Assessment of Skeleton Health Tuan Van Nguyen and





































- Slides: 71

Assessment of Skeleton Health Tuan Van Nguyen and Nguyen Dinh Nguyen Garvan Institute of Medical Research Sydney, Australia Vietnam Osteoporosis Workshop, HCMC 2006

Overview • Background • Normal bone and bone remodelling • Bone loss and age • Definitions • Measurements of bone strength: – Bone mass and DXA, QUS – Bone turnover markers Vietnam Osteoporosis Workshop, HCMC 2006

Background • Aging population: fastest growing age group • Osteoporosis and osteoporotic fracture: agerelated disorders • Osteoporosis and osteoporotic fracture: – Common – Cause serious disability and excess mortality – Major economic burden on healthcare system Vietnam Osteoporosis Workshop, HCMC 2006

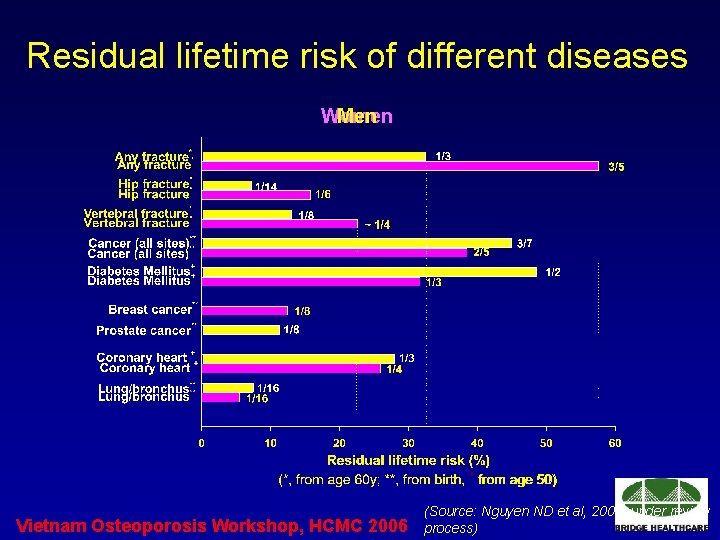
Residual lifetime risk of different diseases Women Men Vietnam Osteoporosis Workshop, HCMC 2006 (Source: Nguyen ND et al, 2006, under review process)

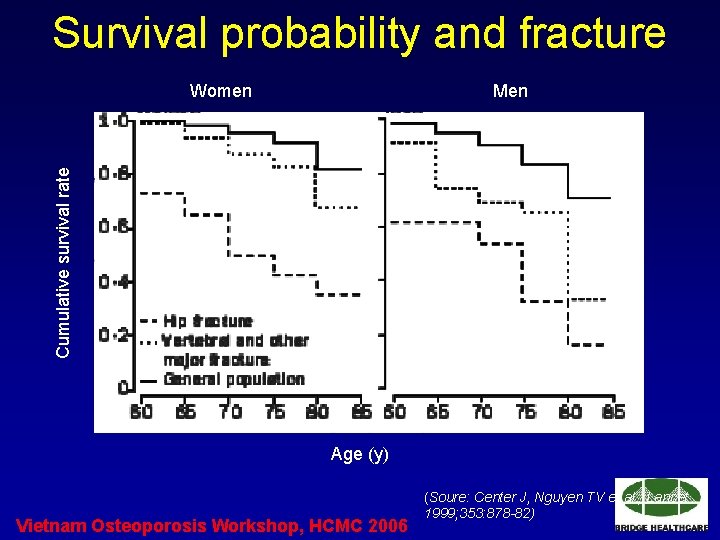
Survival probability and fracture Men Cumulative survival rate Women Age (y) Vietnam Osteoporosis Workshop, HCMC 2006 (Soure: Center J, Nguyen TV et al. , Lancet 1999; 353: 878 -82)

Burden of Osteoporotic fractures • Annual cost of all osteoporotic fractures: $20 billion in USA and ~$30 billion on EU 1. • Worldwide direct and indirect cost of hip fracture: US$131. 5 billion 2. (Sources: 1 Cummings et al. , Lancet 2002; 359: 1761 -67; 2 Johnell O, Am J Med 1997; 103: 20 S-26) Vietnam Osteoporosis Workshop, HCMC 2006

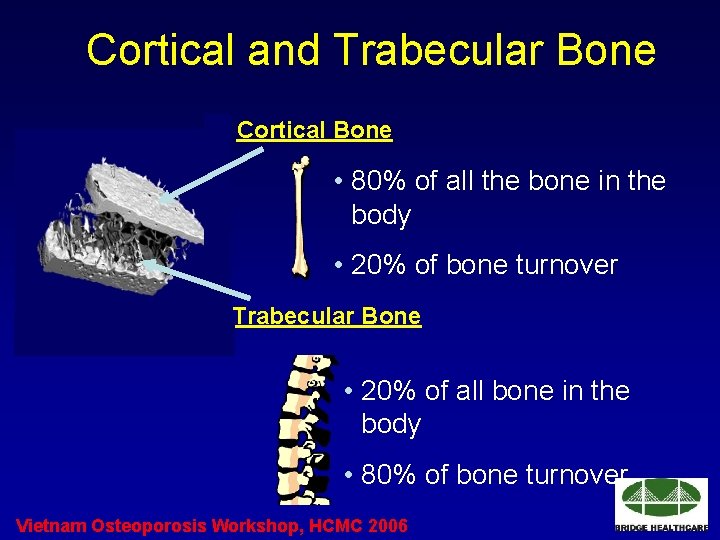
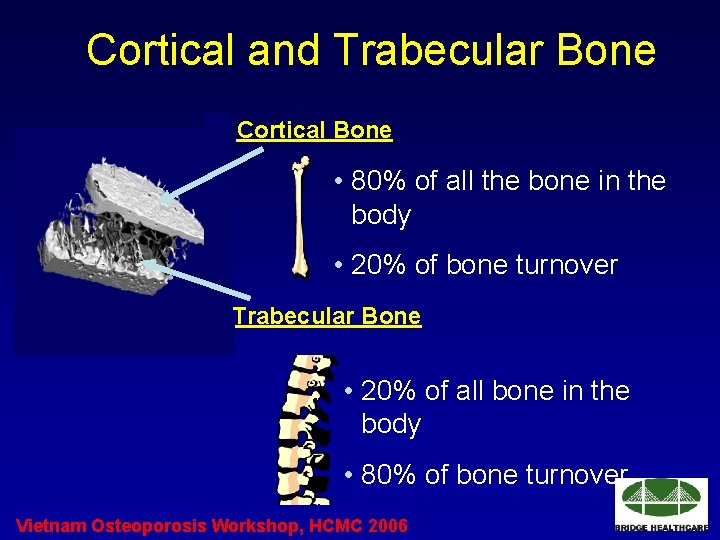
Cortical and Trabecular Bone Cortical Bone • 80% of all the bone in the body • 20% of bone turnover Trabecular Bone • 20% of all bone in the body • 80% of bone turnover Vietnam Osteoporosis Workshop, HCMC 2006

