Pediatric Respiratory Emergencies Amy Gutman MD prehospitalmdgmail com






















- Slides: 40

Pediatric Respiratory Emergencies Amy Gutman MD prehospitalmd@gmail. com www. Prepared. Rescuer. com

Overview • Review critical aspects of emergency care of pediatric respiratory emergencies – Epidemiology – Anatomy – Specific disease processes • Key concept: children have unique pathophysiology & respond differently to respiratory illnesses than adults • Importantly: – How to recognize “sick” – Management strategies for respiratory distress – Timely recognition of respiratory distress & appropriate intervention key to preventing progression to cardiac arrest

Sick or Not Sick?

Epidemiology • 26% US population, 10% EMS calls – Rate of ED visits in poorest communities higher than rate in wealthiest communities (414 visits: 1, 000 children vs 222: 1, 000 • Respiratory distress #1 cause of admissions & death during 1 st year except for congenital abnormalities • Most pediatric cardiac arrests begin as respiratory failure • Minimal training, few ill pediatric patients makes it difficult to obtain & maintain skills • Multiple sized patients, equipment sizes & drug dosages confusing in stressful situations 86%

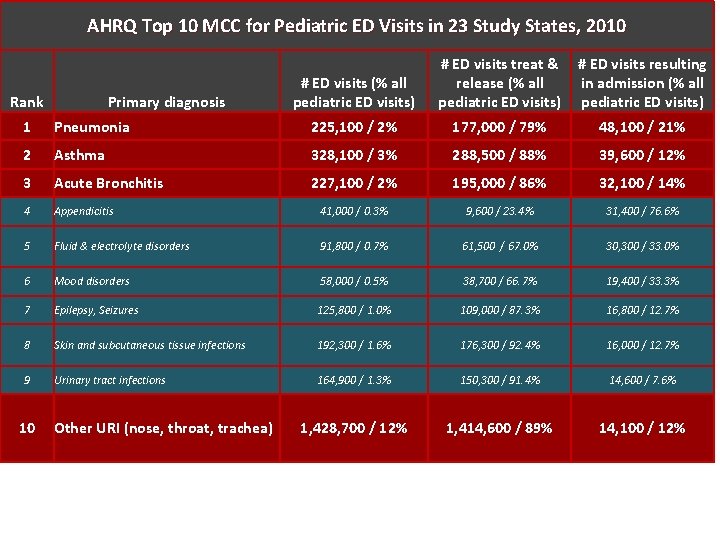
Top 10 MCC for Pediatric Visits in 23 Study States , 2010 AHRQ Statistical Brief #52. ED Healthcare Cost and # ED visits treat & # ED visits resulting Utilization Project (HCUP); May 2010 # ED visits (% all pediatric ED visits) release (% all pediatric ED visits) in admission (% all pediatric ED visits) 225, 100 / 2% 177, 000 / 79% 48, 100 / 21% 328, 100 / 3% 288, 500 / 88% • Asthma Majority of ED visits “treat-and-release” 39, 600 / 12% Rank 1 2 3 Primary diagnosis Pneumonia Acute Bronchitis 227, 100 / 2% 195, 000 / 86% 32, 100 / 14% 41, 000 / 0. 3% 9, 600 / 23. 4% 31, 400 / 76. 6% • Appendicitis However, 500, 000 pediatric ED visits result in admission, with the& electrolyte mostdisorders common cause being respiratory 5 Fluid 91, 800 / 0. 7% 61, 500 / 67. 0% 30, 300 / 33. 0% 4 6 disorders 58, 000 / 0. 5% 38, 700 / 66. 7% • Mood Four of the ten most common admitted conditions: 19, 400 / 33. 3% 8 125, 800 / 1. 0% 16, 800 / 12. 7% – Pneumonia, asthma, acute bronchitis, & URI 109, 000 / 87. 3% –and. Insubcutaneous 0 -4 yrs, tissue respiratory conditions 1/3 ED visits resulting in admission Skin infections 192, 300 /= 1. 6% 176, 300 / 92. 4% 16, 000 / 12. 7% 9 Urinary tract infections 7 10 Epilepsy, Seizures Other URI (nose, throat, trachea) 164, 900 / 1. 3% 150, 300 / 91. 4% 14, 600 / 7. 6% 1, 428, 700 / 12% 1, 414, 600 / 89% 14, 100 / 12%

