APL Pierre Fenaux Hopital Avicenne Paris 13 University






































































- Slides: 94

APL Pierre Fenaux (Hopital Avicenne, Paris 13 University)

Etiology of APL About 10% of AML (about 130 new cases/year in France, probably more than 2000/year in India) n Incidence depending on ethnic (or environmental) factors n More and more often therapy related (after brest carcinoma) n

APL characteristics Morphology: M 3, M 3 v n Cytogenetics: t(15; 17) (t(11; 17, t(5; 17) very rare) complex or variant translocations n molecular biology: PML-RAR (bcr 1> bcr 2>bcr 3) others (PLZF-RAR, etc very rare) n Coagulopathy: DIC+fibrinolysis n

Prognostic factors in APL n WBC >10000/mm 3 (and platelets<40000/mm 3) (Sanz score) n RT-PCR analysis after consolidation treatment (but depends on sensitivity of the assay used) n other factors (M 3 v, bcr breakpoint…. : generally redundant with

Treatment of APL sensitive to n Anthracycline+/- Ara. C chemotherapy n ATRA n Arsenic derivatives

Treatment of APL n « classical » treatment n. Treatment with no or limited amount of chemotherapy?

« Classical » treatment of APL? 1)Newly diagnosed APL 2)Relapsing APL 3)Specific situations n Children n Elderly patients

Newly diagnosed APL : Induction and consolidation treatment should combine ATRA and anthracycline based chemotherapy: n n Slightly increases the CR rate (from 80 to>90%) considerably reduces relapses (from 50 to 25%)

Newly diagnosed APL Remaining issues: 1)with ATRA chemotherapy combinations -when to start chemotherapy? -anthracycline alone or with Ara. C? -prophylaxis and treatment of « ATRA syndrome » ? - treatment of coagulopathy? -CNS prophylaxis? -maintenance treatment 2)introduction of new agents (Arsenic, gentuzumab GO) 3)Role of allo SCT in first CR

When should chemotherapy be started?

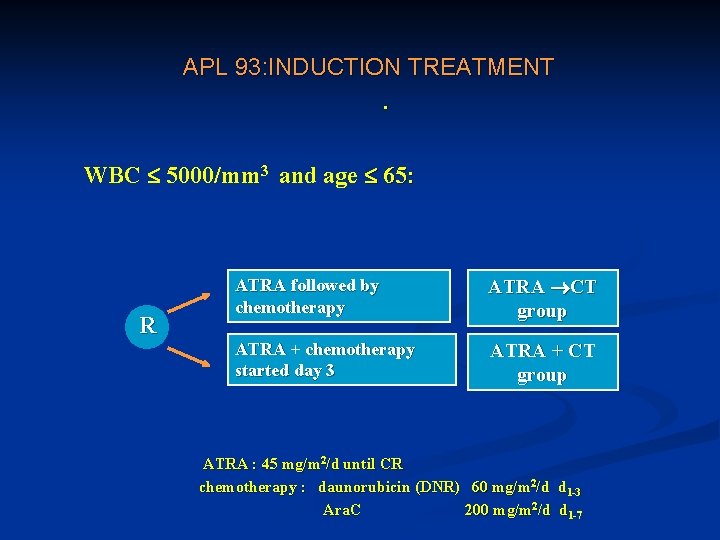
APL 93: INDUCTION TREATMENT. WBC 5000/mm 3 and age 65: R ATRA followed by chemotherapy ATRA CT group ATRA + chemotherapy started day 3 ATRA + CT group ATRA : 45 mg/m 2/d until CR chemotherapy : daunorubicin (DNR) 60 mg/m 2/d d 1 -3 Ara. C 200 mg/m 2/d d 1 -7

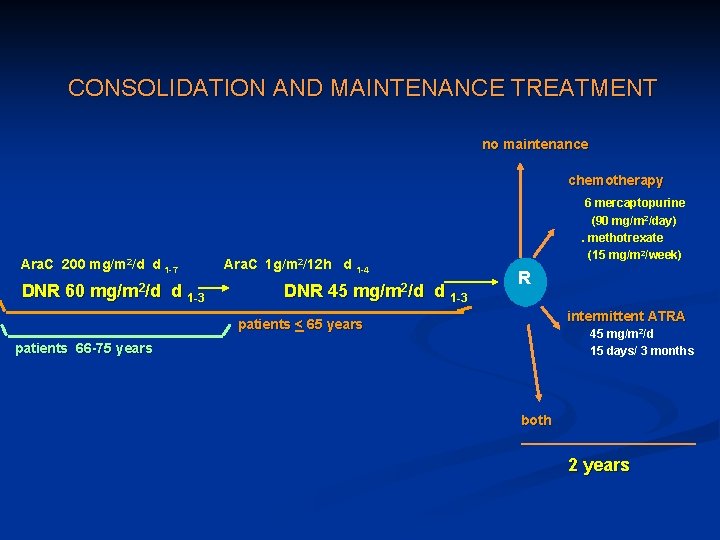
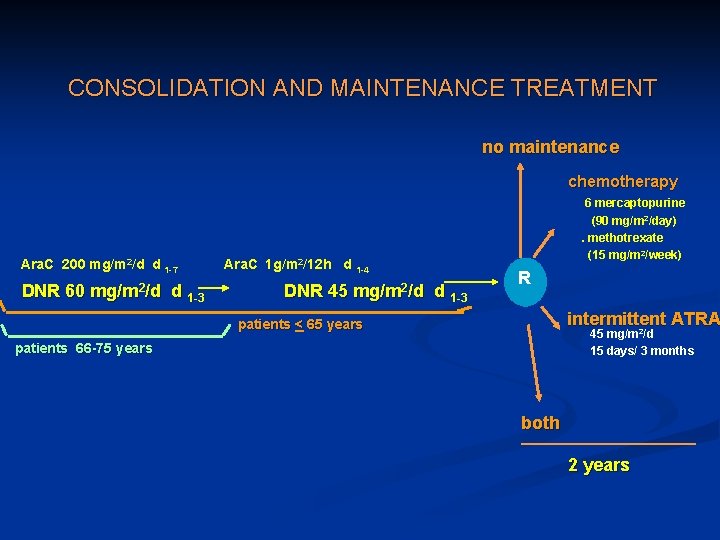
CONSOLIDATION AND MAINTENANCE TREATMENT no maintenance chemotherapy Ara. C 200 mg/m 2/d d 1 -7 Ara. C 1 g/m 2/12 h d 1 -4 DNR 60 mg/m 2/d d 1 -3 DNR 45 mg/m 2/d d 1 -3 . 6 mercaptopurine (90 mg/m 2/day). methotrexate (15 mg/m 2/week) R intermittent ATRA patients < 65 years 45 mg/m 2/d 15 days/ 3 months patients 66 -75 years both 2 years

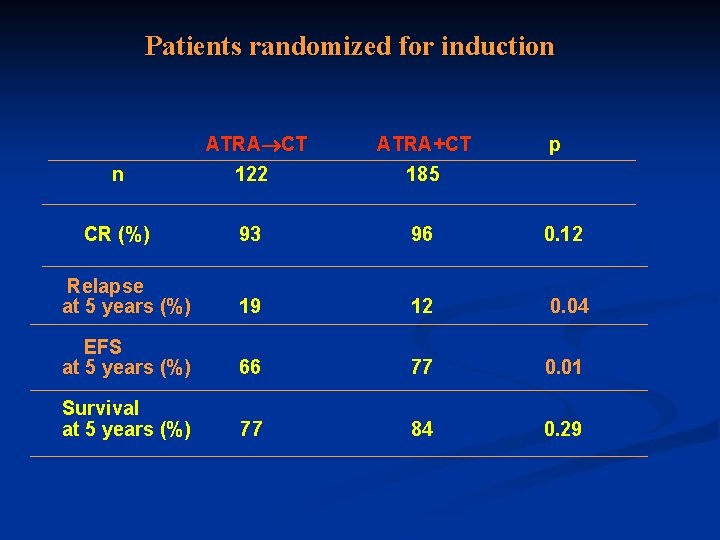
Patients randomized for induction ATRA CT ATRA+CT p n 122 185 CR (%) 93 96 0. 12 Relapse at 5 years (%) 19 12 0. 04 EFS at 5 years (%) 66 77 0. 01 Survival at 5 years (%) 77 84 0. 29

Prophylaxis and treatment of ATRA syndrome? High dose steroids or chemotherapy?

