Diabetes Mellitus Definition metabolic disorder characterized by hyperglycemia

Diabetes Mellitus Definition: metabolic disorder characterized by hyperglycemia due to an absolute or relative lack of insulin or to a cellular resistance to insulin Major classifications • 1. Type 1 Diabetes • 2. Type 2 Diabetes

Diabetes Mellitus Impact on health of American population • 1. Sixth leading cause of death due to cardiovascular effects resulting in atherosclerosis, coronary artery disease, and stroke • 2. Leading cause of end stage renal failure • 3. Major cause of blindness • 4. Most frequent cause of non-traumatic amputations

Diabetes Mellitus • 5. Diabetes affects estimated 15. 7 million people (10. 3 million are diagnosed; 5. 4 million are undiagnosed) • 6. Increasing prevalence of Type 2 Diabetes in older adults and minority groups (African American, American Indian and Hispanic populations) • 7. Estimated 11 % of older U. S. population (65 – 74) have diabetes

Diabetes Mellitus Diabetes Type 1 Definition • 1. Metabolic condition in which the beta cells of pancreas no longer produce insulin; characterized by hyperglycemia, breakdown of body fats and protein and development of ketosis • 2. Accounts for 5 – 10 % of cases of diabetes; most often occurs in childhood or adolescence • 3. Formerly called Juvenile-onset diabetes or insulin-dependent diabetes (IDDM)

Diabetes Mellitus Pathophysiology • 1. Autoimmune reaction in which the beta cells that produce insulin are destroyed • 2. Alpha cells produce excess glucagons causing hyperglycemia Risk Factors • 1. Genetic predisposition for increased susceptibility; HLA linkage • 2. Environmental triggers stimulate an autoimmune response • a. Viral infections (mumps, rubella, coxsackievirus B 4) • b. Chemical toxins

Diabetes Mellitus Manifestations 1. Process of beta cell destruction occurs slowly; hyperglycemia occurs when 80 – 90% is destroyed; often trigger stressor event (e. g. illness)

Diabetes Mellitus 2. Hyperglycemia leads to • a. Polyuria (hyperglycemia acts as osmotic diuretic) • b. Glycosuria (renal threshold for glucose: 180 mg/d. L) • c. Polydipsia (thirst from dehydration from polyuria) • d. Polyphagia (hunger and eats more since cell cannot utilize glucose) • e. Weight loss (body breaking down fat and protein to restore energy source • f. Malaise and fatigue (from decrease in energy) • g. Blurred vision (swelling of lenses from osmotic effects)

Diabetes Mellitus • Diagnosis – Patient is symptomatic plus • Casual plasma glucose (non-fasting) is 200 mg/dl OR • Fasting plasma glucose of 126 mg/dl or higher OR • Two hour plasma glucose level of 200 mg/dl or greater during an oral glucose tolerance test

Diabetes Mellitus Diabetic Ketoacidosis (DKA) 1. Results from breakdown of fat and overproduction of ketones by the liver and loss of bicarbonate 2. Occurs when Diabetes Type 1 is undiagnosed or known diabetic has increased energy needs, when under physical or emotional stress or fails to take insulin 1. 3. • • • Mortality as high as 14% Pathophysiology a. Hypersomolarity (hyperglycemia, dehydration) b. Metabolic acidosis (accumulation of ketones) c. Fluid and electrolyte imbalance (from osmotic diuresis)

Diabetes Mellitus Diagnostic tests • a. Blood glucose greater than 250 mg/d. L • b. Blood p. H less than 7. 3 • c. Blood bicarbonate less than 15 m. Eq/L • d. Ketones present in blood • e. Ketones and glucose present in urine • f. Electrolyte abnormalities (Na, K, Cl) • G. serum osmolality < 350 mosm/kg (normal 280 -300)

Diabetes Mellitus • DKA – Signs and symptoms • Kussmals respirations – Blow off carbon dioxide to reverse acidosis • • • Fruity breath Nausea/ abdominal pain Dehydration Lethargy Coma Polydipsia, polyuria, polyphagia

