Basic Advanced Airway Management Amy Gutman MD Director

“Basic” Advanced Airway Management Amy Gutman MD Director, Department of Emergency Medicine HAHV-Kingston Hospital Amy. gutman@emcare. com / amy. gutman@hahv. org

Objectives Airway Anatomy Decision-Making Algorithms Utilizing video-assisted intubation Not an “end-all-be-all” advanced airway lecture – just the basics 2

Case Study You are called to the bedside of a morbidly obese male with “shortness of breath”. He is in obvious respiratory distress, then becomes apneic You make one attempt to endotracheally intubate, but have difficulty due to his body habitus, large tongue, & short neck Patient rapidly decompensates; attempts made to BVM ventilate & oxygenate are failing What is your next step? ? 3
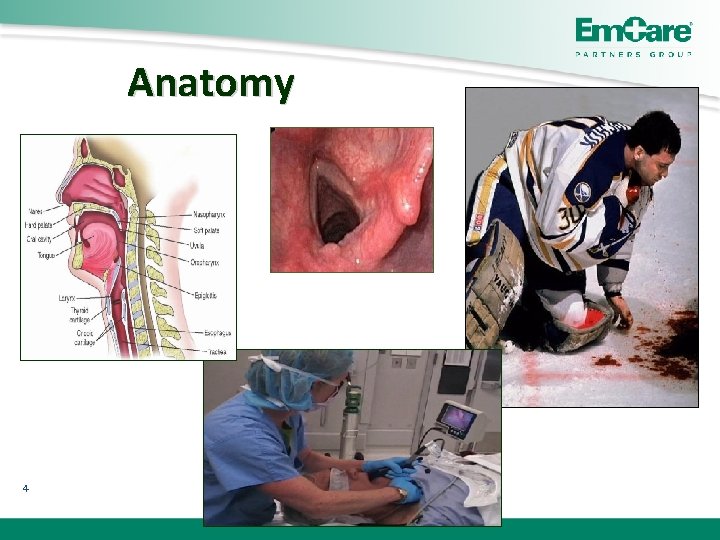
Anatomy 4
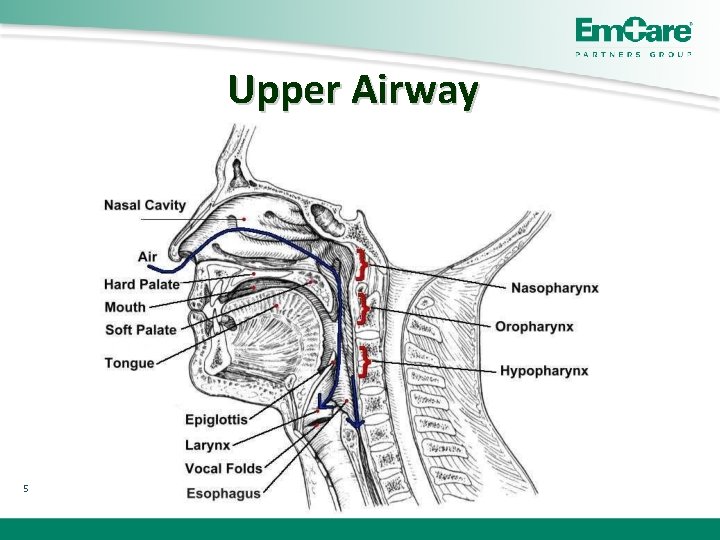
Upper Airway 5
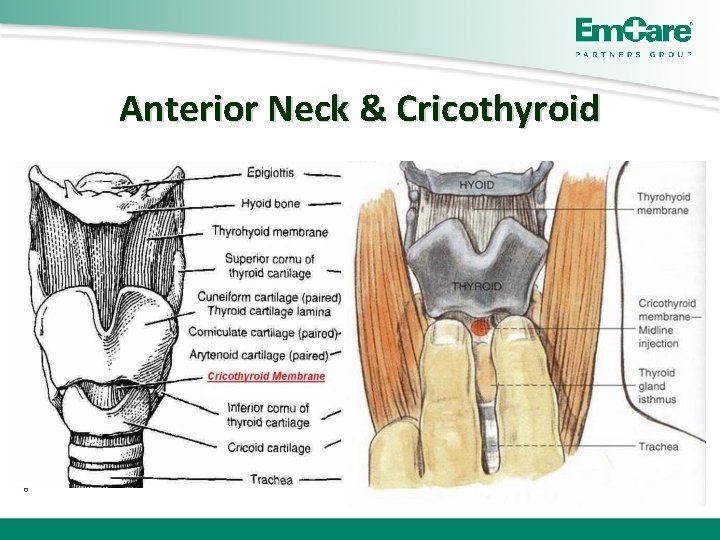
Anterior Neck & Cricothyroid 6
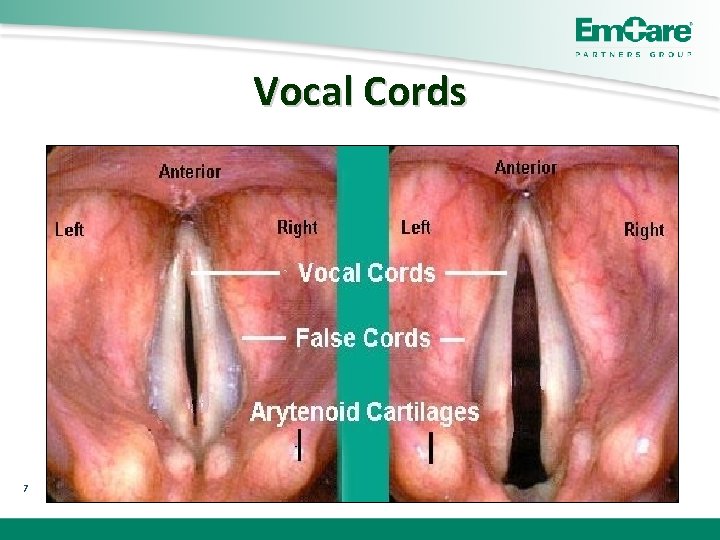
Vocal Cords 7
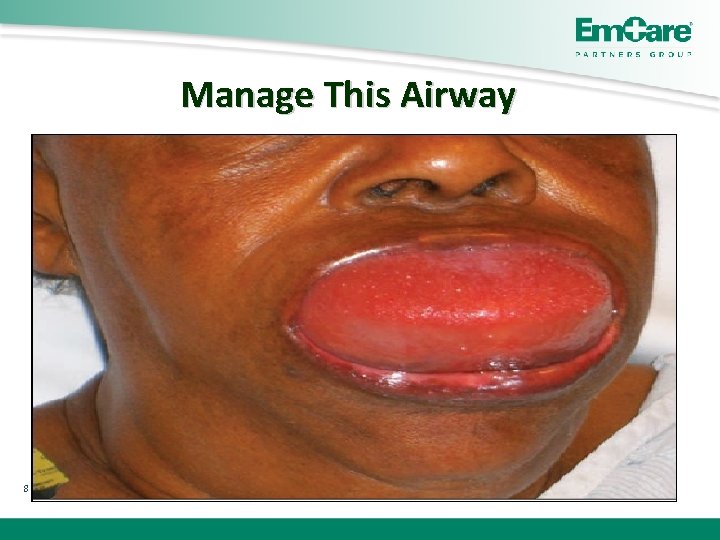
Manage This Airway 8 A: Tongue Edema Post Lye Injury Swelling B: Neck Injury With Epiglottis
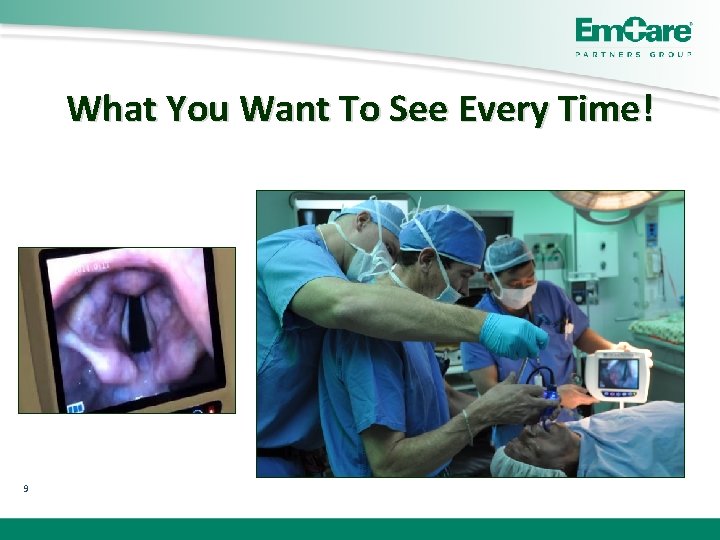
What You Want To See Every Time! 9

