Activated Clotting Time Applications Therapeutics and Technologies Marcia

























































- Slides: 72

Activated Clotting Time Applications, Therapeutics and Technologies Marcia L. Zucker, Ph. D. Director of Clinical Support Response Biomedical Corporation mzucker@responsebio. com ITC Educational Services, Edison, NJ


There was…. . • The Lee-White clotting time – Add blood to glass tube, shake • No activator • Manual – Place in heat block – Examine for clot every 30 seconds • Very slow • Subjective clot detection

Time goes on…

1966 - Hattersley • Activated Clotting Time – Add blood to glass tube with dirt, shake • Diatomaceous earth activator • Still manual – Place in heat block – Visual clot detection • Subjective clot detection

Particulate Contact Activation • Initiation of intrinsic coagulation cascade – Factor XII (Hageman factor) – Prekallikrein (Fletcher factor) • Shortens contact activation period • Proposed as both screening assay for coagulation defects and for heparin monitoring • Critical fibrin clot endpoint

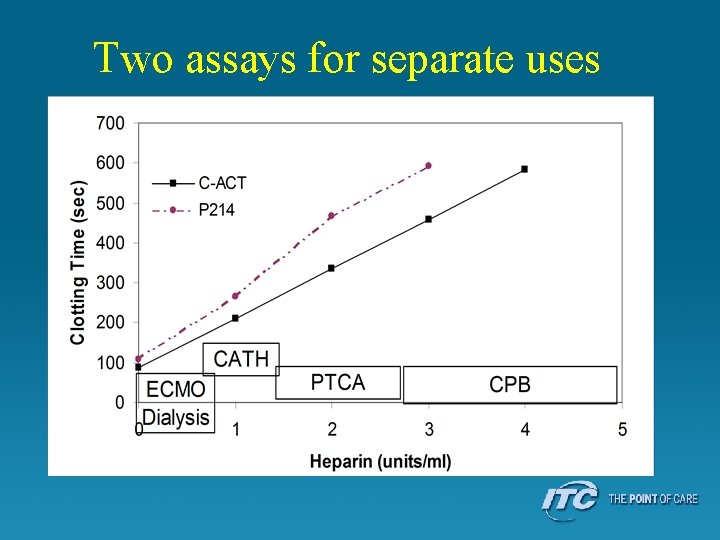
Semi - Automation - 1969 • HEMOCHRONOMETER – Later - HEMOCHRON – Add blood to tube, shake • Manual sample treatment – Place in test well • Automated heating • Objective fibrin clot detection – two different activators • CA 510 (later FTCA 510) – diatomaceous earth – P 214 glass bead

Mechanical Detection • Magnet in tube, detector in instrument • Upon fibrin clot formation, magnet is deflected • Clotting time displayed

Two assays for separate uses

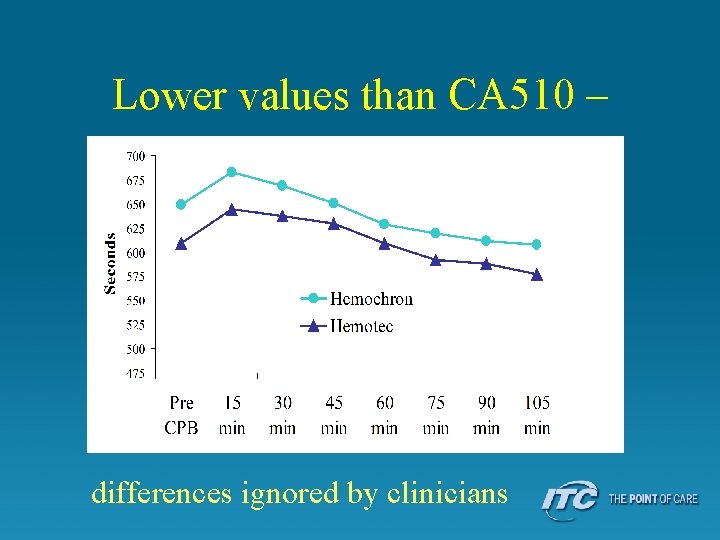
1980’s • Hemo. Tec ACT (later Medtronics ACTII) – Add blood to dual cartridge • Liquid kaolin activator – Place in instrument • Automated mixing – Objective clot detection • • Flag moves up and down As fibrin forms, motion slows Mechanical clot detection Instrument displays clotting time

Lower values than CA 510 – differences ignored by clinicians

1980’s - ACT Differences • Reported in literature >20 years – Clinical evaluations of Hemochron - mid 1970’s – By 1981 – • poor correlation between ACT and heparin level – By 1988 • Hemochron and Hemo. Tec clinically different • Early ’ 80’s to Present – Improved clinical outcome with ACT use • Reviewed: Draft NACB Laboratory medicine practice guideline for point of care coagulation testing – http: //www. nacb. org/lmpg/poct_LMPG_draft_PDF. stm

