RESPIRATORY FUNCTIONS OTHER FUNCTIONS OF RESPIRATORY SYSTEM PULMONARY














![LUNG VOLUMES [ l ] INSPIRATORY RESERVE VOLUME IRV maximal inspiratory level ~2. 5 LUNG VOLUMES [ l ] INSPIRATORY RESERVE VOLUME IRV maximal inspiratory level ~2. 5](https://slidetodoc.com/presentation_image_h/ac6b24888e9323e318c4842cee2fb385/image-22.jpg)







- Slides: 39

RESPIRATORY FUNCTIONS OTHER FUNCTIONS OF RESPIRATORY SYSTEM PULMONARY DEFENCE FUNCTIONS (e. g. mucociliary clearance, function of pulmonary macrophages, …) METABOLIC AND ENDOCRINE FUNCTIONS (e. g. production of surfactant, conversion of angiotensin I to angiotensin II, …)

RESPIRATORY SYSTEM AIR PASSAGES (CONVECTION) LUNGS AS GAS EXCHANGING ORGAN PUMP THAT ENABLES VENTILATION OF THE LUNGS (chest wall with respiratory muscles) TRANSPORT OF O 2 AND CO 2 IN THE BLOOD NERVOUS SYSTEM CONTROLLING THE RESPIRATORY MUSCLES (areas in CNS, efferent motor neurons to respiratory muscles, and afferent neurons from various receptors) 1

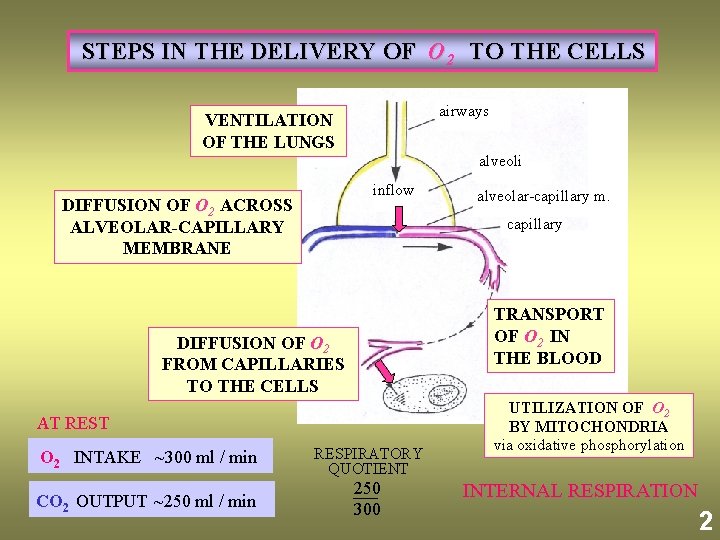
STEPS IN THE DELIVERY OF O 2 TO THE CELLS VENTILATION OF THE LUNGS airways alveoli inflow DIFFUSION OF O 2 ACROSS ALVEOLAR-CAPILLARY MEMBRANE alveolar-capillary m. capillary TRANSPORT OF O 2 IN THE BLOOD DIFFUSION OF O 2 FROM CAPILLARIES TO THE CELLS AT REST O 2 INTAKE ~300 ml / min RESPIRATORY QUOTIENT CO 2 OUTPUT ~250 ml / min 250 300 UTILIZATION OF O 2 BY MITOCHONDRIA via oxidative phosphorylation INTERNAL RESPIRATION 2

PLAN I BASIC PHYSICAL FEATURES OF GASES II AIR PASSAGES III MEASURABLE PARAMETERS · · DEAD SPACE LUNG VOLUMES FUNCTIONAL INVESTIGATIONS CHARACTERISTIC PRESSURES IV COMPOSITION OF ALVEOLAR AIR V ALVEOLAR-CAPILLARY MEMBRANE

GENERAL CHARACTERISTICS OF GASES RAPID PRESSURE EQUILIBRATION in the closed volume MOVEMENT proceeds from the areas of high pressure to the areas of low pressure -DOWN THE PRESSURE GRADIENT Diffusion of a gas ACROSS a BARRIER (between two areas) depends on the PROPERTY of the barrier IN A MIXTURE OF GASES RATE of DIFFUSION of GAS COMPONENTS depends on the INDIVIDUAL PARTIAL PRESSURE GRADIENTS In a mixture of gases EQUILIBRATED WITH A LIQUID each component DISSOLVES independently in proportion to its: PARTIAL PRESSURE in the gaseous phase SOLUBILITY in the fluid 3

RELATIONS BETWEEN n V MEASURED QUANTITIES T P IDEAL GAS EQUATION P= n RT V PV=n. RT P - pressure [Pa] [mm Hg] n - amount of substance [mol] V - volume [m 3] [l] T - absolute temperature [K] R - universal gas constant [J/K. mol] If n and T do not change then PV = constant physical unit of work and energy [ J ] 4

PARTIAL PRESSURES IN A MIXTURE OF GASES Dalton´s law - law of partial pressures Mixture of two gas components (in a given volume) n 1 , n 2 - amounts of gas substances ntot = n 1 + n 2 F 1 + F 2 = 1 According to Dalton´s law: PARTIAL PRESSURES can be expressed in terms of fractions: P 1 = F 1 Ptot P 2 = F 2 Ptot P 1 + P 2 = Ptot 5

