Congenital Adrenal Hyperplasia Authors Dawn Lim MBBS MRCP

Congenital Adrenal Hyperplasia Author(s): Dawn Lim, MBBS, MRCP (UK), M. Med (S'pore) Level: Basic Academic Affiliation: Singapore General Hospital, Associate Consultant Version No: 1. 0 Submitted: March 2013 Editors’ Review:

2 Disclaimer/Liability • The information provided in the VAP is made available in good faith and is derived from sources believed to be reliable and accurate at the time of release. • The materials presented on the VAP may include links to external Internet sites. These external information sources are outside the control of Duke-NUS. The user of the Internet links is responsible for making his or her own decision about the accuracy, reliability and correctness of the information found. • In no event shall Duke-NUS be liable for any indirect, special, incidental, or consequential damages arising out of any use of reliance of any information contained in the VAP. Nor does Duke-NUS assume any responsibility for failure or delay in updating or removing the information contained in the VAP. • Moreover, information provided on the VAP does not constitute medical advice or treatment nor should it be considered as a replacement of the patient/physician relationship or a physician’s professional judgment. Duke-NUS expressly disclaims all liability for treatment, diagnosis, decisions and actions taken or not taken in reliance upon information contained in the VAP. This work is licensed under a Creative Commons Attribution-Non. Commercial-No. Derivs 3. 0 Unported License To view a copy of this license, visit [http: //creativecommons. org/licenses/by-nc-nd/3. 0/]

3 Financial Disclosures (past 3 years) • No Disclosures

4 Learning Objectives • To review normal adrenal steroid biosynthesis • To understand the pathophysiology of 21 -hydroxylase deficiency CAH • To appreciate the spectrum of clinical presentations of CAH in males and females • To know the investigations required for the diagnosis of 21 -OHD CAH • To understand the principles and goals of management

5 Outline • Introduction to Congenital Adrenal Hyperplasia • Normal adrenal steroid biosynthesis • Pathophysiology of 21 -OHD CAH • Classification & presentation • Diagnosis • Principles of management

6 What is Congenital Adrenal Hyperplasia (CAH)? • A group of genetic enzyme deficiencies that impair normal adrenal steroid synthesis • Autosomal recessive disorders with distinctive clinical phenotypes • Most common: 21 -hydroxylase deficiency (90%), encoded by the CYP 21 A 2 gene • Others: – 11β-hydroxylase deficiency – 3β-hydroxysteroid dehydrogenase deficiency

7 Normal Adrenal Steroid Biosynthesis 3β: 3β-hydroxysteroid dehydrogenase 21: 21 -hydroxylase 11β: 11β-hydroxylase Cholesterol Pregnenolone 17α 3β Progesterone 17 -hydroxypregnenolone 17, 20 3β 3β 17α 21 Deoxycorticosterone 11β Corticosterone 17 -hydroxyprogesterone 21 11 - Deoxycortisol 11β Cortisol DHEA 17, 20 Androstenedione 17βR Testosterone 5αR Dihydroxytestosterone 18 Aldosterone MINERALOCORTICOIDS GLUCOCORTICOIDS 17α: 17α-hydroxylase; 17, 20: 17, 20 lyase; 17βR: 17β reductase; 5αR: 5α-reductase SEX STEROIDS

