ITE Review Must Know Cardio Angela Pugliese MD



































- Slides: 40

ITE Review Must Know Cardio Angela Pugliese MD Department of Emergency Medicine Henry Ford Hospital

Outline • • • Dysrhythmias ACS CHF/Cardiogenic Pulmonary Edema Cardiomyopathies DVT PE Pericardial Disorders Myocarditis/Pericarditis Aortic Dissection/AAA HTN Emergency/Urgency Valvular Heart Disease EKG Trivia

First and Foremost • KNOW ACLS • Meds that can be given through the ET tube - LEAN • • L - lidocaine E - epinephrine A – atropine N – nalaxone • Give 2 times normal dose diluted in normal saline

Dysrhythmias • Always assess hemodynamics……. • SHOCK THE UNSTABLE PATIENT

Dysrhythmias • SVT • Regular • Vagal maneuvers and adenosine • Afib • Irregularly irregular • Normal EF – CA/Beta blockers, Low EF – dig/amiodarone • Think anticoagulation • WPW • Short PR, delta wave • Narrow tx like SVT • Wide procainamide vs amiodarone • A-flutter • Rate control • MAT • Irregularly irregular, p-wave variation 3 types • Treat underlying cause ie COPD/CHF • Avoid beta blockers, think CA block or mag

Dysrhythmias • Sick Sinus Syndrome • Combination brady-tachy arrhythmia • Refer to cardiology for pacer • Vtach • 3 + PVCs with rate >120 • Amiodarone, lidocaine, procainamide • Torsades • Axis swinging from + to – in single lead • Mag and overdrive pacing • Vfib • ACLS

Dysrhythmias • AV Blocks • 1 st – prolonged PR, no treatment if no symptoms • 3 rd – AV dissociation, requires pacing • 2 nd • Mobitz 1 (Wenckebach) • Mobitz 2 – avoid atropine, needs pacing

ACS • Continuum • Angina – Unstable Angina – NSTEMI - STEMI • AMI – STEMI or CP with elevated markers • Treatment – • ASA, plavix, heparin, nitro • Thrombolytics – TPA • Give within 30 minutes if PCA > 60 min away • Complications • Vfib highest in first hour • LV failure • >20 % loss = pulm edema • > 40% loss = shock

CHF/Cardiogenic Pulm Edema • Left sided • Ischemic heart disease, HTN • Aortic/mitral valvular disease • Right sided • Left sided failure, pulm HTN, tricuspid/pulmonic disease • Signs and symptoms • SOB, ‘cardiac asthma’ • Pleural effusions • S 3, JVD, dependent edema

CHF/Cardiogenic Pulm Edema • CXR/Symptom progression • Stage 1 – cephalization, dyspnea • Stage 2 – interstitial edema (kerley B lines), dry cough • Stage 3 – alveolar edema (butterfly pattern), wet cough pink frothy sputum • Lab – BNP <100 excludes • Treatment • • OXYGEN BIPAP Afterload reduction, diuresis Think pressors for shock (dopamine, dobutamine)

Cardiomyopathies • Idiopathic Dilated – most common • Restrictive • Hypertrophic

Dilated Cardiomyopathies • All four chambers, systolic pump failure • Have signs of left and right failure • Afib most common dysrhythmia • Tx – vasodilators, diuretics

Restrictive Cardiomyopathies • Diastolic restrictive of ventricular filling • Mimics constrictive pericarditis • Right sided symptoms predominate • Exercise intolerance • Tx – diuretics, AVOID vasodilators

Hypertrophic Cardiomyopathy • • LVH without dilation (septum greater) 50% inherited DOE, syncope or pre-syncope with exertion Sudden death with exercise induced dysrhythmias • Tx • • Propanolol Avoid increasing myocardial contractility Septal myomectomy for severe cases Abx prophylaxis for dental procedures

DVT • Virchow’s Triad • Venostasis, hypercoagulability, vessel wall injury • Presentation • Unilateral pain, swelling and edema (>3 cm difference) • Diagnosis • Duplex US (repeat testing in 7 days) • Tx • Aimed at preventing PE • Anti-coagulation • Thrombolytics (vascular surgery consult

