OXYGENATION Paula Ruedebusch ARNP DNP INTRAPLEURAL PRESSURE Pressure

OXYGENATION Paula Ruedebusch, ARNP, DNP
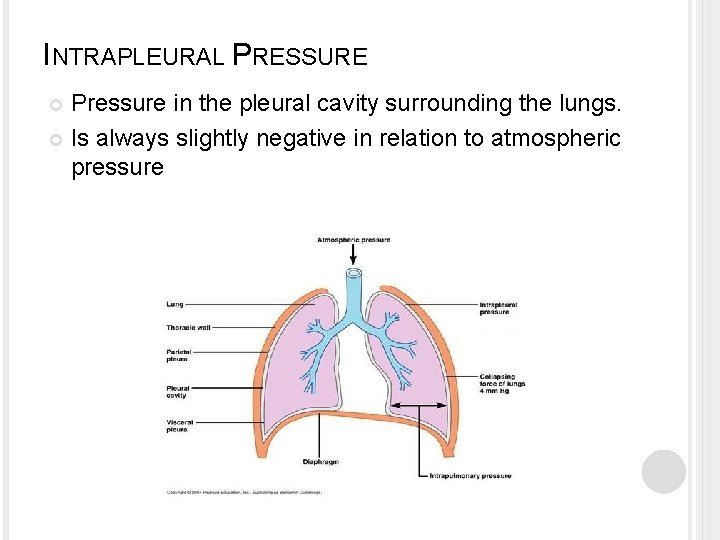
INTRAPLEURAL PRESSURE Pressure in the pleural cavity surrounding the lungs. Is always slightly negative in relation to atmospheric pressure
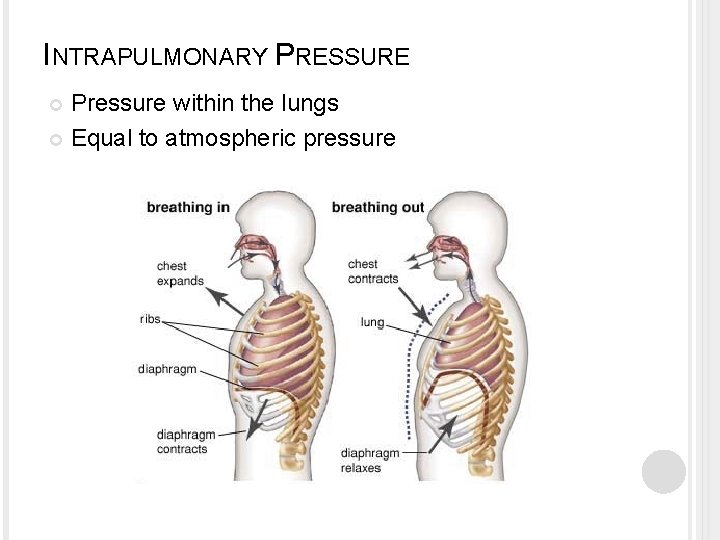
INTRAPULMONARY PRESSURE Pressure within the lungs Equal to atmospheric pressure
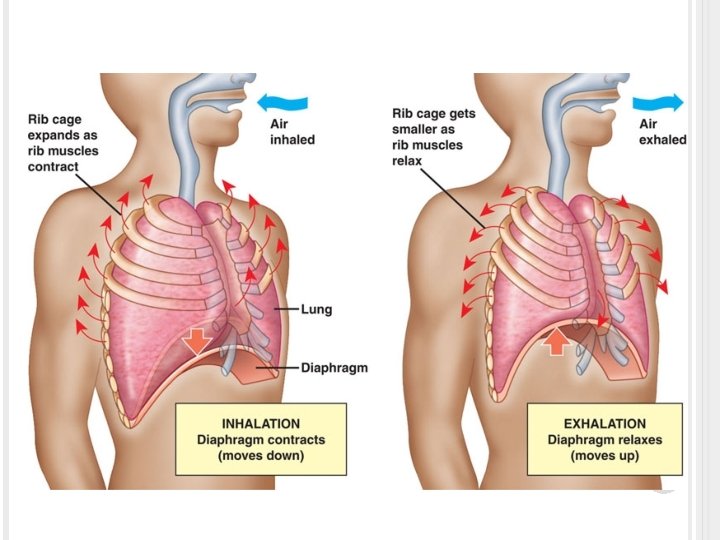

