Urinary Bladder Transitional Cell Carcinoma Megan Palmisano DVM

Urinary Bladder Transitional Cell Carcinoma Megan Palmisano, DVM University of Florida Class of 2020 Laura Javsicas, VMD, DACVIM/ Jim Nutt, VMD, DACVS Rhinebeck Equine L. L. P.

Signalment/History 20 year old Warmblood Mare • 3 month history of pollakiuria • Initially associated with estrus cycle but has persisted • Up to date on vaccinations • No history of neurologic disease

History • Worked up by r. DVM 3 weeks prior to referral for • • Bladder enlarged Aseptically drained bladder, large amount of debris present Urinary Analysis revealed no significant abnormalities Complete Blood Count and Serum Biochemistry were within normal limits Top differential at that time was Sabulous Cystitis Hematuria observed 1 week after urinary bladder drained, and a small 1 x 1 cm stone visualized in the stream The diet was transitioned from alfalfa and a high calcium ration balancer to timothy pellets and oats to decrease calcium carbonate build up within the urinary bladder.

Clinical Findings Presented for evaluation of possible sabulous cystitis • Physical Examination was within normal limits, no evidence of urine scald or urinary incontinence Diagnostic Plan: • • • Neurologic examination Abdominal Ultrasound Rectal palpation Transrectal Ultrasound Urinary catheterization Cystoscopy

Diagnostics • Neuro Examination • • Abdominal ultrasound • • No abnormalities noted Normal cortico-medullary distinction No free peritoneal fluid Urinary bladder not visualized Trans-rectal palpation • • • Normal sized follicles present on both ovaries Small urinary bladder palpable Bladder ballottement revealed a firm moderately sized soft tissue structure within the bladder lumen was palpable
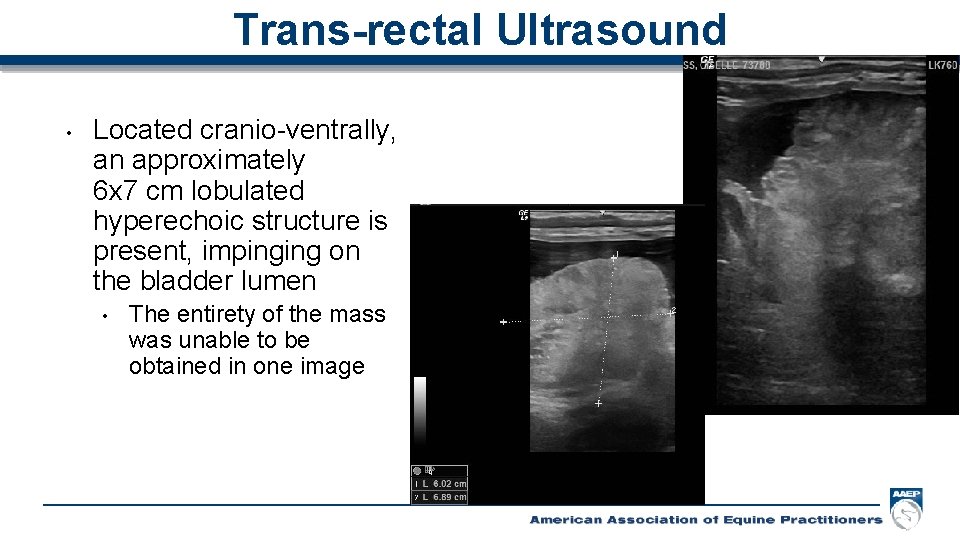
Trans-rectal Ultrasound • Located cranio-ventrally, an approximately 6 x 7 cm lobulated hyperechoic structure is present, impinging on the bladder lumen • The entirety of the mass was unable to be obtained in one image
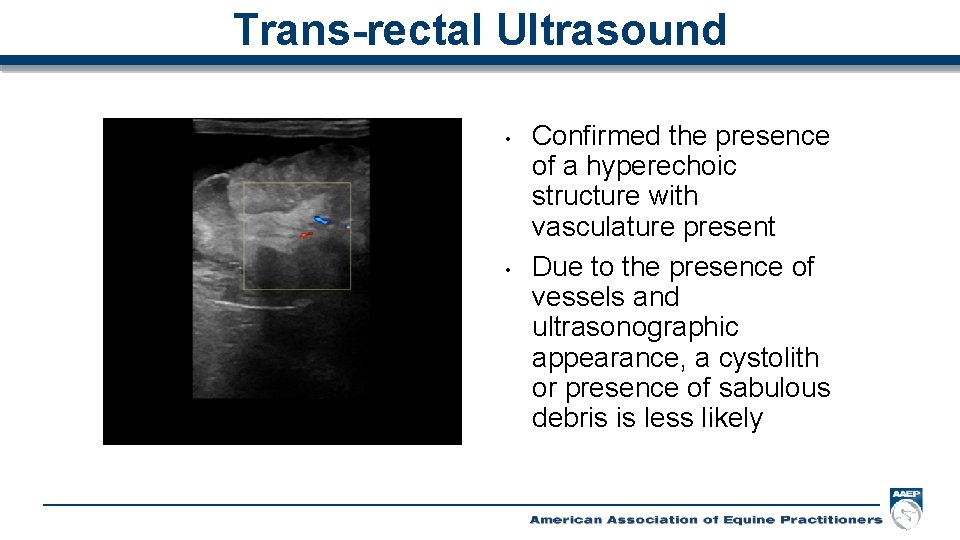
Trans-rectal Ultrasound • • Confirmed the presence of a hyperechoic structure with vasculature present Due to the presence of vessels and ultrasonographic appearance, a cystolith or presence of sabulous debris is less likely
Problem List Pollakiuria • • Neurologic Trauma Cystolith Neoplasia Hyperechoic/soft tissue structure within urinary bladder • • Neoplasia Hematoma Differential Diagnoses Primary Urinary Bladder Neoplasia • • Squamous Cell Carcinoma Transitional Cell Carcinoma Sabulous cystitis • • Less likely, ultrasound does not show sludge in the urinary bladder No evidence of urine scald Cystolith • Less likely, the structure within the bladder lumen is not of mineral opacity Neurologic disease • • No evidence of incontinence/urine scald Normal neurologic examination

