Acute Coronary Syndromes Terry White RN EMPT 1




































- Slides: 47

Acute Coronary Syndromes Terry White, RN, EMP-T 1

The History of Paramedics Begins with Cardiac Care 4 The original Paramedic idea was based upon the need for rapid response to, identification of and emergency care for victims of: èSudden Cardiac Death (SCD) èAcute Myocardial Infarction (AMI) 2

Ischemic Coronary Syndromes 4 Acute Coronary Syndromes èAngina Pectoris èUnstable Angina èAcute Myocardial Injury èAcute Myocardial Infarction 4 Presentation with suspected ischemia u Non-diagnostic ECG u ST segment depression u ST segment elevation/New BBB 3

Ischemic Coronary Syndromes 4 Angina Pectoris èAcute pain, usually in the chest, resulting from an increased demand for oxygen and a decreased ability to provide it èUsually due to a partially occluded coronary artery or vasospasm 4

Ischemic Coronary Syndromes 4 Angina Pectoris èTypical Presentation u Squeezing, Crushing, Heavy, Tight – Fist to chest = Levine’s sign u Pain/Discomfort may radiate to shoulders, arms, neck, back, jaw or epigastrium u Usually lasts 3 -5 min and rarely exceeds 15 min u Not changed by swallowing, coughing, deep breathing or positional changes 5

Ischemic Coronary Syndromes 4 Angina Pectoris èTypical Presentation u Anxiety u Diaphoresis or clammy skin u Nausea, vomiting u Shortness of breath u Weakness u Palpitations u Syncope 6

Ischemic Coronary Syndromes 4 Angina Pectoris èUsually Provoked by: u Exercise u Eating u Emotion/Stress èUsually Relieved by: u Rest; Removal of provoking factor u Nitroglycerin 7

Ischemic Coronary Syndromes 4 Stable Angina Pectoris èReasonably Predictable frequency, onset, duration èRelief predictable with rest, nitroglycerin 8

Ischemic Coronary Syndromes 4 Stable Angina Pectoris èTreatment Goals u Reduce myocardial oxygen demand u Improve myocardial oxygen supply 9

Ischemic Coronary Syndromes 4 Stable Angina Pectoris èTreatment u Physical/Psychological rest u Position of comfort, sitting or supine u Oxygen u ECG Monitor – Assess the underlying rhythm u Nitroglycerin, 0. 4 mg SL q 5 min as long as BP > 90 mm Hg – Continue until pain relieved or contraindicated 10

Ischemic Coronary Syndromes 4 Stable Angina Pectoris èTransport Considerations u Many persons stay home and treat themselves u Treat first-time angina, unstable angina or angina requiring more than 3 NTG (>15 min) as AMI u When in doubt, treat as AMI 11

Ischemic Coronary Syndromes 4 Stable Angina Pectoris èVariant Angina (Prinzmetal’s Angina) u Occurs at rest u Episodes at regular times of day u Results from coronary vasospasms u Treated long term with calcium channel blockers u May result in abnormal 12 lead ECG changes that resolve with minimal treatment 12

Ischemic Coronary Syndromes 4 Unstable Angina èProlonged chest pain/ischemic symptoms or an atypical presentation of angina without ECG or laboratory evidence of AMI (Injury) èUsually associated with significant or progressing occlusion of a coronary artery or severe vasospasm èConsidered “Pre-infarction Angina” 13

Ischemic Coronary Syndromes 4 Unstable Angina èMay have Typical or Atypical Signs & Symptoms u. Atypical Presentation – Increased frequency or duration of episodes – Onset with less exertion than normal – Increased severity of symptoms – Requires greater number of NTG tablets to relieve symptoms 14

Ischemic Coronary Syndromes 4 Unstable Angina èTreatment same as Angina PLUS: u IV, NS (no dextrose), TKO – Some exceptions to restricting fluid u 12 Lead ECG – Assess for RVI u Morphine sulfate, 2 - 4 mg q 5 -15 min slow IV titrated to pain relief and BP > 90 u Aspirin, 160 -325 mg PO 15 – Chewed & swallowed if possible – Determine if hypersensitive to ASA

