Nursing Care and Interventions with Diseases of the



























- Slides: 48

Nursing Care and Interventions with Diseases of the Liver, Gallbladder & Pancreas Keith Rischer RN, MA, CEN 1

Today’s Objectives… Ø Ø Ø Ø Review pathophysiology and systemic manifestations of the inflammatory response. Compare and contrast pathophysiology & manifestations of diseases of the liver, pancreas and gallbladder. Interpret abnormal laboratory test indicators of liver, pancreatic and gallbladder function. Identify the diagnostic tests, nursing priorities, and client education with diseases of the liver, pancreas and gallbladder. Analyze assessment data from clients with cirrhosis to determine nursing diagnoses and formulate a plan of care for clients with diseases of the liver, pancreas and gallbladder. Prioritize assessment based nursing care for clients experiencing chronic pancreatic or gall bladder disease. Integrate nutrition therapy in care of clients with hepatic, pancreatic or gallbladder disease. 2

Inflammatory Response Occurs in response to injury Ø Localized Ø Immediate Ø Beneficial Ø Appropriate level of response Ø Non Specific Ø 3

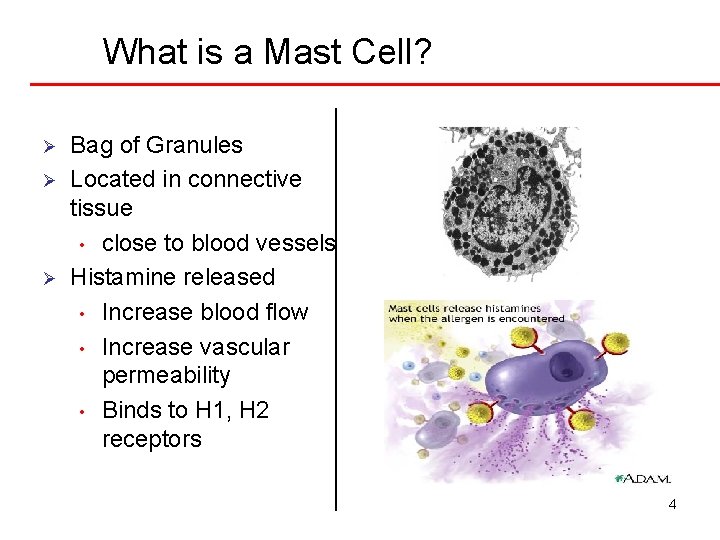
What is a Mast Cell? Ø Ø Ø Bag of Granules Located in connective tissue • close to blood vessels Histamine released • Increase blood flow • Increase vascular permeability • Binds to H 1, H 2 receptors 4

Causes Bacteria-viral Ø Trauma Ø Lacerations Ø Allergic response Ø Bites Ø Burns Ø 5

Purpose of inflammation Neutralizes and Dilutes Toxins Ø Removes necrotic materials Ø Provides an environment for healing Ø 6

Systemic Manifestations of Acute Inflammation Ø Fever/chills • Benefits ü Increased killing of microorganisms ü Increased phagocytosis by neutrophils ü Increased activity of interferon Leukocytosis Ø Plasma Proteins Ø 7

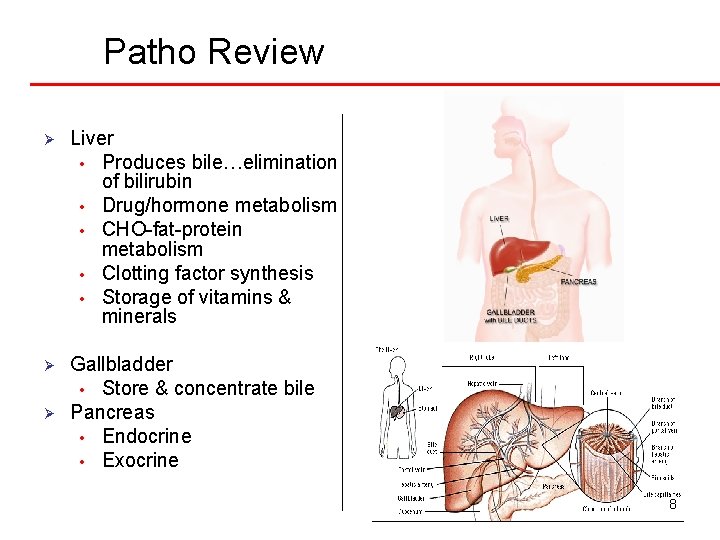
Patho Review Ø Liver • Produces bile…elimination of bilirubin • Drug/hormone metabolism • CHO-fat-protein metabolism • Clotting factor synthesis • Storage of vitamins & minerals Ø Gallbladder • Store & concentrate bile Pancreas • Endocrine • Exocrine Ø 8