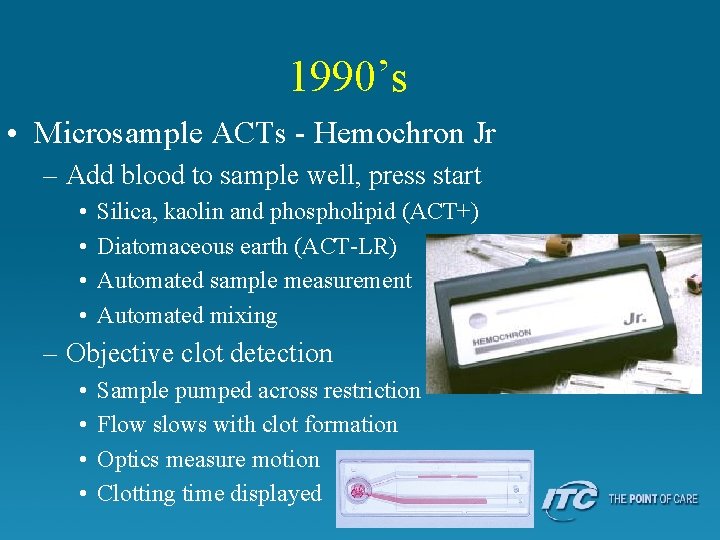
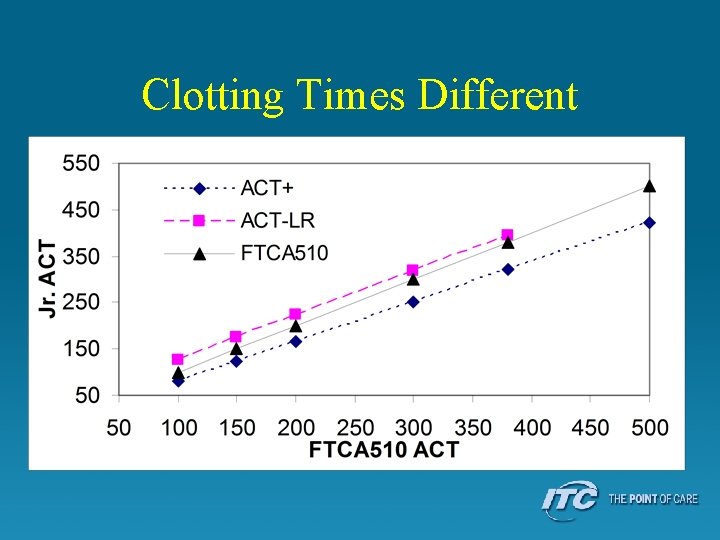
1990’s • Microsample ACTs - Hemochron Jr – Add blood to sample well, press start • • Silica, kaolin and phospholipid (ACT+) Diatomaceous earth (ACT-LR) Automated sample measurement Automated mixing – Objective clot detection • • Sample pumped across restriction Flow slows with clot formation Optics measure motion Clotting time displayed

Clotting Times Different

2000 • Abbott - i-STAT – Add blood to cartride, press start • Diatomaceous earth or kaolin – Insert into instrument • Automated mixing – No clot detection • Synthetic thrombin substrate • Electro-active compound formed and detected amperometrically • “Clotting time” reported

Clotting Times Likely Different • i-STAT ACT Package Insert – Used to monitor moderate- and high-level heparin – Prewarmed vs. non-prewarmed calibration modes – Good correlation with Hemochron (Celite below) • Intercept varied by site (+4 to -73 sec) • Slope range 0. 85 – 1. 19 – Few publications • All show wide scatter vs Hemochron or Medtronics

Today • • Hemochron Response Hemochron Signature Elite Medtronics ACT Plus Medtronics HMS+ Helena Actalyke XL / Mini Gem PCL Abbott i-STAT

Activated Clotting Time ic ns tri In Extrinsic Pathway ay thw Pa AC T Common Pathway CLOT

Why do we use an ACT? • Maintain Balance – Bleeding Thrombosis • Point of Care – Immediate turn around – Rapidly adjust anticoagulant dosing as needed • Heparin – half life varies by patient – Dose required varies by patient – Potency varies by lot • Direct thrombin inhibitors – very short half life – Require immediate intervention – No antidote available

NACB Guidelines • National Academy of Clinical Biochemistry • Evidence Based Guidelines for POC Testing – http: //www. nacb. org/lmpg/poct_lmpg_draft. stm • Chapter 4 – Coagulation Testing • Caveats: – Assume all systems equally safe / effective / precise – Correlation studies excluded – Few good outcome trials

NACB Guidelines • Is there evidence of improved clinical outcome using ACT testing? In cardiovascular surgery? • Is there evidence for optimal target times to be used with ACT monitoring? – Strongly recommend ACT monitoring of heparin anticoagulation and neutralization in cardiac surgery. – (Class A, Level I at least one randomized controlled trial, Level II– 1 small randomized controlled trials, non-randomized controlled trials). – Insufficient evidence to recommend specific target times for use during cardiovascular surgery. – (Class I – conflicting evidence across clinical trials).