ATRA syndrome or leukocyte activation syndrome (can occur after arsenic) Fever n Pleural +/- pericardial effusion n Pumonary infiltrates n Weight gain n Cardiac failure n Renal failure n Generally preceded by increasing WBC counts n

Prophylaxis and treatment of ATRA syndrome 1)Treatment : high dose DXM (10 mg/12 H) 2)Prophylaxis increasing WBC: - Add chemotherapy? - Add high dose DXM?

Incidence of ATRA syndrome according to initial randomization (age < 66 and WBC < 5, 000) (De Botton, Leukemia, 2002) No ATRA Sd ATRA CT * 100 (82%) 22 (18%) ATRA + CT 167 (91%) 17 (9%) ] p =. 026

Should Ara. C be added to anthracyclines?

PETHEMA LPA 96 PETHEMA LPA 99 INDUCTION Nov/96 - Oct/99 AIDA CONSOLIDATION Median follow up 70 mo. Nov/99 - Present CONSOLIDATION Risk-Adapted MAINTENANCE MTX + 6 -MP + ATRA Median follow up 30 mo.

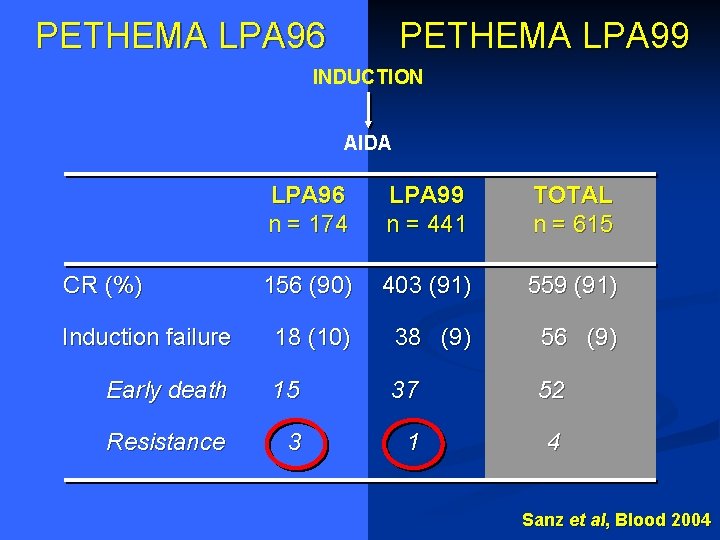
PETHEMA LPA 96 PETHEMA LPA 99 INDUCTION AIDA LPA 96 n = 174 LPA 99 n = 441 TOTAL n = 615 156 (90) 403 (91) 559 (91) 18 (10) 38 (9) 56 (9) Early death 15 37 52 Resistance 3 1 4 CR (%) Induction failure Sanz et al, Blood 2004

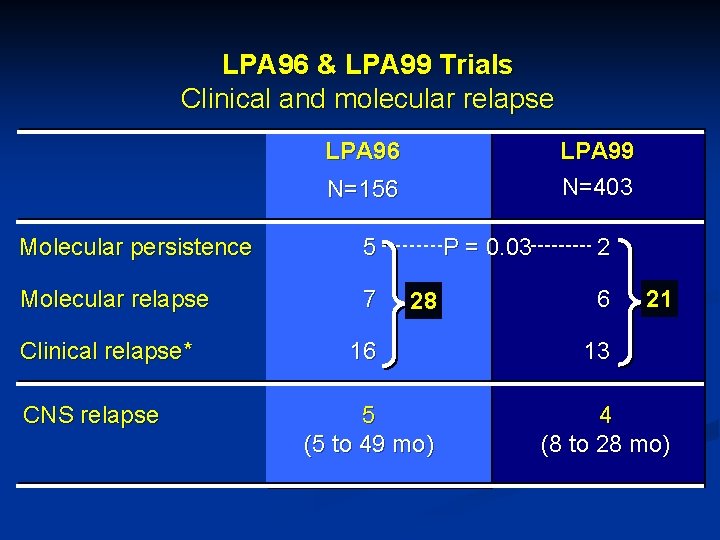
LPA 96 & LPA 99 Trials Clinical and molecular relapse LPA 96 LPA 99 N=403 N=156 Molecular persistence 5 Molecular relapse 7 Clinical relapse* CNS relapse P = 0. 03 28 16 5 (5 to 49 mo) 2 6 21 13 4 (8 to 28 mo)

LPA 96 & LPA 99 Trials Deaths in CR LPA 96 N=156 LPA 99 N=403 Before consolidation 0 1 (81 yrs) During consolidation 2 (50, 54 yrs) 4 3 (58, 64, 69, 72 yrs) 8 1 (73 yrs) 3 (33, 78, 81 yrs) After consolidation

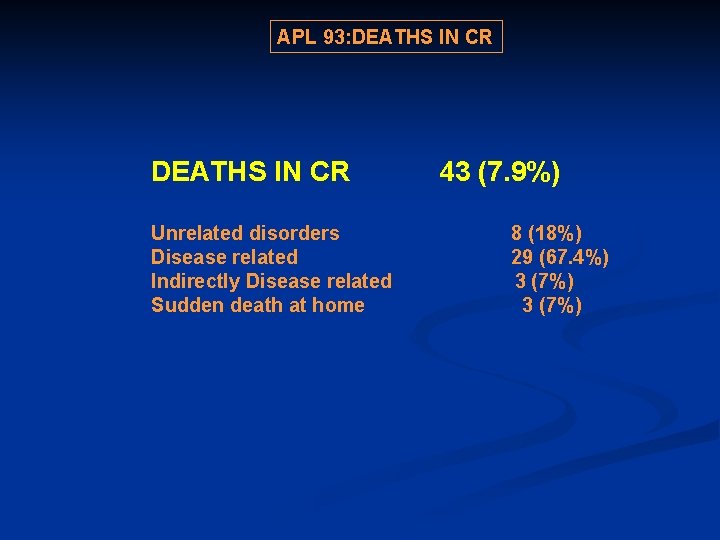
APL 93: DEATHS IN CR 43 (7. 9%) Unrelated disorders 8 (18%) Disease related 29 (67. 4%) Indirectly Disease related 3 (7%) Sudden death at home 3 (7%)