Urinary Bladder Neoplasia Primary Urinary Bladder Neoplasia 1. Epithelial Origin, most commonly diagnosed • • Squamous Cell Carcinoma Transitional Cell Carcinoma • • Lymphosarcoma Rhabdomyosarcoma Leiomyosarcoma Fibromatous polyps 2. Non-epithelial origin Metastatic Neoplasia 1. Carcinoma 2. Lymphosarcoma 3. Hemangiosarcoma 4. Melanoma

Cystoscopy • • • Performed under standing sedation while restrained in the stocks Perineum aseptically prepared A urinary catheter was placed and the bladder drained • • A moderate amount of translucent, serosanguinous urine was voided The sample had both sludge and sloughed mucosa present in the sample An aseptic sample was obtained for urinary analysis and culture A cystoscopy was performed with a 1. 5 meter endoscope
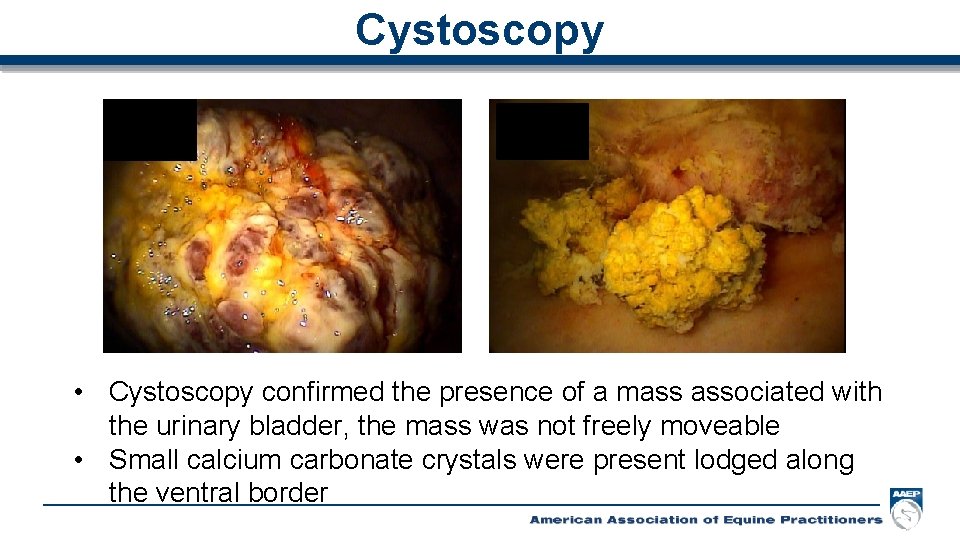
Cystoscopy • Cystoscopy confirmed the presence of a mass associated with the urinary bladder, the mass was not freely moveable • Small calcium carbonate crystals were present lodged along the ventral border
Diagnostic Plan Lidocaine was infused into the urinary bladder and biopsy forceps were inserted through the 1. 5 m endoscope • Multiple samples were obtained of the mass taken from various areas • A larger sample was obtained with uterine biopsy forceps passed adjacent to the 1. 5 m scope into the bladder • The samples were saved in 10% Buffered Formalin and submitted for histopathology • The mare was administered IV Gentamicin, Naxcel and Banamine after biopsy
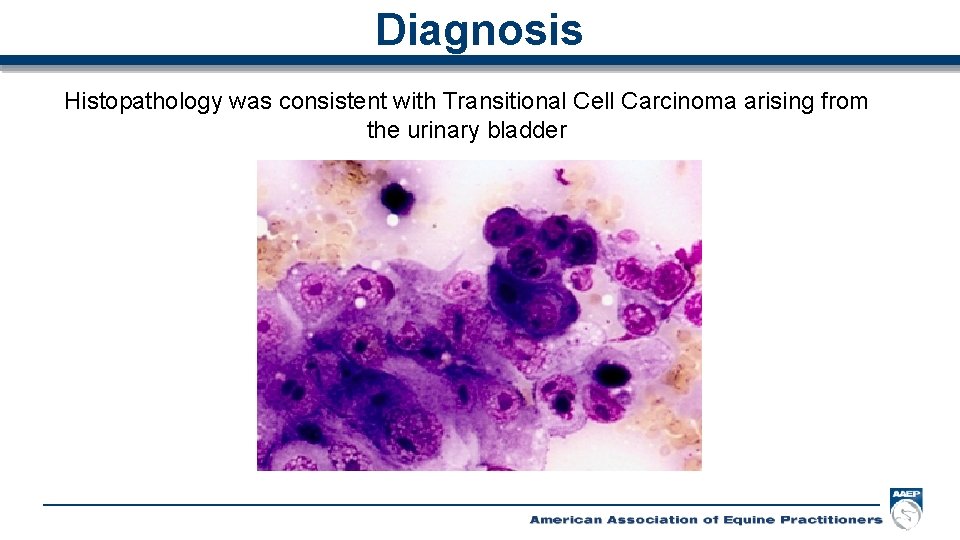
Diagnosis Histopathology was consistent with Transitional Cell Carcinoma arising from the urinary bladder

Therapeutic Plan Oncologists were consulted and a follow up appointment was scheduled for 10 days after discharge for further treatment • The most common urinary bladder neoplasm is squamous cell carcinoma • • Treatment is often palliative not curative Most recent case reports utilize Cisplatin as the chemotherapy agent of choice, in conjunction with removal/resection and Piroxicam therapy Treatment was elected, general anesthesia and aggressive resection were recommended • • Due to the owner’s concern for general anesthesia, standing surgical debulking was planned Chemotherapy with Cisplatin injected via scope Veterinary Oncology Consultants

Therapeutic Plan • Started on Piroxicam (100 mg PO SID) • • • NSAID, COX 2 specific, anti-inflammatory, angiogenesis antagonist and causes apoptosis of neoplastic cells Used frequently in cases of Squamous Cell Carcinoma in equids and urinary neoplasms in small animal as a neoplastic antagonist increasing median survival Piroxicam in conjunction with chemotherapy has been utilized in published case reports in horses with urinary bladder neoplasia.