NACB Guidelines • Is there evidence of improved clinical outcome using ACT testing? In interventional cardiology? • Is there evidence for optimal target times to be used with ACT monitoring? – Strongly recommend ACT monitoring of heparin anticoagulation in interventional cardiology. – (Class A, Level II– 1 - small randomized controlled trials, nonrandomized controlled trials, Level II-2 – Case controlled analytic studies from more than one center or research group). – Recommend target times specific to ACT system • Targets differ if specific platelet inhibitors are used concurrently with heparin.

NACB Guidelines • Target Times: – Without intravenous platelet inhibitors: • >250 seconds using the Medtronics ACTII • >300 seconds using the HEMOCHRON FTCA 510 tube – (Class B – Level II– 1 - small randomized controlled trials, nonrandomized controlled trials, Level II-2 – Case controlled analytic studies from more than one center or research group). – With the intravenous platelet inhibitors: • abciximab or eptifibatide: – 200 -300 seconds • tirofiban: – 250 – 300 » (Class B – Level I- at least one randomized controlled trial).

NACB Guidelines • Is there evidence of improved clinical outcome using ACT testing? In ECMO? • Is there evidence for optimal target times to be used with ACT monitoring? – Extra. Corporeal Membrane Oxygenation – Strongly recommend ACT monitoring to control heparin anticoagulation during ECMO. – (Class A – Level III – opinions of respected authorities based on clinical experience, descriptive studies or reports of expert committees). – Target times for ECMO based on the ACT system. – (Class B – Level III – opinions of respected authorities based on clinical experience, descriptive studies or reports of expert committees).

NACB Guidelines • Is there evidence of improved clinical outcome using ACT testing? In other applications (e. g. vascular surgery, intravenous heparin therapy, dialysis, neuroradiology, etc. )? • Is there evidence for optimal target times to be used with ACT monitoring? – There is insufficient evidence to recommend for or against ACT monitoring in applications other than cardiovascular surgery, interventional cardiology or extracorporeal oxygenation. – (Class I).

ACT - Clinical Applications • Essential - outcome studies show evidence – Cardiac surgery – Percutaneous coronary intervention (PCI) – ECMO / (Dialysis) • Common – insufficient evidence for “essential” – Critical care – Interventional radiology – Electrophysiology – Vascular surgery

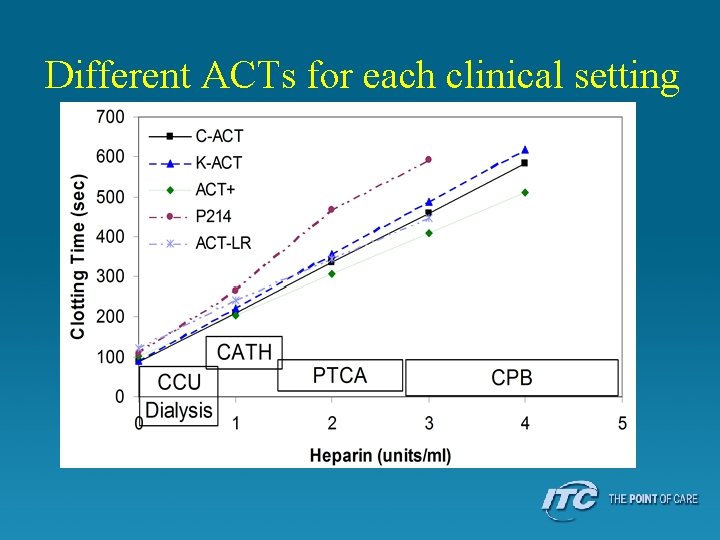
Different ACTs for each clinical setting

Clinical Applications • Essential – Cardiac surgery – Percutaneous coronary intervention (PCI) – ECMO / (Dialysis) • Common – Critical care – Interventional radiology – Electrophysiology – Vascular surgery

• Benefits Monitoring - ACT – Industry Standard Since 1970 s – Recommended as 1 o method in Am. SECT guidelines – ACT improves outcome in CPB, PCI • NACB draft LMPG for POC coagulation – Easy to run • Disadvantages – Each system yields different numbers – Most sensitive to hypothermia and hemodilution – Little or no correlation to heparin level • especially true for pediatric patients

