Diagnosis and Treatment Plan for Complete Denture Patients
























































- Slides: 60

Diagnosis and Treatment Plan for Complete Denture Patients

INTRODUCTION “Examination is defined as scrutiny or investigation for the purpose of making a diagnosis or assessment” The goal in clinical examination is to recognize normal anatomy and physiology, normal variations, and early signs and symptoms of any disease. A through, comprehensive examination also allows modification or possible deferment of treatment when indicated.

Importance of case History Case history taking is important to know if the patient has recently become edentulous or has been edentulous for a long time. A “green ridge” may be bony spicules remaining from the extraction sites or bony undercuts with a thin mucosal covering. The intraoral examination will determine if any surgical correction is necessary, the prosthodontist must realize these possibilities and discuss with the patient. The examination should be carried out meticulously. A systematic recording of case history along with careful examination and evaluation leads to a diagnosis, probable prognosis and the tentative plan.

History taking and examination

Personal data Name Obtaining the name of the patient not only helps in maintaining records but also helps in creating a more personal and ambient atmosphere for the patient in the dental clinic. Addressing the patient by his/her name gives a rather personal touch to the dentist patient relationship. Age is an indicator of the patient’s ability to wear and use a prosthesis. Through the fourth decade of life, tissues heal rapidly and are resilient. Beyond fifth decade healing is not rapid. Woman facing the physiologic and psychological problems often present as exacting or hysterical patients who are very conscious about esthetics. Men are preoccupied and present as indifferent patients who are concerned more with comfort or function.

Sex Generally appearance is a higher priority for women than for men. Though younger men often grow indifferent to their own appearances as they age and are concerned with comfort and function. Occupation A patient’s job & social training often determine the values he or she places on oral health, as well as the esthetics and other qualities desired in a denture. Race can be critical factor in the characterization of dentures i. e. , choice of denture base shade, denture base stains.

Chief Complaint The patient should be questioned regarding his or her chief complaint such as 1. Inability to chew 2. Impaired speech 3. Poor appearance 4. Others. History of presenting illness The duration of the edentulous state is of importance in ascertaining a proper diagnosis and treatment plan for the patient. Also the manner in which there was a loss of teeth helps to understand the patients personal interest in his or her oral hygiene and other habits.

Expectations The reason the patient seeks prosthetic treatment is important. His or her expectations must be determined. These should then be evaluated to determine I they are realistic, practitioner should not make unrealistic promises regarding treatment outcome. Mental Attitude/ Personality House classified patients as: Philosophical Exacting Indifferent Hysterical

Philosophical Patient The best mental attitude for denture acceptance is the philosophical type. This patient is rational, sensible, calm and composed in difficult situations. These patients are confident, easy going and cooperative. The philosophical patient overcomes conflicts and organizes his time and habits in an orderly manner, he eliminates frustrations and learns to adjust rapidly. Prognosis is excellent. Exacting Patient The exacting type may have all of the good attributes of the philosophical patient; however he may require extreme care, effort and patience on Prosthodontist’s part. This patient is methodical, precise and accurate and at times makes several demands. Once satisfied, an exacting patient may become the practioners greatest supporter.

Indifferent Patient The indifferent type of patient presents a questionable or unfavourable prognosis. This patient exhibits little concern if any; he is apathetic and uninterested and lacks motivation. The indifferent patient pays no attention to instructions, will not cooperate and is prone to blame the dentist for poor dental health. An education program in dental conditions and dental treatment is the recommended treatment plan before denture construction. Hysterical Patient The hysterical type is emotionally unstable, excitable, excessively apprehensive and hypertensive. The prognosis is often unfavorable and additional professional help (psychiatric) is required prior to and during treatment. This patient must be made aware that his/her problem is primarily systemic and that many of his symptoms are not result of dentures. Prognosis is poor.

Medical History General health A thorough and accurate medical history must be obtained during the diagnostic phase of complete denture therapy and must be updated as necessary. The medical history provides important insights regarding the patients dental prognosis. Not surprisingly, patients who exhibit good health are better prosthetic risks than those in poor health. Hence the practitioner must be aware of local and systemic factors and must be consider them during treatment planning. Systemic factors that may affect complete denture therapy include: Anaemia, Arthritis, Bells palsy, Carcinomas, Diabetes, Lupus erythematosus, Nicotinic stomatitis, Pagets disease, Parkinsons disease, Pemphigus vulgaris, Plummer- Vinson syndrome, Scleroderma, TB, Xerostomia.

