Case Report Nutritional Management of Small Bowel Obstruction

Case Report: Nutritional Management of Small Bowel Obstruction By Christine Bannon ARAMARK Dietetic Internships December 14, 2014

Abstract Purpose: Follow the Nutrition Care Process Case: 82 yr old female with small bowel obstruction (SBO) who required total parental nutrition (TPN) Previous hospital visit for SBO – noninvasive treatment and low fiber Hospitalized again for SBO secondary to adhesions PMH: Uterine cancer requiring hysterectomy TPN, lysis of adhesions, and right partial colectomy Discharged after 15 days on oral low fiber
Disease Description – Small Bowel Obstruction The small intestine is a complex organ that plays a major role in the absorption of nutrients When contents of the intestine are blocked and unable to pass freely, this is considered a small bowel obstructions (SBO). Signs & Symptoms Abdominal distention Constipation Vomiting Abdominal pain and cramps Nausea Diarrhea

Disease Description – Causes Mechanical - characterized by the narrowing of the intestinal lumen Nonmechanical - factors that interfere with the muscle action or innervation of the bowel Inflammation or trauma to the bowel Neoplasms Paralytic ileus Adhesions (Most common) Mesenteric embolus or thrombus Hernias Hypokalemia Volvulus (twisted bowel) Compression from outside the intestinal tract

Evidence-Based Nutrition Recommendations Title: Reoperation on the Abdomen Encased in Adhesions Purpose: To determine the short and long-term outcomes after lysis of adhesions Method: 40 patients who had recently undergone lysis of adhesions were contacted to evaluate the outcome Results: 1 postoperative death, 24 early complications. 28 out of 31 had resolved SBO from the surgery Long-term outcomes: all subjects able to tolerate oral feedings

Evidence-Based Nutrition Recommendations Title: Burden of Adhesions in Abdominal & Pelvic Surgery: A Systematic Review and Metanalysis Purpose: To estimate the burden of complications associated with abdominal adhesions Method: Analysis of 196 papers from Pub. Med, Embase, and Central which reported incidences of adhesion related complications Results: Increase risk of developing a SBO in open abdominal/pelvic surgery. Adhesive SBO associated with longer hospital stays.

Case Presentation An 82 year old woman is admitted to the hospital after a night of worsening abdominal pain, nausea and vomiting. Patient was recently admitted one month prior for a SBO which was treated conservatively with no invasive processors. Since then, patient has followed a low-fiber diet. Once admitted, patient underwent a series of radiographs to diagnose her with another SBO and renal failure secondary to dehydration

Nutrition Case Process (NPC): Assessment Past Medical History Hypertension High cholesterol Type 2 diabetes mellitus Hypothyroidism Arthritis Fractured spine and coccyx Osteoporosis Missing right kidney from birth Reflux Constipation Hysterectomy from uterine cancer which was last treated with radiation in 2005

Food/Nutrition Related History Lack of appetite for one week prior to admission Follows a low-fiber diet which was prescribed to her since her last hospitalization for SBO Lactose – intolerant Home medications can be found in Table 1

Nutrition-Focused Physical Findings No appetite at admission No identified chewing/swallowing issues with good oral health Trace bilateral edema in lower extremities Appeared well nourished No bowel movement for 2 days prior to admission

Anthropometric Measurements 4’ 9” (57”) 121 pounds (55 kg) BMI of 26. 6 = overweight IBW: 100 pounds 121% of IBW

Biochemical Data, Medical Test, and Lab Normal Patient’s Procedures Sodium Went through a series of x-rays and radiographs to confirm SBO Potassium diagnosis. Glucose Labs were taken as followed: BUN Creatinine Magnesium 136 -144 133 (L) Acute Renal Failure (AFR), dehydration 3. 6 -5. 1 3. 4 (L) Obstruction 234 (H) Acute inflammation 8 -20 21 (H) Dehydration, hypovolemia 0. 6 -1. 1 2. 1 (H) ARF, dehydration, inadeq. dietary protein, reduced muscle mass 1. 9 Indicates wnl Phosphorous Albumin Rationale Not tested 1. 9 (L) Acute inflammation

Nutrient Needs 1138 -1365 calories 55 -69 gm of protein 1138 -1369 ml of fluid Protein needs are elevated due to: Moderate protein depletion (Albumin 2. 1 -2. 7) Mildly metabolically stressed Nutritional needs are summarized in Table 2.

