Acute and Chronic Pancreatitis The Pancreas one hard



























































- Slides: 61

Acute (and Chronic) Pancreatitis:

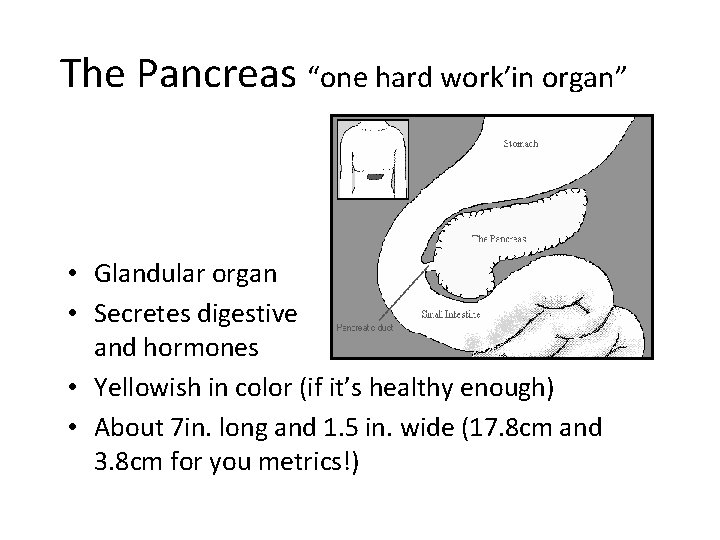
The Pancreas “one hard work’in organ” • Glandular organ • Secretes digestive enzymes and hormones • Yellowish in color (if it’s healthy enough) • About 7 in. long and 1. 5 in. wide (17. 8 cm and 3. 8 cm for you metrics!)

Location • Sits outside the posterior curve of stomach behind the duodenum and the spleen stomach • Located in retro peritoneal space, mostly behind stomach • Divided into head, body, and tail portions • Connected to the small intestine at the duodenum

Pancreas • A major mixed gland – Has both endocrine and exocrine functions • 98% exocrine – Secretion of digestive enzymes and bicarbonate by pancreatic acini and ducts • 2% endocrine – Peptide hormones vital in regulating carbohydrate metabolism and blood sugar • “Detects” levels of nutrients absorbed from intestine via hepatic portal vein

– Islets of Langerhans’ cells • throughout pancreas • Alpha cells which secrete glucagon – Increase glucose concentration in blood • Beta cells which secrete insulin – Lower blood glucose • Delta cells which secrete somatostatin – Regulate other pancreatic hormones

Somatostatin Facts • 3 rd peptide secreted from pancreas • Tends to dampen rise in both insulin and glucagon, preventing roller-coaster rides with the blood sugar! • May inhibit GH secretion from pituitary, since GH has anti-insulin effects

So, what are those enzymes? • Pancreatic Acinar cells secrete pancreatic enzymes • Produce digestive enzymes and bicarbonate. Secretes about 1, 500 -2, 000 cc of digestive solution per day • Lipase • Amylase • Trypsin Main • Phospholipase (PLA 2) ones

Acute pancreatitis • Pathophys- insult leads to leakage of pancreatic enzymes into pancreatic and peripancreatic tissue leading to acute inflammatory reaction • Inflammation of the pancreas • Pancreatic enzymes activated prematurely (before reaching intestines) • Activates inflammatory mediators to area • Increasing vascular permeability • Leads to edema and fluid shifts from intravascular spaces to the interstitum • Vasodilation occurs, increased capillary leakage and pooling of fluid in the venous system can result in shock and reduced cardiac function • Destruction of connective tissue in the vascular wall and causes microemboli can lead to DIC and bleeding

Acute pancreatitis • Phospholipase A irritates pancreatic tissue and causes tissue necrosis • Lipase overflowing into the tissues and systemic circulation leads to fat necrosis of the pancreas and surrounding areas • Risk of mortality increases with development of infection or pulmonary, cardiac, and renal complications

Causes of Acute Pancreatitis • Obstruction – Cholelithiasis – Ampullary or pancreatic tumor – Duodenal obstruction – Papillary obstruction – Hypertensive Oddi’s sphincter – Ampullary stenosis – Biliary disease

