NonSTSegment Elevation Acute Coronary Syndromes Risk Stratification Based

Non-ST-Segment Elevation Acute Coronary Syndromes: Risk Stratification Based on the ACC/AHA UA / NSTEMI Guidelines

ED Risk Stratification for Chest Pain For the past 20 years. . . R/O MI In 2002: · Does this patient need fibrinolytic therapy? · Should this patient get antithrombin and anti-platelet agents? · Can I safely send this patient home?

ED CCU Cath Lab Risk Stratification for Chest Pain Three levels of risk stratification are pertinent to the ED: l Low, intermediate, or high risk that ischemic symptoms are a result of CAD l Low, intermediate, or high risk of short-term death or nonfatal MI from ACS l Dynamic, ongoing risk-oriented evaluation of low- or intermediate-risk patients for “conversion” to high-risk status that is linked to intensity of treatment
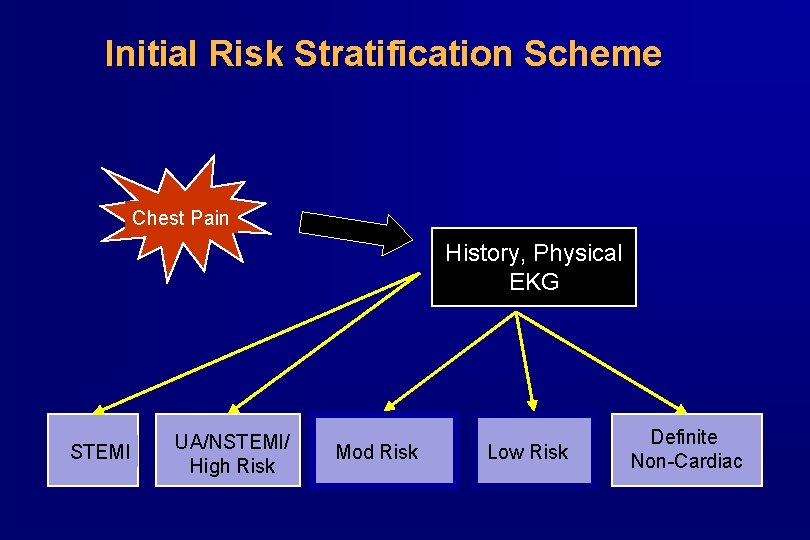
Initial Risk Stratification Scheme Chest Pain History, Physical EKG STEMI UA/NSTEMI/ High Risk Mod Risk Low Risk Definite Non-Cardiac

Risk Stratification Tools in the ED • History and Physical • Standard ECG and Non-standard ECG leads · Cardiac Biomarkers • Troponin I or T, CK-MB, myoglobin · Predictive Indices / Schemes · Non-Invasive Imaging Studies · Echocardiogram · Exercise testing · Technetium-99 m-sestamibi: stress and rest

Initial Evaluation Risk Stratification (1) I IIa IIb III Early risk stratification by symptoms, physical findings, ECG, cardiac markers 12 -lead ECG within 10 min for ongoing pain, or ASAP if pain has resolved at presentation Cardiac markers, Troponins and CK-MB, for initial assessment Monitoring, repeat ECG and cardiac markers in 6 -12 hours, if initial results normal
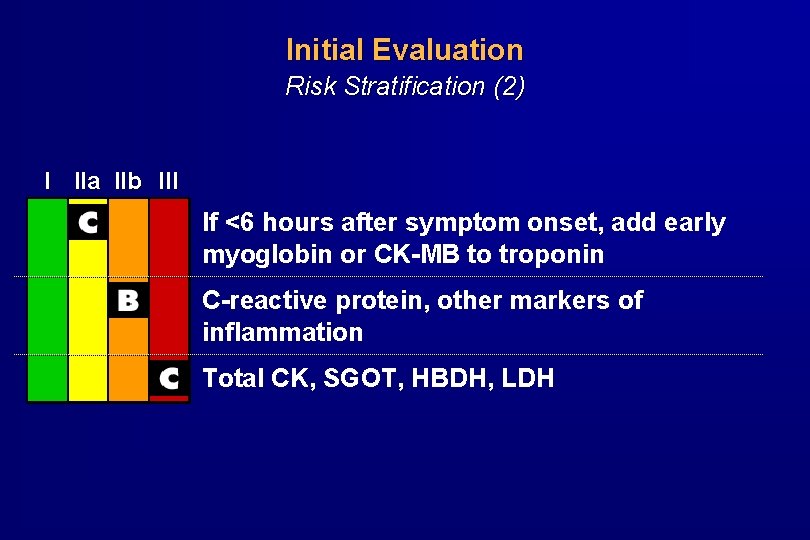
Initial Evaluation Risk Stratification (2) I IIa IIb III If <6 hours after symptom onset, add early myoglobin or CK-MB to troponin C-reactive protein, other markers of inflammation Total CK, SGOT, HBDH, LDH

