Eye Ear Nose and Throat Infections Ophthalmologist ENT




















































- Slides: 66

Eye, Ear, Nose, and Throat Infections

• Ophthalmologist • ENT specialist – Familiar with these infections – Preliminary empiric therapy

• Eye infections – Conjuctivitis – Keratitis – Endophtalmitis • Throat infections – Pharyngitis – Epiglottitis

• Ear infections – Otitis externa – Otitis media – Mastoiditis • Sinus infections – Sinusitis

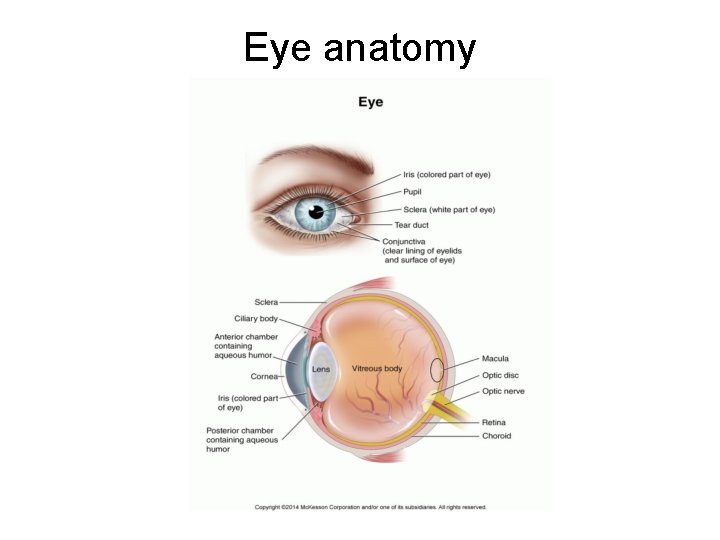
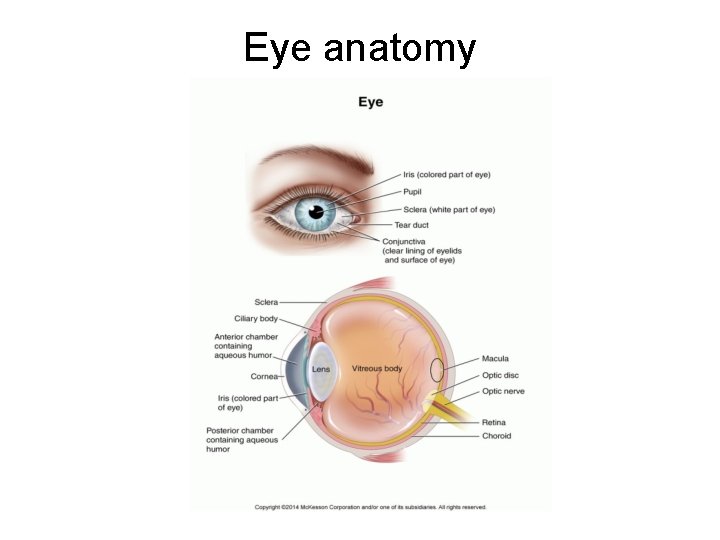
Eye anatomy

Conjuctivitis • Inflammation of conjuctiva • Doesn’t threaten the vision • Rapid respond to therapy

Conjuctivitis • Direct contact with the environment • Tears – Antibacterial agents – Lysozyme, Ig. A, Ig. G • Decresed tear production – Recurrent infections

