DISEASES OF THE URINARY SYSTEM Cystitis Cystic calculi











































- Slides: 63

DISEASES OF THE URINARY SYSTEM Cystitis Cystic calculi Urinary obstruction ARF & CRF Incontinence

Urinary system is made up of: Kidneys (2) Ureters (2) Bladder (1) Urethra (1) Main job of the urinary system: Waste removal Red blood cell production Regulation of water and electrolyte balance Controls blood pressure

THE URINARY SYSTEM and ITS FUNCTIONS Functions of the kidneys Excretion: produce urine Maintain homeostasis: Blood filtration, reabsorption, secretion Fluid balance regulation Acid-base balance regulation Hormone production

DISEASES OF THE URINARY SYSTEM IS NORMALLY STERILE AND RESISTANT TO BACTERIAL INFECTION B/C OF: Voiding of urine Urethral/ureteral peristalsis Glycosaminoglycans in the surface mucosal layer p. H (6. 0 – 6. 3): water and blood neutral

URINARY SYSTEM DISORDERS About 4 million cats a year are destroyed or abandoned for “elimination problems”.

Feline Idiopathic (Interstitial) Cystitis aka FUS/ FLUTD FACTS: Occurs in cats almost any age Occurrence in males > females cause unknown, multi-factorial, virus(? ) not caused by bacterial infection recurrence is likely

Feline Idiopathic (Interstitial) Cystitis Clinical Signs pollakiuria Hematuria Dysuria Periuria (sinks, tubs, carpet, etc. )

Feline Idiopathic (Interstitial) Cystitis Diagnostics Urinalysis/culture to rule out bacteria as cause Only 1%-3% of all feline cystitis is caused by bacteria Radiographs to rule out bladder stones

Feline Idiopathic (Interstitial) Cystitis Treatment Avoid unnecessary antibiotics Change diet from dry to moist or add water to dry food Reduce stress from other cats, kids, etc Provide hiding places Pheromone therapy Behavior modification drugs (may also have pain reducing effects) Amitryptilline (tri-cyclic antidepressant) Clomipramine Glycosaminoglycan replacement Cosequin for cats Adequan

FELIWAY

Feline Idiopathic (Interstitial) Cystitis Client info Disease is self-limiting As many as 85% of cats will have resolution of clinical signs in 7 -10 days May be recurring problem No definitive cure, but diet change is the most effective (Hill’s c/d Stress) Reduce stress

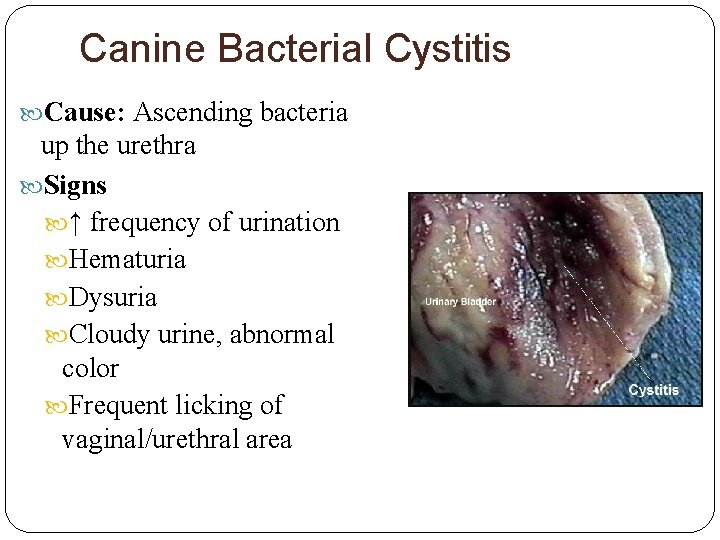
Canine Bacterial Cystitis Cause: Ascending bacteria up the urethra Signs ↑ frequency of urination Hematuria Dysuria Cloudy urine, abnormal color Frequent licking of vaginal/urethral area