Clinical Assessment (1) · Rapid, focused evaluation · Decisions based on this evaluation have substantial clinical and economic consequences · Are the symptoms a manifestation of ACS? · If so, what is the prognosis? · Identify signs of life-threatening instability · Triage to most appropriate area · Typically an ED or chest pain unit

Clinical Assessment (2) · Risk status determined in the ED by: · · · · Assessment of anginal symptoms Careful physical examination Electrocardiogram Cardiac biomarkers CAD risk factors Illicit drug use Initial risk stratification assignment drives pace of subsequent evaluation and treatment

Clinical Assessment (3) · High-risk features apparent in the ED: · · · · Accelerated pattern of angina Ongoing rest pain > 20 min Signs of CHF Hemodynamic instability Arrhythmias - Atrial or ventricular Advanced age (> 75 years) Ischemic ECG changes Elevated cardiac markers

Electrocardiogram · Carries diagnostic and prognostic value · Especially valuable if captured during pain · ST-segment depression or transient ST-segment elevation are primary ECG markers of UA/NSTEMI · 75% of patients with + CK-MB do not develop Q waves · Differentiation between UA and NSTEMI relies upon positive biomarkers · Inverted T-waves suggestive of ischemia, particularly with good chest pain story
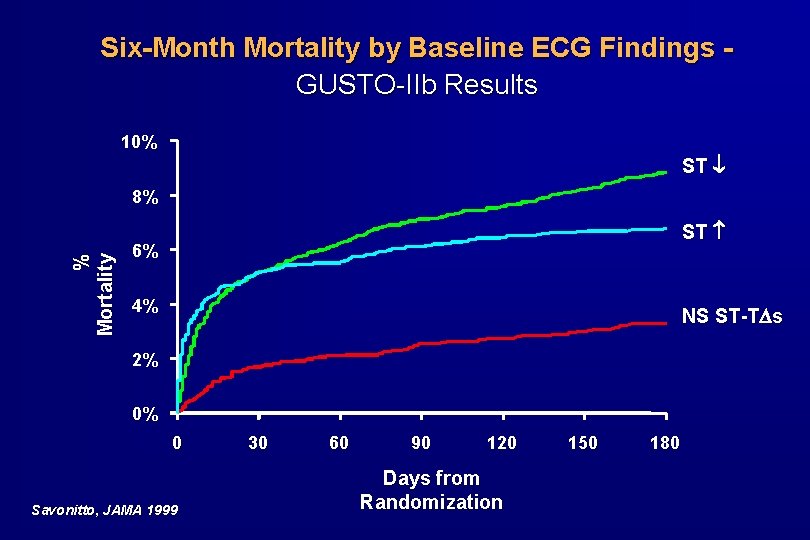
Six-Month Mortality by Baseline ECG Findings GUSTO-IIb Results 10% ST % Mortality 8% ST 6% 4% NS ST-T s 2% 0% 0 Savonitto, JAMA 1999 30 60 90 120 Days from Randomization 150 180