Causes of Acute Pancreatitis • Infection – Parasitic (ascariasis, clonorchiasis) – Viral (mumps, rubella, hepatitis, Epstein-Barr, HIV) – Bacterial (mycoplasma, legionella, leptospirosis)

Causes of Acute Pancreatitis • Vascular – Ischemia – Atherosclerotic emboli • Trauma – Accidental or postoperative trauma – Endoscopic retrograde cholangiopancreatography – Surgical procedures

Causes of Acute Pancreatitis • Toxins and Drugs – – – Alcohol Azathioprine Estrogen Furosemide Corticosteroids NSAIDS Opiates Procainamide Scorpion venom Sulfonamides Tetracycline Thiazide diuretics • Hereditary Factors – Hereditary pancreas • Miscellaneous – – – – Perforated peptic ulcer Crohn’s disease Reye’s syndrome Hypothermia Lupus Pregnancy Malignancy Idiopathic causes (dunno ! )

More Statistics • Cholelithiasis most common cause in the U. S. , Western Europe, and Asia (45% of cases) • Chronic alcohol ingestion is second leading cause (35%) • Pseudocytes and abscesses account for 70 to 80% of mortality

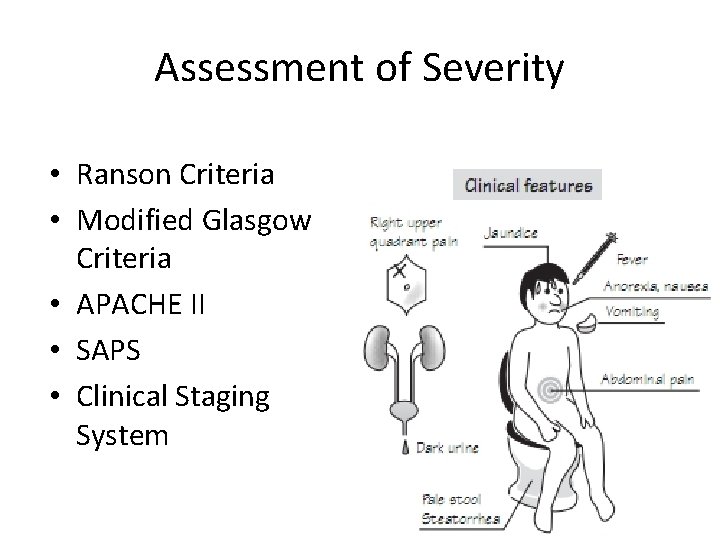
Signs & Symptoms • Severe epigastric abdominal pain - abrupt onset (may radiate to back) • Nausea & Vomiting • Weakness • Tachycardia • +/- Fever; +/- Hypotension or shock – Grey Turner sign - flank discoloration due to retroperitoneal bleed in pt. with pancreatic necrosis (rare) – Cullen’s sign - periumbilical discoloration (rare)

Acute Pancreatitis • Clinical Manifestations – Epigastric or midabdominal pain – May radiate to back – Fever, leukocytosis – Nausea and vomiting – Abdominal distention – Hypotension and shock, DIC – ATN, ARDS – Formation of pancreatic fluid collections (pseudocytes and abscesses)

Clinical Manifestations (continued) – Atelectasis, Pneumonia, Pleural Effusions, Pulmonary edema, – Tetany may develop as a result of deposition of calcium in areas of fat necrosis or decreased parathorome – Transient hyperglycemia – Lleus, colonic obstruction – CNS hypoperfusion with confusion

Differential Diagnosis • • Biliary colic Perforated hollow viscus Mesenteric ischemia Closed-loop intestinal obstruction Inferior wall MI Dissecting aneurysm Ectopic pregnancy

Diagnosis • Based on clinical presentation, history, physical and labs • Amylase and lipase levels • Amylase elevated in 80% – More sensitive early on • Lipase is more sensitive if symptoms have been present for more than 24 hours

Diagnosis • Both amylase and lipase levels may be normal with CT proved pancreatitis • Ultrasonography or CT is definitive • Radiography may reveal a “sentinel loop” – Localized ileus in midepigastric region – Pleural effusions may also be present • MRI, abdominal plain films, Chest X-ray Upright