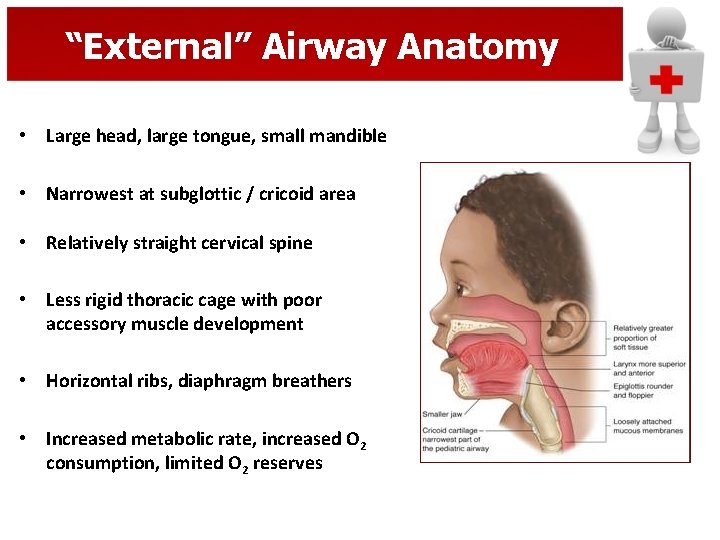
“External” Airway Anatomy • Large head, large tongue, small mandible • Narrowest at subglottic / cricoid area • Relatively straight cervical spine • Less rigid thoracic cage with poor accessory muscle development • Horizontal ribs, diaphragm breathers • Increased metabolic rate, increased O 2 consumption, limited O 2 reserves

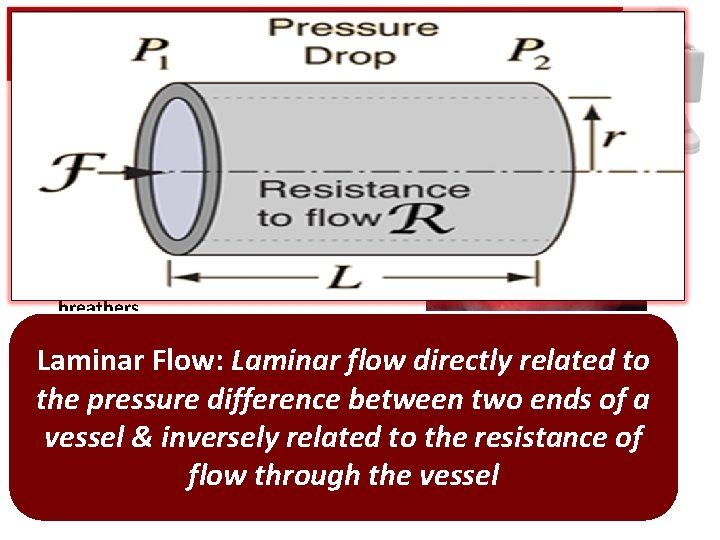
Smaller “Internal” Airway • Epiglottis floppy, U shaped & anterior • Larynx anterior • Short floppy trachea • Small soft airways in obligate nasal breathers – Nose = 50% airway resistance – Large tonsils, adenoids rapidly swell Laminar Flow: Laminar flow directly related to pressure difference between two ends of a • the Pliable / floppy trachea collapses easily (Poiseuille’s Law) vessel inversely to the resistance of – Adult: & 1 mm edema = 81%related size – Pedi: 1 mm edema size flow= 44% through the vessel

Patient Needs • Fear of separation, being hurt & the unknown • Allow family to be with patient as long as it does not distract you • Never lie! • Always explain your plan to child • Position at eye level, remain calm, speak slowly

ce ar pe Ap n tio • Pre-arrival preparation & scene size-up ula rc Ci an in Sk Assessment Work of Breathing • General assessment (Pediatric Assessment Triangle) – “Sick” vs “Not Sick” vs “Could Rapidly Become Sick” – Clinical indicators reflect CV, respiratory & neurological status • ABCDE & transport decision • Ongoing assessment including more thorough history & exam CUPS: CUPS Critical, Unstable, Potentially Unstable, Stable

HPI & Exam • HPI – – • How fast deteriorating? Fever? Noisy breathing? What has been done so far? PMH – Prematurity, hospitalizations, Illnesses, intubations, immunizations? – Allergies? – Medications? • Exam – – – Sick or Not Sick? Rate? Noisy? Position? Color? Symmetric?