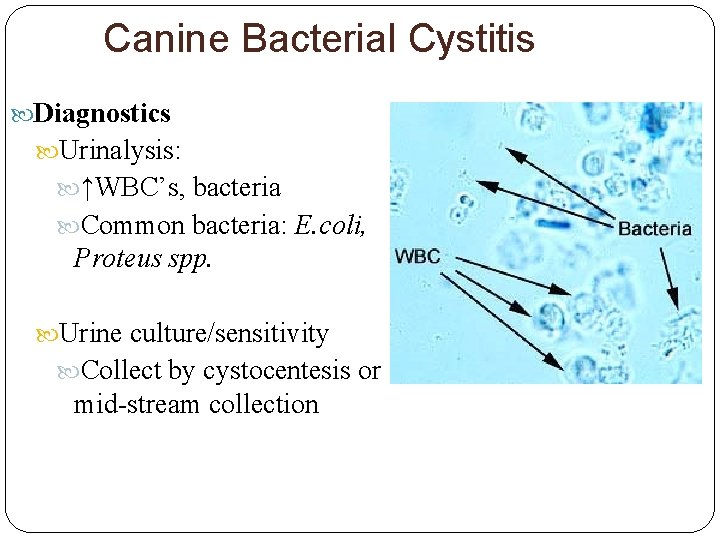
Canine Bacterial Cystitis Diagnostics Urinalysis: ↑WBC’s, bacteria Common bacteria: E. coli, Proteus spp. Urine culture/sensitivity Collect by cystocentesis or mid-stream collection

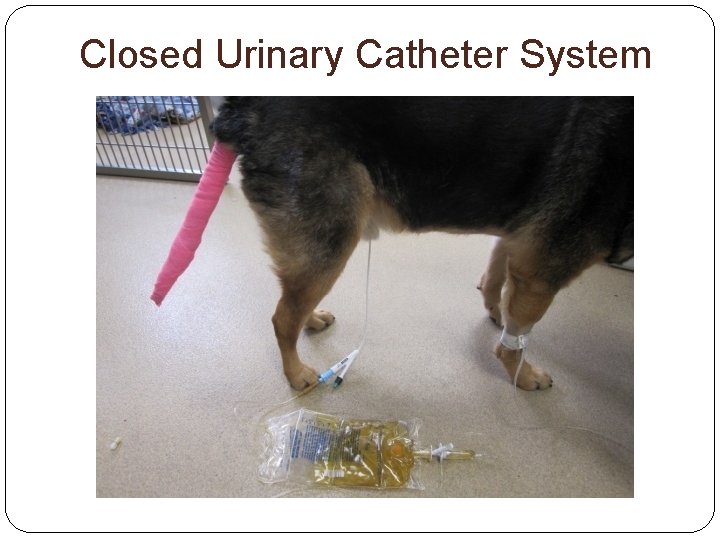
Canine Bacterial Cystitis Treatment Antibiotics according to culture/sensitivity results Treat acute infections x 10 -14 d Chronic infections x 4 -6 w Avoid trauma to urinary tract during surgery Patients needing indwelling catheters should have a closed system