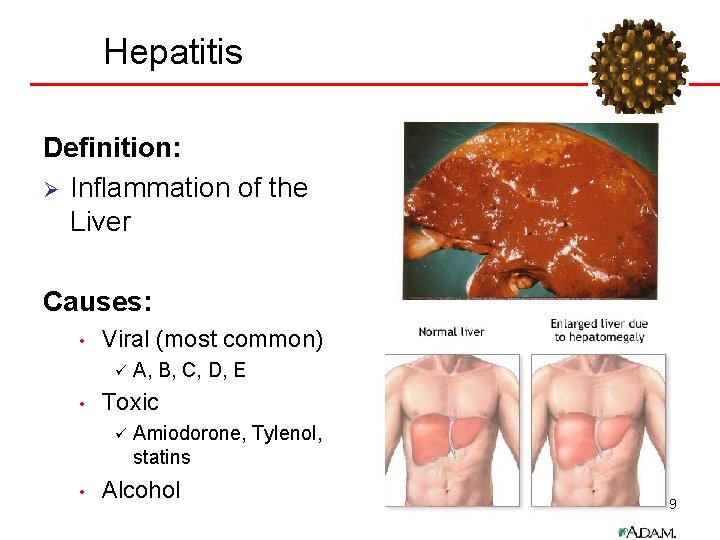
Hepatitis Definition: Ø Inflammation of the Liver Causes: • Viral (most common) ü • Toxic ü • A, B, C, D, E Amiodorone, Tylenol, statins Alcohol 9

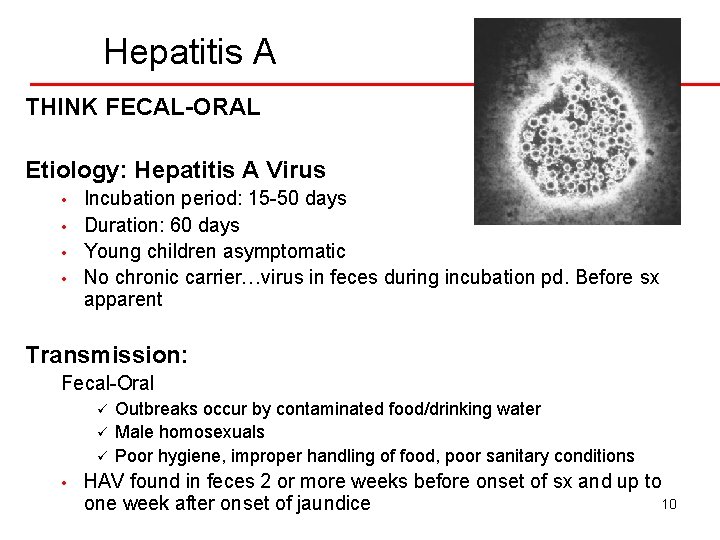
Hepatitis A THINK FECAL-ORAL Etiology: Hepatitis A Virus • • Incubation period: 15 -50 days Duration: 60 days Young children asymptomatic No chronic carrier…virus in feces during incubation pd. Before sx apparent Transmission: Fecal-Oral ü ü ü • Outbreaks occur by contaminated food/drinking water Male homosexuals Poor hygiene, improper handling of food, poor sanitary conditions HAV found in feces 2 or more weeks before onset of sx and up to 10 one week after onset of jaundice

Hepatitis A: Prevention • • • Good hygiene Water treatment Hepatitis A vaccine ü booster • 6 -12 mos after first dose Immunoglobulin before exposure or within 2 weeks after exposure ü protects about 2 months 11

Hepatitis B THINK BODY SECRETIONS-BLOOD Etiology: Hepatitis B Virus • • Incubation period: 48 -180 days (mean 56 -96) Chronic & carrier status Transmission • Exposure to infected blood, blood products or body fluids ü • Perinatal: mother to baby (10 -85% liklihood) ü • • 90% become chronic carrier… 25% mortality as adults Percutaneously (IV drug use, needle sticks) ü • Found in most body secretions Nurses at risk! STD-30% cases r/t heterosexual activity Major source of spread are healthy, chronic carriers 12

