Approach to myopathy u Hereditary u acquired history

































































- Slides: 67



Approach to myopathy u Hereditary u acquired

history u u u u u Onset age distribution Course Myalgia Cramp Contracture Dark urine Myotonia , Stiffness /warming up phenomena Aggravating: exercise /diet/temperature/drug

exam u Limb girdle u Scapuloperoneal u Distal u Ocular or pharyngeal u Neck extensor u Atrophy or hypertrophy u Myotonia or paramyotonia

Ptosis usually without opthalmoplegia u Myotonic dystrophy u Congenital myopathy u Ptosis with opthalmoplegia u Oculopharyngeal muscular dystrophy u Mitochondrial myopathy u

Weakness u Constant u Longlife u Progressive u Dystrophy u fluctuation acquired MG periodic P metabolic static congenital

u Age u Distribution u Inheritance

Work up Muscles enzyme u R/o metabolic screen u EMG&NCS (myotonia , fibrillation, R/o neuropathy) u Muscle biopsy (dystrophy/ congenital myopathy, stain for enzyme level) u Genetic study u Other : u Forearm exercise test u specific Enzymes level u

? When do you suspect

Hereditary myopathy

u Structural u functional

classification u Dystrophy u Congenital myopathy u Channelopathies & myotonia u Metabolic (fatty acid/ glycogensis/mitochondrial)

muscular dystrophy are inherited myopathy characterized by progressive muscles weakness °eneration &subsequent replacement by fibrous & fatty connective tissue u Historically were categorized by their: u Age onset /distribution of weakness& pattern of inheritance u The genetic mutation &abnormal gene product were defined for many of them u

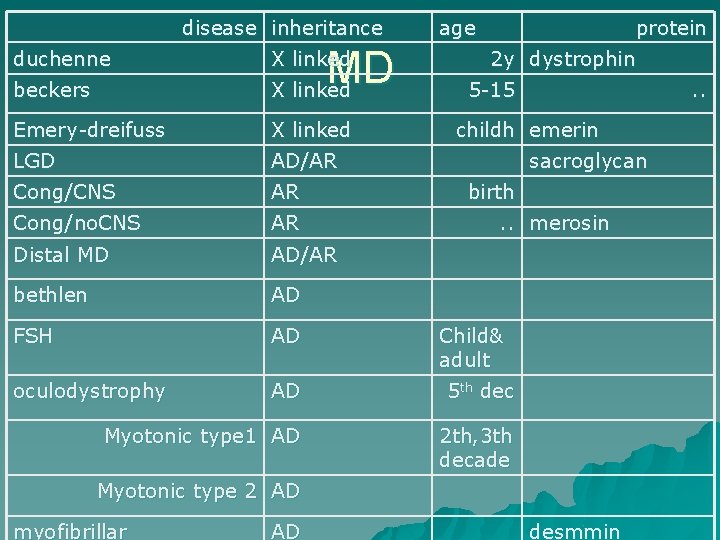
disease inheritance age protein beckers MD X linked Emery-dreifuss X linked LGD AD/AR Cong/CNS AR Cong/no. CNS AR Distal MD AD/AR bethlen AD FSH AD oculodystrophy AD 5 th dec Myotonic type 1 AD 2 th, 3 th decade duchenne X linked 2 y dystrophin 5 -15 . . childh emerin sacroglycan birth. . merosin Child& adult Myotonic type 2 AD myofibrillar AD desmmin

Duchenne MD u Incidence: 1/3500 male birth u 1/3 new mutation u c/p: as early as 2 -3 y with delay milestones u Progressive limb girdle pattern u Fall 5 -6 y/difficult climb stair 8 y, confined to wheelchair 12 y

Joint constructers 6 -10 y u Calf hypertrophy is early u Muscles atrophy late u Progressive kyphscliosis due to Paraspinal muscles weakness u Reflex: biceps/knee/lost by age 10 y u ankle preserved late in disease u Respiratory s/s after age 10 u

u Cardiac: generally asymptomatic u CHF, arrhythmia late u 90% abnormal ECG : tall rt R wave, deep left Q wave u Echo: hypokinesia , dilatation of ventricular wall u GI: intestinal pseudo obstruction u IQ: one SD below N

lab u u u A dystrophin gene deletion can be detected by: DNA analyses from leukocytes by PCR in 2/3 patient or DNA muscles The other 1/3 DX by… muscles biopsy( dystrophin def by stain &WB , typical features of MD) CK: 20 -100 XN , decline later EMG: myopathic &fibrillation Note : if DNA study +ve no need for EMG &muscles biopsy

Beckers MD Is milder form u 5/100, 000 u Age : 5 -15 y u Wheelchair at 30 y u Cardiac similar to duchenne u Death by age 40 u Dx: DNA, muscle biopsy decrease in dystrophin u CK: moderatly elevated u

treatment u No treatment prevent the progression corticosteroid : controlled trial with predinsone 0, 75 mg/kg demonstrate moderate improvement in strength &delay progression to wheel chair& respiratory compromise