Tidal volume � Approx. 500 m. L of air is inspired and expired with each breath Lung compliance � Expansibility or stretchability of lung tissue, plays a significant role in the ease of ventilation Lung recoil � The continual tendency of the lungs to collapse away from the chest wall. � Elastic fibers in lung tissue contribute to lung recoil, also surface tension of fluid lining the alveoli.
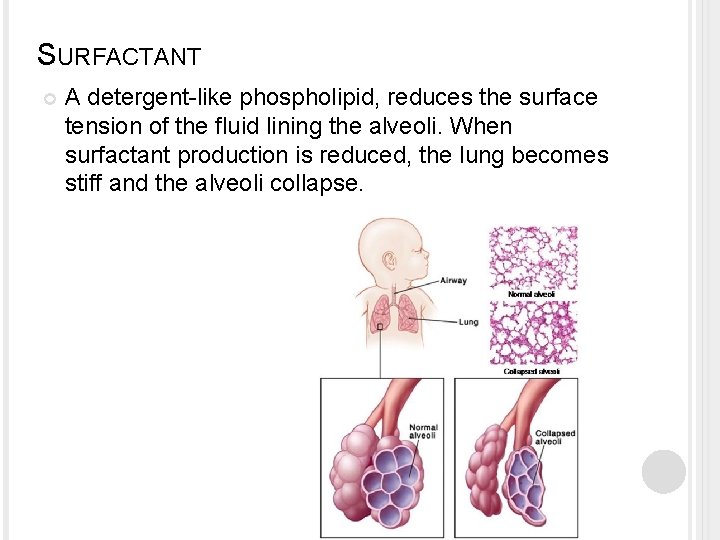
SURFACTANT A detergent-like phospholipid, reduces the surface tension of the fluid lining the alveoli. When surfactant production is reduced, the lung becomes stiff and the alveoli collapse.

SURFACTANT

ALVEOLAR GAS EXCHANGE Diffusion refers to the movement of oxygen and carbon dioxide between the air (in the alveoli) and the blood (in the capillaries). The appropriate gas moves passively from an area of higher pressure or concentration to an area of lesser pressure or concentration.

TRANSPORT OF OXYGEN AND CARBON DIOXIDE Most of O 2 (97%) combines loosely with hemoglobin as oxyhemoglobin. The remaining is dissolved and transported in the fluid of the plasma and cells.

OXYGEN TRANSPORT Several factors affect the rate of oxygen transport from the lungs to the tissues: � Cardiac output Any pathologic condition that decreases cardiac output diminishes the amount of O 2 delivered to the tissues. � Number of erythrocytes and blood hematocrit Excessive reductions in the blood hematocrit, such as occur in anemia, reduce oxygen transport. � Exercise In well trained athletes , oxygen transport can be ↑ up to 20 times the normal rate, due to ↑ C. O. and to ↑ use of O 2 by the cells.