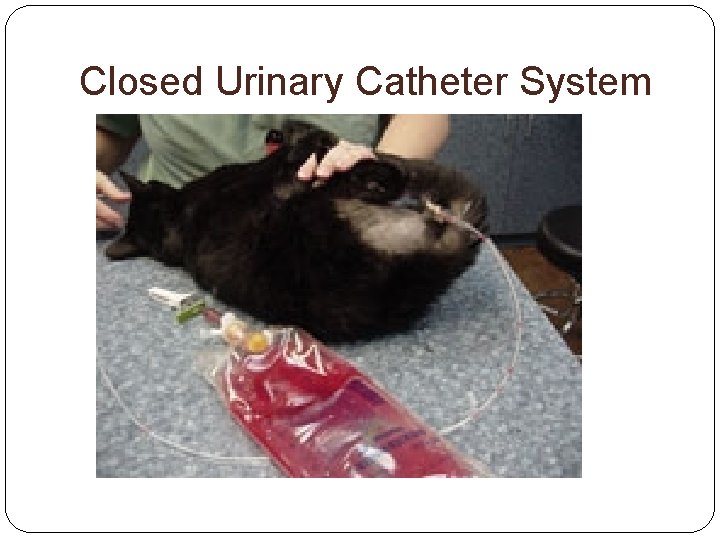
Closed Urinary Catheter System

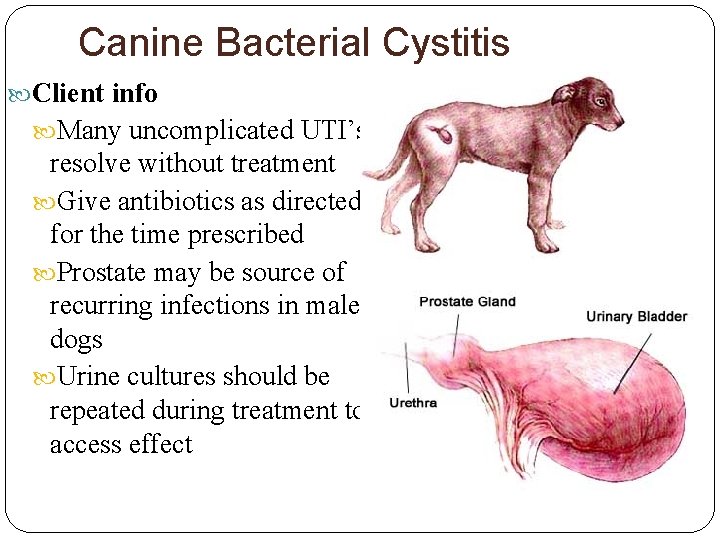
Canine Bacterial Cystitis Client info Many uncomplicated UTI’s resolve without treatment Give antibiotics as directed for the time prescribed Prostate may be source of recurring infections in male dogs Urine cultures should be repeated during treatment to access effect

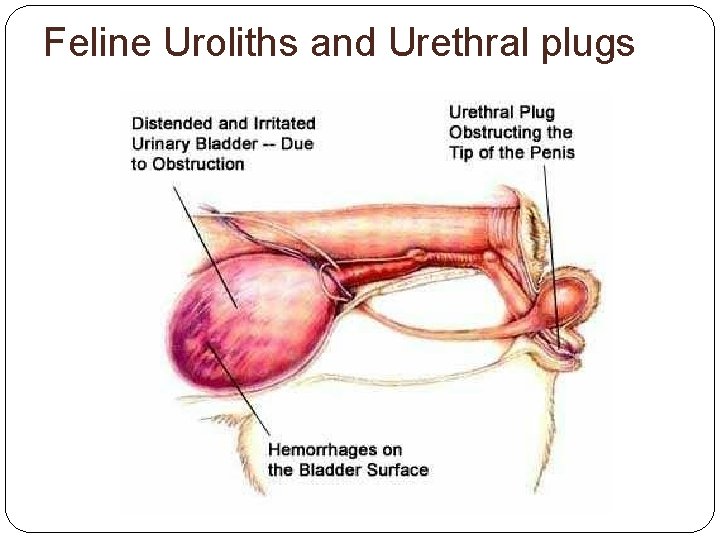
Feline Uroliths and Urethral Plugs “Plugged” or “Blocked” male cats are commonly seen in small animal practice and can be fatal if not relieved

Feline Uroliths & Urethral Plugs The two most common causes of urethral blockage are uroliths and urethral plugs UROLITHS: composed predominantly of minerals URETHRAL PLUGS: composed predominantly of matrix (mucoprotein, rbcs, wbcs, epithelial cells, etc. )

Feline Uroliths and Urethral Plugs Signs Hematuria Dysuria Periuria Anorexia, vomiting Collapse, death Non-specific signs: Hiding Crying while urinating Frequent trips to the litterbox

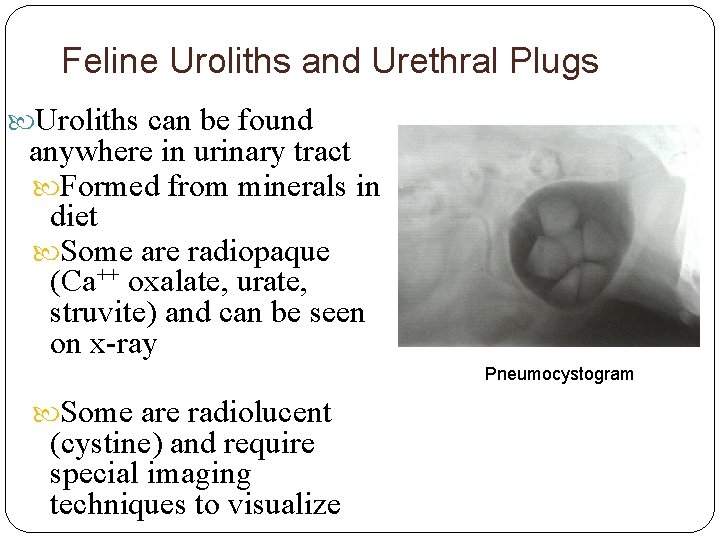
Feline Uroliths and Urethral Plugs Uroliths can be found anywhere in urinary tract Formed from minerals in diet Some are radiopaque (Ca++ oxalate, urate, struvite) and can be seen on x-ray Pneumocystogram Some are radiolucent (cystine) and require special imaging techniques to visualize

