Bladder and Bowel Dysfunction UTIs in Children Presented

Bladder and Bowel Dysfunction & UTIs in Children Presented by Valari Cathey, APRN, MS, CPNP Department of Pediatric Urology OU Children’s Physicians

�Dominic Frimberger, MD, Dorsa Ahlefeld, APRN �New peds urologist coming in July 2018: �Adam Rensing, MD �Balagee Sundaram, MD Pediatric Urology Team

�Describe common terms associated with bladder and bowel dysfunction along with age associated norms from the ICCS (International Children’s Continence Society) �Explore potential etiologies of abnormal toileting habits �Discuss management and treatment options including medications to address common types of bladder bowel dysfunction Objectives


� Terminology is changing and the term dysfunctional elimination syndrome (DES) is now discourage by the ICCS (International Children’s Continence Society) • Journal of Urology, 191 (6): 1863 -1865, June, 2014 • http: //www. jurology. com/article/S 0022 -5347(14)002456/fulltext Terminology

�Bladder Bowel Dysfunction (BBD) now recommended ◦ More descriptive term ◦ Encompasses the parallel dysfunction ◦ Broader term which can be subcategorized into lower urinary tract (LUT) dysfunction and bowel dysfunction Terminology Austin PF, Bauer SB, Bower W, et al. The Standardization of Terminology of Lower Urinary Tract Function in Children and Adolescents: Update Report from The Standardization Committee of the International Children’s Continence Society. (2014). The Journal of Urology, 191 (6): 1863 -1865/doi. org/10. 1002/nau. 22751. [Pub. Med]

�Abnormal potty habits develop in a variety of age groups and can last for days, weeks, months or years �LUT symptoms are characterized after 5 years of age for incontinence disorders and after a minimum of 4 years of age for bowel disorders ◦ However, the terminology may be applicable to those <5 years of age if the child has achieved voluntary control ◦ Ages used by the DSM-5 and ICD-10 Bladder Bowel Dysfunction Austin PF, Bauer SB, Bower W, et al. The Standardization of Terminology of Lower Urinary Tract Function in Children and Adolescents: Update Report from The Standardization Committee of the International Children’s Continence Society. (2014). The Journal of Urology, 191 (6): 1863 -1865

� Common problem pediatric ◦ 20 -25% referrals to pediatric urologists � Wide spectrum of conditions ◦ ◦ ◦ Visual Learners!! Daytime incontinence Enuresis Underactive bladder Overactive bladder Dysfunctional voiding Voiding postponement

Continuous incontinence leaks day and night Intermittent incontinence leakage of urine in discrete quantities � Congenital � Daytime incontinence ◦ occurs while awake malformations ◦ ectopic ureter ◦ exstrophy variant � Functional loss of external urethral sphincter function ◦ external sphincterotomy � Enuresis ◦ occurs only during sleep ◦ should not be used to refer to daytime incontinence � Iatrogenic causes ◦ vesicovaginal fistula Incontinence- continuous or intermittent Austin PF, Bauer SB, Bower W, et al. The Standardization of Terminology of Lower Urinary Tract Function in Children and Adolescents: Update Report from The Standardization Committee of the International Children’s Continence Society. (2014). The Journal of Urology, 191 (6): 1863 -1865 https: //doi. org/10. 1002/nau. 22751. [Pub. Med]