CARDIAC OUTPUT
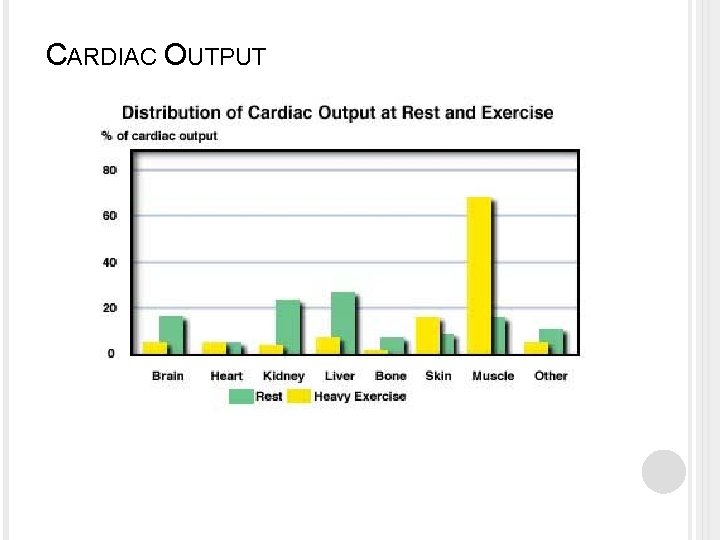
CARDIAC OUTPUT

RESPIRATORY REGULATION Respiratory regulation maintains correct concentration of O 2: CO 2 Chemosensitive center in the medulla oblongata � responsive to ↑in blood CO 2 or hydrogen ion concentration. � Can ↑ the activity of the inspiratory center and the rate and depth of respiration. Neural receptors

FACTORS AFFECTING RESPIRATORY FUNCTION Health status Age Medications Environment Stress

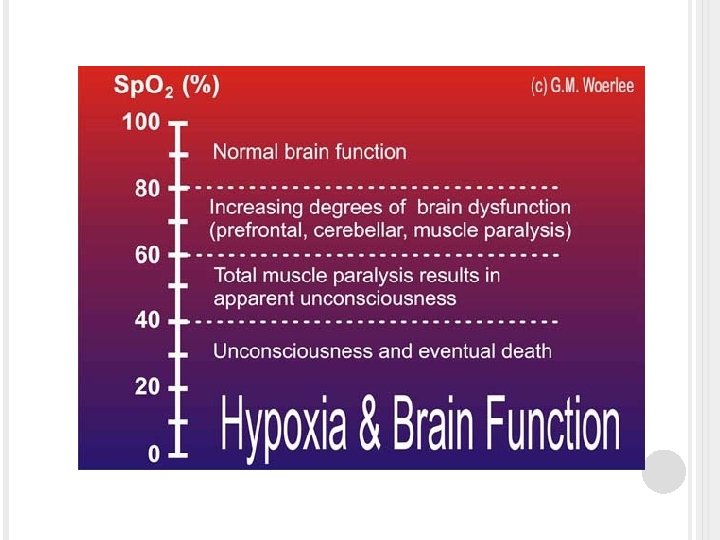
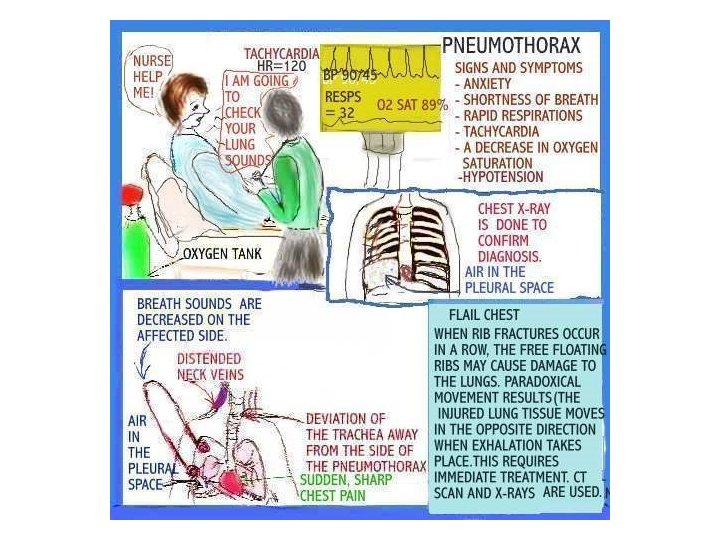
ALTERATIONS IN RESPIRATORY FUNCTION Hypoxia is a condition insufficient oxygen anywhere in the body, from the inspired gas to the tissue. The clinical signs box lists signs of hypoxia. Hypoventilation can lead to hypoxia. � Causes Disease of respiratory muscle Drugs, or anesthesia With hypoventilation CO 2 often accumulates in the blood, a condition called hypercarbia or hypercapnia. Hypoxemia refers to reduced oxygen in the blood and is characterized by low Pa. O 2 or hemoglobin saturation.