Cortical (Compact) Bone • 80% of the skeletal mass • Provides a protective outer shell around every bone in the body • Slower turnover • Provides strength and resists bending or torsion Vietnam Osteoporosis Workshop, HCMC 2006

Trabecular (Cancellous) Bone 20% of the skeletal mass, but 80% of the bone surface. • • less dense, more elastic, and higher turnover rate than cortical bone. • appears spongy • found in the epipheseal and metaphysal regions of long bones and throughout the interior of short bones. • constitutes most of the bone tissue of the axial skeleton (skull, ribs and spine). • interior scaffolding maintains bone shape despite compressive forces. Vietnam Osteoporosis Workshop, HCMC 2006

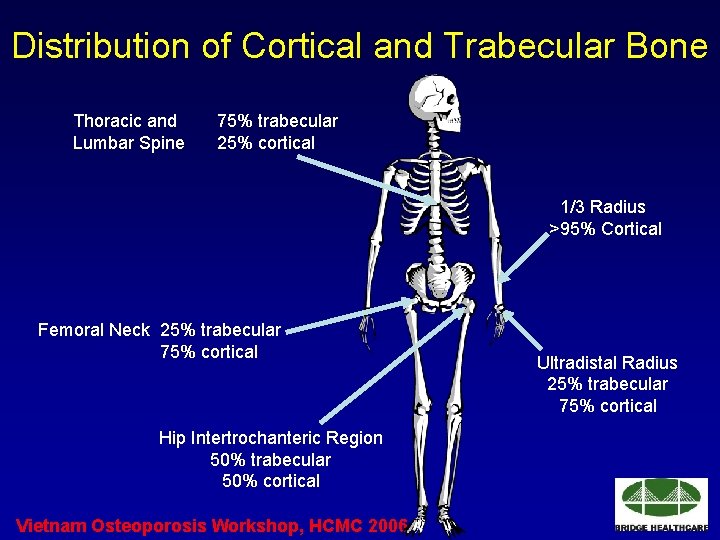
Distribution of Cortical and Trabecular Bone Thoracic and Lumbar Spine 75% trabecular 25% cortical 1/3 Radius >95% Cortical Femoral Neck 25% trabecular 75% cortical Hip Intertrochanteric Region 50% trabecular 50% cortical Vietnam Osteoporosis Workshop, HCMC 2006 Ultradistal Radius 25% trabecular 75% cortical

How does bone loss happen? Bone is a living, growing, tissue • Healthy bones are not quiescent. They are constantly being remodeled. • This is not simply a problem of bony destruction, but imbalance between the formation and destruction of bone. Vietnam Osteoporosis Workshop, HCMC 2006

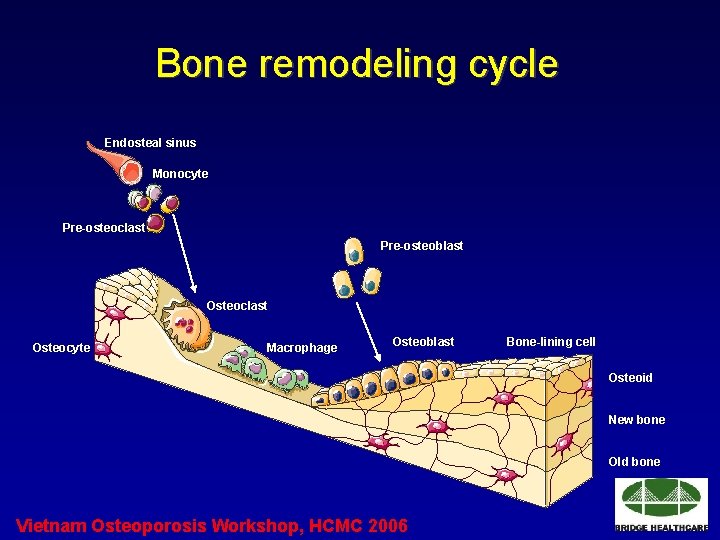
Bone remodeling cycle Endosteal sinus Monocyte Pre-osteoclast Pre-osteoblast Osteocyte Macrophage Osteoblast Bone-lining cell Osteoid New bone Old bone Vietnam Osteoporosis Workshop, HCMC 2006

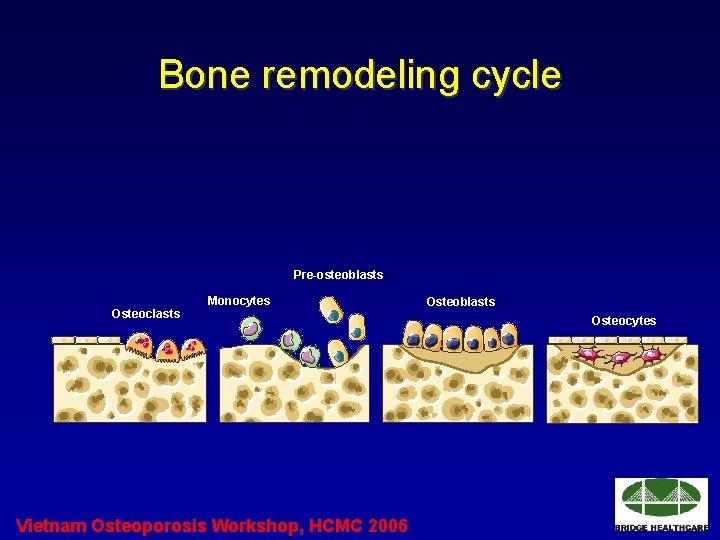
Bone remodeling cycle Pre-osteoblasts Osteoclasts Monocytes Vietnam Osteoporosis Workshop, HCMC 2006 Osteoblasts Osteocytes

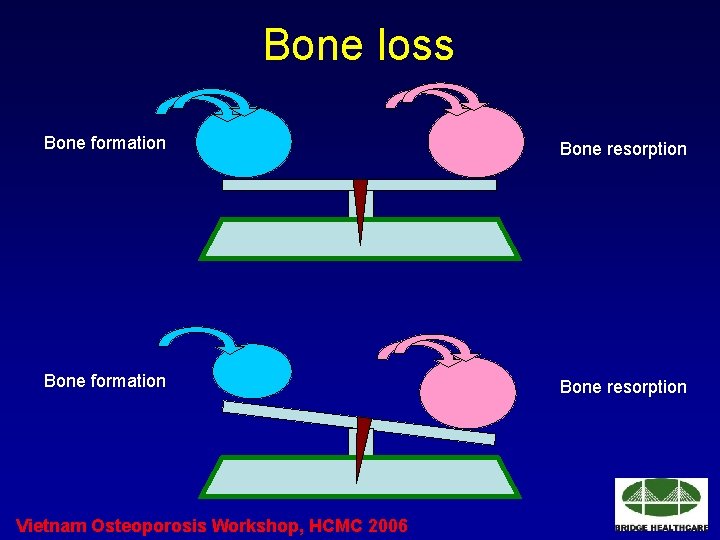
Bone loss Bone formation Bone resorption Vietnam Osteoporosis Workshop, HCMC 2006