Acute Pancreatitis • Lab studies – CBC, electrolytes, liver enzymes, calcium, magnesium, PT/PTT – May have hemoconcentration due to third spacing of fluid – May have hypocalcemia caused by “soap” formation • Saponification of triglycerides and calcium – Frequently have hypomagnesemia – WBC usually elevated – Liver enzymes may be elevated from biliary obstruction

Evaluation • amylase…Nonspecific !!! – Amylase levels > 3 x normal very suggestive of pancreatitis • May be normal in chronic pancreatitis!!! – Enzyme level severity – False (-): acute on chronic (Et. OH); Hyper. TG – False (+): renal failure, other abdominal or salivary gland process, acidemia • lipase – More sensitive & specific than amylase

Lab studies (continued) – Elevated Serum Amylase • Rises rapidly, usually within hours after attack • Remains elevated for about 4 days • Reference range in adults 0 -140 U/dl – Elevated Urine Amylase • Rises in a few hours after the rise in serum amylase and lipase • Remains elevated for about 7 to 10 days • The rise in urine amylase is secondary to an increase in the renal clearance of amylase

Lab studies (continued) – Elevated Serum Lipase • Also rapidly rises within hours after attack • Remains elevated for about 4 days • Reference range in adults 130 U/L – Elevated C-reactive protein measures severity – Amylase clearance to Creatinine clearance by the kidney (increases significantly compared with Creatinine clearance) • Normal ratio for amylase clearance is between 2 -5% • In pancreatitis, the ratio is increased

Danger Signals: First Few Hours • • Encephalopathy Hypoxemia Tachycardia > 130/min Hypotension < 90 mm. Hg Hct > 50 Oliguria < ml/hr Azotemia

Radiographic Evaluation • AXR - “sentinel loop” or small bowel ileus • US or CT may show enlarged pancreas with stranding, abscess, fluid collections, hemorrhage, necrosis or pseudocyst • MRI/MRCP newest “fad” – Decreased nephrotoxicity from gadolinium – Better visualization of fluid collections – MRCP allows visualization of bile ducts for stones – Does not allow stone extraction or stent insertion • Endoscopic US (even newer but used less) – Useful in obese patients

CT Criteria of Severity a. Normal b. Enlargement c. Peripancreatic inflammation d. Single fluid collection e. Multiple fluid collections

CT Severity Index • CT Grade – A is normal (0 points) – B is edematous pancreas (1 point) – C is B plus extrapancreatic changes (2 points) – D is severe extrapancreatic changes plus one fluid collection (3 points) – E is multiple or extensive fluid collections (4 points) • Necrosis score – – None (0 points) < 1/3 (2 points) > 1/3, < 1/2 (4 points) > 1/2 (6 points) • TOTAL SCORE = CT grade + Necrosis 0 -1 = 0% mortality 2 -3 = 3% mortality 4 -6 = 6% mortality 7 -10 = 17% mortality

Acute Pancreatitis • Morbidity and mortality highest if necrosis present (especially if necroctic area infected) – Dual phase CT scan useful for initial eval to look for necrosis • However, necrosis may not be present for 48 -72 hours

Prognosis • Many different scoring systems – Ranson (most popular & always taught in med-school) • No association found with score, and mortality or length of hospitalization – APACHE II – CT severity Index • Recent studies show this to be most predictive of adverse outcomes – CT score > 5 associated with 15 x mortality rate – Problem is 1 CT study showing this was conducted 72 hours after admission (Ranson/Apache are 24 & 48 hours) – Imrie Score • Atlanta Classification used to help compare various scores (clinical research trials)

Assessment of Severity • Ranson Criteria • Modified Glasgow Criteria • APACHE II • SAPS • Clinical Staging System

Ranson Criteria • Admission – – – Age > 55 WBC > 16, 000 Glucose > 200 LDH > 350 AST > 250 • During first 48 hours – – – Hematocrit drop > 10% Serum calcium < 8 Base deficit > 4. 0 Increase in BUN > 5 Fluid sequestration > 6 L Arterial PO 2 < 60 5% mortality risk with <2 signs 15 -20% mortality risk with 3 -4 signs 40% mortality risk with 5 -6 signs 99% mortality risk with >7 signs

Ranson’s Criteria • During 1 st 48 hours: – fall in HCT > 5 mg% – BUN rise> 5 mg% – Serum Calcium < 8 mg% – Base deficit > 4 meq/L – Estimated fluid sequestration > 6 L – Arterial PO 2 < 60 mm Hg

How Sick Are You? • Using Ranson’s Criteria will predict the severity of the nonalcoholic acute pancreatitis (possible score of 11) – Age>55 years – WBC > 16, 000/mm 3 – Serum glucose > 200 mg/dl – SGOT > 300 IU/L

Ranson’s Criteria • Relation to morbidity/mortality – 2 or fewer signs: 1% mortality – 3 signs: severe pancreatitis – 3 -4 signs: 15% mortality – 5 -6 signs: 40% mortality – More than 6 signs: better ask for the priest for fire proofing!!

