Nutrition Therapy for Paralytic Ileus Lara Snead Sodexo







































- Slides: 40

Nutrition Therapy for Paralytic Ileus Lara Snead Sodexo Dietetic Intern February 4, 2013

Objectives Differentiate an ileus from a small bowel obstruction Identify indications for nutrition support Discuss medical and nutrition care throughout case study’s hospital course

General Information GG is a 64 YO Male Admitted on 11/12/2012 w/COPD Initially seen as a Nursing Screen Referral on 11/13 by RD Seen by dietetic intern 9 times Remains an inpatient @ WAH

Past Medical History COPD HTN Anemia Cellulitis of LEs Rashes PVD

Social History Lives with parents Smokes about 1 pack/day Drinks alcohol almost qday

Anthropometric Data Ht: 5’ 7” (67”) Admit Wt: 139# (63 kg) IBW: 148# (67 kg) BMI: 21. 8 kg/m 2 (Normal wt category)

Hospital Course 11/12: Right femoral endarterectomy & embolectomy; fasciotomies 11/13: Seen by RD – intubated, sedated, on 2 pressors, nonresponsive to voice/questions NPO; banana bag Drsg to R shin & thigh Kcal: 1134 -1449 (18 -23), Prot: 63 -76 (1. 0 -1. 2) Lactate-4. 5 H ↓, MAP-80’s Rec. initiate EN w/Glucerna 1. 2 @ 30 m. L/hr, ↑ as tol. to 45 m. L/hr (1296 kcal, 65 g prot)

Hospital Course, Cont. 11/15: Tolerating Nepro @ 20 m. L/hr RLE w/inner & outer incisions w/staples OTA, leg is warm, ecchymotic Rec. to Δ TF to Glucerna 1. 2 @ 45 m. L/hr (1296 kcal, 64 g prot) ↑ BG (167, 235, 193 mg/d. L) 11/19: Extubated, alert & responsive but delirious Likely need amputation of R toes vs. foot Kcal: 1575 -1890 (25 -30), Prot: 75 -88 (1. 2 -1. 4) Tolerating feeds – rec. advance to Glucerna 1. 2 @ 60 m. L/hr (1728 kcal, 86 g prot)

Hospital Course, Cont. � 11/27: �Reintubated – full vent �NPO – OGT on LCS (500 m. L out in 4 hrs) �KUB: SBO, perforated viscus - no plan for surgery (allow to heal) �Rec. TPN – 2 L (NS): 11% Dex, 4. 2% AA, 175 m. L Lipids (1434 kcal, 84 g prot) � 11/30: �KUB: C/w ileus vs. SBO �Gastrografin via NGT �Cont. TPN �If no extravasation, begin Osmolite 1. 5 @ 20 and ↑ as tol. to 35 m. L/hr + PS (1332 kcal, 68 g prot)

SBO vs. Ileus SBO – partial/complete blockage of small/large intestine Tumor, adhesions, hernias, twisting/narrowing of intestines Ileus – absence of intestinal peristalsis without mechanical obstruction Normal times after surgery: Small bowel – several hrs Stomach – 24 -48 hrs Colon – 48 -72 days When postop ileus persists longer, considered pathologic and called a paralytic ileus