Bone Remodelling: Normal and Osteoporosis Vietnam Osteoporosis Workshop, HCMC 2006

Vietnam Osteoporosis Workshop, HCMC 2006

Vietnam Osteoporosis Workshop, HCMC 2006

Vietnam Osteoporosis Workshop, HCMC 2006

Vietnam Osteoporosis Workshop, HCMC 2006

Vietnam Osteoporosis Workshop, HCMC 2006

Vietnam Osteoporosis Workshop, HCMC 2006

Vietnam Osteoporosis Workshop, HCMC 2006

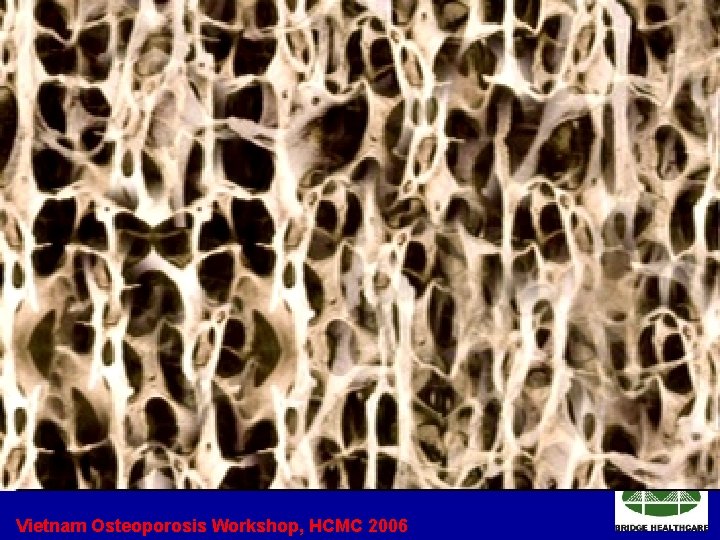
Bone mass declines with age • Remodeling occurs at discrete foci called bone remodeling units (BRUs). • Number of active BRUs with age bone turnover. • Osteoblasts not able to completely fill cavities created by osteoclasts and less mineralized bone is formed. • Endosteal bone loss partially compensated by periosteal bone formation trabecular thinning. Vietnam Osteoporosis Workshop, HCMC 2006

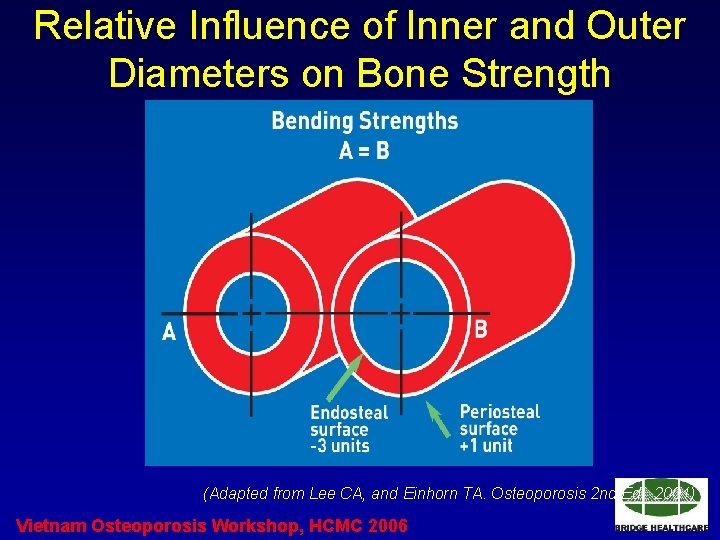
Relative Influence of Inner and Outer Diameters on Bone Strength (Adapted from Lee CA, and Einhorn TA. Osteoporosis 2 nd Ed. 2001) Vietnam Osteoporosis Workshop, HCMC 2006

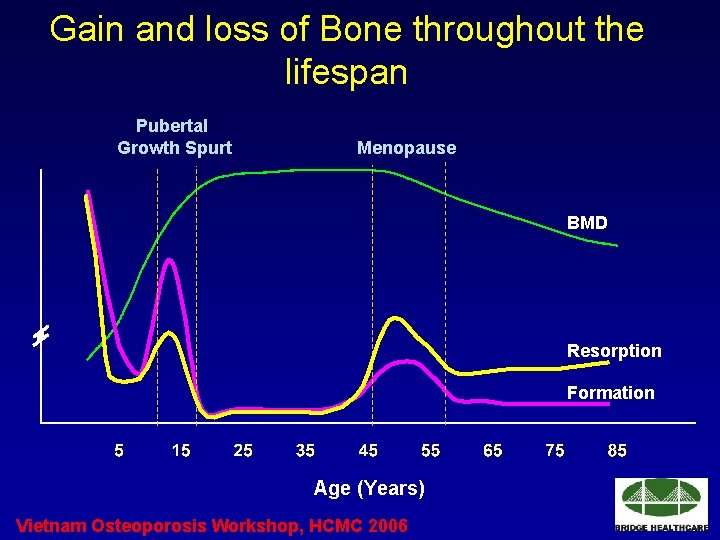
Gain and loss of Bone throughout the lifespan Pubertal Growth Spurt Menopause BMD Resorption Formation Age (Years) Vietnam Osteoporosis Workshop, HCMC 2006

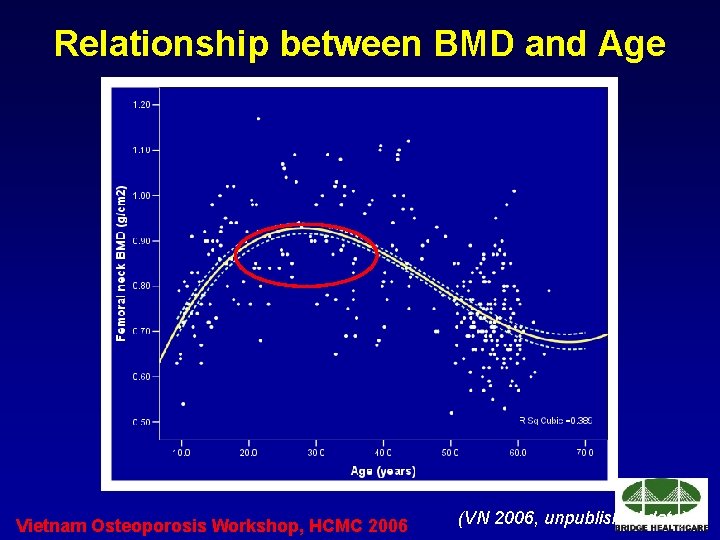
Relationship between BMD and Age Vietnam Osteoporosis Workshop, HCMC 2006 (VN 2006, unpublished data)