Ischemic Coronary Syndromes 4 Unstable Angina èTreatment u Metoprolol, 5 mg slow IV q 5 min to 15 mg total, prn for HR/BP in absence of contraindications u In longer or interfacility transports, consider: – Nitroglycerin IV infusion, 10 -20 mcg/min – Heparin – GP IIB/IIIA inhibitors u Thrombolytics Checklist (just in case) u Transport, destination? 16

Ischemic Coronary Syndromes 4 Acute Myocardial Injury èPresentation of Unstable Angina or Acute Ischemia with potential for myocardium salvage (penumbra) èDiagnostic evidence of Injury (ECG or elevated Enzymes) u Does not necessarily imply necrosis of the myocardium u Presentation, Signs and Symptoms are the same as Acute MI 17

Ischemic Coronary Syndromes 4 Acute Myocardial Infarction (AMI) èNecrosis of myocardial tissue caused by a lack of oxygenation and blood flow resulting from an occluded coronary artery èOften also used to describe acute injury when extent of necrosis is unknown but imminent èDiagnostic evidence of injury is present (elevated enzymes and possibly ECG) 18

Ischemic Coronary Syndromes 4 Acute Myocardial Infarction (AMI) èPrecipitating Factors u Coronary thrombosis (most common) u Coronary vasospasm u Microemboli u Severe Hypotension/Shock u Acute Hypoxia u Acute Volume Overload 19

Ischemic Coronary Syndromes 4 Acute Myocardial Infarction (AMI) èLocation, size of infarct and severity depends on site of vessel occlusion u majority involve left ventricle u LCA – anterior, septal, lateral u RCA – inferior, right ventricle 20

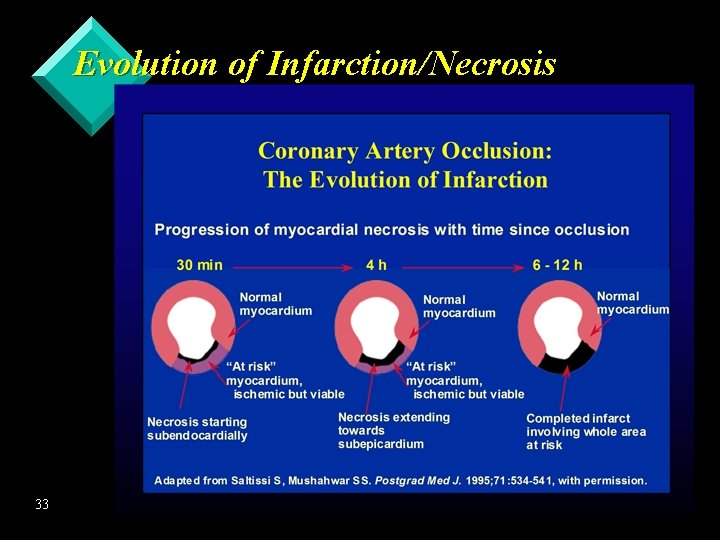
Ischemic Coronary Syndromes 4 Acute Myocardial Infarction (AMI) èOften defined further as u subendocardial: involves only subendocardial muscle u transmural: full thickness of ventricular wall involved 21