When to choose which ACT? • Different pharmaceutical interventions – Antifibrinolytics – Novel anticoagulants • Different patient populations – Especially pediatric patients • Different monitoring preferences – Heparin Level – Need for specialty assays • Dosing • Fibrinogen

Pharmaceutical Intervention • Amicar or Tranexamic Acid – No effect on standard celite ACT – Continued debate on efficacy • Multiple reports of reduction in post-operative blood loss and reduced transfusion requirements • Aprotinin – Significant elevation of Celite ACT – Two dosing regimens – Patient size independent • Full Hammersmith – 2 x 106 KIU loading dose; 2 x 106 KIU pump prime; 0. 5 x 106 KIU/hr infusion • Half Hammersmith – 1 x 106 KIU loading dose; 1 x 106 KIU pump prime; 0. 25 x 106 KIU/hr infusion

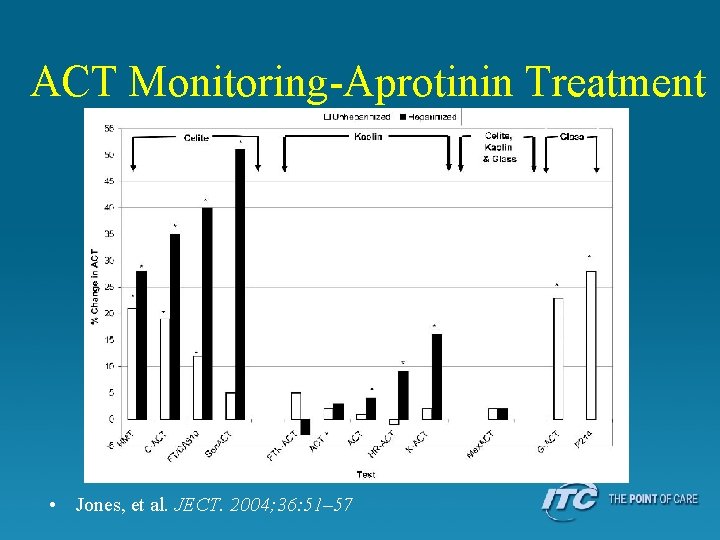
ACT Monitoring-Aprotinin Treatment • Celite® ACT • HEMOCHRON FTCA 510; Actalyke C-ACT; i-STAT ACTCelite – Not recommended • Still used with target times of >750 seconds • Kaolin ACT • HEMOCHRON FTKACT; Actalyke K-ACT; i-STAT ACTKaolin; Medtronics HR-ACT – Unaffected by moderate doses of aprotinin • Used with target times of > 480 seconds • Combination ACT reagents • HEMOCHRON Jr ACT+; Actalyke MAX-ACT; GEM PCL ACT – Unaffected by ALL doses of aprotinin • Used with target times of > 400 seconds

ACT Monitoring-Aprotinin Treatment • Jones, et al. JECT. 2004; 36: 51– 57

Novel Pharmaceuticals • None FDA approved for cardiac surgery • Direct thrombin inhibitors (DTIs) – Used if patient at risk for HIT • Heparin induced thrombocytopenia • “Heparin allergy” – Argatroban – Refludan – Angiomax

ACT Monitoring - DTIs • Argatroban – Synthetic analog of L-arginine • Reversible binding to thrombin – PCI monitoring: ACT 300 – 450 • Papers state standard ACT targets for CPB • Refludan – Recombinant hirudin • Irreversible inhibition of thrombin – Routine monitoring with a. PTT • No recent reports in CPB • Original studies used ECT - No longer available

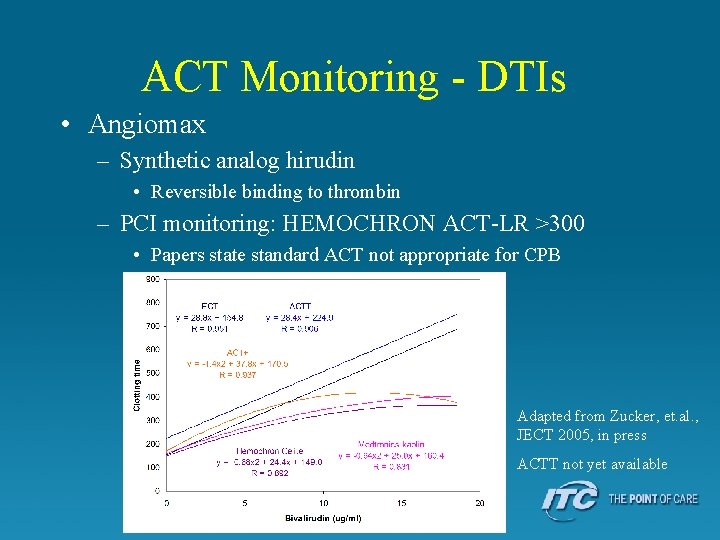
ACT Monitoring - DTIs • Angiomax – Synthetic analog hirudin • Reversible binding to thrombin – PCI monitoring: HEMOCHRON ACT-LR >300 • Papers state standard ACT not appropriate for CPB Adapted from Zucker, et. al. , JECT 2005, in press ACTT not yet available