Monosymptomatic Non-monosymptomatic � Enuresis � Children without other lower urinary tract symptoms ◦ Primary ◦ Secondary Enuresis with other lower urinary tract symptoms ◦ Primary ◦ Secondary Austin PF, Bauer SB, Bower W, et al. The Standardization of Terminology of Lower Urinary Tract Function in Children and Adolescents: Update Report from The Standardization Committee of the International Children’s Continence Society. (2014). The Journal of Urology, 191 (6): 1863 -1865 https: //doi. org/10. 1002/nau. 22751. [Pub. Med]
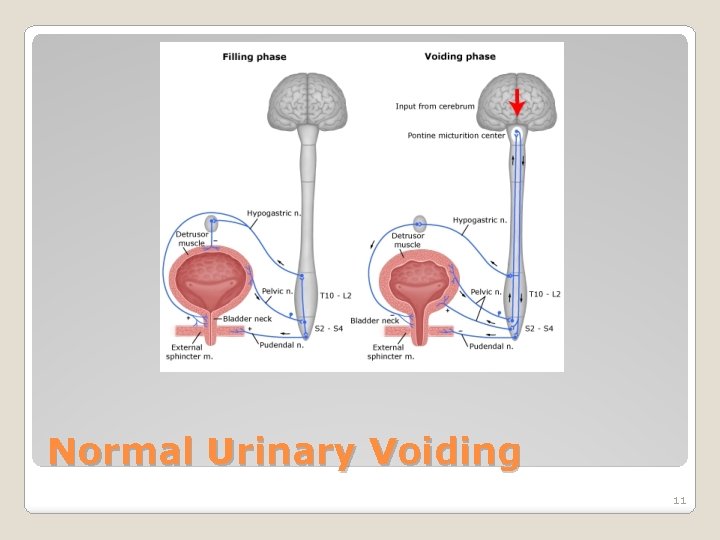
Normal Urinary Voiding 11
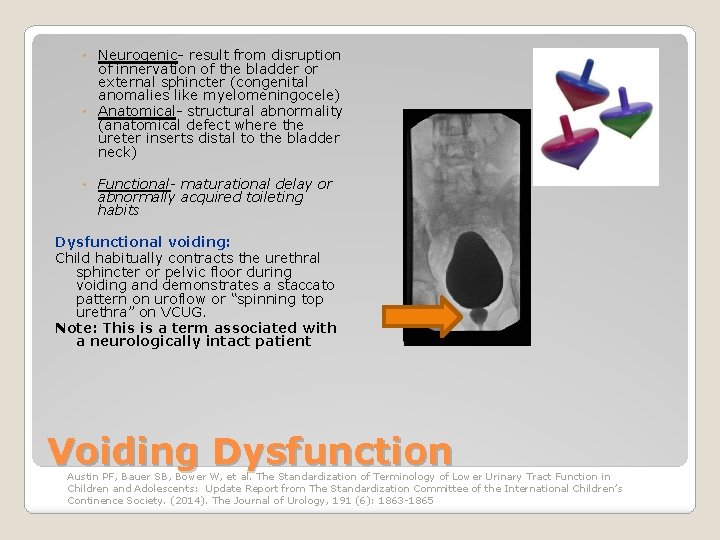
◦ Neurogenic- result from disruption of innervation of the bladder or external sphincter (congenital anomalies like myelomeningocele) ◦ Anatomical- structural abnormality (anatomical defect where the ureter inserts distal to the bladder neck) ◦ Functional- maturational delay or abnormally acquired toileting habits Dysfunctional voiding: Child habitually contracts the urethral sphincter or pelvic floor during voiding and demonstrates a staccato pattern on uroflow or “spinning top urethra” on VCUG. Note: This is a term associated with a neurologically intact patient Voiding Dysfunction Austin PF, Bauer SB, Bower W, et al. The Standardization of Terminology of Lower Urinary Tract Function in Children and Adolescents: Update Report from The Standardization Committee of the International Children’s Continence Society. (2014). The Journal of Urology, 191 (6): 1863 -1865

�Disposable diapers �Family dynamics �Children’s hectic schedules �Modern day games and activities �Bathroom access and fears �Constipating diet �Bladder irritants like sodas, juices Factors Contributing to Abnormal Potty Habits

� Lower urinary tract symptoms R 39. 9 ◦ Involuntary urine leakage immediately after completion of voiding (Post-void dribbling. N 39. 43) ◦ Daytime accidents or uncontrolled urine leakage (Urge incontinence-N 39. 41) ◦ Bedwetting (Primary or secondary nocturnal enuresis-N 39. 44) Abnormal Toileting Habits
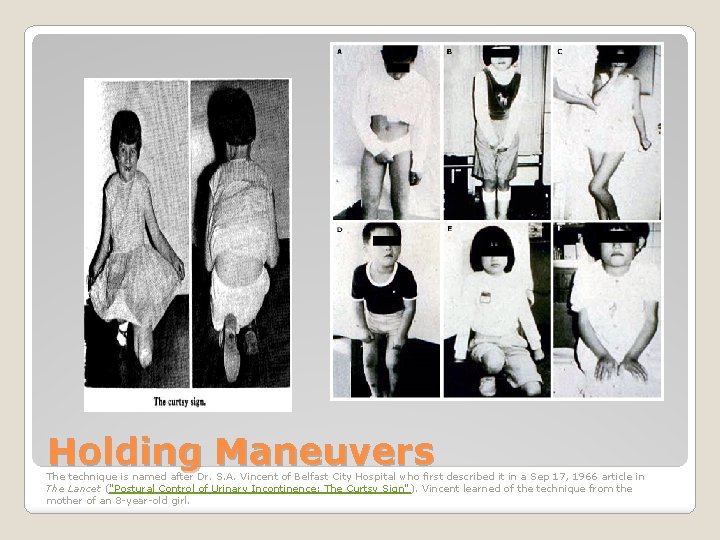
Holding Maneuvers The technique is named after Dr. S. A. Vincent of Belfast City Hospital who first described it in a Sep 17, 1966 article in The Lancet ("Postural Control of Urinary Incontinence: The Curtsy Sign" ). Vincent learned of the technique from the mother of an 8 -year-old girl.