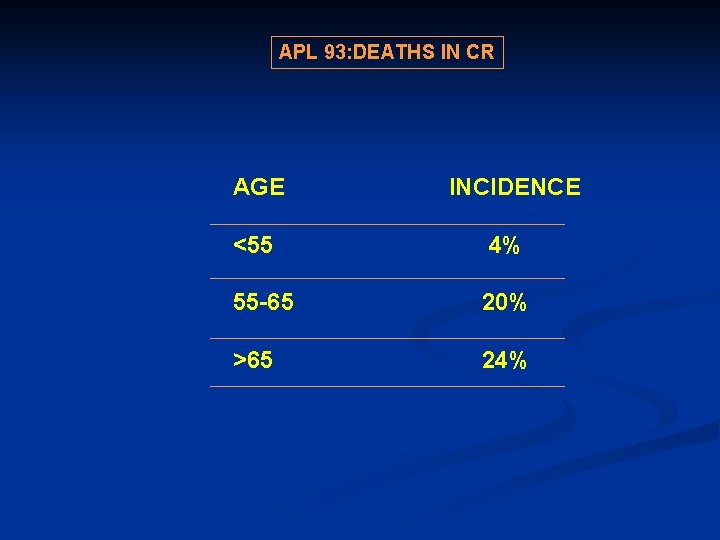
APL 93: DEATHS IN CR AGE INCIDENCE <55 4% 55 -65 20% >65 24%

APL 2000 trial Patients aged <60 with WBC<10000/mm 3: Reference arm (APL 93): ATRA+DNR+ Ara. C+ combined maintenance (ARA C+) VS same without Ara. C (ARA C -)

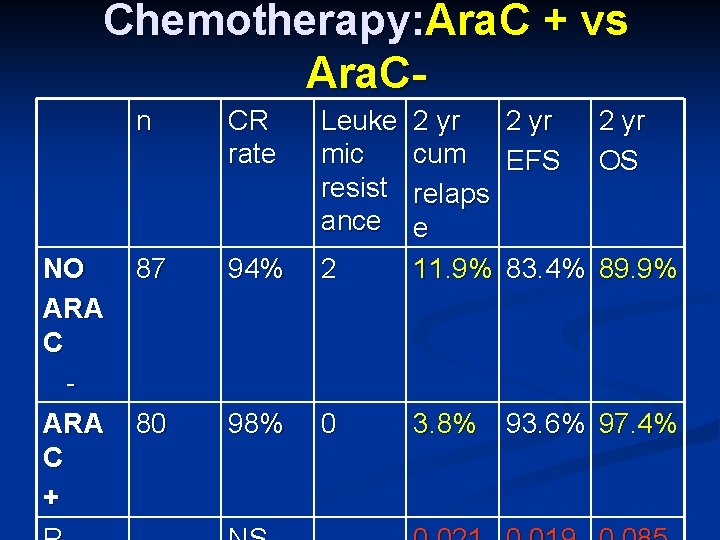
Chemotherapy: Ara. C + vs Ara. C- NO ARA C + n CR rate Leuke mic resist ance 87 94% 2 2 yr cum EFS OS relaps e 11. 9% 83. 4% 89. 9% 80 98% 0 3. 8% 93. 6% 97. 4%

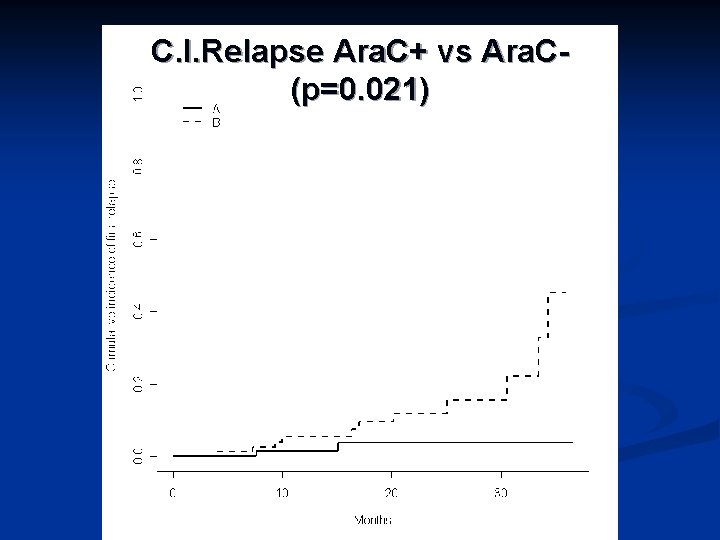
C. I. Relapse Ara. C+ vs Ara. C(p=0. 021)

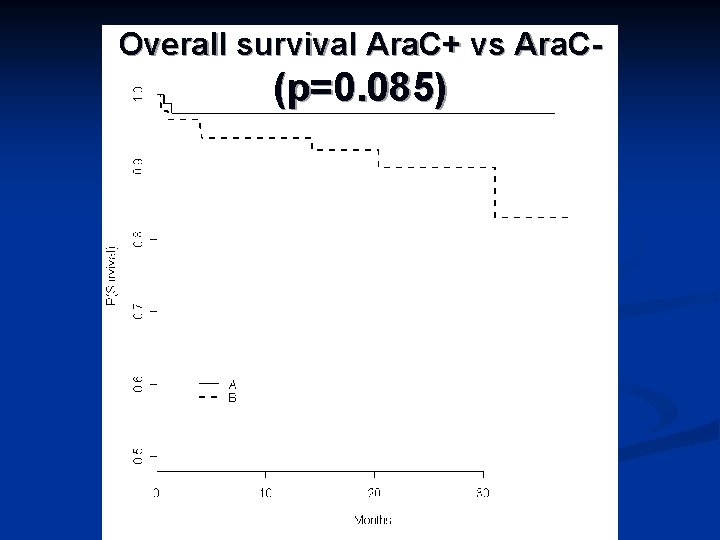
Overall survival Ara. C+ vs Ara. C- (p=0. 085)

APL 2000 : patients with WBC>10000/mm 3 n <60 yrs: reference APL 93 but with Ara. C 2 g/m 2/12 h d 1 to 5 during last consolidation course n >60 yrs: reference APL 93 with Ara. C 1 g/m 2/12 h d 1 to 4 during last consolidation course

APL 2000 trial: patients with WBC>10000/mm 3

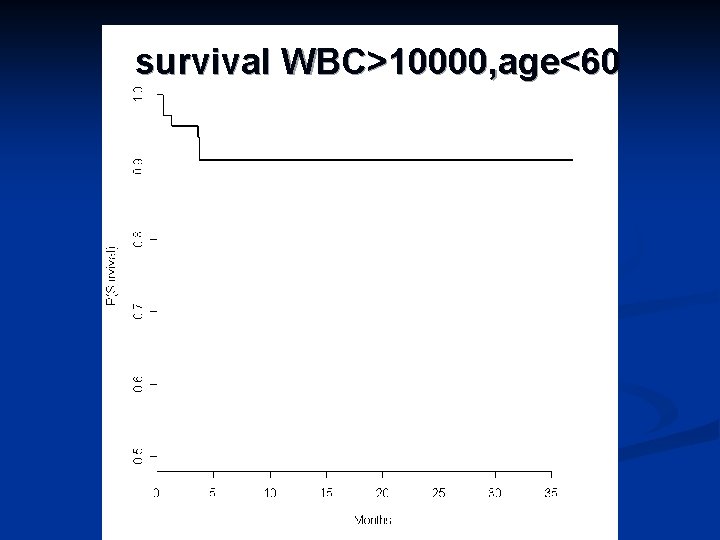
survival WBC>10000, age<60

High dose Ara. C in APL (Lengfelder, ASH 2003) 133 pts treated with ATRA and DAT-HAM -DAT -maintenance n 89% CR, 9% relapse n WBC<5000: 6% relapse n WBC>5000: 14% relapse n

Ara. C in APL? Probably required in high risk patients (ie high WBC counts , persisting PMLRAR levels) n In standard risk patients : - can high cumulative doses of anthracyclines can be substituted for Ara. C? -Idarubicin better than DNR? n

Should CNS prophylaxis be made?