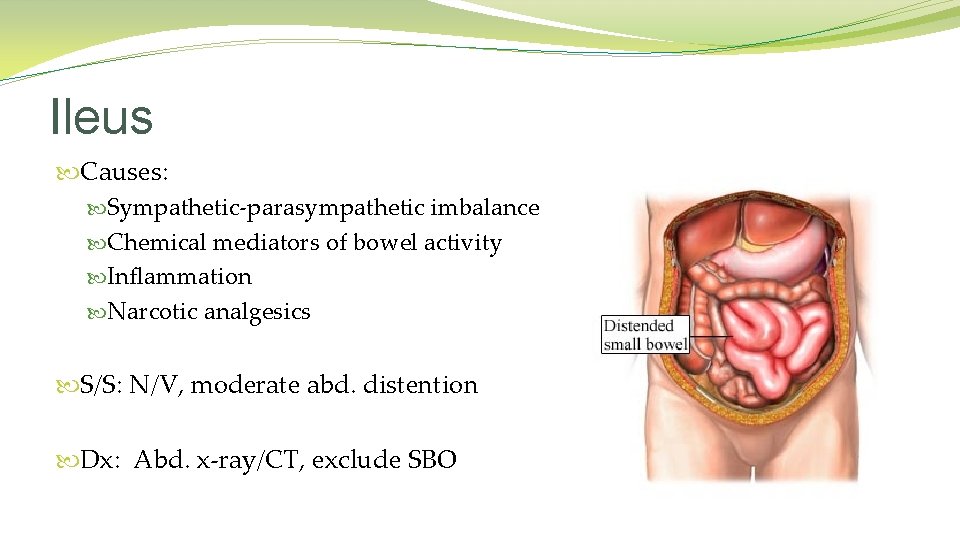
Ileus Causes: Sympathetic-parasympathetic imbalance Chemical mediators of bowel activity Inflammation Narcotic analgesics S/S: N/V, moderate abd. distention Dx: Abd. x-ray/CT, exclude SBO

Ileus Management Nasogastric tube for decompression Early postop enteral feeding Gum-chewing Meds: Limit narcotics Erythromycin – antibiotics, motilin receptor antagonist Metoclopramide (Reglan) – antiemetic, prokinetic

Hospital Course, Cont. 12/4: TF w/Jevity 1. 2 @ 10 off d/t ↑ residuals of 1. 2 L; ↑ NGT output Vomited & asp. Skin: Necrotic feet, Stage 2 sacral (not seen) Alb-0. 9 L, plan to check prealbumin Cont. TPN Rec. 24 hr metabolic cart

Hospital Course, Cont. 12/7: CT on 12/5 showed↑ dilated SB c/w high-grade SBO Tracheostomy on 12/6 Indirect Calorimetry – avg. 2200 kcal, RQ <0. 8 NGT on LCS w/100 m. L out overnight Δ TPN to 2 L (NS): 19% Dex, 4. 5% AA, 275 m. L Lipids (2206 kcal, 90 g prot) Trial Jevity 1. 2 @ 10 m. L/hr if NGT output remains <400 m. L/next 24 hrs

Indirect Calorimetry �“Gold standard” �Resting Energy Expenditure (REE) �Respiratory quotient (RQ) �CO 2 production : O 2 consumption �< 0. 82 – underfeeding, predominant lipid catabolism �> 1 w/excessive CO 2 production – overfeeding, lipogenesis, ↑ resp. demand � GG: �REE: Avg. 2200 kcal �RQ: < 0. 8 – indicated underfeeding � TPN – 2 L (NS): 1434 kcal, 84 g prot (65% of needs) � TPN Δ’d to 2 L (NS): 2206 kcal, 90 g prot

Hospital Course, Cont. 12/10: ↑ Na+/Cl- likely r/t ↑ kcal in same volume RD Δ’d TPN to 2. 5 L (NS) – 15% Dextrose, 3. 6% AA, 275 m. L Lipids (2185 kcal, 90 g prot)

Hospital Course, Cont. � 12/11: �Alert, more responsive, tolerating T-piece �Did not tolerate EN on 12/9 �SBFT: Not SBO, normal transit times; SB & LB dilation c/w ileus �↓ abd. distention, NGT clamped but had 800 m. L out overnight �Flexiseal w/600 m. L out overnight �Skin: Unchanged �Na+-148 H, Cl--111 H, BUN-21 H, Prealbumin-4. 4 L �Cont. TPN, add ½NS IVF’s until stooling improves, trial Reglan, check prealbumin �If NG output <500 m. L in next 24 hrs, trial Jevity 1. 2 @ 10 m. L/hr

Follow Up - 12/14 TPN: 2. 5 L (NS) – 15% Dextrose, 3. 6% AA, 275 m. L Lipids (2185 kcal, 90 g prot) TF: Jevity 1. 2 @ 20 m. L/hr (576 kcal, 27 g prot) General: Alert, responds w/nods, nonverbal, full vent w/trach GI: Abd. distended, denies abd. pain, ↑ BS, no residuals Flexiseal w/500 m. L liquid brown stool out/3. 5 hours Neg. for C. diff (12/11) Skin: R toes necrotic, inner/outer R calf w/staples