COMPOSITION OF DRY ATMOSPHERIC AIR O 2 20. 98 % N 2 78. 06 % CO 2 0. 04 % FO 2 0. 21 FN 2 0. 78 FCO 2 = 0. 0004 other constituents BAROMETRIC (ATMOSPHERIC) PRESSURE AT SEA LEVEL 1 atmosphere = 760 mm Hg PARTIAL PRESSURES OF GASES IN DRY AIR AT SEA LEVEL PO 2 = 760 x 0. 21 = 160 mm Hg PN 2 = 760 x 0. 78 = 593 mm Hg PCO 2 = 760 x 0. 0004 = 0. 3 mm Hg 1 k. Pa = 7. 5 mm Hg (torr) 6

I PHYSICAL FEATURES OF GASES II AIR PASSAGES III MEASURABLE PARAMETERS · · DEAD SPACE LUNG VOLUMES FUNCTIONAL INVESTIGATION CHARACTERISTIC PRESSURES IV COMPOSITION OF ALVEOLAR AIR V ALVEOLAR-CAPILLARY MEMBRANE

AIR PASSAGES ANATOMICAL DEAD SPACE – CONDUCTING ZONE NASAL PASSAGES Other functions: PHARYNX air is warmed, cleaned and takes up water vapour LARYNX respiratory reflex responses to the irritants TRACHEA speech and singing (special function of larynx) BRONCHIOLES TERMINAL BRONCHIOLES RESPIRATORY TRANSITIONAL ZONE RESPIRATORY BRONCHIOLES ALVEOLAR DUCTS ZONE TOTAL ALVEOLAR VOLUME at the end of quiet expiration ~3 l TOTAL AREA ~ 100 m 2 7

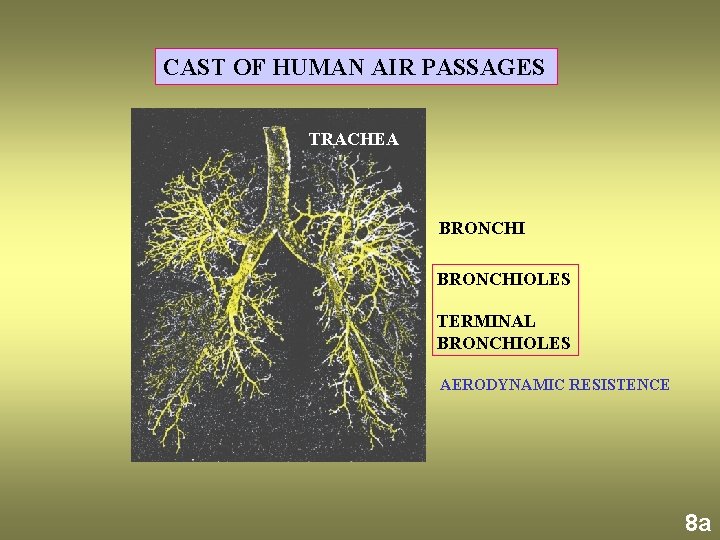
CAST OF HUMAN AIR PASSAGES TRACHEA BRONCHIOLES TERMINAL BRONCHIOLES AERODYNAMIC RESISTENCE 8 a

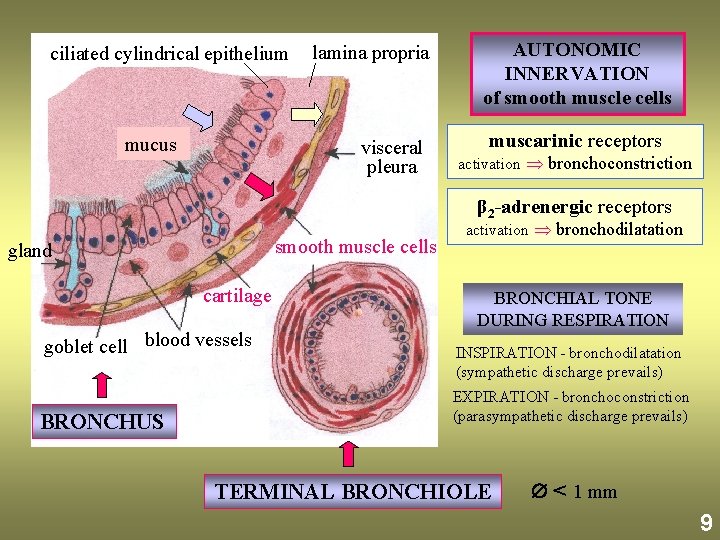
ciliated cylindrical epithelium lamina propria AUTONOMIC INNERVATION of smooth muscle cells visceral muscarinic receptors activation bronchoconstriction pleura mucus β 2 -adrenergic receptors smooth muscle cells gland cartilage goblet cell blood vessels BRONCHUS activation bronchodilatation BRONCHIAL TONE DURING RESPIRATION INSPIRATION - bronchodilatation (sympathetic discharge prevails) EXPIRATION - bronchoconstriction (parasympathetic discharge prevails) TERMINAL BRONCHIOLE < 1 mm 9