Hepatitis B: Prevention Hepatitis B vaccine • Ø Ø Ø series of 3; use of HBIG for post-exposure prophylaxis Screening of donor blood Use of disposable equipment Sterilization of non-disposable equipment Abstinence/condom use Needle exchange programs Use of standard precautions and PPE 13

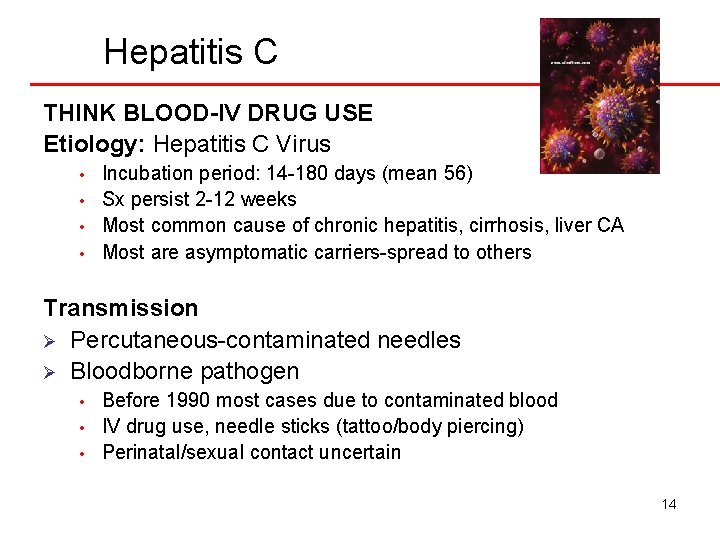
Hepatitis C THINK BLOOD-IV DRUG USE Etiology: Hepatitis C Virus • • Incubation period: 14 -180 days (mean 56) Sx persist 2 -12 weeks Most common cause of chronic hepatitis, cirrhosis, liver CA Most are asymptomatic carriers-spread to others Transmission Ø Percutaneous-contaminated needles Ø Bloodborne pathogen • • • Before 1990 most cases due to contaminated blood IV drug use, needle sticks (tattoo/body piercing) Perinatal/sexual contact uncertain 14

Hepatitis C: Prevention Screening of donor blood Ø Use of disposable equipment Ø Sterilization of non-disposable equipment Ø Abstinence/condom use Ø No vaccine or use of IG at this time Ø 15

Chronic Hepatitis Responsible for most cases of cirrhosis, liver CA • • HCV responsible for 80% cases Smolders over years…silently destroying liver cells Most asymptomatic but then develop… • • Malaise Easy fatigability Jaundice Hepatomegaly 16

Hepatitis-Cirrhosis: Laboratory Assessment AST-Aspartate aminotransferase Ø ALT-Alanine aminotransferase Ø ALP-Alkaline Phosphatase Ø Total bilirubin Ø Albumin Ø Ammonia Ø INR-Prothrombin time (PT) Ø 17

Hepatitis-Cirrhosis: Early Clinical Manifestations • • • Fatigue Significant change in weight Gastrointestinal symptoms Abdominal pain and liver tenderness Pruritus 18

Hepatitis-Cirrhosis: Late Clinical Manifestations • • • Jaundice and icterus Dry skin Rashes Petechiae, or ecchymoses (lesions) Peripheral dependent edema of the extremities and sacrum 19

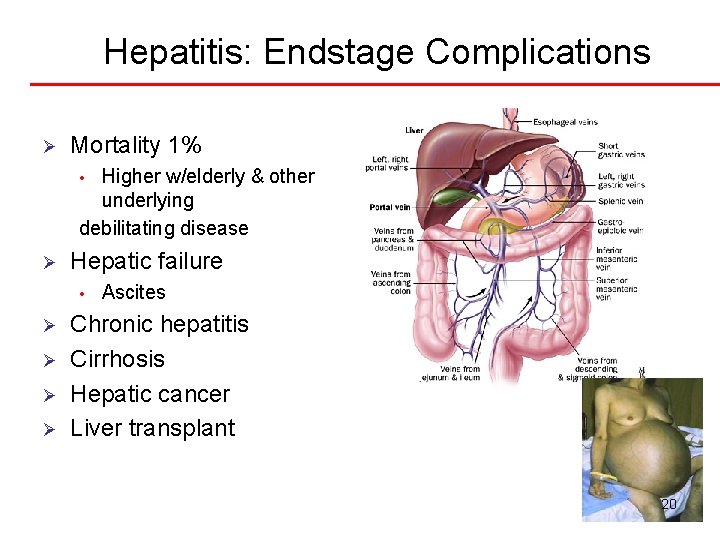
Hepatitis: Endstage Complications Ø Mortality 1% Higher w/elderly & other underlying debilitating disease • Ø Hepatic failure • Ø Ø Ascites Chronic hepatitis Cirrhosis Hepatic cancer Liver transplant 20

