Emergency Medical Responder First on Scene TENTH EDITION






























































- Slides: 69

Emergency Medical Responder First on Scene TENTH EDITION CHAPTER 12 Obtaining a Medical History and Vital Signs Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Media Directory Slide 49 Blood Pressure Assessment Video Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

OBTAINING A MEDICAL HISTORY Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Obtaining a Medical History • Medical history ▪ Previous medical conditions and events for patient Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Obtaining a Medical History • Signs ▪ Something you can see and observe about patient • Pale skin • Rapid pulse • Open wound to chest ▪ All are obvious. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Figure 12. 1 history. Get down at eye level with your patient and make good eye contact as you begin your medical Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Obtaining a Medical History • Symptom ▪ Something patient feels or may complain about • Can be obvious or very subtle • Pain, nausea common symptoms Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Table 12. 1 Common Signs and Symptoms Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Obtaining a Medical History • Interviewing Your Patient ▪ An alert patient is the best source of information. ▪ Chief complaint • Ask questions slowly and clearly. • Allow time for patient to process and respond. • Listen carefully. • Document important details. continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Obtaining a Medical History • Interviewing Your Patient ▪ Establish a good rapport. • • • Introduction Consent Patient's name Patient's age Chief complaint continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Obtaining a Medical History • Interviewing Your Patient ▪ SAMPLE history tool • • • Signs/symptoms Allergies Medications Past pertinent medical history Last oral intake Events leading to the illness or injury continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Obtaining a Medical History • Interviewing Your Patient ▪ OPQRST is the most commonly used for assessment of pain or discomfort. • • • Onset Provocation Quality Region/Radiate Severity Time Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Obtaining a Medical History • Additional Sources of Information ▪ ▪ Family members Bystanders First responders Medical identification jewelry Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Figure 12. 2 Consider using bystanders or family members when your patient is unresponsive or unable to provide a medical history on his own. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Think About It • You become suddenly ill and a medical provider begins asking you personal medical history questions. What would make you more likely to be honest and forthright with answers? • How could you apply this answer to your own assessment practices? continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Think About It • How would you handle questions such as: ▪ Have you been drinking? ▪ Have you taken any drugs that are not prescribed for you? ▪ Is there a chance you could be pregnant? Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

VITAL SIGNS Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • • • Respiration Pulse Blood pressure Skin signs Pupils Perfusion Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Mental status ▪ Level Of Consciousness (LOC) or level of responsiveness evaluated using AVPU scale. • • Alert Verbal, responsive to verbal stimuli Pain, responsive only to painful stimuli Unresponsive, unconscious, or completely unresponsive Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Baseline vital signs ▪ First set of vital signs obtained • Trending ▪ Comparing multiple sets of vital signs from same patient over time • Careful analysis of vital signs can alert you to current or developing problems. • Do not rush to a conclusion too soon. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Respiration ▪ Act or process of breathing in (inhaling) and out (exhaling) • Evaluate ▪ Rate, depth, sound, ease • Work of breathing ▪ Effort that patient must exert to breathe Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Table 12. 2 Assessment Signs—Respirations Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Respiratory assessment ▪ Grasp patient's wrist as if you were going to count pulse rate. ▪ Hold his arm firmly against his upper abdomen. ▪ Observe abdomen and chest move in and out. ▪ Listen for abnormal sounds. continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Respiratory assessment ▪ Count number of breaths patient takes in 15 or 30 seconds. ▪ While counting respirations, note depth and ease of breathing. ▪ Document rate, depth, ease. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Table 12. 3 Respiration Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Figure 12. 3 a Emergency Medical Responder assessing respirations on a supine patient. continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Figure 12. 3 b Emergency Medical Responder assessing respirations on a seated patient. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Pulse ▪ Remote heartbeat ▪ Gives insight into circulatory status of patient ▪ Good pulse indicates blood is moving well throughout body. continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Pulse ▪ Central pulses • Carotid, femoral ▪ Peripheral pulses • Brachial, radial, pedal Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Figure 12. 4 Locating the carotid pulse point in the neck. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