Follow Up - 12/14 Meds: Pepcid, Reglan Labs: Prealbumin 21 -43 mg/d. L Zinc 60 -130 mcg/d. L Hgb 13. 5 -18 g/d. L Hct 39 -52% WBC 4. 5 -11. 0 K/u. L 8. 0 L ↑ 47 L 6. 4 L 19. 6 L 20. 1 H Pending blood transfusion

Nutrition Care Plan Dx: Altered GI function R/T ? malabsorption vs. hypermotility side effect of Reglan AEB 500 m. L liquid stool out in 3. 5 hours. Goal: Stool output <400 m. L/day Plan: 1. Cont. TPN 2. Δ TF to Vivonex @ 20 m. L/hr (480 kcal, 24 g prot) 3. Rec. d/c Reglan 4. Check CRP 5. Add 25 mg Zn to TPN x 10 days 6. Rec. SLP consult for swallow eval (had been tol. T-piece) Monitor: TF tolerance, stool output, labs

Follow Up 12/18 TPN: 2. 5 L Non-Standard (2185 kcal, 90 g prot) TF on hold since 12/16 d/t vomiting 12/17 CT: C/w paralytic ileus General: Nonverbal, eyes closed, agitated, full vent No NGT output, clamped during visit (1. 3 L on 12/17) GI: Abd. less distended, NT, soft, ↑ BS Flexiseal w/500 m. L liquid brown stool out/8 hrs Skin: Unchanged

Follow Up 12/18 Meds: Pepcid, Ativan, KCl *Reglan d/c’d – no Δ’s in stool output; ↑ vomiting Labs: K+ 3. 5 -5. 1 m. Eq/L Cl 98 -107 mmol/L CO 2 21 -32 mmol/L Hgb 13. 5 -18 g/d. L Hct 39 -51% WBC 4. 5 -11 K/u. L 3. 1 L 115 H 18 L 6. 7 L ↑ 20. 5 L ↑ 14. 0 H ↓ Pending blood transfusion Low K+ r/t ↑ vomiting & NGT output High Cl- and low CO 2 r/t diarrhea

Nutrition Care Plan Dx: Altered GI function R/T ? malabsorption AEB >500 m. L stool output/8 hours. Goal: Stool output <400 m. L/day Plan: 1. Cont. TPN 2. Rec. restarting Reglan 3. Rec. Imodium 4. Rec. GI consult Monitor: Stool output, labs, ileus status

Follow Up - 12/21 TPN: 2. 5 L Non-Standard (2185 kcal, 90 g prot) TF not resumed despite order for Vivonex @ 20 m. L/hr 48 hrs prior + issue w/feeding pump & bottle General: Nonverbal, nods responses; full vent NGT clamped, no output recorded GI: No N/V; abd. soft, ND/NT, + BS *Reglan restarted (10 mg BID) Flexiseal Δ’d w/200 m. L out/~1 hour; 800 m. L out/previous 24 hrs Neg. for C. diff (12/19) Skin: BUE anasarca (R>L), rash all over body, Stage 1 sacral (not seen) Bedscale wt: 184# ← 139# (11/13) *45# wt gain since admit likely r/t edema – no reliable I/O recorded, no wts recorded

Follow Up - 12/21 Meds: Benadryl, Fluconazole, Mg. SO 4 (12/20) Labs: Na+ K+ 135 -145 m. Eq/L 3. 5 -5. 1 m. Eq/L 145 ← 149* H↓ 3. 6 ↑ CO 2 21 -32 mmol/L c. Ca 8. 2 -10. 6 mg/d. L Mg 1. 8 -2. 4 mg/d. L 28 ↑ 11. 58 H 1. 7 L *Na+ was high previous day d/t pt receiving D 5/NS + Na. HCO 3 for low CO 2 D/w ACNP to check Prealbumin and C-Reactive Protein (CRP)