HYPOXIA Signs and Symptoms of ACUTE hypoxia: � Person appears anxious � Person assumes sitting position, often leaning forward slightly to permit greater expansion of the thoracic cavity. Signs and Symptoms of CHRONIC hypoxia: � Person appears fatigued and is lethargic � Clubbed fingers and toes With clubbing the base of the nail becomes swollen and the ends of the fingers and toes increase in size, the angle between the nail and the base of the nail increase to more than 180 degrees.
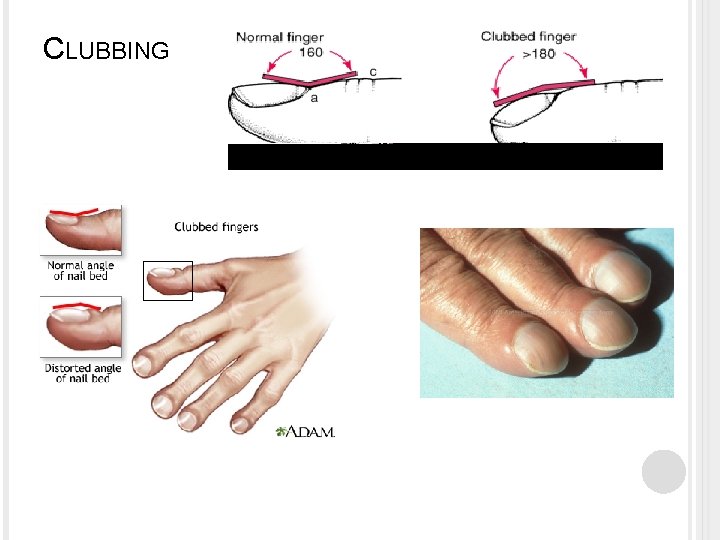
CLUBBING

ALTERED BREATHING PATTERNS Rate, volume, rhythm, relative ease or effort of respiration Eupnea Tachypnea Bradypnea Apnea Hyperventilation Kussmaul’s breathing (video) 1: 15 � https: //www. youtube. com/watch? v=TG 0 vp. Kae 3 Js Cheyne-Stokes respiration (video) 2: 08 � https: //www. youtube. com/watch? v=Vkux. P 7 i. Ch. YY

OBSTRUCTED AIRWAY An upper airway obstruction that is in the nose, pharynx, or larynx � Causes: Foreign body such as food Tongue falls back in unconscious Collection of secretion in the passageways Respirations sound gurgly or bubbly Lower airway obstruction involves partial or complete occlusion the passage in the bronchi and lungs � Causes: Accumulation of mucus or inflammatory exudate Malignancy Foreign Body

NURSING MANAGEMENT Health History � Current and past respiratory problems � Lifestyle � Cough? � Sputum or pain? � Meds � Risk factors for impaired O 2 status Physical Exam � Inspection � Palpation � Percussion � Auscultation

PHYSICAL EXAM The nurse use 4 physical examination techniques: � Inspection, palpation, percussion, and auscultation. Observes: � the rate, depth, rhythm, and quality of respirations, noting the position the client assumes for breathing. Inspects: � Also inspects for variations in the shape of the thorax that may indicate adaptation to chronic respiratory conditions. e. g. , client with emphysema frequently develop a barrel chest.
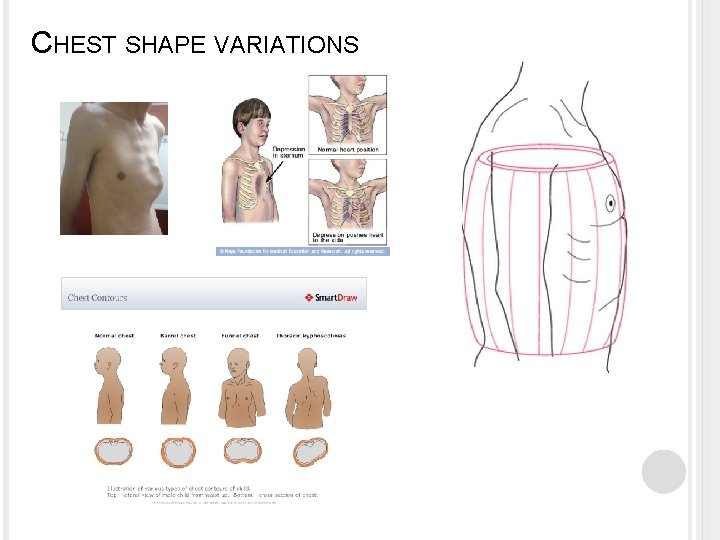
CHEST SHAPE VARIATIONS
AVERAGE RESPIRATORY RATES: *INFANTS: ABOUT 30 BREATHS PER MINUTE *PRESCHOOLER: AROUND 25 BREATHS PER MINUTE *ADOLESCENTS &ADULTS: 12 - 18 BREATHS PER MINUTE
HYPOXEMIA VS. HYPOXIA Hypoxemia = low levels of oxygen in blood Can cause: Hypoxia = low levels of oxygen in body tissues