Diabetes Mellitus Treatment • a. Requires immediate medical attention and usually admission to hospital • B. Frequent measurement of blood glucose and treat according to glucose levels with regular insulin (mild ketosis, subcutaneous route; severe ketosis with intravenous insulin administration) • c. Restore fluid balance: initially 0. 9% saline at 500 – 1000 m. L/hr. ; regulate fluids according to client status; when blood glucose is 250 mg/d. L add dextrose to intravenous solutions

Diabetes Mellitus • DKA – d. Correct electrolyte imbalance: client often is initially hyperkalemic • As patient is rehydrated and potassium in pushed back into the cell they become hypokalemic • Monitor K levels – e. Monitor cardiac rhythm since hypokalemia puts client at risk for dysrrhythmias – f. Treat underlying condition precipitating DKA – G. Acidosis is corrected with fluid and insulin therapy and rarely needs bicarb

Diabetes Mellitus Diabetes Type 2 • A. Definition: condition of fasting hyperglycemia occurring despite availability of body’s own insulin • B. Was known as non-insulin dependent diabetes or adult onset diabetes – Both are misnomers, it can be found in children and type II DM may require insulin

Diabetes Mellitus Pathophysiology • 1. Sufficient insulin production to prevent DKA; but insufficient to lower blood glucose through uptake of glucose by muscle and fat cells • 2. Cellular resistance to insulin increased by obesity, inactivity, illness, age, some medications

Diabetes Mellitus Risk Factors • 1. History of diabetes in parents or siblings; no HLA • 2. Obesity (especially of upper body) • 3. Physical inactivity • 4. Race/ethnicity: African American, Hispanic, or American Indian origin • 5. Women: history of gestational diabetes, polycystic ovary syndrome, delivered baby with birth weight > 9 pounds • 6. Clients with hypertension; HDL cholesterol < 35 mg/d. L, and/or triglyceride level > 250 mg/dl.

Diabetes Mellitus • Syndrome X or Metabolic Syndrome – Chronic, low grade inflammatory process – Gives rise to diabetes type 2, ischemic heart disease, left ventricular hypertrophy – Group of disorders with insulin resistance as the main feature – Includes • • Obesity especially around the waist and abdomen Low levels of physical activity High blood pressure Increased blood cholesterol (high LDL, low HDL, high triglycerides

Diabetes Mellitus Manifestations 1. Client usually unaware of diabetes • a. Discovers diabetes when seeking health care for another concern • b. Most cases aren’t diagnosed for 5 -6 years after the development of the disease • c. Usually does not experience weight loss

Diabetes Mellitus 2. Possible symptoms or concerns • a. Hyperglycemia (not as severe as with Type 1) • b. Polyuria • c. Polydipsia • d. Blurred vision • e. Fatigue • f. Paresthesias (numbness in extremities) • g. Skin Infections

Diabetes Mellitus Hypersomolar Hyperglycemic Nonketotic Syndrome (HHNS) 1. Potential complication of Diabetes Type 2 2. Life threatening medical emergency, high mortality rate, as high as 50% 3. Enough insulin is secreted to prevent ketosis, but not enough to prevent hyperglycemia 4. High blood sugar causes an extreme diuresis with severe electrolyte and fluid loss

• Characterized by – Plasma osmolarity 340 m. Osm/l or greaternormal 280 -300 – Blood glucose severely elevated, 800 -1000 – Altered level of consciousness

Diabetes Mellitus 4. Precipitating factors • a. Infection (most common) – pneumonia • b. Therapeutic agent or procedure • c. Acute or chronic illness – – 5. MI Stroke Pancreatitis pregnancy Slow onset 1 – 14 days

Diabetes Mellitus Pathophysiology • a. Hyperglycemia leads to increased urine output and dehydration • b. Kidneys retain glucose; glucose and sodium rise • c. Severe hyperosmolar state develops leading to brain cell shrinkage Manifestations • a. Altered level of consciousness (lethargy to coma) • b. Neurological deficits: hyperthermia, motor and sensory impairment, seizures • c. Dehydration: dry skin and mucous membranes, extreme thirst, tachycardia, polyuria, hypotension