Hepatitis: Care Planning Priorities Ø Fatigue • • Physical rest Nutritional intake Sm. Frequent meals ü High carb-low fat ü Ø Ø Nausea Knowledge deficit • • Ø Avoid Tylenol, ETOH Diet Drug therapy • Interferon: SQ and po 21

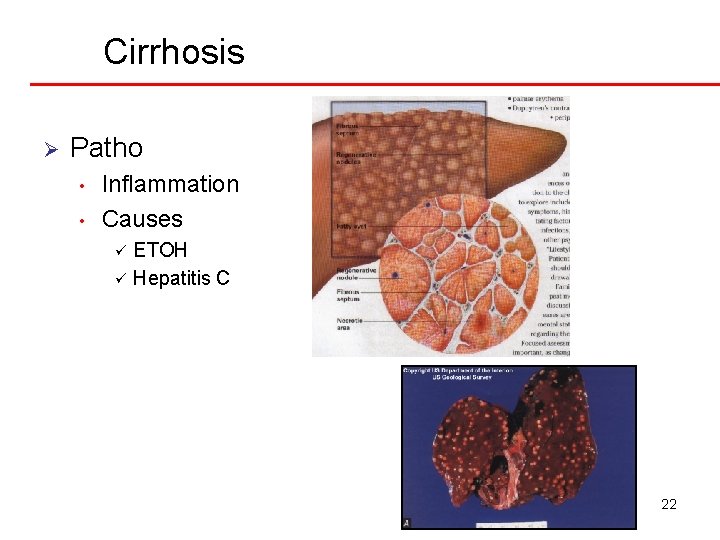
Cirrhosis Ø Patho • • Inflammation Causes ETOH ü Hepatitis C ü 22

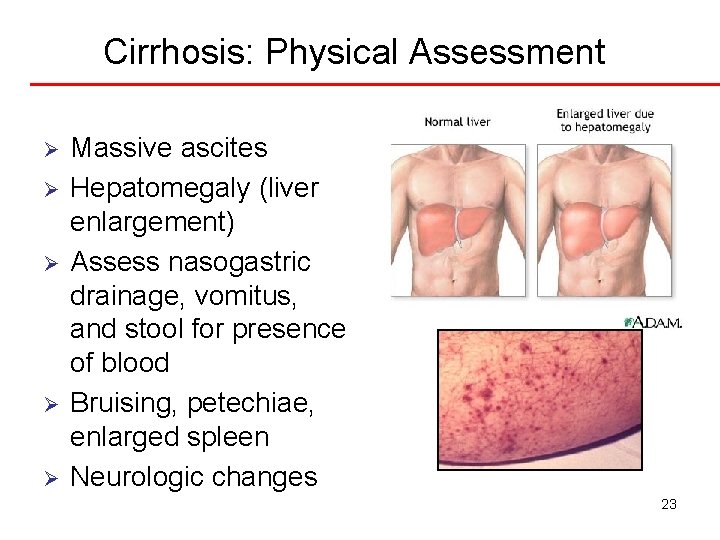
Cirrhosis: Physical Assessment Ø Ø Ø Massive ascites Hepatomegaly (liver enlargement) Assess nasogastric drainage, vomitus, and stool for presence of blood Bruising, petechiae, enlarged spleen Neurologic changes 23

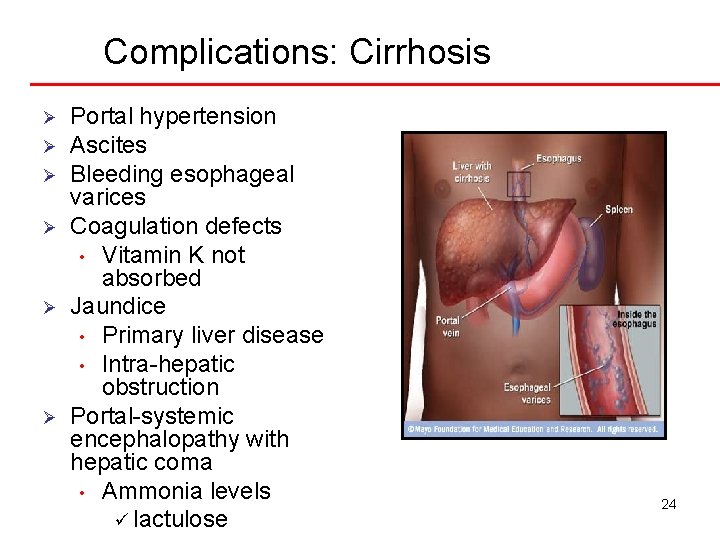
Complications: Cirrhosis Ø Ø Ø Portal hypertension Ascites Bleeding esophageal varices Coagulation defects • Vitamin K not absorbed Jaundice • Primary liver disease • Intra-hepatic obstruction Portal-systemic encephalopathy with hepatic coma • Ammonia levels ü lactulose 24