SYMPTOMS OF HYPOXIA Although they can vary from person to person, the most common hypoxia symptoms are: Changes in the color of your skin, ranging from blue to cherry red Confusion Cough Fast heart rate Rapid breathing Shortness of breath Sweating Wheezing
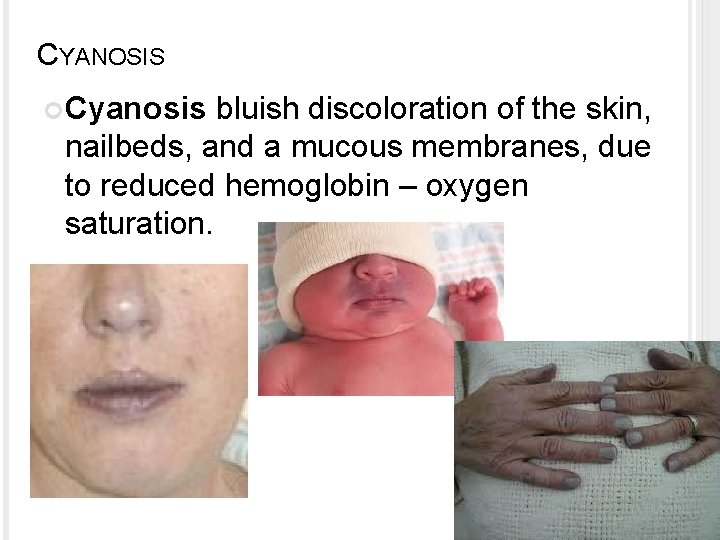
CYANOSIS Cyanosis bluish discoloration of the skin, nailbeds, and a mucous membranes, due to reduced hemoglobin – oxygen saturation.