Emery-dreifuss X linked u onset : childhood u Triad of: 1 -early contracture elbow, ankle &posterior cervical 2 -progressive scapulohumroperoneal 3 -cardiomyopathy with atrial conduction defect u

u CK : normal to or only moderate elevated u The muscle biopsy : myopathic &fewer dystrophic u DNA: mutation gene in Xq 28 code for protien emerin

Limb girdle dystrophy u u AR majority Onset: adolescence or late childhood: sever child recessive muscular dystrophy

AR: defect in sacroglycan component of the DGC( sacroglycanopathy) u Alpha sacrglycan adhelin is account for 20% u Onset: childhood& variable u No intellectual impairment or cardiac u Muscle biopsy : immune stain absent or diminished for sacroglycan u

u AD: onset: second and third decades u Protein defect: caveolin-3 u There are multiple subtypes u AD type 1: 1 A, 1 B … u AR type 2:

Congenital muscular dystrophy AR Perinatal onset u c/p: hypotonia &proximal weakness, arthrogryposis u Two types u CNS involvement: sever mental retardation , visual, seizure. . cerebrocular dysplasia, progressive death by age 10 -12 u No CNS : classic type MRI (hypomyelination), benign outcome, non progressive u Muscle biopsy : dystrophy… u

FSH u u u u Inheritance: AD Variable expression within the families Age: childhood or adult life C/P: weakness early facial then descending to scapula stabilizer muscles &muscles of the upper limb& distal weakness. . peroneal , the rate of progression to forearm &pelvic girdle Asymmetrical/ deltoid preserved / joint contracture are uncommon Popeye hand/ winging scapula/ no muscle hypertrophy Early onset worse prognosis 20% require wheelchair

Work up u CK: N or mild elevation u Muscles biopsy: myopathic dystrophic& occasionally prominent mononuclear infiltrate u Gene: ch 4 q 35 gene deletion

Myotonic dystrophy u u u AD, CTG repeat Affect : skeletal, cardiac, smooth muscles, eye, endocrine &brain Onset : at any age , usually at late 2 nd decade Some individual can be symptoms free their entire life Sever form : congenital myotonic dystrophy

u C/P: weakness: (facial, temporalis wasting, ptosis, neck flexor, distal weakness progress to involve limb girdle) u Weakness >myotonia u May be areflexic

systemic u u u u u Posterior sub scapular cataract Testicular atrophy& impotence Intellectual impairment Hypersomnia (central & obstructive) Respiratory failure Elevation of serum glu, rarely frank DM GI: dysphagea, pseudo obstruction Cardiac conduction defect sudden death Fetal loss in female

PROMM u AD u Proximal weakness, no distal weakness u Myotonia &myalgia u Less cardiac &other organ involvement except cataract

Work up u CK: N or mild elevation u EMG: myopathic & myotonia u Muscle biopsy: atrophic, non specific u Gene : CTG repeat >50 in ch 19 q 13. 2

ttt u Myotonia rarely sever to require tt: phenytoin is the only safe drug u Annual ECG. . pacemaker may required u Positive pressure ventilation support u High risk in surgery (cardiac &respiratory) u Sedation & opiod use with caution

Distal dystrophy u Types u AD: 4 th &6 th decade u AR: in early adult onset/late second or early 3 rd u CK : elevated 200 x. N AR

oculopharengeal AD u Onset: 5 th &6 th decade u Ptosis &dysphagea later all extra ocular muscles &extremities affected (limb girdle) but distal can be significant in some variant u Slow progressive , death from aspiration pneumonia or starvation u Ck: n or mild elevated u Muscle biopsy : rim vacuoles u Genetic GCG repeat in ch 14 u


Congenital myopathy u Are distinguished from dystrophy in three respect: u Characteristic morphologic alteration u At birth u Non progressive u However there are exception to all these generalization u Inheritance: are variable

u u u c/p: hypotonia with subsequent developmental delay Reduce muscles bulk, slender body build &long narrow face Skeletal abnormalities: high arched palate , pectus exacavitum, kyphscliosis, dislocated hip, pes cavus) u Absent or reduced muscle stretch reflex u Weakness: limb girdle mostly, but distal weakness exist CK &EMG may be normal Muscle biopsy: the diagnostic method u u

Central core myopathy u Characterized by discrete zones of myofibrillar disruption in the center of muscles fiber u AD but can be sporadic u Mutation ch 19, similar to malignant hyperthermia patient u So anesthesia precaution are necessary

Nemaline myopathy Pathology: the presence of rods or melamine bodies within muscles fiber u AD or AR u c/p: u Sever neonatal form which is fatal in the first year of life u Mild static u Slowly progressive from birth or early childhood u Note : rods can present in HIV related myopathy , some inflammatory u

(Centro nuclear (myotubular u Pathology: large central nuclei in the muscle fiber u X linked/AD/AR u sever neonatal/static or slowly progressive u c/p: ptosis & opthalmoparesis u Genetic defect: mutation in myotubularin gene Xp 28

Metabolic myopathy

Metabolic myopathy u Glucose/glycogen metabolism u Fattay acid metabolism u Purine nucleotide u mitochondrial

