m Laryngospas and Negative Pressure Pulmonary Edema v













- Slides: 23

m Laryngospas and Negative Pressure Pulmonary Edema ��. ���������

v Laryngospasm is a form of airway obstruction. v Laryngospasm is usually easily detected and managed, but may present atypically and/or be precipitated by factors which are not immediately recognized. v If poorly managed, it has the potential to cause morbidity and mortality such as severe hypoxaemia, pulmonary aspiration, and post-obstructive

SIGNS • Inspiratory stridor/airway obstruction • Increased inspiratory efforts/tracheal tug • Paradoxical chest/abdominal movements • Desaturation • Bradycardia esp. in children

THINK OF • Airway irritation and/or obstruction • Blood/secretions in the airway • Regurgitation and aspiration • Excessive stimulation/“light” anaesthesia

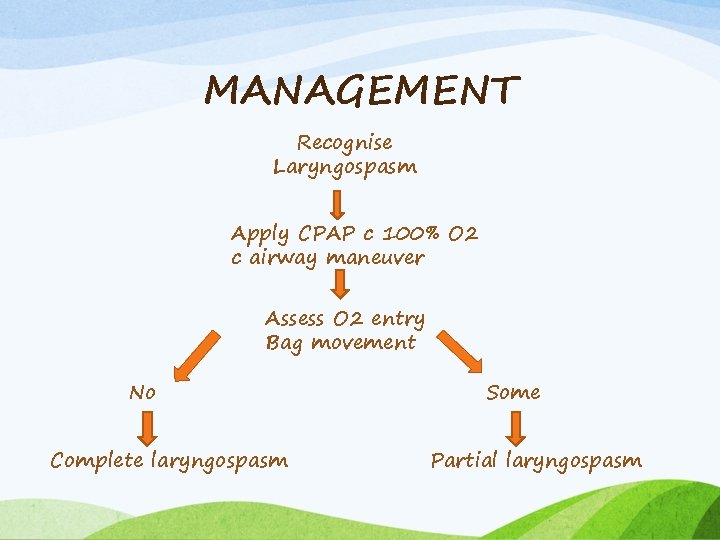
MANAGEMENT Recognise Laryngospasm Apply CPAP c 100% O 2 c airway maneuver Assess O 2 entry Bag movement No Complete laryngospasm Some Partial laryngospasm

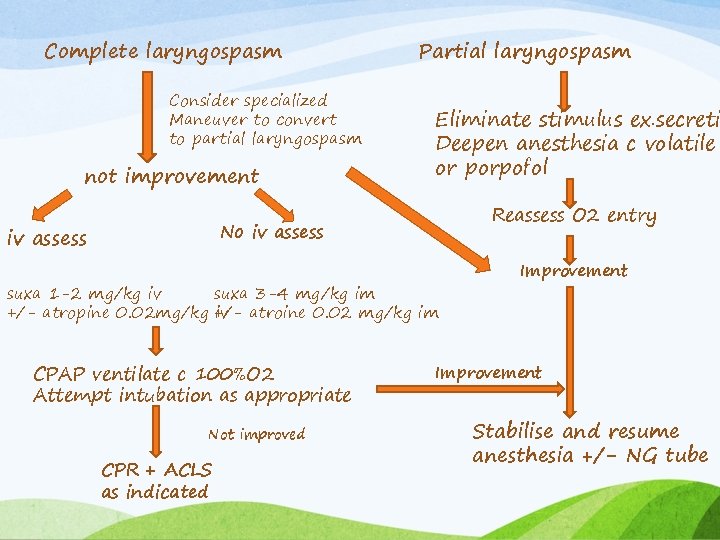
Complete laryngospasm Consider specialized Maneuver to convert to partial laryngospasm not improvement Partial laryngospasm Eliminate stimulus ex. secreti Deepen anesthesia c volatile or porpofol Reassess O 2 entry No iv assess suxa 1 -2 mg/kg iv suxa 3 -4 mg/kg im +/- atropine 0. 02 mg/kg +/iv atroine 0. 02 mg/kg im CPAP ventilate c 100%O 2 Attempt intubation as appropriate Not improved CPR + ACLS as indicated Improvement Stabilise and resume anesthesia +/- NG tube