Patient populations • Pediatric Patients are NOT little adults – Reports of both shorter and longer heparin half life • Pediatric Patients are NOT all the same – In neonates, coagulation factor levels confound dilutional effects – Once patient exceeds 2 years of age, only dilutional effects need to be considered • These can be very important • Test volume is critical

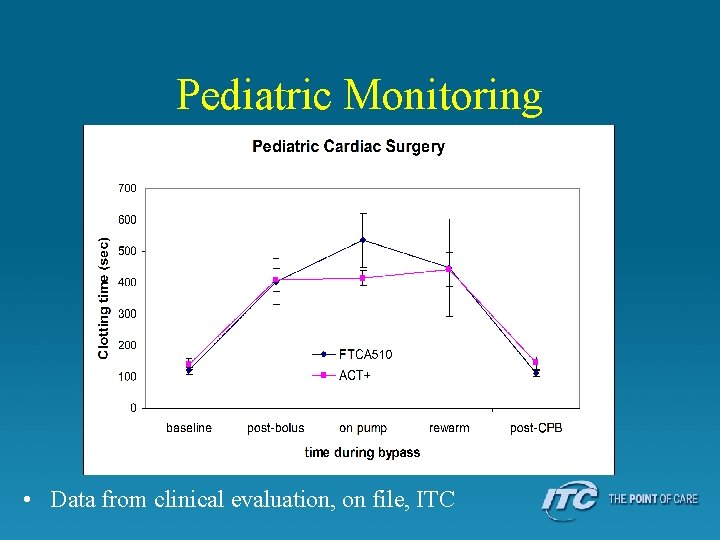
Pediatric Monitoring • Data from clinical evaluation, on file, ITC

Monitoring - Heparin Level • Benefits – Measures concentration, not activity – Correlates with laboratory standards • Disadvantages – Each system yields different numbers • apples and oranges do not compare – Correlation to anticoagulation status is still disputed – Target for neonate, pediatric and adult patients may differ

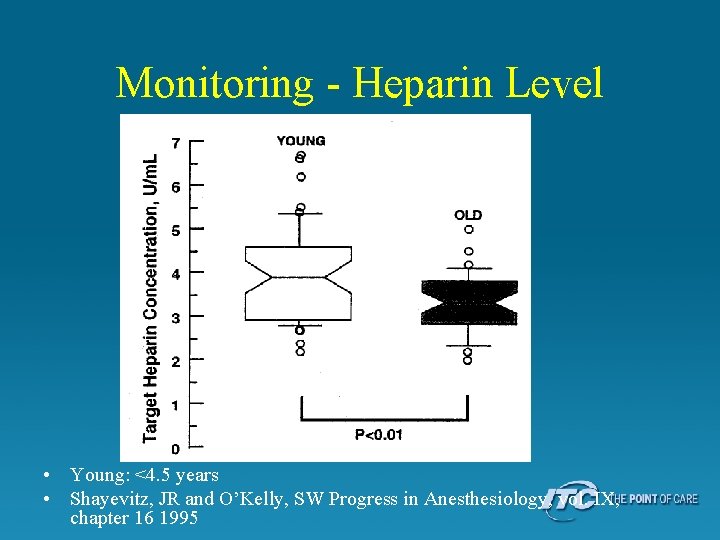
Monitoring - Heparin Level • Young: <4. 5 years • Shayevitz, JR and O’Kelly, SW Progress in Anesthesiology, vol. IX, chapter 16 1995

Monitoring - Heparin Level • αXa / αIIa Activity - laboratory only, impractical • Not available with microsample systems • Medtronic Hepcon HMS – Indirect measure of protamine reversible heparin activity • Thromboplastin based • HEMOCHRON PRT – ACT based protamine titration • HEMOCHRON Hi. TT – unaffected by hemodilution, hypothermia – insensitive to aprotinin • Thrombin Time based • Correlates with αXa and αIIa activity

Heparin Monitoring Dilemma ACT Heparin Level Which Value Determines Response?