Evolution of AMI 22

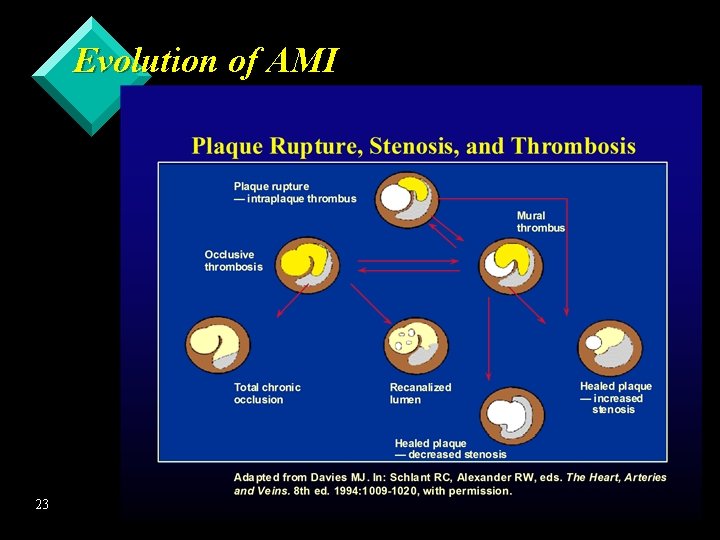
Evolution of AMI 23

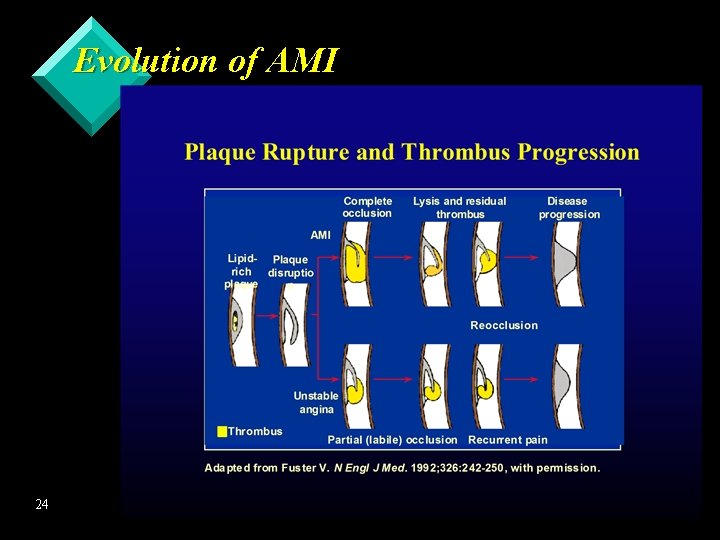
Evolution of AMI 24

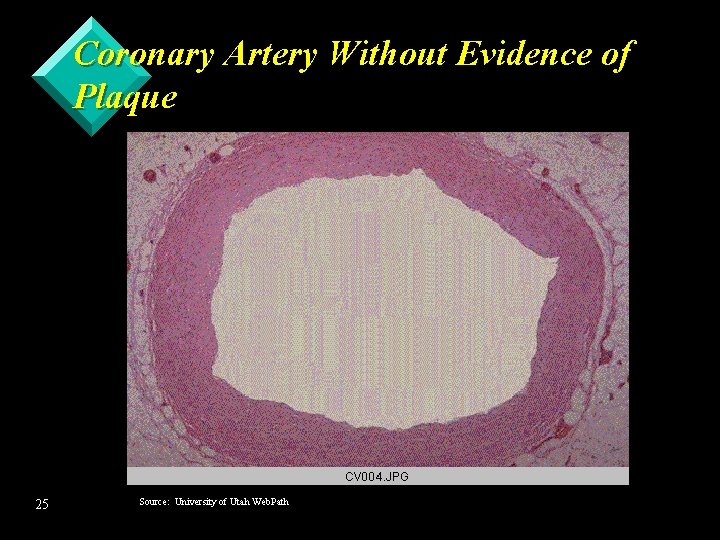
Coronary Artery Without Evidence of Plaque 25 Source: University of Utah Web. Path

