ASTHMA Dr Shreedhar Paudel 19 th March 2009





















































- Slides: 56

ASTHMA Dr. Shreedhar Paudel 19 th March, 2009

Asthma • ↑ed responsiveness of trachea and bronchi to various stimuli • Manifests by widespread narrowing of airways ↓ causing paroxysmal dyspnoea, wheezing or cough

Triggers • Aeroallergens such as house dust, mites, molds, industrial allergens • Smoke→ passive smoking & domestic smoke • Hydrocarbons • Drugs→ aspirin, NSAIDS

Pathophysiology • Edema & inflammation of mucous membrane lining the airways→ allergic & nonspecific stimuli→ spasm of bronchial smooth muscles ↓ airway close prematurely during expiration ↓ lungs are hyperinflated, ↓ elasticity, retention of carbondioxide & respiratory acidosis

Clinical Features • Begins with cold or spasmodic coughing (at night) • Dyspnoea • Prolonged expiration and wheezing • Profuse sweating • Cyanosis • Apprehension, restlessness, fatigue

Clinical Features contd…. . • Hyperresonance —air trapping • Severe obstruction → breath sounds become feeble (silent chest)—no wheezing which again appear if child starts to improve • Severe hypoxemia → cyanosis & cardiac arrythmia • Pulsus paradoxus– decrease in BP >10 mm. Hg with inspiration • Barrel shaped chest in some cases

Grading • Mild: --h/o cough + h/o past episodes --no restriction of activities—episodic treatment --CXR, blood count, lung function test. Normal --respond well to bronchodilators

Grading contd… • Moderate: --activities restricted --requires daily treatment --all features of asthma present --lung function test –severely impaired

Grading contd… • Severe: --Activities restricted --patient in severe distress --hospitalized management required --clinically very severe but on auscultation-- silent chest

Diagnosis • Recurrent episodes of coughing & wheezing • Aggravated or triggered by exercise, viral infection or inhaled allergens (highly suggestive) • Sometimes persistent coughing with no h/o wheezing

Investigations • Blood—eosinophilia • Sputum—eosinophilia ( not very effective) • Chest X-Ray --B/L & symmetric air trapping --patches of atelectasis due to mucus plugs --prominent pulmonary artery --bronchial cuffing (Edema)

Investigations contd…. . • Immunological test (confirmatory)→by exposing to allergens → risky • Lung function test FEV 1 is ↓ed in obstructive airway disease Gold Std Test– reversal of FEV 1 to near normal with administration of Salbutamol • Oxygen exercise test or running → exercise induced asthma

Differential Diagnosis • Airway obstruction due to --congenital malformation --Foreign body in the airway --Infectious bronchiolitis --cystic fibrosis --immunologic deficiency diseases --hypersensitive pneumonitis --Allergic bronchopulmonary aspergillosis

Management • Avoiding allergens, exposure to nonspecific irritants (tobacco, smoke, strong odors, ice cold drinks) • Improving bronchodilation • Reducing mediator induced inflammation

Drug therapy Mainstay of treatment to ensure • Full night sleeps • Clear chest in the morning • Normal physical activity, regular attendence at work

Drugs • Relievers (remove spasm) Salbutamol—drug of choice (2 mg oral dose 8 hrly) or (1 -2 puffs of 100 microgram/puff metered aerosol every 4 -6 hrly) --metered dose inhalers can be modified for use by infants by using spacer devices

Drugs contd… • Preventors Corticosteroids– reduces edema & also prevents edema ↓ ↓ PGs formation ↓Leukotrienes (bronchoconstrictors) ↓Ig. E levels

Preventor drugs contd… • Beclomethasone (nebuliser)--S/E—oral thrush • 8 puffs of a metered dose of Beclomethasone are equivalent to a dose of 7. 5 mg of prednisolone

Severe Asthma • Aminophylline IV drip • IV steroid • Ventillator • Antibiotics—only if infection exacerbates asthma

Exercise induced asthma • Most effectively prevented by inhalation of beta 2 agonist immediately before exercise • Use of a muffler or cold weather mask to warm & humidify air before inhalation is also effective


• 12 years old known case of asthmatic with treatment of Salbutamol and beclomethasone suddenly comes with distress and can not even read two sentences • On examination—chest is hyperinflated, can not hear air entry into lungs (silent chest)

Status Asthmaticus • Clinical diagnosis-- defined by increasingly severe asthma that is not responsive to drugs that are usually effective ↓ respiratory distress despite the administration of sympathomimetic drugs with or without theophylline ↓ admitted to hospital