Dental History Chief complaint: According to De. Van, “ the dentist should meet the mind of the patient before he meets the mouth of the patient. ” hence the dentist must determine the reason the patient is seeking prosthodontic treatment. Reasons For Loss Of Teeth: The patient should be questioned regarding the cause of teeth loss (e. g. periodontal, caries, congenital, trauma etc) Duration Of Edentulousness The maxillary/mandibular responses to the question proves about bone resorption patterns and progression.

Previous Denture Experience: The patient should be questioned regarding the number & types of previous dentures; patients should be made to comment on the reasons for replacement and should be educated regarding the realistic limitations. A patient with a history of several dentures over a short time is a poor prosthodontic risk. Existing Or Current Dentures: The patient should be questioned about the length of time for which the dentures have been worn. Careful clinical observation may provide valuable information about denture experience, dental care, knowledge, parafunctional habits etc.

Denture success: The patient should be asked about the estheitics and function of existing dentures. Responses indicate the patients ability to wear or adjust to complete dentures. Denture success should be rated as “favorable” or “unfavorable”. Pre-extraction records: Pre-extraction photographs, radiographs, casts and facial measurements may prove helpful in denture therapy. These adjuncts may be used to recreate anterior esthetics and facial support and aid in evaluation of vertical dimension of occlusion.

CLINICAL EVALUATION Extraoral Examination Facial Form: Classification according to House & Loop, Frush &Fisher & Williams. Ø Square Ø Tapering Ø Ovoid Ø Different combinations

Facial Profile (Acc. To Angle): The facial profile is examined by viewing the patient from the side. This helps in diagnosing gross deviations in the maxillomandibular relationship. Profile is obtained by joining the two reference lines, line joining the forehead and the deepest point in curvature of upper lip (A). Line joining point A & most anterior point on the chin (B). Based on Relationship of these lines a. Straight/orthognathic: The two lines form a nearly straight line b. Concave/prognathic: The two references lines form an angle with the convexity towards the tissue. This is associated with a prognathic mandible or a retrognathic maxilla as in Class III malocclusions c. Convex/retrognathic: The two lines form an angle with the concavity facing the tissue. This profile occurs as a result of a prognathic maxilla or a retrognathic mandible as seen in Class II malocclusion.


Facial Symmetry: It is examined to determine disproportions in transverse and vertical plane. In most patients, the right and left sides are not identical which is also termed as normal asymmetry. Some degree of asymmetry is accepted as normal whereas gross asymmetries are recorded.

Complexion: As all of us are aware that our aim is to achieve a harmonious blending of shape, shade, arrangement and position so that the final result is a “removable restoration that creates an illusions of being what it is not” so as to get an Esthetic denture which is defined as “the cosmetic effect produced by a dental prosthesis which affects the desirable beauty, attractiveness character and dignity of the individual. These shades should be comparable with the patient’s general facial coloration & complexion. Pallor may indicate anaemia, hyperthyroidism or nephrosis, systemic disease such as TB. Ruddy complexion sign of polycythemia or neoplasm. Bronzed skin occurs in Addison’s disease. Diffuse, bluish purple color may indicate Vit B 2 deficiency. Lemon-yellow complexion of jaundice is associated with gallbladder, liver or bile duct disorders. Complexion marred by ulcerated lesions may be due to basal cell and squamous cell carcinoma.

Skin color Dark Skin, hair and eye Fair Along with patient’s age Medium Helps in determining the tooth shade. Hair Black Brown White Grey Eye Black Brown Green Grey

Lip support: If tissues around the mouth has wrinkles and rest of the face does not, significant improvement can be done. If present anterior teeth are set lingually, the lip will lack support and plans to bring new teeth forward can be made. The long standing wrinkles do not disappear at once. Lip Thickness: Thin Lips: Patients with thin lips present special problems. Any slight change in the labiolingual tooth position makes a sudden change in lip contour. Even overlapping of teeth may distort the surface of lips. Thick Lips: Variations in the arch form and individual tooth arrangement do not make obvious changes.

Lip Length: Patients with short upper lips will expose all the upper anterior teeth, much of labial flange as well. Care must be taken to select color and form of denture base. Long lip shows less of anterior teeth. Lip Fullness: This is directly related to the support it gets from the mucosa or denture base and the teeth behind it. An existing denture with thick labial flange could make the lip appear to be too full rather than displaced. If the existing dentures have the teeth set to far palatally, the patient may feel that the new and corrected tooth arrangement makes the lip too full.