Definition of Osteoporosis (WHO) A systematic skeleton disease characterized by: - low bone mass - microarchitectural deterioration of bone tissue - consequent increase in bone fragility and susceptibility to fracture Consensus Development Conference: Diagnosis, Prophylaxis, and Treatment of Osteoporosis, Am J Med 1993; 94: 646 -650. WHO Study Group 1994. Vietnam Osteoporosis Workshop, HCMC 2006

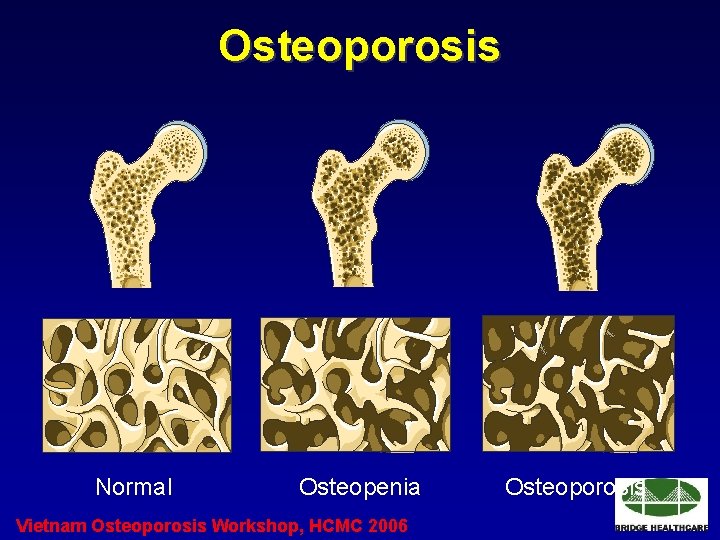
Osteoporosis Normal Osteopenia Vietnam Osteoporosis Workshop, HCMC 2006 Osteoporosis

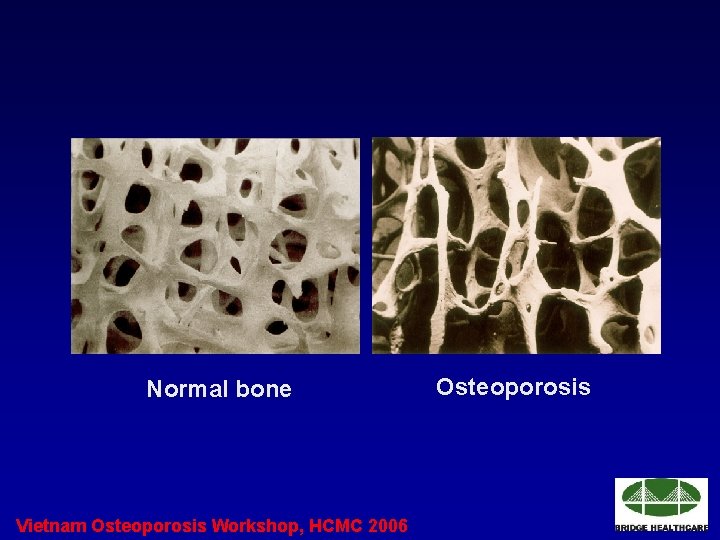
Normal bone Vietnam Osteoporosis Workshop, HCMC 2006 Osteoporosis

Definition of Osteoporosis (NIH) Osteoporosis is defined as a skeletal disorder characterized by: -compromised bone strength predisposing a person to an increased risk of fracture. -bone strength primarily reflects the integration of bone density and bone quality. (Source: NIH Consensus Development Panel on Osteoporosis JAMA 285: 785 -95; 2001) Vietnam Osteoporosis Workshop, HCMC 2006

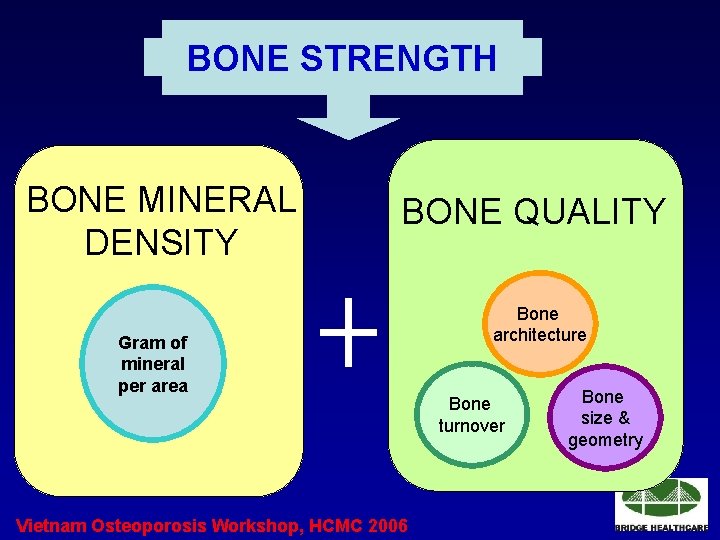
BONE STRENGTH BONE MINERAL DENSITY BONE QUALITY Gram of mineral per area Vietnam Osteoporosis Workshop, HCMC 2006 Bone architecture Bone turnover Bone size & geometry

Bone Quality • • • Architecture Turnover Rate Damage Accumulation Degree of Mineralization Properties of the collagen/mineral matrix ( NIH Consensus Development Panel on Osteoporosis. JAMA 285: 785 -95; 2001) Vietnam Osteoporosis Workshop, HCMC 2006

Bone mass, Bone mineral density (BMD) • Bone mass = the amount of bone tissue as the total of protein and mineral or the amount of mineral in the whole skeleton or in a particular segment of bone. (unmeasurable) • BMD = the average concentration of mineral per unit area assessed in 2 dimensions (measurable) Vietnam Osteoporosis Workshop, HCMC 2006

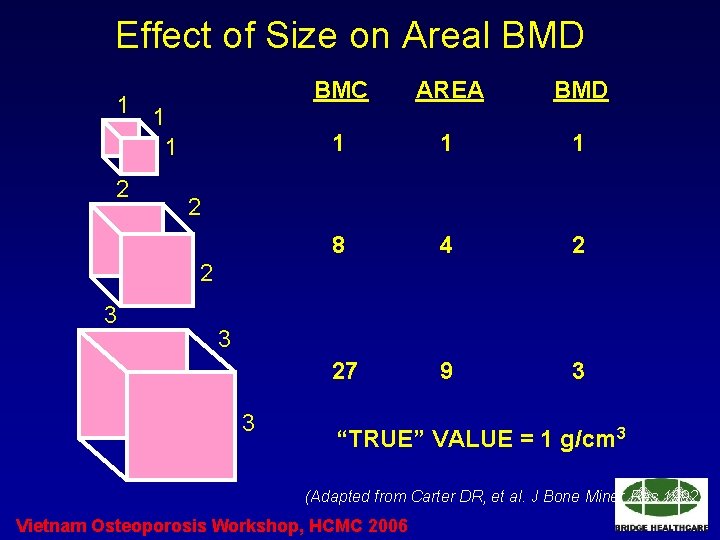
Effect of Size on Areal BMD 1 1 1 2 BMC AREA BMD 1 1 1 8 4 2 27 9 3 2 2 3 3 3 “TRUE” VALUE = 1 g/cm 3 (Adapted from Carter DR, et al. J Bone Miner Res 1992) Vietnam Osteoporosis Workshop, HCMC 2006