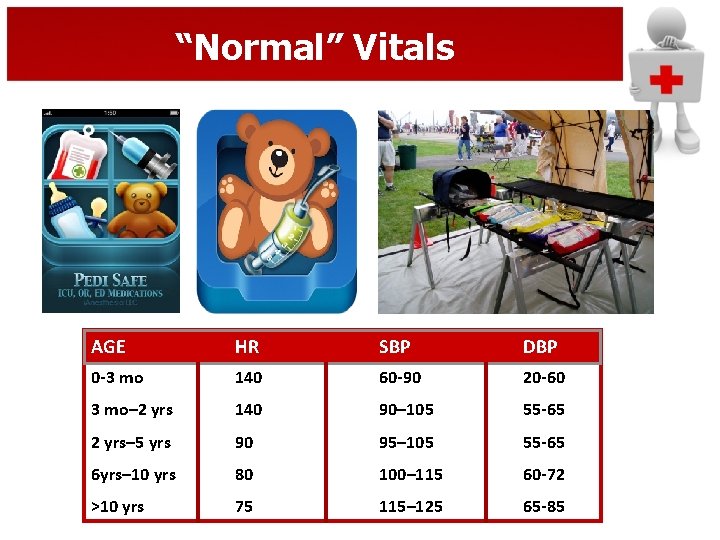
“Normal” Vitals AGE HR 0 -3 mo 140 60 -90 20 -60 3 mo– 2 yrs 140 90– 105 55 -65 2 yrs– 5 yrs 90 95– 105 55 -65 6 yrs– 10 yrs 80 100– 115 60 -72 >10 yrs 75 115– 125 65 -85 HR SBP SB DBP

Appearance • Alertness • Distractibility • Consolability • Eye contact • Speech/cry • Spontaneous motor activity • Color

Abnormal Breathing Sounds • Stridor – High pitched sound heard on inspiration – Indicates upper airway obstruction • Grunting – Short, low pitched sound heard in expiration – Auto-PEEP to keep small airways open as progresses towards respiratory failure • Wheezing – High-pitched whistling sound heard expiration > inspiration – Indicates lower airway obstruction • Crackles – Crackling sounds heard on inspiration – Associated with cardio-vascular disease, lung disease, infection

Respiratory Distress vs Failure • Distress – Maintain oxygenation only by increasing work of breathing • Failure – Cannot compensate for inadequate oxygenation despite extra respiratory effort & rate – Circulatory & respiratory system collapse Distress Tachypnea Nasal Flaring / Pursed Lips Stridor / Wheezing AMS / Agitation Tachycardia Delayed Capillary Refill Pale Failure RR > 60 Retractions Grunting Mottling Head Bobbing Severe Air Hunger Bradycardia Hypotension Arrest Bradypnea Inefficient respirations Cyanosis / Grey No air movement

Management Strategies • Treat symptoms, not the disease • Kids in respiratory distress needs oxygenation as uncorrected respiratory distress deteriorates to bradycardia & cardiac arrest • Priority is to support breathing effort – Remember the basics! • If pulse remains low or breathing inadequate, re-evaluate airway, ventilations, O 2 & tubing


Airway Management • Use PAT to determine oxygenation status & delivery device • Neutral “sniffing” head position – Towel under shoulders; do not flex head which collapses trachea – Head-tilt chin lift or jaw-thrust • <5 seconds to look, listen & feel • Suction airway • Appropriate ventilation volume & rate – 4 -6 mg/kg – Maintain optimal CO, venous return, cerebral blood flow & coronary perfusion – Limits regurgitation & aspiration

7 Ps…Not Just For RSI 1. Preparation 2. Pre-oxygenation 3. Premedication 4. Paralyze 5. Pass tube 6. Placement proof 7. Post-intubation care

Endotracheal Intubation Sanders Jr RC, Ron M. Walls RM, et al. Level of Trainee & Tracheal Intubation Outcomes. NEAR for Children Investigators. Pediatrics. 131: 3, March 2013 • 2005 AHA: • METHODS: – Cuffed ETT effective & safe for all ages 15 PICU Prospective multicenter observational cohort (7/2010 – 12/11) – • Un-cuffed ETT recommended in neonates • Outcome measures: FPS, overall success, & adverse associated events • • RESULTS: Rapidly deoxygenate & • 1265 primary ETI encounters by pediatric providers decompensate • – Prepare 1 st & overall attempt success Residents (37%, 51%) to start compressions • 1 st & overall attempt success Fellows (70%, 89%) – “Hail Mary” plan • 1 st & overall attempt success Attendings (72%, 94%) • OR 4. 29; 95% CI (3. 24– 5. 68) • Overall ETI FPS rate 68% • Attending vs Fellow vs Resident assoc with fewer adverse events (OR 0. 42; 95% CI, 0. 31– 0. 57) – EM physicians FPS rate 74%* – EMS overall success rate: 50%– 80% • CONCLUSIONS: • Resident tracheal intubation success low with high adverse events • Necessary intensive resident procedural training before “live” ETIs *Resuscitation. 2012 Nov; 83(11): 1363 -8.