Lip Mobility: Class I – normal Class II – reduced mobility Class III – paralysis Some stroke patients may have paralysis of half the lip leading to unilateral mouth droop and facial asymmetry and counseling should be done regarding treatment limitations as they might have unrealistic expectations regarding function and esthetics. Lips should be examined for cracking, fissuring at the corners and ulceration. These changes could be caused by Vit B complex deficiency or infections from organisms such as candida albicans.

Muscle Tone: Classification According to House: Class I: The patient exhibits normal tension tone and placement of the muscles of mastication and facial expression. No degenerative changes are apparent. Majority of edentulous patients have experienced some degree of degeneration and usually only immediate denture patients have normal musculature. Class II: The patient displays approximate normal function but slightly impaired muscle tone. Maximum muscle function cannot be used following the loss of all natural teeth. Class III: The patient exhibits greatly impaired muscle tone and function. This is usually coupled with poor health, inefficient dentures, and loss of vertical dimension, wrinkles, decreased biting force and drooping commissures.

EXAMINATION OF THE TEMPOR MANDIBULAR JOINT: Good prosthodontic treatment bears a direct relation to the temporomandibular articulation since occlusion is one of the most important parts of the treatment of complete dentures. The TMJ affects the dentures which further affect the health and function of the joints. CLINICAL EXAMINATION OF THE TEMPOROMANDIBULAR JOINT: The examination should include the auscultation and palpation of the TMJ and the musculature associated with mandibular movements as well as the functional analysis of the mandibular movements. PALPATION: lateral palpation, posterior palpation Lateral Palpation: Exert slight pressure on the condyloid process with the index fingers, palpate both sides simultaneously. Register any tenderness to palpation of joint and any irregularities in condyloid movement during opening and closing maneuvers. The co-ordination of action between the left and right condylar heads should be assessed at the same time.

Posterior palpation: Position the little fingers in the external auditory meatus and palate the posterior surface of the condyle during opening and closing movements of the mandible. Palpation should be carried out in such a way that the condyle displaces the little finger when closing. MOVEMENTS OF THE MANDIBLE ØOpening movement ØClosing ØProtrusive excursion ØRetrusive ØLateral All these are examined as part of the functional analysis. The amount and direction of these actions are recorded during the clinical examinations. Deviations in speed can only be registered with electronic devices e. g. Kinesiograph. The first signs of initial temporomandibular joint problem include deviations of the mandibular opening and closing paths in the sagittal and frontal planes. The characteristic movement deviations include incongruency of the opening and closing and uncoordinated zigzag movements. The ‘C’ and ‘S’ types of deviations are typical signs of functional disturbances.

Neuro muscular evaluation Speech : Patients who are capable of articulate speech with existing dentures usually have no problems producing articulate speech with new dentures. Patients with speech impediments require special attention when the dentist places the anterior teeth and forms the palatal portion of the denture base. Speech is classified as : “normal” or “affected”. Coordination: Patients with good neuromuscular coordination can be expected to learn to manipulate dentures relatively quickly. Whereas patients with poor coordination may never adapt to a denture completely. Neuromuscular coordination is classified as: Class 1: Excellent Class 2: Fair Class 3: Poor

Intra oral examination Arch size The size of the maxilla and mandible ultimately will determine the amount of basal seat available for denture formation. The greater the size: greater the support, larger the contact surface, greater the retention. If discrepancy is present, in the size of maxilla and mandible, it should be noted. This condition may arise from a developmental source, trauma, and early loss of teeth in one arch with resultant increase in resorption or from a severe Class II or Class III malocclusion. This may lead to a poor relationship of teeth in one arch to the other. Class 1: Large ( best for retention and stability) Class 2: Medium (good retention and stability but not ideal) Class 3: Small (difficult to achieve good retention and stability)

Arch form The arch may be Class 1: Square Class 2: Tapered Class 3: Ovoid and opposing arch may or may not have the same form. The form of the arch will influence the support of the denture. If the arch form is not same in both the arches some problems in tooth arrangement can be anticipated.

Residual ridge contour / form Ridge form is characterized traditionally as by its crosssectional contour as a whole arch. Maxillary ridge and vault form is classified as: Class 1: U shaped arch is generally favorable for supporting a denture since it has broad base for occlusal stresses and parallel sides that enhance adhesion and resistance to displacement as well as encourage border seal. Class 2: V-shaped has a narrow crest that is not conducive to the reception of masticatory stresses without irritation and discomfort. Less favorable for retention because of its sloping sides and has a tendency to progress towards narrowness. The thin sharp mandibular ridge presents difficulty in prosthetic management.