Diabetes Mellitus Treatment • a. Usually admitted to intensive care unit of hospital for care since client is in life-threatening condition: unresponsive, may be on ventilator, has nasogastric suction • b. Correct fluid and electrolyte imbalances giving isotonic or colloid solutions and correct potassium deficits • c. Lower glucose with regular insulin until glucose level drops to 250 mg/d. L • Monitor for renal failure • d. Treat underlying condition

Diabetes Mellitus Complications of Diabetes A. Alterations in blood sugars: hyperglycemia and hypoglycemia B. Macrocirculation (large blood vessels) • 1. Atherosclerosis occurs more frequently, earlier in diabetics • 2. Involves coronary, peripheral, and cerebral arteries C. Microcirculation (small blood vessels) • 1. Affects basement membrane of small blood vessels and capillaries • 2. Involves tissues affecting eyes and kidneys D. Prevention of complications • 1. Managing diabetes • 2. Lowering risk factors for conditions • 3. Routine screening for complications • 4. Implementing early treatment

Diabetes Mellitus Complications of Diabetes: Alterations in blood sugars A. Hyperglycemia: high blood sugar • 1. DKA (mainly associated with Diabetes Type 1) • 2. HHS (mainly associated with Diabetes Type 2) • 3. Dawn phenomenon: rise in blood sugar between 4 am and 8 am, not associated with hypoglycemia – Glucose released from the liver in the early AM secondary to growth hormones – Altering the time and dose of the insulin (NPH or Ultralente) by 2 -3 units stabilizes the blood sugar

Diabetes Mellitus • 4. Somogyi effect: combination of hypoglycemia during night with a rebound morning hyperglycemia that may lead to insulin resistance for 12 to 48 hours

Diabetes Mellitus B. Hypoglycemia (insulin reaction, insulin shock, “the lows”): low blood sugar • 1. Mismatch between insulin dose, carbohydrate availability and exercise • 2. May be affected by intake of alcohol, certain medications

Diabetes Mellitus Specific manifestations • a. Cool, clammy skin • b. Rapid heartbeat • c. Hunger • d. Nervousness, tremor • e. Faintness, dizziness • f. Unsteady gait, slurred and/or incoherent speech • g. Vision changes • h. Seizures, coma • 5. Severe hypoglycemia can result in death • 6. Clients taking medications, such as beta-adrenergic blockers may not experience manifestations associated with autonomic nervous system • 7. Hypoglycemia unawareness: clients with Diabetes Type 1 for 4 or 5 years or more may develop severe hypoglycemia without symptoms which can delay treatment

Diabetes Mellitus Treatment for mild hypoglycemia • a. Immediate treatment: client should take 15 gm of rapid-acting sugar (half cup of fruit juice; 8 oz of skim milk, 3 glucose tablets, 3 life savers • b. 15/15 rule: wait 15 minutes and monitor blood glucose; if still low, client should eat another 15 gm of sugar • c. Continue until blood glucose level has returned to normal • d. Client should contact medical care provider if hypoglycemia occurs more that 2 or 3 times per week

Diabetes Mellitus Treatment for severe hypoglycemia is often hospitalization a. Client is unresponsive, has seizures, or has altered behavior; blood glucose level is less than 50 mg/d. L b. If client is conscious and alert, administer 15 gm of sugar c. If client is not alert, administer • 1. 25 %– 50% solution of glucose intravenously, followed by infusion of 5% dextrose in water • 2. Glucagon 1 mg by subcutaneous, intramuscular, or intravenous route; follow with oral or intravenous carbohydrate d. Monitor client response physically and also blood glucose level

Diabetes Mellitus Complications Affecting Cardiovascular System, Vision, and Kidney Function A. Coronary Artery Disease • 1. Major risk of myocardial infarction in Type 2 diabetics – Increased chance of having a silent MI and delaying medical treatment • 2. Most common cause of death for diabetics (40 – 60%) • 3. Diabetics more likely to develop Congestive Heart Failure

Diabetes Mellitus B. Hypertension • 1. Affects 20 – 60 % of all diabetics • 2. Increases risk for retinopathy, nephropathy