More reasons for selecting a system • Heparin and Protamine Dose Optimization – In vitro dosing systems • Not available on microsample systems • Hemochron Rx. Dx – Heparin Response Time (HRT) – Protamine Response Time (PRT) – PDAO • HMS – HDR – HPT

Heparin Dose Optimization • Traditional dosing regimens recommend fixed drug doses by body weight. – Regimen does not account for patients whose response to heparin is different than the average “normal” patient. • Patients differ in their response to heparin; may be resistant or sensitive to heparin • Can represent 20 - 40% of patient population • Response can vary up to 12 fold between patients

Protamine Dose Optimization • Minimize protamine dose – Reduce time for infusion – Avoid protamine related adverse events • • hypotension shock bleeding platelet dysfunction

Clinical Benefits • Individualize heparin dose • Reduce blood products needed for post-operative transfusions – i. e. red blood cells, platelets, fresh frozen plasma and cryoprecipitate Jobes DR, et al. 1995. J Thorac Cardiovasc Surg 110: 36 -45 • Reduced potential for protamine reaction – Protamine reduced by average of 30% – Zucker ML. , et al. 1997. J Extra-Corp Tech. 29: 176 -180. • Reduced incidence of return to OR for bleeding

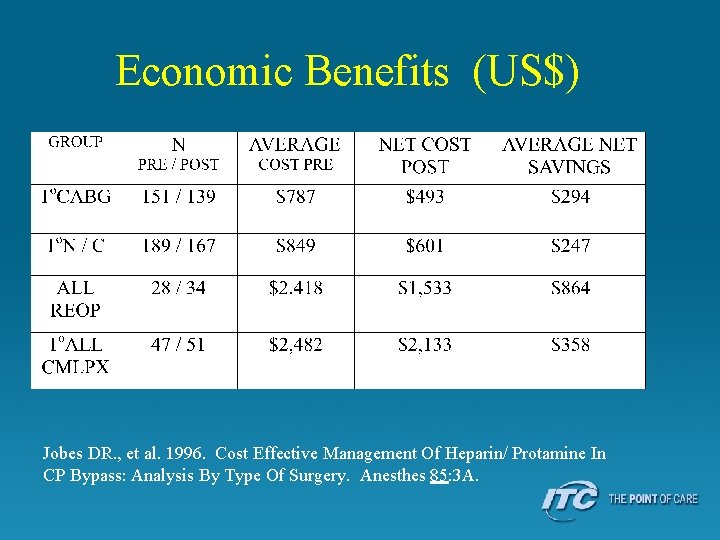
Economic Benefits (US$) Jobes DR. , et al. 1996. Cost Effective Management Of Heparin/ Protamine In CP Bypass: Analysis By Type Of Surgery. Anesthes 85: 3 A.

Heparin neutralization verification • Test Options – ACT - global indicator of coagulation • PDAO /ACT – protamine titration – HEMOCHRON Response • Heparinase ACT – enzymatic confirmation – Medtronics ACTPlus – Thrombin time – highly sensitive to heparin • TT/HNTT – protamine titration – HEMOCHRON Response – a. PTT - intrinsic pathway – HEMOCHRON tube systems – HEMOCHRON microsample systems

Clinical Applications • Essential – Cardiac surgery – Percutaneous coronary intervention (PCI) – ECMO / (Dialysis) • Common – Critical care – Interventional radiology – Electrophysiology – Vascular surgery

Procedures • Diagnostic – Catheterization • locate and map vessel blockage(s) • determine need for interventional procedures – Electrophysiology • Interventional – Balloon angioplasty – Atherectomy (roto-rooter) – Stent placement

Diagnostic – Low dose heparin • Catheterization and Electrophysiology – 2500 - 5000 unit bolus dose – frequently not monitored – if monitored – • ACT » HEMOCHRON FTCA 510; HEMOCHRON Jr ACT-LR; Medtronics LR-ACT: Actalyke C-ACT; GEM PCL ACT-LR – Targets ~ 200 seconds • a. PTT

Interventional • Angioplasty, Atherectomy, Stent placement • HEMOCHRON FTCA 510; HEMOCHRON Jr ACTLR; Medtronics LR-ACT or HR-ACT: Actalyke CACT, MAX-ACT; GEM PCL ACT-LR; i-STAT ACTCelite – 10, 000 unit bolus dose or – 2 - 2. 5 mg/kg – target ACT 300 - 350 seconds • Target must be reduced if Reo. Pro Used – Reo. Pro is one of 3 “GPIIb/IIIa” Inhibitors • GPIIb/IIIa receptor critical in platelet aggregation

Novel Pharmaceuticals • Platelet Inhibitors – Oral • Aspirin • Plavix – Parenteral • Reo. Pro • Integrilin • Aggrastat • Low Molecular Weight Heparins (LMWH) – None FDA approved for interventional cardiology – Lovenox – Fragmin