Bone Densitometry • Non-invasive test for measurement of BMD • Major technologies – Dual-energy X-ray Absorptiometry (DXA) – Quantitative Ultrasound (QUS) – Quantitative Computerized Tomography (QCT) • Many manufacturers • Numerous devices • Different skeletal sites Vietnam Osteoporosis Workshop, HCMC 2006

DXA (or DEXA) Vietnam Osteoporosis Workshop, HCMC 2006

DXA (or DEXA) • Gold-standard” for BMD measurement • Measures “central” or “axial” skeletal sites: spine and hip • May measure other sites: total body and forearm • Extensive epidemiologic data • Correlation with bone strength in-vitro • Validated in many clinical trials Vietnam Osteoporosis Workshop, HCMC 2006

DXA Technology Detector (detects 2 tissue types - bone and soft tissue) Very low radiation to patient. Patient Photons Very little scatter radiation to technologist Collimator (pinhole for pencil beam, slit for fan beam) X-ray Source (produces 2 photon energies with different attenuation profiles) Vietnam Osteoporosis Workshop, HCMC 2006

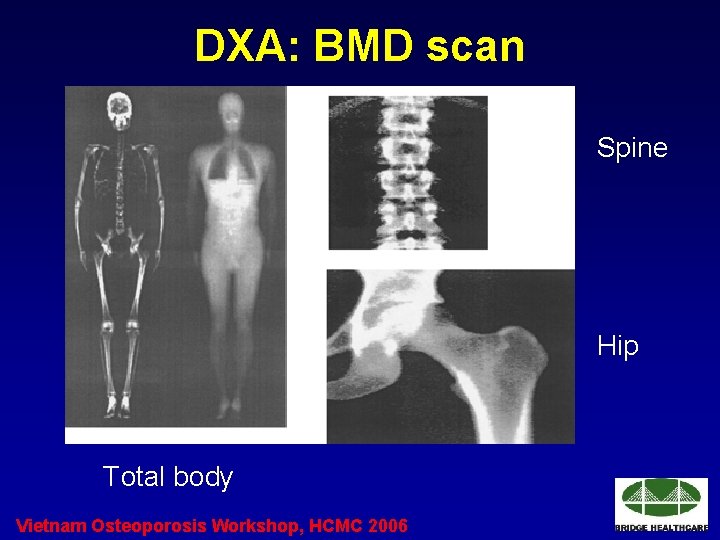
DXA: BMD scan Spine Hip Total body Vietnam Osteoporosis Workshop, HCMC 2006

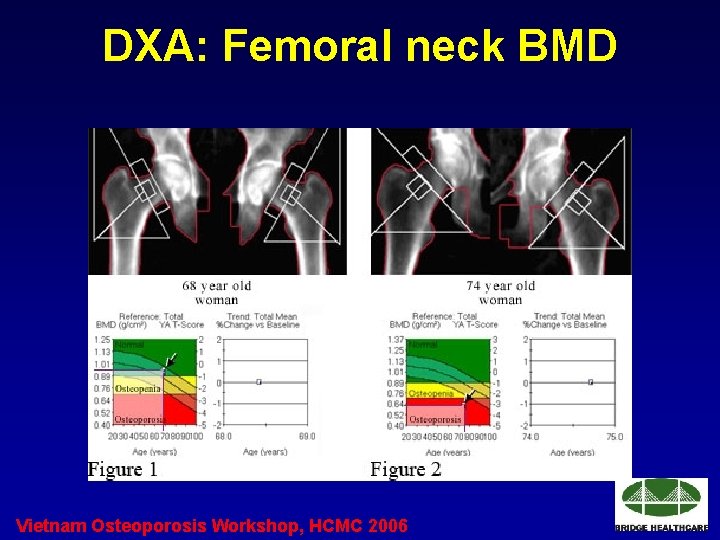
DXA: Femoral neck BMD Vietnam Osteoporosis Workshop, HCMC 2006

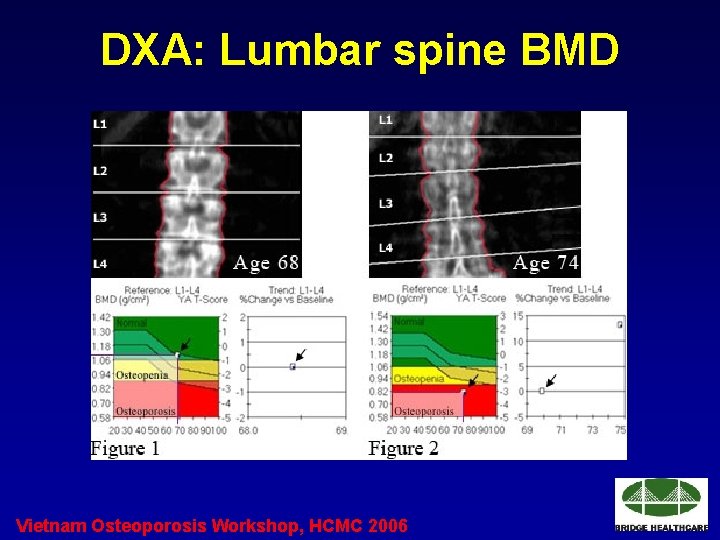
DXA: Lumbar spine BMD Vietnam Osteoporosis Workshop, HCMC 2006

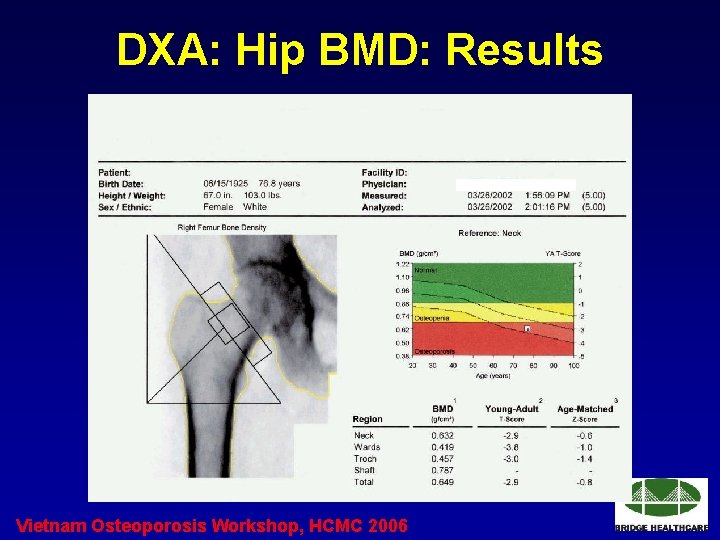
DXA: Hip BMD: Results Vietnam Osteoporosis Workshop, HCMC 2006

