General Approach to the Poisoned Patient An introduction





































- Slides: 43

General Approach to the Poisoned Patient (An introduction to Toxicology) Khalid Gabralla, MD Assistant Professor Emergency Medicine King Saud University

Outline Initial approach Toxic Syndromes Decontamination Diagnostic Tests Observation

Case. . . 18 year old man found “down” EMS transports Reports from scene: “he took something” No pill bottles on scene No family with him Friends that found him are long gone He is now in your ED

You are never going to know exactly what he took. . . What do I do with him? What do I order? How do I treat him? How do I decontaminate him? Do I give him an antidote? When can he go to psych (MEDICALLY CLEARED?

You can. . . Start with the basics Airway, breathing, circulation Get a better history form many sources! Get EMS to get pill bottles, tell you what they do know (found outside, inside, garage…) Call friends, family, neighbors Check Medical charts to see what he is on regularly Establish a pattern to his symptoms Toxic syndrome (TOXIDROM)

TOXIDROME constellation of physical findings that can be attributed to a specific class of toxins and can provide important clues to narrow the differential diagnosis

Toxidromes Not every drug fits into a broad based category Lots of meds have unique effects not easily grouped Polydrug overdoses may result in overlapping and confusing mixed syndromes. 5 Basic Toxidromes Sympathomimetic Opiate Anticholinergic Cholinergic Seditive Hypnotic

Toxidromes: Sympathomimetic Cocaine Methamphetamine/Amphetamines Ecstasy (MDMA) ADHD meds like ritalin, adderal Ephedrine Caffeine

Why do they do what they do? Excessive SYMPATHETIC stimulation involving epinephrine, norepinephrine and dopamine Excessive stimulation of alpha and beta adrenergic system

Features: Tachycardia +/- arrythmias Mydriasis Diaphorisis Hypertension +/- ICH Confusion with agitation Seizures Rhabdomyolysis Renal failure can result

What do you do about it? Supportive care Monitor airway, diagnose ICH, rhabdo IVF for insensible loses and volume repletion Benzos, benzos, benzos BP mgmt if severe NEVER GIVE BETA BLOCKERS Behavioral Agitation CNS excitation Cardiac excitation

Toxidrome: Opiate Morphine and codeine Heroin Methadone Meperidine Hydrocodone Oxycodone

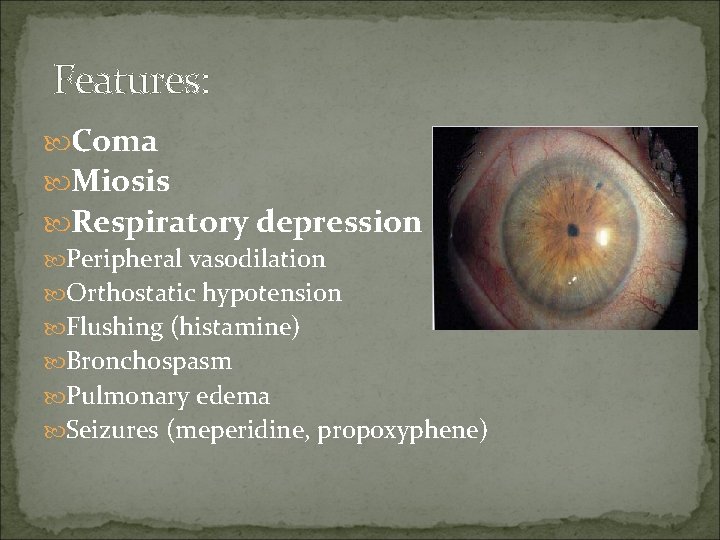
Features: Coma Miosis Respiratory depression Peripheral vasodilation Orthostatic hypotension Flushing (histamine) Bronchospasm Pulmonary edema Seizures (meperidine, propoxyphene)

What do you do about it? Competitive opioid antagonist: Naloxone Goal of return of spontanous respirations sufficient to ventilate the patient appropriately May have to re-dose as opiates may act longer than antagonist

Toxidrome: Anticholinergic • Antihistamines, • Antiparkinsonians, • Atropine, • Scopolamine, • Amantadine, • Antipsychotics, • Antidepressants, • Antispasmodics, • Mydriatics, • Muscle relaxants, • Many plants (e. g. , jimson weed, Amanita muscaria)

Why do they do what they do? By definition these agents ANTAGONIZE the effects of endogenous Acetylcholine by blocking the receptors.