Extramedullary relapses: European and Pethema group experience 806 pts included in APL 91 , APL 93 , PETHEMA 96 trial n 738 (92%) CR. 174 relapses n 14 EMD relapses = 8% of the relapses n

EM site : CNS (n=10), skin (n=3), orbital (n=1) n Associated bone marrow (BM) relapse (n=9) (only molecular in 4 of them) n

Patients with EM relapse characterized, by n younger age (p=. 03) n higher WBC counts (p=. 007 ) n N 0 high dose Ara. C (p=0. 03)

Outcome of EMD relapses n n 4 (29%) pts still alive after 41+ to 53+ months. Median survival from EMD 13 months, Supports CNS treatment in pts with high WBC counts(>10000) -intratheca. I MTX+ Ara. C -high dose Ara. C?

Treatment of coagulopathy n Intensive platelet support (maintain plts>50000/mm 3) n 0 thers measures (heparin, antifibrinolytic agents, fibrinogen)?

Should APL patients receive maintenance therapy?

Maintenance treatment in APL Is it useful? n What should be used? n For how long? n

CONSOLIDATION AND MAINTENANCE TREATMENT no maintenance chemotherapy Ara. C 200 mg/m 2/d d 1 -7 Ara. C 1 g/m 2/12 h d 1 -4 DNR 60 mg/m 2/d d 1 -3 DNR 45 mg/m 2/d d 1 -3 . 6 mercaptopurine (90 mg/m 2/day). methotrexate (15 mg/m 2/week) R intermittent ATRA 2 patients < 65 years 45 mg/m /d 15 days/ 3 months patients 66 -75 years both 2 years

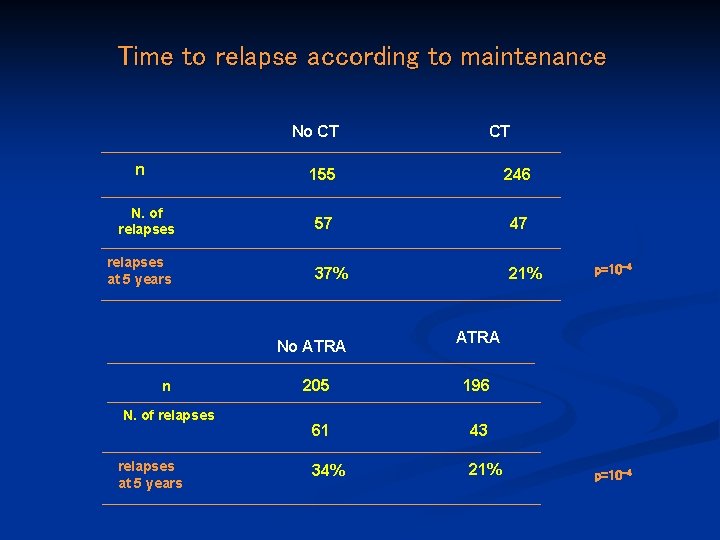
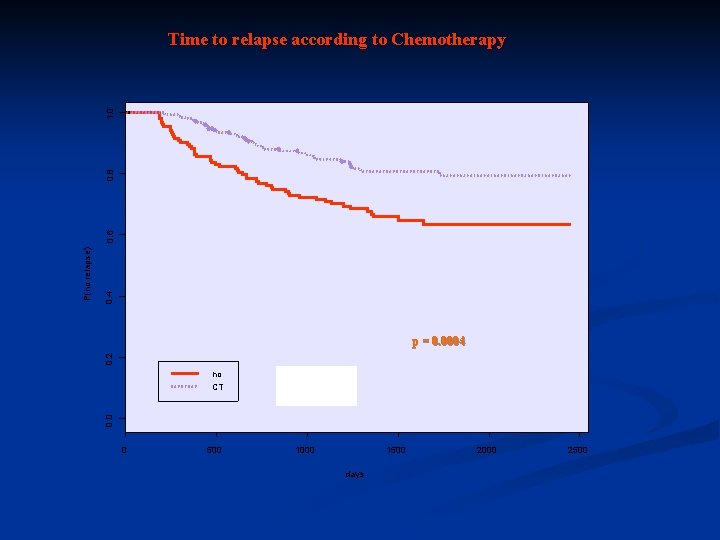
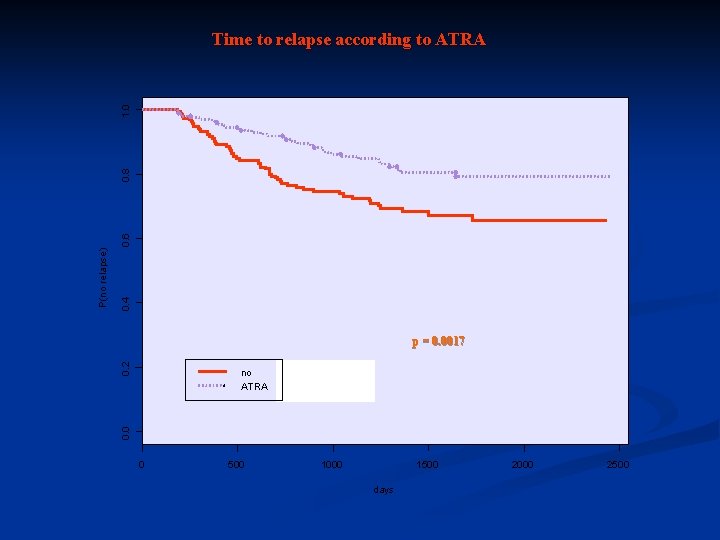
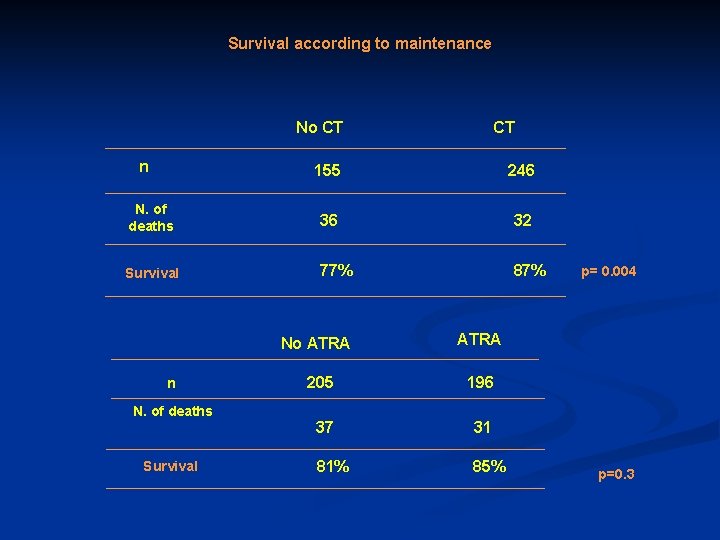
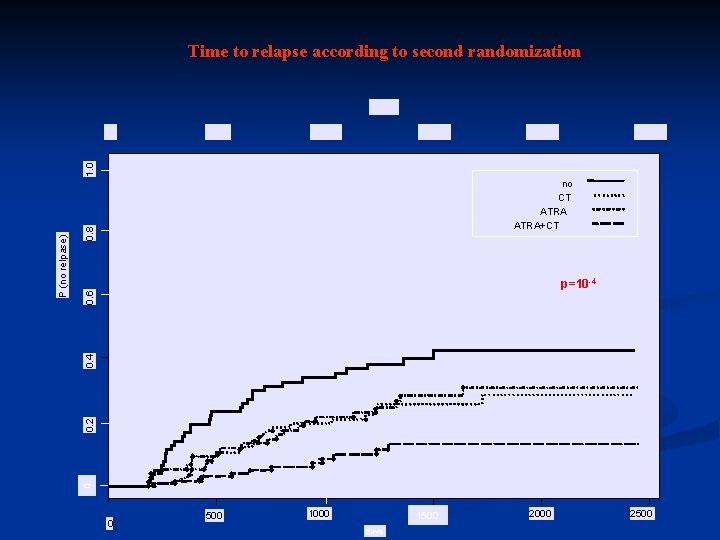
Time to relapse according to maintenance No CT n N. of relapses at 5 years 155 246 57 47 37% 21% No ATRA n N. of relapses at 5 years CT p=10 -4 ATRA 205 196 61 43 34% 21% p=10 -4