Transitional Cell Carcinoma Debulking • Preoperative antibiotics and anti-inflammatory were administered • • • Performed under standing sedation while restrained in the stocks Caudal Epidural performed • • • Gentamicin (6. 6 mg/kg IV q 24 h) Naxcel (2. 2 mg/kg IV q 12 h) Banamine (1. 1 mg/kg IV q 12 h) 7. 5 mg Detomidine and 60 mg Carbocaine qs with saline to 8 m. L Tail tied and perineum washed, urinary catheterization performed Modified endotracheal tube passed through the urethra to facilitate easy access to the bladder Lidocaine was infused into the urinary bladder Procedure performed via endoscopic guidance using 1. 5 m endoscope
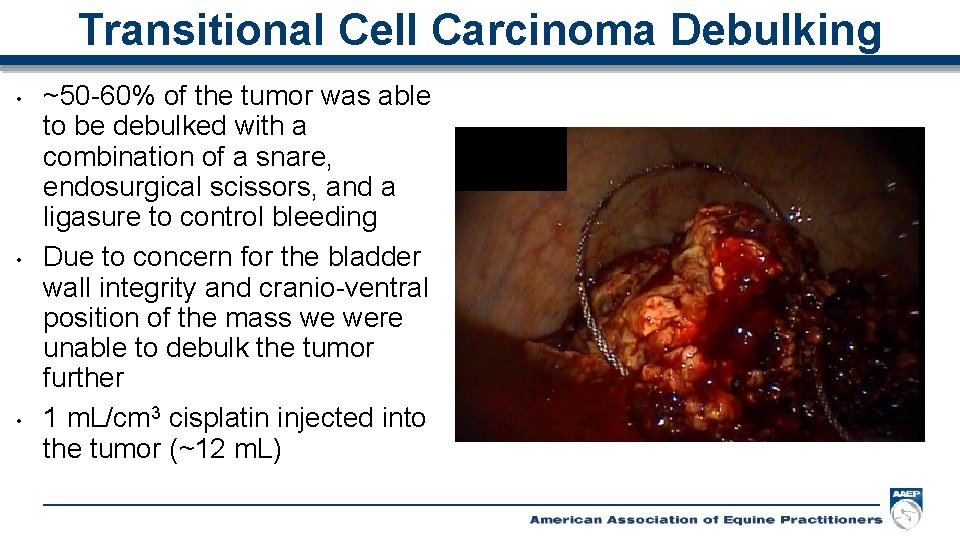
Transitional Cell Carcinoma Debulking • • • ~50 -60% of the tumor was able to be debulked with a combination of a snare, endosurgical scissors, and a ligasure to control bleeding Due to concern for the bladder wall integrity and cranio-ventral position of the mass we were unable to debulk the tumor further 1 m. L/cm 3 cisplatin injected into the tumor (~12 m. L)