General Concepts Every airway is difficult until patient has a confirmed tracheal tube Just because you have never missed an airway, do not assume that you never will Limit problems by anticipating that everything is just a minute away from becoming a SNAFU 10
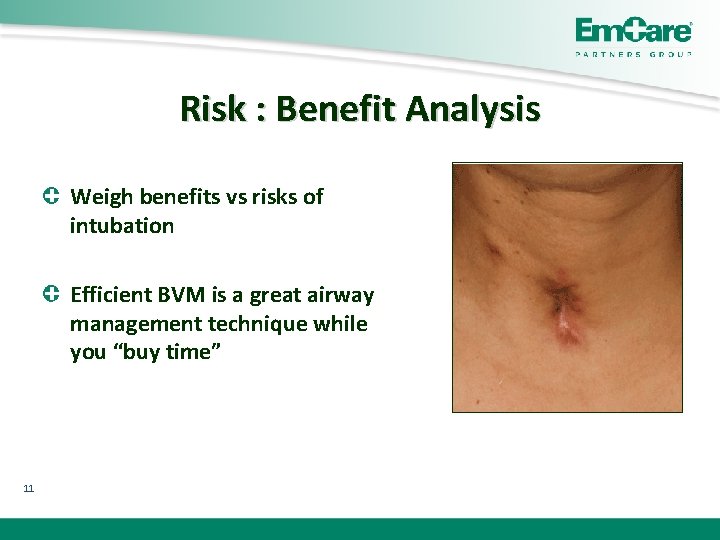
Risk : Benefit Analysis Weigh benefits vs risks of intubation Efficient BVM is a great airway management technique while you “buy time” 11

Preventing Intubation Properly position Facilitate O 2 delivery – – OP/ NP airways CPAP Meds: breathing treatments, diuretics Calm patient down Think smarter, not faster 12
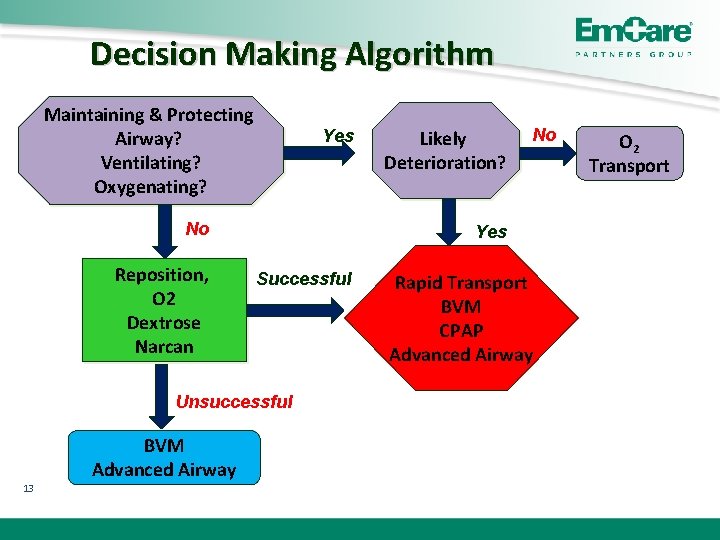
Decision Making Algorithm Maintaining & Protecting Airway? Ventilating? Oxygenating? Yes No Reposition, O 2 Dextrose Narcan 13 No Yes Successful Unsuccessful BVM Advanced Airway Likely Deterioration? Rapid Transport BVM CPAP Advanced Airway O 2 Transport
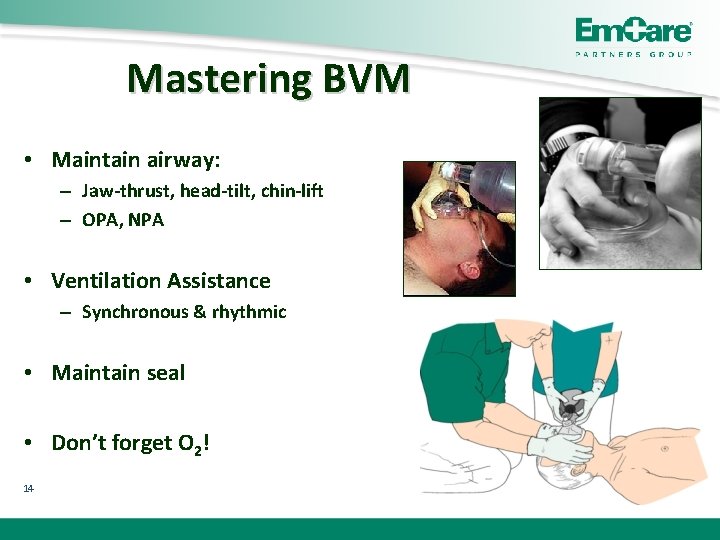
Mastering BVM • Maintain airway: – Jaw-thrust, head-tilt, chin-lift – OPA, NPA • Ventilation Assistance – Synchronous & rhythmic • Maintain seal • Don’t forget O 2! 14
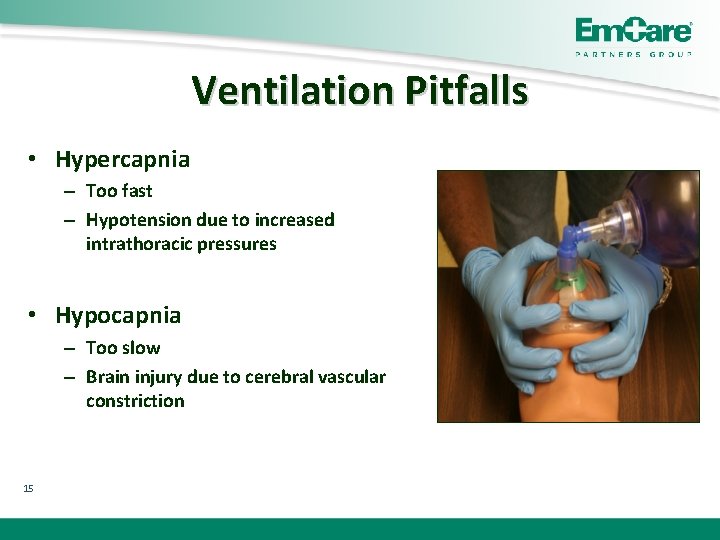
Ventilation Pitfalls • Hypercapnia – Too fast – Hypotension due to increased intrathoracic pressures • Hypocapnia – Too slow – Brain injury due to cerebral vascular constriction 15
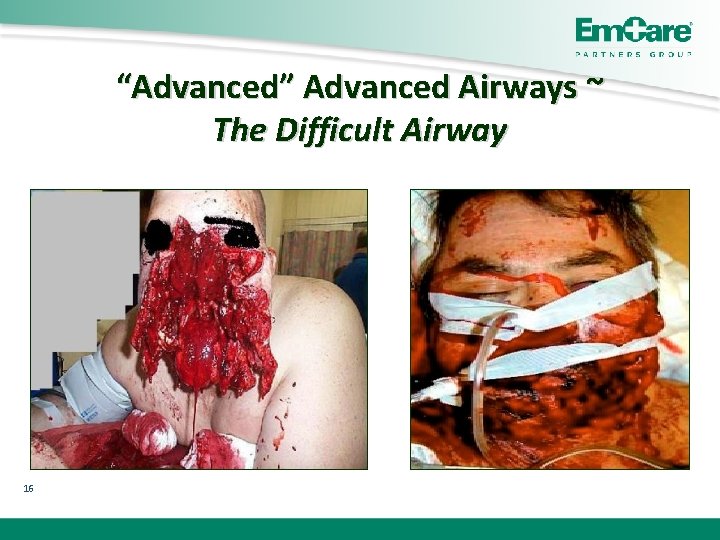