0. 4 0. 2 p = 0. 0004 no CT 0. 0 P(no relapse) 0. 6 0. 8 1. 0 Time to relapse according to Chemotherapy 0 500 1000 1500 days 2000 2500

0. 4 0. 2 p = 0. 0017 no ATRA 0. 0 P(no relapse) 0. 6 0. 8 1. 0 Time to relapse according to ATRA 0 500 1000 1500 days 2000 2500

Survival according to maintenance No CT n CT 155 246 N. of deaths 36 32 Survival 77% 87% p= 0. 004 No ATRA n N. of deaths Survival ATRA 205 196 37 31 81% 85% p=0. 3

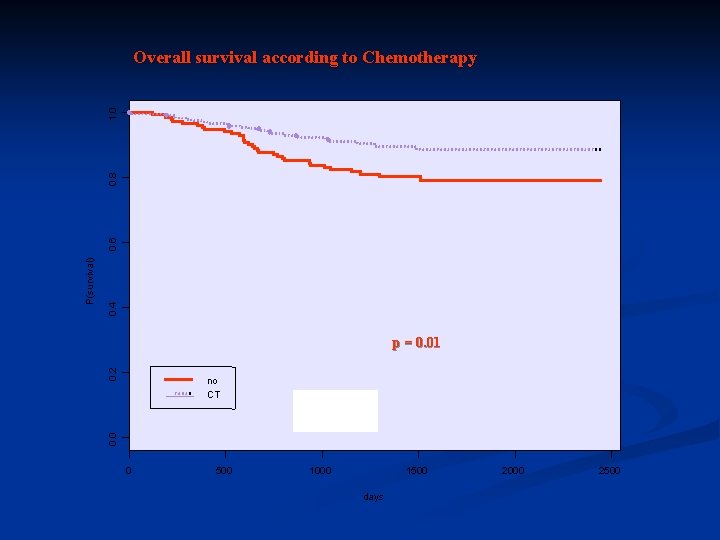
0. 4 0. 2 p = 0. 01 no CT 0. 0 P(survival) 0. 6 0. 8 1. 0 Overall survival according to Chemotherapy 0 500 1000 1500 days 2000 2500

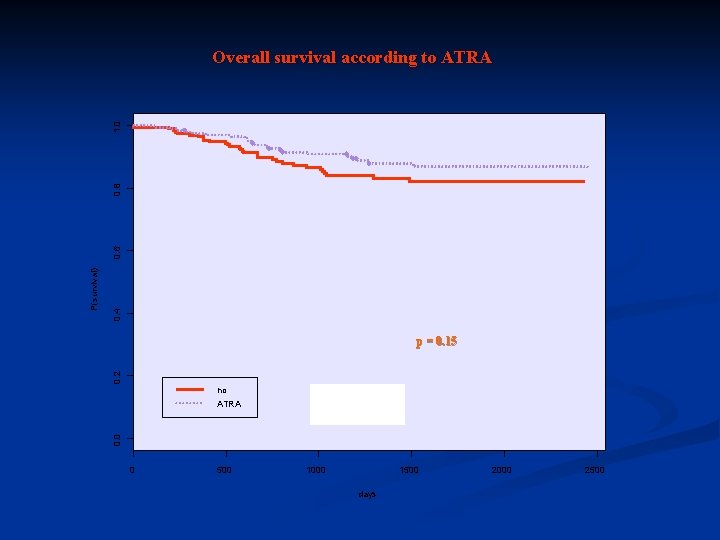
0. 4 0. 2 p = 0. 15 no ATRA 0. 0 P(survival) 0. 6 0. 8 1. 0 Overall survival according to ATRA 0 500 1000 1500 days 2000 2500

0. 8 no CT ATRA+CT 0 0. 2 0. 4 0. 6 p=10 -4 0 P P (no relpase) 1. 0 Time to relapse according to second randomization 500 1000 1500 days 2000 2500

Time to relapse according to second randomization in patients with WBC counts >5000/mm 3

Maintenance treatment in APL USEFUL: US intergroup (continuous ATRA during one year)

Duration of maintenance treatment (APL 93 trial): 46 patients < 1 year ( due to side effects): 21/46 (45%) relapses 313 patients > 1 year: 49/313 (16%) relapses Maintenance discontinuation <1 year may be deleterious

SIDE EFFECTS OF MAINTENANCE TREATMENT . Increased Liver enzymes : - ATRA 7% - CT 35% - ATRA+CT 34% • Cytopenias with CT usual • Pneumocystis pneumonia 3 • Deaths 6, from sepsis

Introduction of new agents (ATO, GO) in first line treatment -

Role of arsenic during first line treatment of APL? 1) high risk patients: add arsenic to current treatment -US intergroup study: in all patients -European APL study: in patients with WBC >10000/mm 3 2) standard risk patients: Arsenic used to lower the amount (avoid? ) chemotherapy

A role for allo SCT in first CR?

Allo SCT in first CR : rarely indicated For patients remaining RT-PCR positive after induction? n For patients with VERY high WBC counts (eg>50000/mm 3)? n

First line treatment of APL with limited (or no? ) chemotherapy

Treatment of APL with Arsenic and limited amounts of chemotherapy Lu et al (Blood, 2002) : As 4 S 4 1. 103 APL in CR after ATRA (n = 19) ATRA + CT (n = 84) - As 4 S 4 2 weeks on/2 weeks off during 4 years - 9 relapses 2. 19 newly diagnosed APL - As 4 S 4 for induction - 19 CR - As 4 S 4 for maintenance : 3/15 patients

Induction treatment of APL with ATRA and ATO (Shen, PNAS, 2004, 101, 5328) ATRAvs ATO+ATRA followed by 9 cycles of chemotherapy (3 DNRAra. C, 3 homoharringtonine-Ara. C) n 61 pts; similar CR rates n lower PML-RAR in the combined arm n 0/20 relapses in the combined arm, vs 7/37 with monotherapy (p<0. 05) n