What goes wrong? CNS muscarinic blockade: Peripheral muscarinic effects: Confusion Mydriasis Agitation Anhidrosis Myoclonus Tachycardia Tremor Urinary retention Abnormal speech Ileus Hallucinations Coma

What do you do about it? Supportive care IVF to replace insensible losses from agitation, hyperthermia Benzos to stop agitation Physostigmine Induces cholinergic effects Short acting May help with uncontrollable delirium Do not use if ingestion not known Danger with TCAs

Toxidrome: Cholinergic Organophosphate and carbamate insecticides. Physostigmine, edrophonium, some mushrooms.

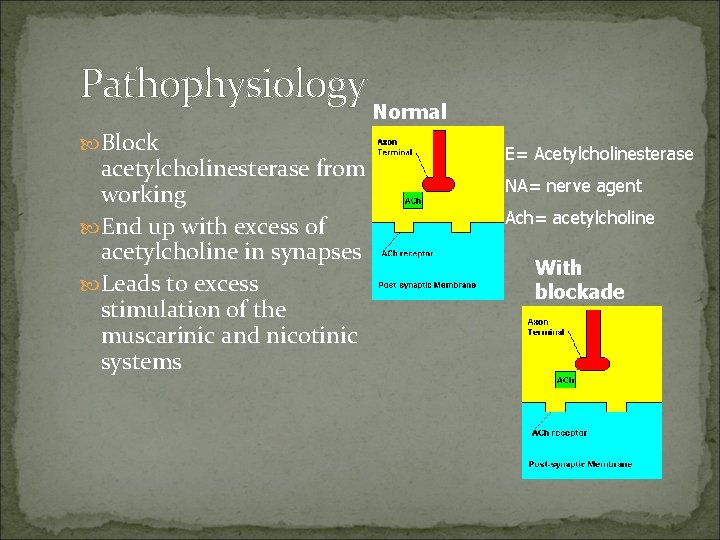
Pathophysiology Block acetylcholinesterase from working End up with excess of acetylcholine in synapses Leads to excess stimulation of the muscarinic and nicotinic systems Normal E= Acetylcholinesterase NA= nerve agent Ach= acetylcholine With blockade

Toxidrome: Cholinergic Features: S - Salivation L - Lacrimation U - Urination D - Diaphoresis G - Gasterointestinal upset vomiting, diarrhea E - Eye miosis

What do you do about it? Antagonize muscarinic symptoms Atropine Stop aging of enzyme blockade 2 -PAM Prevent and terminate seizures Diazepam Supportive care

Toxidrome: Sed-Hypnotic

Why do they do what they do? Different agents have different mechanisms Many interfere in the GABA system

What goes wrong?

What goes wrong? CNS depression, lethargy Can induce respiratory depression Can produce bradycardia or hypotension

What do you do about it? Supportive care Be wary of the benzo “antidote” Flumazinil Is an antagonist at the benzo receptor RARELY INDICATED If seizures develop either because of benzo withdrawal, a co-ingestant or metabolic derangements, have to use 2 nd line agents, barbiturates, for seizure control

So back to our patient. . . Agitated, pupils 8 mm, sweaty, HR 140’s, BP 230/130 Sympathomimetic Unarousable, RR 4, pupils pinpoint Opiate Confused, pupils 8 mm, flushed, dry skin, no bowel sounds, 1000 cc output with Foley Anticholinergic Vomiting, urinating uncontrollably, HR 40, Pox 80% from bronchorrhea, pupils 2 mm Cholinergic Lethargic, HR 67, BP 105/70, RR 12, pupils midpoint Sedative Hypnotic

So ED approach: Airway, breathing, circulation Establish IV, O 2 and cardiac monitor Consider coma cocktail Thiamine, D 50, Narcan Evaluate history and a thorough physical exam Look at vitals, pupils, neuro, skin, bowel sounds. . . Gives you hints regarding the general class of toxins Guides your supportive care Draw blood / urine for testing Time to consider decontamination options

Gastric Decontamination Overview Induce vomiting – Ipecac Take out pills from the stomach – Lavage Adsorb the toxins in the gut – Charcoal Flush out the system – Whole Bowel

Gastric Decontamination Overview The vast majority of patients are unlikely to benefit from gastric decontamination They have ingested nontoxic substances They have ingested nontoxic amount of toxic substances They present long after decontamination would be expected to be of any benefit!

Gastric Decontamination Overview Patients who theoretically may benefit from decontamination: - Present early after ingestion (1 hour) - Have taken a delayed release products - Have taken potentially life-threatening overdose No prospective studies have demonstrated outcome benefit with gastric decontamination.