ETT & Resuscitation • Smartphone apps: – Rapi. Tube, Difficult Airway, Pedi. Stat , Pedi. Safe • Traditional Calculations: – Un-cuffed = (Age / 4) + 4 – Cuffed = (Age / 4) + 3 – General = Age + 16/4 • [6 yo + 16]/4 = 22; 22/4 = 5. 5 ETT • Ready ETT 0. 5 mm smaller & larger • Use blade you like: – In very young Miller directly lifts floppy epiglottis – In older children Macintosh slides into vallecula & indirectly lifts epiglottis

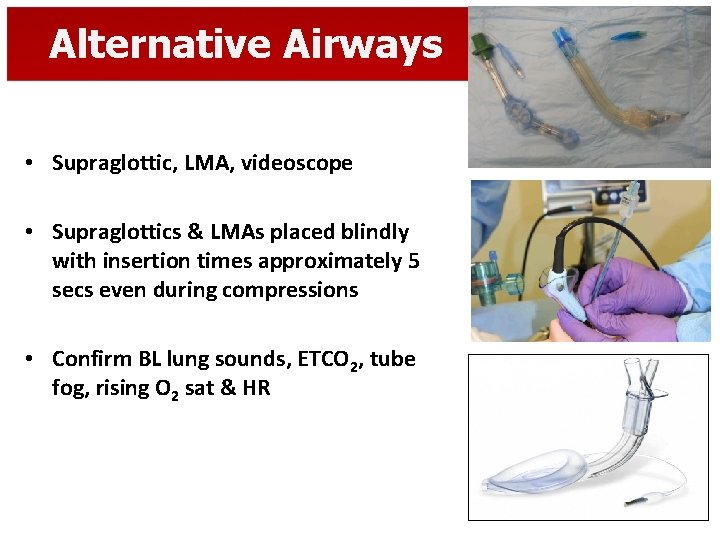
Alternative Airways • Supraglottic, LMA, videoscope • Supraglottics & LMAs placed blindly with insertion times approximately 5 secs even during compressions • Confirm BL lung sounds, ETCO 2, tube fog, rising O 2 sat & HR

Secure The Tube! Secure The Baby!

Upper vs Lower Airway Diseases • Upper Airway – – – Foreign Body Obstruction Retropharyngeal Abscess Bacterial Tracheitis Epiglottitis Croup • Lower Airway – RSV / Bronchiolitis – Asthma – Bronchitis / Pneumonia

Apparent Life Threatening Events (ALTE) • Lifeless, pulseless or unresponsive infant recovering spontaneously & “looks normal” – 1 -2% infants – Most common at 2 -3 mo, uncommon >2 yrs • All require transport & admission • DDX: Arrythmias Congenital heart disease Abuse / Trauma GERD Infectious / Metabolic / Neurological Respiratory compromise – Munchausen’s – – –

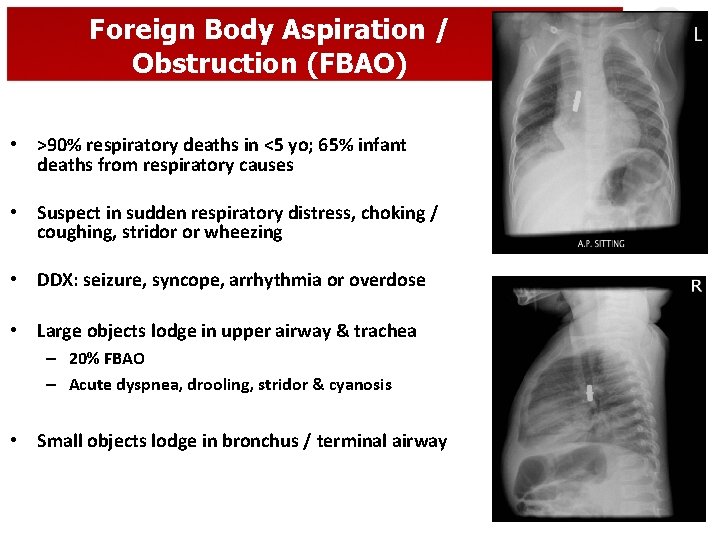
Foreign Body Aspiration / Obstruction (FBAO) • >90% respiratory deaths in <5 yo; 65% infant deaths from respiratory causes • Suspect in sudden respiratory distress, choking / coughing, stridor or wheezing • DDX: seizure, syncope, arrhythmia or overdose • Large objects lodge in upper airway & trachea – 20% FBAO – Acute dyspnea, drooling, stridor & cyanosis • Small objects lodge in bronchus / terminal airway