�A thickened bladder wall points to a longstanding history LUTS, UTI and at times bladder pathology from outlet obstruction in boys �Normal values do not exist and bladder wall thickness varies depending on degree of bladder fullness Bladder wall thickness Austin PF, Bauer SB, Bower W, et al. The Standardization of Terminology of Lower Urinary Tract Function in Children and Adolescents: Update Report from The Standardization Committee of the International Children’s Continence Society. (2014). The Journal of Urology, 191 (6): 1863 -1865

� Burning with urination ◦ (Dysuria-R 30. 0) � Causes �UTIs �Local skin irritation �Concentrated urine �Holding behaviors � Treatment �Time void �Encourage more water �Girls change to wide legged voiding posture and slow down �Encourage uncircumcised boys to retract foreskin with urination �Screen for labial adhesions Dysuria

Wrong Way but love enthusiasm

� 3 -30% of girls, most asymptomatic �Etiology uncertain, one theory is low estrogen levels in these prepubertal girls �Theory supported since always resolves with puberty as natural estrogen levels increase Labial Adhesions

�Only treat if symptomatic ◦ Dysuria ◦ Post-void dribbling ◦ UTIs �Treatments ◦ Medical management (up to 70% recurrence) �Estrogen cream (Premarin) applied to labia 2 x/day for 4 -6 weeks �Steroid cream is also an option (Diprolene) ◦ Surgical therapy (up to 50% recurrence) �Rarely perform at our institution Labial Adhesions

�Most children 3 -12 years of age void 37 times daily �Daytime urinary frequency is children who void >8 times per day while awake ◦ increased frequency of urination-R 35. 0 �Causes ◦ Exclude UTI and DM concerns first ◦ Constipation ◦ Certain fluids promote diuresis ◦ Failure to empty-rare �Treatments ◦ Avoid known bladder irritants ◦ Manage constipation Urinary Frequency The Standardization of Terminology of Lower Urinary Tract Function in Children and Adolescents: Update Report from The Standardization Committee of the International Children’s Continence Society. ( 2014). The Journal of Urology: 1863 -1865.

�Caffeinated beverages ◦ Teas, coffees, chocolate drinks, and sodas �Carbonated ◦ Sodas drinks �Citrus drinks ◦ Orange juice and lemonade �Carbohydrate containing beverages ◦ Kool-Aid, Powerade, Gatorade, Vitaminwater Avoiding Known Bladder Irritants
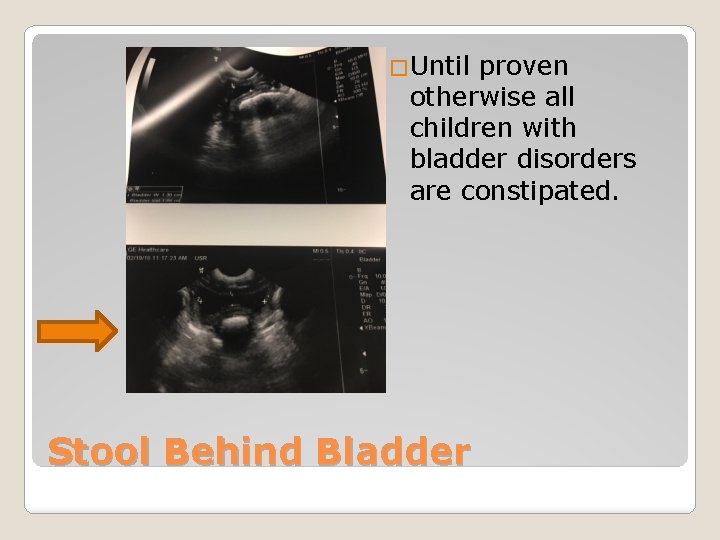
�Until proven otherwise all children with bladder disorders are constipated. Stool Behind Bladder
�Large retrospective studies have shown that in 234 children with chronic constipation ◦ 29% had daytime urinary incontinence ◦ 34% had nighttime urinary incontinence ◦ 11% UTIs �In a 1997 article, Loening-Baucke reported that the relief of chronic constipation resulted in disappearance of daytime urinary incontinence by 89% and nocturnal enuresis by 63% and disappearance of recurrent UTIs in all with no anatomical problems Constipation Loening-Baucke V. Urinary incontinence and urinary tract infection and their resolution with treatment of chronic constipation of childhood. Pediatrics. 1997; 100: 228– 32. https: //doi. org/10. 1542/peds. 100. 2. 228. [Pub. Med]

Bristol Stool Scale

�Step #1 - � Start from below first with enemas or suppositories if family willing. ◦ Glycerin or Ducolax suppositories start working in 15 -60 minutes. ◦ Enemas work best! They start working in 1 -5 minutes. ◦ Give a suppository or enema 3 days in a row. �Then give one enema or suppository weekly until accidents resolve �and regularity established. Treatment of Constipation

� Step #2 - � Give 1 -2 days in a row on the weekend. � Repeat a laxative every weekend until symptoms resolve and bowel movements are more regular (daily, soft, long and skinny poops). ◦ Chocolate ex-lax �½ to 2 squares ◦ Pedia-Lax tablets �Start working in 30 minutes �Duration of action 6 hours ◦ 1 -3 tablets 2 -5 years of age ◦ 3 -6 tablets 5 years and older Treatment of Constipation