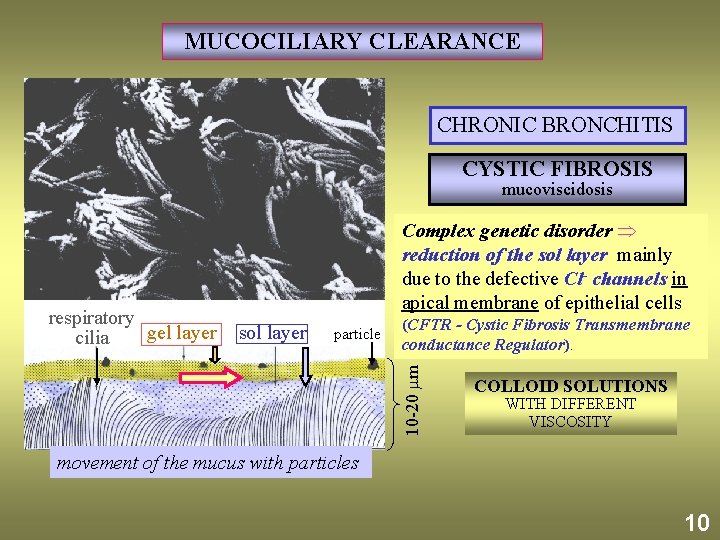
MUCOCILIARY CLEARANCE CHRONIC BRONCHITIS CYSTIC FIBROSIS mucoviscidosis particle (CFTR - Cystic Fibrosis Transmembrane conductance Regulator). 10 -20 m respiratory gel layer sol layer cilia Complex genetic disorder reduction of the sol layer mainly due to the defective Cl- channels in apical membrane of epithelial cells COLLOID SOLUTIONS WITH DIFFERENT VISCOSITY movement of the mucus with particles 10

I PHYSICAL FEATURES OF GASES II AIR PASSAGES III MEASURABLE PARAMETERS · · DEAD SPACE LUNG VOLUMES FUNCTIONAL INVESTIGATION CHARACTERISTIC PRESSURES IV COMPOSITION OF ALVEOLAR AIR V ALVEOLAR-CAPILLARY MEMBRANE

VT = VA + VD VT tidal volume ~ 500 ml VA part of tidal volume entering alveoli ~ 350 ml VD part of tidal volume remaining in the dead space ~ 150 ml f = 12/min ∙ V = VT x f PULMONARY MINUTE VENTILATION 6 l/min · VA = VA x f ALVEOLAR VENTILATION 4. 2 l/min · VD = VD x f DEAD SPACE VENTILATION 1. 8 l/min At the same PULMONARY VENTILATION (6 l/min) ALVEOLAR VENTILATION at RAPID SHALLOW BREATHING can be SIGNIFICANTLY REDUCED and INADEQUATE in comparison with SLOW DEEP BREATHING 11

DEAD SPACE IN RESPIRATORY SYSTEM TOTAL GAS VOLUME NOT EQUILIBRATED WITH BLOOD (without exchange of gasses) ANATOMICAL dead space - volume of air passages FUNCTIONAL (total) dead space ANATOMICAL dead space + total VOLUME of ALVEOLI without functional capillary bed IN HEALTHY INDIVIDUALS both spaces are practically identical 12

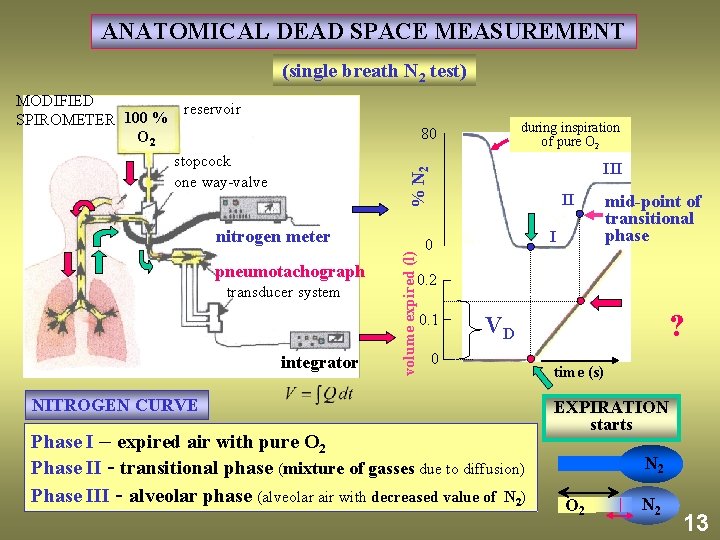
ANATOMICAL DEAD SPACE MEASUREMENT (single breath N 2 test) MODIFIED reservoir SPIROMETER 100 % O 2 during inspiration of pure O 2 80 III % N 2 stopcock one way-valve pneumotachograph transducer system integrator volume expired (l) nitrogen meter II I 0 mid-point of transitional phase 0. 2 0. 1 ? VD 0 NITROGEN CURVE Phase I – expired air with pure O 2 Phase II - transitional phase (mixture of gasses due to diffusion) Phase III - alveolar phase (alveolar air with decreased value of N 2) time (s) EXPIRATION starts N 2 O 2 N 2 13