Choking / FBAO • Able to talk / minimal distress, rapid transport in position of comfort • Responsive but significant distress: – Child: abdominal thrusts or Heimlich – Infant: chest thrusts, back blows • Unresponsive, open airway & only remove object if visible / accessible – Begin CPR with airway check – Look for FB prior to starting each ventilation; if visible attempt removal with Magill’s – Airway management via PPV or advanced airway attempt • Rapid transport & notify receiving hospital • Medical Control for needle cricothyroidotomy if unable to clear obstruction, unable to intubate or ventilate Even If obstruction clears prior to your arrival, still transport

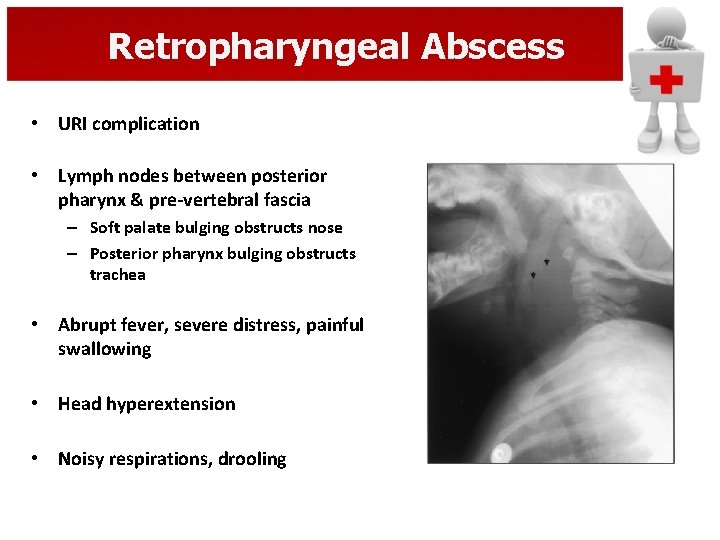
Retropharyngeal Abscess • URI complication • Lymph nodes between posterior pharynx & pre-vertebral fascia – Soft palate bulging obstructs nose – Posterior pharynx bulging obstructs trachea • Abrupt fever, severe distress, painful swallowing • Head hyperextension • Noisy respirations, drooling

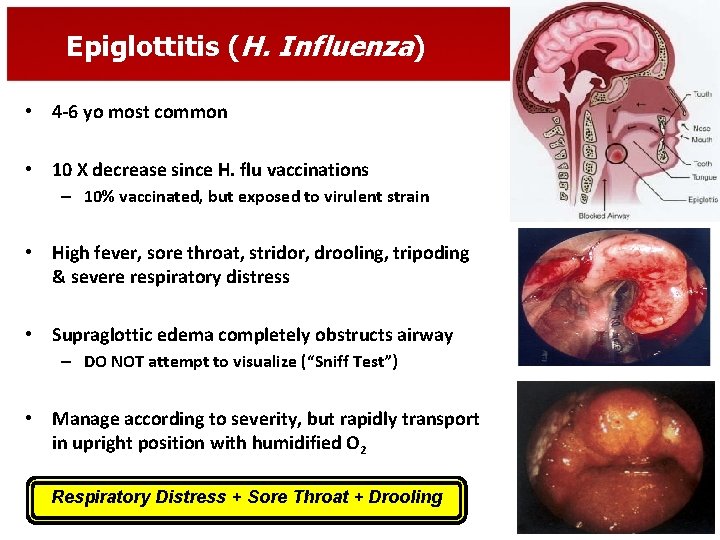
Epiglottitis (H. Influenza) • 4 -6 yo most common • 10 X decrease since H. flu vaccinations – 10% vaccinated, but exposed to virulent strain • High fever, sore throat, stridor, drooling, tripoding & severe respiratory distress • Supraglottic edema completely obstructs airway – DO NOT attempt to visualize (“Sniff Test”) • Manage according to severity, but rapidly transport in upright position with humidified O 2 Respiratory Distress + Sore Throat + Drooling