Management • Oxygen with humidity—as patients are hypoxemic --usually needs 35 -50% oxygen to keep Pa. O 2 at normal • IV Fluids—up to twice the maintainence rate until urine flow is≥ 2 ml/kg/hr --afterwards at maintainence rate

Management contd… • Bronchodilators --Aminophylline 4 -7 mg/kg followed by 0. 7 mg/kg/hr • Buffer ( keep arterial p. H≥ 7. 30) --Na. HCO 3→ 1 -2 meq/kg iv initially

Management contd… • Corticosteroids Hydrocortisone IV --2 mg/kg/hr for 12 hrs thereafter→ 1 mg/kg/hr • Antibiotics Only if bacterial infection suspected

Some tips about Asthma • Measure FEV 1 to monitor progress of treatment (peak flow meter)→amount of air exhaled (crude way of measuring Peak flow—how far is the child able to put off the candle by blowing air through mouth) • Why does a child with asthma become symptomatic easily? ↑ oxygen requirement; small lung volume No collateral ventilation in children

Tips…. • Child with wheeze—give relievers & remove spasm • Child with severe asthma --nebuliser therapy --iv aminophylline --steroids • Child cyanosed --nebuliser --refer to ICU—ventillator --if leucocytosis, ↑fever→ceftriaxone


Bronchiectasis • Bronchiectasis is a suppurative disease that causes localized, irreversible dilation of part of the bronchial tree • classified as an obstructive lung disease, along with bronchitis and cystic fibrosis • Involved bronchi are dilated, inflamed, and easily collapsible, resulting in airflow obstruction and impaired clearance of secretions

Causes • Secondary to other diseases like --whooping cough --pneumonia --congenital → immotile cilia syndrome → secretions in bronchus → dilatation --cystic fibrosis • Aspiration of foreign body or mucus plug in the bronchus may occlude the bronchial lumen and cause segmental area of collapse

Clinical features(symptoms) • Repeated h/o cough-- though treated → Foul smelling, copious, mucopurulent expectoration • Fever • Flattening or retraction of ribs

Clinical features(signs) • Increased temperature • Clubbing • Bronchial breath sounds • Coarse crepitation cleared by coughing

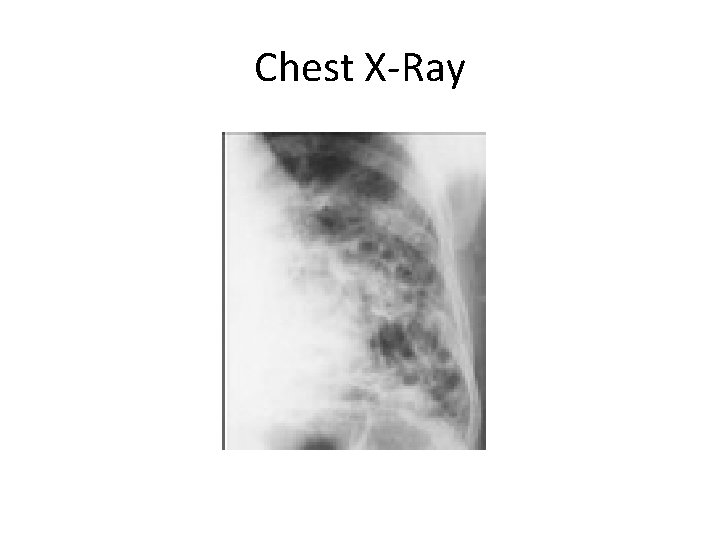
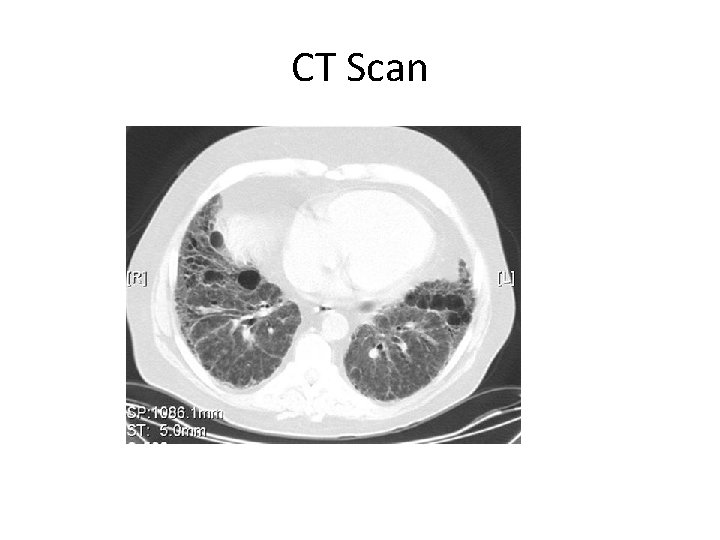
Investigations • Chest X-Ray --honeycomb appearance of involved lung • CT Scan --replaces bronchography --defining test for bronchiectasis --can show much damage & where the damage is

