Drugs for Diabetes Mellitus Diabetes Mellitus Overview of

Drugs for Diabetes Mellitus

Diabetes Mellitus: Overview of the Disease and Its Treatment Diabetes mellitus Ø Ø Disorder of carbohydrate metabolism Ø Ø Greek word for “fountain” Latin word for “honey” Deficiency of insulin Resistance to action of insulin Sustained hyperglycemia, polyuria, polydipsia, ketonuria, and weight loss

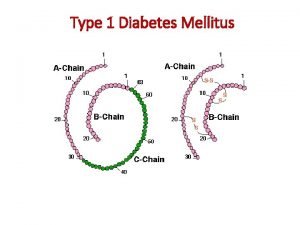
Types of Diabetes Mellitus Type 1 diabetes 5%– 10% of all cases Also called insulin-dependent diabetes mellitus (IDDM) or juvenile-onset diabetes mellitus Ø Primary defect is destruction of pancreatic beta cells Ø Ø

Types of Diabetes Mellitus Type 2 diabetes Most prevalent form of diabetes Approximately 22 million Americans have it Also called non–insulin-dependent diabetes mellitus (NIDDM) or adult-onset diabetes mellitus Ø Insulin resistance and impaired insulin secretion Ø Ø Ø

Complications of Diabetes Short-term Ø Hyperglycemia and hypoglycemia Long-term Ø Macrovascular damage • Heart disease • Hypertension • Stroke • Hyperglycemia • Altered lipid metabolism

Complications of Diabetes Long-term (cont’d) Ø Microvascular damage • Retinopathy • Nephropathy • Neuropathy • Gastroparesis • Amputation secondary to infection

Diabetes and Pregnancy Before insulin: many babies born to severely diabetic women died Factors during pregnancy Placenta produces hormones that antagonize the actions of insulin Ø Production of cortisol increases threefold Ø Glucose can pass freely from the maternal to the fetal circulation (fetal hyperinsulinemia) Ø

Diabetes and Pregnancy Proper glucose levels needed in pregnant patient and in fetus to prevent teratogenic effects Fetal death frequently occurs near term Earlier delivery is desirable Gestational diabetes

Diagnosis of Diabetes Excessive plasma glucose is diagnostic of diabetes Patient must be tested on two separate days, and both tests must be positive Three tests Ø Ø Ø Fasting plasma glucose (FPG) Casual plasma glucose Oral glucose tolerance test (OGTT) Hemoglobin A 1 c, oral glucose tolerance test

Prediabetes Impaired fasting plasma glucose between 100 and 125 mg/d. L Impaired glucose tolerance test Increased risk for developing type 2 diabetes May reduce risk with diet changes and exercise and possibly with certain oral antidiabetic drugs Many people who meet criteria for “prediabetes” never develop diabetes, even if they do not take precautions against diabetes

Overview of Diabetes Treatment Primary goal is to prevent long-term complications Tight control of blood glucose level is important Also important to control blood pressure and blood lipids

Type 1 Diabetes Requires comprehensive plan Integrated program of diet, self-monitoring of blood glucose, exercise, and insulin replacement Dietary measures Total number of carbohydrates, not the type of carbohydrates, is most important Ø Glycemic index Ø

Type 2 Diabetes Similar to type 1, requires comprehensive plan Should be screened and treated for: Ø Hypertension, nephropathy, retinopathy, neuropathy, dyslipidemias Glycemic control with: Ø Ø Modified diet and exercise Drug therapy
Monitoring Treatment Self-monitoring of blood glucose (SMBG) Hemoglobin A 1 c

Insulin: Physiology Biosynthesis Secretion Metabolic actions Metabolic consequences of insulin deficiency

Seven Types of Insulin Short duration: rapid acting Ø Ø Ø Short duration: slower acting Ø Regular insulin (Humulin R, Novolin R) Intermediate duration Ø Ø Insulin lispro (Humalog) Insulin aspart (Novo. Log) Insulin glulisine (Apidra) Neutral protamine Hagedorn (NPH) insulin Insulin detemir (Levemir) Long duration Ø Insulin glargine

Insulin Concentration Ø Ø 100 units/m. L (U-100) 500 units/m. L (U-500) Mixing insulins Ø Ø NPH with short-acting insulins Short-acting insulin drawn first