� Step daily #3 - Start Miralax following the bowel clean and continue � Start the child on Miralax (Polyethylene glycol) the day after the bowel clean out is done. ◦ 5 years of age and younger ¼ of the adult dose daily. ◦ All older children on ½ of adult dose daily. ◦ Give the medication with 1/2 - to 1 cup of fluid at any meal. ◦ Recommend parents adjust the dose as needed, every 3 -4 days up to 2 capfuls daily if needed. ◦ Take the medication as long as needed. ◦ It is an osmotic laxative, only traps water in the stool. ◦ It does not cause dependence or stimulate a bowel movement. ◦ It works to soften the stool. Treatment of Constipation

�Step #4 - Start immediately �Make sure child is drinking lots of water or water based fluids to help keep the stool soft. ◦ The urine is the best indicator of hydration. The lighter in color it is the better. �Then slowly increase dietary fiber (fruits, vegetables, whole grains) about 25 grams per day. �Decrease constipating foods (meats, dairy and white processed foods). Treatment of Constipation

Child’s dose is typically 1 capful for every year of age mixed in 4 -8 ounces of fluid over 4 -6 hours. �Example: 8 year old=8 capfuls, take 1 capful every 30 minutes for 4 hours to total 8 capfuls of Miralax/PEG. Miralax clean out

Proper Posture

◦ Typically referred pain from constipation or erections Penile Pain

�Stenotic meatal opening resulting from how it healed after circumcision �A problem usually detected once toilet training begins �Upward deflection of urine stream with each urination �We watch them urinate to verify diagnosis �Treat with a clinic meatotomy by one of the surgeons under local anesthetic ◦ Can go to OR if necessary Meatal Stenosis

�As the bladder contracts against a closed sphincter the bladder thickens and becomes more forceful and quick to empty. �A thickened bladder wall points to a longstanding history LUTS �Normal values to not exist and thickness varies depending on degree of bladder fullness ◦ Thick if greater than 3 mm when bladder full ◦ Thick if greater than 6 mm when bladder full Causes of Urinary Urgency The Standardization of Terminology of Lower Urinary Tract Function in Children and Adolescents: Update Report from The Standardization Committee of the International Children’s Continence Society. (2016). Neurourology and Urodynamcis 35: 471 -481.

� International Children’s Continence Society, overactive bladder (OAB) is “urinary urgency, usually accompanied by frequency and nocturia, with or without urinary incontinence, in the absence of urinary tract infection or other obvious pathology ◦ the most common voiding dysfunction in children � According to two fairly recent, large-scale studies, ◦ Prevalence of OAB in children is in the 15– 20% range �a higher prevalence of OAB in boys the ◦ Chung et al noted a decreasing prevalence of OAB with age � 23. 0% at 5 years old � 12. 2% at 13 years old Overactive Bladder Chung JM, Lee SD, Kang DI, et al. Prevalence and associated factors of overactive bladder in Korean children 5– 13 years old: A nationwide multicenter study. Urology. 2009; 73: 63– 7. https: //doi. org/10. 1016/j. urology. 2008. 063. [Pub. Med]

�>1 episode per month with 3 episodes over three months �Typically decreases ◦ 5 -6 year olds -10% ◦ 6 -12 year olds -5% ◦ 12 -18 year olds -4% with age Daytime Urinary Incontinence

�Female gender �History of nocturnal enuresis �Urinary tract infections �Encopresis Risk factors for urge incontinence
History Physical examination Studies Urinalysis Uroflow PVR +/- KUB Initial Evaluation