Post Operative Treatment Post-operatively was continued on IV antibiotics (Naxcel and Gentamicin) and IV Banamine • Repeat cystoscopy after 24 hours revealed minimal bleeding and a 5060% reduction in the mass size Discharge instructions • Banamine (1000# dose PO BID for 3 days post op) • Naxcel (2. 2 mg/kg, IM SID for 3 days) • Phenazopyridine (2. 2 mg/kg, PO BID for 5 days) • Piroxicam (100 mg/day PO) started after Banamine is discontinued • Recommended recheck examination at 2 -3 weeks post-op
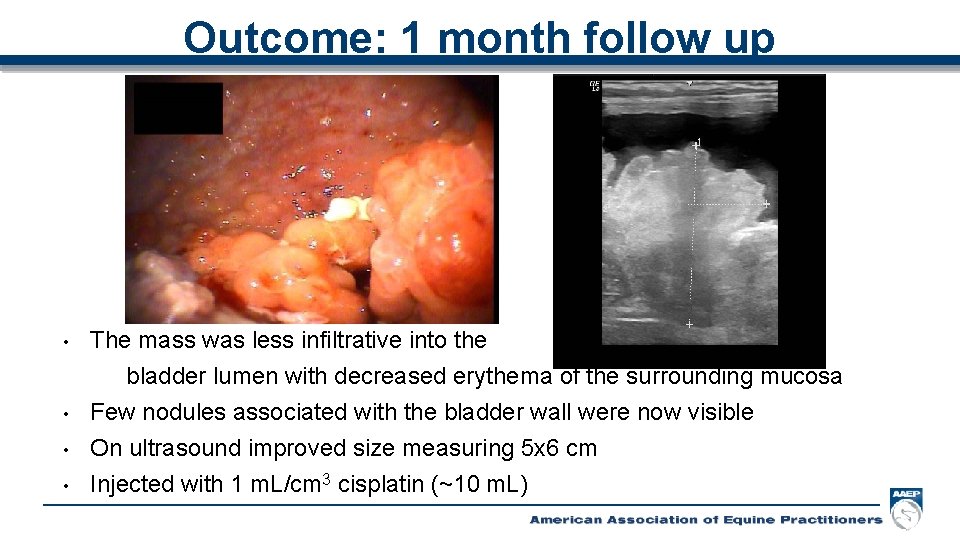
Outcome: 1 month follow up • • The mass was less infiltrative into the bladder lumen with decreased erythema of the surrounding mucosa Few nodules associated with the bladder wall were now visible On ultrasound improved size measuring 5 x 6 cm Injected with 1 m. L/cm 3 cisplatin (~10 m. L)
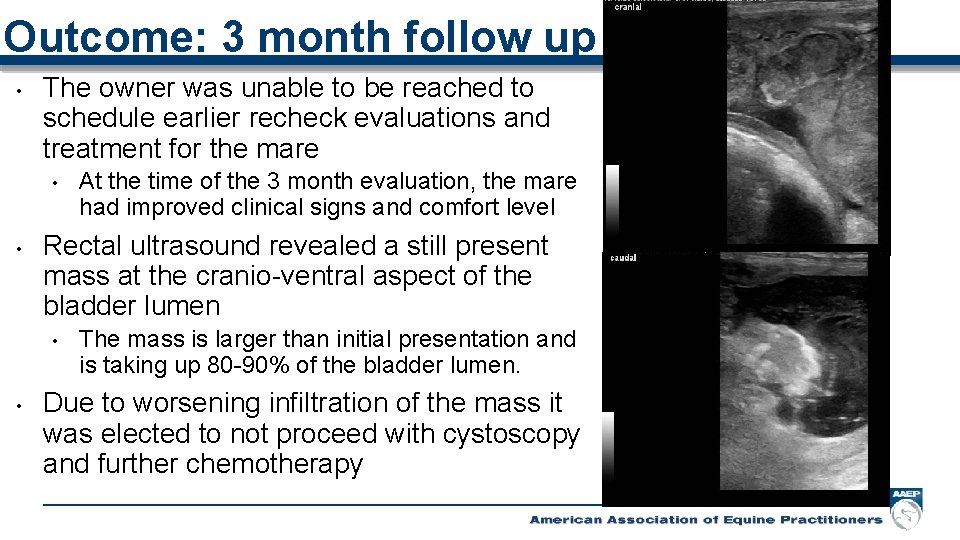
Outcome: 3 month follow up • The owner was unable to be reached to schedule earlier recheck evaluations and treatment for the mare • • Rectal ultrasound revealed a still present mass at the cranio-ventral aspect of the bladder lumen • • At the time of the 3 month evaluation, the mare had improved clinical signs and comfort level The mass is larger than initial presentation and is taking up 80 -90% of the bladder lumen. Due to worsening infiltration of the mass it was elected to not proceed with cystoscopy and further chemotherapy