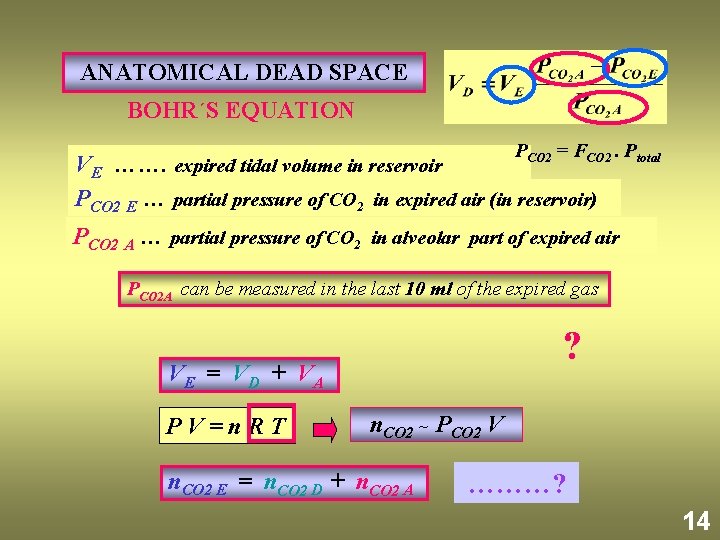
ANATOMICAL DEAD SPACE BOHR´S EQUATION P = F CO 2 VE ……. expired tidal volume in reservoir PCO 2 E … partial pressure of CO 2 in expired air (in reservoir) . Ptotal PCO 2 A … partial pressure of CO 2 in alveolar part of expired air PCO 2 A can be measured in the last 10 ml of the expired gas ? VE = VD + VA PV=n. RT n. CO 2 ~ PCO 2 V n. CO 2 E = n. CO 2 D + n. CO 2 A ………? 14

FUNCTIONAL (TOTAL) DEAD SPACE BOHR´S EQUATION FUNCTIONAL DEAD SPACE is obtained if alveolar PCO 2 A is replaced by arterial partial pressure PCO 2 a HELTHY SUBJECTS - both partial pressures are nearly identical FUNCTIONAL dead space equals ANATOMICAL dead space RESPIRATORY DISEASES - numerous alveoli are without functional capillary bed PCO 2 A PCO 2 a 15

I PHYSICAL FEATURES OF GASES II AIR PASSAGES III MEASURABLE PARAMETERS · · DEAD SPACE LUNG VOLUMES FUNCTIONAL INVESTIGATION CHARACTERISTIC PRESSURES IV COMPOSITION OF ALVEOLAR AIR V ALVEOLAR-CAPILLARY MEMBRANE

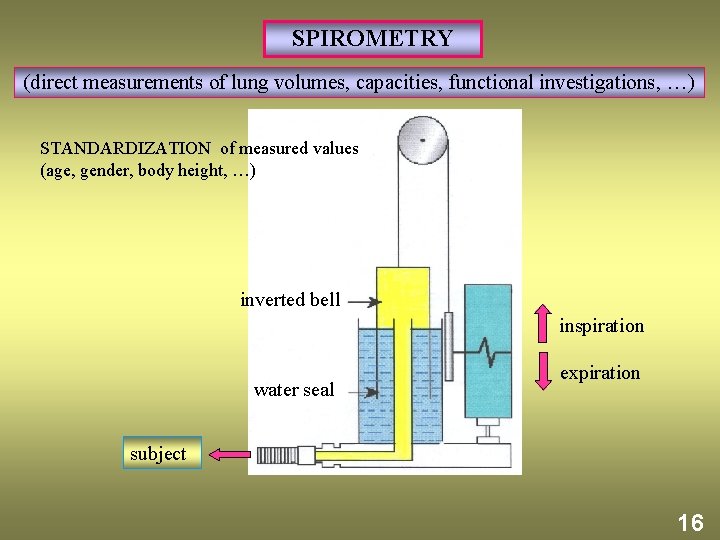
SPIROMETRY (direct measurements of lung volumes, capacities, functional investigations, …) STANDARDIZATION of measured values (age, gender, body height, …) inverted bell inspiration water seal expiration subject 16
![LUNG VOLUMES l INSPIRATORY RESERVE VOLUME IRV maximal inspiratory level 2 5 LUNG VOLUMES [ l ] INSPIRATORY RESERVE VOLUME IRV maximal inspiratory level ~2. 5](https://slidetodoc.com/presentation_image_h/ac6b24888e9323e318c4842cee2fb385/image-22.jpg)
LUNG VOLUMES [ l ] INSPIRATORY RESERVE VOLUME IRV maximal inspiratory level ~2. 5 end of quiet inspiration TIDAL VOLUME VT EXPIRATORY RESERVE VOLUME ERV ~1. 7 ~1. 3 RESIDUAL VOLUME RV end of quiet expiration maximal expiratory level DILUTION METHOD He n=c. V Vr …. . reservoir volume ci He …known initial concentration of He cf He …final measured concentration of He RV He reservoir (V) n. RV He = ni, r He – nf, r He (difference between initial and final amounts of He in reservoir) RV reservoir (V) 17