“Advanced” Advanced Airways ~ The Difficult Airway 16
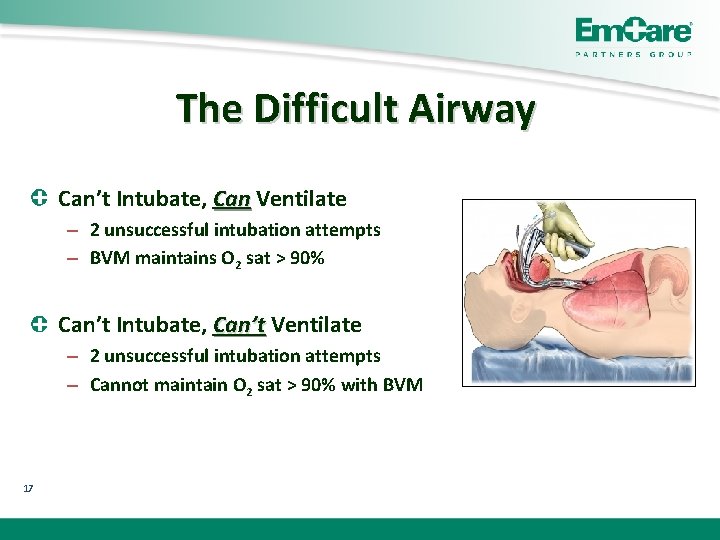
The Difficult Airway Can’t Intubate, Can Ventilate – 2 unsuccessful intubation attempts – BVM maintains O 2 sat > 90% Can’t Intubate, Can’t Ventilate – 2 unsuccessful intubation attempts – Cannot maintain O 2 sat > 90% with BVM 17
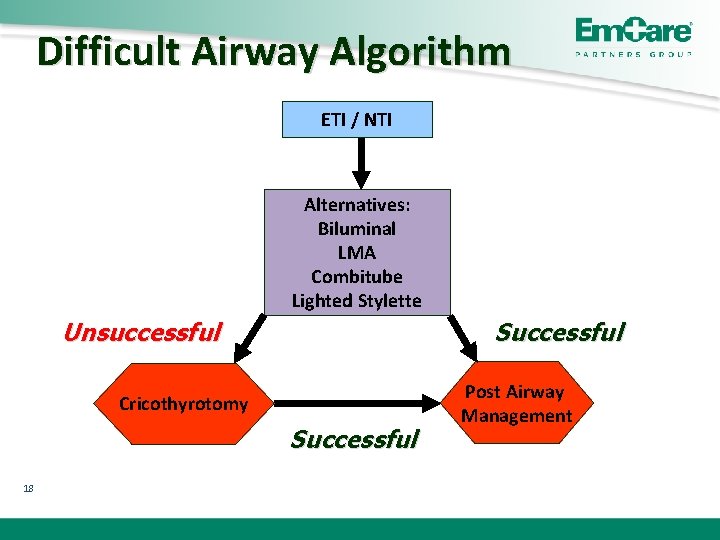
Difficult Airway Algorithm ETI / NTI Alternatives: Biluminal LMA Combitube Lighted Stylette Successful Unsuccessful Cricothyrotomy Successful 18 Post Airway Management
Plan A, B, C…D…. . F �A: “Alternate” �Tube �Blade �Approach �B: “Blind, BVM, Bougie” �Blind �BVM �Bougie-assisted �C: “Cric” �Surgical Airways 19
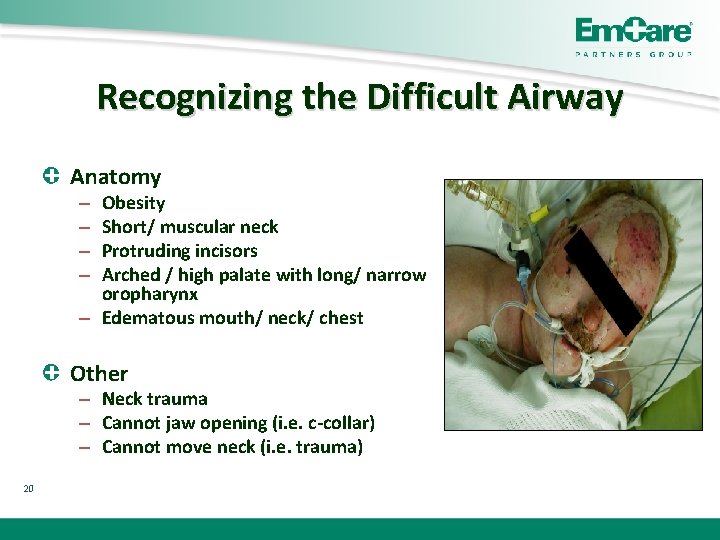
Recognizing the Difficult Airway Anatomy Obesity Short/ muscular neck Protruding incisors Arched / high palate with long/ narrow oropharynx – Edematous mouth/ neck/ chest – – Other – Neck trauma – Cannot jaw opening (i. e. c-collar) – Cannot move neck (i. e. trauma) 20

LEMON Rule �L �E �M �O �N 21 Look Externally Evaluate 3 -3 -2 Rule Mallanpati Score Obstruction Present Neck Mobility
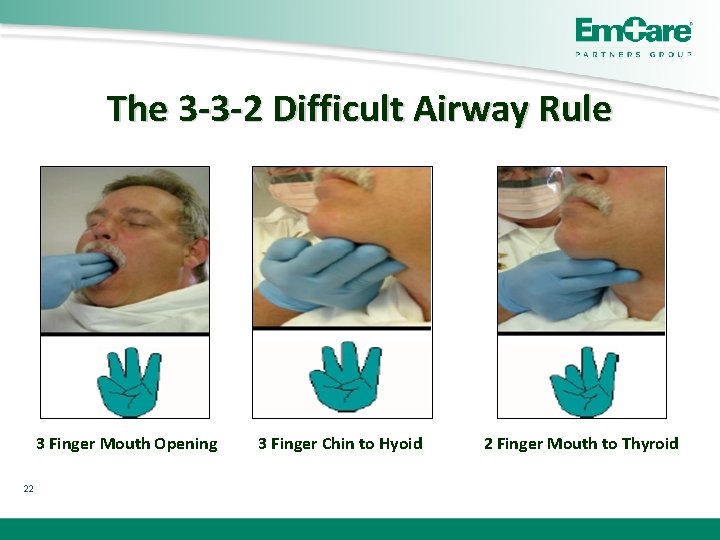
The 3 -3 -2 Difficult Airway Rule 3 Finger Mouth Opening 22 3 Finger Chin to Hyoid 2 Finger Mouth to Thyroid
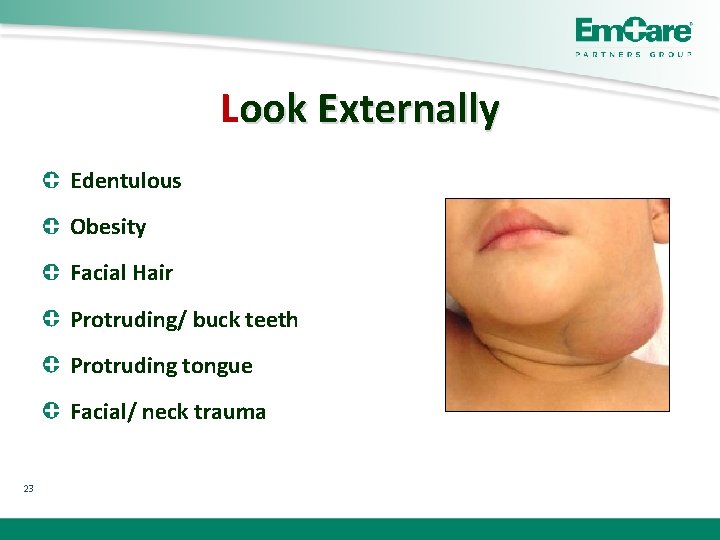