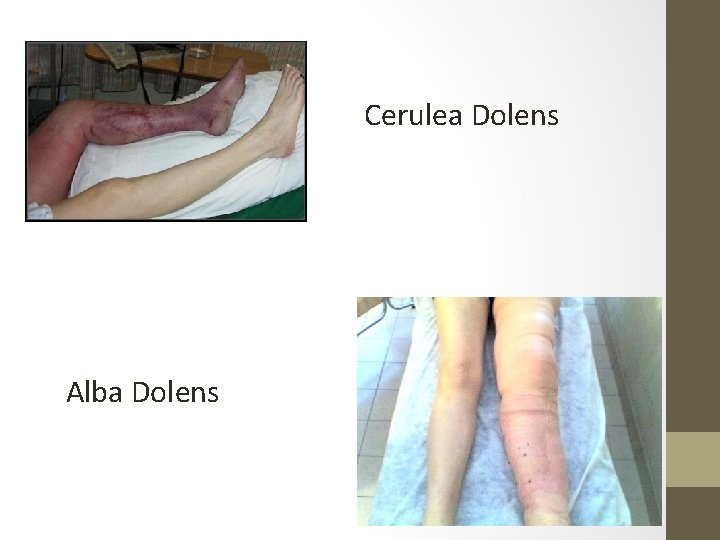
Cerulea Dolens Alba Dolens

Pulmonary Embolism • Presentation • Dyspnea • Classic triad – dyspnea, pleuritic CP or tachypnea • CXR • Dyspnea, hypoxia and normal are very suggestive • Diagnostics • EKG, d-dimer, V/Q, CT, Angiography • Tx – • Anticoagulation • Thrombolytics • Hemodynamic instability • TPA, 100 mg over 2 hours

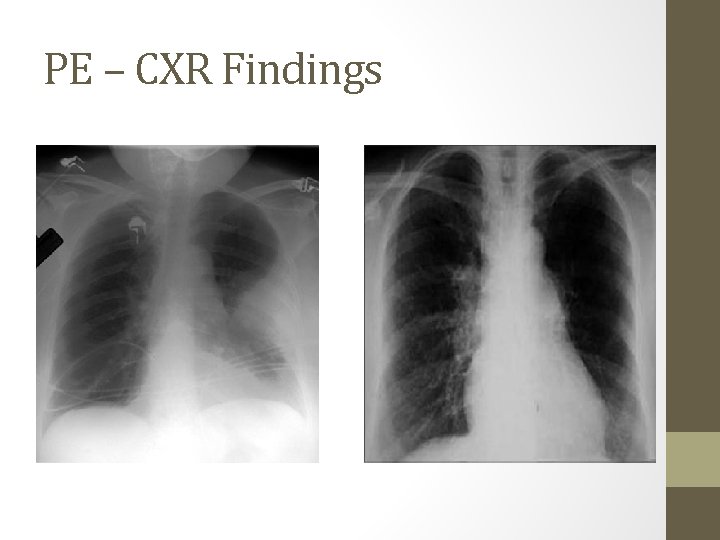
PE – CXR Findings

PE - Diagnostics • EKG – sinus tach most common • S 1, Q 3, T 3 • D-dimer – know Well’s, low risk pt only • V/Q • Limited in lung disease • Needs clinical context • Low-mod pretest prob with normal study 98% exculsion • CTA • 95% sensitive for segmental or large PE, 75% for subsegmental • Angiography • Gold standard

Pericardial Disorders • Pericarditis • Idiopathic and viral most common causes • Diagnosis • • • Hx – sharp precordial pain relieved by sitting up and leaning forward PE – friction rub EKG – diffuse concave ST elevation, PR depression Echo – to look for effusion BUN/Crt – look for uremia • Treatment • Outpatient NSAID for idiopathic/viral and reliable pts

Pericardial Disorders • Pericardial Tamponade • Becks Triad – hypotension, JVD, muffled heart tones • Tachycardia is earliest finding • Diagnosis • EKG – electrical alternans, low voltage • Echo – gold standard, large effusion, diastolic RV collapse • Treatment • Monitor, IV, O 2 • Aggressive volume resuscitation and pressors if needed • Cardio/CT surgery consult and pericardiocentesis (under US)

Myocarditis • Presentation • Range from non specific fatigue to florid CHF • Watch for tachycardia out of proportion to fever • Diagnosis • Echo – dilated chambers with diffuse or focal hypokinesis • Labs – elevated ESR, trop rise and fall slowly • Biopsy for definitive • Etiology • Viral most common cause • Treatment • Supportive, treat like CHF • Avoid immunosuppressives and NSAIDs • IVIG for Kawasaki

Endocarditis • Localized infection of endocardium with hallmark vegetation • Causative Organisms • Native valve – non-viridan strep • Prosthetic valve – coag-neg strep (<60 day post op) • IVDA – staph aureus (found on right, ie pulmonic) • Presentation • Fever most common finding • Signs of metastatic infection • • Roth spots Splinter hemorrhages Osler nodes – TENDER nodules on volar fingers Janeway lesions – non tender macules on fingers, palms, soles

Endocarditis • Diagnosis • Positive blood cultures • Duke criteria • Treatment • Native valve – ampicillin + gent or vanc + gent • Prosthetic – vanc + gent + rifampin