Diabetes Mellitus • C. Stroke: – Type 2 diabetics are 2 – 6 times more likely to have stroke as well as Transient Ischemic Attacks (TIA) or mini stroke

Diabetes Mellitus D. Peripheral Vascular Disease • 1. Increased risk for Types 1 and 2 diabetics • 2. Development of arterial occlusion and thrombosis resulting in gangrene • 3. Gangrene from diabetes most common cause of non-traumatic lower limb amputation
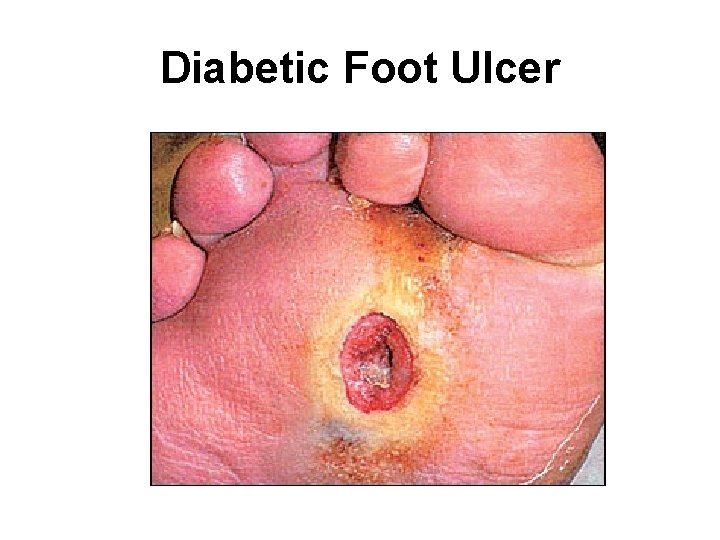
Diabetic Foot Ulcer

Diabetes Mellitus Diabetic Retinopathy 1. Definition • a. Retinal changes related to diabetes – • 2. • • 3. Hemorrhage, swelling, decreased vision b. Leads to retinal ischemia and breakdown of blood-retinal barrier Leading cause of blindness ages 25 – 74 a. Affects almost all Type 1 diabetics after 20 years b. Affects 60 % of Type 2 diabetics Diabetics should be screened for retinopathy and receive treatment (laser photocoagulation surgery) to prevent vision loss 1. 4. Should be sent immediately to ophthalmologist upon diagnosis because may already have damage Diabetics also have increased risk for cataract development

Diabetes Mellitus Diabetic Nephropathy • 1. Definition: glomerular changes in kidneys of diabetics leading to impaired renal function • 2. First indicator: microalbuminuria • 3. Diabetics without treatment go on to develop hypertension, edema, progressive renal insufficiency • a. In type 1 diabetics, 10 – 15 years • b. May occur soon after diagnosis with type 2 diabetes since many are undiagnosed for years • 4. Most common cause of end-stage renal failure in U. S. • 5. Kimmelstiel-Wilson syndrome: glomerulosclerosis associated with diabetes

Diabetes Mellitus • Male erectile dysfunction – Half of all diabetic men have erectile dysfunction

Diabetes Mellitus Collaborative Care A. Based on research from 10 -year study of Type 1 diabetics conducted by NIH focus is on keeping blood glucose levels as close to normal by active management interventions; complications were reduced by 60% B. Treatment interventions are maintained through • 1. Medications • 2. Dietary management • 3. Exercise C. Management of diabetes with pancreatic transplant, pancreatic cell or Beta cell transplant is in investigative stage

Diabetes Mellitus Other Complications from Diabetes • A. Increased susceptibility to infection • 1. Predisposition is combined effect of other complications • 2. Normal inflammatory response is diminished • 3. Slower than normal healing • B. Periodontal disease • C. Foot ulcers and infections: predisposition is combined effect of other complications

Diabetes Mellitus Diagnostic tests to monitor diabetes management 1. Fasting Blood Glucose (normal: 70 – 110 mg/d. L) 2. Glycosylated hemoglobin (c) (Hemoglobin A 1 C) • a. Considered elevated if values above 7% • b. Blood test analyzes excess glucose attached to hemoglobin. Since rbc lives about 120 days gives an average of the blood glucose over previous 2 to 3 months – Not a fasting test, can be drawn any time of the day – % of glycated (glucose attached) hemoglobin measures how much glucose has been in the bloodstream for the past 3 months )