Look Externally Edentulous Obesity Facial Hair Protruding/ buck teeth Protruding tongue Facial/ neck trauma 23
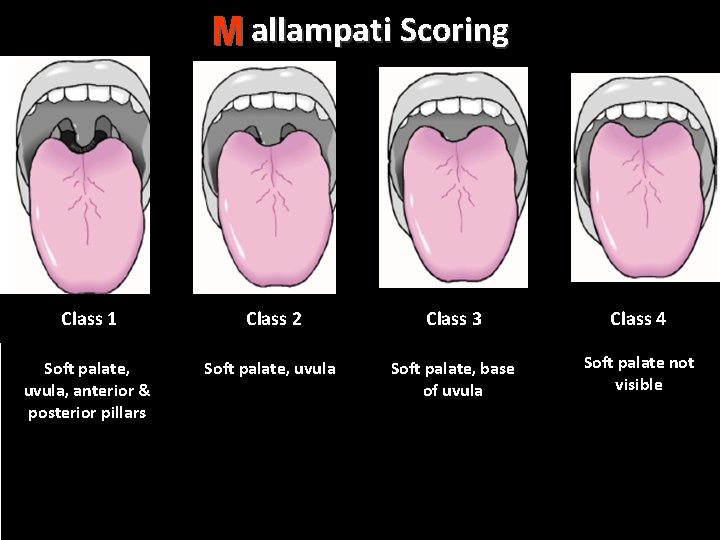
Mallampati Scoring M Class 1 Class 2 Class 3 Class 4 Soft palate, uvula, anterior & posterior pillars Soft palate, uvula Soft palate, base of uvula Soft palate not visible 24
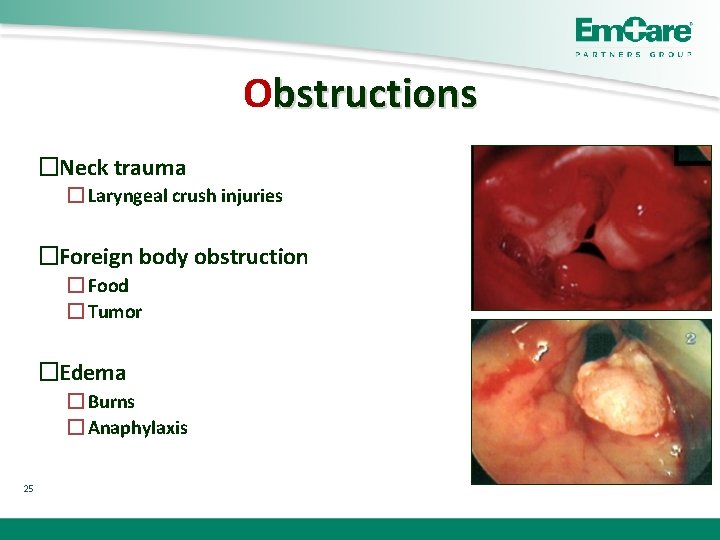
Obstructions �Neck trauma � Laryngeal crush injuries �Foreign body obstruction � Food � Tumor �Edema � Burns � Anaphylaxis 25

Neck Mobility Cannot manipulate in trauma or some populations – Kyphotic – Prior surgery Ability to flex, extend or manipulate head/ neck increases likelihood of visualizing cords 26
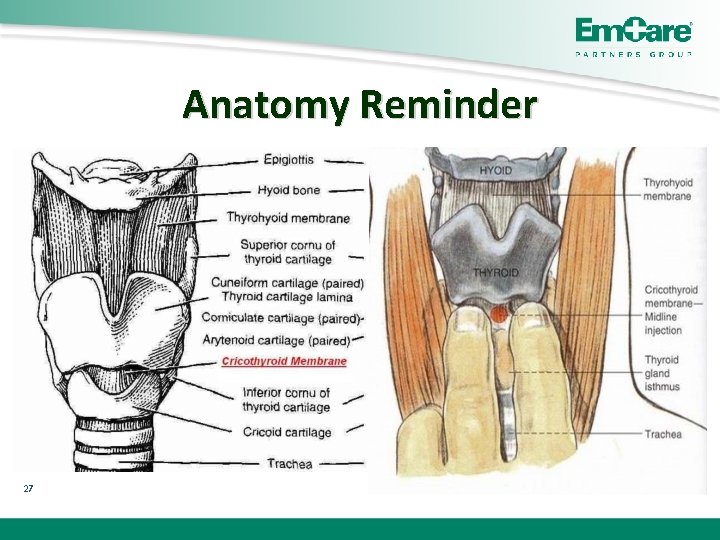
Anatomy Reminder 27

Advanced Airway Tools You GUARANTEE Failure If You Do Not Prepare! � Preoxygenate, BVM, Full O 2 tank � 2 large bore IV / IO & IVF � Monitor � 2 sizes ETT, checked cuffs, back-up � Blade, checked light, back-up � Alternative airway / videoscope checked � Handle, checked batteries, back-up � Stylette, back-up � Suction � Mc. Gills � ETCO 2 detector, back-up � Syringe x 2 � Manpower & tape 28
Advanced Airway Techniques Focus today on videoscope, but have knowledge of alternatives 29 • Endotracheal • Digital • Bougie • Nasotracheal • LMA • Supraglottic • Awake • Fiberoptic • Videoscope • Surgical