Cirrhosis: Care Planning Priorities • Excess fluid volume ü Diuretics ü Low sodium diet ü Paracentesis • • Risk for imbalanced nutrition Chronic pain Risk for impaired skin integrity Potential for hemorrhage 25

Cirrhosis: Nursing Priorities Ø Fluid-electrolyte management • • Ø Bleeding precautions • • • Ø Na+, K+, BUN, I&O Assess INR-PT-platelet-Hgb Monitor ortho’s Assess sx bleeding Neurologic assessment/monitoring • • • Assess ammonia levels Monitor LOC/orientation Fall risk 26

Liver Case Study Ø Ø Ø 67 yr male PMH: DMII, ETOH abuse, high cholesterol, PAF, CRI, Kidney CA 2001, cardiomyopathy CC: painless jaundice that started appx 4 weeks ago when wife noted eyes becoming yellow…did not seek medical care right away Became visibly jaundiced, developed dark urine, stools light in color, weak but no N-V-D or abd pain MD office: Bili of 25. Amiodorone and Lipitor DC’d. US abd done • Hepatic duct dilation w/further testing found to have pancreatic mass 27

Liver Case Study Ø Ø Ø VS: T-97. 8 P-65 R-20 BP-90/37 sats 96% 2 l n/c BMI 33. 6 Dx: • Ø CXR: cardiomegaly, pulmonary vascular congestion, mild CHF Assessment: • • • Conjuctival icterus, as well as skin Bibasilar crackles CV-no edema GI: abd distended, BS present Neuro: oriented x 3 but lethargic 28

Labs 29

Liver Case Study Nursing Priorities… Ø Medical Priorities… Ø GI Ø • • Ø Pancreatic malignancy Hepatitis/cirrhotic liver CV • • • Hypotension AFib Dilated cardiomyopathy 30

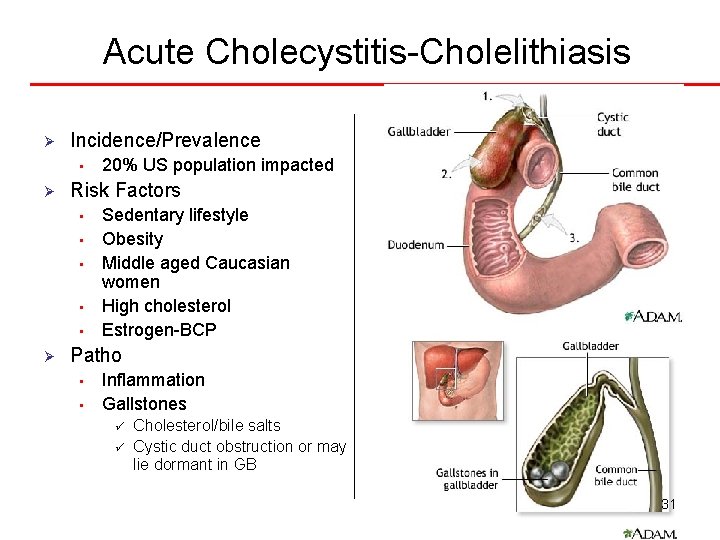
Acute Cholecystitis-Cholelithiasis Ø Incidence/Prevalence • Ø Risk Factors • • • Ø 20% US population impacted Sedentary lifestyle Obesity Middle aged Caucasian women High cholesterol Estrogen-BCP Patho • • Inflammation Gallstones ü ü Cholesterol/bile salts Cystic duct obstruction or may lie dormant in GB 31