Metabolic myopathy u Clues to hereditary metabolic myopathy u Excersize induce weakness &myoglobinuria…glycogen &lipid u Part of diffuse neurological syndrome…mitochondrial

Glucose/glycogen Glucose &its storage is essential for the short term anaerobic energy (glycogensis) u Two clinical presentation: u 1 -dynamic: type V/V 111/1 X//XX 1 u 2 -static: fix weakness 1/111/1 V u Inheritance: AR except for phosphoglycerate kinase u

Glycogensis with exercise u u u u intolerance C/P: exercise intolerance in the childhood followed by excertional induced muscle pain &myoglobinurea in sec or 3 rd decade. . (Second wind phenomena) work up: CK/EMG normal between the attack in early stage but after attack( myopathic &fibrillation) Forearm exercise test Enzyme assay Muscle biopsy Genetic for mutation

What is 0 ther causes of ? myoglobinurea

Glycogensis with fixed weakness Acid maltase deficiency: u Enzyme convert glycogen to glucose u Three clinical variant: u Infantile: pompes: progressive weakness , enlargement of heart, tongue &liver death by age 2 u Juvenile type: proximal weakness, may calf hypertrophy death by age 20 from respiratory failure u Adult type: 2&7 th progressive limb girdle or scapuloperoneal. no liver , no heart involvement u

Work up u CK : moderately increased u EMG: myopathic changes &myotonic discharge in paraspinus u Enzyme assay: u Muscle biopsy: a vacuolar myopathy with high glycogen content u Genetic: mutation in ch 17

Fatty acid metabolism u Lipids are essential for aerobic metabolism u Dynamic & static u CPT: carnitine palmitoyl transeferase deficiency u Carnitine deficiency

CPT u u u Type 1: infancy &child hood with hepatic dysfunction Type 2: exertional myalgia &myoglobinurea, it is the most frequently definable metabolic defect presenting with myoglobinurea AR , gene 1 p 32 The attacks occur after prolonged exercise, fasting, febrile illness Unlike mecardle disease the patient can tolerate brief exercise , no second wind phenomena Muscle strength are normal at rest

lab CK: n at rest u Forearm exercise test : N u EMG: n at rest , &myopathic during the attack u Muscle biopsy: usually N , except of myopathic changes after rhabdomylsis u Enzyme assay u ttt &meal frequency: increase CHO intake &education about fasting &exercise u

Mitochondrial u Kearns-sayer: opthalmoplegia, retinitis pigmentosa, heart block, hearing loss, short stature, ataxia, delayed 2 nd sexual characteristic, PN, respiratory u MERF: myoclonic epilepsy, generalized seizure, ataxia, dementia, hearing loss, optic atrophy , PN, cardiomyopathy &cutenous lipoma u MNGLE: mitochondrial neurogastrointestinal encephalomyopathy POLIP : polyneuropathy, opthalmoplasia, leukoencephalopathy& intestinal pseudo obstruction u

channelopathy u Non dystrophic myotonia u Periodic paralysis u It due to mutation in different channels gene leading to : u Hyper excitability : myotonia u In excitability: paralysis

Chloride channelopathy u Mutation in CL channel. . hyperexcitability after depolarization u Myotonia congenita: u AD. . thomsen /AR: becker u C/P: muscle hypertrophy, myotonia/becker type has fluctuating limb girdle weakness

Sodium channleopathy u AD Onset: first decade Phenotypic types: Paramyotonia congenita u Hyperkalemic periodic paralysis u myotonia : Potassium sensitive disorder : myotonia fluctuant myotonia permanent acetazolamide responsive myotonia u u u

Calcium channelopathy u Hypokalemic u malignant hyperthermia

C/P of channelopathy

Paramytonia congenita AD u Onset : 1 st decade u Paradoxical myotonia (Aggravated by warm as well cold) u Face , neck, forearm u After several attempt of eye closure the patient can not open the eye u ttt: Na channels blocker mexiletine u

Hyperkalamic periodic paralysis u u u u K sensitive periodic paralysis Onset : 1 st decade Attack last: 1 -2 h During attack: areflexic with no ocular or respiratory muscles weakness Strength is n between the attack, but some patient has interictal limb girdle weakness Some families have myotonia ¶myotonia Aggravated: fasting/cold, shortly after exercise, K load, early AM

u Episodes are rarely serous enough to require acute ttt u ttt: u oral CHO u Prevention: thiazide, B agonist, low K, high CHO u Avoid fasting, strenuous exercise/

myotonia u No weakness u Aggravated by K diet/ excretion u Can response to acetazolamide

hypokalemia AD: u It is the most frequent form of periodic paralysis u Common in male u Age: adolescence u The attacks 3 -24 h/vague prodorme of stiffness &heaviness& rarely ocular, bulbar, respiratory involved u Early Myotonia of eyelid & late interictal proximal weakness u

Aggravated: CHO meal, cold, hrs post exercise, sleep u Work up: K level q 30 min /TFT/ u R/O 2 nd causes of hypokalemia u Tttt: u Acute: oral K Q 30 min , if symptoms sever iv K u Prevention: u Low CHO, low sodium diet , spirnolactone, trimetrine u