Feline Uroliths and Urethral Plugs Uroliths damage bladder, making it more susceptible to bacterial infection, hematuria Uroliths can cause blockage of the urethra of males Bladder will fill with urine Kidneys will stop working Patient will become azotemic

Feline Uroliths and Urethral plugs

Feline Uroliths and Urethral Plugs • Diagnosis Palpation of bladder • Obstructed bladders are full and tight Radiographs may show uroliths Ultrasonography Urolith analysis is necessary to determine its constituents EKG: atrial standstill, bradycardia, due to hyperkalemia

Feline Uroliths and Urethral Plugs Treatment Medical treatment (non-obstructed) Dissolve struvite uroliths by acidifying urine and feeding diet low in Mg (Hill’s S/D, c/d) Should resolve in 4 -8 wk Re-radiograph, and continue diet 1 mo after uroliths gone Cystotomy to remove stones Antibiotics according to culture/sensitivity

Feline Uroliths and Urethral Plugs

Feline Uroliths and Urethral Plugs Medical treatment (obstructed) This is a medical emergency Anesthetize *USE LESS ANESTHESIA IN AZOTEMIC CATS* Pass Tom catheter and back flush Sew catheter in place for 1 -3 d, using a closed system

Feline Uroliths and Urethral Plugs

Closed Urinary Catheter System

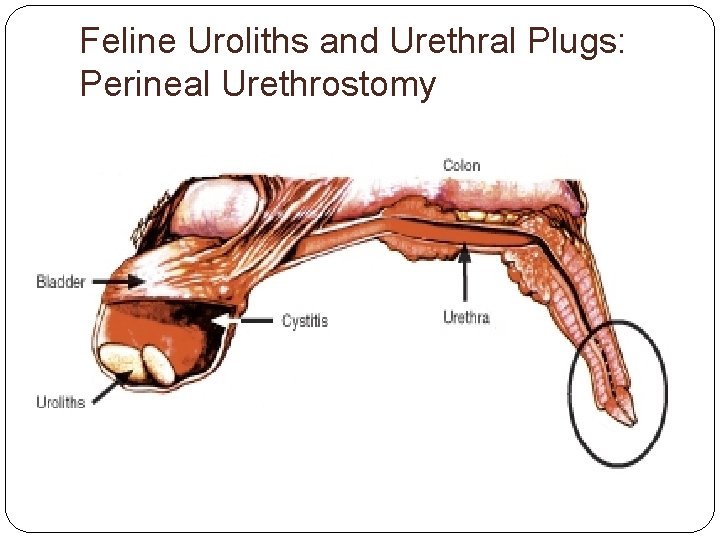
Feline Uroliths and Urethral Plugs Surgical treatment (chronic obstructors) Perineal urethrostomy (PU) New opening for urethra is created proximal to narrowing Urethral opening looks similar to female anatomy *Goal of surgery is to decrease the likelihood of life-threatening obstruction*

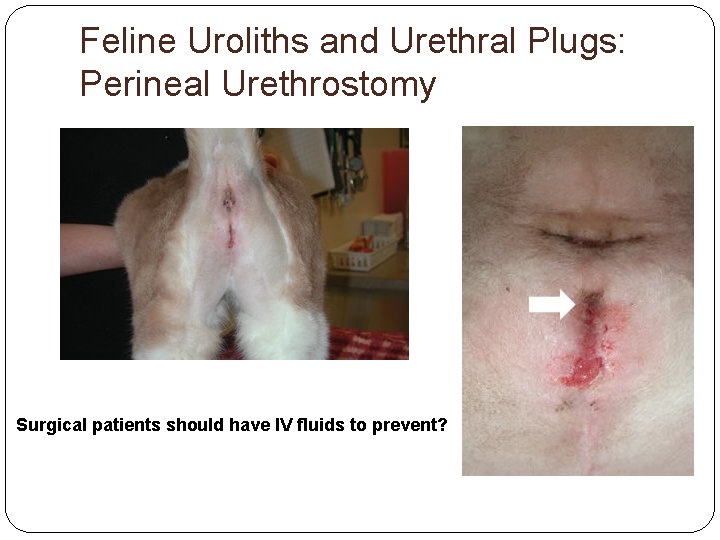
Feline Uroliths and Urethral Plugs: Perineal Urethrostomy