Which Skeletal Sites Should Be Measured? Every Patient • Spine – L 1 -L 4 (L 2 -L 4) • Hip – Total Proximal Femur – Femoral Neck Some Patients • Forearm (33% Radius) – If hip or spine cannot be measured – Hyperparathyroidism – Very obese – Trochanter Vietnam Osteoporosis Workshop, HCMC 2006

BMD measurement: subject to variability • In vivo/in situ BMD inaccuracy: effect of bone structure, bone size and shape, and extra-osseous soft tissue • Measurement error: within subject and between-subject variations. • Between machine variation. Vietnam Osteoporosis Workshop, HCMC 2006

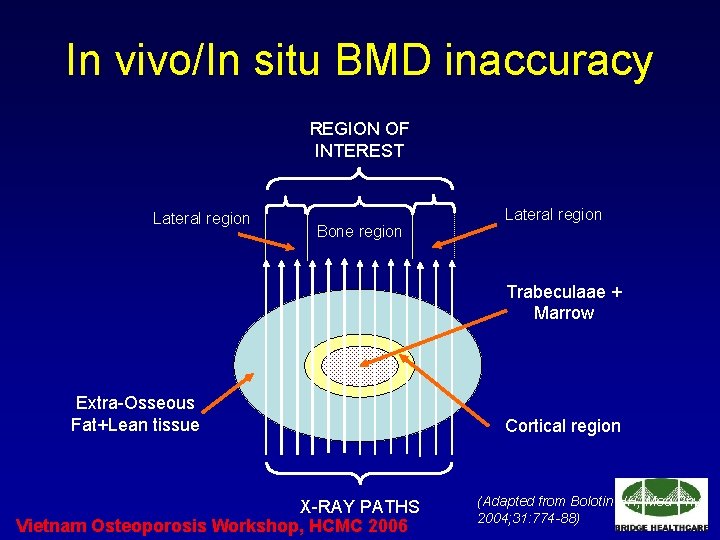
In vivo/In situ BMD inaccuracy REGION OF INTEREST Lateral region Bone region Lateral region Trabeculaae + Marrow Extra-Osseous Fat+Lean tissue X-RAY PATHS Vietnam Osteoporosis Workshop, HCMC 2006 Cortical region (Adapted from Bolotin HH, Med Phys 2004; 31: 774 -88)

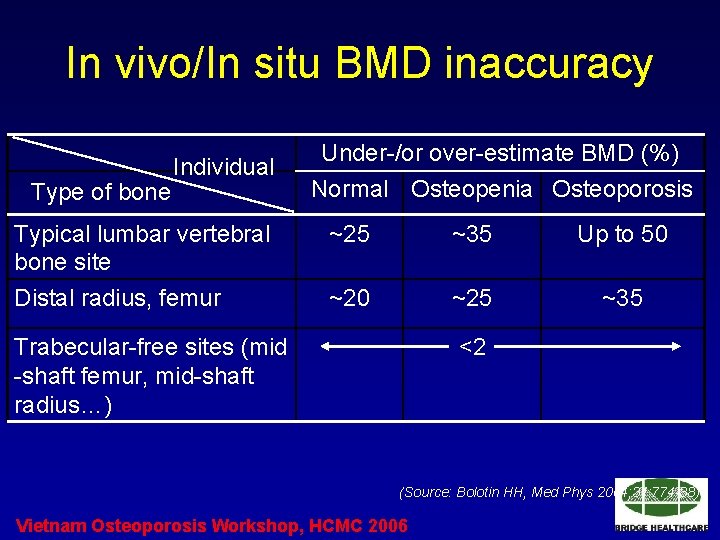
In vivo/In situ BMD inaccuracy Type of bone Individual Under-/or over-estimate BMD (%) Normal Osteopenia Osteoporosis Typical lumbar vertebral bone site ~25 ~35 Up to 50 Distal radius, femur ~20 ~25 ~35 Trabecular-free sites (mid -shaft femur, mid-shaft radius…) <2 (Source: Bolotin HH, Med Phys 2004; 31: 774 -88) Vietnam Osteoporosis Workshop, HCMC 2006

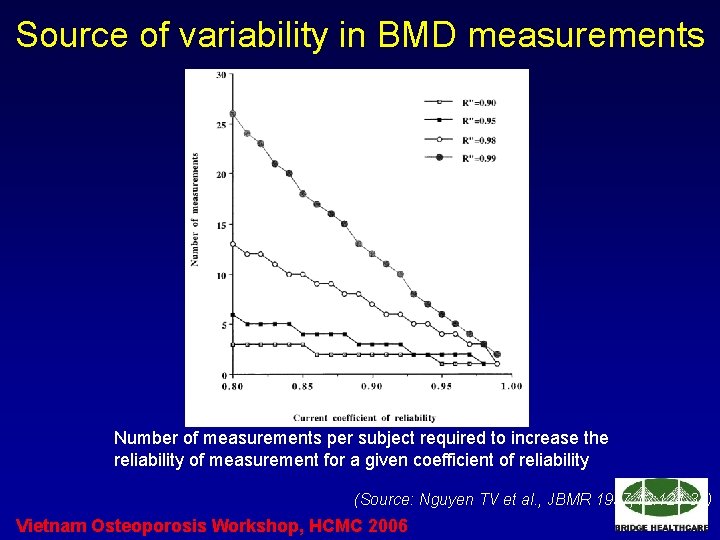
Source of variability in BMD measurements Number of measurements per subject required to increase the reliability of measurement for a given coefficient of reliability (Source: Nguyen TV et al. , JBMR 1997; 12: 124 -34) Vietnam Osteoporosis Workshop, HCMC 2006

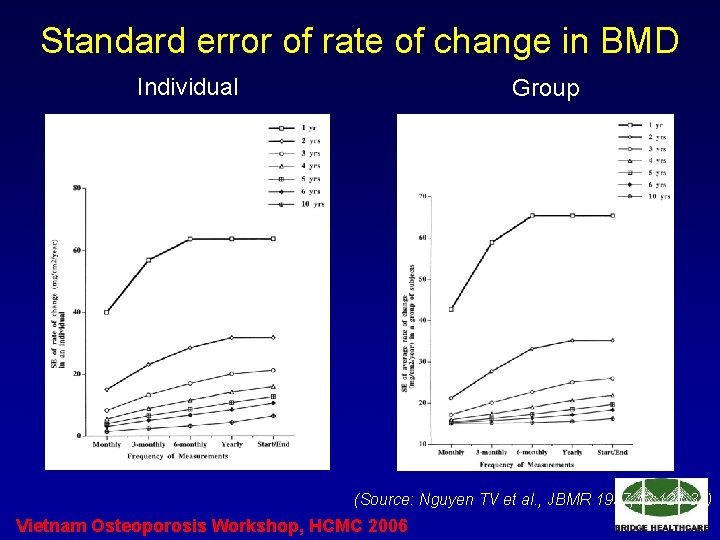
Standard error of rate of change in BMD Individual Group (Source: Nguyen TV et al. , JBMR 1997; 12: 124 -34) Vietnam Osteoporosis Workshop, HCMC 2006