Biomarkers: CK/CKMB · Until recently the principal serum marker used in evaluation of ACS despite known limitations: · Low levels in healthy persons limits specificity · MB band may be elevated in skeletal muscle damage · Different MB isoforms exist in myocardium (MB 2) and in plasma (MB 1), and differentiating assay is not widely available

Biomarkers: Troponins · Very useful in diagnosis and prognosis of ACS · · Normally not detectable in blood of healthy persons; c. Tn. I or c. Tn. T can be positive with negative CK-MB = “minor myocardial damage” Predictive of MI and death when elevated, independent of CK-MB levels Elevated troponins validated as a predictor of enhanced treatment benefit from aggressive therapies (LMW heparins, GP IIb/IIIa inhibitors, early invasive strategy)
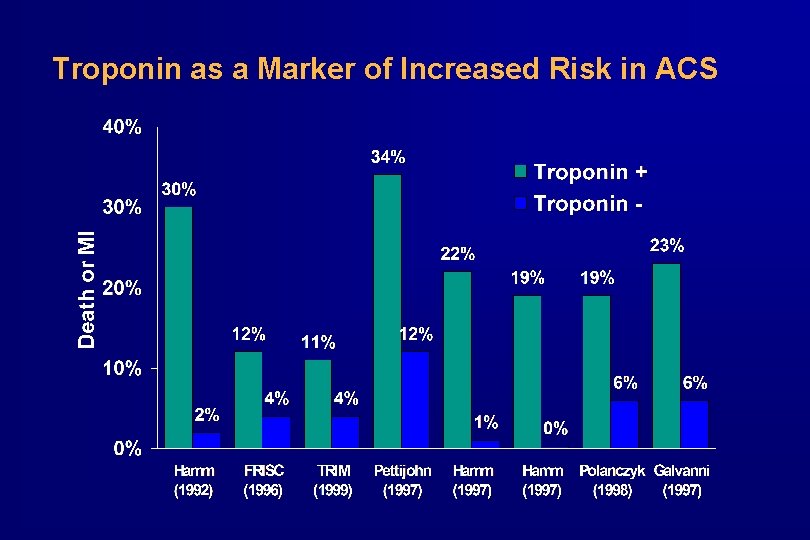
Troponin as a Marker of Increased Risk in ACS
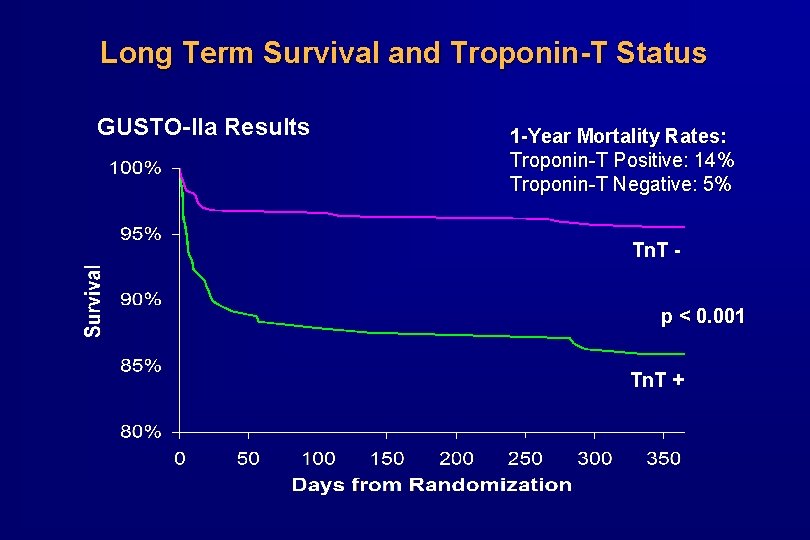
Long Term Survival and Troponin-T Status GUSTO-IIa Results 1 -Year Mortality Rates: Troponin-T Positive: 14% Troponin-T Negative: 5% Tn. T p < 0. 001 Tn. T +