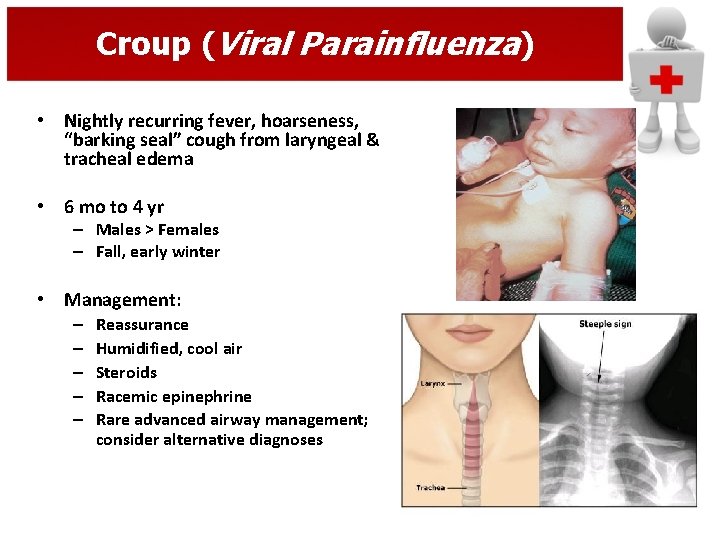
Croup (Viral Parainfluenza) • Nightly recurring fever, hoarseness, “barking seal” cough from laryngeal & tracheal edema • 6 mo to 4 yr – Males > Females – Fall, early winter • Management: – – – Reassurance Humidified, cool air Steroids Racemic epinephrine Rare advanced airway management; consider alternative diagnoses

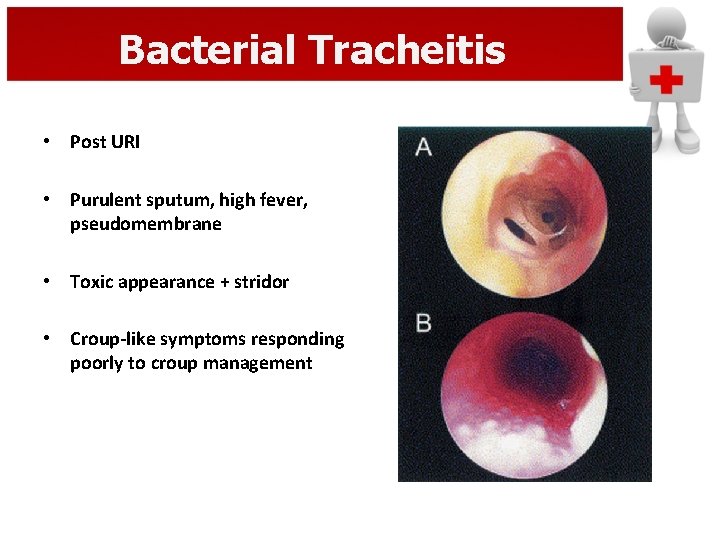
Bacterial Tracheitis • Post URI • Purulent sputum, high fever, pseudomembrane • Toxic appearance + stridor • Croup-like symptoms responding poorly to croup management

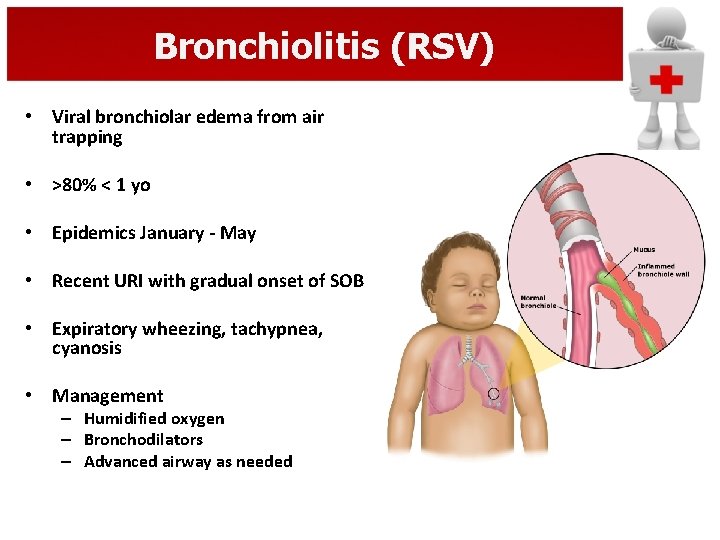
Bronchiolitis (RSV) • Viral bronchiolar edema from air trapping • >80% < 1 yo • Epidemics January - May • Recent URI with gradual onset of SOB • Expiratory wheezing, tachypnea, cyanosis • Management – Humidified oxygen – Bronchodilators – Advanced airway as needed

Asthma • Lower airway hypersensitivity causing bronchospasm, edema & mucus production – Varying degrees of respiratory distress – All that wheezes is not asthma – Non-wheezers often in severe respiratory distress • Important History – – Prior ICU admission / intubations >3 ED visits or >2 admissions in past yr >1 MDI used in past mo or every 4 hrs Symptom progression despite aggressive treatment • Management is aggressive airway, pharmacology & fluid resuscitation – – Position of comfort, humidified O 2 Beta-2 agents (Albuterol) Anticholinergics (Atropine, Ipatropium) Subcutaneous beta agents (Epinephrine 1: 1000, 0. 1 to 0. 3 mg SQ)