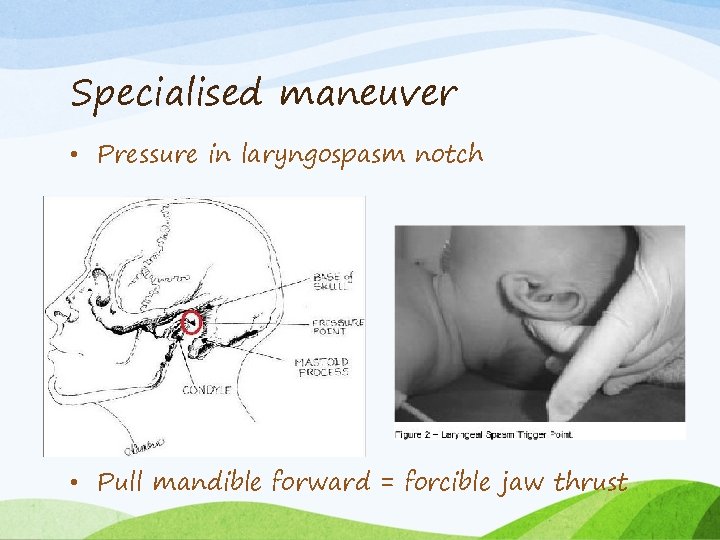
Specialised maneuver • Pressure in laryngospasm notch • Pull mandible forward = forcible jaw thrust

Negative Pressure Pulmonary Edema

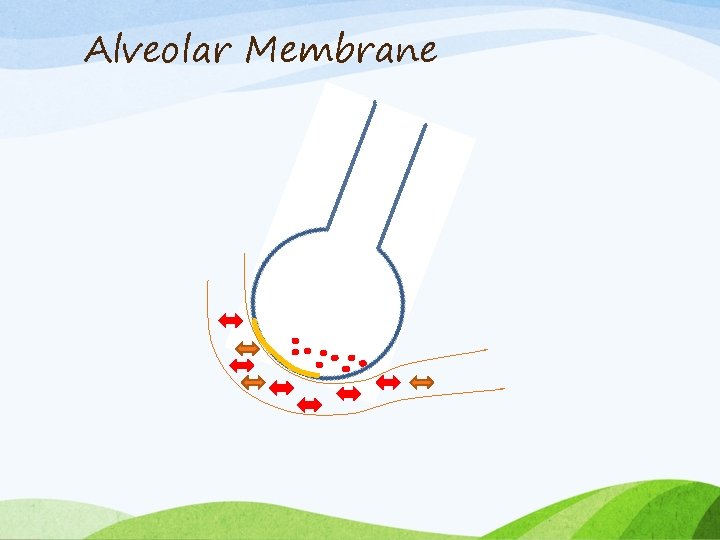
Mechanism of Edema Formation • Two theories on the edema fluid formation • One of theory suggests significant fluid shifts due to changes in intrathoracic pressure and hydrostatic transpulmonary gradient due to increased blood flow in pulmonary vessel. • The second proposed mechanism involves the disruption of the alveolar epithelial and pulmonary microvascular membranes from severe mechanical stress which leads to increased pulmonary capillary permeability and protein-rich pulmonary edema.

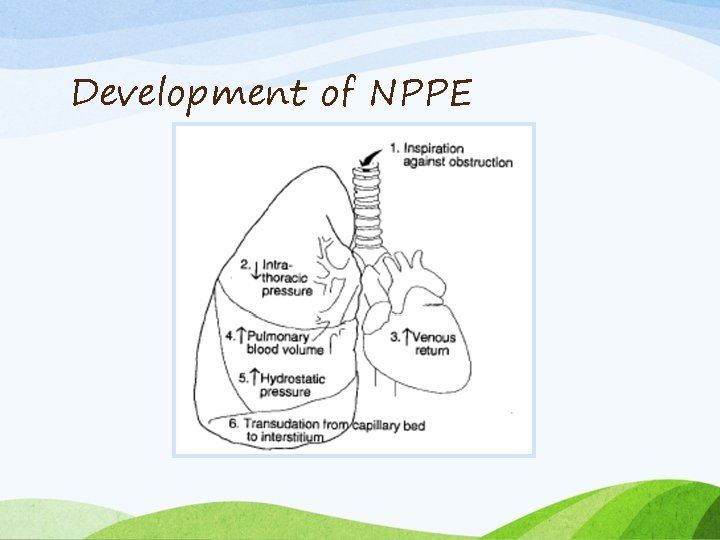
Negative Pressure Pulmonary Edema • Inspiratory efforts against a closed glottis (modified Mueller maneuver) may result in pleural pressures (> - 100 cm H 2 O) • Hypoxic pulmonary vasoconstriction • These changes result in: • Increased transmural pressure • Fluid filtration into the lung • Development of pulmonary edema and capillary failure.