ARAMARK Nutrition Status Classification Moderate nutritional risk (status 3) 4 points: GI obstructions 3 points: Vomiting 3 points: Poor appetite Total of 10 points Follow up in 3 -5 days

Malnutrition Identification Malnutrition diagnosed with 2 out of the 6 Characteristics 1. Intake (fair to poor longer than 1 week) 2. Weight loss 3. Loss of muscle mass 4. Loss of subcutaneous fat 5. Fluid accumulation 6. Functional status Chronic vs. Acute Etiology Inflammation is chronic and mild-moderate degree vs. inflammation is acute and severe degree

Malnutrition Identification (cont. ) Malnutrition diagnosed with 2 out of the 6 Characteristics 1. Intake – Patient reported consuming <75% of her estimated energy needs for longer than a week 2. Weight loss 3. Loss of muscle mass 4. Loss of subcutaneous fat 5. Fluid accumulation – edema noted in lower extremities 6. Functional status Chronic vs Acute Etiology Acute due to hypoalbuminemia (1. 9)

NCP: Diagnoses Altered Gastrointestinal Function (NC-1. 4) related to small bowel obstruction as evidenced by abdominal distention, vomiting and lack of bowel movement. Malnutrition (NI-5. 2) related to small bowel obstruction as evidenced by fluid retention and oral energy intake < 50%-75% for one week.

NCP: Interventions Medical Interventions Nasogastric tube was place for suction to prevent further nausea and vomiting Right Partial Colectomy Lysis of adhesions Medications and their rationale the patient was placed on can be found on Table 3.

NCP: Interventions Nutrition Interventions Parental Nutrition (ND 2. 2) Day 1 standard formula: 70 gm amino acids, 150 gm dextrose, 20 gm lipid with 10 gm zinc, 100 mg thiamine, 1 mg folic acid, 500 mg vitamin C, 60 mg selenium Provides: 990 kcal (22 kcal/kg ideal wt), 70 gm protein (1. 5 gm/kg ideal wt) Justification: Malnourished Enteral feeding can not be safely attempted Nonfunctional gut TPN expected to be needed for at least 7 days

NCP: Interventions Additional consults were needed from nephrology due to patient’s acute renal failure(ARF)diagnosis Nephrology findings: ARF was secondary to dehydration Intervention: Intravenous fluid needed

NCP: Monitoring and Evaluation Parenteral nutrition formula (FH-1. 3. 2. 1) Weight (AD-1. 1. 2) Domain: ANTHROPOMETRIC MEASUREMENTS (AD) Digestive system (mouth to rectum) (bowel function, bowel sounds) (PD-1. 1. 5) Domain: FOOD/NUTRITION-RELATED HISTORY (FH) Domain: NUTRITION-FOCUS PHYSICAL FINDINGS (PD) Potassium (BD-1. 2. 7), Magnesium (BD-1. 2. 8), Phosphorus(BD-1. 2. 11), Glucose, casual(BD-1. 5. 2) Domain: BIOCHEMICAL DATA, MEDICAL TESTS AND PROCEDURES (BD)

Follow-Ups (F/U) F/U #1 (11/14) PES: Inadequate energy intake(NI-1. 2) related to small bowel obstruction as evidenced by poor appetite. Intervention: Parenteral Nutrition/IV Fluids (2. 2) when able Goal: Initiate PN when able Achievement: PN was started F/U #2 (11/15) PES: Inadequate parenteral nutrition infusion (NI-2. 7) related to day 1 standard TPN formula as evidenced by 72. 5% of energy needs being met. Intervention: Modify volume of parenteral nutrition (ND-2. 2. 4), Modify composition of parenteral nutrition(ND-2. 2. 1) Modified TPN order: 70 gm amino acids, 235 gm dextrose, 30 gm lipid with 10 gm zinc, 100 mg thiamine, 1 mg folic acid, 500 mg vitamin C, 60 mg selenium Provides: 1380 kcal (30 kca/kg ideal wt), 70 gm protein (1. 5 gm/ideal wt) Goal: Meet 50 -75% of nutritional needs Achievement: PN order was modified and 100% of nutritional needs were reached