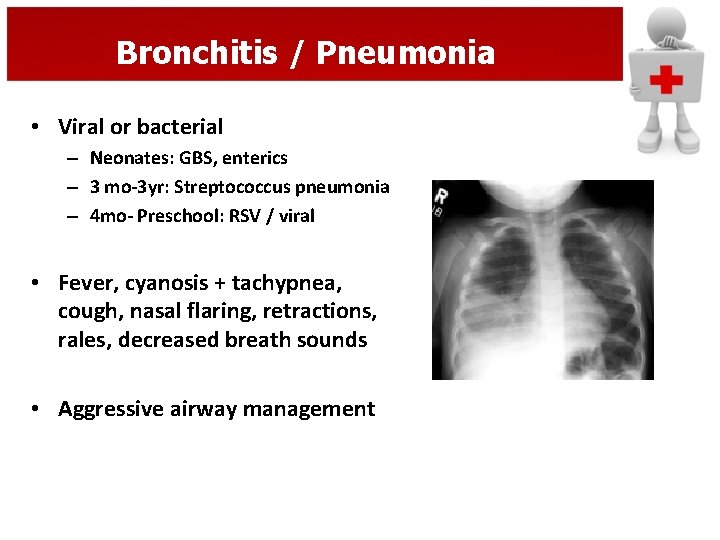
Bronchitis / Pneumonia • Viral or bacterial – Neonates: GBS, enterics – 3 mo-3 yr: Streptococcus pneumonia – 4 mo- Preschool: RSV / viral • Fever, cyanosis + tachypnea, cough, nasal flaring, retractions, rales, decreased breath sounds • Aggressive airway management

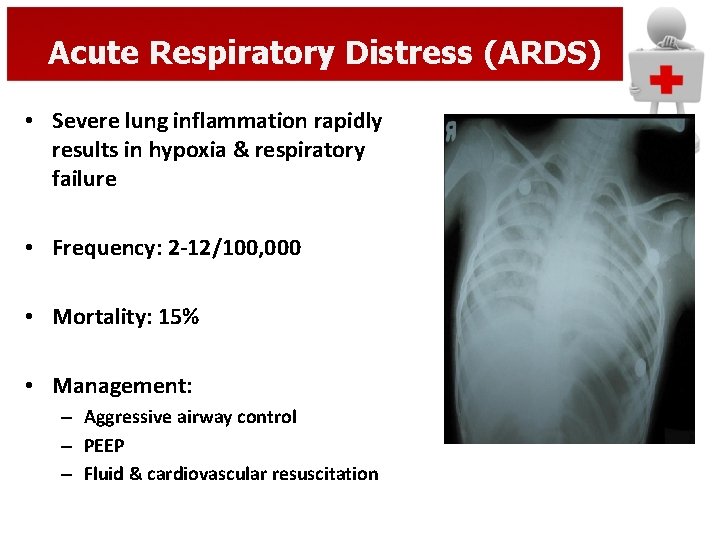
Acute Respiratory Distress (ARDS) • Severe lung inflammation rapidly results in hypoxia & respiratory failure • Frequency: 2 -12/100, 000 • Mortality: 15% • Management: – Aggressive airway control – PEEP – Fluid & cardiovascular resuscitation

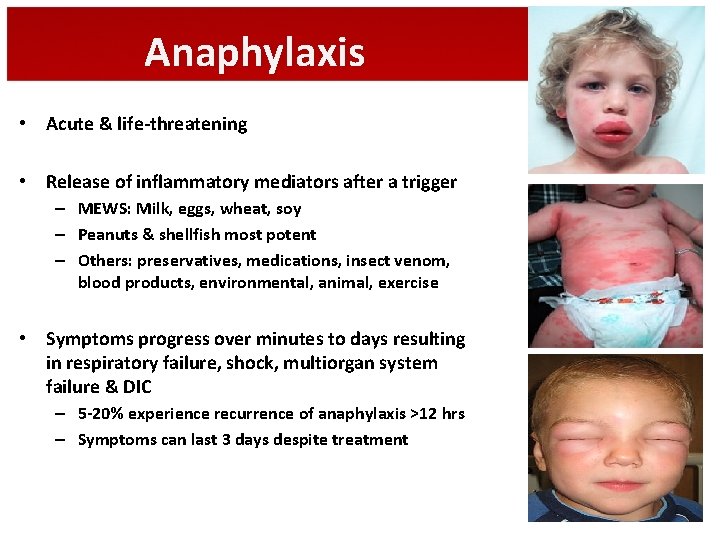
Anaphylaxis • Acute & life-threatening • Release of inflammatory mediators after a trigger – MEWS: Milk, eggs, wheat, soy – Peanuts & shellfish most potent – Others: preservatives, medications, insect venom, blood products, environmental, animal, exercise • Symptoms progress over minutes to days resulting in respiratory failure, shock, multiorgan system failure & DIC – 5 -20% experience recurrence of anaphylaxis >12 hrs – Symptoms can last 3 days despite treatment