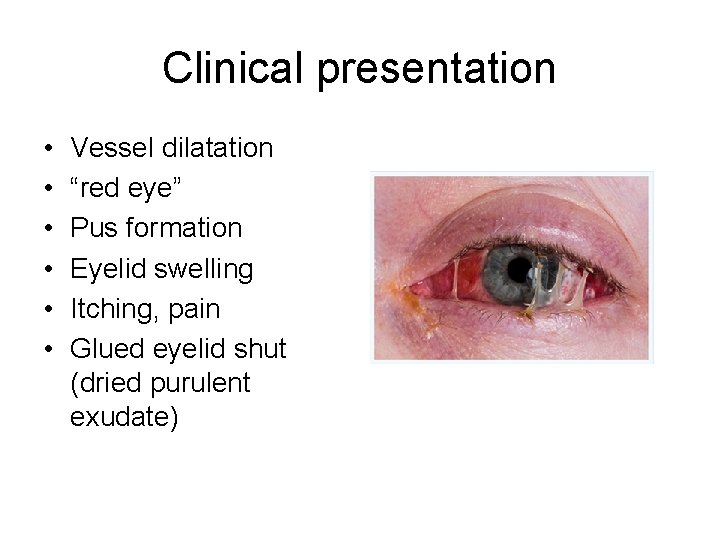
Clinical presentation • • • Vessel dilatation “red eye” Pus formation Eyelid swelling Itching, pain Glued eyelid shut (dried purulent exudate)

Causes • Bacteria • • Staph. aureus Str. pneumoniae H. influenzae M. catarrhalis N. gonorrhoeae N. meningitidis P. aeruginosa C. trachomatis • Viruses • • • Adenoviruses Enteroviruses HSV VZV Measles

Causes • Fungi • Candida • Blastomyces • Sporothrix schenckii • Parasites • Trichinella spiralis • Taenia solium • Schistosoma haematobium • Lola loa • Onchocerca volvulus

Causes • Viral • The most common • Highly contagious • Spread to the 2 nd eye in 24 -48 hrs • Bacterial • Highly contagious • Profuse pus formation

Causes • Allergic and toxic • Pollens • Symmetrical • Itching • Systemic diseases • Reiter syndrome • Vasculitis • SLE

Diagnosis • History & examination • Severe cases – Swab or scraping: Gram stain & culture – Viral: mononuclear cell exudate – Allergic: eosinophils

Treatment • Topical antibiotics? • To do or not to do? – Are your eyelids glued in the morning? (+5) – Does your eye itch? (-1) – Do you have recurrent conjuctivitis? (-2) • Score: • 5 – bacterial 77% • 2 – bacterial 2%

Treatment • Prefered therapy – Moxifloxacin 0. 5% sol TID 7 days • Alternate therapy – Gentamycin – Tobramycin – Polymyxin B / bacitracin – Neomycin / polymixin

Eye anatomy

Keratitis • Inflammation of cornea • Prompt treatment • Corneal perforation – blindness

Predisposing conditions • Minimal injury of cornea – Trauma – Contact lens abrasion – Eye surgery • • Impaired tear production Diabetes mellitus Immunosupression Comatose patient

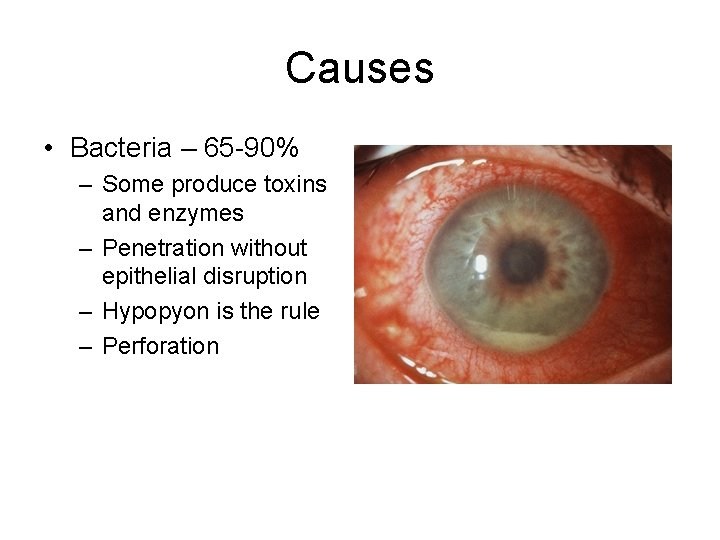
Causes • Bacteria – 65 -90% – Some produce toxins and enzymes – Penetration without epithelial disruption – Hypopyon is the rule – Perforation

Causes • • • Staph. aureus P. aeruginosa (contact lenses) N. gonorrhoeae N. meningitidis H. influenzae