Source of variability in BMD measurements • Group level: Intra-subject estimation error could contribute about 90% of the variability component power of study, and underestimate the RR (BMDfracture). • Individual level: false +ve & false –ve error rates of diagnostic BMD. • measurement error by multiple measurement. • long-term intra-subject variation by: the length of follow-up and/or the frequency of measurements. • Studies with 3 -5 yrs of follow-up: optimal “cost benefits”. • More than 2 measurements/year: not improve the precision appreciably. (Source: Vietnam Osteoporosis Workshop, HCMC 2006 Nguyen TV et al. , JBMR 1997; 12: 124 -34)

“True” level and “True” biological change of BMD • Factors affect to BMD level and BMD change: – Invivo/in situ BMD inaccuracy – Random error – Measurement errors: intra- and between-subject variability – Systematic errors – Effect of regression-toward-the mean (Sources: Bolotin HH, Med Phys 2004; 31: 774 -88; Nguyen TV et al. , JBMR 1997; 12: 124 -34; Nguyen TV et al, JCD 2000; 3: 107 -19) Vietnam Osteoporosis Workshop, HCMC 2006

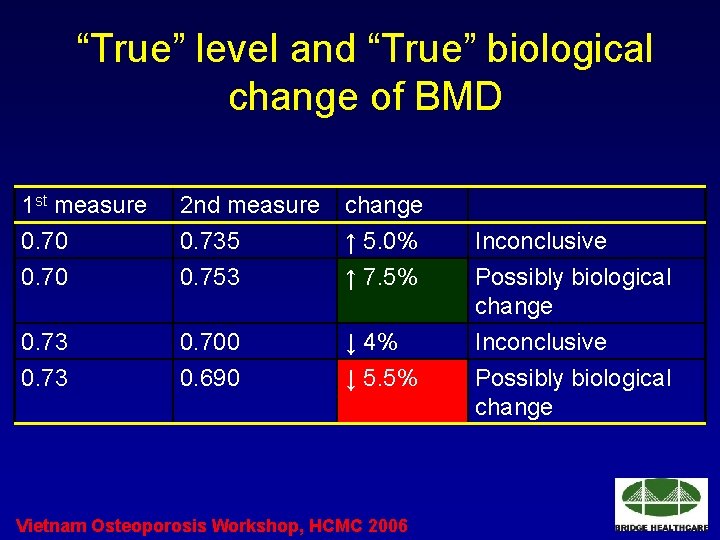
“True” level and “True” biological change of BMD • BMD level: – Good agreement between observed and true values – Individual with low BMD: 20% false +ve and false –ve of diagnosis of osteoporosis. • BMD change: – Overall average increase in BMD of 2%: no conclusion of significant change for an individual. – An observed of at least 5. 5% or of at least 7. 5%: could be a significantly biological change. (Source: Nguyen TV et al, JCD 2000; 3: 107 -19) Vietnam Osteoporosis Workshop, HCMC 2006

“True” level and “True” biological change of BMD 1 st measure 0. 70 2 nd measure 0. 735 0. 753 change ↑ 5. 0% ↑ 7. 5% 0. 73 0. 700 0. 690 ↓ 4% ↓ 5. 5% Vietnam Osteoporosis Workshop, HCMC 2006 Inconclusive Possibly biological change

BMD Values From Different Manufacturers Are Not Comparable • Different dual energy methods • Different calibration • Different detectors • Different edge detection software • Different regions of interest Vietnam Osteoporosis Workshop, HCMC 2006

Peripheral BMD Testing Accurate & Precise • What it can do – Predict fracture risk – Tool for osteoporosis education • What it cannot do – Diagnose osteoporosis – Monitor therapy 1. A “normal” peripheral test does not necessarily mean that the patient does not have osteoporosis. 2. WHO criteria do not apply to peripheral BMD testing. Vietnam Osteoporosis Workshop, HCMC 2006

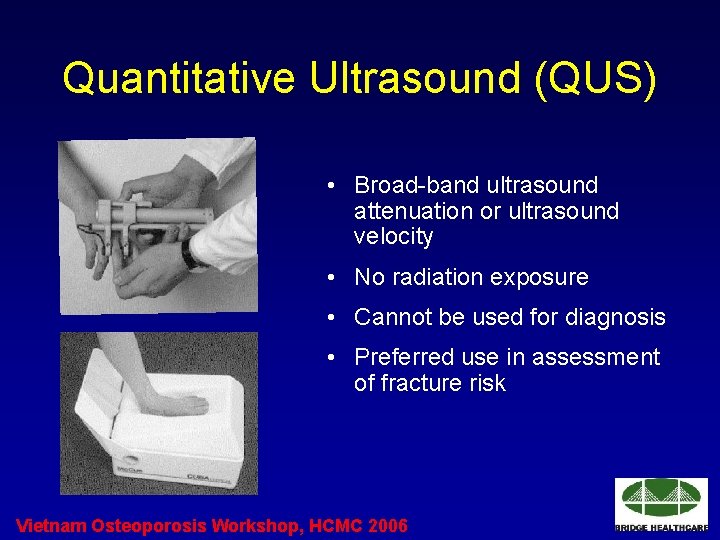
Quantitative Ultrasound (QUS) • Broad-band ultrasound attenuation or ultrasound velocity • No radiation exposure • Cannot be used for diagnosis • Preferred use in assessment of fracture risk Vietnam Osteoporosis Workshop, HCMC 2006

Bone Quality Architecture Turnover Rate Damage Accumulation Degree of Mineralization Properties of the collagen/mineral matrix ( NIH Consensus Development Panel on Osteoporosis. JAMA 285: 785 -95; 2001) Vietnam Osteoporosis Workshop, HCMC 2006

Cortical and Trabecular Bone Cortical Bone • 80% of all the bone in the body • 20% of bone turnover Trabecular Bone • 20% of all bone in the body • 80% of bone turnover Vietnam Osteoporosis Workshop, HCMC 2006

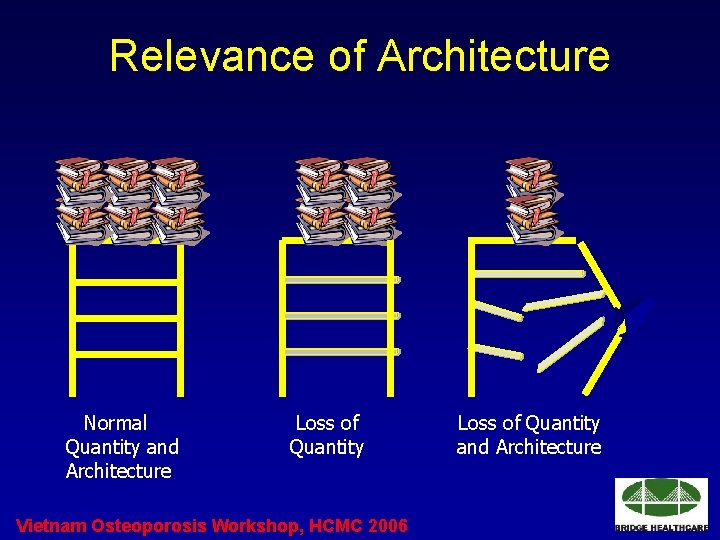
Relevance of Architecture Normal Quantity and Architecture Loss of Quantity Vietnam Osteoporosis Workshop, HCMC 2006 Loss of Quantity and Architecture