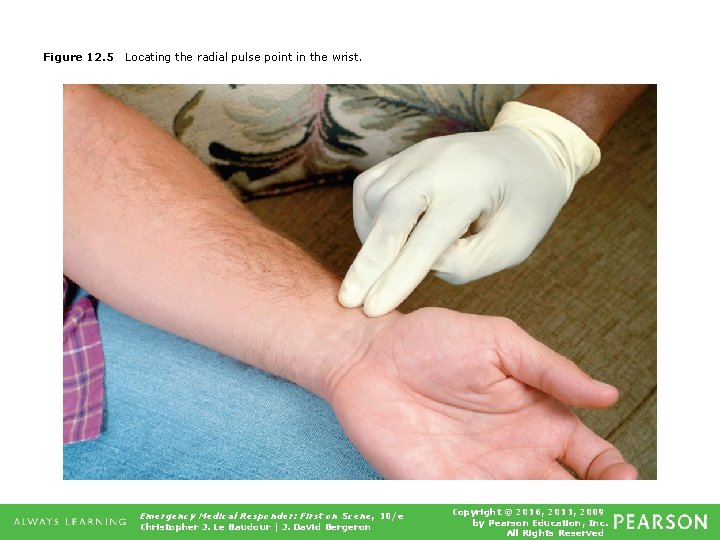
Figure 12. 5 Locating the radial pulse point in the wrist. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Pulse ▪ Assess for rate, strength, rhythm. • Responsive patient ▪ Check radial pulse. • Unresponsive patient ▪ Check carotid pulse. • Radial pulse may not be detectable if blood pressure is too low or if there is extremity injury. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

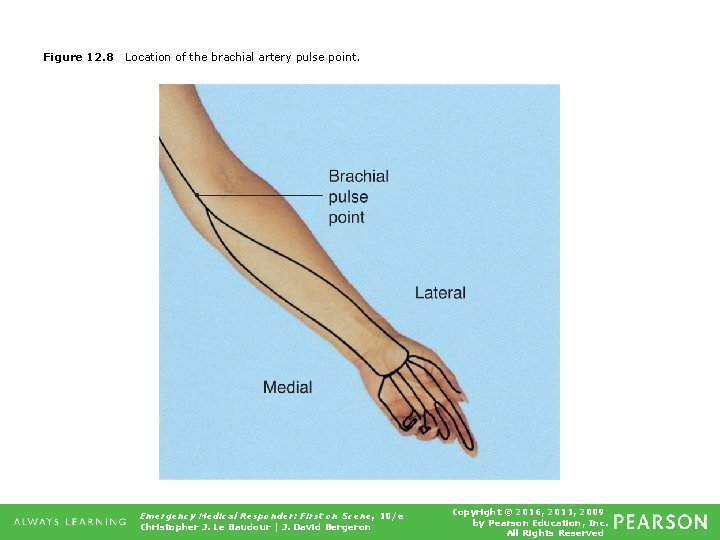
Vital Signs • Pulse rate for adults is between 60 and 100 beats per minute. ▪ Tachycardia • Rate above 100 ▪ Bradycardia • Rate below 60 • Pulse point for infants under the age of one year is brachial pulse in upper arm. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

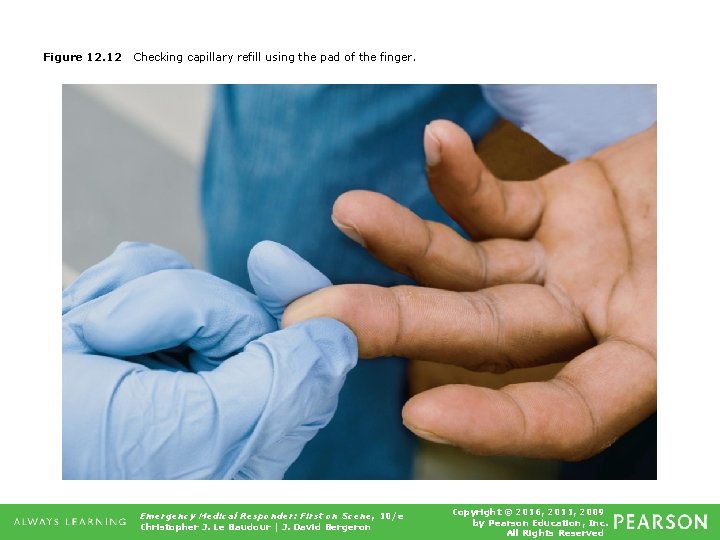
Vital Signs • Capillary refill ▪ Time it takes for capillaries to refill after being blanched ▪ Select appropriate finger or toe. ▪ Using thumb and index finger, squeeze pad of finger or toe from both sides. Observe pad as it blanches. continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Capillary refill ▪ Quickly release pressure. • Observe color return to pad. • Document findings. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Figure 12. 12 Checking capillary refill using the pad of the finger. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Blood pressure ▪ Measurement of pressure of blood against walls of arteries, both when heart beats and when it is at rest ▪ Systolic • Pressure within arteries when heart beats • Contraction phase of heart continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Blood pressure ▪ Diastolic • Pressure that remains in arteries when heart is at rest • Resting phase of heart Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