Biomarkers: Myoglobin · Utility limited by release kinetics (early) and by lack of cardiac specificity · Isolated elevation of myoglobin 4 -8 hours after pain onset with a a non-diagnostic ECG must be supplemented by a more cardiac-specific marker · Sufficiently sensitive that a negative myoglobin 4 -8 hours after pain onset is useful in excluding myocardial necrosis

Integration of Biomarkers with Clinical History · Time since symptom onset should be a factor in marker selection and in repeat assay strategy · Elevated serum levels of troponins persist for 7 -14 days after initial release · Delta values, as close as 2 hours apart, may be sufficiently sensitive to assist with serial evaluations · Serial cardiac marker strategy not specified
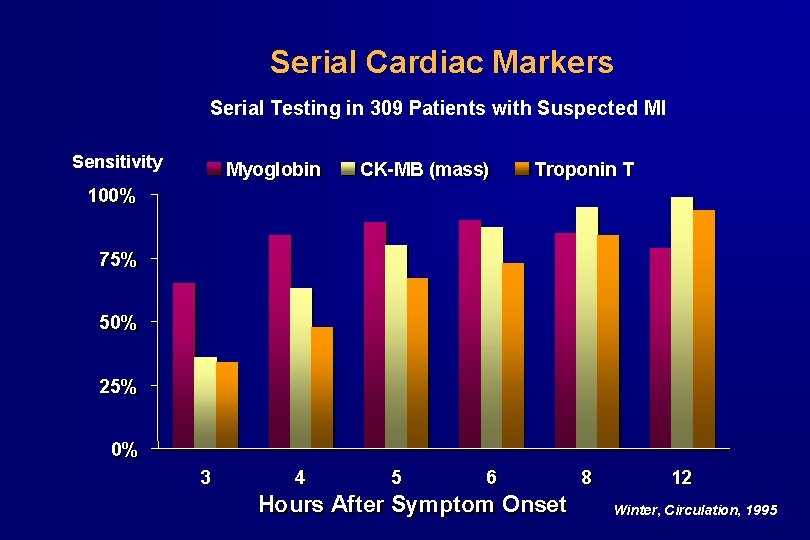
Serial Cardiac Markers Serial Testing in 309 Patients with Suspected MI Sensitivity Myoglobin CK-MB (mass) Troponin T 100% 75% 50% 25% 0% 3 4 5 6 Hours After Symptom Onset 8 12 Winter, Circulation, 1995