Anaphylaxis Management • Early aggressive airway management • Medications: – – Diphenhydramine Histamine blocker (pepcid, zantac) Nebulized or MDI albuterol (2. 5 -5 mg/dose) Epinephrine 1: 1000 IM • Anaphylactic Shock: – – Beware of “compensated shock” Trendelenburg position 20 m. L/kg crystalloid bolus; repeat to 60 -80 m. L/kg prn Vasopressors: • Epinephrine (0. 1 -1 mcg/kg/min IV) • Dopamine (2 -20 mcg/kg/min IV) • Norepinephrine (0. 1 -2 mcg/kg/min IV)

Pediatric Bronchospasm / Respiratory Distress • EMS: – ALS or rapid transport without ALS if potential delay – Encourage or assist patient to self-administer MDI – MDI contraindicated if max dose administered, pt cannot physically use device, device not prescribed for patient • ALS: – IV, O 2, Monitor – Albuterol / atrovent nebulizer or MDI – Medical Control: • Epinephrine 0. 15 -0. 3 mg IM autoinjector • Magnesium Sulfate 25 mg/kg IV over 5 min – Treat for shock as needed • Notify receiving hospital

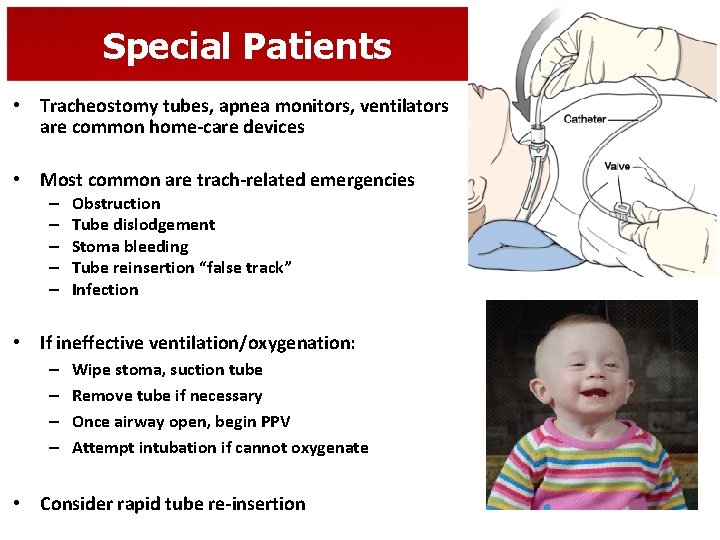
Special Patients • Tracheostomy tubes, apnea monitors, ventilators are common home-care devices • Most common are trach-related emergencies – – – Obstruction Tube dislodgement Stoma bleeding Tube reinsertion “false track” Infection • If ineffective ventilation/oxygenation: – – Wipe stoma, suction tube Remove tube if necessary Once airway open, begin PPV Attempt intubation if cannot oxygenate • Consider rapid tube re-insertion

References • • • • Emergency Care & Transportation of the Sick and Injured, 9 th ED Massachusetts OEMS (www. dph. org) Alameda County EMS www. emsonline. com Premier Health Care Services Continuing Education and Training Pediatric Advanced Life Support (PALS) Pediatric Education for the Prehospital Provider (PEPP) Pediatric Emergency Assessment, Recognition & Stabilization (PEARS) healthtraining@inh. com NAEMT Emergency pediatric Care www. emsc. org E Humphreys PA-C, EMT-I “Pediatric Respiratory Emergencies” (2009) J Reynolds MD “Pediatric Respiratory Emergencies” (2012) S Villanueva MD, FACEP “Pediatric Respiratory Emergencies”. 2011. “Management of acute lung injury & ARDS in children”. Critical Care. 2009.

Summary • Pre-arrival preparation important • Standardized approach to assessment & management • Knowledge of normal child development and age-specific physiology important • “Sick/not sick” determination is paramount in treatment & transport decisions Find me: Kingston ED Email me: prehospitalmd@gmail. com / Website: www. Prepared. Rescuer. com Text me: 513 -255 -1353