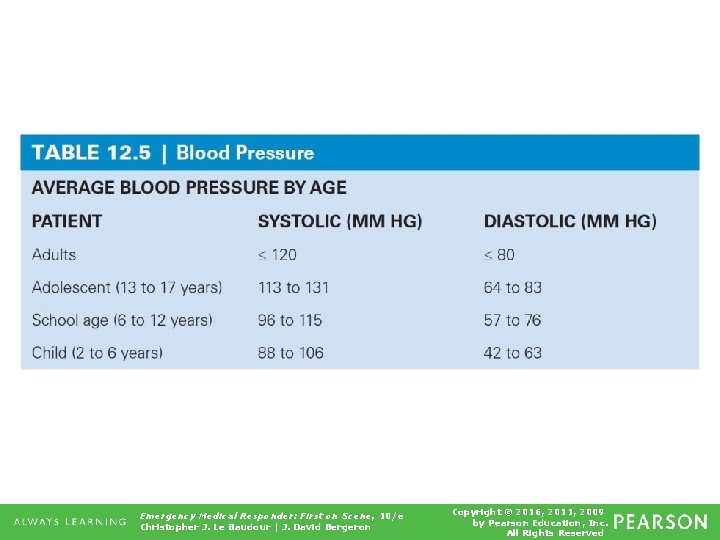
Vital Signs • Reading of 120/80 considered normal blood pressure • Take several readings to identify changes in status. • Systolic reading above 140 considered high blood pressure (hypertension) Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Table 12. 5 Blood Pressure Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Blood Pressure Assessment Video Click on the screenshot to view a video on the topic of taking blood pressure. Back to Directory Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Auscultation ▪ Listening to internal sounds of the body with a stethoscope ▪ Have patient sit or lie down. ▪ Remove clothing on arm. ▪ Support arm at level of heart. ▪ Select correct-size blood pressure cuff. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Figure 12. 6 Adjust the earpieces of the stethoscope so they point forward slightly, into the ear canal. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Figure 12. 7 a Proper position for taking a blood pressure while seated. continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Figure 12. 7 b Obtaining a blood pressure on a supine patient. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Figure 12. 8 Location of the brachial artery pulse point. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

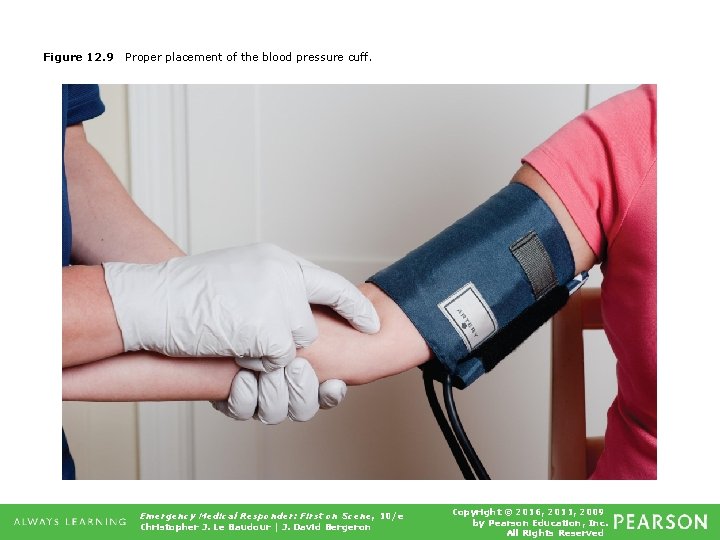
Figure 12. 9 Proper placement of the blood pressure cuff. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Figure 12. 10 Pulse sounds will be heard through the stethoscope between the systolic and diastolic readings. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Auscultation ▪ Let rest of air out of cuff quickly. ▪ Record time, arm used, position of person, pressure readings. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

12. 1. 1 Place the cuff snugly around the upper arm. continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