Biomarkers: Bedside Testing · Consideration of bedside marker assay recommended when hospital lab turnaround time > 30 -60 minutes · Ready-for-use availability must be balanced against need for stringent QC and training of ED personnel, CLIA concerns, political hazards, etc · Prognostic value limited because many assays are qualitative, not quantitative
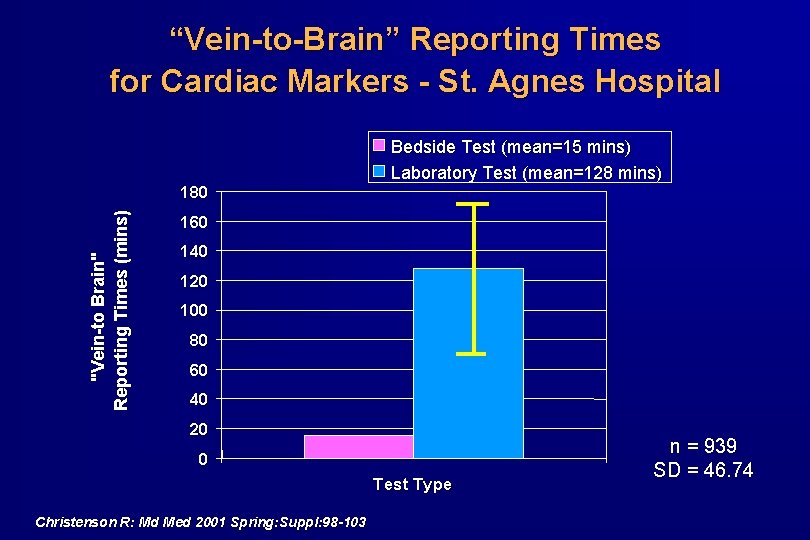
“Vein-to-Brain” Reporting Times for Cardiac Markers - St. Agnes Hospital "Vein-to Brain" Reporting Times (mins) 180 Bedside Test (mean=15 mins) Laboratory Test (mean=128 mins) 160 140 120 100 80 60 40 20 0 Test Type Christenson R: Md Med 2001 Spring: Suppl: 98 -103 n = 939 SD = 46. 74
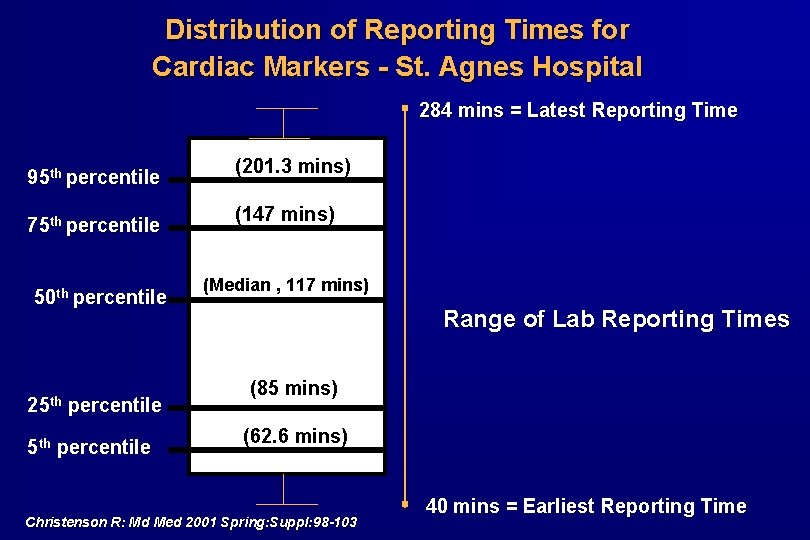
Distribution of Reporting Times for Cardiac Markers - St. Agnes Hospital 284 mins = Latest Reporting Time 95 th percentile 75 th percentile 50 th percentile 25 th percentile (201. 3 mins) (147 mins) (Median , 117 mins) Range of Lab Reporting Times (85 mins) (62. 6 mins) Christenson R: Md Med 2001 Spring: Suppl: 98 -103 40 mins = Earliest Reporting Time

Noninvasive Studies · Guidelines do not consider use of these tests in the ED setting, although: · Many EDs now use rest sestamibi scanning in the risk stratification process · Stress testing used after patients have “ruled out” · Reality dictates that appropriate provocative testing often not likely after patient leaves ED · ED is the “first, last, and best shot” at intervening in patients with risk concerns

Predictive Indices - Risk Scores in the ED n Combine clinical history, physical exam findings, ECG signs of ischemia, and cardiac marker results l PURSUIT and TIMI Risk Scores n Therapies such as LMW heparin and GP IIb/IIIa inhibitors have greater benefit in patients with higher risk scores n Have not been tested prospectively in the ED n Risk scores not specifically recommended by the ACC/AHA Guidelines

Immediate Management I IIa IIb III Classify as non-cardiac, chronic stable angina, possible ACS, or definite ACS Evaluate for immediate reperfusion therapy if definite ACS and ST-segment present Pharmacological or exercise stress test, if possible ACS and serial biomarkers and ECGs are normal Admit pts with definite ACS, ongoing pain, biomarkers, new ST or deep T-wave inversion, abnormal hemodynamics, or (+) stress test

The “Key” to Risk Stratification n Link ongoing evaluation of risk to changes in intensity of therapy n Develop risk stratification schemes that reflect capabilities of ED and needs/preferences of cardiologists n Develop treatment pathways that provide for independent response of emergency physicians to recognition of higher risk levels

The “Rallying Cry” for CRUSADE. . . A seamless transition of optimal care—diagnostic and therapeutic—from the ED to the Cardiology Service. . . starts with a successful risk stratification strategy

- Slides: 28