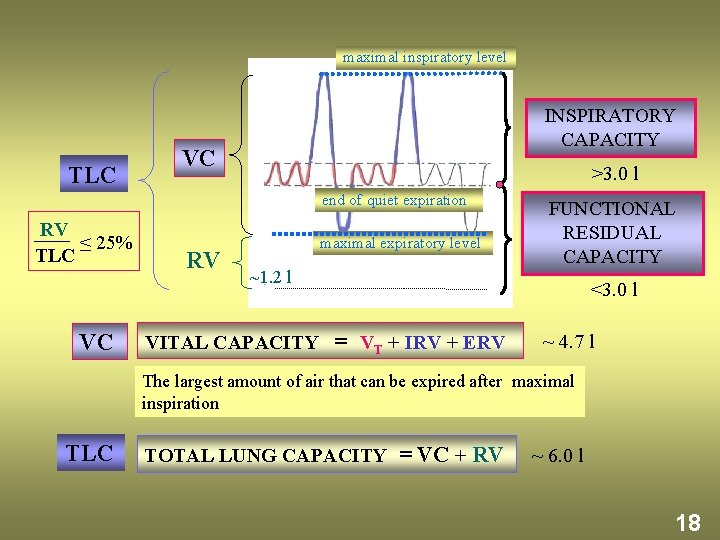
maximal inspiratory level TLC INSPIRATORY CAPACITY VC >3. 0 l end of quiet expiration RV ≤ 25% TLC VC RV maximal expiratory level ~1. 2 l VITAL CAPACITY = VT + IRV + ERV FUNCTIONAL RESIDUAL CAPACITY <3. 0 l ~ 4. 7 l The largest amount of air that can be expired after maximal inspiration TLC TOTAL LUNG CAPACITY = VC + RV ~ 6. 0 l 18

I PHYSICAL FEATURES OF GASES II AIR PASSAGES III MEASURABLE PARAMETERS · · DEAD SPACE LUNG VOLUMES FUNCTIONAL INVESTIGATION CHARACTERISTIC PRESSURES IV COMPOSITION OF ALVEOLAR AIR V ALVEOLAR-CAPILLARY MEMBRANE

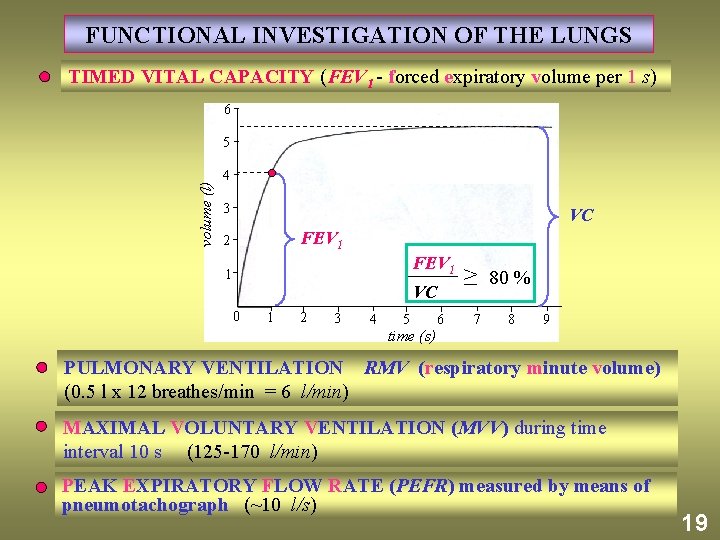
FUNCTIONAL INVESTIGATION OF THE LUNGS TIMED VITAL CAPACITY (FEV 1 - forced expiratory volume per 1 s) 6 volume (l) 5 4 3 VC FEV 1 2 FEV 1 1 VC 0 1 2 3 4 5 time (s) 6 ≥ 80 % 7 8 9 PULMONARY VENTILATION RMV (respiratory minute volume) (0. 5 l x 12 breathes/min = 6 l/min) MAXIMAL VOLUNTARY VENTILATION (MVV) during time interval 10 s (125 -170 l/min) PEAK EXPIRATORY FLOW RATE (PEFR) measured by means of pneumotachograph (~10 l/s) 19

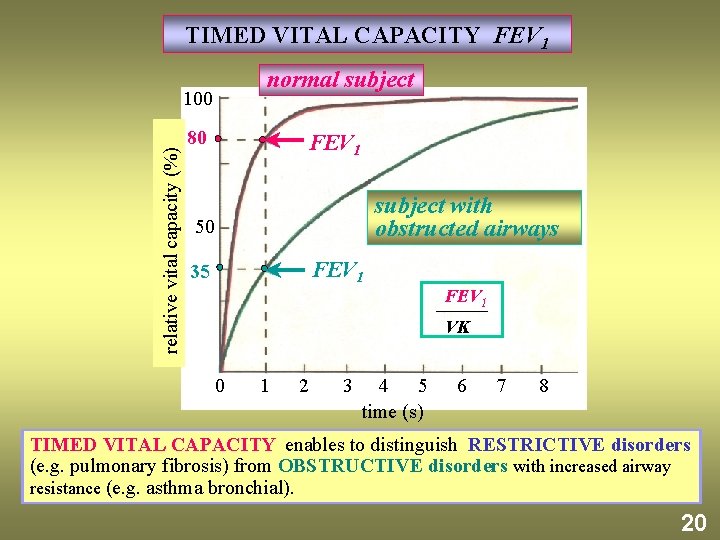
TIMED VITAL CAPACITY FEV 1 normal subject relative vital capacity (%) 100 80 FEV 1 subject with obstructed airways 50 FEV 1 35 FEV 1 VK 0 1 2 3 4 5 time (s) 6 7 8 TIMED VITAL CAPACITY enables to distinguish RESTRICTIVE disorders (e. g. pulmonary fibrosis) from OBSTRUCTIVE disorders with increased airway resistance (e. g. asthma bronchial). 20