ATRA+ATO without chemotherapy in standard risk APL (Estey et al) ATRA 45 mg/m 2/d+ATO 0. 15 mg/kg. d (+GO or idarubicin if WBC>10000) n then ATRA 15 d/month +ATO 5 d/w 4 w/month during 6 months n 32 pts, 88% CR (including molecular CR) n Only 3 relapses n

Treatment of newly diagnosed APL with ATO alone (Ghavamzabeh, ASH 2004) ATO 0. 15 mg/kg/d during 60 days, then 28 days n 68 pts. 90. 4% CR n Treatment Complications: » ATRA syndrome « (10 cases, 4 fatal) liver abn (19 cases) n 13 relapses, 2 year survival 86% n

Treatment of relapsing APL

n TREATMENT OF RELAPSING APL(European APL group experience) (De Botton, JCO, in press) n 564 patients <66 years in APL 91 and APL 93 trials : 525 (93%) achieved CR. n 122 /140 (87%) relapsing patients achieved CR 2 ATRA: 8 ATO: 4 Chemotherapy(CT): 24 ATRA+CT: 98

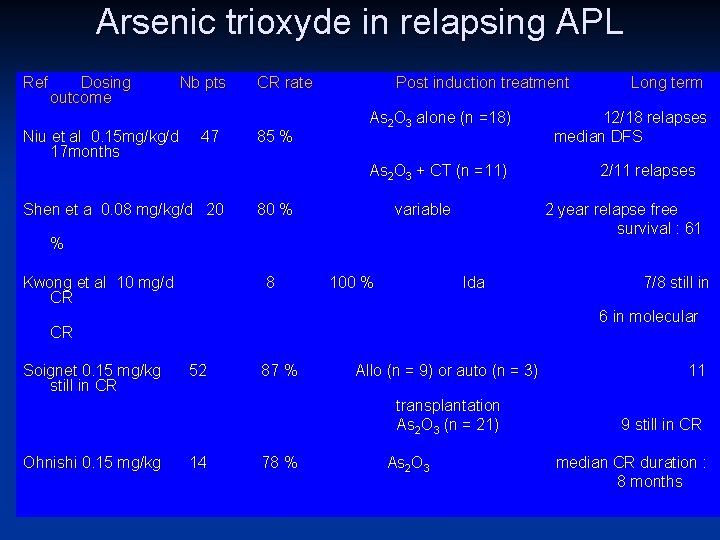
Arsenic trioxyde in relapsing APL Ref Dosing Nb pts CR rate Post induction treatment Long term outcome As 2 O 3 alone (n =18) 12/18 relapses Niu et al 0. 15 mg/kg/d 47 85 % median DFS 17 months As 2 O 3 + CT (n =11) 2/11 relapses Shen et a 0. 08 mg/kg/d 20 80 % variable % Kwong et al 10 mg/d CR 8 2 year relapse free survival : 61 100 % Ida 7/8 still in 6 in molecular CR Soignet 0. 15 mg/kg 52 still in CR 87 % Allo (n = 9) or auto (n = 3) transplantation As 2 O 3 (n = 21) Ohnishi 0. 15 mg/kg 14 78 % As 2 O 3 11 9 still in CR median CR duration : 8 months

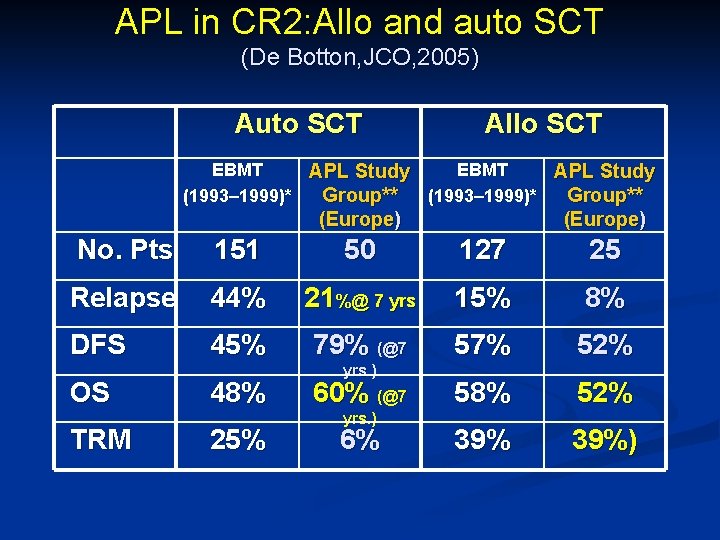
APL in CR 2: Allo and auto SCT (De Botton, JCO, 2005) Auto SCT Allo SCT EBMT APL Study (1993– 1999)* Group** (Europe) No. Pts 151 50 127 25 Relapse 44% 21%@ 7 yrs 15% 8% DFS 45% 79% (@7 57% 52% 58% 52% 39%) OS TRM 48% 25% yrs. ) 60% (@7 yrs. ) 6%

0. 6 0. 4 0. 2 AUTO ALLO 0. 0 P(No event) 0. 8 1. 0 Event-free survival (EFS) from transplantation 0 500 1000 1500 Days from transplant 2000 2500 3000

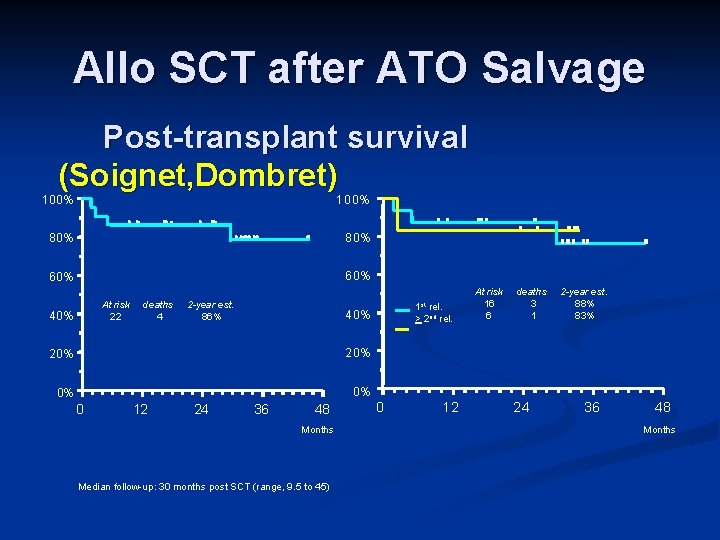
Allo SCT after ATO Salvage Post-transplant survival (Soignet, Dombret) 100 % 1 0 0 % 8 0 % 6 0 % At risk deaths 2 -year est. 22 4 86% 40 % 4 0 % 2 0 % 0 % 0 12 24 1 st rel. 36 48 Months Median follow-up: 30 months post SCT (range, 9. 5 to 45) > 2 nd rel. 0 12 At risk deaths 2 -year est. 16 3 88% 6 1 83% 24 36 48 Months

European APL group recommendations for APL patients in first relapse Induction with ATO (0. 15 mg/kg, max 50 days) n Consolidation with ATO (5 days/w for 25 doses) n donor and<40 yrs: allo no donor: Ida Ara. C -if PCR neg: auto -if PCR pos: GO, etc. . elderly pts: maintenance ATO, ATRA low dose CT, GO ,

Treatment of APLmolecular relapse by Gentuzumab ozogamycin(GO) (Lo Coco, Blood, 2004) 16 pts with molecular relapse (8, 5, 2, 1) n GO 6 mg/m 2 x 2 + 1 n 14 molecular CR achieved n 7 pts still in CR (7+ to 31+ months), 7 relapses after 3 to 15 months n