Follow-Ups (cont. ) F/U #3 (11/16) PES: Altered nutrition-related laboratory values (phosphorous) (NC-2. 2) related to SBO as evidenced by phosphorus levels of 1. 4. Intervention: Recommend modify composition of parenteral nutrition (ND-2. 2. 1). Recommend mineral supplement therapy (phosphorous) (ND-3. 2. 4. 6) Goal: Meet 50 -75% of nutritional needs Achievement: Phosphorus was repleted. Dextrose was unchanged and serum glucose remained elevated

Follow-Up (cont. ) F/U #4 (11/17) PES: Parenteral Nutrition Administration Inconsistent with Needs (NI-2. 10) related to SBO as evidenced by elevated glucose in the 200’s. Intervention: Recommend modify composition of parenteral nutrition (ND-2. 2. 1) (decreased dextrose, increased lipid). Nutrition-Related Medication Management (ND-6) to add 0. 15 units of insulin/gm of dextrose. Modified TPN order: 1800 mls total volume, 75 ml/hr X 24 hrs. 70 gm protein, 200 gm dextrose, and 42 gm lipid. Provides: 1380 kcal (30 kcal/kg ideal wt) and 70 gm protein (1. 5 gm/kg ideal wt) Goal: Blood Glucose >200 Achievement: PN modified. Additional insulin was added. Blood glucose improving in upper 100’s but remains elevated. F/U #5 (11/18) PES: Impaired nutrient utilization (NC-2. 1) related to ileus as evidenced by no bowel movement Intervention: Continue Parenteral Nutrition/IV Fluids (2. 2) Achievement: PN was continued at recommended rate

Follow-Up (cont. ) F/U #6 (11/20) PES: Altered Gastrointestinal Function (NC-1. 4) related to small bowel obstruction as evidenced by lack of bowel movement/sound. Intervention: Continue Parenteral Nutrition/IV Fluids (2. 2) Goal: Meet 50 -75% of nutritional needs Achievement: PN was continued at recommended rate. (+) Hypoactive bowel. F/U #7 (11/21) PES: Altered Gastrointestinal Function (NC-1. 4) related to small bowel obstruction as evidenced by lack of bowel movement/sound. Intervention: Continue Parenteral Nutrition/IV Fluids (2. 2) Goal: Meet 50 -75% of nutritional needs Achievement: PN was continued at recommended rate

Follow-Up (cont. ) F/U #8 (11/22) PES: Altered Gastrointestinal Function (NC-1. 4) related to small bowel obstruction as evidenced by nausea and lack of bowel movement. Intervention: Continue Parenteral Nutrition/IV Fluids (2. 2) Goal: Meet 50 -75% of nutritional needs Achievement: PN was continued at recommended rate. Hypoactive bowel sounds heard. Patient begins to have flatus. F/U #9 (11/23) PES: Inadequate oral intake (NI-2. 1) related to TPN order as evidenced by clear liquid diet. Intervention: Begin Clear liquid diet(ND-1. 2. 8. 3) while continuing Parenteral Nutrition/IV Fluids (2. 2) at goal rate. Achievement: Patient tolerating clear liquids well. Small bowel movement is noted.

Follow-Up (cont. ) F/U #10 (11/24) PES: Inadequate oral intake (NI-2. 1) related to TPN order as evidenced by clear liquid diet. Intervention: Advance to Full liquid diet (ND-1. 2. 8. 4) when able. Modify rate of parenteral nutrition (ND-2. 2. 3) to 40 ml/hr. Goal: Meet 50 -75% of nutritional needs. Achievement: Diet advanced to full liquid diet. TPN rate was reduced. F/U #11 (11/25) PES: Inadequate oral intake (NI-2. 1) related to TPN order as evidenced by full liquid diet. Intervention: Advance to General/healthful diet (ND-1. 1) when able. Modify rate of parenteral nutrition (ND-2. 2. 3) to be discontinued completely. Goal: Meet 50 -75% of nutritional needs. Achievement: Diet advanced to regular for lunch. TPN order was discontinued.