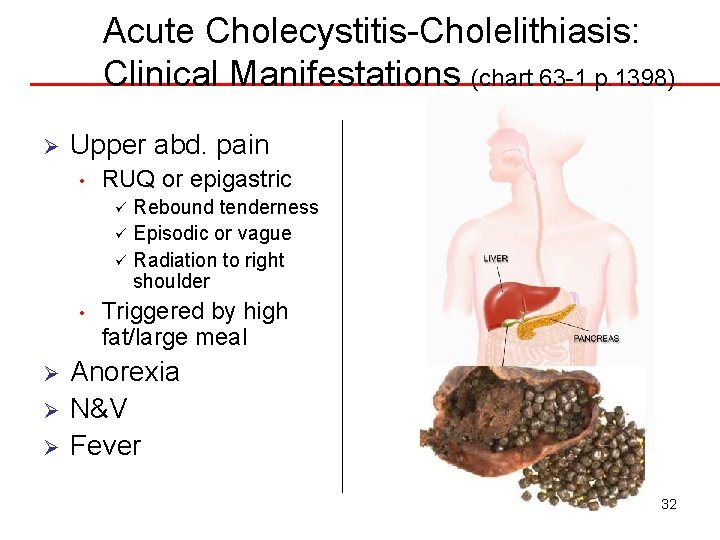
Acute Cholecystitis-Cholelithiasis: Clinical Manifestations (chart 63 -1 p. 1398) Ø Upper abd. pain • RUQ or epigastric Rebound tenderness ü Episodic or vague ü Radiation to right shoulder ü • Ø Ø Ø Triggered by high fat/large meal Anorexia N&V Fever 32

Acute Cholecystitis-Cholelithiasis Diagnostic & Interventions Ø Laboratory Findings • Ø Diagnosis • Ø WBC CT or US Interventions • Nonsurgical Diet ü Pharmocological ü • Surgical ü laparoscopic 33

Acute Cholecystitis-Cholelithiasis: Nursing Priorities Ø Ø Acute pain Impaired skin integrity Risk of infection Knowledge deficit • • Pain management Diet therapy Low-fat ü Smaller, more frequent meals ü • Wound/incision care ü • • Signs of infection Activity restrictions Follow-up care 34

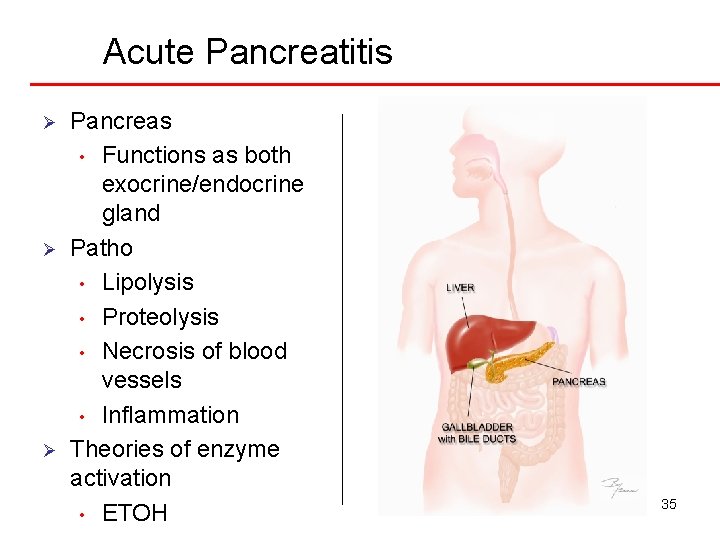
Acute Pancreatitis Ø Ø Ø Pancreas • Functions as both exocrine/endocrine gland Patho • Lipolysis • Proteolysis • Necrosis of blood vessels • Inflammation Theories of enzyme activation • ETOH 35

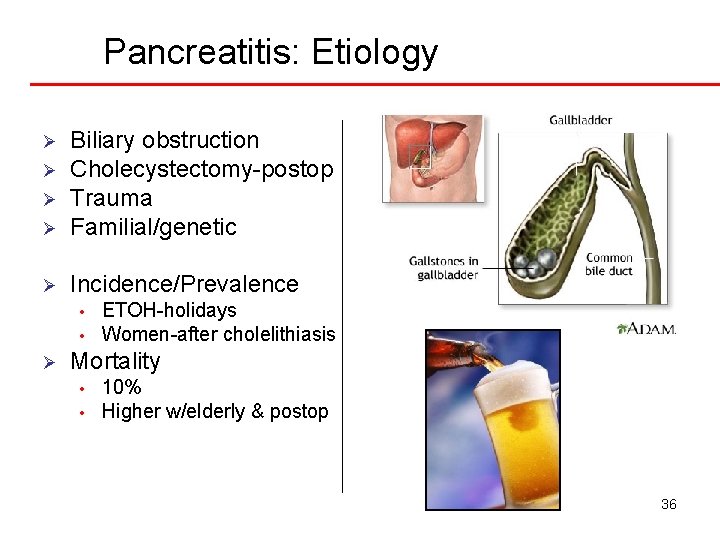
Pancreatitis: Etiology Ø Biliary obstruction Cholecystectomy-postop Trauma Familial/genetic Ø Incidence/Prevalence Ø Ø Ø • • Ø ETOH-holidays Women-after cholelithiasis Mortality • • 10% Higher w/elderly & postop 36