Class 3: Flat residual ridge is the most difficult for restoration by the prosthodontist. The normal pattern of resorption for maxillary arch is upward and inward as compared to the downward and outward progression of bone loss of the mandibular ridge. (Lack of vertical height produces less resistance to horizontal forces) Jaw relationship thus normally progresses to cross-bite situations and complicate the distribution of prosthetic stress to the basal support.

Mandibular ridge form Class 1: Inverted U shaped (parallel walls from medium to tall with broad crest) Class 2: Inverted U shaped (short with flat crest) Class 3: Unfavorable Inverted W Short inverted V Tall, thin inverted V Undercut

Ridge relation Laney Smith described ridge relationship as the anteroposterior position of the mandibular ridge relative to the maxillary residual ridge when the jaws are in centric relation and separated by the distance they will be separated by the prosthesis. CLASSIFICATION BY ANGLE: Angle Class I (Normal): - Anterior segment of the mandibular ridge is directly below or slightly posterior to the maxillary anterior ridge segment. Angle Class II (Retrognathic): - Anterior segment of the mandibular ridge is retruded beyond the normal position as it relates to the maxillary anterior ridge segment. Angle Class III (Prognathic): - Anterior segment of the mandibular ridge is protruded beyond the normal position as it relates to the maxillary anterior ridge segment.

Ridge parallelism Classification according to Angle Class I – Both ridges are parallel to the occlusal plane Class II – The mandibular ridge is divergent from occlusal plane anteriorly Class III – The maxillary ridge is divergent from the occlusal plane anteriorly and/or both ridges are divergent anteriorly Importance: Ridges that are not parallel to each other will cause movement of the bases when teeth occlude because of an unfavorable direction of forces


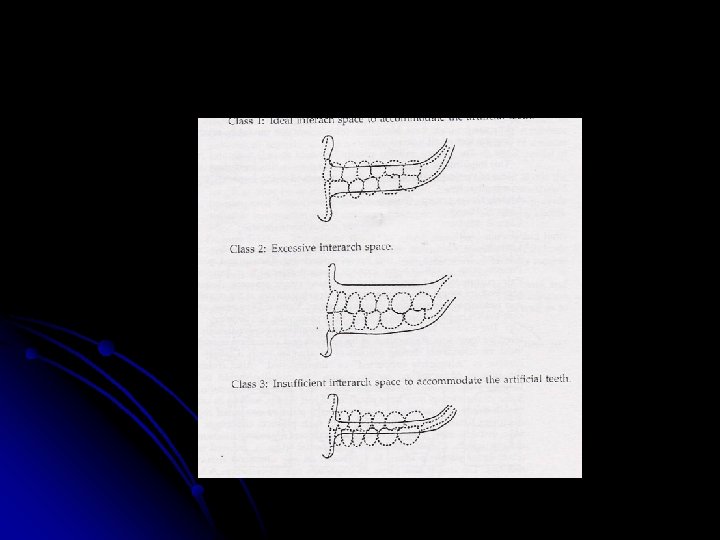
Intermaxillary space This is the space between the maxillary and the mandibular arches. Normally it should be 20 mm. If the space is less than 20 mm it is difficult to obtain stability of the denture base, which is compromised as the teeth are set away from the basal seat. Class I: Ideal interarch space to accommodate the artificial teeth Class II: Excessive interarch space Class III: Insufficient interarch space to accommodate the artificial teeth


MUCOSA: Mucosal displaceability Classification by House Class 1: Normal uniform density of mucosal tissue (approx 1 mm thick). Investing membrane is firm but not tense and forms an ideal cushion for the basal seat of the denture Class 2 a: Soft tissues have thin investing membrane and are highly susceptible to irritation under pressure Class 2 b: Soft tissues have mucous membrane twice the noraml thickness. Class 3: Excessively flabby to the degree that surgical excision is indicated

HARD PALATE SHAPE OF PALATAL VAULT U Shaped: It is most favorable for retention and lateral stability V Shaped: It is less favorable for retention because slightest movement of denture base will cause the seal to be broken with a resultant loss of retention Flat palatal vault: Is unfavorable. Usually accompanied by resorbed ridges and although retention may be satisfactory in a downward direction, any lateral or rotatory forces results in poor resistance and less retention

SOFT PALATE Classification is based upon the angle formed with the hard palate. The more acute angle of the soft palate in relation to the hard palate, the more muscle activity that is necessary for velopharyngeal closure (closing of nasopharynx). More the soft palate is markedly displaced in function, the less can be covered by the denture base. CLASS I: Indicates a soft palate that is rather horizontal as it extends posteriorly with minimal muscle activity. When the vibrating muscle is located, a few mm separate the anterior and posterior vibrating lines allowing for wide posterior palatal seal but not very deep. Considered as most favorable as more tissue surfaces can be covered leading to more retentive denture base.