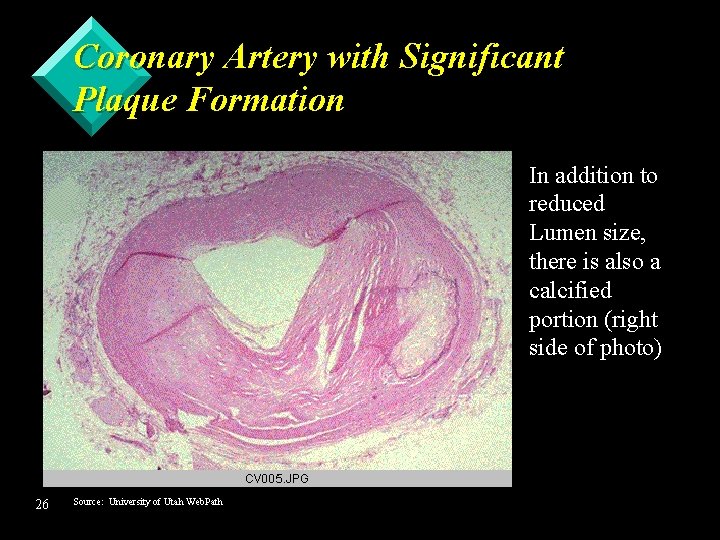
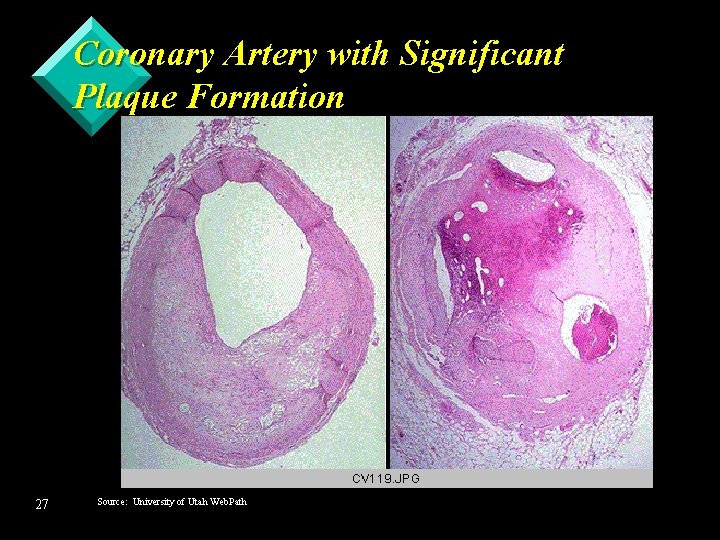
Coronary Artery with Significant Plaque Formation In addition to reduced Lumen size, there is also a calcified portion (right side of photo) 26 Source: University of Utah Web. Path

Coronary Artery with Significant Plaque Formation 27 Source: University of Utah Web. Path

Rupture of Atheromatous Plaque Results in Thrombus Formation 4 Rupture of “Vulnerable” plaque’s soft lipid core is the initiating event in most acute ischemic coronary events 4 Occlusion is dependent on clot formation and accompanying fibrinolysis 4 A thrombotic occlusion that is relatively persistent (i. e. , 2 to 4 hours or longer) may result in acute myocardial infarction 28

Rupture of Atheromatous Plaque Results in Thrombus Formation 4 Repeated thrombus formations may further decrease the lumen size 4 Intermittent non-occlusive thrombus formation results in Unstable Angina 4 Incomplete occlusion may also result in MI possibly due to coronary artery spasm 29