IMPAIRED OXYGENATION Can be life-threatening ü Mild to severe ü Diseases, injuries ü Frightening, frustrating ü
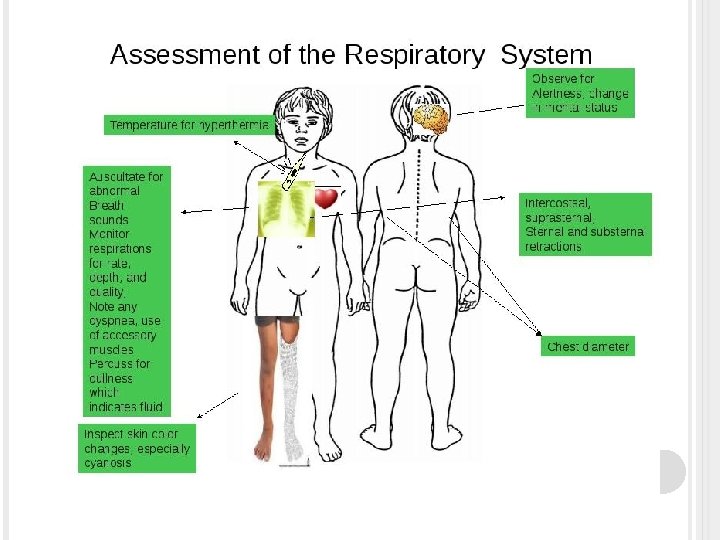
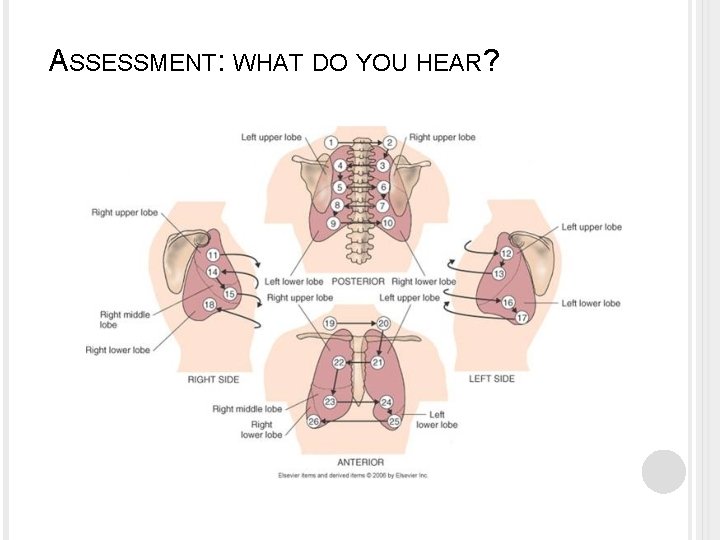
ASSESSMENT: WHAT DO YOU HEAR?
NORMAL BREATH SOUNDS Normal breath sounds are the inspiratory and expiratory sounds heard through the chest wall of a healthy individual http: //www. easyauscultation. com/cases? coursecaseorder=1&coursei d=201
AIRWAY PATENCY Nursing priority with: � Patient status changes � Facial/dental surgery � Upper respiratory tract obstruction � Emergency Situations
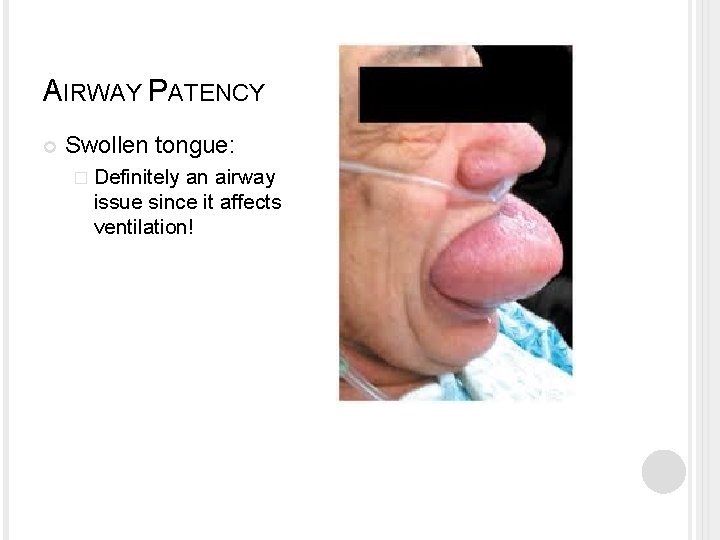
AIRWAY PATENCY Swollen tongue: � Definitely an airway issue since it affects ventilation!
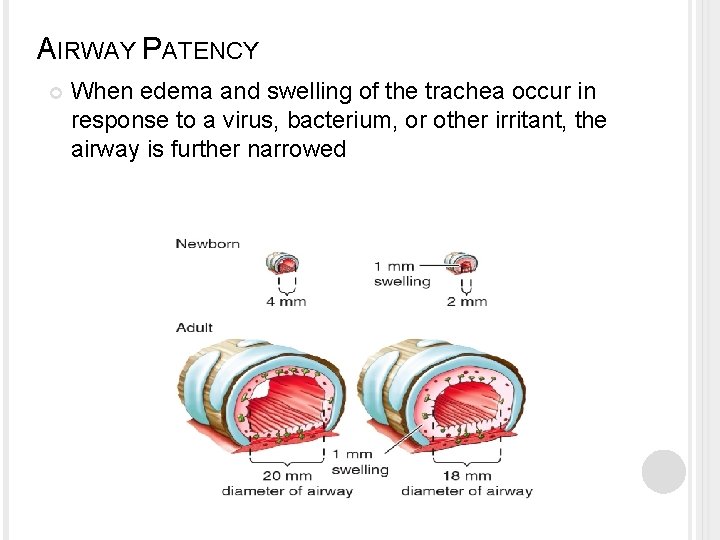
AIRWAY PATENCY When edema and swelling of the trachea occur in response to a virus, bacterium, or other irritant, the airway is further narrowed
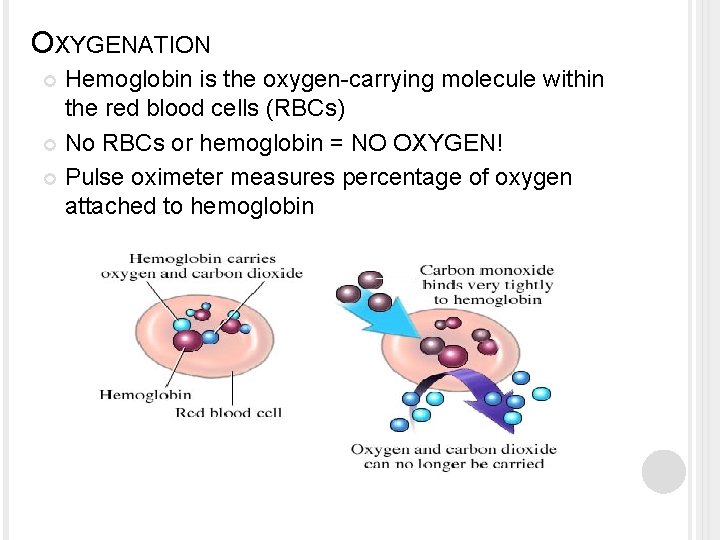
OXYGENATION Hemoglobin is the oxygen-carrying molecule within the red blood cells (RBCs) No RBCs or hemoglobin = NO OXYGEN! Pulse oximeter measures percentage of oxygen attached to hemoglobin