I PHYSICAL FEATURES OF GASES II AIR PASSAGES III MEASURABLE PARAMETERS · · DEAD SPACE LUNG VOLUMES FUNCTIONAL INVESTIGATION CHARACTERISTIC PRESSURES IV COMPOSITION OF ALVEOLAR AIR V ALVEOLAR-CAPILLARY MEMBRANE

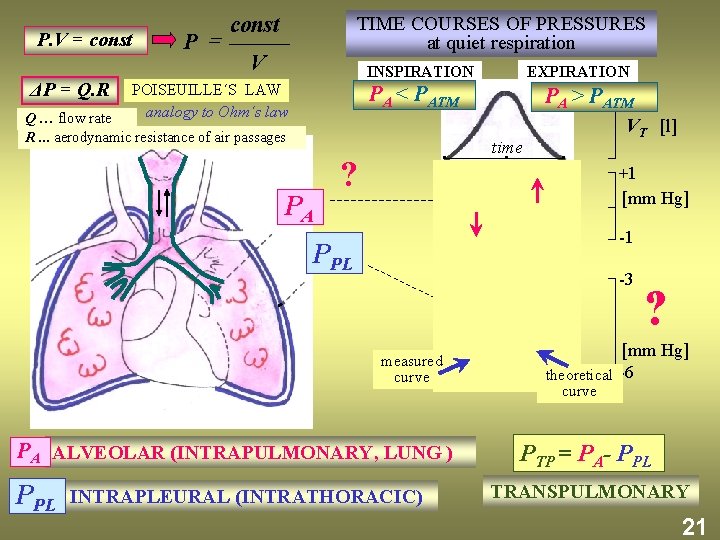
P. V = const ΔP = Q. R P = const TIME COURSES OF PRESSURES at quiet respiration V EXPIRATION INSPIRATION POISEUILLE´S LAW analogy to Ohm´s law PA < PATM Q … flow rate R. . . aerodynamic resistance of air passages PA > PATM VT [l] time ? +1 [mm Hg] -1 PPL -3 measured curve PA ALVEOLAR (INTRAPULMONARY, LUNG ) PPL INTRAPLEURAL (INTRATHORACIC) ? [mm Hg] theoretical -6 curve PTP = PA- PPL TRANSPULMONARY 21

I PHYSICAL FEATURES OF GASES II AIR PASSAGES III MEASURABLE PARAMETERS · · DEAD SPACE LUNG VOLUMES FUNCTIONAL INVESTIGATION CHARACTERISTIC PRESSURES IV COMPOSITION OF ALVEOLAR AIR V ALVEOLAR-CAPILLARY MEMBRANE

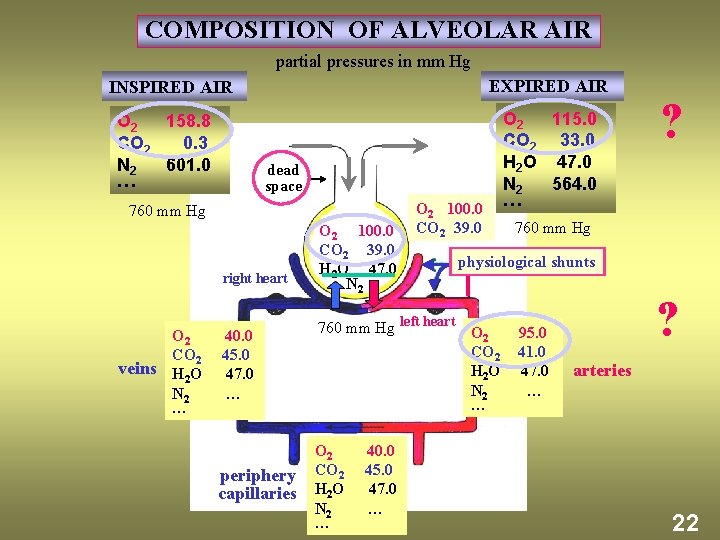
COMPOSITION OF ALVEOLAR AIR partial pressures in mm Hg EXPIRED AIR INSPIRED AIR O 2 158. 8 CO 2 0. 3 N 2 601. 0 … dead space 760 mm Hg right heart O 2 40. 0 CO 2 45. 0 veins H O 47. 0 2 N 2 … … O 2 100. 0 CO 2 39. 0 H 2 O 47. 0 N 2 O 2 100. 0 CO 2 39. 0 O 2 115. 0 CO 2 33. 0 H 2 O 47. 0 N 2 564. 0 … 760 mm Hg physiological shunts 760 mm Hg left heart O 95. 0 2 CO 2 41. 0 H 2 O 47. 0 N 2 … … O 2 40. 0 periphery CO 2 45. 0 capillaries H 2 O 47. 0 N 2 … … ? ? arteries 22