Uroflow
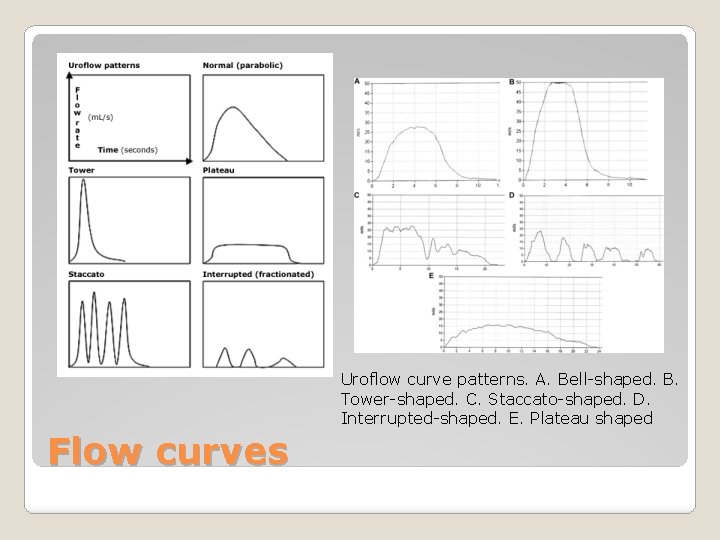
Uroflow curve patterns. A. Bell-shaped. B. Tower-shaped. C. Staccato-shaped. D. Interrupted-shaped. E. Plateau shaped Flow curves
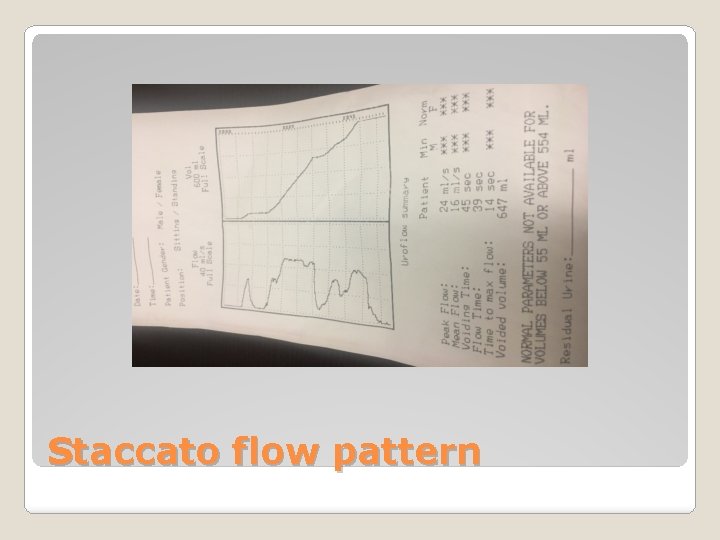
Staccato flow pattern

� Age of toilet training and/or any dry days or nights � Number of voids during the day � Frequency of incontinent episodes � Type of incontinence ◦ Before or after urinatingafter vaginal reflux ◦ Dribbles or saturates ◦ Day only or day and night ◦ Symptoms like urgency or dysuria � Voided volumes � Maximum voided volume can be compared with expected bladder capacity, as deduced from the standard formula [30 + (30 x age)]ml History I. Franco, A. von Gontard, M. De Gennaro, et al. Evaluation and treatment of nonmonosymptomatic nocturnal enuresis: a standardization document from the International Children's Continence Society

� Bowel habits ◦ Get specific, ask kid and parents �How often? Large? Pebbles? Painful? Hard? or Soft? �Use Bristol stool scale � Dietary intake ◦ Nibbler/grazer or meal eater ◦ Fluid choices � History of urinary tract infections ◦ Fever or afebrile ◦ Bag, cup or catheterized collections � Developmental delays ◦ Children who are developmentally delayed may also be delayed in gaining bladder control History

�Comorbidity �Family history ◦ Must ask specifically about nocturnal enuresis ◦ Who and for how long? �Social history ◦ Caregivers ◦ Daycare and/or school setting �Does teacher allow to use restroom �Send a school note to allow for voiding at least every 2 hours History

� In a large study of 8213 children aged 7½ to 9 years, children with daytime wetting had significantly increased rates of psychological problems: ◦ ◦ � ADHD 25% Separation anxiety 11% Oppositional behavior 11% Conduct problems 12% 10, 000 children aged 4 -9 years were analyzed ◦ Delayed development, difficult temperament and maternal depression/anxiety were associated with daytime wetting and soiling ◦ Joinson C, Heron J, Butler U, von Gontard A. Psychological differences between children with and without soiling problems. Pediatrics 2006; 117: 1575 e 84. ◦ Joinson C, Heron J, von Gontard A, Butler U, Golding J, Emond A. Early childhood risk factors associated with daytime wetting and soiling in school-age children. J Pediatr Psychol 2008; 33: 739 e 50. Comorbidity

�Focus on neurological and urological abnormalities ◦ Lower back �Signs of tethered cord- sacral dimpling, tuft of hair or assymetrical gluteal folds ◦ Neurological examination �Abnormal gait ◦ External urological examination �Labial adhesions can lead to post-void dribbling and dysuria ◦ Observation of urination �Helps evaluate voiding posture and if they strain (valsalva) Physical Examination

� � Urinalysis Uroflow Post-void bladder ultrasound +/- KUB � Renal ultrasound ◦ ◦ � Voiding cystourethrogram (VCUG) ◦ � never achieved a dry day after complying with program Cystoscopy ◦ � order if urodynamics abnormal Video urodynamics ◦ � Febrile UTIs MRI of the spine ◦ � hematuria Recurrent UTIs greater than 15 years of age with hematuria Urethral dilation is not recommended Medical Tests Available

� Children 4 - 6 years old: ◦ Single PVR >30 ml or >21% of bladder capacity (BC) ◦ Repetitive PVR >20 ml or >10% BC � Children 7 - 12 years old: ◦ Single PVR >20 ml or 15% BC ◦ Repetitive PVR >10 ml or 6% BC �Standard conditions: ◦ Not be under-distended (<50%) ◦ Not over-distended (>115%) in relation to the EBC; ◦ PVR obtained immediately after voiding (<5 minutes). PVR