Ipecac Emetine and Cephaeline Induces emesis DOES NOT HAVE A ROLE IN ED CARE

Gastric Lavage Rarely, if ever, indicated Life threatening ingestions that occurred within < 1 hour American Academy of Clinical Toxicology Airway protection is key Lots of complications

Activated Charcoal No proven outcome benefit, and its use should be carefully weighed against potential complications. Works to adsorb substances to its matrix Not for metals, caustics, alcohol, alkali, acid, hydrocarbons contraindications Aspiration, ARDS, bowel obstruction Dosing 1 g/kg po dose, +/- single dose of cathartic

If GI decontamination is considered, no matter the method, potential benefit must be weighed against the potential complications.

Now you are ready to order diagnostic studies. . . Want to evaluate Acid base status Renal function Liver function Cardiac conduction ECG Drug levels Based on history or clinical findings Any toxin specific findings CK for cocaine, …etc

Other common ingestants may have common dx test abnormalities. . . Paracetamol level, LFT, coags Salicylates ASA level, metabolic acidosis, respiratory alkalosis, renal insufficiency, anion gap SSRI Prolonged QTc Toxic Alcohols Osmolal. gap with ethylene glycol, methanol and isopropyl alcohol Anion gap acidosis with EG and methanol

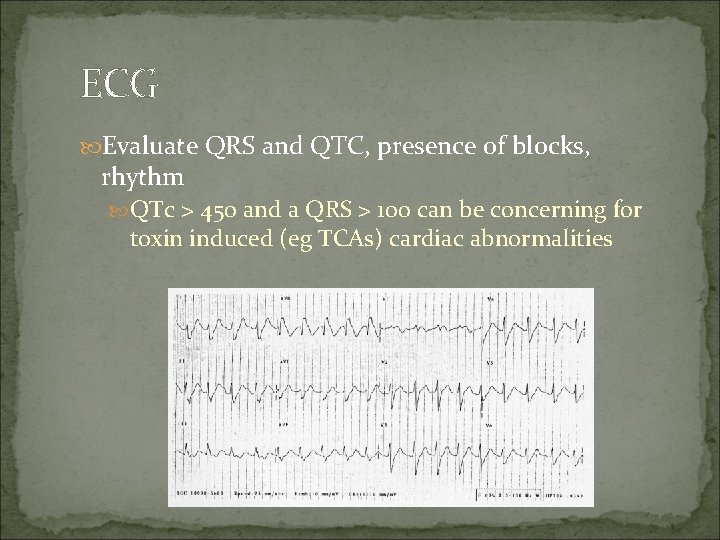
ECG Evaluate QRS and QTC, presence of blocks, rhythm QTc > 450 and a QRS > 100 can be concerning for toxin induced (eg TCAs) cardiac abnormalities

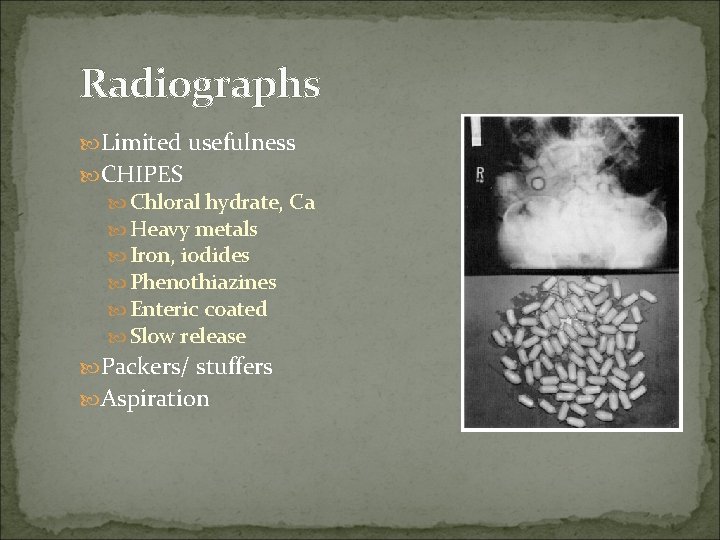
Radiographs Limited usefulness CHIPES Chloral hydrate, Ca Heavy metals Iron, iodides Phenothiazines Enteric coated Slow release Packers/ stuffers Aspiration

Observation Period Normal labs, normal ECG, normal exam, no history of extended release drug Approximately 6 hours Extended release medications, oral hypoglycemics involved Depending on agent, 12 -24 hours

So back to your patient. . . How do I treat him Good supportive care, good physical examination How do I decontaminate him( if I need to do!) A. Charcoal as long as he is not in aspiration risk What do I order Chem, ASA, Paracetamol, ECG at a minimum Do I give him an antidote Coma cocktail, others as indicated by clinical condition & or labs. When can he go to psych? Observe for 6 hours and re-evaluate

Thank You.