Administration Subcutaneous injection Ø Ø Ø Subcutaneous infusion Ø Ø Syringe and needle Pen injectors Jet injectors Portable insulin pumps Implantable insulin pumps (experimental) Intravenous infusion

Storage Unopened vials should be stored under refrigeration until needed Should not be frozen Can be used until expiration date if kept in refrigerator After opening, can be kept up to 1 month without significant loss of activity Keep out of direct sunlight and extreme heat

Storage Mixtures of insulin in vials are stable for 1 month at room temperature and for 3 months under refrigeration Mixtures in pre-filled syringes should be stored in refrigerator for at least 1 week and should be stored vertically with needle pointing up

Insulin: Therapeutic Use Indications Ø Ø Ø Principal: diabetes mellitus Required by all type 1 and some type 2 patients IV insulin for DKA Hyperkalemia: can promote uptake of potassium Aids in the diagnosis of GH deficiency

Insulin Therapy of Diabetes Dosage Dosing schedules Ø Ø Ø Conventional therapy Intensive conventional therapy Continuous sub. Q infusion Achieving tight glucose control

Complications of Insulin Treatment Hypoglycemia Lipohypertrophy Allergic reactions Hypokalemia Drug interactions Ø Ø Ø Hypoglycemic agents Hyperglycemic agents Beta-adrenergic blocking agents

Oral Hypoglycemics Biguanides Ø Sulfonylureas Thiazolidinediones (glitazones) Ø Ø Metformin (Glucophage) Rosiglitazone (Avandia) Pioglitazone (Actos) Meglitinides (Glinides) Ø Ø Repaglinide (Prandin) Nateglinide (Starlix)

Oral Hypoglycemics Alpha-glucosidase inhibitors Ø Ø Acarbose (Precose) Miglitol (Glyset) Gliptins Combination products

Combination Products Metformin/Glyburide Metformin/Glipizide Metformin/Saxagliptin Metformin/Pioglitazone Metformin/Repaglinide Metformin/Sitagliptin Pioglitazone/Glimepiride Rosiglitazone/Metformin Sitagliptin/Simvastatin

Injected Drugs (Other than Insulin) Exenatide Adjunctive therapy to improve glycemic control in patients with type 2 diabetes Ø Adverse effects • Hypoglycemia • Gastrointestinal effects Ø Liraglutide Pramlintide

Acute Complications of Poor Glycemic Control Diabetic ketoacidosis (DKA) and hyperglycemic hyperosmotic nonketotic syndrome (HHNS): Both conditions are hyperglycemic crises Hyperglycemia is more severe in HHNS No ketoacidosis in HHNS

Diabetic Ketoacidosis Severe manifestation of insulin deficiency Symptoms evolve quickly in a period of hours or days Most common complication in pediatric patients and leading cause of death Characteristics Ø Ø Ø Hyperglycemia Ketoacids Hemoconcentration Acidosis Coma

Diabetic Ketoacidosis Altered glucose metabolism Ø Ø Ø Hyperglycemia Water loss Hemoconcentration Altered fat metabolism Ø Production of ketoacids

Diabetic Ketoacidosis Treatment Ø Ø Ø Insulin replacement Bicarbonate for acidosis Water and sodium replacement Potassium replacement Normalization of glucose levels

HHNS Large amount of glucose excreted in urine Dehydration and loss of blood volume Increases the blood concentrations of electrolytes and nonelectrolytes (particularly glucose); also increases hematocrit Blood “thickens” and becomes sluggish

HHNS Little or no change in ketoacid levels Little or no change in blood p. H No sweet or acetone-like smell to urine or breath HHNS occurs most frequently with type 2 diabetes mellitus with acute infection, acute illness, or some other stress

HHNS Can evolve slowly Ø Metabolic changes begin a month or two before signs and symptoms become apparent If untreated, HHNS can lead to coma, seizures, and death Management Ø Correct hyperglycemia and dehydration with IV insulin, fluids, and electrolytes

Glucagon for Insulin Overdose Preferred treatment is IV glucose Ø Immediately raises blood glucose level Glucagon can be used if IV glucose is not available Ø Ø Delayed elevation of blood glucose Will not work in starvation • Promotes glycogen breakdown and the malnourished have little glycogen left
- Slides: 35