OXYGEN SATURATION Pulse oximeter is used to measure the percentage of oxygen attached to hemoglobin Part of normal vital signs

NURSING REMINDERS When assessing a patient, determine if the patient is: � Short of breath and/or in respiratory distress � Just finishing physical activity or exertion � Wearing the pulse ox properly and it is turned on � Comfortable only when in tripod position?
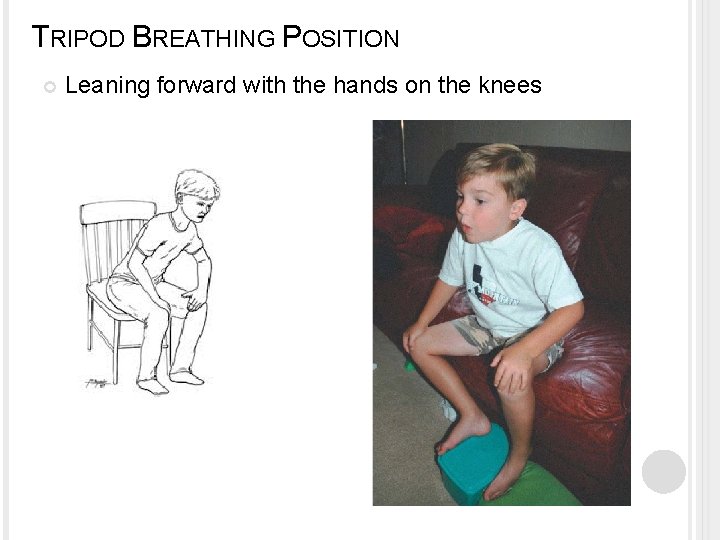
TRIPOD BREATHING POSITION Leaning forward with the hands on the knees

TEST YOURSELF! What is the first thing you do when someone has difficulty breathing? 1. Have them raise their feet 2. Sit them up in a high upright position 3. Give them water to drink 4. Take their blood pressure

QUESTIONS?
- Slides: 41