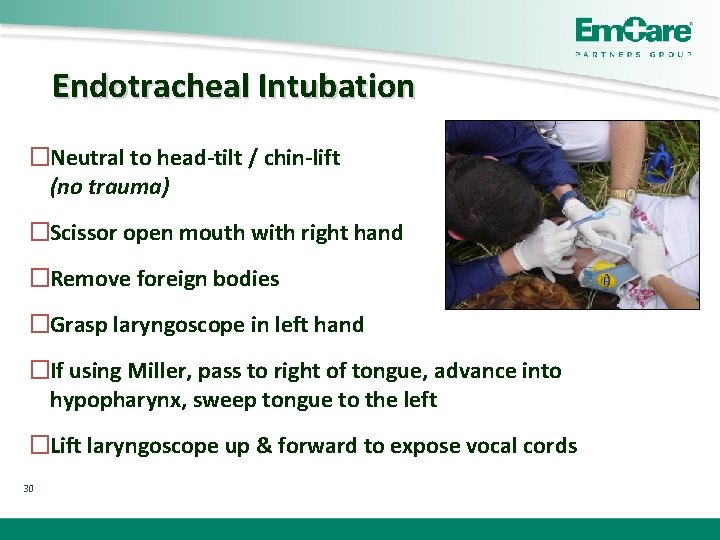
Endotracheal Intubation �Neutral to head-tilt / chin-lift (no trauma) �Scissor open mouth with right hand �Remove foreign bodies �Grasp laryngoscope in left hand �If using Miller, pass to right of tongue, advance into hypopharynx, sweep tongue to the left �Lift laryngoscope up & forward to expose vocal cords 30
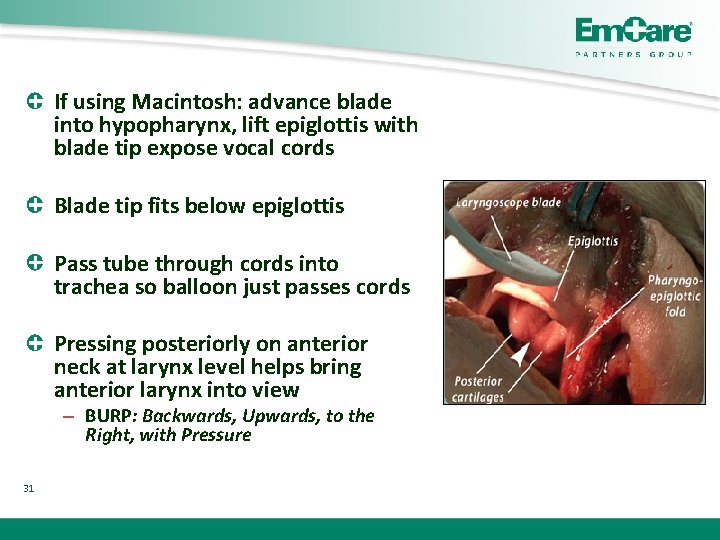
If using Macintosh: advance blade into hypopharynx, lift epiglottis with blade tip expose vocal cords Blade tip fits below epiglottis Pass tube through cords into trachea so balloon just passes cords Pressing posteriorly on anterior neck at larynx level helps bring anterior larynx into view – BURP: Backwards, Upwards, to the Right, with Pressure 31
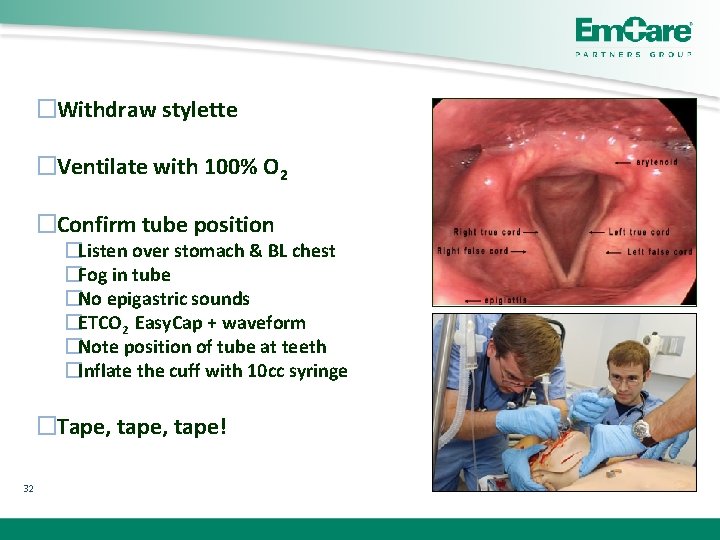
�Withdraw stylette �Ventilate with 100% O 2 �Confirm tube position �Listen over stomach & BL chest �Fog in tube �No epigastric sounds �ETCO 2 Easy. Cap + waveform �Note position of tube at teeth �Inflate the cuff with 10 cc syringe �Tape, tape! 32
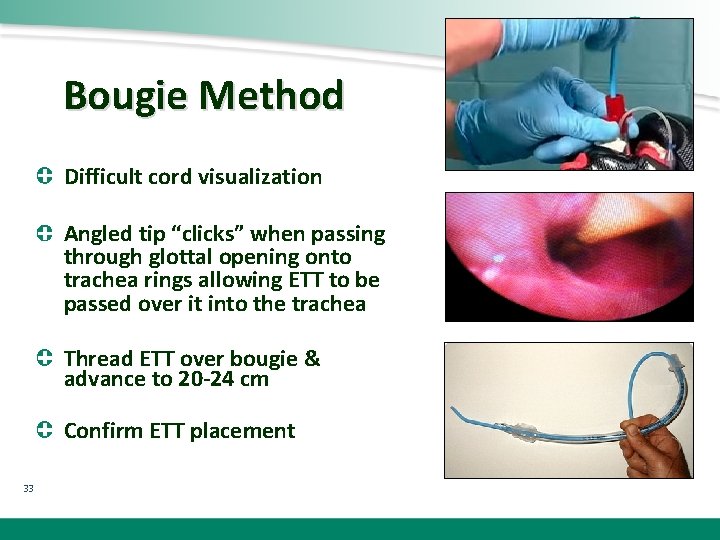
Bougie Method Difficult cord visualization Angled tip “clicks” when passing through glottal opening onto trachea rings allowing ETT to be passed over it into the trachea Thread ETT over bougie & advance to 20 -24 cm Confirm ETT placement 33