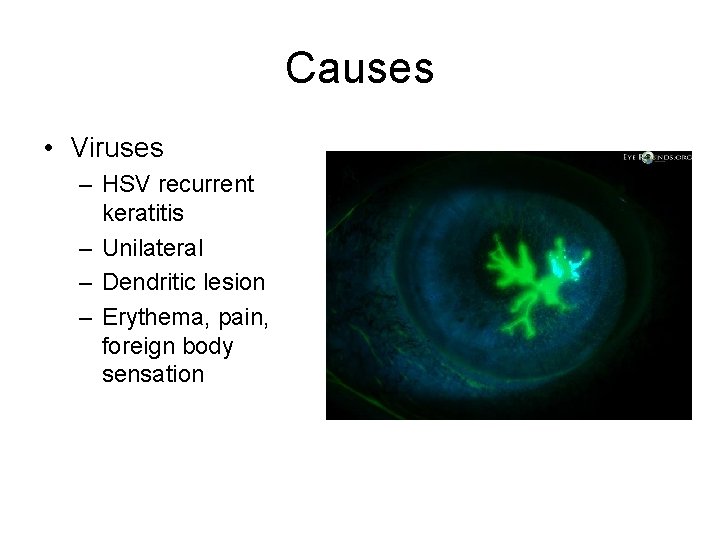
Causes • Viruses – HSV recurrent keratitis – Unilateral – Dendritic lesion – Erythema, pain, foreign body sensation

Causes • Fungi – After organic material injury (tree branch) – Prolonged corticoid eye drop therapy – Aspergillus • Protoza – Unsterilized tap water for contact lens cleaning – Acanthamoeba

Clinical presentation • • • Eye pain Foreign body sensation Corneal edema – impaired vision Photophobia Reflex tearing

Diagnosis • Medical history & exam • Swab or scraping – Gram stain, Giemsa stain, methenamine silver stain, culture • Therapy – Emergently – Experienced ophthalmologist

Endophthalmitis • • Serious infection Ocular chamber & adjacent structures Involving all tissue layers: panophthalmitis Often leads to blindness

Predisposing conditions • Posttraumatic – Staph. aureus and epidermidis – Str. spp – Bacillus cereus – Fungi • Organic matter penetrating injuries

Predisposing conditions • Hematogenous – Any source of bacteremia – 2/3 – right eye • Candida albicans • G + and G – bacteria • Bacillus cereus

Predisposing conditions • Contiguous spread – Uncontrolled keratitis – Delays in antibiotic therapy

Predisposing conditions • Ocular surgical procedures – Staph. aureus and epidermidis – Str. spp • Early – 1 – 5 days after the surgery • Delayed – Weeks to months after the surgery • Opportunistic pathogens

Clinical presentation • • • Eye pain Eye redness Photophobia Reduced vision Fever, algic syndrome

Diagnosis and therapy • • • Cultures and smears Systemic broad spectrum antibiotics Intravitreal antibiotic injection 1/10 patients – enucleation Experienced ophthalmologist

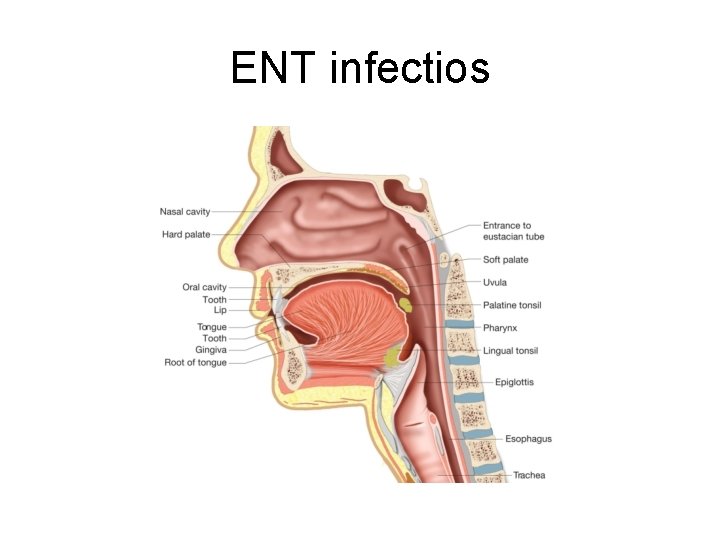
ENT infectios

Pharyngitis • Common infectious disease • Usually self-limiting • Antibiotics malpractice