Treatment of APL in children and elderly patients

APL in children (De Botton, JCO, 2004) 10% of APL n Often high WBC counts n Similar response to ATRA+ chemo as in adults n Concerns about: Initial doses of ATRA (25 mg/m 2) High cumulative doses of anthracyclines n

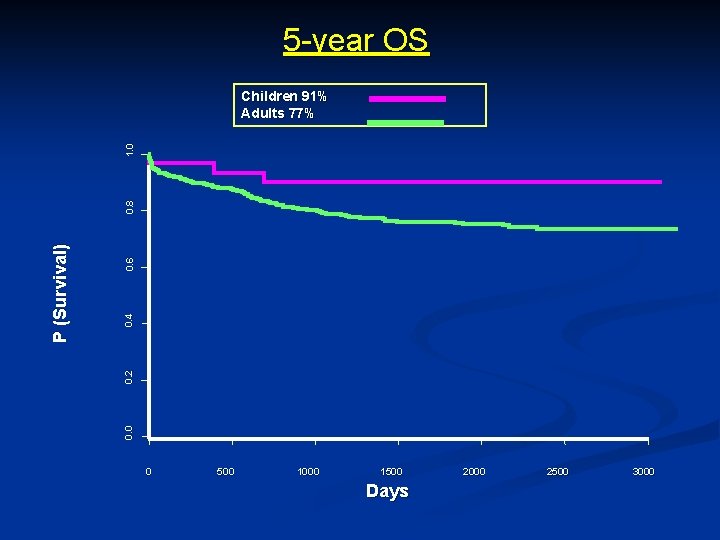
5 -year OS 0. 6 0. 4 0. 2 0. 0 P (Survival) 0. 8 1. 0 Children 91% Adults 77% 0 500 1000 1500 Days 2000 2500 3000

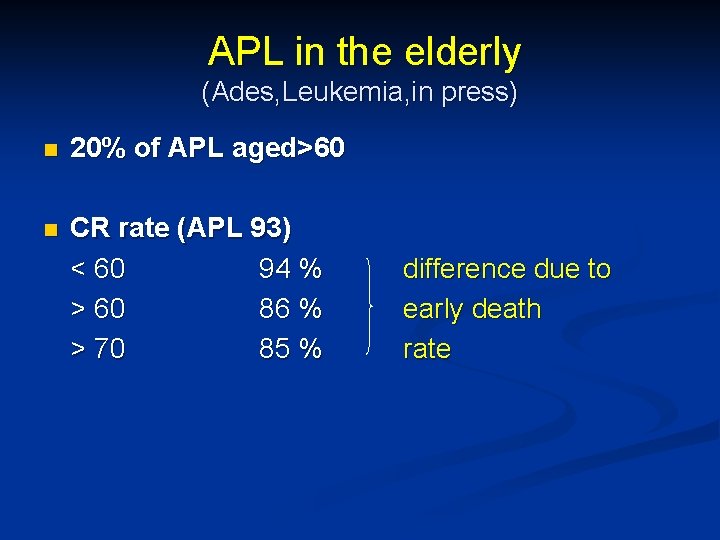
APL in the elderly (Ades, Leukemia, in press) n 20% of APL aged>60 n CR rate (APL 93) < 60 94 % > 60 86 % > 70 85 % difference due to early death rate

APL in the elderly (2) Relapse at 4 years - 26 % in pts < 60 - 20 % in pts > 60 n Survival at 4 years - 79 % in pts < 60 - 55 % in pts > 60 due to deaths in CR n

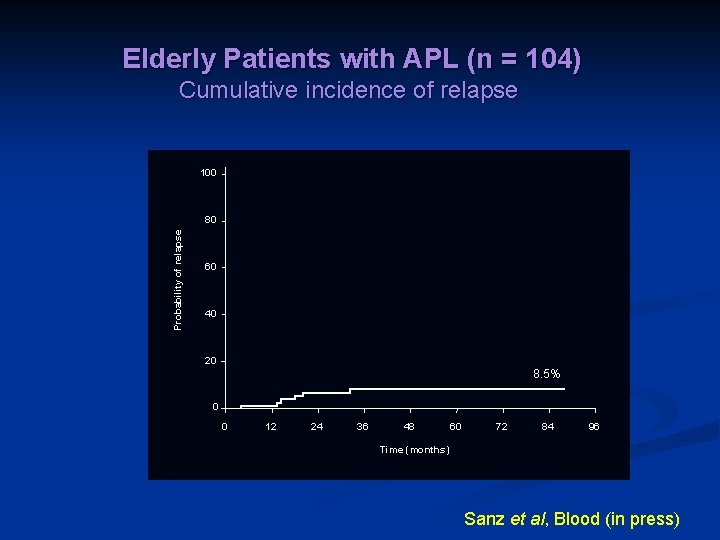
Elderly Patients with APL (n = 104) Cumulative incidence of relapse 100 Probability of relapse 80 60 40 20 8. 5% 0 0 12 24 36 48 60 72 84 96 Time (months) Sanz et al, Blood (in press)

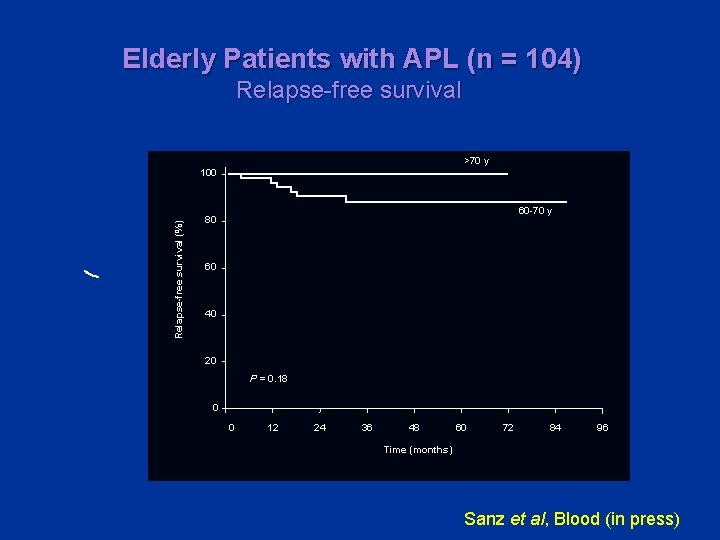
Elderly Patients with APL (n = 104) Relapse-free survival >70 y Relapse-free survival (%) 100 60 -70 y 80 60 40 20 P = 0. 18 0 0 12 24 36 48 60 72 84 96 Time (months) Sanz et al, Blood (in press)

Arsenic derivatives for APL in children and elderly patients? Children: add Arsenic to reduce the cumu. Iative dose of anthracyclines? n Elderly patients (or cardiac problems…): add arsenic to reduce the total amount of chemotherapy n


Question 1: All but one of the following parameters are prognostic factors in APL A: pretreatment WBC count n B: age n C: hemoglobin level n D: PML-RAR alpha transcript after consolidation treatment n

Question 2: all but one of the following symptoms are hallmarks of the ATRA syndrome n A: pulmonary infiltrates n B: pleural effusion n C: clinical bleeding n D: unexplained fever

Question 3: what is the major component of treatment of initial coagulopathy in APL? A: heparin n B: platelet transfusions n C: tranexamic acid or other antifibrinolytic drugs n D: fibrinogen infusions n