Bone Architecture Trabecular Perforation The effects of bone turnover on the structural role of trabeculae Risk of Trabecular Perforation increases with: • Increased bone turnover • Increased erosion depth • Predisposition to trabecular thinning Vietnam Osteoporosis Workshop, HCMC 2006

Structural Role of Trabeculae Compressive strength of connected and disconnected trabeculae 1 Bell et al. Calcified Tissue Research 1: 75 -86, 1967 Vietnam Osteoporosis Workshop, HCMC 2006 16 X

Resorption Cavities as Mechanical Stress Risers Normal Osteoporotic (Adapted from Parfitt A. M. et al. Am J Med 91, Suppl 5 B: 5 B-34 S) Vietnam Osteoporosis Workshop, HCMC 2006

Hip strength indice • CSMI (cm 4): Cross-sectional moment of inertia • CSA (cm 2): Cross sectional area • Z (cm 3): Section modulus= CSMI/distance from the centre of the mass to the superior neck margin. • Cstress (N/mm 2): Compressive stress on the superior surface of the FN during a fall on the greater trochanter. Calculated by combining CSMI and CSA. • FND (cm): Femoral neck Diameter • Buckling ratio= radius/thickness Vietnam Osteoporosis Workshop, HCMC 2006

Cross-Sectional Moment of Inertia CSMI = /4 (r 4 outer – r 4 inner) Area (cm 2) CSMI (cm 4) Bending Strength 2. 77 0. 61 100% 2. 77 1. 06 149% Vietnam Osteoporosis Workshop, HCMC 2006 2. 77 1. 54 193%

Bone strengh indice: summary • Not well-studied • Derived from BMC, BMD, and several assumptions • Used in research field. Vietnam Osteoporosis Workshop, HCMC 2006

Bone Turnover Markers • Components of bone matrix or enzymes that are released from cells or matrix during the process of bone remodeling (resorption and formation). • Reflect but do not regulate bone remodeling dynamics. Vietnam Osteoporosis Workshop, HCMC 2006

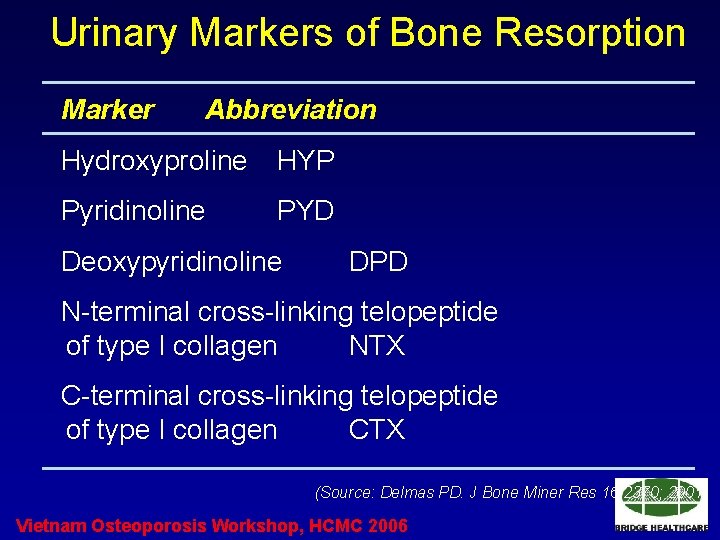
Urinary Markers of Bone Resorption Marker Abbreviation Hydroxyproline HYP Pyridinoline PYD Deoxypyridinoline DPD N-terminal cross-linking telopeptide of type I collagen NTX C-terminal cross-linking telopeptide of type I collagen CTX (Source: Delmas PD. J Bone Miner Res 16: 2370; 2001) Vietnam Osteoporosis Workshop, HCMC 2006

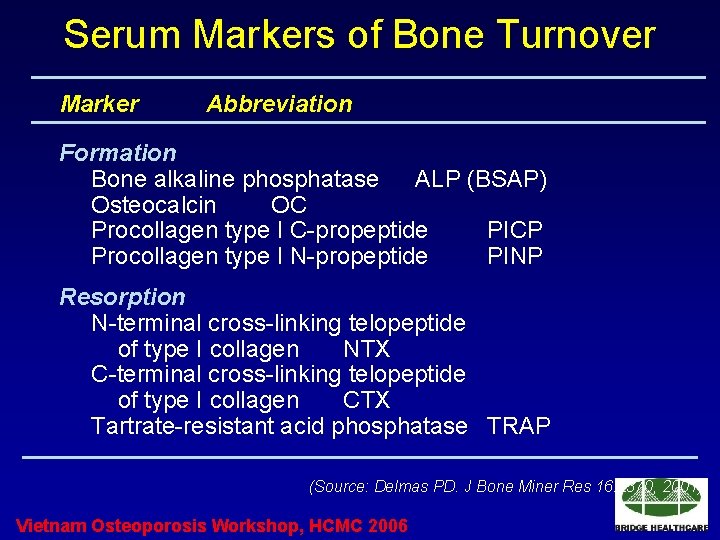
Serum Markers of Bone Turnover Marker Abbreviation Formation Bone alkaline phosphatase ALP (BSAP) Osteocalcin OC Procollagen type I C-propeptide PICP Procollagen type I N-propeptide PINP Resorption N-terminal cross-linking telopeptide of type I collagen NTX C-terminal cross-linking telopeptide of type I collagen CTX Tartrate-resistant acid phosphatase TRAP (Source: Delmas PD. J Bone Miner Res 16: 2370, 2001) Vietnam Osteoporosis Workshop, HCMC 2006

Bone Turnover Effects Bone Quality • Very low turnover excessive mineralization and the accumulation of microdamage • Very high turnover accumulation of perforations and a negative bone balance Vietnam Osteoporosis Workshop, HCMC 2006

Summary • Osteoporosis and osteoporotic fractures are common among aging population • “Gold standard” of assessment skeleton health is BMD via DXA machine. • BMD measurement is subject to bias and errors. • Additional measure of bone health: QUS (BMD), bone strength indice and bone turnover markers. Vietnam Osteoporosis Workshop, HCMC 2006

Lời Cảm tạ • Chúng tôi xin chân thành cám ơn Công ty Dược phẩm Bridge Healthcare, Australia là nhà tài trợ cho hội thảo. Vietnam Osteoporosis Workshop, HCMC 2006

Thank you! Vietnam Osteoporosis Workshop, HCMC 2006