� Routine urodynamic testing in the evaluation of urinary incontinence is not recommended for the following reasons. ◦ Invasive ◦ Expensive ◦ Requires specialized equipment and training ◦ Typically not necessary to make the diagnosis or affect outcome Urodynamic testing
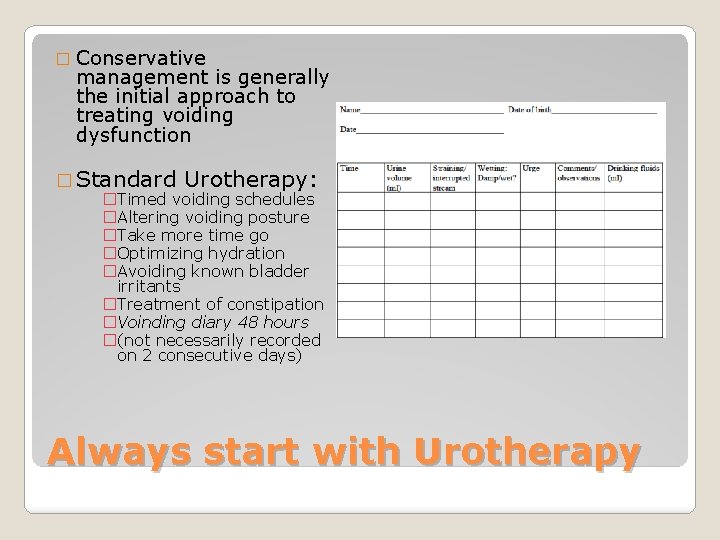
� Conservative management is generally the initial approach to treating voiding dysfunction � Standard Urotherapy: �Timed voiding schedules �Altering voiding posture �Take more time go �Optimizing hydration �Avoiding known bladder irritants �Treatment of constipation �Voinding diary 48 hours �(not necessarily recorded on 2 consecutive days) Always start with Urotherapy

� Voiding before the child feels the urge to urinate ◦ At least every 2 hours at home and school �Send a school note �Some teachers will set their telephone to alarm �Young children and those with ADHD will need to be reminded �Watch alarm reminders available for older children (>6 years) � Taking the time to empty to completion ◦ Double voiding if needed 2 -3 times/day at home � Avoiding Valsava voiding ◦ Use a pinwheel for teaching proper muscle contraction and relaxation Proper positioning Timed Voiding

�Not covered by insurance �Range in price from $40 -$80 �Available at pottymd. com and bedwettingstore. com Vibrating watch reminders

� Water, Water � Calculating needs water � Iphone App: Water Your Body for $0. 99 Alternatives: Crystal light Propel Sugar-free Kool-Aid Mio Hydration � 40 pounds (4 years) ◦ 1. 5 - 16 ounce bottles � 60 pounds ◦ 2 - 16 ounce bottles � 80 pounds ◦ 2. 5 – 16 ounce bottles ◦ Estimate- Easiest way about ½ their body weight in ounces of water per day

�Used for non-neurogenic dysfunctional voiding, those with detrusor-sphincter dyssynergia �Teaches children how to voluntarily control their sphincter and pelvic floor muscles ◦ Appears to reduce voiding dysfunction in observational studies especially those with postvoid residual volumes 1] Kaye, J. D. and Palmer, L. S. , 2008. Animated biofeedback yields more rapid results than nonanimated biofeedback in the treatment of dysfunctional voiding in girls. The Journal of urology, 180(1), pp. 300 -305. [2] Wenske S, Combs AJ, Van Batavia JP, Glassberg KI, 2012. Can staccato and interrupted/fractionated uroflow patterns alone correctly identify the underlying lower urinary tract condition? The Journal of urology, 187 (6), pp. 2188– 2193. USA Biofeedback Training

� The most commonly used anticholinergic agent is oxybutynin (Ditropan). � Works by decreasing the frequency of uninhibited bladder muscle contractions during filling phase and increases bladder capacity. ◦ Comes in liquid and tablet formulation ◦ 1 mg/ml and 5, 10 and 15 mg tablets immediate and extended release �ER shown to be superior to IR in studies �ER needs to be swallowed �IR chew or swallow ◦ Recommended daily dose is 0. 3 -0. 6 mg/kg ◦ Max 20 mg/day ◦ Start twice daily and increase to three times daily if needed Pharmacologic Therapy Ramsay S, Bolduc Stephane. Overactive bladder in children. Can Urol Assoc J. 2017 Jan-Feb; 11(1 -2 Suppl 1): S 74 S 79.