Discharge Care No driving X 6 weeks No lifting/baths Outpatient F/U in 2 weeks Wear abdominal binder when out of bed X 2 months Ice for discomfort Low-fiber diet

Conclusion SBO is a serious medical and nutritional concern that can lead to lengthy hospital stays. Clinicians needs to monitor GI function daily in order to prevent GI atrophy TPN plays an essential role in the management of electrolytes and can supply adequate nutrients when enteral feedings can not be done Patients should be routinely cautioned on the risk and complications associated with adhesions before undergoing any abdominal or pelvic surgery
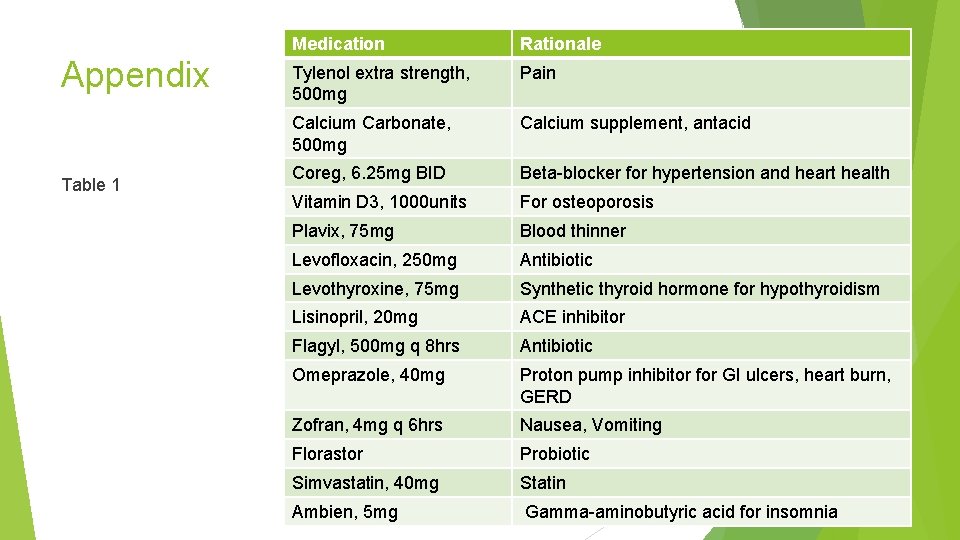
Appendix Table 1 Medication Rationale Tylenol extra strength, 500 mg Pain Calcium Carbonate, 500 mg Calcium supplement, antacid Coreg, 6. 25 mg BID Beta-blocker for hypertension and heart health Vitamin D 3, 1000 units For osteoporosis Plavix, 75 mg Blood thinner Levofloxacin, 250 mg Antibiotic Levothyroxine, 75 mg Synthetic thyroid hormone for hypothyroidism Lisinopril, 20 mg ACE inhibitor Flagyl, 500 mg q 8 hrs Antibiotic Omeprazole, 40 mg Proton pump inhibitor for GI ulcers, heart burn, GERD Zofran, 4 mg q 6 hrs Nausea, Vomiting Florastor Probiotic Simvastatin, 40 mg Statin Ambien, 5 mg Gamma-aminobutyric acid for insomnia