Duke Criteria • Major • Positive blood culture • Evidence of endocardial involvement (TEE) • Minor • • • Predisposition Fever Vascular and/or immunologic phenomenon Microbiology evidence Echo evidence • Need 2 major or 1 major with 3 minor or 5 minor

Endocarditis Prophylaxis • Needed for procedures with significant manipulation of infected tissue • Not needed for foley, intubation, routine dental cleaning • • • Prosthetic valve Hx of endocarditis Cyanotic congenital heart lesions Acquired valvular disease (ie rheumatic fever) Hypertrophic cardiomyopathy

Aortic Dissection • Males age 50 -70 • HTN most common risk factor • Presentation • pain • Classification – type A vs B • Definitive Testing – • TEE – unstable patients • CTA – may miss rapid moving flap • Treatment – • 10 -15 units of blood on standby with surgical consultation • Control HR and BP, esmolol first then nipride • Treat pain with IV narcotics

Aortic Dissection • EKG – • Usually abnormal • STEMI most common misdiagnosis (inferior) • CXR findings • Widened mediastinum • Right side • Tracheal deviation • Left side • Apical cap • Effusion • Depressed mainstem bronchus

Expanding/Ruptured AAA • > 95 % infrarenal • Males > 60 • Presentation • Thing middle age male with syncope or near syncope and lower abdominal or back pain • PE classic pulsatile abdominal mass • Diagnosis and Management • • Bedside echo IV, O 2, monitor 10 units of blood on standby Surgical consultation

HTN Emergency/Urgency • End Organ Damage • DBP > 115 • Arrest and lower BP rapidly, 30% in first hour • Asymptomatic pt discharge to follow up with PCP • Oral agents to lower BP over 24 -48 hours

Valvular Disorders

Mitral Valve Prolapse • Click murmur syndrome • High pitched late systolic murmur with mid-systolic click • Most common – 5 -10% of population • Presentation • Young women – palpitations • Elderly – syncope • Treatment • Only symptomatic pts • Beta blockers for CP or dysrhythmias • ASA or anticoagulation with hx TIA/stroke

Mitral Regurgitation • Acute • • Rupture chordae tendineae or papillary muscle after… Presents with fulminant CHF Apical systolic murmur Tx- hemodynamic support and CT surgery consult • Chronic • • Evolves slowly and usually coexists with mitral stenosis High pitched holosystolic murmur Afib in 75% of patients Abx prophylaxis

Aortic Stenosis • Etiology • <65 bicuspid valve • >65 calcification • Symptoms • Exertional dyspnea or syncope • Harsh crescendo-decrescendo murmur radiating to carotids • Treatment • Mild – d/c home avoid strenuous activity • CHF – admit, reduce preload/afterload • Refer all symptomatic patients for surgical therapy
EKG Trivia

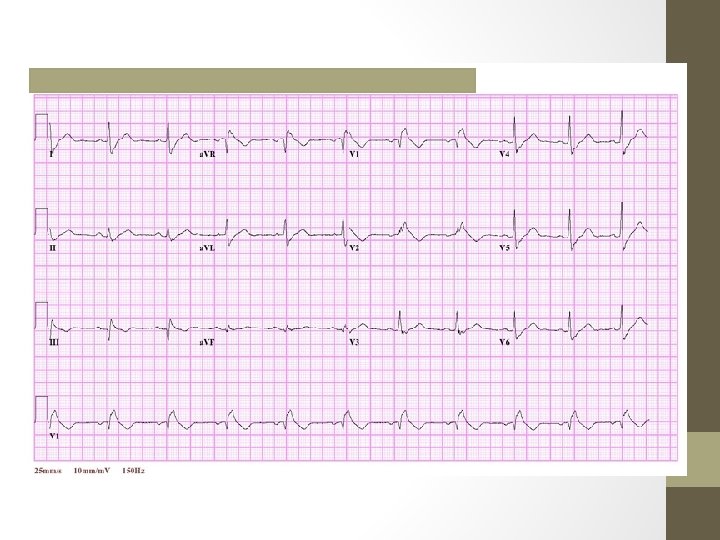
EKG & Electrolytes, etc. • • • Hypothermia = ‘J wave’ or osborn wave Sinus brady an afib w/out RVR Hypokalemia = Prolonged QT Also seen in hypomag Hyperkalemia = Peaked T’s (5. 5 -6. 5) Prolonged PR, flattened p’s, wide QRS (6. 5 -8) Sine wave, vfib, asystole (>8) Hypocalcemia = Prolonged QT

EKG & Electrolytes, etc • Hypercalcemia = • shortened ST and QT intervals • Narrow QRS • Digitalis = • Sagging ST, concave up • Treatment – multiple dose charcoal and FAB



The END