Acute Pancreatitis • Goal of treatment is to stop autodigestion • Prevent systemic complications – Maintain hemodynamic stability • Monitor BP, urine output, and peripheral circulation • PA catheter if needed • Parenteral fluids, fluid resuscitation if needed (Crystalloids, colloids, blood if needed) • May require vasoactive drugs (Dopamine) to increase SVR

Therapy • Remove offending agent (if possible) • Supportive !!! • #1 - NPO (until pain free) – NG suction for patients with ileus or emesis – TPN may be needed • #2 - Aggressive volume repletion with IVF – Keep an eye on fluid balance/sequestration and electrolyte disturbances

Therapy continued • #3 - Narcotic analgesics usually necessary for pain relief…textbooks say Meperidine… – NO conclusive evidence that morphine has deleterious effect on sphincter of Oddi pressure • #4 - Urgent ERCP and biliary sphincterotomy within 72 hours improves outcome of severe gallstone pancreatitis – Reduced biliary sepsis, not actual improvement of pancreatic inflammation • #5 - Don’t forget PPI to prevent stress ulcer

Acute Pancreatitis – Improve oxygenation • Supplemental oxygen • May need mechanical ventilation (ARDS) • Monitor Sp. O 2 via pulse ox • Monitor lung sounds • Suction if rhonchi present • Assume Fowler’s position if in compromise – Promotes maximum lung expansion • Watch for atelectasis or hypoxia • Encourage cough and deep breath, walk to maintain lung function

Acute Pancreatitis – Maintain metabolic balance • Monitor for electrolyte imbalances such as hypokalemia and hypocalcemia (assess for Chvostek’s and Trousseau’s sign) • Watch for arrhythmias • Watch glucose, may need insulin • Monitor BUN and Creatinine • Follow amylase and lipase levels • Obtain daily albumin levels

Acute Pancreatitis – Pain management • Narcotics to relieve pain around the clock • Demerol not MSO 4, but morphine lasts longer so. .

Pancreatitis • Nursing Interventions – Administer analgesics, antacids, anticholinergics as ordered, monitor effects – Withhold food/fluid and eliminate odor and sight of food from environment to decrease pancreatic stimulations – Maintain NG tube and assess for drainage

Pancreatitis • Nursing Interventions (continued) – Institute nonpharmacologic measures to decrease pain • Assist patient to position of comfort (knee-chest; fetal position) – Teach relaxation techniques and provide a quiet, restful environment

Patient and Family Teaching • Talk about conditions which caused illness • Importance to sticking to a bland, low-fat, high carbohydrate diet avoiding large meals and caffeine • Make sure they know the symptoms of acute pancreatitis

Pancreatitis • Nursing Interventions (continued) – Provide patient teaching and discharge planning concerning • Dietary regimen when oral intake permitted – High-carbohydrate, high-protein, low-fat diet – Eating small, frequent meals instead of 3 large ones – Avoid caffeine products – Eliminate alcohol – Maintain relaxed atmosphere after meals

Pancreatitis • Nursing Interventions (continued) – Recognition and reporting of signs of complications • • • Continued nausea and vomiting Abdominal distention with increased fullness Persistent weight loss Severe epigastric or back pain Frothy/foul-smelling bowel movements Irritability, confusion, persistent elevation of temperature (2 days)

Acute Pancreatitis • Measure all Intake and Output – Vomit, blood loss, etc. • Auscultate bowel sounds – Initially will diminish or absent • Weigh daily • Measure abdominal girth if ascites is suspected • Check oral and nasal mucosa for signs of dryness and cracking