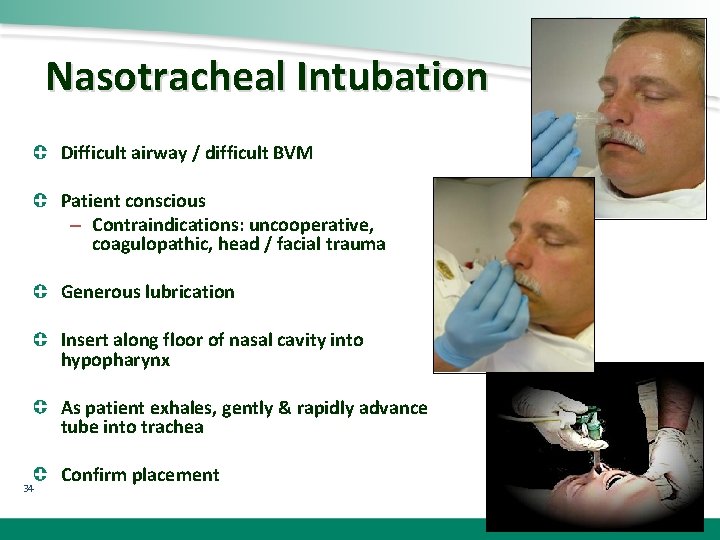
Nasotracheal Intubation Difficult airway / difficult BVM Patient conscious – Contraindications: uncooperative, coagulopathic, head / facial trauma Generous lubrication Insert along floor of nasal cavity into hypopharynx As patient exhales, gently & rapidly advance tube into trachea 34 Confirm placement
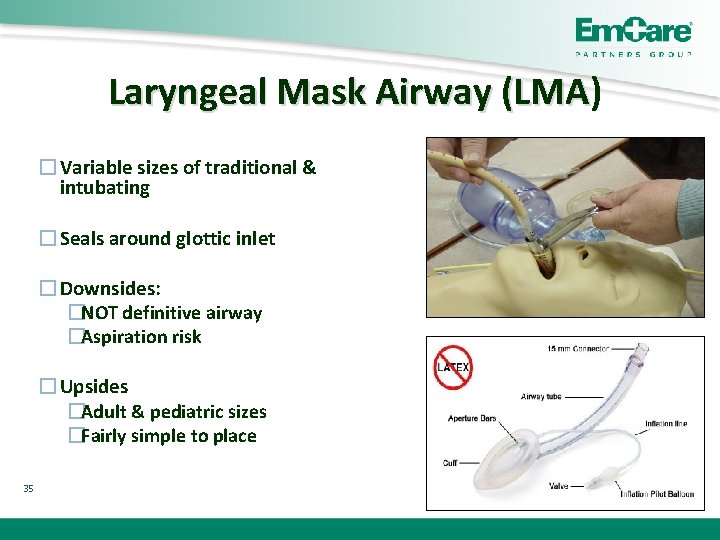
Laryngeal Mask Airway (LMA) (LMA �Variable sizes of traditional & intubating �Seals around glottic inlet �Downsides: �NOT definitive airway �Aspiration risk �Upsides �Adult & pediatric sizes �Fairly simple to place 35
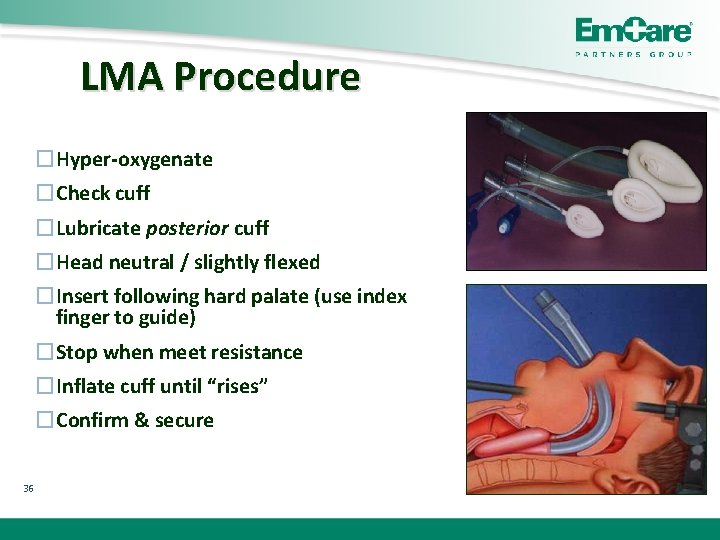
LMA Procedure �Hyper-oxygenate �Check cuff �Lubricate posterior cuff �Head neutral / slightly flexed �Insert following hard palate (use index finger to guide) �Stop when meet resistance �Inflate cuff until “rises” �Confirm & secure 36
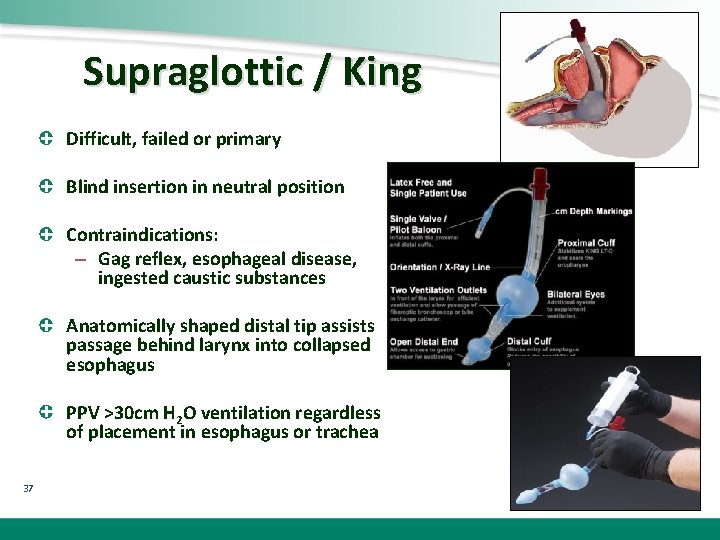
Supraglottic / King Difficult, failed or primary Blind insertion in neutral position Contraindications: – Gag reflex, esophageal disease, ingested caustic substances Anatomically shaped distal tip assists passage behind larynx into collapsed esophagus PPV >30 cm H 2 O ventilation regardless of placement in esophagus or trachea 37
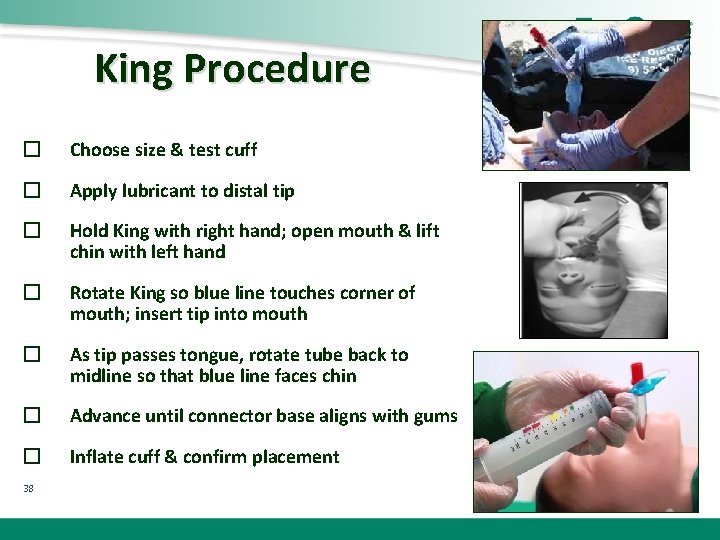
