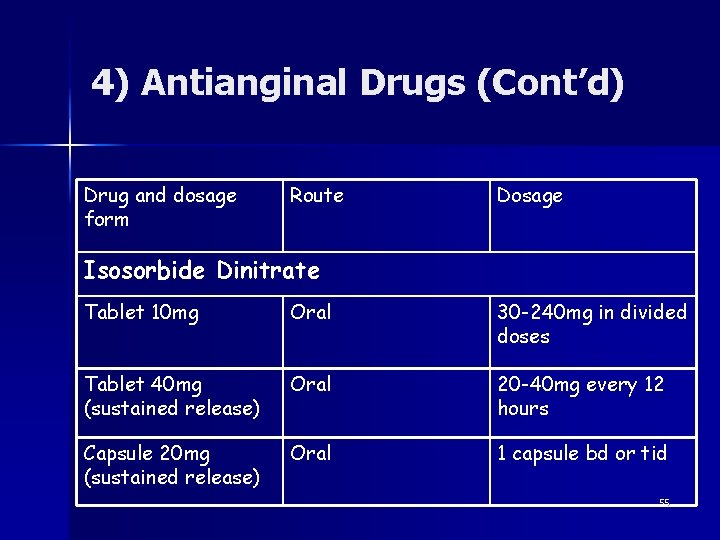
4) Antianginal Drugs (Cont’d) Drug and dosage form Route Dosage Isosorbide Dinitrate Tablet 10 mg Oral 30 -240 mg in divided doses Tablet 40 mg (sustained release) Oral 20 -40 mg every 12 hours Capsule 20 mg (sustained release) Oral 1 capsule bd or tid 55

4) Antianginal Drugs (Cont’d) – Tolerance n Tolerance to nitrate induced vasodilation can develop rapidly n This may be due to depletion of sulfhydryl (S-H) groups in the vascular smooth muscle. These groups are needed to convert nitrate to NO 56

4) Antianginal Drugs (Cont’d) – Adverse Effects n Headache n Orthostatic hypotension – Symptoms include light headedness and dizziness n Reflex tachycardia 57

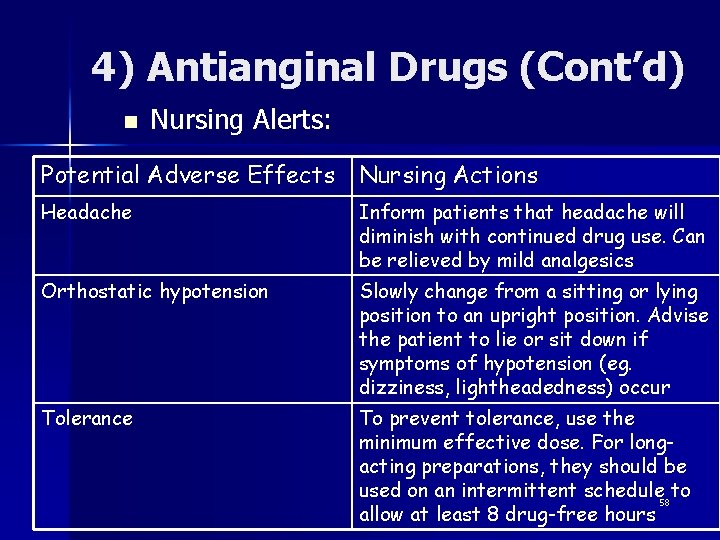
4) Antianginal Drugs (Cont’d) n Nursing Alerts: Potential Adverse Effects Nursing Actions Headache Inform patients that headache will diminish with continued drug use. Can be relieved by mild analgesics Orthostatic hypotension Slowly change from a sitting or lying position to an upright position. Advise the patient to lie or sit down if symptoms of hypotension (eg. dizziness, lightheadedness) occur Tolerance To prevent tolerance, use the minimum effective dose. For longacting preparations, they should be used on an intermittent schedule 58 to allow at least 8 drug-free hours

5) Antiarrhythmic Drugs Antiarrhythmic drugs are primary used to treat cardiac arrhythmias, which is a disturbance or irregularity in the heart rate, rhythm, or both n Antiarrhythmic drugs are divided into 4 classes n 59

5) Antiarrhythmic Drugs (Cont’d) n (i) Class I – Sodium channel blockers – Have a membrance-stablizing or anaesthetic effect on the cell of the myocardium – Are subdivided into I-A, I-B, I-C n I-A: n Quinidine – 200 -400 mg tid or qid po n Procainamide – 25 -50 mg/min slow iv injection; max: 1 g daily 60