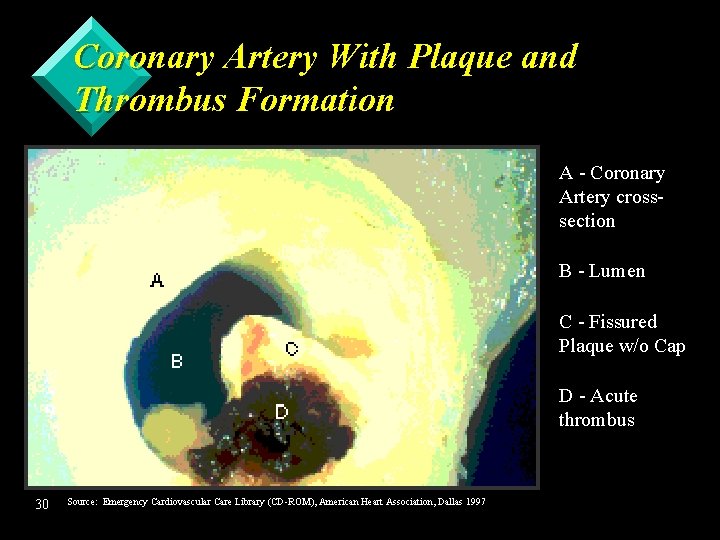
Coronary Artery With Plaque and Thrombus Formation A - Coronary Artery crosssection B - Lumen C - Fissured Plaque w/o Cap D - Acute thrombus 30 Source: Emergency Cardiovascular Care Library (CD-ROM), American Heart Association, Dallas 1997

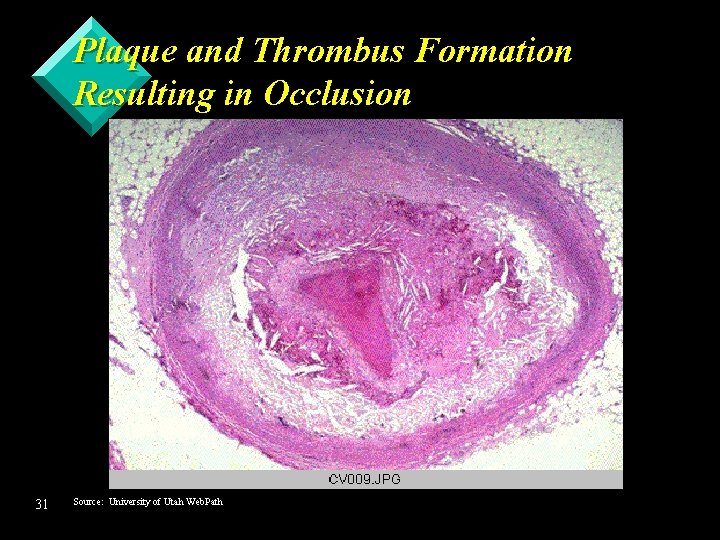
Plaque and Thrombus Formation Resulting in Occlusion 31 Source: University of Utah Web. Path

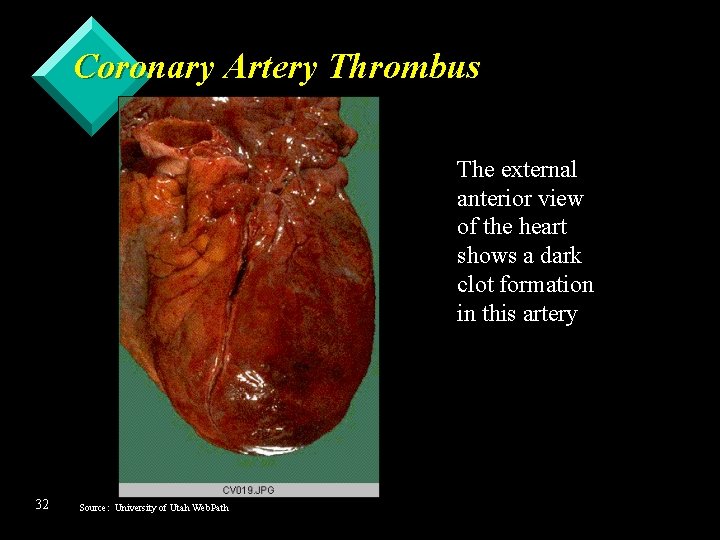
Coronary Artery Thrombus The external anterior view of the heart shows a dark clot formation in this artery 32 Source: University of Utah Web. Path

