Prof Dr Esraa ALMaini 2019 2020 Endometrial hyperplasia






















- Slides: 26

Prof. Dr Esraa AL-Maini 2019 -2020 Endometrial hyperplasia

Endometrial thickness guidelines premenopausal women : Endometrial thickness in normal endometrial vary according to day of cycle ≤ 4 mm on day 4 of the menstrual cycle ≤ 8 mm by day 8.

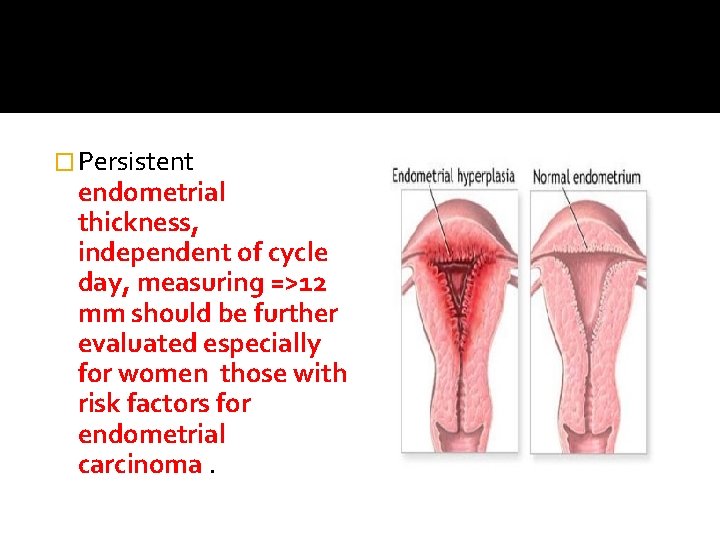
� Persistent endometrial thickness, independent of cycle day, measuring =>12 mm should be further evaluated especially for women those with risk factors for endometrial carcinoma.

Etiology for endometrial hyperplasia. A-Endogenous estrogen. The most common cause Chronic anovulation is associated with _The polycystic ovary syndrome(PCOS) _ Ovarian tumor (eg, granulosa cell tumor _ Obese women B- Exogenous estrogen.

Classification endometrial hyperplasia The World Health Organization classification of endometrial hyperplasia is based upon two factors: 1. Simple or complex glandular/stromal architectural pattern 2. The presence or absence of nuclear atypia

. Endometrial carcinoma is more than 10 -fold more likely in atypical hyperplasia (simple or complex).

Risk factors 1 -Increasing age 2 -Unopposed estrogen therapy 3 -Late menopause (after age 55) 4 -Nulliparity 5 -Polycystic ovary syndrome (Chronic anovulation) 6 -Obesity 7 -Diabetes 8 -Hereditary nonpolyposis colorectal cancer 9 -Tamoxifen 10 -Early menarche 11 -Estrogen secreting tumor 12 -Family history of endometrial, ovarian, breast, or colon cancer

Clinical manifestations. Endometrial hyperplasia should be suspected in: 1 - Women with heavy, prolonged, frequent (ie, less than 21 days). 2 - Irregular uterine bleeding. Abnormal uterine bleeding in perimenopausal or postmenopausal women is the most common clinical symptom of endometrial neoplasia, although such (PMB)bleeding is usually (80%) due to a benign condition.

Diagnostic and surveillance methods for endometrial hyperplesia 1 -Transvaginal sonography; may have a role in diagnosing endometrial hyperplasia in pre- and postmenopausal women 2 -Endometrial biopsy : diagnosis of endometrial hyperplasia requires histological examination of the endometrial tissue. 1 -Office biopsy(out patients) 2 -D/C biopsy. 3 -Hysteroscopic guided biopsy


Indication for evaluation of the endometrium 1 -Abnormal -uterine bleeding with risk factors 2 -Failure to respond to medical treatment for abnormal uterine bleeding 3 -unopposed estrogen replacement therapy 4 - Asymptomatic women presence of endometrial cells on Pap smear if they are at increased risk of endometrial cancer 5 -Women with hereditary nonpolyposis colorectal cancer