Discussion • Urinary Bladder Neoplasia is uncommonly diagnosed • • Offer poor prognosis and often metastatic by the time of diagnosis Transmural metastasis, and metastasis via lymphatics can occur Horses often present for clinical signs secondary to the size of the mass Successful management involves a multimodal approach Often management is palliative not curative Anecdotally Piroxicam has been utilized in the management of equine transitional cell carcinoma and squamous cell carcinoma improving long term prognosis • Piroxicam is a non-steroidal anti-inflammatory used in human and canine transitional cell carcinoma treatment • Chemotherapy agents such as cisplatin and 5 -fluorouracil have been utilized with success to decrease both size and inflammation associated with the mass • • • Cisplatin treatment can be performed as often as every 2 -4 weeks

Discussion • • • Treatment can prolong median survival time, but varies greatly based on whether metastasis has occurred and the amount of tumor able to be removed Surgical resection under general anesthesia with one subsequent surgery revealed no recurrence of the mass within the bladder. Euthanasia elected secondary to metastasis <1 year later 5 Standing debulking performed using a perineal urethrostomy in a gelding prolonged median survival time, no clinical signs at 30 months post-op 2 • • After debulking/removal with persistent clinical signs subsequent urinalysis with culture should be performed • Secondary urinary tract infections are possible Cisplatin in conjunction with Piroxicam has been reported in each published case with varying success dependent on the severity of the neoplasia and evidence of metastasis on presentation