Causes • Viruses – Rhino, corona, adeno, HSV, EBV, CMV, influenza, parainfluenza, coxsackie A, HIV • Bacteria – Group A streptococci (GAS) • Children 50% of all cases • Adults 10%

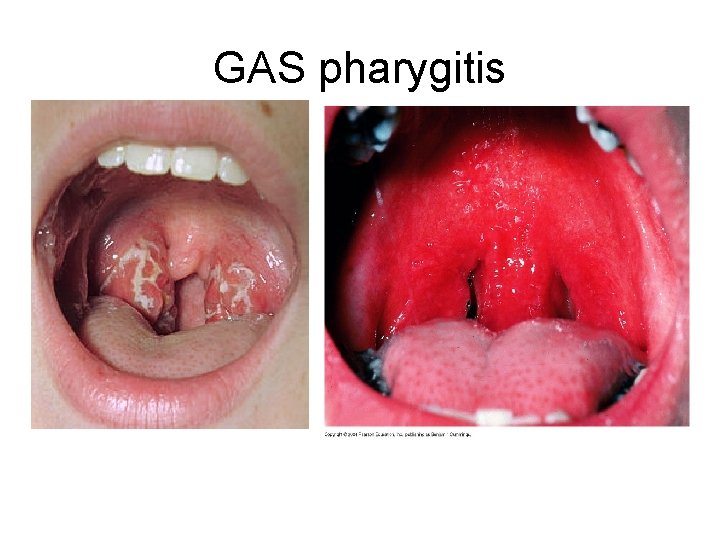
GAS pharygitis

Diagnosis • • • Centor clinical criteria Tonsillar exudates Tender anterior cervical adenopathy Fever Abscence of cough

Therapy • Penicillin the drug of choice – Oral Penicillin 10 days – Benzathine penicillin 1. 2 -2. 4 MU im once • Penicillin-allergic patients – Clarithromycin, clindamycin, cephalosporins 10 days, azithromycin 3 days

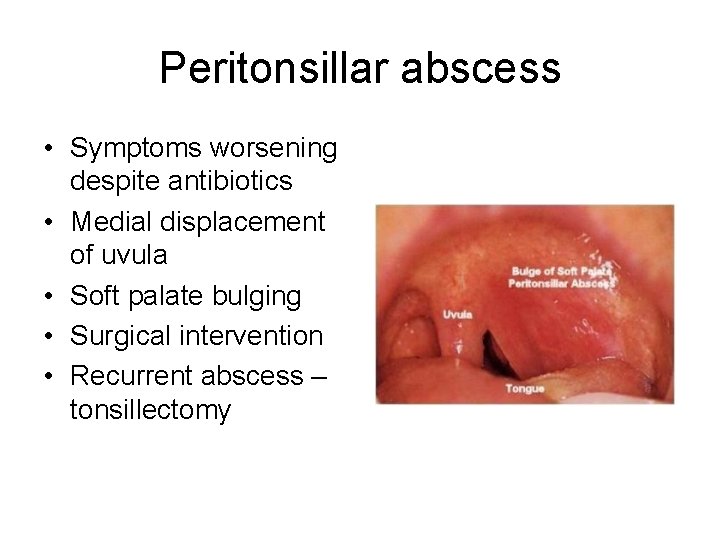
Peritonsillar abscess • Symptoms worsening despite antibiotics • Medial displacement of uvula • Soft palate bulging • Surgical intervention • Recurrent abscess – tonsillectomy

Epiglottitis • • • High fever Difficulty swallowing Drooling Difficulty breathing Indirect laryngoscopy Swollen, cherry-red epiglottis

Epiglottitis • High risk of airway obstruction • Children – Mortality 80% • Adult – Closely monitored • Endotracheal intubation

Epiglottitis • Causes – H. influenzae – Str. pneumoniae – Staph. aureus • Therapy – 3 rd generation cephalosporins iv 7 -10 days