B. Indications for additional diagnostic evaluation by hysteroscopy/directed biopsy 1 -Endometrial hyperplasia with atypia by office biopsy, further evaluation by Dilation and curettage (D&C) is needed to exclude a coexistent endometrial adenocarcinoma(% 25) 2. Non diagnostic office biopsy. Endometrial hyperplasia/cancer needs to be excluded in women with a non diagnostic office biopsy. hysteroscopy/directed biopsy 3. Persistent bleeding. After benign endometrial biopsy or treatment of endometrial pathology. hysteroscopy/directed biopsy 4. Postmenopausal women. hysteroscopy/directed biopsy

Management of hyperplasia without atypia � 1 - Observation alone �The risk of progressing to endometrial cancer is less than 5% over 20 years. �The majority o will regress spontaneously during follow-up. �Observation alone with follow-up endometrial biopsies to ensure disease regression can be considerd , especially when identifiable risk factors such as obesity and the use of (HRT) can be reversed.

2 -Treatment with progestogens Higher disease regression rate than observation alone. indications: 1 -In women who fail to regress following observation alone 2 - In symptomatic women with abnormal uterine bleeding. Types of progesterone; 1 - Local progesterone ([LNG-IUS]) should be the first-line medical treatment because compared with 2: It has a higher disease regression rate More favourable bleeding profile It is associated with fewer adverse effects. 2 -Continuous oral progesterone should be used (medroxyprogesterone 10– 20 mg/day or norethisterone 10– 15 mg/day) for women who decline the LNG-IUS. Cyclical progestogens should not be used

The duration of treatment and follow-up of hyperplasia without atypia �- Treatment with oral progestogens or the LNG-IUS should be for a minimum of 6 months in order to induce histological regression , women should be encouraged to retain the LNG-IUS for 5 YEARS this reduces the risk of relapse � 1 -If adverse effects are tolerable � 2 -fertility is not desired � 3 -If it alleviates abnormal uterine bleeding symptoms.

FOLLOW UP ; � � � -Endometrial surveillance with outpatient endometrial biopsy should be arranged at a minimum of 6 -monthly intervals. -At least two consecutive 6 -monthly negative biopsies should be obtained. -Women should be advised to seek a further advice if abnormal vaginal bleeding recurs after completion of treatment because this may indicate disease relapse. In women at higher risk of relapse; -As body mass index (BMI) of 35 or greater Those treated with oral progestogens 6 -monthly and endometrial biopsies are recommended Once two consecutive negative endometrial biopsies have been obtained long-term follow-up should be considered with annual endometrial biopsies.

3 -Surgical management( Hysterectomy ) should not first-line treatment because progestogen induces remission in the majority avoids the morbidity Hysterectomy is indicated in women not wanting to preserve their fertility when 1 -Progression to atypical hyperplasia during follow-up, 2 - No histological regression after 12 months of treatment 3 - Relapse of endometrial hyperplasia after completing progestogen 4 - Persistence of bleeding symptoms 5 -The woman declines to undergo endometrial surveillance or comply with medical treatment

Types of surgery 1 - Postmenopausal women should be offered a bilateral salpingo-oophorectomy together with the total hysterectomy. 2 - premenopausal women, the decision to remove the ovaries should be individualised; reduce the risk of a future ovarian malignancy. 3 - A laparoscopic approach is preferable. 4 - Endometrial ablation is not recommended.

Management of atypical hyperplasia 1 - Total Hysterectomy because of - The risk of underlying malignancy 25%, Progression to cancer 25 -50% laparoscopic approach - Postmenopausal should be offered bilateral salpingo-oophorectomy - -premenopausal women, the decision to remove the ovaries individualised; but removal will reduce the risk of a future ovarian malignancy. Endometrial ablation is not recommended

� 2 --Women with atypical hyperplasia who wish to preserve their fertility or who are not suitable for surgery � Women wishing to retain their fertility should be counselled about the risks � Pretreatment investigations should aim to rule out invasive endometrial cancer or co-existing ovarian cancer by TVUS and endometrial biopsy � First-line treatment with the LNG-IUS should be recommended, with oral progestogens as a secondbest alternative � Once fertility is no longer required, hysterectomy should be offered because high risk of disease relapse

� followed up �TVUS and endometrial biopsy : at 3 months interval until minimum two consecutive negative biopsies are obtained So two negative and asymptomatic women long-term follow-up with endometrial biopsy every 6– 12 months is recommended until a hysterectomy is performed.