CLASS III: Indicates the most acute contour in relation to the hard palate, creating marked elevation of the musculature to create velopharyngeal closure. Seen usually in configuration with a high V-shaped palatal vault. As there is greater elevation of the soft palatal musculature in function a few mm separate the vibrating lines and so, smaller area for the posterior palatal seal is there than class I. Along with being smaller, it is also deeper than class I configuration. CLASS II: Designates those palatal contours that lie between class I and class III Position of the patient: The classification of soft palate are determined when the patient is in upright position and the head is held erect.


MAXILLARY TUBEROSITY: Extremely large maxillary tuberosities make it necessary to locate the back end of the occlusal-plane too low, omit some posterior teeth or shorten the denture bases from their correct border extent and contour. Pendulous fibrous maxillary tuberosities are frequently encountered. They occur unilaterally or bilaterally and may interfere with denture construction by excessive encroachment on or obliteration of the interarch space. Surgical treatment is the choice and occasionally maxillary bone must be removed. Absence of maxillary tuberosities and loss of pterygomaxillary notch: Advanced bone resorption or excessive surgical resection of the tuberosity area can lead to absence of one or both tuberosities. This is frequently accompanied with obliteration of the pterygomaxillary notch area which is essential for enhancing for maximum breath to the posterior palatal seal area and the patient should be informed as the maxillary denture will not be as resistant to posterior downward dislodgement when incising takes place.

TONGUE: Smith described two anatomic tongue types: Long, narrow, tapered Short, broad and thick The first type presents fewer problems but while making impression; it might jeopardize lingual border seal. The second fills more of space in the floor of mouth so as to provide posterior denture flange and hence better border seal. Classification of tongue size according to House: CLASS I: Normal in size, development and function, sufficient teeth are present to maintain normal form and function. CLASS II: Teeth have been absent long enough to permit a change in the form and function of the tongue. CLASS III: Excessively large tongue. All teeth have been absent for an extended period of time, allowing for abnormal development of a class III tongue.

Tongue position Classified according to Wright Normal : the tongue fills the floor of the mouth and is confined by mandibular teeth. Lateral borders rest on the occlusal surfaces of the posterior teeth and apex rests on the incisal edges of the anterior teeth. Class 1: Retracted – the tongue is retracted. The floor of the mouth pulled downward, is exposed back to the molar area. The lateral borders are raised above the occlusal plane and the apex is pulled down into the floor of the mouth. Class 2: Retracted – the tongue is very tense and pulled backward and upward. The apex is pulled back into the body of the tongue and almost disappears, the lateral borders rest above the mandibular occlusal plane. The floor of the mouth is raised and tense.

Saliva Class 1: Normal quantity and quality of saliva. Cohesive and adhesive properties of saliva. Class 2: Excessive saliva, contains much mucous. Class 3: Xerostomia, remaining saliva is mucinous.

FLOOR OF THE MOUTH It presents a wide variation in anatomy and functional relation to the ridge crest. If the floor is near the crest, at rest or the magnitude of movement is great, magnitude of retention and stability is poor. The floor of the mouth in the sublingual gland mylohyoid areas can be very high and close to the ridge crest at times may spill over the ridge and eliminate alveolingual sulcus. If there tissues cannot be placed selectively by the denture flange than the prognosis of mandibular denture is poor.

LATERAL THROAT FORM Niel described soft palate configuration throat form but distinguished this category from lateral throat form. He defined lateral throat form as the contour of the hard lingual surfaces of the mandibular ridge in the molar area and the velum like tissue distal to the mylohyoid ridge in the retromylohoid fossa as it functions under the influence of tongue. Lateral throat form is classified according to the extent of anterior movement of the retromylohoid curtain as the tongue is extended anteriorly beyond the vermillion border of the lower lip. Examination: With the index finger passively contacting the curved wall of mucosa in the retromolar fossa with the tongue at rest, patient is instructed to protrude the tongue.

