Causes of acquired hemolytic anemia Entrapment Immune WarmreactiveIg













- Slides: 21


Causes of acquired hemolytic anemia • • • Entrapment Immune – – Warm-reactive(Ig. G) antibody Cold-reactive Ig. M antibody (cold agglutinin disease) Cold-reactive Ig. G antibody (paroxysmal cold hemoglobinuria) Drug-dependent antibody • Autoimmune • Haptene Traumatic hemolytic anemia – Impact hemolysis – Macrovascular defects – prostheses – Microvascular causes • Thrombotic thrombocytopenic purpura/hemolytic-uremic syndrome • Other causes of microvascular abnormalities • Disseminated intravascular hemolysis Hemolytic anemia due to toxic effects on the membrane – Spur cell hemolytic anemia – External toxins • Animal or spider bites • Metals (e. g. , copper) • Organic compounds Paroxysmal nocturnal hemoglobinuria

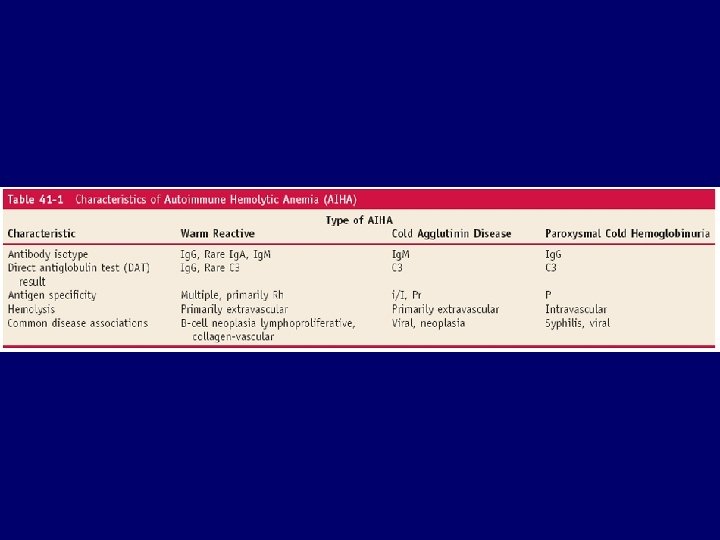
IMMUNE HEMOLYTIC ANMEIA • Warm-reactive antibody (Ig. G) • Cold-reactive Ig. M antibody (cold agglutinin disease) • Cold-reactive Ig. G antibody (PCH) • Drug-dependent antibody 1. Autoimmune 2. Haptene