5) Antiarrhythmic Drugs (Cont’d) n I-B: n Lidocaine – 50 - 100 mg single bolus injection; followed by 14 mg/min infusion n I-C: n Flecainide – 100 mg bd po; max: 400 mg daily n Propafenone – 150 -300 mg tid po 61

5) Antiarrhythmic Drugs (Cont’d) – Side effects of Class I: n Nausea, vomiting n Dizziness n Visual disturbances n Pro-arrhythmic effect n Heart block 62

5) Antiarrhythmic Drugs (Cont’d) n (II) Class II – Beta Blockers – Block sympathetic stimulation of beta receptors in the heart & decrease the heart rate n Propranolol – 10 -40 mg tid or qid po n Acebutolol – 400 -1200 mg daily po in 2 to 3 divided dose n Esmolol – 50 -200 mcg/kg/min IV infusion 63

5) Antiarrhythmic Drugs (Cont’d) – Side effects of Class II: n Nausea n Headache n Hypotension n Dizziness 64

5) Antiarrhythmic Drugs (Cont’d) n (III) Class III – Potassium channel blocker – Prolong duration of action potential, slow repolarization, and prolong the refractory period in both atria and ventricles n Amiodarone – 200 mg one to three times daily po n Bretylium – 5 -10 mg/kg IV infusion over 15 -30 min q 6 -8 h 65

5) Antiarrhythmic Drugs (Cont’d) n Sotalol – Has combined Class II & Class III effects – A beta blocker that also delays repolarization – 160 -320 mg po daily in 2 divided dose – Side effects of Class III: n Proarrhythmias (Amiodarone & Sotalol) n Hypotension (Bretylium & Sotalol) n Malaise, fatigue & tremor (Amiodarone) 66

5) Antiarrhythmic Drugs (Cont’d) n Class IV: – Calcium Channel Blockers (CCB) – Block the movement of Ca into conductile & contractile myocardial cells – Verapamil & Diltiazem are the only approved CCB in arrhythmias n Verapamil – 40 -120 mg tid po 67

5) Antiarrhythmic Drugs (Cont’d) n Diltiazem – 0. 25 mg/kg IV injection over 2 min, second bolus of 0. 35 mg/kg if needed; followed by 5 -15 mg/hr continuous IV infusion if necessary – Side effects of Class IV: n Proarrhythmias n Heart (Verapamil) block n Hypotension, headache, dizziness, constipation 68

5) Antiarrhythmic Drugs (Cont’d) n Nursing Alerts – Antiarrhythmic drugs are capable of causing new arrhythmias, as well as an exacerbation of existing arrhythmias – Older adults taking antiarrhythmic drugs are at greater risk for adverse reactions such as development of additional arrhythmias or aggravating of existing arrhythmias, hypotension, and congestive heart failure. Careful monitoring is necessary for early identification and management of adverse effects 69

6) Drugs used for Dyslipidemia n Used in the management of elevated blood lipids, which is a major risk factor for atherosclerosis and vascular disorders such as coronary artery disease and strokes 70

6) Drugs used for Dyslipidemia (Cont’d) n (i) HMG Co. A reductase inhibitors (Statins) – Inhibits HMG Co. A reductase, the ratelimiting enzyme in cholesterol synthesis – Increase LDL receptors in hepatocytes n This enables hepatocytes to remove more LDLs from the blood – Also decrease VLDL levels and increase HDL levels 71

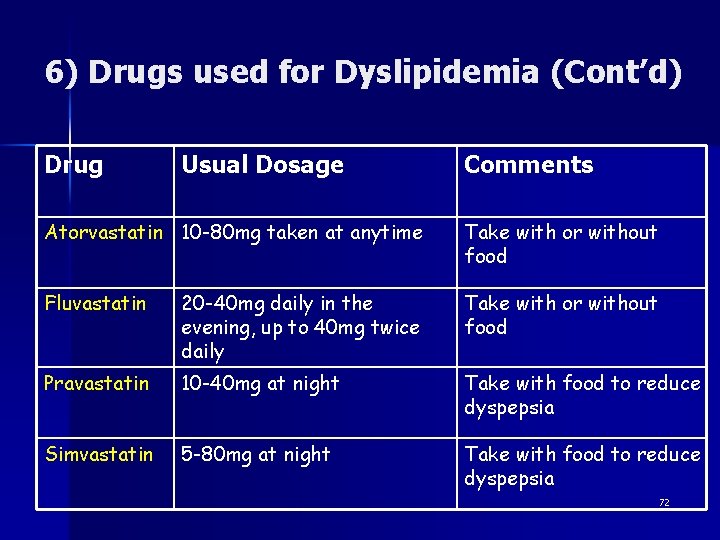
6) Drugs used for Dyslipidemia (Cont’d) Drug Usual Dosage Comments Atorvastatin 10 -80 mg taken at anytime Take with or without food Fluvastatin 20 -40 mg daily in the evening, up to 40 mg twice daily Take with or without food Pravastatin 10 -40 mg at night Take with food to reduce dyspepsia Simvastatin 5 -80 mg at night Take with food to reduce dyspepsia 72