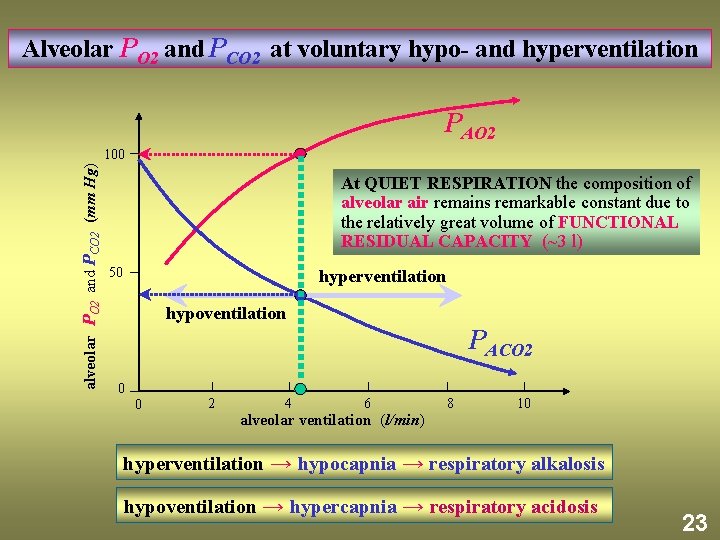
Alveolar PO 2 and PCO 2 at voluntary hypo- and hyperventilation PAO 2 alveolar PO 2 and PCO 2 (mm Hg) 100 At QUIET RESPIRATION the composition of alveolar air remains remarkable constant due to the relatively great volume of FUNCTIONAL RESIDUAL CAPACITY (~3 l) 50 hyperventilation hypoventilation PACO 2 0 0 2 4 6 alveolar ventilation (l/min) 8 10 hyperventilation → hypocapnia → respiratory alkalosis hypoventilation → hypercapnia → respiratory acidosis 23

I PHYSICAL FEATURES OF GASES II AIR PASSAGES III MEASURABLE PARAMETERS · · DEAD SPACE LUNG VOLUMES FUNCTIONAL INVESTIGATION CHARACTERISTIC PRESSURES IV COMPOSITION OF ALVEOLAR AIR V ALVEOLAR-CAPILLARY MEMBRANE

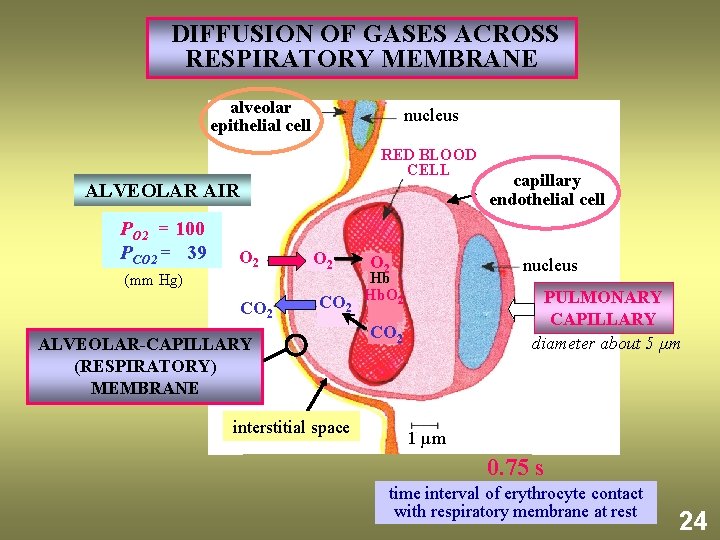
DIFFUSION OF GASES ACROSS RESPIRATORY MEMBRANE alveolar epithelial cell nucleus RED BLOOD CELL ALVEOLAR AIR PO 2 = 100 PCO 2 = 39 O 2 (mm Hg) CO 2 ALVEOLAR-CAPILLARY (RESPIRATORY) MEMBRANE interstitial space capillary endothelial cell O 2 nucleus CO 2 PULMONARY CAPILLARY diameter about 5 µm Hb Hb. O 2 1 µm 0. 75 s time interval of erythrocyte contact with respiratory membrane at rest 24

FACTORS AFFECTING RATE OF DIFFUSION OF GASE IN THE LUNGS (O 2 or CO 2) FICK´S LAW – LAW OF DIFFUSION (ml/min) TOTAL SURFACE AREA OF THE ALVEOLARCAPILARY MEMBRANE A (~ 100 m 2 ) ( A : emphysema) DIFFUSION DISTANCE - THICKNESS OF THE BARRIER l (~1 μm) ( l : inflammation, pulmonary edema) PARTIAL PRESSURE DIFFERENCE (PA - Pc) DIFFUSION COEFFICIENT OF THE GAS k. D determined by molecular mass, solubility of the gas in the respiratory membrane ( k. D : pulmonary fibrosis). 25