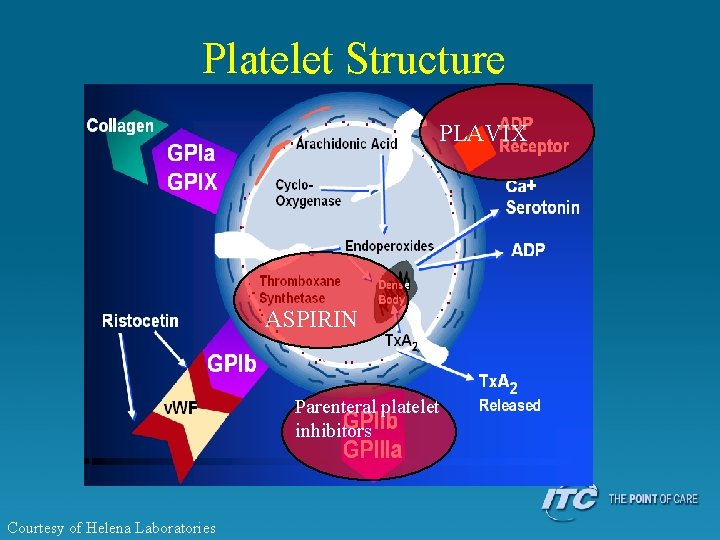
Platelet Structure PLAVIX ASPIRIN Parenteral platelet inhibitors Courtesy of Helena Laboratories

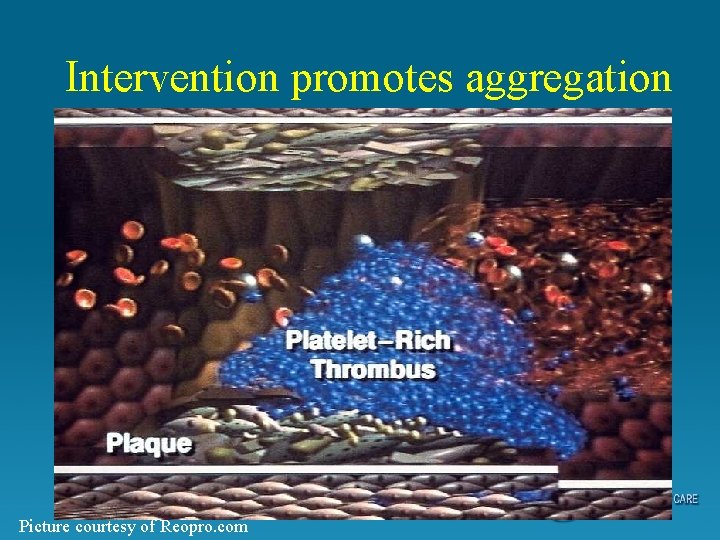
Intervention promotes aggregation Picture courtesy of Reopro. com

ACT Monitoring - Platelet Inhibitors • Aspirin – No reported effects on ACT – No anecdotal reports of effects on ACT • Plavix – No reported effects on ACT – Anecdotal reports • Increased bleeding at sheath pull • ACTs don’t return to “normal” prior to sheath pull – Plateau ~ 180 – 220 seconds

ACT Monitoring - Platelet Inhibitors • Reo. Pro – elevates ACTs • Study used FTCA 510 and Medtronics HR-ACT – target time = 250 sec with Reo. Pro • determined using FTCA 510 tube • Integrelin – No reported clinically significant effects on ACT – Slight decrease in ACT • Study used FTCA 510 and ACT-LR • Aggrastat – No reported effects on ACT

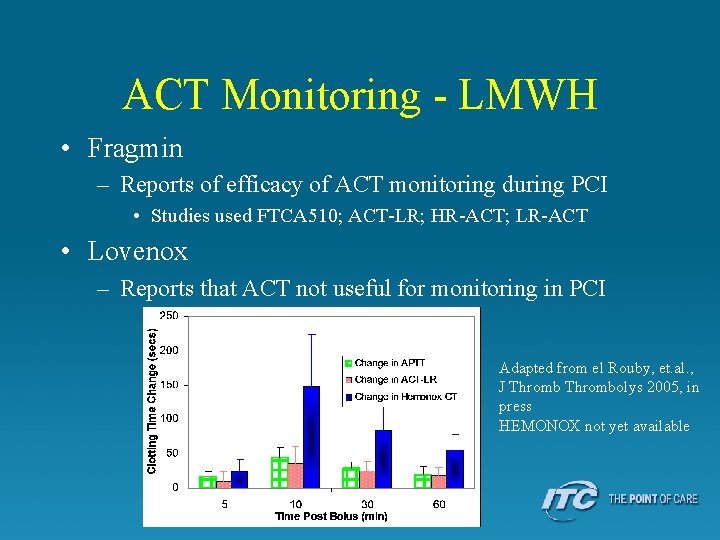
ACT Monitoring - LMWH • Fragmin – Reports of efficacy of ACT monitoring during PCI • Studies used FTCA 510; ACT-LR; HR-ACT; LR-ACT • Lovenox – Reports that ACT not useful for monitoring in PCI Adapted from el Rouby, et. al. , J Thrombolys 2005, in press HEMONOX not yet available