Chest X-Ray

CT Scan

Investigations…. . • • • Blood tests Sputum culture Lung function test Sweat test for cystic fibrosis Bronchoscopy if surgical intervention is possible

Management • The goals of treatment are to: --Treat any underlying conditions and respiratory infections --Help remove mucus from lungs --Prevent complications • Early diagnosis and treatment of bronchiectasis are important for preventing further damage

Management contd. . • • Antibiotics– for repeated chest infection Bronchodilators Corticosteroids-reduces inflammation Mucus thinners—acetylcysteine Expectorants Saline nasal washes Surgical management—if single lobe→lobectomy

• Next Topic…. .

Pleural Effusion • Pleural effusion is defined as an abnormal accumulation of fluid in the pleural space. • Excess fluid results from the disruption of the equilibrium that exists across pleural membranes

Types of fluids • Four types of fluids can accumulate in the pleural space: --serous fluid (hydrothorax) --Blood (hemothorax) --Chyle (chylothorax) --Pus (pyothorax or empyema)

Pathophysiology • The normal pleural space contains approximately 1 m. L of fluid --representing the balance between (1) hydrostatic and oncotic forces in the visceral and parietal pleural vessels (2) extensive lymphatic drainage • Pleural effusions result from disruption of this balance.

Causes • Transudative pleural effusions are often caused by abnormal lung pressure— CHFcommonest cause, Nephrotic syndrome • Exudative effusions form as a result of inflammation (irritation and swelling) of the pleura—pneumonia, tuberculosis, lung cancer and other lung infections

Symptoms • Shortness of breath • Chest pain—usually a sharp pain worse with cough or deep breaths • Cough, fever • Hiccups • Rapid breathing • Sometimes no symptoms at all

Signs • Inspection—decreased movement on affected side, asymmetric expansion on affected side (hoover sign) • Palpation—decreased vocal fremitus • Percussion– dull • Auscultation—inaudible breath sounds --bronchial breath sound --pleural friction rub

Diagnosis • Aspiration of fluid—biochemical analysis --cytological analysis ↓ exudate or transudate • Chest X-Ray—homogeneous radio-opaque shadow --Mediastinal shift --seen only with massive effusions (usually >1000 m. L) • Ultrasound


Treatment • Directed at --removing the fluid --preventing its re-accumulation --addressing the underlying cause of the fluid buildup • Therapeutic thoracocentesis -- if the fluid collection is large and causing pressure, shortness of breath, or other breathing problems, such as low oxygen levels • Treatment of the underlying cause of the effusion then becomes the goal

Possible complications • Collapse – as lung is surrounded by a fluid collection for a long time • Empyema -- Pleural fluid that becomes infected may turn into an abscess • Pneumothorax – complication of thoracentesis procedure • Rare cases require surgery to remove the collection

Some clinical cases • A mother brings her 9 months old baby to ER with the complain of fever and fast breathing for 3 days. – On examination- temperature is 102 degree F, RR is 65/min, sub-costal indrawing is present, dull on percussion over right chest but no abnormal sound heard on auscultation. – What is your provisional diagnosis? – What should be your next step?

Cases…. • 1 and ½ yr old M child presented in the middle of the night with noisy breathing --parents were afraid & it increased when child was excited O/E—running nose --100 F temp --no chest indrawing --non toxic --RR not increased

Cases… • Two years old child presented in ER with increased respiartory rate and Increased temperature, looks toxic and there is drooling of saliva from the mouth. What is the diagnosis?

Cases…. . • 6/12 yrs, M child presented in the month of January with --noisy breathing --wheeze( with chest indrawing) --100 F temp --past h/o running nose for few days -- very irritable --↑ RR On examination --B/L Ronchi & crepetations

Cases…. • 12 years old known case of asthmatic with treatment of Salbutamol and beclomethasone suddenly comes with distress and can not even read two sentences • On examination—chest is hyperinflated, can not hear air entry into lungs (silent chest)

Next Class • Assessment exam for respiratory disorders in children