Diabetes Manageent Unit 6 Chapter 59 P 580

Diabetes Manageent Unit 6 Chapter 59 P. 580


Key Points �DM is a group of metabolic diseases characterized by chronic hyperglycemia due to problems with insulin secretion and/or the effectiveness of endogenous insulin ( insulin resistance). �related to: �An endocrine disorder causes Abnormal insulin production �Impaired insulin utilization �Both abnormal production and impaired utilization �Diabetes mellitus is a contributing factor to: *cardiovascular disease, *HTN * RF, *blindness, and *CVA

Key Points �Hallmark symptoms associated with diabetes mellitus are the 3 P’s �Consistent management of blood glucose levels within the normal range (? ? ? ) is the goal of Rx �Type 1 DM is: an autoimmune disorder characterized by beta cell destruction. �It occurs in genetically susceptible individuals , and typical onset is before the age of 30. �Type 2 DM is due to resistance to endogenous insulin and frequently occurs in individuals with a family disposition who are obese and over the age of 40.
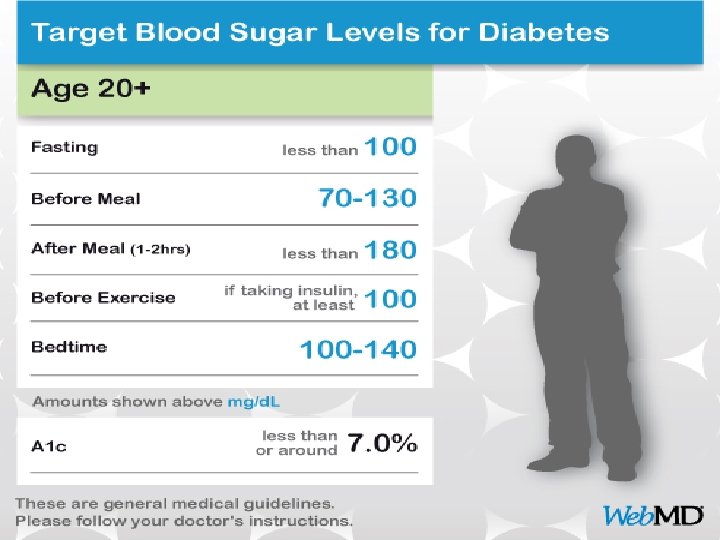

�Normal and diabetic blood sugar ranges �For the majority of healthy individuals, normal blood sugar levels are as follows: �Between 4. 0 to 6. 0 mmol/L (72 to 108 mg/d. L) when fasting �Up to 7. 8 mmol/L (140 mg/d. L) 2 hours after eating �For people with diabetes, blood sugar level targets are as follows: �Before meals: 4 to 7 mmol/L for people with type 1 or type 2 diabetes �After meals: under 9 mmol/L for people with type 1 diabetes and under 8. 5 mmol/L for people with type 2 diabetes

Key Points �Risk factors for the developing insulin resistance: � Obesity, �physical inactivity, �high triglycerides (> 250 mg/d. L), and � hypertension. �Pancreatitis and hyperthyroidism may lead to hyperglycemia �Parenteral nutrition and glucocorticoids may lead to transient iatrogenic hyperglycemia

Diagnostic Procedures and Nursing Interventions �Two findings (separate days) of one of the following are required: required �Symptoms of diabetes plus casual plasma glucose concentration 200 mg/d. L (without regard to time since last meal). �FBS 126 mg/d. L (8 hr fasting). �Two-hour glucose 200 mg/d. L with an OGTT (10 to 12 hr fasting).

Diagnostic Procedures and Nursing Interventions �Fasting blood glucose (FBS): �Client fasts (no food or drink other than water) for the 8 hr prior to the blood draw. � Antidiabetic medications should be postponed until after the level is drawn. �Oral glucose tolerance test �Client consumes a balanced diet for the 3 days prior to the test. �Then the client fasts for the 10 to 12 hr prior to the test. �A fasting blood glucose level is drawn at start of the test. � The client then consumes a specified amount of glucose. �BGL are drawn every 30 min for 2 hr. �Clients must be assessed for hypoglycemia throughout the procedure.

Diagnostic Procedures and Nursing Interventions �Glycosylated hemoglobin (Hb. A 1 c) �The target is 4 to 6%. Hb. A 1 c is the best indicator of average blood glucose level for past 120 days. �Assists in evaluating treatment effectiveness and compliance. �Pre-meal glucose �The target is 90 to 130 mg/d. L. �Ensure that the client follows the proper procedure �Supplemental short-acting insulin may be prescribed for elevated pre-meal glucose levels.