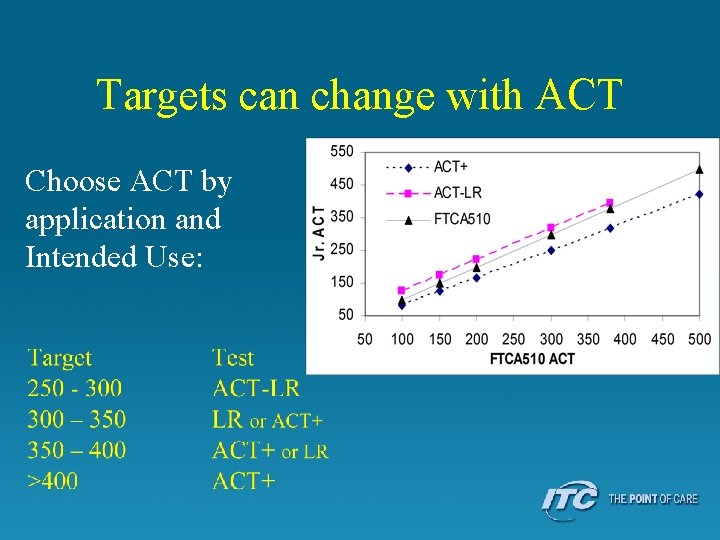
Targets can change with ACT Choose ACT by application and Intended Use:

Clinical Applications • Essential – Cardiac surgery – Percutaneous coronary intervention (PCI) – ECMO / (Dialysis) • Common – Critical care – Interventional radiology – Electrophysiology – Vascular surgery

ECMO (Dialysis) • ACT used to monitor low dose heparin – P 214 glass activated ACT has been the “standard” • Hemo. Tec HR and LR also used • Targets generally 180 - 220 seconds – Changing ACT requires changing target • Target often 220 -260 with ACT-LR • Not all ACTs have low heparin indication • Also indicated for low dose: – GEM PCL ACT-LR; Actalyke G-ACT

Clinical Applications • Essential – Cardiac surgery – Percutaneous coronary intervention (PCI) – ECMO / (Dialysis) • Common – Critical care – Interventional radiology – Electrophysiology – Vascular surgery

ACT or a. PTT • Determine when to pull the femoral sheath • HEMOCHRON FTCA 510; HEMOCHRON Jr ACT-LR; Medtronics LR-ACT; Actalyke C-ACT; GEM PCL ACT-LR – Premature sheath pull can lead to bleeding. – Delayed removal can increase time in CCU. – Target set at each site. • ACT targets range from 150 – 220 seconds • a. PTT targets range from 40 – 70 seconds • Monitor heparin therapy – Target times determined by each facility • HEMOCHRON FTCA 510; HEMOCHRON Jr ACT-LR; Medtronics LR-ACT; Actalyke C-ACT; GEM PCL ACT-LR

Clinical Applications • Essential – Cardiac surgery – Percutaneous coronary intervention (PCI) – ECMO / (Dialysis) • Common – Critical care – Interventional radiology – Electrophysiology – Vascular surgery

Low dose heparin • Interventional Radiology – Targets generally ~250 - 300 • Sometimes target “twice baseline” • Twice baseline can differ by ACT heparin sensitivity – More centers targeting “increase from baseline” • e. g. >130 second increase from baseline

Clinical Applications • Essential – Cardiac surgery – Percutaneous coronary intervention (PCI) – ECMO / (Dialysis) • Common – Critical care – Interventional radiology – Electrophysiology – Vascular surgery

Low dose heparin • Vascular Surgery and Electrophysiology – Targets generally ~200 – 250 • frequently no monitoring – Change from baseline is critical factor • Is heparin having an effect? • Is patient responding “normally”? – ~20% patients “resistant” <80 sec/unit/ml blood – ~60% patients “normal” 80 -120 sec/unit/ml blood – ~20% patients “sensitive” >120 sec/unit/ml blood

Summary • ACT is NOT a standardized test – Each assay yields different results • Activator differences • Endpoint detection differences • Current targets developed on Hemochron – First available non-manual system – Targets must be adjusted for other systems

Summary • While all systems correlate, they yield different results • Targets may need to be adjusted by clinical application • Inter-operator differences minimized with microcoagulation technology

The future of ACT?