Feline Uroliths and Urethral Plugs: Perineal Urethrostomy Surgical patients should have IV fluids to prevent?

https: //youtu. be/2 Kcu. W -trv. PI Feline Perineal Urethrostomy

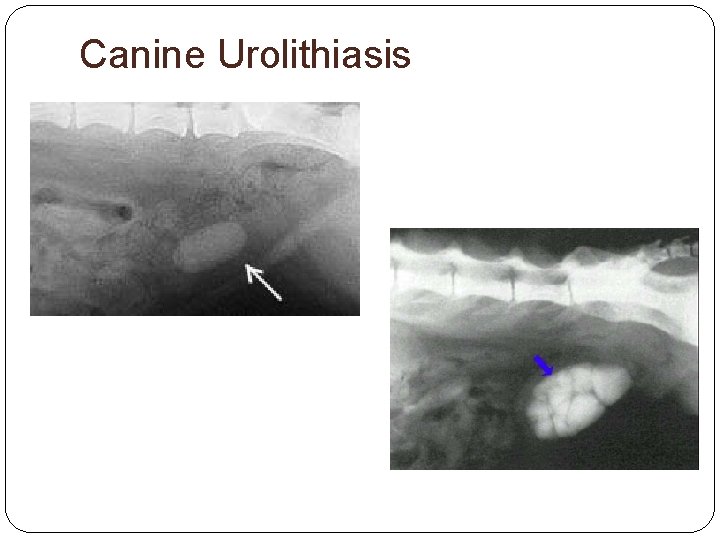
CANINE UROLITHIASIS

Canine Urolithiasis Uroliths damage mucosa of urinary tract making it susceptible to infection Uroliths can obstruct urine flow in males Struvite: more common in females 3 -8 years Calcium oxalate: more common in males 5 - 12 years Urates: common in Dalmatians Most common uroliths in dogs?

Canine Urolithiasis The distal portion of the canine urethra is contained in the narrow canal of the os penis. This can be a common location for urethral stones to become lodged.

Canine Urolithiasis Clinical Signs pollakiuria Dysuria Hematuria Dx Urinalysis Crystalluria Hematuria ↑ bacteria Radiographs

Canine Urolithiasis

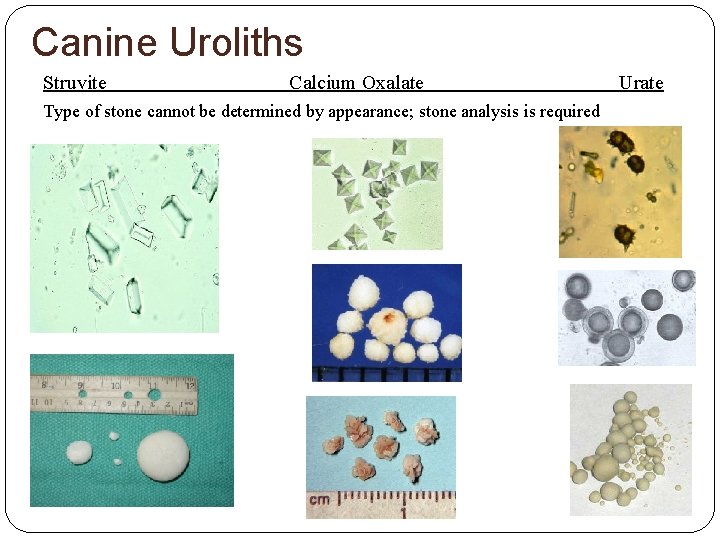
Canine Uroliths Struvite Calcium Oxalate Type of stone cannot be determined by appearance; stone analysis is required Urate

Urolithiasis (Canine) • Treatment Medical management - dissolve stones if Struvite • Prescription diets • Acidify urine – Urinary acidifiers ( Methogel (methionine)) • ↑ urine output – increase water intake Antibiotics for bacterial infection Surgical removal ( Ca Oxalate) • Some uroliths are not amenable to Medical Rx • Prevention is key • STONE ANALYSIS IS VITAL FOR APPROPRIATE TREATMENT