Acute Pancreatitis – Electrolyte replacement – Reduction of pancreatic secretions • “resting the pancreas” • NPO halts pancreatic enzymes • NG tube reduces HCL in stomach • Administer histamine 2 blockers to further reduce acid • Nutritional support via TPN – Renal support – Surgical therapies – Complications prevention (pulmonary, cardiac, and renal

After the acute phase • Once subsided, BS will resume, abdominal pain will diminish, and patient should report feeling hungry – May resume eating – Clear liquids – Small carbs – No spicy foods or caffeinated beverages – No fat or high protein – May need antispasmotics, anticholinergics and antacids to reduce gastric and pancreatic juices

Complications • Necrotizing pancreatitis – Significantly increases morbidity & mortality – Usually found on CT with IV contrast • Pseudocysts – Suggested by persistent pain or continued high amylase levels (may be present for 4 -6 wks afterward) – Cyst may become infected, rupture, hemorrhage or obstruct adjacent structures • Asymptomatic, non-enlarging pseudocysts can be watched and followed with imaging • Symptomatic, rapidly enlarging or complicated pseudocysts need to be decompressed

Complications continued #2 • Infection – Many areas for concern: abscess, pancreatic necrosis, infected pseudocyst, cholangitis, and aspiration pneumonia -> SEPSIS may occur – If concerned, obtain cultures and start broad-spectrum antimicrobials (appropriate for bowel flora) – In the absence of fever or other clinical evidence for infection, prophylactic antibiotics is not indicated • Renal failure – Severe intravascular volume depletion or acute tubular necrosis may lead to ARF

Complications continued #3 • Pulmonary – Atelectasis, pleural effusion, pneumonia and ARDS can develop in severe cases • Other – Metabolic disturbances • hypocalcemia, hypomagnesemia, hyperglycemia – GI bleeds • Stress gastritis – Fistula formation

Long-term Sequelae • Chronic Pancreatitis – Characterized by chronic and progressive loss of pancreatic parenchyma – Both endocrine (DM) and exocrine (steatorrhea, azotorrhea) insufficiency develop when 80% to 90% of gland is destroyed – Pancreatic calcification (from intraductal calcium carbonate deposits) may be apparent on plain abdominal x-ray – Patients may require insulin, pancreatic enzyme replacement (Creon), and medium-chain triglycerides

Long-term Sequelae • Pseudocyst Formation – Collection of enzyme-rich pancreatic fluid and tissue debris arising within areas of necrosis – Result from the formation of granulation tissue within the pancreas – May be asymptomatic and resolve spontaneously – Treatment • Drainage • Resection • Indicated if they persist for more than 6 weeks, are enlarging, or are symptomatic

Prognosis • 85 -90% mild, self-limited – Usually resolves in 3 -7 days • 10 -15% severe requiring ICU admission – Mortality may approach 50% in severe cases

Long-term Sequelae • Pleural Fistulas and Pancreatic Ascities – Result from pancreatic fluid entering pleural space or abdomen – Treatment includes: • Repeated aspiration • Diuretics • Carbonic anhydrase inhibitors • Surgical resection

Chronic pancreatitis • Pathophys - irreversible parenchymal destruction leading to pancreatic dysfunction • • • Persistent, recurrent episodes of severe pain Anorexia, nausea Constipation, flatulence Steatorrhea Diabetes

Chronic pancreatitis • #1 - etiology is chronic Et. OH abuse (90%) • Gallstones • Hyperparathyroidism • Congenital malformation (pancreas divisum) • Idiopathic • MRCP of pancreas divisum

Evaluation • or normal amylase and lipase • Plain AXR / CT may show calcified pancreas • Pain management critical – Et. OH cessation may improve pain – Narcotic dependency is common

Complications • Exocrine insufficiency typically manifests as weight loss and steatorrhea – If steatorrhea present, a trypsinogen level < 10 is diagnostic for chronic pancreatitis – Manage with low-fat diet and pancreatic enzyme supplements (Pancrease, Creon) • Endocrine insufficiency may result from islet cell destruction which leads to diabetes

Conclusion • Pancreatitis is common – YOU WILL SEE IT!!! • 10 -15% are severe = ICU admission – Mortality may approach 50% in severe cases • These are the cases where knowing future complications would be great (ie finding a marker that correlates with severity…and that’s what the clinical researchers are attempting to do)