Diabetes Mellitus • 3. Urine glucose and ketone levels (part of routine urinalysis) – a. Glucose in urine indicates hyperglycemia (renal threshold is usually 180 mg/d. L) – b. Presence of ketones indicates fat breakdown, indicator of DKA; ketones may be present if person not eating 4. Urine albumin (part of routine urinalysis) • a. If albumin present, indicates need for workup for nephropathy • b. Typical order is creatinine clearance testing

Diabetes Mellitus 5. Cholesterol and Triglyceride levels • a. Recommendations • 1. LDL < 100 mg/dl • 2. HDL > 45 mg/d. L • 3. Triglycerides < 150 mg/d. L • b. Monitor risk for atherosclerosis and cardiovascular complications 6. Serum electrolytes in clients with DKA or HHNS

Diabetes Mellitus A. • 2. • • • Medications Insulin 1. Sources: standard practice is use of human insulin prepared by alteration of pork insulin or recombinant DNA therapy Clients who need insulin as therapy: a. All type 1 diabetics since their bodies essentially no longer produce insulin b. Some Type 2 diabetics, if oral medications are not adequate for control (both oral medications and insulin may be needed) c. Diabetics enduring stressor situations such as surgery, corticosteroid therapy, infections, treatment for DKA, HHNS d. Women with gestational diabetes who are not adequately controlled with diet e. Some clients receiving high caloric feedings including tube feedings or parenteral nutrition

Diabetes Mellitus • Injection sites – Abdominal areas is the most preferred because of rapid absorption – Do not aspirate insulin injections – Administration covered in the lab
Diabetes Mellitus
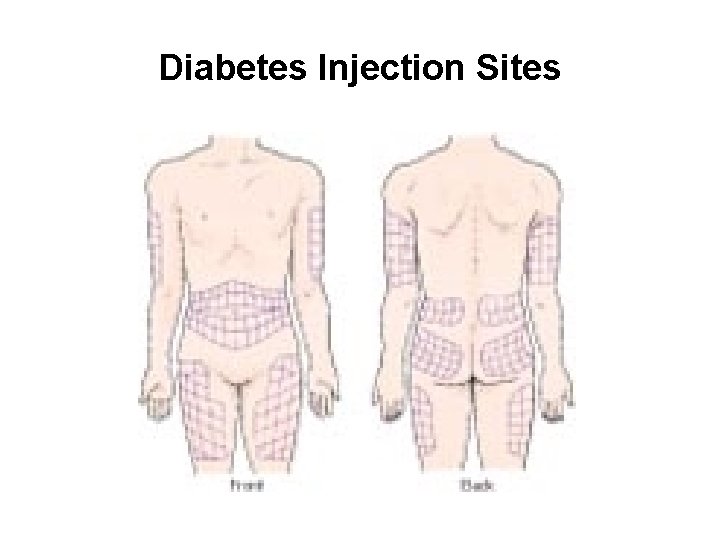
Diabetes Injection Sites

Diabetes Mellitus • When rapid acting or short acting insulin is mixed with longer acting insulin, draw the short acting insulin into the syringe first. • Prevents contamination of the shorter acting insulin with the longer acting insulin • Draw up clear, then cloudy • Insuling glargine (Lantus) should not be mixed with any other insulin
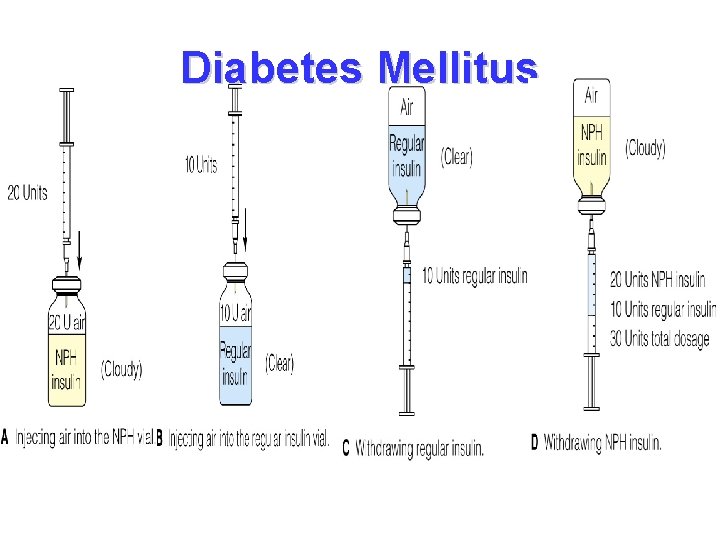
Diabetes Mellitus • Mixing insulin