Question 4: APL patient with WBC=15000/mm 3. First line treatment? A: ATRA followed by anthracycline based CT n B: anthracycline based CT` n C: ATRA plus anthracycline based CT n D: arsenic derivative alone n

Question 5: what is your induction treatment for first relapse APL (WBC< 10000/mm 3) A: ATRA alone n B: Arsenic derivative alone` n C: ATRA+ anthracycline based CT n D: Gentuzumab (mylotarg) n


LUNG PNEUMOCYSTIS INFECTION 3 patients ATRA+CT at 5 months ATRA+CT at 13 months CT at 19 months maintenance prematurely stopped 1 relapse Prophylaxis required

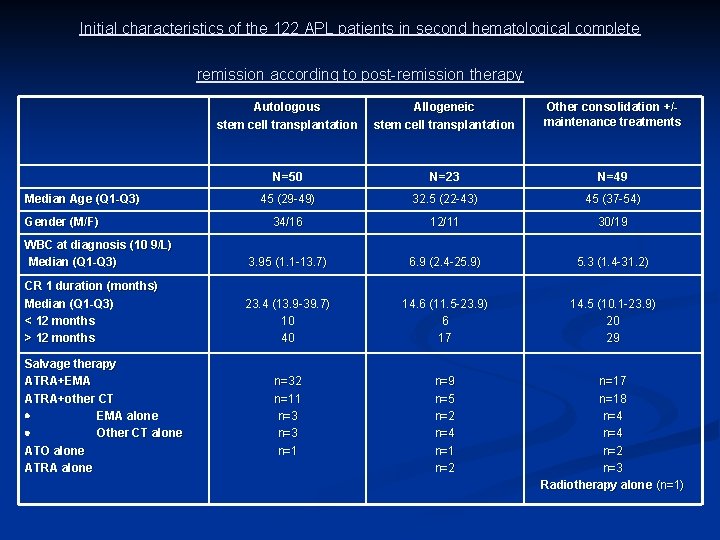
Initial characteristics of the 122 APL patients in second hematological complete remission according to post-remission therapy Autologous stem cell transplantation Allogeneic stem cell transplantation Other consolidation +/- maintenance treatments N=50 N=23 N=49 45 (29 -49) 32. 5 (22 -43) 45 (37 -54) 34/16 12/11 30/19 WBC at diagnosis (10 9/L) Median (Q 1 -Q 3) 3. 95 (1. 1 -13. 7) 6. 9 (2. 4 -25. 9) 5. 3 (1. 4 -31. 2) CR 1 duration (months) Median (Q 1 -Q 3) < 12 months > 12 months 23. 4 (13. 9 -39. 7) 10 40 14. 6 (11. 5 -23. 9) 6 17 14. 5 (10. 1 -23. 9) 20 29 n=32 n=11 n=3 n=1 n=9 n=5 n=2 n=4 n=1 n=2 n=17 n=18 n=4 n=2 n=3 Radiotherapy alone (n=1) Median Age (Q 1 -Q 3) Gender (M/F) Salvage therapy ATRA+EMA ATRA+other CT EMA alone Other CT alone ATO alone ATRA alone

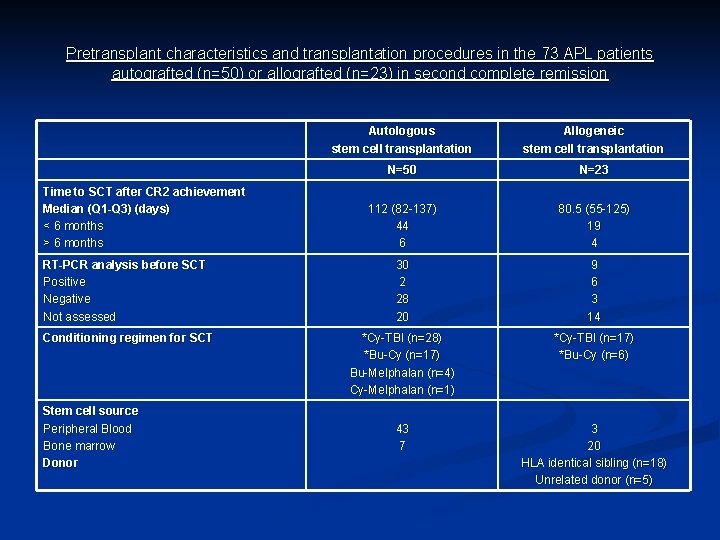
Pretransplant characteristics and transplantation procedures in the 73 APL patients autografted (n=50) or allografted (n=23) in second complete remission Time to SCT after CR 2 achievement Median (Q 1 -Q 3) (days) < 6 months > 6 months RT-PCR analysis before SCT Positive Negative Not assessed Conditioning regimen for SCT Stem cell source Peripheral Blood Bone marrow Donor Autologous stem cell transplantation Allogeneic stem cell transplantation N=50 N=23 112 (82 -137) 44 6 80. 5 (55 -125) 19 4 30 2 28 20 9 6 3 14 *Cy-TBI (n=28) *Bu-Cy (n=17) Bu-Melphalan (n=4) Cy-Melphalan (n=1) *Cy-TBI (n=17) *Bu-Cy (n=6) 43 7 3 20 HLA identical sibling (n=18) Unrelated donor (n=5)

n ; n 7 -year RFS, EFS and OS in the auto SCT group were 79. 4%, 60. 6% and 59. 8%, respectively, with a TRM of 6%. 7 -year RFS, EFS and OS in the allo SCT group were 92. 3%, 52. 2% and 51. 8%, respectively, with a TRM of 39%. No significant differences in RFS and EFS were seen between auto and allo SCT (p=. 19 and p=. 11, respectively) but was OS significantly better in the auto SCT group than in the allo SCT group (p=. 04). In non-transplanted patients, 7 -year RFS, EFS and OS were 38%, 30. 4% and 39. 5%, respectively. n n n

Patients with very high WBC counts (> 50 000/mm 3) n n = 44 n M = 24, F = 20 n 36/44 (82%) CR n 2 deaths during consolidation courses, 3 relapses before second randomization 15 subsequent relapses

As 2 O 3 alone versus As 2 O 3 + ATRA in relapsing APL (1) (Raffoux et al, JCO, 2003) n N = 20 n First relapse = 7 ; second or subsequent relapse = 13 n As 2 O 3 : 0, 15 mg/kg/d n ATRA : 45 mg/m²/d

As 2 O 3 alone versus As 2 O 3 + ATRA in relapsing APL (2) (Raffoux et al, JCO, in press) n n n CR 80 % in each treatment group median time to CR 42 days in each treatment group similar improvement in coagulopathy 3 pts reached molecular CR after one course. All 3 had also received chemotherapy (for high WBC counts) pharmacokinetic profile of As 2 O 3 similar in the 2 arms adverse events similar in both arms

As 2 O 3 alone versus As 2 O 3 + ATRA in relapsing APL (3) (Raffoux et al, JCO, in press) n 10 pts received As 2 O 3 ± ATRA consolidation (2 courses). Only 2/8 PCR negative after 2 consolidation courses n 8 allo or autologous SCT Similar survival n

Role of Arac in the incidence of CNS relapses 5 CNS relapses in 159 PETHEMA pts (3%) (treated without Ara. C) vs 5 in 579 APL 91 and 93 pts (0. 9%) (treated with high dose Ara. C) (p=. 07). n CNS involvement at relapse in PETHEMA (28% of relapses) more frequent than in APL 91 and 93 (3%)(p=. 001). n