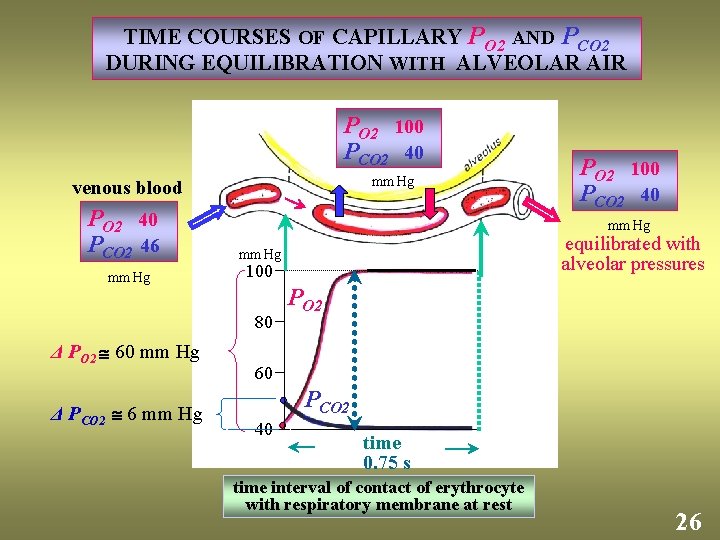
TIME COURSES OF CAPILLARY PO 2 AND PCO 2 DURING EQUILIBRATION WITH ALVEOLAR AIR PO 2 100 PCO 2 40 mm Hg venous blood PO 2 40 PCO 2 46 mm Hg Δ PCO 2 6 mm Hg equilibrated with alveolar pressures mm Hg 100 80 Δ PO 2 60 mm Hg PO 2 100 PCO 2 40 PO 2 60 PCO 2 40 time 0. 75 s time interval of contact of erythrocyte with respiratory membrane at rest 26


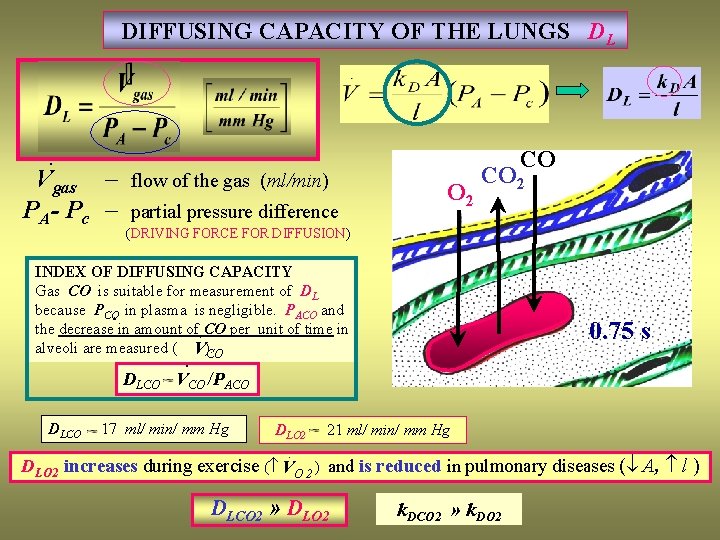
DIFFUSING CAPACITY OF THE LUNGS DL · Vgas – flow of the gas (ml/min) PA- Pc – partial pressure difference CO O 2 CO 2 (DRIVING FORCE FOR DIFFUSION) INDEX OF DIFFUSING CAPACITY Gas CO is suitable for measurement of DL because PCO in plasma is negligible. PACO and the decrease in amount of CO per unit of time in alveoli are measured ( ). VCO 0. 75 s · DLCO VCO /PACO DLCO 17 ml/ min/ mm Hg DLO 2 21 ml/ min/ mm Hg DLO 2 increases during exercise ( VO 2 ) and is reduced in pulmonary diseases ( A, l ) DLCO 2 » DLO 2 k. DCO 2 » k. DO 2

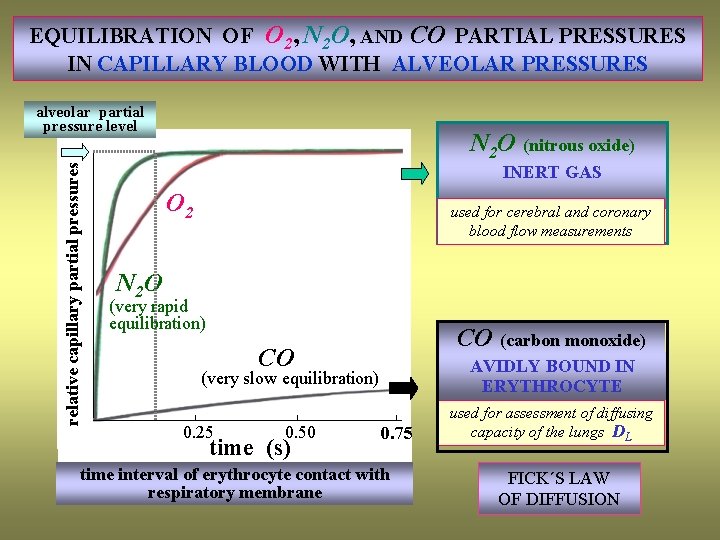
EQUILIBRATION OF O 2, N 2 O, AND CO PARTIAL PRESSURES IN CAPILLARY BLOOD WITH ALVEOLAR PRESSURES relative capillary partial pressures alveolar partial pressure level N 2 O (nitrous oxide) INERT GAS O 2 used for cerebral and coronary blood flow measurements N 2 O (very rapid equilibration) CO (carbon monoxide) CO AVIDLY BOUND IN ERYTHROCYTE (very slow equilibration) 0. 25 0. 50 time (s) 0. 75 time interval of erythrocyte contact with respiratory membrane used for assessment of diffusing capacity of the lungs DL FICK´S LAW OF DIFFUSION

END