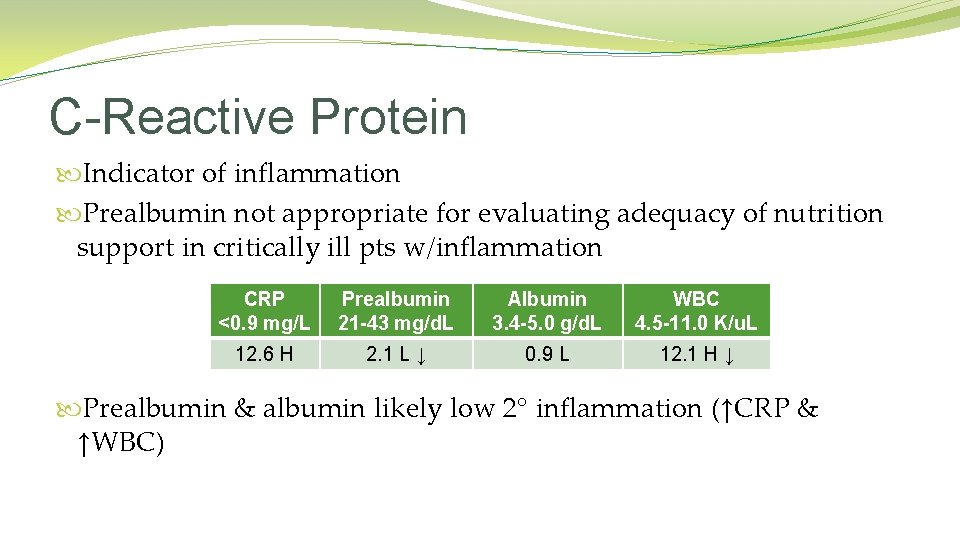
C-Reactive Protein Indicator of inflammation Prealbumin not appropriate for evaluating adequacy of nutrition support in critically ill pts w/inflammation CRP <0. 9 mg/L Prealbumin 21 -43 mg/d. L Albumin 3. 4 -5. 0 g/d. L WBC 4. 5 -11. 0 K/u. L 12. 6 H 2. 1 L ↓ 0. 9 L 12. 1 H ↓ Prealbumin & albumin likely low 2° inflammation (↑CRP & ↑WBC)

Nutrition Care Plan �Dx: Altered GI function R/T ? zinc deficiency vs. unknown etiology AEB stool output of 800 m. L/24 hrs. �Goal: Decrease stool output to <600 m. L/24 hrs �Plan: 1. 2. 3. 4. 5. 6. 7. 8. Rec. Octreotide & Cholestyramine Rec. Lactinex Add 25 mg Zn to TPN x 10 days Remove Ca from TPN Decrease Reglan to 5 mg BID Rec. GI consult Trial trophic feeds of Vivonex @ 20 m. L/hr – do not advance Strict I/O’s �Monitor: Stool output, labs, wt, GI input, TF tolerance, I/O’s

Hospital Course 12/24: TPN: 2. 5 L Non-Standard (2185 kcal, 90 g prot) TF: Vivonex @ 20 m. L/hr (480 kcal, 24 g prot) R subclavian central line infection – plan for new line on L GI consulted – did not see pt, rec. d/c Reglan W/Reglan, no significant residuals, no vomiting Flexiseal: 1. 2 L out on 12/23, 770 m. L out on 12/22 (Neg. for C. diff) Cont. TPN Rec. Imodium & Cholestyramine Trial increase Vivonex to 40 m. L/hr if stool decreases

Hospital Course 12/26: No new line placed – TPN stopped Tolerating Vivonex @ 40 m. L/hr Flexiseal: 250 m. L on 12/25, 550 m. L out on 12/24 Imodium & Cholestyramine added Rec. increasing TF to 60 m. L/hr If no significant Δ’s in stooling, Δ TF to Impact 1. 5 @ 60 m. L/hr (2160 kcal, 135 g prot) D/w ACNP to check Zn level – if still low, add Zn. SO 4 x 10 days