Assessment Signs and Symptoms by Type of Diabetes Type 1 Type 2 Polyuria, polydipsia, polyphagia Weight loss Obesity Fatigue Increased frequency of infections Rapid onset Gradual onset Controlled by exogenous insulin Controlled by oral antidiabetic medications and insulin



Signs and Symptoms by Glucose Alteration Hypoglycemia (≤ 50 mg/d. L) Hyperglycemia (> 250 mg/d. L) Cool, clammy skin Hot, dry skin Diaphoresis Absence of diaphoresis Anxiety, irritability, confusion, blurred vision Alert to coma (varies) Hunger Nausea and vomiting, abdominal pain (with ketoacidosis) General weakness, seizures (severe hypoglycemia) Rapid deep respirations (acetone/fruity odor due to ketones)

Additional appropriate assessments �Blood glucose levels and factors affecting levels �Intake and output, weight. �Skin integrity and healing status of any wounds. �Sensory alterations (tingling, numbness). �Condition of feet and foot care practices. �Dietary practices. �Exercise patterns. �Client’s self monitoring blood glucose skill proficiency. �Client’s self medication administration proficiency. �Pain levels.

NANDA Nursing Diagnoses �Risk for injury �Imbalanced nutrition: More than body requirements �Risk for impaired skin integrity �Deficient knowledge �Self-care deficit



Nursing Interventions �Comprehensive education in diabetes management. �Provide information regarding the importance of foot care and provide �Instructions for foot care, including: �Inspect feet daily. � Wash feet daily with mild soap and warm water. �Pat feet dry gently, especially between the toes. �Use mild foot powder (powder with cornstarch) on sweaty feet. �Do not use commercial remedies to remove calluses or corns.

Nursing Interventions �Cut toenails even with rounded contour of toes. �The best time to cut nails is after a bath/shower. �Separate overlapping toes with cotton or wool. �Avoid open-toe, open-heel shoes. Leather shoes are preferred to plastic ones. �Wear slippers with soles. Do not go barefoot. Shake out shoes before putting them on. �Wear clean, absorbent socks. �Do not use hot water bottles or heating pads to warm feet. Wear socks for warmth. �Avoid prolonged sitting, standing, and crossing of legs.

Nursing Interventions � Encourage the client to take measures to reduce risk of injury (wearing shoes, adequate lighting). Cleanse cuts with warm water and mild soap, gently dry and apply a dry dressing. � Instruct clients to monitor healing and to seek intervention promptly. � Refer clients to dieticians for nutritional management of diabetes. � Some guidelines to encourage are: � Count grams of carbohydrates consumed to calculate dose (1 unit/15 g of carbohydrate). � Restrict calories and increase physical activity as appropriate to facilitate weight loss for clients who are obese or to prevent obesity. � Include fiber in the diet to increase carbohydrate metabolism and to help control cholesterol levels. � Use artificial sweeteners.

Nursing Interventions �Teach the client guidelines to follow when sick: �Monitor blood glucose every 4 hr. �Continue to take insulin or oral antidiabetic agents. �Consume 8 oz of sugar-free non-caffeinated liquid every hour to prevent dehydration. �Meet carbohydrate needs through solid food if not consume liquids �Test urine for ketones and report if abnormal (should be negative to small). �Rest.

Nursing Interventions �Call the primary care provider if: �Blood glucose is higher than 250 mg/d. L. �Ketones are moderate or large. �Fever higher than 38. 9° C, fever that does not respond to or lasts more than 12 hr. �Feeling dizzy or confused. �Experiencing Tachypnea. �Vomited more than once. �Diarrhea occurs more than five times or for longer than 24 hr. �Illness lasts longer than 2 days.

Nursing Interventions �Teach the client , in response to hypoglycemia symptoms, to: �Check blood glucose level. �Treat with 15 g carbohydrates. �Recheck blood glucose in 15 min. �If still low, give 15 g more of carbohydrates. �Recheck blood glucose in 15 min. �If blood glucose is within normal limits, take 7 g protein (if the next meal is more than an hour away). � 15 g of carbohydrates examples: 120 ml orange juice, 60 ml grape juice, 240 milk, � 7 g protein: 30 gm of cheese (1 string cheese). �Fluid is more readily absorbed (juice, non-diet soft drink, skim milk).

Nursing Interventions �Teach the client , in response to hyperglycemia, to: �Encourage oral fluid intake. �Administer insulin as prescribed. �Restrict exercise when blood glucose levels are > 250 mg/d. L. �Test urine for ketones and report if abnormal. �Consult the primary care provider if symptoms progress. �Know the onset, peak, and duration of administered insulin, plan for administration of prescribed insulin, and monitor client for signs of hypoglycemia

Nursing Interventions � Provide information regarding self administration of insulin, following guidelines including: � Rotation of injection sites (prevent lipohypertrophy) � Inject at a 90° angle (45° if thin). Aspiration for blood is not necessary. � When mixing regular with NPH insulin, draw up regular insulin first and then the NPH. � Observe the client perform self-administration and offer additional instruction as indicated. � Provide information regarding oral antidiabetic medications: � Administer as prescribed (30 min before first main meal). � Monitor renal function. � Monitor liver function � Advise women of childbearing age taking thiazolidinedione that additional contraception methods may be needed since these drugs reduce the blood levels of some oral contraceptives.