Evolution of Infarction/Necrosis 33

Ischemic Coronary Syndromes 4 Acute Myocardial Infarction (AMI) èPresentation u Similar – – Last longer Not easily relieved with rest or NTG Sx/Sx may be more severe (feeling of impending doom) Pain often radiates to arms, neck, jaw, back, epigastrium u Some 34 to Angina but present atypically with complaints of only weakness or shortness of breath u Dysrhythmias u Sudden Cardiac Death

Ischemic Coronary Syndromes 4 Acute Myocardial Infarction (AMI) èPresentation u 10 -20% have “silent” MI (no chest pain) – common in elderly, older women, diabetics u If 35 adding chest pain to the patient’s list of Sx/Sx completes a clear picture of AMI, then the patient is having an AMI!! u Vital Signs and monitoring ECG leads DO NOT provide DIAGNOSTIC evidence of AMI!! u Clinical diagnosis in absence of 12 Lead ECG or Enzyme changes

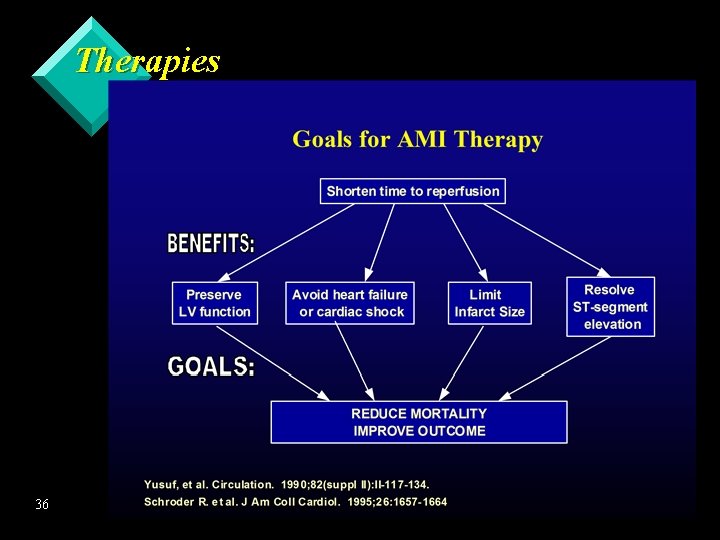
Therapies 36

Ischemic Coronary Syndromes 4 Acute Myocardial Infarction (AMI) èTreatment Goals u Decrease – – – myocardial oxygen demand Remove physical/psychological stressors Relieve pain Reduce workload of the heart (BP, HR) u Inhibit further clot formation u Rapid identification/diagnosis u Transport for reperfusion therapy 37

Ischemic Coronary Syndromes 4 Acute Myocardial Infarction (AMI) èTreatment same as Angina PLUS: u IV, – – – u 12 NS, large bore TKO with some exceptions No dextrose containing solutions Fluid boluses appropriate in some cases 2 nd line if time permits Minimize number of attempts Lead ECG – Diagnostic evidence of AMI present – Assess for RVI 38

Ischemic Coronary Syndromes 4 Acute Myocardial Infarction (AMI) èTreatment u Morphine – – – sulfate, 2 - 4 mg q 5 -15 min slow IV Maintain BP > ~ 90 mm Hg Titrated to Pain relief Reduce PVR and workload on the heart u Aspirin, 160 -325 mg PO – Chewed & swallowed if possible – Determine if hypersensitive to ASA u “MONA 39 greets all patients”

Ischemic Coronary Syndromes 4 Acute Myocardial Infarction (AMI) èTreatment u Metoprolol, 5 mg slow IV q 5 min to 15 mg total, prn for HR/BP in absence of contraindications u In longer or interfacility transports, consider: – Nitroglycerin IV infusion – Heparin u Thrombolytics Checklist – Exclusions for thrombolysis 40

Ischemic Coronary Syndromes 4 Acute Myocardial Infarction (AMI) èTreatment u Transport for reperfusion therapy; Destination? – Thrombolysis vs Coronary Artery Catheterization – For patients with associated pulmonary edema, hypotension or cardiogenic shock, consider transport to facility with capability of angiography & revascularization 41