6) Drugs used for Dyslipidemia (Cont’d) – Adverse Effects n Headache, GI side effects (e. g. abdominal pain, flatulence, diarrhoea, nausea and vomiting) n Hepatoxicity n Myopathy 73

6) Drugs used for Dyslipidemia (Cont’d) n (ii) Fibric acid derivatives (Fibrates) – Increase oxidation of fatty acids in liver and muscle tissue, decrease hepatic production of triglycerides, decrease VLDL cholesterol and increase HDL cholesterol – Main indication is hypertriglceridemia (high plasma triglycerides) 74

6) Drugs used for Dyslipidemia (Cont’d) Drug and dosage form Usual Dosage Clofibrate capsule 500 mg 2 g daily in 2 -4 divided doses Fenofibrate Capsule 100 mg 3 capsules daily in the course of main meals Capsule (Micronized fenofibrate) 200 mg 1 capsule daily 75

6) Drugs used for Dyslipidemia (Cont’d) Drug and dosage form Usual Dosage Gemfibrozil Capsule 300 mg 1. 2 g daily in 2 divided doses Usual range 0. 9 -1. 5 g daily Tablet 600 mg 76

6) Drugs used for Dyslipidemia (Cont’d) – Adverse Effects n Nausea, vomiting and GI upset n Cholelithiasis (stones in the gall bladder) and cholecystitis (inflammation of the gallbladder) n Myopathy 77

6) Drugs used for Dyslipidemia (Cont’d) n (iii) Bile acid sequestrants – Bind bile acids in the intestinal lumen. This causes the bile acids to be excreted in faeces and prevents them being re-circulated to the liver – Mainly used as an adjunct to Statins to decrease LDL cholesterol levels 78

6) Drugs used for Dyslipidemia (Cont’d) – Cholestyramine n Usual dosage – 12 -24 g daily in water in one to four divided doses; Max: 36 g daily n Adverse effects – Constipation, diarrhoea, nausea, vomiting, gastro -intestinal discomfort – Decreased absorption of fat-soluble vitamins 79

6) Drugs used for Dyslipidemia (Cont’d) n (iv) Nicotinic acid – Inhibits mobilization of free fatty acids from peripheral tissues, thereby reducing hepatic synthesis of triglycerides and secretion of VLDL, which leads to decreased production of of LDL cholesterol – Besides reducing LDL and VLDL levels, also effective in increasing HDL levels 80

6) Drugs used for Dyslipidemia (Cont’d) – Normal dose n 1 -2 g three times daily – Adverse effects n Flushing, itching, nausea, vomiting, diarrhoea n Hepatotoxic n Hyperglycaemia and hyperuricaemia 81

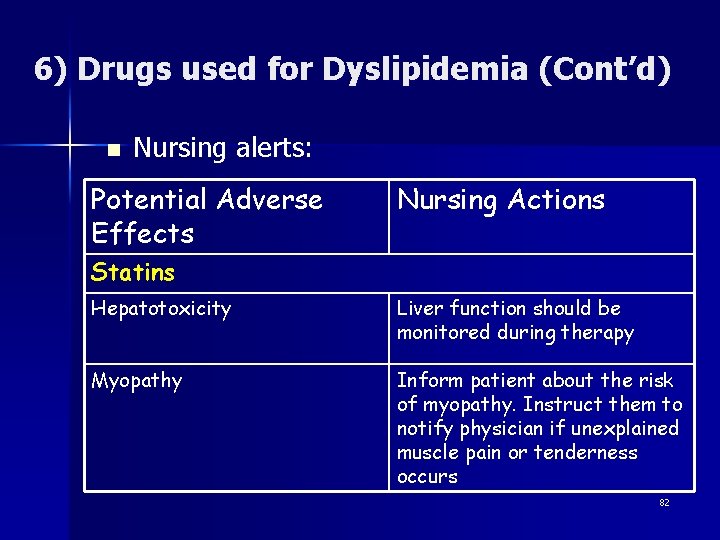
6) Drugs used for Dyslipidemia (Cont’d) n Nursing alerts: Potential Adverse Effects Nursing Actions Statins Hepatotoxicity Liver function should be monitored during therapy Myopathy Inform patient about the risk of myopathy. Instruct them to notify physician if unexplained muscle pain or tenderness occurs 82