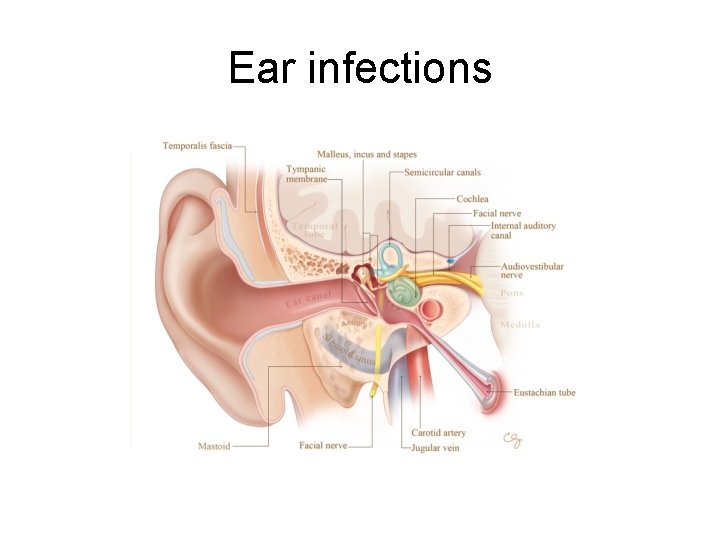
Ear infections

Otitis externa • Immunocompetent – Mild disease • Immunocompromised – Possible life – threatening

Otitis extrena • Local itching and pain • Redness and swelling of the external canal skin • Tenderness of the auricula

Causes • • Gram-negative bacteria P. aeruginosa the most prevalent Staph. epidermidis or aureus Candida or Aspergillus

Therapy • Polymyxin neomicin sol. + Hydrocortison sol. • Clotrimazol or miconazol

Malignant otitis externa • Immunocompromised • Severe pain • Spreading of necrotizing infection – Skull, meninges, brain • • CT scan, MRI Gallium scan P. aeruginosa almost always! Systemic therapy 6 weeks + surgical debridement

Otitis media • Most commonly in childhood • Up to 3 y/o 2/3 of children at least 1 episode • Consequence of the Eustachian tube obstruction

Otitis media • • Viral upper respiratory infection Serous fluid accumulation Eustachian tube obstruction 5 -10 days later – fluid infected with mouth flora

Clinical presentation • • • Ear pain Ear drainage Occasionally hearing loss Fever Vertigo, tinnitus, nystagmus Loose stools (children)

Diagnostic criteria • Abrupt onset of middle-ear inflamation • Presence of middle-ear effusion (any) – – Bulging of the tympanic membrane Limited mobility of the tympanic membrane Air-fluid level behind the tympanic membrane Otorrhea • Signs of middle-ear inflamation (any) – Erythema of the tympanic membrane – Otalgia that interferes with normal activity or sleep

Causes • • • Str. pneumoniae H. influenzae M. catarrhalis GAS Staph. aureus

Therapy • Amoxycillin • after 72 hrs – revision – Improvement – continuation – Failure • Amoxycillin – clavulante • Cefuroxime • 10 days

Mastoiditis • Rare otitis media complication • Manifestation – Swelling, redness, tenderness in the area of the mastoid bone • Possible spreading – temporal bone – temporal lobe – brain abscess • CT, MRI • Prolonged antibiotic therapy