� The immediate-release (IR) (Ditropan®) and extended -release (ER) (Ditropan XL®) formulations of oxybutynin are currently the only pharmacological agents FDA approved for the treatment of OAB in children age 5 years and older in North America for IR and 6 years and older for ER. ◦ However, only one small clinical trial published has evaluated the efficacy compared to placebo in children. ◦ It showed no improvement in frequency of daytime wetting between oxybutynin and placebo. ◦ Observational studies report improvement in symptoms. �Adult data has shown a reduction in urinary incontinence. Oxybutynin Chang SJ, Van Laecke E, Bauer SB, et al. Treatment of daytime urinary incontinence: A standardization document from the International Children’s Continence Society. Neurourol Urodyn. 2017; 36: 43– 50. https: //doi. org/10. 1002/nau. 22911. [Pub. Med]

�Side effects ◦ 58% reported no side effects ◦ 19% constipation ◦ 17% dry mouth ◦ 14% flushing ◦ 5% heat intolerance Oxybutynin ◦ CNS side effects more common in children typically in first month �Hallucination �Agitation �Sedation �Confusion �Amnesia �Nightmares

Percentage of children who wet the bed Chronological age � 16% � 5% � 10 years � 1 -2% � 15 years+ years Primary Nocturnal Enuresis (monosymptomatic enuresis) Nocturnal enuresis in children: Management. (2016). www. uptodate. com

�Primary ◦ Never achieved nighttime dryness ◦ 80% of children �Secondary ◦ Dry 6 months before the wetting begins ◦ 20% of children ◦ Address underlying stressor if one can be identified but most have no cause and are treated in the same manner as primary enuresis Nocturnal enuresis in children: Management. (2016). www. uptodate. com

�Deep sleepers or sleep disorders �Significant stress or those with psychological issues �Increased urine production at night and ADH �Daytime bowel and bladder problems (20%) �Drinking fluids before bedtime �Certain medications ◦ Diuretics –lithium �Familial tendencies Theories about Nocturnal Enuresis P. Smith. Overcoming Bladder & Bowel Problems in Children. 2004. “What are abnormal potty habits”, p. 49 -53. &. H. Bennett, MD. 2005. Waking Up Dry. “Why Kids Wet the Bed. ” p. 17 -29.

�Determine if any period of dryness �Number of wet nights per week �Presence of daytime wetting or symptoms �Family history of nocturnal enuresis �Ask what the family has tried History I

�Reassuring parents that time is the ultimate cure and that enuresis is not associated with a physical abnormality �Alarm clocks �Dysfunctional elimination program if daytime incontinence present or constipation is an issue ◦ At least 4 years of age or older �Bedwetting alarms ◦ 6 years and older �Pharmacological agents ◦ 7 years and older Treatment of Nocturnal Enuresis I. Franco, A. von Gontard, M. De Gennaro, et al. Evaluation and treatment of nonmonosymptomatic nocturnal enuresis: a standardization document from the International Children's Continence Society. Journal of Pediatric Urology (2013) 9, 234 e 243 y.

�Emits an auditory and/or tactile stimulus in response to wetting ◦ A behavioral conditioning approach �The most effective treatment option for enuresis ◦ 50 -80% successful �Types of alarms ◦ Wearable alarms ◦ Wireless alarms ◦ Bell-and-pad alarms Bedwetting Alarms H. Bennett, MD. 2005. Waking Up Dry. “The Bedwetting Alarm. ” p. 99 -112.


�Most alarm users do not respond without assistance to the alarm in the beginning �Caregiver’s must go in and wake the child then tell them what to do next �As the child starts to make the association, the caregivers’ role is less �The first few weeks are the most difficult �Can take 6 -12 weeks to achieve continence What to expect from alarms

�Families �May not have to be motivated be an option if child shares a room with sibling �Need to be used nightly �No insurance plans cover the cost of an alarm �Obtain over the internet or via telephone ◦ www. bedwettingstore. com ◦ www. pottymd. com ◦ www. amazon. com �Cost average $90 ($60 -$200) Bedwetting Alarms H. Bennett, MD. 2005. Waking Up Dry. “The Bedwetting Alarm. ” p. 99 -112.

�DDAVP ◦ Since December 2007, the nasal spray is no longer FDA approved for treatment of enuresis due to the risk for hyponatremic seizures ◦ Enhances reabsorption of water in the kidneys by increasing cellular permeability of the collecting ducts ◦ The oral dose titrated from 1 -3 tablets (0. 2 -0. 6 mg)every 7 -10 days ◦ Take prior to bedtime ◦ FDA approved for children greater than or equal to 6 years of age Medications
�DDAVP TABLETS ◦ Must take medication nightly to stay dry � 25% exhibit a reduction in wetting � 25% become completely dry � 50% no change ◦ Very expensive but covered by most insurances �Cost 0. 1 mg tablet $4. 13 and 0. 2 mg tab $5. 96 ($180 to $540 per month) ◦ Limit fluids 1 hour before and 8 hours after administration ◦ Not recommended if child has illness (vomiting, diarrhea, fever) Medications