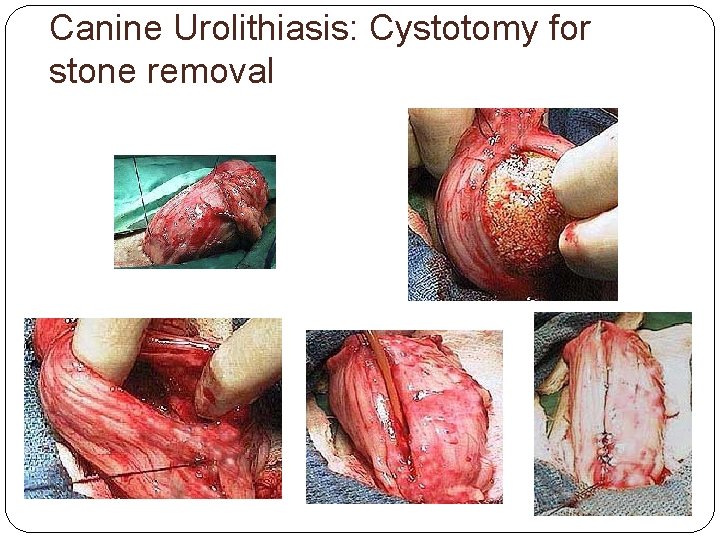
Canine Urolithiasis: Cystotomy for stone removal

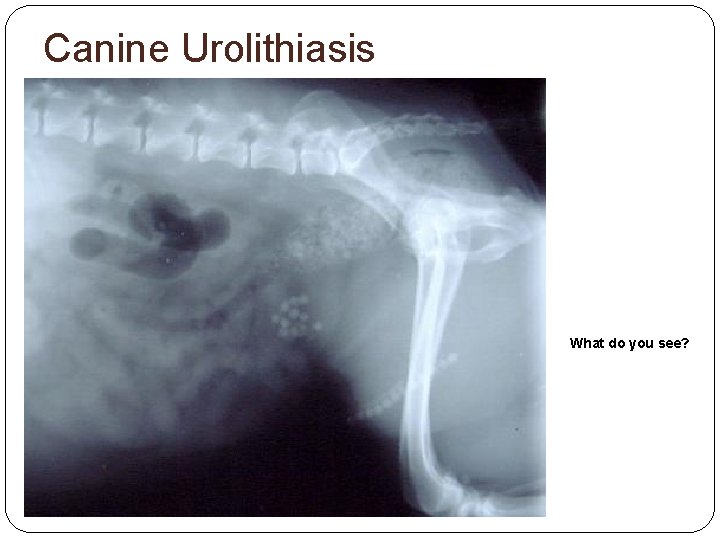
Canine Urolithiasis What do you see?

Canine Urolithiasis Client info Special diet may be required for life Table scraps/treats should be limited Long-term antibiotics may be required Uroliths may recur at any time Always provide plenty of fresh water Allow plenty of bathroom time and frequency

EDUCATION “It is possible to store the mind with a million facts and still be entirely uneducated. ” - Alec Bourne

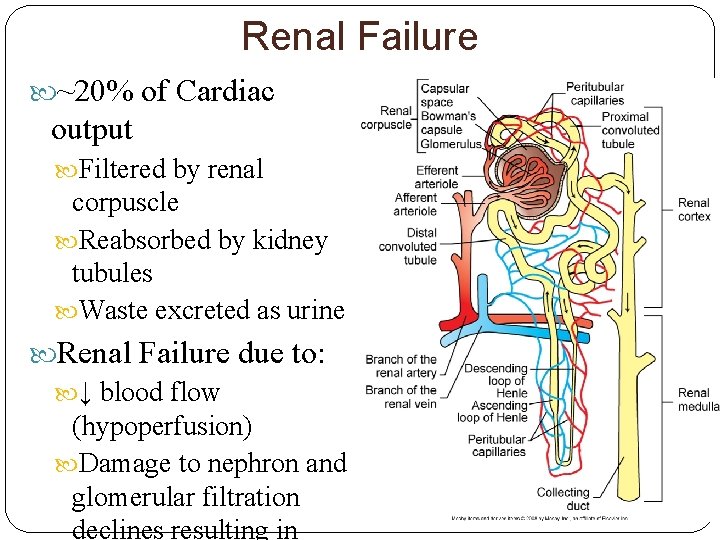
Renal Failure ~20% of Cardiac output Filtered by renal corpuscle Reabsorbed by kidney tubules Waste excreted as urine Renal Failure due to: ↓ blood flow (hypoperfusion) Damage to nephron and glomerular filtration declines resulting in

AZOTEMIA Pre-renal dehydration Renal Primary kidney disorders Post-renal Urinary tract obstruction