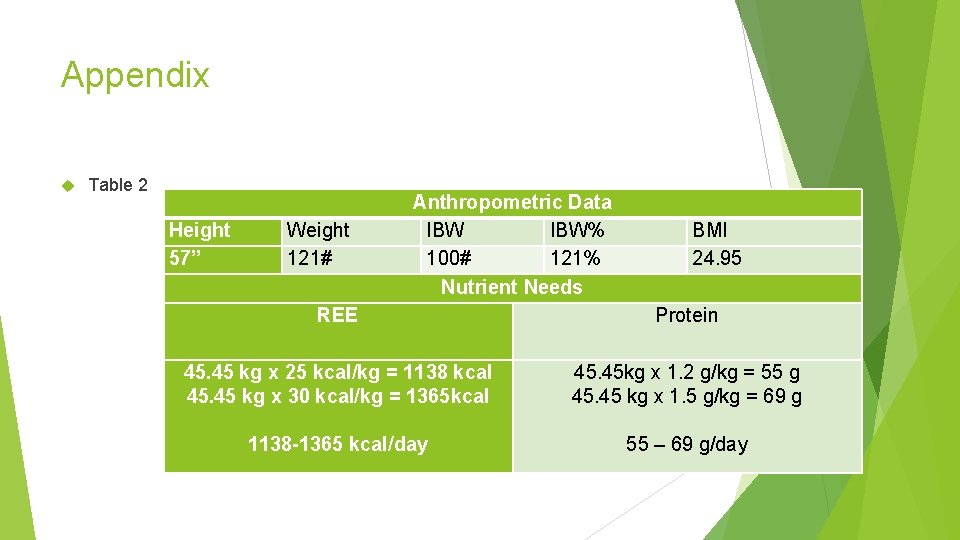
Appendix Table 2 Height 57” Weight 121# Anthropometric Data IBW% 100# 121% Nutrient Needs BMI 24. 95 REE Protein 45. 45 kg x 25 kcal/kg = 1138 kcal 45. 45 kg x 30 kcal/kg = 1365 kcal 1138 -1365 kcal/day 45. 45 kg x 1. 2 g/kg = 55 g 45. 45 kg x 1. 5 g/kg = 69 g 55 – 69 g/day
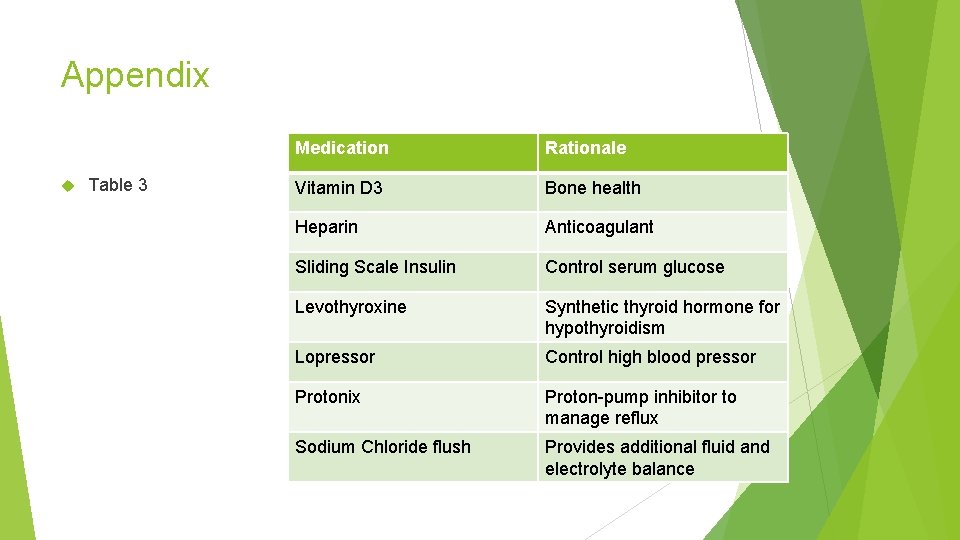
Appendix Table 3 Medication Rationale Vitamin D 3 Bone health Heparin Anticoagulant Sliding Scale Insulin Control serum glucose Levothyroxine Synthetic thyroid hormone for hypothyroidism Lopressor Control high blood pressor Protonix Proton-pump inhibitor to manage reflux Sodium Chloride flush Provides additional fluid and electrolyte balance
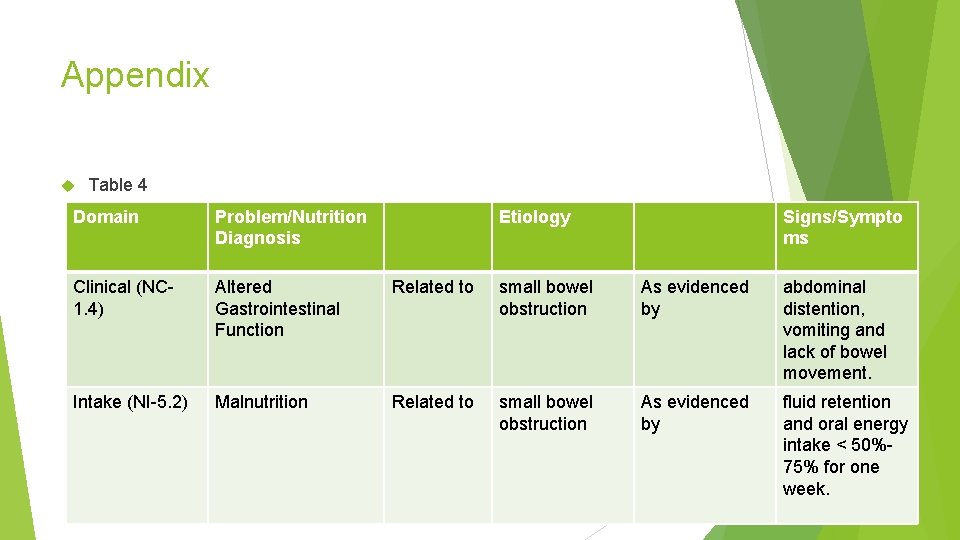
Appendix Table 4 Domain Problem/Nutrition Diagnosis Etiology Signs/Sympto ms Clinical (NC 1. 4) Altered Gastrointestinal Function Related to small bowel obstruction As evidenced by abdominal distention, vomiting and lack of bowel movement. Intake (NI-5. 2) Malnutrition Related to small bowel obstruction As evidenced by fluid retention and oral energy intake < 50%75% for one week.