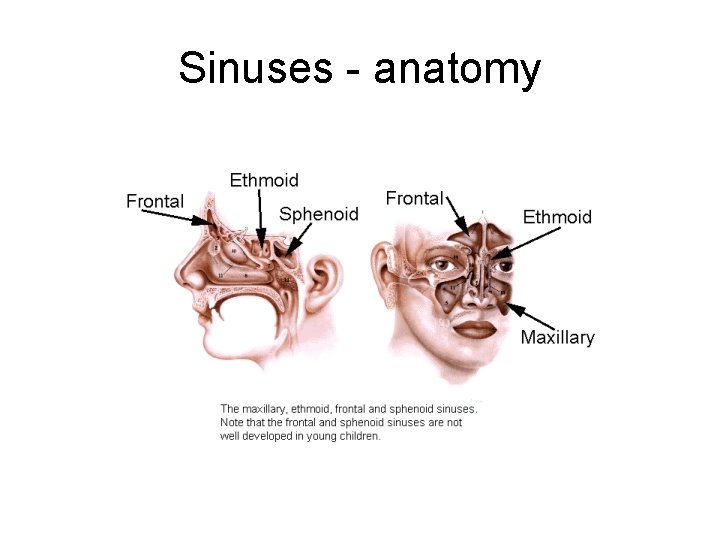
Sinuses - anatomy

Sinusitis • • Nasal and sinus mucosa inflammation Rhinosinusitis Viral upper respiratory infection preceding 0. 5 – 1% progress to bacterial sinusitis

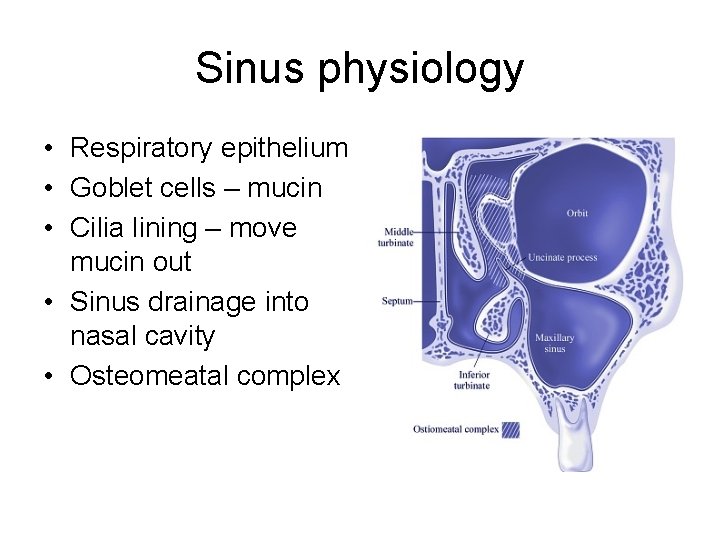
Sinus physiology • Respiratory epithelium • Goblet cells – mucin • Cilia lining – move mucin out • Sinus drainage into nasal cavity • Osteomeatal complex

Pathogenesis • • OMC obstruction Sinus drainage impaired Accumulation of serous fluid Fluid infection with oral flora

Predisposing conditions • • • Septal deformities Nasal polyps Intranasal neoplasms Indwelling nasal tubes Nasogastric tubes Nasal allergies Dental abscess Cystic fibrosis (abnormally voscous mucous) Kartagener syndrome (impaired ciliary function)

Clinical presentation • • Headache Facial pressure Nasal obstruction Nasal discharge Loss of smell Foul-smelling breath Fever

Bacterial causes • • Str. pneumoniae H. influenzae M. catarrhalis S. aureus S. epidermidis GAS G-neg bacteria Anaerobs

Diagnosis • WBC often normal, CRP may be elevated • Culture of nasal swabs poorly corelate with intrasinus cultures • Direct sampling complicated and painful • X-rays, CT, MRI not helpful for the etiology diagnosis • Medical history & exam

Bacterial sinusitis • Peristent acute sinusitis symptoms >10 days • Abrupt onset with high fever (39°C) and purulent nasal discharge, facial pressure lasting 3 -4 consecutive days • Sudden worsening of typical viral upper respiratory infection

Therapy • Amoxycillin – clavulanic acid 2 x 1. 0 g • Fluoroquinolones – Levofloxacin 1 x 250 mg – Moxifloxacin 1 x 400 mg • Doxycyclin 2 x 100 mg • Cefuroxim – axetil 2 x 250 -500 mg • Cefixim 1 x 400 mg

Therapy • • Intravenous therapy Frontal, ethmoid, sphenoid sinusitis Prevent the infection spreading Vital organs beyond the thin sinus walls

Therapy • Nasal decongestants in viral infections • Saline irrigation • Intranasal corticosteroids in patients with nasal allergy • Symptomatic treatment • Bed resting, fluid replacement, analgesics, antipyretics