Acute Renal Failure Three distinct phases: Induction: the time from the initial insult until decreased renal function is apparent (hours to days) Maintenance: the time period during which renal tubular damage occurs (weeks to months) Recovery: the time during which renal function improves, existing nephrons hypertrophy and compensate for those damaged, and tubular repair occurs (when possible)

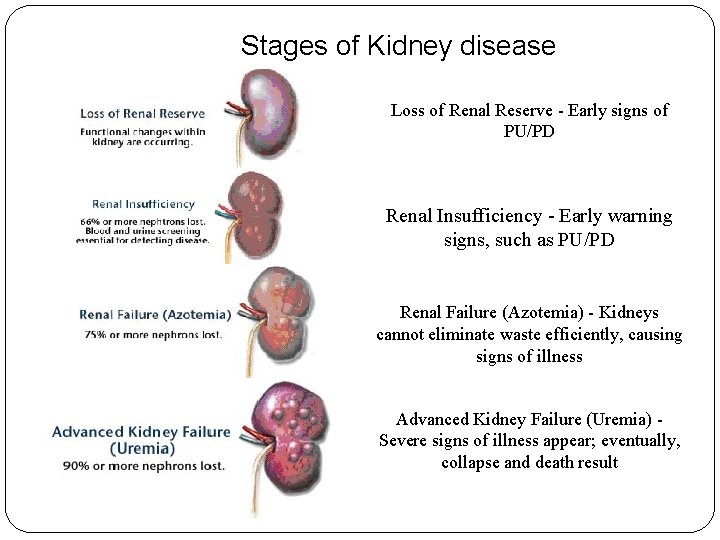
Stages of Kidney disease Loss of Renal Reserve - Early signs of PU/PD Renal Insufficiency - Early warning signs, such as PU/PD Renal Failure (Azotemia) - Kidneys cannot eliminate waste efficiently, causing signs of illness Advanced Kidney Failure (Uremia) Severe signs of illness appear; eventually, collapse and death result

Acute Renal Failure An abrupt decrease in glomerular filtration →azotemia Causes Damage to nephron Nephrotoxic drugs Aminoglycosides (gentamicin, streptomycin) Chemotherapeutic agents Antifungal medications Analgesics (acetaminophen) Anesthetics (methoxyflurane [Metafane]) Ethylene glycol (antifreeze) Antibiotic (Amikacin)

Acute Renal Failure More causes: Infections (pyelonephritis) Immune-mediated diseases (Glomerulonephritis) ↓ Renal perfusion Shock Hypovolemia/dehydration Hypotension

Acute Renal Failure Signs (non-specific) Kidneys are enlarged and painful on palpation Signs of azotemia Anorexia, dehydrated Vomiting/diarrhea Weakness Fever

Acute Renal Failure Diagnosis Urinalysis urine sediment - casts low sp. gravity (unable to concentrate urine) CBC dehydration (↑PCV) Chem panel ↑ BUN, Creatinine

Acute Renal Failure Tx (aim is to restore renal hemodynamics) Relieve any urinary obstruction Discontinue any toxic drugs IV fluids Correct dehydration Correct acid/base imbalance

Acute Renal Failure Client info Renal function may never be like it was before injury Prognosis is guarded especially with older pets Care must be taken to avoid events that may precipitate further damage to kidney Appropriate diet Adequate water access

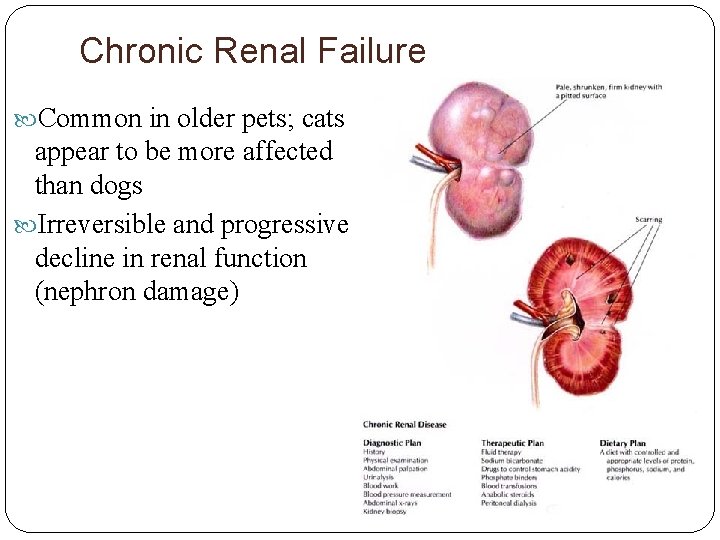
Chronic Renal Failure Common in older pets; cats appear to be more affected than dogs Irreversible and progressive decline in renal function (nephron damage)