�Drugs for nocturnal enuresis in children (other than desmopressin and tricyclics). ◦ Evidence suggests combination therapy with anticholinergic therapy increased the efficacy of other established therapies such as imipramine, desmopressin and enuresis alarms by reducing the relapse rates, by about 20%, �not possible to identify the characteristics of children who would benefit from combination therapy Cochrane Review-

�Imipramine (has dual alpha agonist and anticholinergic activity) ◦ Decreases time spent in REM sleep ◦ Stimulates ADH secretion ◦ Relaxes detrusor muscle �Dosing ◦ 25 mg for children 5 to 8 years ◦ 50 mg for older children up to 12 years of age ◦ 75 mg in children > 12 years of age �Effect is quick and stop if no changes after a 3 week trial with a week at max dose Medications Management of nocturnal enuresis in children. (2009). www. uptodate. com

� Imipramine ◦ Side effects are uncommon � 5% develop neurological symptoms ◦ Nervousness ◦ Personality change ◦ Sleep disturbance � Cardiovascular disturbance- obtain baseline and periodic EKGs in those with cardiac disease ◦ Especially in overdose �Black box warning ◦ Increased possibility of suicide in those with depressive symptoms Medications

�Abnormal toileting habits are the most common cause of urinary tract infections in children ◦ Not emptying the bladder often enough ◦ Constipation ◦ Poor hygiene �Other contributing factors ◦ Gender ◦ Poor bladder immunity ◦ Structural anomalies associated with febrile urinary tract infections Causes of Urinary Tract Infections
The Culprits E. Coli Found in 90% of UTIs ◦ Escherichia Coli ◦ Enterococcus ◦ P. aeruginosa ◦ Klebsiella sp. ◦ Proteus sp. ◦ Enterobacter sp. ◦ Coag-negative staph ◦ Staph aureus ◦ Candida sp. Common Pathogens

Specimen Collection Catheterization Best Practical Method � Clean Voided Specimen ◦ 80% Accuracy � Catheterized Specimen ◦ 95% Accuracy � Suprapubic Aspiration ◦ 21 or 22 -guage needle 1 -2 cm above PS ◦ 99 % accuracy ◦ Rarely used in clinic practice � Bagged Specimen ◦ 80% contaminated, false + �NEVER RECOMMENDED Specimen Collection

� 50, 000 -60, 000 cfu/ml of mixed flora �>100, 000 cfu/ml of Proteus mirabilis � 15, 000 cfu/ml of beta Streptococcus, group B �>100, 000 cfu/ml of E. coli Which of these is a UTI if a CCUA?

�Clean catch urine specimens ◦ Culture shows greater than 100, 000 cfu/ml of a single organism �Catheterized urine collections ◦ Greater than 50, 000 cfu/ml Urine Cultures Gold Standard. Dipstick UAs are screening tools

�No significant benefit was demonstrated when compared to placebo or no treatment in children or adults ◦ Small studies ◦ Poor methodological reporting Probiotics for Preventing UTIs Schwendger ER, Tejani AM, Lowewen PS. Probiotics fro preventing urinary tract infections in adults and children. Cochrane Database Syst Rev. 2015 Dec 23; (12).
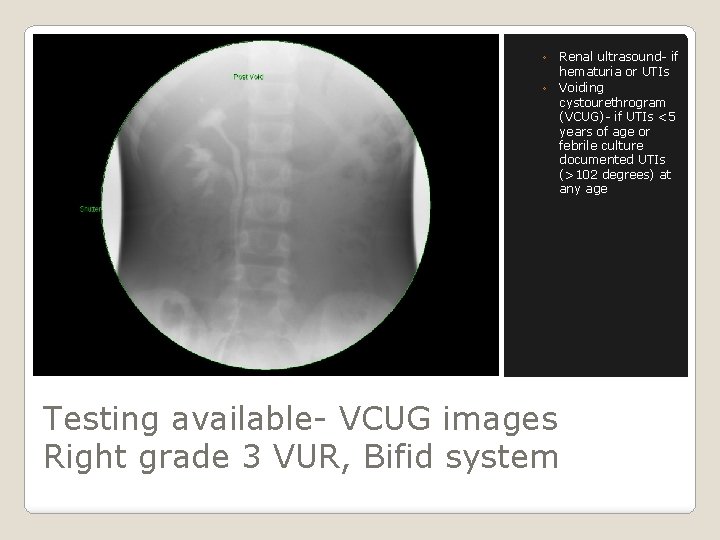
◦ Renal ultrasound- if hematuria or UTIs ◦ Voiding cystourethrogram (VCUG)- if UTIs <5 years of age or febrile culture documented UTIs (>102 degrees) at any age Testing available- VCUG images Right grade 3 VUR, Bifid system

DMSA Nuclear Renal Scan to assess for renal scarring

Questions?
- Slides: 80