Follow Up – 1/2 TF: Impact 1. 5 @ 60 m. L/hr (2160 kcal, 135 g prot) + autoflushes General: Alert, nods to questions, TC during day, vent @ night as tolerated SLP swallow eval: NPO except ice chips GI: Abd. soft, ND/NT, +BS Flexiseal w/400 m. L liquid brown stool during shift Skin: R shin staples removed, incisions healed Bedscale wt: 157#

Follow Up – 1/2 Meds: Cholestyramine, Imodium, Pepcid, ABO, Lactinex, Zn. SO 4, Benadryl, Methylprednisolone Labs: Na+ 135 -145 m. Eq/L Cl 98 -107 mmol/L CO 2 21 -32 mmol/L BUN 7 -20 mg/d. L WBC 4. 5 -11 K/u. L Zn 60 -130 mcg/d. L 146 H ↑ 116 H ↑ 20 L 36 H ↑ 15. 4 H ↑ 58 L ↑

Nutrition Care Plan Dx: Inadequate fluid intake R/T diarrhea AEB Na+-146 H, Cl-116 H, BUN-36 H. Goal: Normal lab values Plan: 1. Cont. Impact @ 60 m. L/hr + autoflushes 2. Add 210 m. L H 2 O flushes q 6 hrs (total 2549 m. L free H 20) Monitor: Stool output, TF tolerance, labs, hydration

Follow Up – 1/8 � 1/4: �Off vent – pt “coughed” out trach �NGT removed �MBS : Mild-mod pharyngeal dysphagia w/delayed swallow & silent asp. �Diet: Mechanical Soft, Nectar Thick Liquids �General: Alert & oriented, able to converse �Drinking liquids, not eating a lot of solid foods; willing to try Resource Shake Thickened �GI: Flexiseal w/350 m. L liquid green stool during shift; abd. ND/NT +BS �Skin: Less anasarcic in BUE, bandage over throat stoma �Bedscale wt: 138# ← 157# (1/2) *Wt loss likely r/t less edema

Follow Up – 1/8 Meds: Cholesyramine, Benadryl, Haldol Labs: BMP WNL, except Cl--110 H ↓; WBC – 12. 2 H ↓ Eosinophils 0 -6% 13. 6 H D/w ACPA d/c of Cholestyramine d/t high eosinophils Eosinophils – WBC that become active during allergic diseases, infections Cholestyramine added around time when eosinophils started to ↑ Possible reaction? Or r/t rash?

Nutrition Care Plan Dx: Inadequate protein-energy intake R/T pt choosing to drink liquids and not eat solid foods AEB meeting ~30% of est. needs. Goal: ≥ 50% PO intake + supplements Plan: 1. Cont. current diet 2. Add Resource Shake Thickened TID 3. Add appetite stimulant Monitor: PO intake, stooling

Follow Up - 1/10 Diet: Mech. Soft, Nectar Thick, Resource Shake TID General: A & O, reports good appetite (on Marinol) PO Intake: 50% of meal, all liquids and supplements GI: No abd. pain, ND/NT +BS, no N/V/C Flexiseal w/50 m. L of light brown stool output during shift 840 m. L out on 1/9 – *needed Cholestyramine Bedscale wt: 137# ← 138# (1/8) Labs: CO 2 BUN 21 -32 mmol/L 7 -20 mg/d. L Cr 0. 6 -1. 3 mg/d. L 17 L ↓ 32 H ↑ 1. 9 H ↑ WBC 4. 5 -11. 0 K/u. L Eosins 0 -6% 15. 2 H ↑ 21. 0 H ↑

Nutrition Care Plan Dx: No acute nutrition problems @ this time. Goal: ≥ 75% PO intake Plan: 1. Cont. current diet & supplements 2. Add Imodium – d/w ACPA Monitor: PO intake, stooling GG LIVED HAPPILY EVER AFTER…

Patient Update 1/14: CT: High-grade mechanical SBO NPO, NGT on LCS Restarted Reglan 1/21: NGT removed PO diet resumed: Mech. soft, thin liquids (per SLP rec’s), Ensure TID Reports good appetite, >75% PO intake Cont. on Reglan Still @ WAH. To be continued…

Questions?