DKA �Diabetic ketoacidosis (DKA) is an acute, life-threatening condition characterized by hyperglycemia (> 300 mg/d. L) resulting in breakdown of body fat for energy and an accumulation of ketones in the blood and urine. �The onset is rapid, and the mortality rate of DKA is 1 to 10%. �Hyperglycemic-hyperosmolar nonketotic syndrome (HHNS) is an acute, lifethreatening condition characterized by profound hyperglycemia (> 600 mg/d. L), dehydration, and an absence of ketosis. The onset is generally over several days, and the mortality rate of HHNS is up to 15% or more. �Priority interventions for both conditions include the administration of fluids and insulin.

Key Factors �Both conditions result in severe hyperglycemia from: �A lack of sufficient insulin (new onset, lack of compliance with Rx). �An increased need for insulin (stress, illness, infection, surgery, trauma). �DKA is more common in individuals with type 1 diabetes mellitus. �HHNS is more common in older adult clients untreated or undiagnosed type 2 diabetes mellitus.

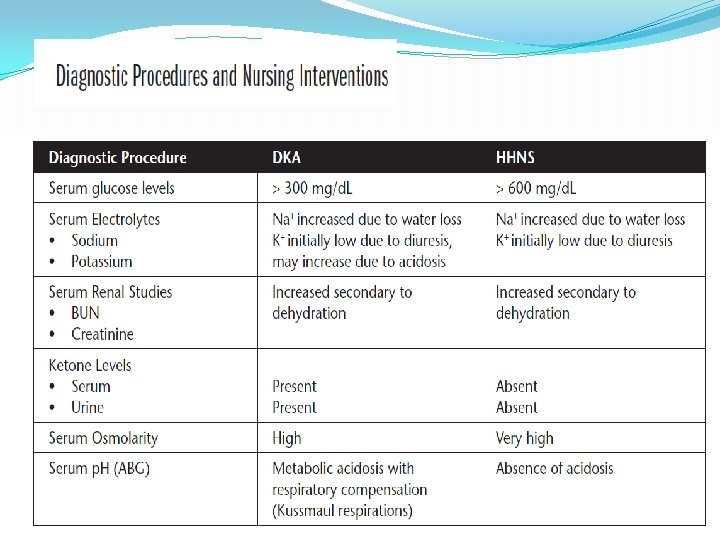

Assessment �Monitor for signs and symptoms. �Polyuria, polydipsia, polyphagia (early signs) �Change in mental status �Signs of dehydration (dry mucous membranes, weight loss, sunken eyeballs resulting from fluid loss such as polyuria) �Kussmaul respiration pattern, rapid and deep respirations, “fruity” breath (DKA/metabolic acidosis) �Nausea, vomiting, and/or abdominal pain (DKA/metabolic acidosis) �Generalized seizures and reversible paralysis (HHNS)

NANDA Nursing Diagnoses �Deficient fluid volume �Deficient knowledge


Nursing Interventions �Always treat the underlying cause �Priority is isotonic fluid replacement. Often large quantities are required to replace losses. Monitor the client for evidence of fluid volume excess. �Administer IV regular insulin to affect a 75 to 150 mg/d. L/hr decrease in serum glucose level. Monitor glucose levels hourly. �When serum glucose levels approach 250 mg/d. L, add glucose to IV fluids to minimize the risk of cerebral edema associated with drastic changes in serum osmolality.

Nursing Interventions �Monitor serum K+. With insulin therapy, K+ will shift into cells and the client will need to be monitored for hypokalemia. Provide potassium replacement therapy as indicated. Make sure urinary output is adequate �Administer sodium bicarbonate by slow IV infusion for severe acidosis (p. H < 7. 0). �Monitor K+ (quick a correction of acidosis can lead to hypokalemia).

Nursing Interventions �Provide client education to prevent reoccurrence: � Take measures to decrease the risk of dehydration. � Monitor glucose every 4 hr when ill and continue to take insulin. �Consume liquids with carbohydrates and electrolytes (for example, sports drinks) when unable to eat solid food. �Notify the primary care provider if illness lasts more than a day.

Complications and Nursing Implications �Rapid onset of hypoglycemia due to an excessively rapid decrease in blood glucose (too much insulin too fast) can lead to: �Electrolyte shifts (for example, hypokalemia). �Cerebral edema (signs include seizures and change in level of consciousness). �Fluid volume excess (signs include crackles, dyspnea, and weight gain). �Renal Failure �Signs include hourly output < 30 m. L/hr. �Monitor hydration and renal function (intake and output, creatinine levels). �Thromboembolism (secondary to dehydration)

- Slides: 39