King Procedure � Choose size & test cuff � Apply lubricant to distal tip � Hold King with right hand; open mouth & lift chin with left hand � Rotate King so blue line touches corner of mouth; insert tip into mouth � As tip passes tongue, rotate tube back to midline so that blue line faces chin � Advance until connector base aligns with gums � Inflate cuff & confirm placement 38
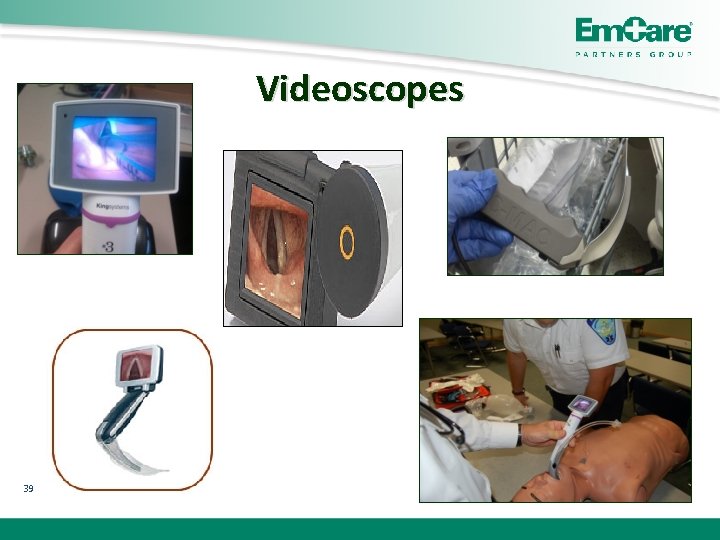
Videoscopes 39
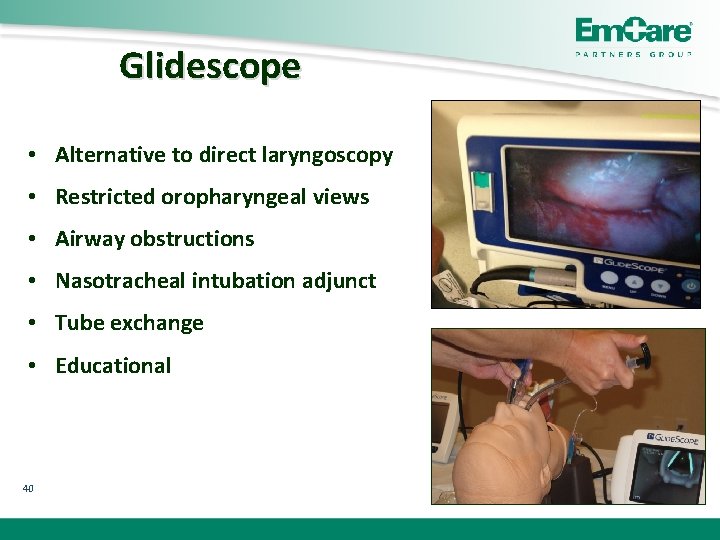
Glidescope • Alternative to direct laryngoscopy • Restricted oropharyngeal views • Airway obstructions • Nasotracheal intubation adjunct • Tube exchange • Educational 40

Glidescope Technique • Open patient’s mouth & insert glidescope exactly as you would a laryngoscope • Watch video screen, not patient • When cords visualized, slide lubricated ETT alongside glidescope handle until visualized on screen passing cords • Remove handle, inflate cuff, confirm placement 41
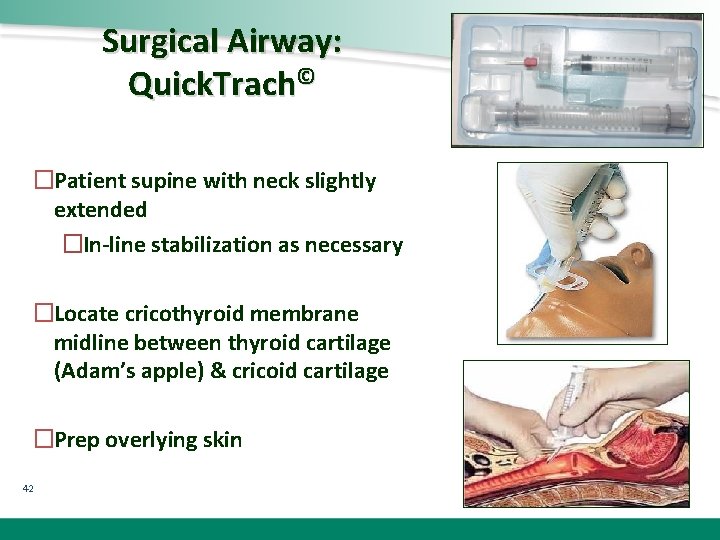
Surgical Airway: Quick. Trach© �Patient supine with neck slightly extended �In-line stabilization as necessary �Locate cricothyroid membrane midline between thyroid cartilage (Adam’s apple) & cricoid cartilage �Prep overlying skin 42
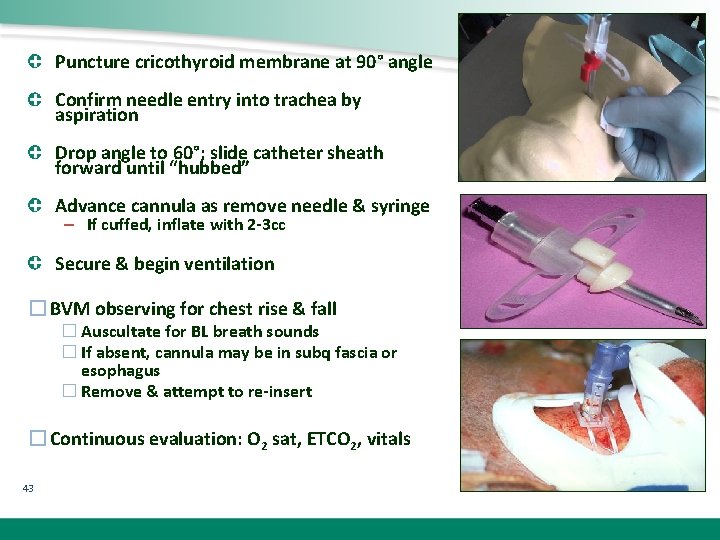