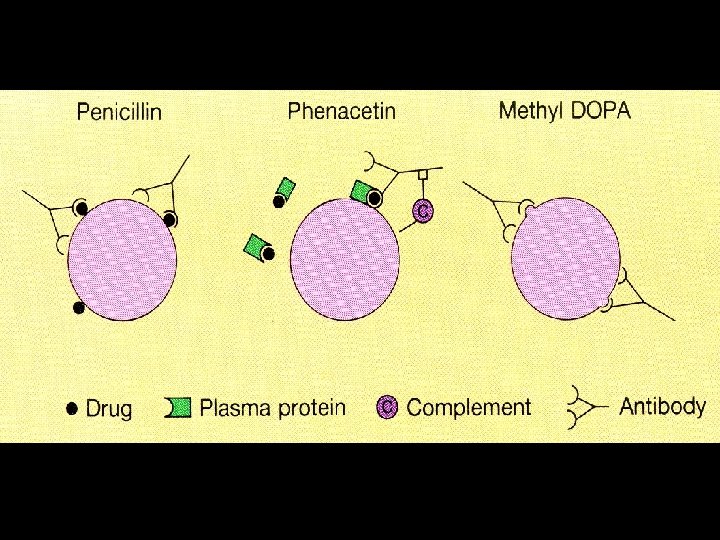
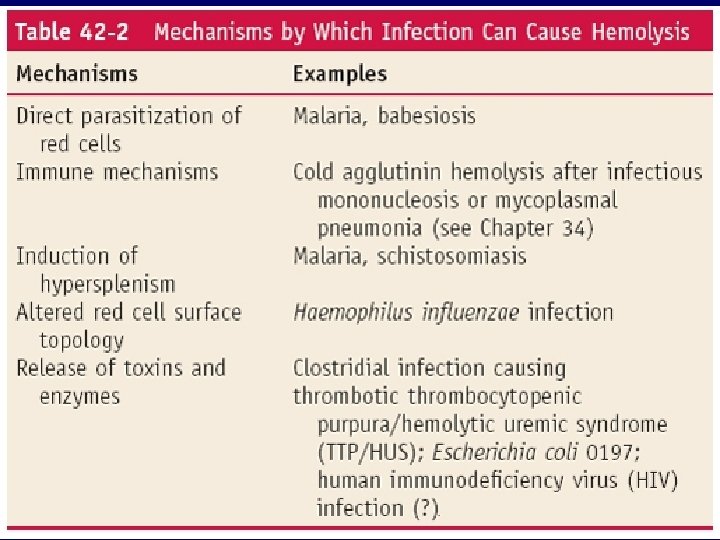
Hemolysis due to antibodies Warm-antibody immunohemolytic anemia • • Idiopathic Lymphomas: Chronic lymphocytic leukemia, non-Hodgkin’s lymphomas, Hodgkin’s disease (infrequent) SLE and other collagen-vascular diseases Drugs – Alpha-Methyldopa type (autoantibody to Rh antigens) – Penicillin type (stable hapten) – Quinidine type (unstable hapten) • • Postviral infections Other tumors (rare) Cold-antibody immunohemolytic anemia • Cold agglutinin disease – Acute: mycoplasma infection, infectious mononucleosis – Chronic: idiopathic, lymphoma • Paroxysmal cold hemoglobinuria

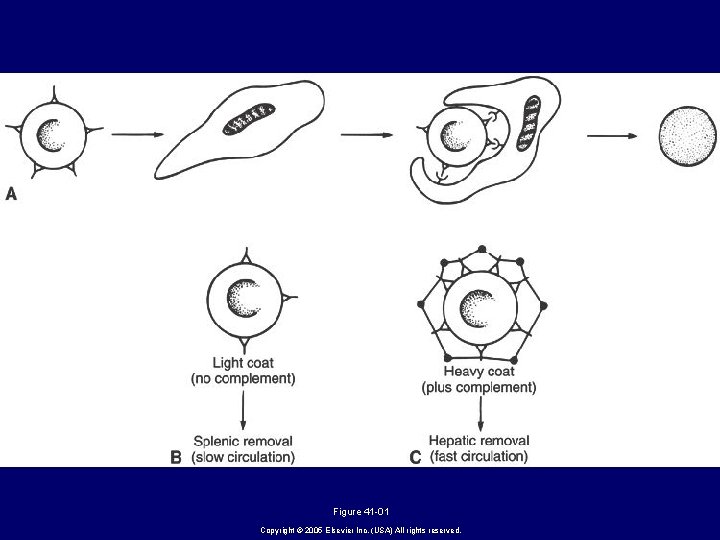
Figure 41 -01 Copyright © 2005 Elsevier Inc. (USA) All rights reserved.