8 Pathophysiology of 21 -OHD CAH 3β: 3β-hydroxysteroid dehydrogenase 21: 21 -hydroxylase 11β: 11β-hydroxylase Cholesterol Pregnenolone 17α 3β Progesterone 17, 20 17α Deoxycorticosterone 11β Corticosterone � 17 -hydroxyprogesterone 21 11 - Deoxycortisol 11β Cortisol DHEA 3β 3β 21 ↑ACTH 17 -hydroxypregnenolone 17, 20 Androstenedione � 17βR Testosterone 5αR Dihydroxytestosterone 18 ↓Aldosterone MINERALOCORTICOIDS GLUCOCORTICOIDS 17α: 17α-hydroxylase; 17, 20: 17, 20 lyase; 17βR: 17β reductase; 5αR: 5α-reductase SEX STEROIDS
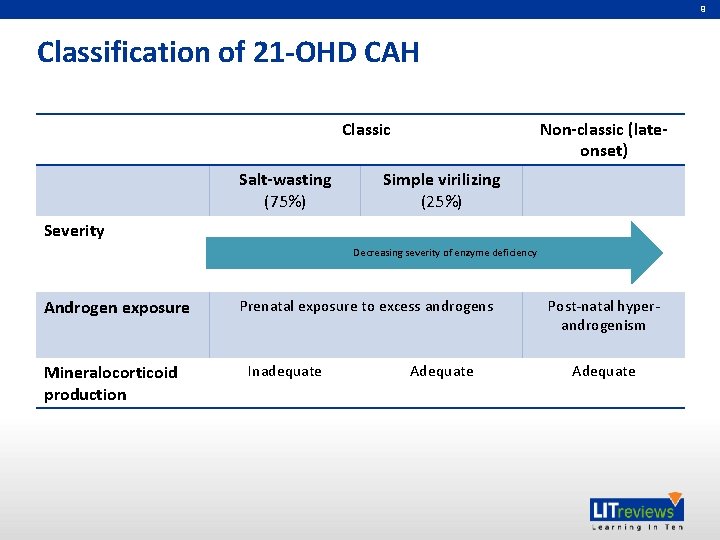
9 Classification of 21 -OHD CAH Classic Salt-wasting (75%) Non-classic (lateonset) Simple virilizing (25%) Severity Decreasing severity of enzyme deficiency Androgen exposure Mineralocorticoid production Prenatal exposure to excess androgens Inadequate Adequate Post-natal hyperandrogenism Adequate
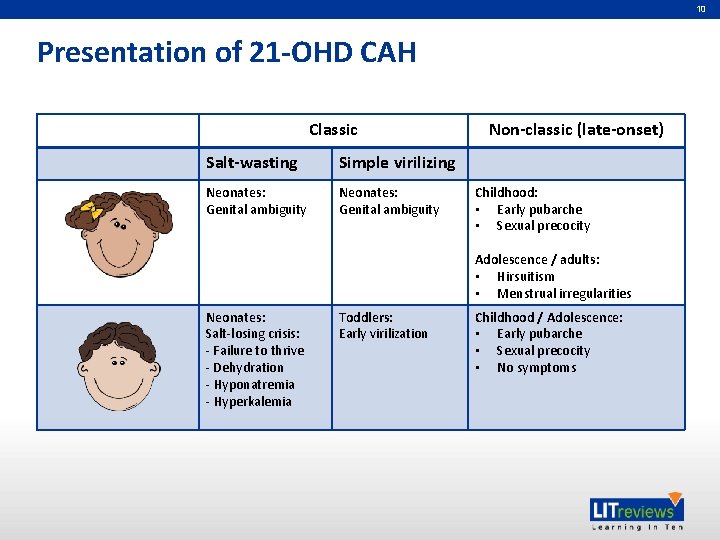
10 Presentation of 21 -OHD CAH Classic Salt-wasting Simple virilizing Neonates: Genital ambiguity Non-classic (late-onset) Childhood: • Early pubarche • Sexual precocity Adolescence / adults: • Hirsuitism • Menstrual irregularities Neonates: Salt-losing crisis: - Failure to thrive - Dehydration - Hyponatremia - Hyperkalemia Toddlers: Early virilization Childhood / Adolescence: • Early pubarche • Sexual precocity • No symptoms
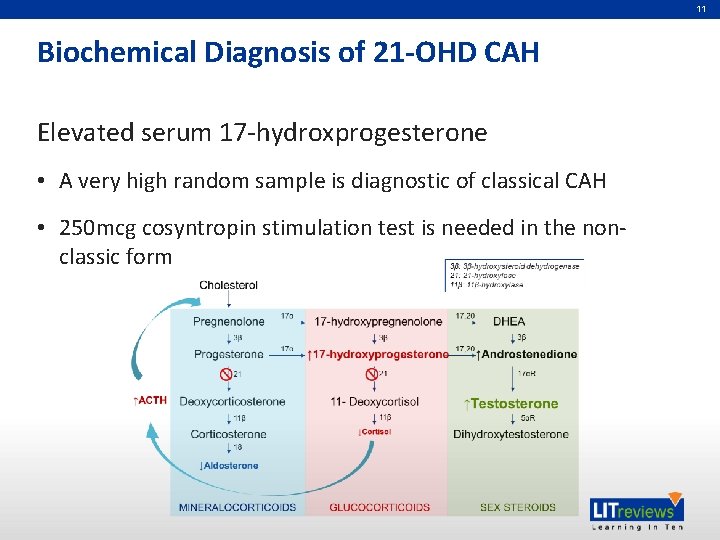
11 Biochemical Diagnosis of 21 -OHD CAH Elevated serum 17 -hydroxprogesterone • A very high random sample is diagnostic of classical CAH • 250 mcg cosyntropin stimulation test is needed in the nonclassic form

12 Other Investigations • Urea, electrolytes, creatinine – ↓ Sodium – ↑ Potassium – Acute renal failure Salt-wasting crises! • Low Cortisol • Elevated Androstenedione and DHEA-S

13 Management goals in Classic CAH 1. Correct cortisol deficiency with glucocorticoids 2. Suppress ACTH overproduction so as to reduce stimulation of the androgen pathway 3. Replacement of mineralocorticoids in salt-wasting CAH (oral fludrocortisone) 4. Surgical repair of ambiguous genitalia in females

14 Management goals in Non-classic CAH Treatment recommended only in symptomatic individuals • Children: Advanced bone maturation • Adolescents: Irregular menses, acne, hirsuitism • Adults: Patient-important hyperandrogenism or infertility

15 Glucocorticoid replacement Classic Salt-wasting Non-classic (lateonset) Simple virilizing Children Hydrocortisone 10 -15 mg/m 2/day divided into 3 doses • Dose titration according to androgen and 17 -OHP levels Adults Prednisolone or dexamethasone may be used Lower doses may be adequate Avoidance of over-treatment that can lead to Cushing’s syndrome

16 Summary • CAH: a group of AR disorders that result in enzyme deficiencies that impair normal adrenal steroid synthesis • 21 -OHD CAH is the most common form – the hallmark of which is an elevated 17 -hydroxyprogesterone • The severity of enzyme deficiency influences the clinical presentation • Diagnosis is crucial in order to prevent life-threatening saltwasting crises in classical CAH • Treatment is targeted to replace the insufficient adrenal hormones and to reduce adrenal androgen excess

17 Key References • Speiser PW, Azziz R, Baskin LS et al. Congenital Adrenal Hyperplasia due to Steroid 21 -Hydroxylase Deficiency: An Endorine Society Clinical Practice Guideline. J Clin Endocrinol Metab 95: 4133 -4160, 2010 • Nimkarn S, Lin-Su K, New MI. Steroid 21 Hydroxylase Deficiency Congenital Adrenal Hyperplasia. Endocrinol Metab Clin N Am 38: 669 -718, 200

Partners in Academic Medicine
- Slides: 18