Diabetes Mellitus • Alternative insulin administration – Insulin pump • Continuous subcutaneous infusion of a basal dose with increases at meal times – Implanted pumps • Implanted into the peritoneal cavity – Inhaled insulin • Under development

Insulin Pump
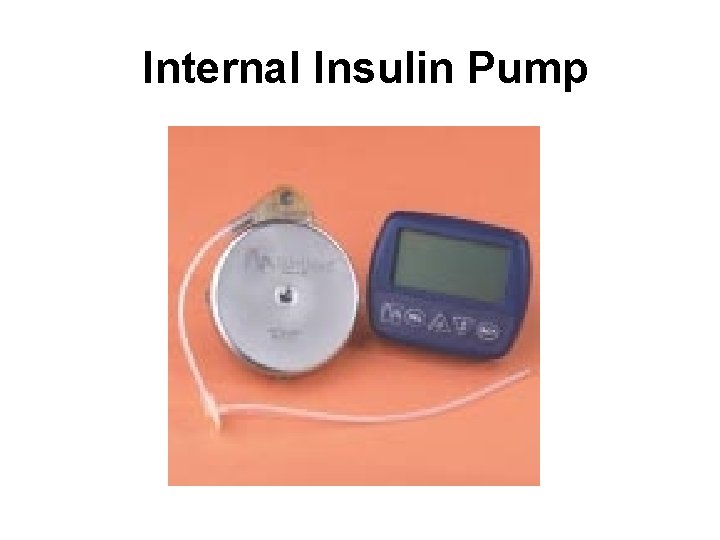
Internal Insulin Pump

Diabetes Mellitus Oral Hypoglycemic Agents • 1. Used to treat Diabetes Type 2 • 2. Client must also maintain prescribed diet and exercise program; monitor blood glucose levels • 3. Not used with pregnant or lactating women • 4. Several different oral hypoglycemic agents and insulin may be prescribed for the client • 5. Specific drug interactions may affect the blood glucose levels • 6. Must have some functioning beta cells

Diabetes Mellitus Classifications and action a. Sulfonylureas • 1. Action: Stimulates pancreatic cells to secrete more insulin and increases sensitivity of peripheral tissues to insulin • 2. Used: to treat non-obese Type 2 diabetics • 3. Example: Glipizide (Glucotrol), Chlorpropamide (Diabinese), Tolazamide (Tolinase)

Diabetes Mellitus b. Meglitinides • 1. Action: stimulates pancreatic cells to secret more insulin • 2. Taken just before meals, rapid onset, limited duration of action • 3. Major adverse effects is hypoglycemia • 4. Used in non-obese diabetics • 5. Example: Repaglinide (Prandin), Nateglinide (Starlix)

Diabetes Mellitus c. Biguanides • 1. Action: decreases overproduction of glucose by liver and makes insulin more effective in peripheral tissues • 2. Used in obese diabetics • 3. Does not stimulate insulin release • 4. Metabolized by the kidney, do not use with renal patients • 5. Example: Metformin (Glucophage

Diabetes Mellitus d. Alpha-glucoside Inhibitors • 1. Action: Slow carbohydrate digestion and delay rate of glucose absorption • 2. Take with first bite of the meal or 15 min. after • 3. Adjunct to diet to decrease blood glucose levels • 4. Example: Acarbose (Precose), Miglitol (Glyset)