Considerations for Fibrinolytics 42

Contraindications for Fibrinolytics 4 Lack of diagnostic 12 Lead ECG changes 4 Chest pain < 20 min or > 12 hours 4 Not oriented, can not cooperate 4 History of stroke or TIA 4 Known bleeding disorder 4 Active internal bleeding in past 2 -4 weeks 43 4 Surgery or trauma in past 3 weeks 4 Terminal illness 4 Jaundice, hepatitis, kidney failure 4 Use of anticoagulants 4 Systolic BP < 180 mm Hg 4 Diastolic BP < 110 mm Hg

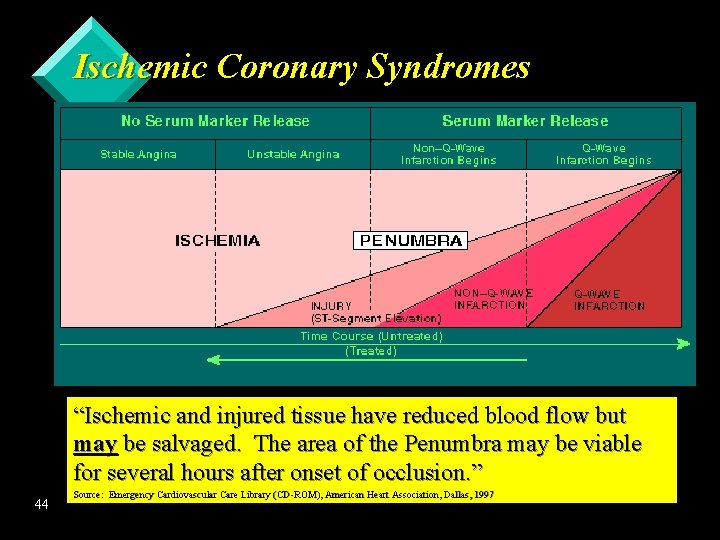
Ischemic Coronary Syndromes “Ischemic and injured tissue have reduced blood flow but may be salvaged. The area of the Penumbra may be viable for several hours after onset of occlusion. ” 44 Source: Emergency Cardiovascular Care Library (CD-ROM), American Heart Association, Dallas, 1997

Ischemic Coronary Syndromes 4 Sudden Cardiac Death (SCD or SCA) èSudden, unexpected biologic death presumably resulting from cardiovascular disease èMost common rhythm of SCA is Ventricular Fibrillation èMay be primary or secondary VF èChain of Survival is the greatest determinant of outcome èTreatment based on ECG rhythm & arrest events 45

Time is Muscle!!! 46

References and Resources 4 Advanced Cardiac Life Support, Edited by R O Cummins, MD, American Heart Association, Dallas, 1997 4 “Emergency Cardiovascular Care Library” (CD-ROM), American Heart Association and Pro. Education International, Dallas, 1997 4 Eisenberg, M S, Life in the Balance: Emergency Medicine and the Quest to Reverse Sudden Death, Oxford University Press, New York, 1997 4 “A Definition of Advanced Types of Atherosclerotic Lesions and a Histological Classification of Atherosclerosis”, A Report From the Committee on Vascular Lesions of the Council on Arteriosclerosis, American Heart Association, 1995 4 “Coronary Artery Calcification: Pathophysiology, Epidemiology, Imaging Methods, and Clinical Implications”, A Statement for Health Professionals From the American Heart Association, 1995 4 Cardiovascular Disease Statistics, American Heart Association, Dallas, 1997 4 “Diagnosis and Therapy of Acute Myocardial Infarction: Today’s Look at Tomorrow’s Therapies and Outcomes”, Du. Pont Pharma, 1997 4 University of Utah Web. Path, http: //medstat. med. utah. edu/webpath/ 47