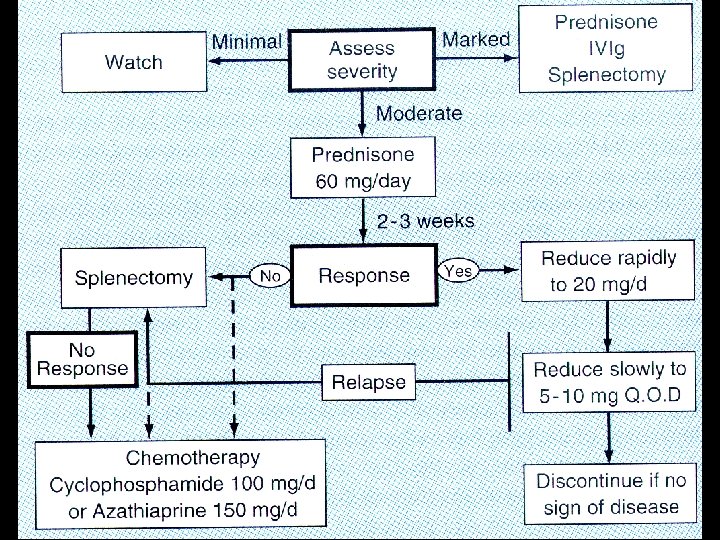
IMMUNE HEMOLYTIC ANEMIA Warm Cold agglutinin Age Young Older Sex Female > male Male > female Hemolysis Extravascular Intra and/or extravascular Antibody Optimal temperature 37 o. C 4 o. C Immunoglobulin Ig. G Ig. M C' fixation no yes Coombs' reaction Ig. G yes no Complement no or yes Therapy Corticosteroid 60% benefit usually no Splenectomy 60% benefit no Immunosuppressive agents probable benefit Avoidance of cold no benefit








Disturbances of the formed elements of blood secondary to intravascular trauma Etiology Fragments Hemolysis Impact: march hemoglobinuria, karate, playing bongo drums, etc. Cardiac (turbulence): Aortic valve prosthesis ++++ Ostium primum repair ++++ Mitral valve prosthesis ++ ++ Calcific aortic stenosis + ± Vessel disease* +++ + + Thrombotic thrombocytopenic purpura Hemolytic uremic syndrome ++++ Disseminated intravascular coagulation Thrombocytopenia 0 ++++ ± ++++ 0 0 ++++ ++ ++++ * Malignant hypertension, Eclampsia, Renal graft rejection, Hemangiomas, Immune disease (scleroderma)




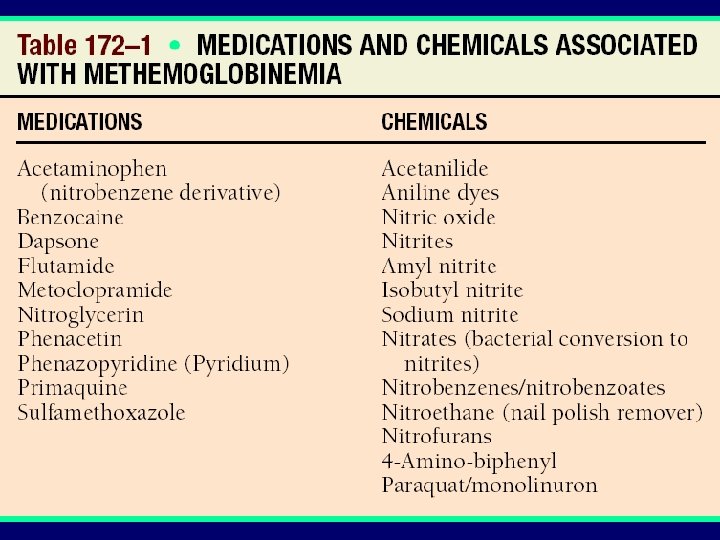
Acquired Hemoglobin Abnormalities: Methemoglobinemia • dominantly inherited abnormality (hemoglobin M) • recessively inherited deficiency of enzyme (methemoglobin reductase) • exposure to drugs or chemicals nitrites, xylocaine, benzene derivatives – life-threatening if > 30 -40% is methemoglobin: methylene blue 1 -2 mg/Kg infusion

Acquired Hemoglobin Abnormalities: Sulfhemoglobinemia • drugs like sulfonamide • disappear spontaneously Carboxyhemoglobinemia • Impairs delivery of oxygen • cherry-red color • faulty heaters, smokers