Development of NPPE

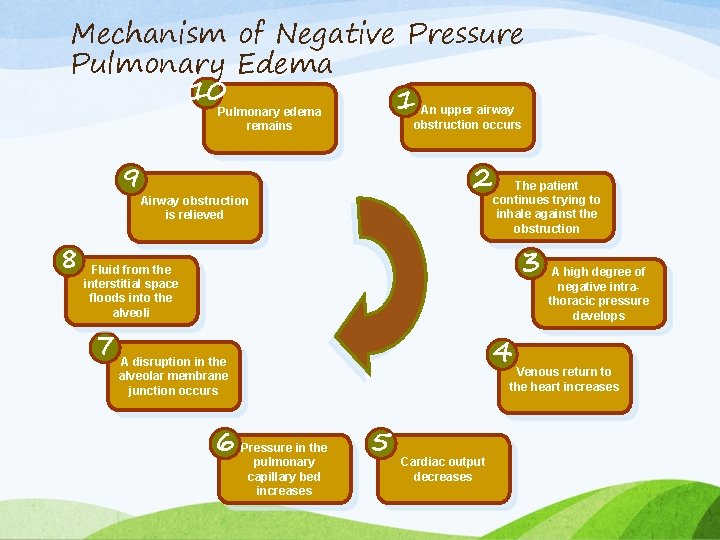
Mechanism of Negative Pressure Pulmonary Edema 10 1 An upper airway obstruction occurs Pulmonary edema remains 9 2 Airway obstruction is relieved 8 The patient continues trying to inhale against the obstruction 3 Fluid from the interstitial space floods into the alveoli 7 A disruption in the 4 A high degree of negative intrathoracic pressure develops Venous return to the heart increases alveolar membrane junction occurs 6 Pressure in the pulmonary capillary bed increases 5 Cardiac output decreases

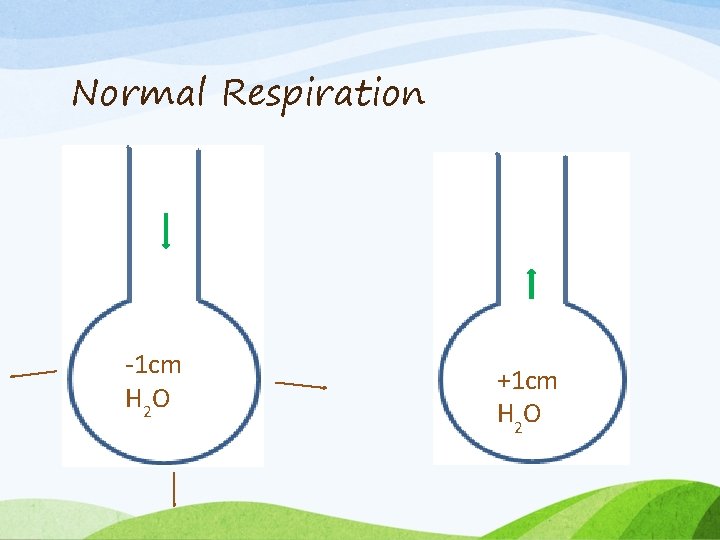
Normal Respiration -1 cm H 2 O +1 cm H 2 O

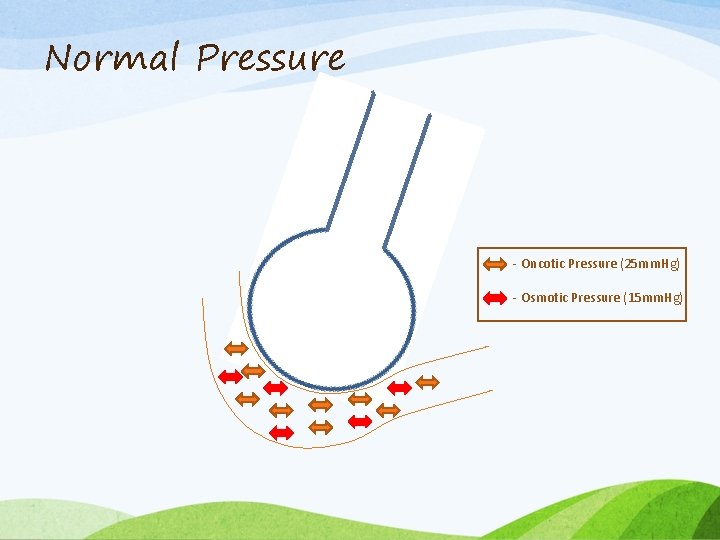
Normal Pressure - Oncotic Pressure (25 mm. Hg) - Osmotic Pressure (15 mm. Hg)