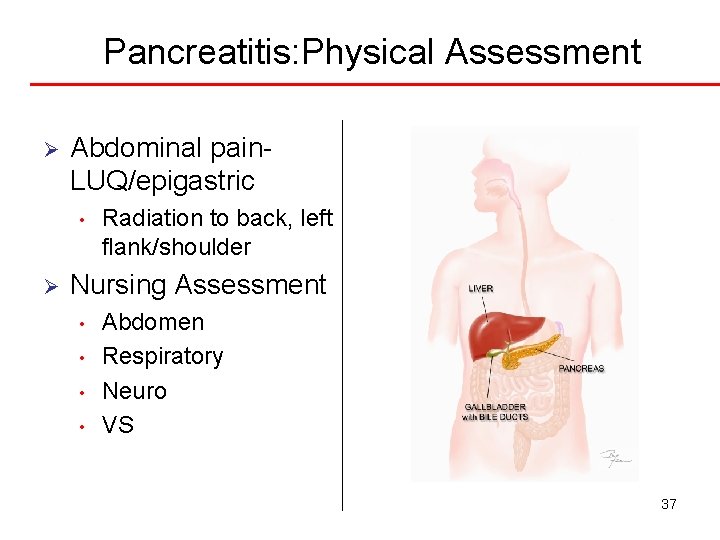
Pancreatitis: Physical Assessment Ø Abdominal pain. LUQ/epigastric • Ø Radiation to back, left flank/shoulder Nursing Assessment • • Abdomen Respiratory Neuro VS 37

Pancreatitis: Laboratory/Diagnostic Assessment Ø Lab • • • Ø Amylase Lipase Glucose Bilirubin WBC Radiographic • • CT MRI 38

Complications of Acute Pancreatitis p. 1404 Table 63 -2 Ø Ø Pancreatic infection Hemorrhage Hypovolemic or septic shock Respiratory • • • Ø Ø Ø Pleural effusion Pneumonia Acute Resp. Distress Syndrome (ARDS) Multisystem organ failure Disseminated intravascular coagulation Diabetes mellitus 39

Pancreatitis: Nursing Priorities Ø Acute Pain • Ø Imbalanced nutrition • • Ø PCA Nothing by mouth in early stages-7 -10 days Antiemetics for nausea and vomiting Total parenteral nutrition Small, frequent, moderate to high-carbohydrate, highprotein, low-fat meals Knowledge deficit • • • ETOH avoidance Recurrent abd pain Jaundice-clay colored stools-darkened urine 40

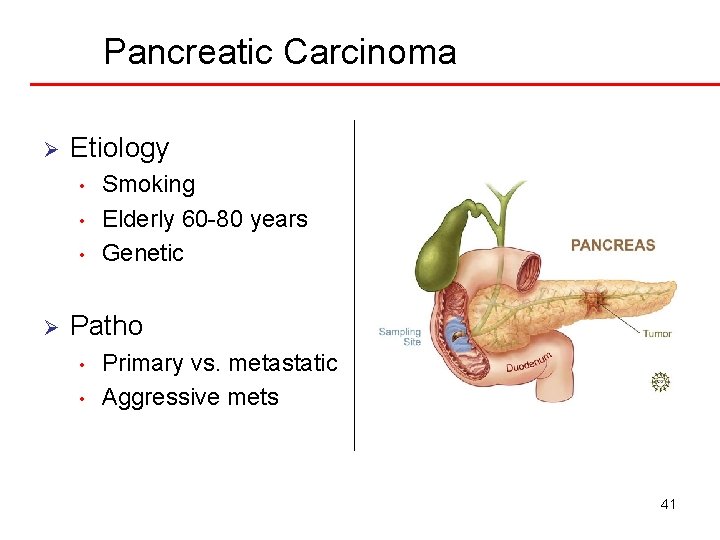
Pancreatic Carcinoma Ø Etiology • • • Ø Smoking Elderly 60 -80 years Genetic Patho • • Primary vs. metastatic Aggressive mets 41