References/Additional Reading 1. Knottenbelt, Derek C. , et al. Clinical Equine Oncology. Elsevier, 2015. 2. Lisowski, Z. M. , et al. “Transitional Cell Carcinoma of the Urinary Bladder in a 12 Year-Old Belgian Warmblood Gelding. ” Equine Veterinary Education, vol. 27, no. 7, 2013, doi: 10. 1111/eve. 12021. 3. Patterson-Kane, J. C. , et al. “Transitional Cell Carcinoma of the Urinary Bladder in a Thoroughbred, with Intra-Abdominal Dissemination. ” Veterinary Pathology, vol. 37, no. 6, 2000, pp. 692– 695. , doi: 10. 1354/vp. 37 -6 -692. 4. Theon, Alain P, et al. “Intratumoral Administration of Cisplatin For Treatment of Sarcoids in 378 Horses. ” AAEP Proceedings, vol. 52, 2006, pp. 337– 339. 5. Zantingh, Alanna, et al. “Case Report: Squamous Cell Carcinoma of the Urinary Bladder in a Horse. ” Vet. Folio, Oct. 2012, www. vetfolio. com/learn/article/casereport-squamous-cell-carcinoma-of-the-urinary-bladder-in-a-horse.
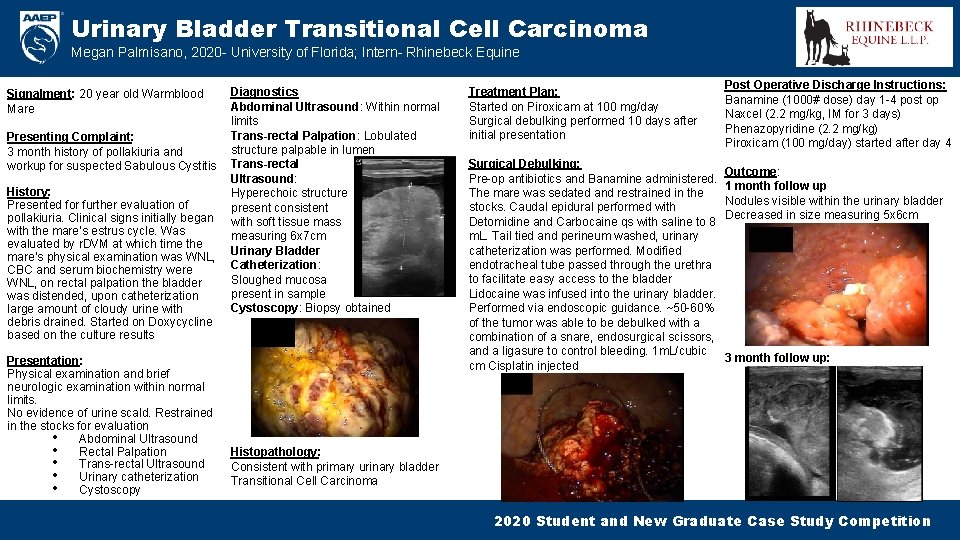
Urinary Bladder Transitional Cell Carcinoma Megan Palmisano, 2020 - University of Florida; Intern- Rhinebeck Equine Diagnostics Abdominal Ultrasound: Within normal limits Trans-rectal Palpation: Lobulated Presenting Complaint: structure palpable in lumen 3 month history of pollakiuria and workup for suspected Sabulous Cystitis Trans-rectal Ultrasound: History: Hyperechoic structure Presented for further evaluation of present consistent pollakiuria. Clinical signs initially began with soft tissue mass with the mare’s estrus cycle. Was measuring 6 x 7 cm evaluated by r. DVM at which time the Urinary Bladder mare’s physical examination was WNL, Catheterization: CBC and serum biochemistry were Sloughed mucosa WNL, on rectal palpation the bladder present in sample was distended, upon catheterization Cystoscopy: Biopsy obtained large amount of cloudy urine with debris drained. Started on Doxycycline based on the culture results Signalment: 20 year old Warmblood Mare Presentation: Physical examination and brief neurologic examination within normal limits. No evidence of urine scald. Restrained in the stocks for evaluation • Abdominal Ultrasound • Rectal Palpation • Trans-rectal Ultrasound • Urinary catheterization • Cystoscopy Treatment Plan: Started on Piroxicam at 100 mg/day Surgical debulking performed 10 days after initial presentation Post Operative Discharge Instructions: Banamine (1000# dose) day 1 -4 post op Naxcel (2. 2 mg/kg, IM for 3 days) Phenazopyridine (2. 2 mg/kg) Piroxicam (100 mg/day) started after day 4 Surgical Debulking: Outcome: Pre-op antibiotics and Banamine administered. 1 month follow up The mare was sedated and restrained in the Nodules visible within the urinary bladder stocks. Caudal epidural performed with Decreased in size measuring 5 x 6 cm Detomidine and Carbocaine qs with saline to 8 m. L. Tail tied and perineum washed, urinary catheterization was performed. Modified endotracheal tube passed through the urethra to facilitate easy access to the bladder Lidocaine was infused into the urinary bladder. Performed via endoscopic guidance. ~50 -60% of the tumor was able to be debulked with a combination of a snare, endosurgical scissors, and a ligasure to control bleeding. 1 m. L/cubic 3 month follow up: cm Cisplatin injected Histopathology: Consistent with primary urinary bladder Transitional Cell Carcinoma 2020 Student and New Graduate Case Study Competition
- Slides: 24