Puncture cricothyroid membrane at 90° angle Confirm needle entry into trachea by aspiration Drop angle to 60°; slide catheter sheath forward until “hubbed” Advance cannula as remove needle & syringe – If cuffed, inflate with 2 -3 cc Secure & begin ventilation � BVM observing for chest rise & fall � Auscultate for BL breath sounds � If absent, cannula may be in subq fascia or esophagus � Remove & attempt to re-insert � Continuous evaluation: O 2 sat, ETCO 2, vitals 43
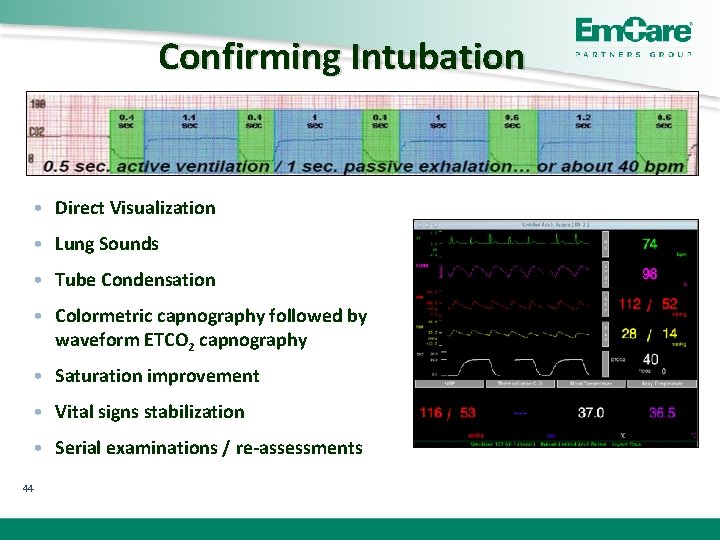
Confirming Intubation • Direct Visualization • Lung Sounds • Tube Condensation • Colormetric capnography followed by waveform ETCO 2 capnography • Saturation improvement • Vital signs stabilization • Serial examinations / re-assessments 44

GUARANTEED Failure If You Do Not Prepare or You Panic! Preoxygenate, BVM, Full O 2 tank 2 large bore IV / IO & IVF Monitor 2 sizes ETT, checked cuffs, back-up Blade, checked light, back-up Alternative airway checked Handle, checked batteries, back-up Stylette, back-up Suction Mc. Gills ETCO 2 detector, back-up Syringe x 2 Manpower & tape 45

References 46

Thank You! Find me in HAHV, Kingston NY Email: – Amy. gutman@emcare. com – Amy. Gutman@hahv. org – preshospitalmd@gmail. com Twitter: – @prehospitalmd Personal Webpage: – www. preparedrescuer. com 47
- Slides: 47