� In women wishing to conceive � Disease regression should be achieved on at least one endometrial sample before women attempt to conceive. � Assisted reproduction may be considered as the live birth rate is higher and it may prevent relapse.

�HRT and endometrial hyperplasia � 1 - Systemic estrogen-only HRT should not be used in women with a uterus. � 2 - All women taking HRT should be encouraged to report any unscheduled vaginal bleeding promptly. � 3 - advised to change to continuous progestogen intake using the LNG-IUS or a continuous combined HRT preparation.

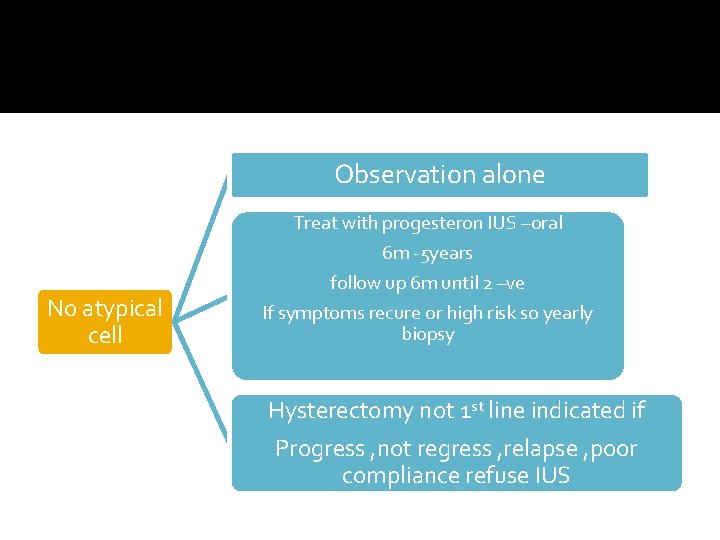
Observation alone Treat with progesteron IUS –oral No atypical cell 6 m -5 years follow up 6 m until 2 –ve If symptoms recure or high risk so yearly biopsy Hysterectomy not 1 st line indicated if Progress , not regress , relapse , poor compliance refuse IUS

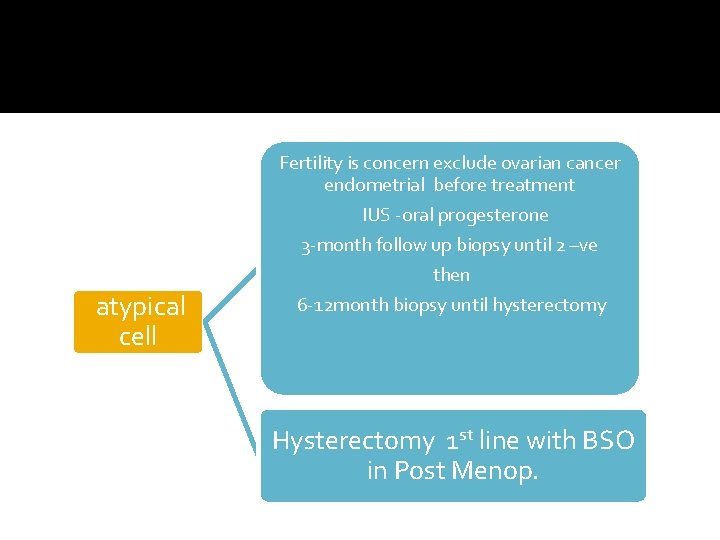
Fertility is concern exclude ovarian cancer endometrial before treatment IUS -oral progesterone 3 -month follow up biopsy until 2 –ve atypical cell then 6 -12 month biopsy until hysterectomy Hysterectomy 1 st line with BSO in Post Menop.

THANK YOU