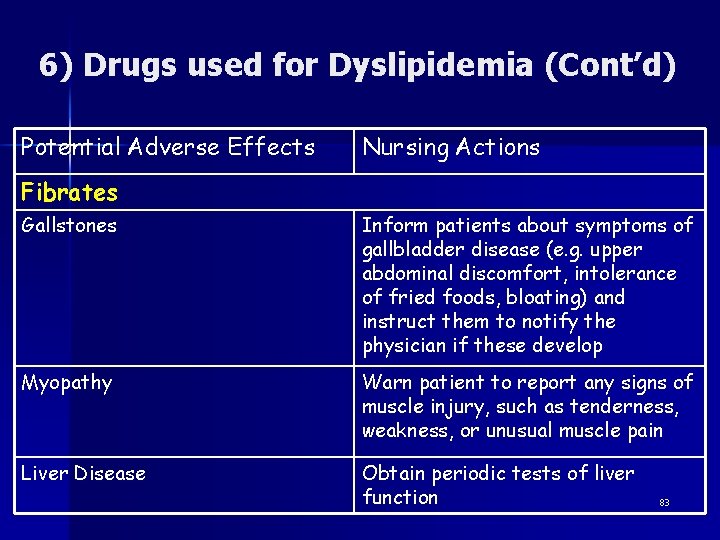
6) Drugs used for Dyslipidemia (Cont’d) Potential Adverse Effects Nursing Actions Fibrates Gallstones Inform patients about symptoms of gallbladder disease (e. g. upper abdominal discomfort, intolerance of fried foods, bloating) and instruct them to notify the physician if these develop Myopathy Warn patient to report any signs of muscle injury, such as tenderness, weakness, or unusual muscle pain Liver Disease Obtain periodic tests of liver function 83

6) Drugs used for Dyslipidemia (Cont’d) Potential Adverse Effects Nursing Actions Bile acid sequestrants Constipation Inform patients that constipation can be minimized by increasing dietary fiber and fluids. A mild laxative may be used if needed. Vitamin deficiency Absorption of fat-soluble vitamins (A, D, E, K) may be impaired. Vitamin supplements may be required 84

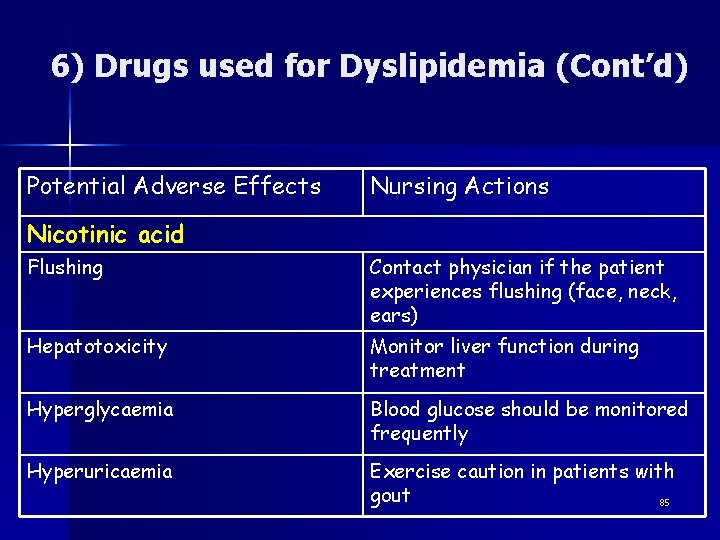
6) Drugs used for Dyslipidemia (Cont’d) Potential Adverse Effects Nursing Actions Nicotinic acid Flushing Contact physician if the patient experiences flushing (face, neck, ears) Hepatotoxicity Monitor liver function during treatment Hyperglycaemia Blood glucose should be monitored frequently Hyperuricaemia Exercise caution in patients with gout 85

87