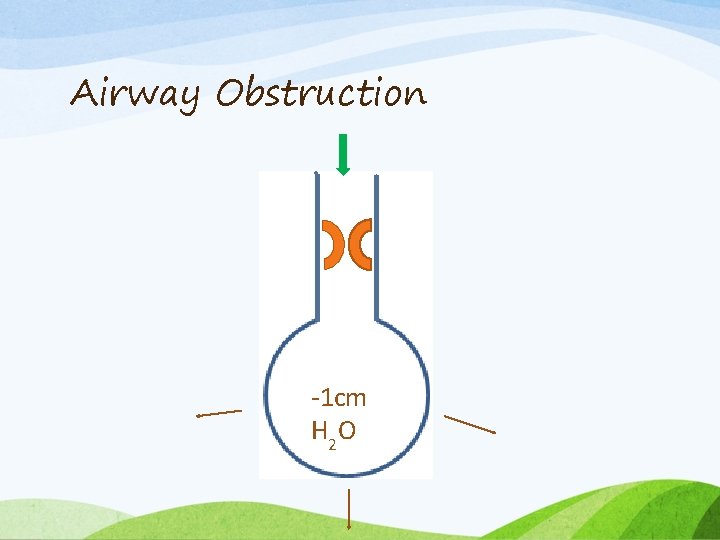
Airway Obstruction -1 cm H 2 O

Altered pressure

Alveolar Membrane

Risk assessment • Laryngospasm • Obesity, OSA • Young male athlets • Epiglotitis • Croup • Partial trachial obstruction by FB • Upper airway pathology ex. laryngomalacia, vocal cord paralysis • Obstructed ETT or LMA • Difficult intubation, nasal, oral or pharyngeal • Surgical site ex. Oropharynx, neck, urogenital • Extubation during light planes of anesthesia • Secretions falling on the vocal cords.

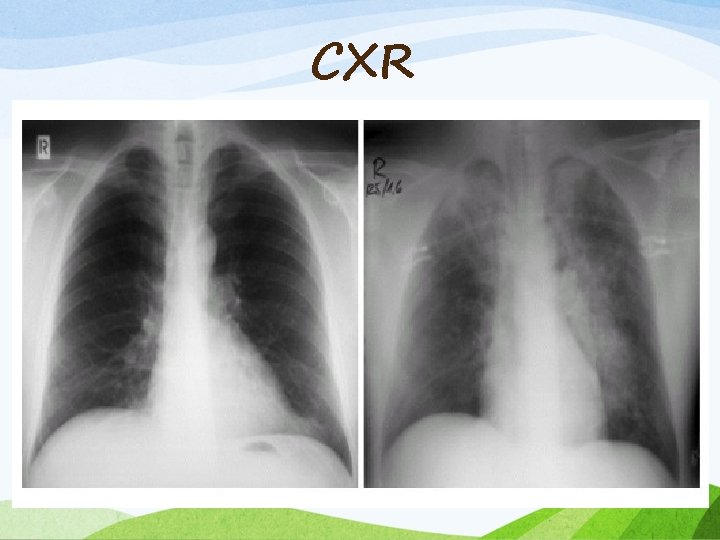
Signs and Symptoms • Frothy pink pulmonary secretions : Hallmark sign • Tachycardia, hypertension • Diaphoresis • Auscultation : Rales, Occasionally wheezing • Hypoxemia on pulse oximetry or ABG • Bilateral, alveolar infiltrates on chest x-ray

CXR

Differential diagnosis • ARDS • Intravascular volume excess • Cardiac abnormalities • Pulmonary emboli

Treatment • Early diagnosis • Reestablishment of the airway • Adequate oxygenation • Application of positive airway pressure • Via face mask or LMA • Endotracheal intubation with vent support • Although NPPE does not result from fluid overload, most authors recommend gentle diuresis using low-dose furosemide(1 mg/kg).

Prevention • Early recognition • Avoid potential obstruction • Ensure adequate depth of anesthesia during use of facemask or LMA • Consider the use of Bite block to ensure patency of artificial airway during emergence from anesthesia • Perform trachial extubation in fully awake Pt.