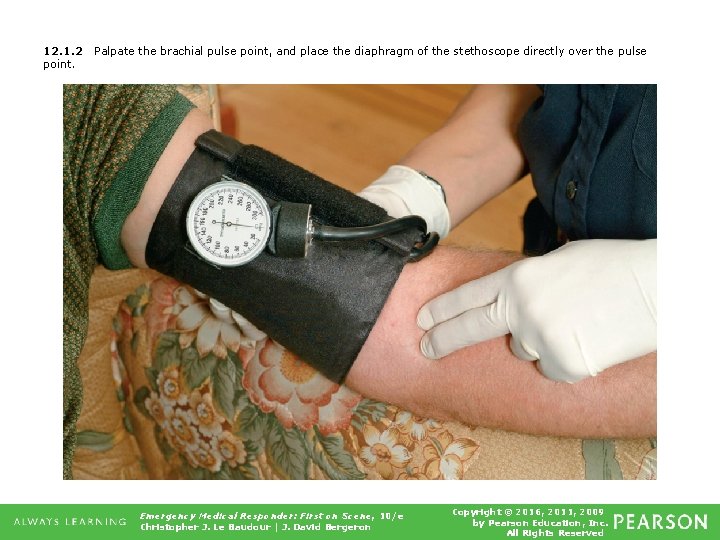
12. 1. 2 point. Palpate the brachial pulse point, and place the diaphragm of the stethoscope directly over the pulse Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Auscultation ▪ Close valve and inflate cuff. • 180 mm. Hg adult • 120 mm. Hg child ▪ Open valve slowly to release pressure from cuff. ▪ Listen carefully as you watch needle move. ▪ Let cuff continue to deflate. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

12. 1. 3 Quickly inflate the cuff then release the pressure to obtain the blood pressure readings. continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

12. 1. 4 Document your readings along with the time. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Palpation ▪ Using one's hands to touch or feel the body. ▪ Not very accurate method ▪ One reading • Approximate systolic pressure ▪ Used when there is too much noise, making it difficult to hear via stethoscope Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

12. 2. 1 Place the cuff and locate the radial pulse prior to inflating the cuff. continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

12. 2. 2 Inflate the cuff until you feel the radial pulse go away. continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

12. 2. 3 Continue inflating the cuff to approximately 30 mm Hg beyond where the pulse went away. continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

12. 2. 4 Release the pressure in the cuff and note the pressure on the gauge when the radial pulse returns. This will be the approximate systolic pressure. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Skin signs ▪ Evaluate color, temperature, and moisture. ▪ Pale or cyanotic ▪ Flushed ▪ Jaundiced continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Skin signs ▪ Examples of skin signs • • Pink, warm, dry (PWD) Pale, cool, moist Flushed, hot, dry Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Table 12. 6 Skin Signs Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Figure 12. 11 Use the back of an ungloved hand to assess skin temperature and moisture. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Evaluate skin color in dark-skinned patients ▪ ▪ Oral mucosa Conjunctiva Nail beds Palms continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Pupils ▪ Note general condition. ▪ Identify any obvious injury or deformity. ▪ Ensure both pupils are round and same size. ▪ Note reaction to changes in light. • Constriction with sudden introduction of light • Dilation when light to pupil is blocked continued on next slide Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Vital Signs • Pupils ▪ PERL stands for: • • Pupils Equal Reactive Light Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Table 12. 7 Pupils Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

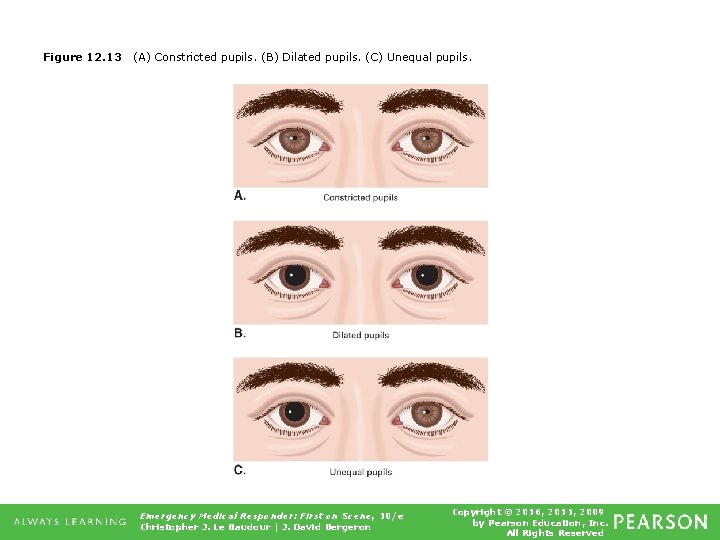
Figure 12. 13 (A) Constricted pupils. (B) Dilated pupils. (C) Unequal pupils. Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved

Think About It • Could vital signs ever be considered unreliable? • What does "treat the patient, not the device" mean and why is this especially important to remember when working with automated or electronic vital sign equipment? Emergency Medical Responder: First on Scene, 10/e Christopher J. Le Baudour | J. David Bergeron Copyright © 2016, 2011, 2009 by Pearson Education, Inc. All Rights Reserved