References 1. Mahan LK, Escott-Stump S. Krause’s Food & Nutrition Therapy. 13 th ed. St. Louis, MO: Saunders Elsevier; 2011: 9 -10/306 -309. 2. Kulaylat MN, Doerr RJ. Small Bowel Obstruction – Surgical Treatment. National Library of Medicine. 2001. http: //www. ncbi. nlm. nih. gov/books/NBK 6873/. Accessed December 14, 2014. 3. Lucey J. Small Bowel Obstruction. NYU Langone Medical Center. http: //www. med. nyu. edu/content? Chunk. IID=96913. Accessed December 12, 2014. 4. Harris EA, Kelly AW, Pockaj BA et al. Reoperation on the Abdomen Encased in Adhesion. The American Journal of Surgery. 2002: 184 (6): 499 -504. dio: 12488146. 5. Ten Broek RPG, Issa Y, van Santbrink EJP, et al. Burden of adhesions in abdominal and pelvic surgery: systematic review and met-analysis. BMJ British Medical Journal 2013; 347: f 5588. doi: 10. 1136/bmj. f 5588. 6. Width M, Reinhard T. The Clinical Dietitian’s Essential Pocket Guide. Philadelphia, PA: Lippincott Williams and Wilkins; 2009.

References 7. ARAMARK Healthcare. Assessment and education policy #2: Nutrition status classification worksheet. Patient Food Services: Policies and Procedures, Volume IV; 2007. 8. White JV, Guenter P, Jensen G et al. Consensus Statement: Academy of Nutrition and Dietetics and American Society for Parenteral and Enteral Nutrition: Characteristics Recommended for the Identification and Documentation of Adult Malnutrition (Undernutrition). Journal of Parenteral and Enteral Nutrition. 2012: 36(3): 275 -283. DOI: 10. 1177/0148607112440285 9. American Dietetic Association. Pocket Guide for International Dietetics & Nutrition Terminology (IDNT) Reference Manual. 3 rd ed. Chicago, IL. 2011. 10. Bordeianou L, Yeh D. Overview of management of mechanical small bowel obstruction in adults. Up. To. Date. http: //www. uptodate. com/contents/overview-ofmanagement-of-mechanical-small-bowel-obstruction-in-adults. Accessed December 7, 2014.
- Slides: 35