Classification Acc to Niel CLASS I: If the lateral throat form changes configuration so as to place heavy pressure on the finger. CLASS III: If the pressure is minimal or no pressure is exerted. CLASS II: Any position of the tissue between these two extremes Overextension in the retromylohyoid areas results in loss of border seal, displacement of denture or soreness that readily radiates to the floor of the mouth, throat and neck


TORI CLASS I: Tori are absent or minimal in size and do not interfere with existing denture. CLASS II: Clinical examination shows several tori of moderate size, often mild difficulties in denture construction and use of surgery not required. CLASS III: Large tori are present. These tori compromise the function of dentures. These tori require surgical removal.

FRENUM ATTACHMENTS Classification according to House: CLASS I: High in the maxilla or low in the mandible with respect to the crest of the ridge CLASS II: Medium CLASS III: Freni encroach on the crest of the ridge may interfere with the denture seal. Surgical correction may be required

EXISTING DENTURES - Anterior tooth shade, mould and material - Posterior tooth shade, mould and material Existing dentures should be evaluated to determine physical, aesthetic and anatomic characteristics. - Aesthetics, phonetics, retention, stability, extensions and contours. - Centric relation and vertical dimension of occlusion. - Occlusal plane orientation. - Palate of the existing denture should be examined. - Post dam - Base adaptation - Midline - Buccal vestibule - Cross bite - Comfort and hygiene

Diagnosis The word diagnosis is derived from Greek word dia (thorough) and gnosis (knowledge) and is defined as “to know apart or to distinguish”. For our purposes diagnosis is defined as 1) The act or process of deciding the nature of a diseased condition by examination 2) A careful investigation of the facts to determine the nature of things or 3) The determination of the nature, location and causes of the disease - by Charles Heartwell. According to glossary of prosthodontics – diagnosis is defined as determination of the nature of disease.

The ability to make diagnosis is predicted on several different factors. The knowledge of how to conduct a careful and thorough investigation of a problem is important, but still more important is the knowledge of the system and the problems that might affect it. A correct diagnosis is the basis for the appropriate and adequate treatment of the patient with the problem. The prosthodontist will know the natural history of the problem and the most effective form of therapy. This information in turn then provides the basis for a prognosis.

DIAGNOSTIC AIDS 1. Pre-extraction records Old diagnostics casts are invaluable aids in determining tooth size, position and arrangement. Old radiographs are also helpful in determining tooth size and bony changes. Photographs showing natural teeth can also relay much information regarding tooth size, position etc; and be helpful in achieving proper esthetics and patient’s satisfaction. 2. Radiographic Examination Of Edentulous Patients Radiograph examination of edentulous patients is advisable prior to the construction of dentures. Use of the orthopantomograph for routine examination of prosthetic patients. Such an examination will often reveal the presence of residual roots, unerupted teeth or other abnormalities in patients who are otherwise free from signs or symptoms that might suggest existence of a pathologic condition.

3. Diagnostics Casts On occasion, ridge relationships, inter-ridge distance or ridge shape and forces cannot be adequately determined by clinical examination alone. It may be necessary to make preliminary impressions and a maxillo mandibular relation record to mount the casts on the articulator. The centric relation and occlusal vertical dimensions records must be viewed around the entire arch. Sufficient space may not be available for both denture bases between the tuberosities of the maxillae and retromolar pad of mandible.

TREATMENT PLANNING -Tissue conditioning: List proposed therapy as finger massage, prescribed medications, type of tissue treatment material to be used and frequency of soft reline changes, etc. -Preprosthetic sugery: List any proposed preprosthetic procedures along with the staging of these procedures. -Articulator -Tooth selection -Denture base material -Denture base shade -Anatomic palate -Characterization PROGNOSIS Give the prognosis and list the reasons for the prognosis

Conclusion The acquisition of knowledge is one of man’s greatest accomplishments. Putting that knowledge to use is the fuel that turns the wheel of progress. Research works may develop mathematical models, devise predictive procedures and test them satisfactorily, but the practicing prosthodontic treating the patient at a time will prove the ultimate worth of any suggestive method. So equipped with the knowledge and understanding of examination and diagnosis, we can become skilled hands to intervene during treatment planning.

References 1. The Dental Clinics of North America – Complete dentures 2. Charles M. Heartwell – Syllabus of complete dentures. 3. Boucher’s – Prosthodontic treatment for edentulous patients. Pg: 51. 4. Sheldon Winkler – Essentials of complete denture prosthodontics. Pg: 39.