Chronic Renal Failure Progressive 1 st function lost: Ability to concentrate urine PU, PD, nocturia Loss of ADH response Other functions lost: Ability to filter blood Azotemia Begins at ~75% of nephron loss ↑ BUN, Creatinine Anemia: erythropoietin secreted by kidneys

Chronic Renal Failure Signs Dull, lethargic, weak Anorexia, wt loss PU/PD, cervical ventroflexion hypokalemia

Chronic Renal Failure Diagnosis Look for abnormal blood work associated with kidney function Anemia ↑ BUN, Creatinine Proteinuria

Chronic Renal Failure Treatment Fluids for dehydration(IV, SQ) Correct electrolyte imbalances Hormones Epoetin

Chronic Renal Failure Client info CRF is progressive and irreversible treatment is aimed at slowing its progress SQ fluids at home are required to maintain hydration Quality of life will decrease; euthanasia may have to be considered

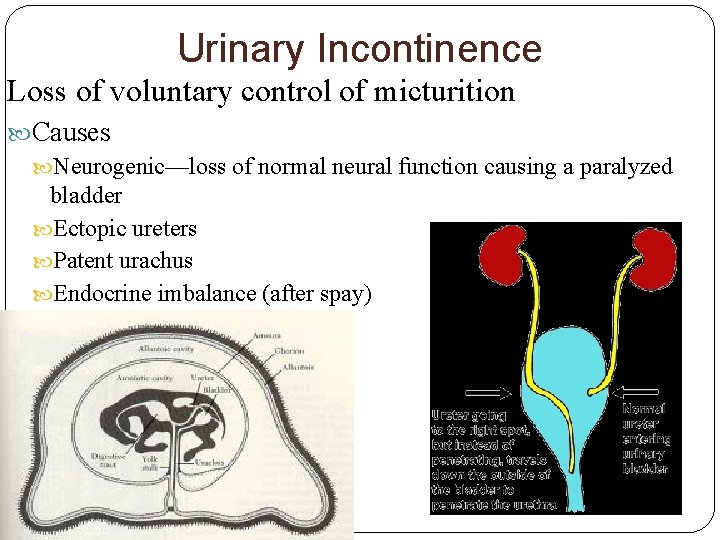
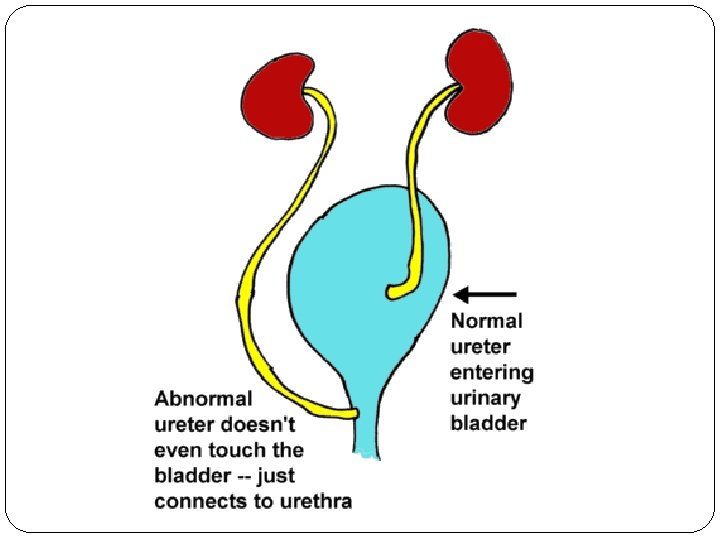
Urinary Incontinence Loss of voluntary control of micturition Causes Neurogenic—loss of normal neural function causing a paralyzed bladder Ectopic ureters Patent urachus Endocrine imbalance (after spay)


Urinary Incontinence Signs Urine leakage when pet is sleeping or exercising Perianal area of pet is always wet Concurrent urinary tract infection Dx Urinalysis X-rays/cystography Chem panel to r/o PU from endocrine disease

Urinary Incontinence Treatment (based on specific cause) Surgical correction Endocrine deficiency in spayed female Diethylstilbestrol Phenylpropanolamine (PROIN: for loss of sphincter tone) Client info Doses will have to be adjusted for individual animals Paralytic bladder incontinence may require manual expression or catheterization several times a day