Case Study Ø 22 year old female presents to the ED for c/o fatigue, N&V and feeling worn out the last several days with dark urine • • • Meds-BCP VS: T-100. 7 P-102 R-20 BP-110/74 sats 98% Assessment ü Mucous membranes tacky/dry ü Generalized abd pain w/tenderness in RUQ 42

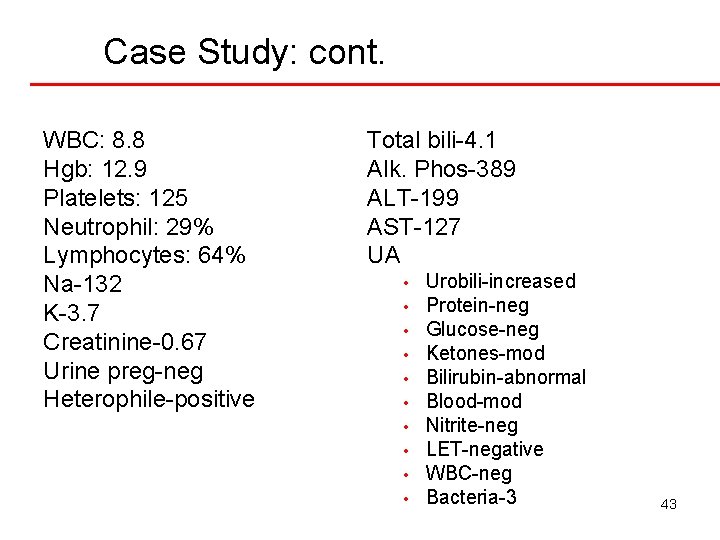
Case Study: cont. WBC: 8. 8 Hgb: 12. 9 Platelets: 125 Neutrophil: 29% Lymphocytes: 64% Na-132 K-3. 7 Creatinine-0. 67 Urine preg-neg Heterophile-positive Total bili-4. 1 Alk. Phos-389 ALT-199 AST-127 UA • • • Urobili-increased Protein-neg Glucose-neg Ketones-mod Bilirubin-abnormal Blood-mod Nitrite-neg LET-negative WBC-neg Bacteria-3 43

Case Study: cont. Ø Nursing priorities… Ø Nursing Interventions… 44

Case Study Ø Ø 40 yr male w/seizure disorder Chief complaint • • Altered mental status Vague abd pain Weakness Hypotension Ø Admission Labs • • • WBC-11, 000 Hgb-12. 2 Platelets-64, 000 Creatinine-2. 7 ALT-502 AST-219 Ammonia-68 Lipase-1947 Glucose-322 CT 45

Case Study: Later… Day of Admission Increasing lethargy, resp. distress Ø ABG Ø • • • p. H- 7. 38 CO 2 - 40 O 2 - 52 HCO 3 - 23 O 2 sats- 84 Fi. O 2 -100% vent…AC 12, PEEP +5 46

Case Study: Day 1 Ø Ø Ø CVP-21 VS-101. 2 -118 -24 -82/40 Labs • • WBC-12. 7 Platelets-56 Creatinine-. 7 ALT-243 AST-219 Lipase 523 ABG ü ü ü p. H-7. 25 CO 2 -52 O 2 -76 O 2 sats-92% Fi. O 2 -100% PEEP now +10 Ø Ø Ø Weight up 8 kg Non icteric IV Infusions • • • Insulin gtt Lasix gtt TPN-Lipids Fentanyl gtt Versed gtt Levophed gtt Neosynephrine gtt Vasopressin gtt Heparin gtt 47

Case Study: Day 2 Ø Ø Ø CVP-16 –weight up another 7. 5 kg…poor u/o VS-100. 5 -110 -24 -84/44 Labs • • • WBC-21. 5 Hgb-12. 5 Platelets-77 Creatinine-0. 9 ALT-143 AST-41 Ammonia-30 Lipase 114 ABG ü ü ü Ø Treatment Plan • • Ø CRRT IV abx-Cipro/Flagyl Hold Lasix gtt NG LCS Lactulose Wean vasoactive gtts as able Continue all previous gtts Pan cultures Nursing Priorities p. H-7. 11 CO 2 -78 O 2 -58 HCO 3 -24 O 2 sats-75% Vent-Fi. O 2 -100%, +15 48