Diabetes Mellitus Thizaolidinediones (Glitazones) • 1. Action: Sensitizes peripheral tissues to insulin • 2. Used in obese diabetics • 3. Inhibits glucose production • 4. Improves sensitivity to insulin in muscle, and fat tissue • 5. Example: Rosiglitazone (Avandia), Pioglitazone (Actos)

Diabetes Mellitus • Patients with Type 2 DM who are obese have insulin resistance, they produce enough insulin – Should use Glucophage, Actos or Avandia – Enhances insulin secretion in tissue, but does not increase amount of insulin secreted

Diabetes Mellitus • Patients with Type 2 DM who are thin do not produce enough insulin, they are not insulin resistant – Need sulfonylurea agents like Diabinese, Tolinase, Glucotrol, Diabeta

Diabetes Mellitus Role of Diet in Diabetic Management A. Goals for diabetic therapy include • 1. Maintain as near-normal blood glucose levels as possible with balance of food with medications • 2. Obtain optimal serum lipid levels • 3. Provide adequate calories to attain or maintain reasonable weight

Diabetes Mellitus B. Diet Composition • 1. Carbohydrates: 60 – 70% of daily diet – Carbohydrates convert quickly to sugars • Advice patient to consume a similar amount of carbs at each meal • Medications can work on a consistent glucose response from foods • 2. Protein: 15 – 20% of daily diet • 3. Fats: No more than 10% of total calories from saturated fats

Diabetes Mellitus • 4. Fiber: 20 to 35 grams/day; promotes intestinal motility and gives feeling of fullness • 5. Sodium: recommended intake 1000 mg per 1000 kcal • 6. Sweeteners approved by FDA instead of refined sugars • 7. Limited use of alcohol: potential hypoglycemic effect of insulin and oral hypoglycemics

Diabetes Mellitus • Diet – Look for more dietary information online at http: //www. diabetes. org/nutrition-andreceipes/nutrition/overview. jsp

Diabetes Mellitus Care of diabetic older clients • A. 40% of all clients with diabetes are over age of 65 • B. Need to include spouse, members of family in teaching who may assist with client meeting medical needs • C. Diet changes may be difficult to implement since client has established eating habits • D. Exercise programs may need adjustment to meet individual’s abilities (such as physical limitations from other chronic illnesses) – Obesity worsens diabetes – Minimum of 30 minutes of moderate exercise like walking or swimming most days of the week

Diabetes Mellitus • E. Individual reluctance to accept assistance to deal with chronic illness, assist with hygiene • F. Limited assets for medications, supplies, dietary • G. Visual deficits or learning challenges to learn insulin administration, blood glucose monitoring

Diabetes Mellitus Nursing Care • A. Assessment, planning, implementation with client according to type and stage of diabetes • B. Prevention, assessment and treatment of complications through client self-management and keeping appointments for medical care • C. Client and family teaching for diabetes management • D. Health promotion includes education of healthy life style, lowering risks for developing diabetes for all clients • E. Blood glucose screening at 3 year intervals starting at age 45 for persons in high risk groups

Diabetes Mellitus Common Nursing Diagnoses and Specific Teaching Interventions A. Risk for impaired skin integrity: Proper foot care • 1. Daily inspection of feet • 2. Checking temperature of any water before washing feet • 3. Need for lubricating cream after drying but not between toes • 4. Patients should be followed by a podiatrist • 5. Early reporting of any wounds or blisters B. Risk for infection • 1. Frequent hand washing • 2. Early recognition of signs of infection and seeking treatment • 3. Meticulous skin care • 4. Regular dental examinations and consistent oral hygiene care

Diabetes Mellitus C. Risk for injury: Prevention of accidents, falls and burns D. Sexual dysfunction • 1. Effects of high blood sugar on sexual functioning, • 2. Resources for treatment of impotence, sexual dysfunction E. Ineffective coping • 1. Assisting clients with problem-solving strategies for specific concerns

Diabetes Mellitus • 2. Providing information about diabetic resources, community education programs, and support groups • 3. Utilizing any client contact as opportunity to review coping status and reinforce proper diabetes management and complication prevention
- Slides: 71