Hemodynamic disturbance DR USHA M HEMODYNAMICS n Literally

Hemodynamic disturbance DR. USHA. M

HEMODYNAMICS n Literally means “Blood movement” is the study of blood flow.

Hemodynamic disturbance 1. 2. 3. 4. 5. 6. Edema Hyperemia & congestion Hemorrhage Thrombosis Infarction Shock

Edema Normal body water distribution: Two compartments: 1. Intracellular – comprising of two- thirds of total body fluid. 2. Extracellular – comprising of one- third of total body fluid. 1. Interstitial compartment- 75% 2. Intra vascular compartment – 25%

Normal fluid exchange n There are two ends for a capillary 1. Arteriolar end 2. Venous end The pressure is high in the arteriolar end then the venous end. Normally the fluid moves out from the vessel in arteriolar end into interstitial tissue. From interstitial tissue same fluid moves back into vessel at venous end. The small amount of fluid which is left in interstitial space is cleared by lymphatics.

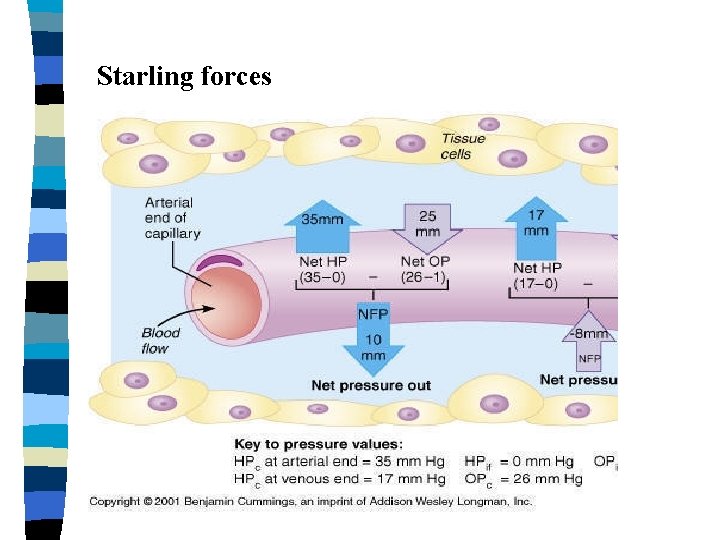
Starling forces


Normal fluid pressures 1. Osmotic pressure Is exerted by the chemical constituents of the body fluids Eg. Electrolytes – crystalloid osmotic pressure proteins (albumin)- oncotic osmotic pressure. 2. Hydrostatic pressure Pressure within the blood vessel.

Edema n Is accumulation of excessive fluid in the interstitial spaces.

Classification of edema according to distribution of fluid Localized edema involving one organ or part of the body. eg-pleural effusion, ascitis, pericardial effusion , etc. 2. Generalized edema Involving the entire body- ANSARCA 1.

Pathogenesis of edema: 1. 2. 3. 4. 5. Increased hydrostatic pressure Increased permeability of the vessel wall Decreased oncotic pressure Sodium retention in the kidneys Obstruction of lymph flow

1. Hydrostatic edema n Results from increased intra vascular pressure (hydrostatic pressure).

Causes : Impaired venous return congestive cardiac failure constrictive pericarditis, ascitis (liver disease) 2. Venous obstruction thrombi, tumor 3. Arteriolar dilatation heat, inflammation 1.

2. Increased vascular permeability n Commonest cause is inflammation. Release of inflammatory mediators like histamine, bradykinin, PAF & others leads to increased permeability. n Other causes: Injury,

3. Decreased plasma oncotic pressure 1. Decresed synthesis in the liver – end stage liver disease. 2. Incresed loss in urine(nephrotic syndrome) or stool (protein losing enteropathy) 3. Inadequte intake-kwashiokar


Lymphatic obstruction n Elephantiasis n Edema of the arm following surgical resection of axillary lymph nodes n Edema of hand following post irradiation fibrosis.
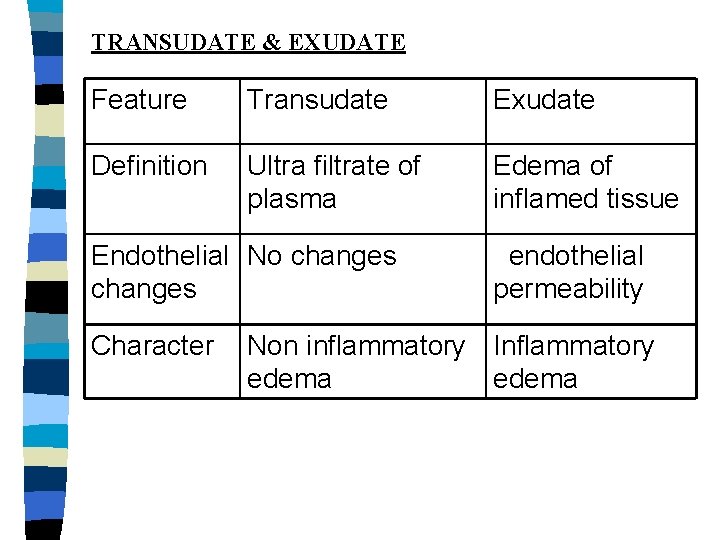
TRANSUDATE & EXUDATE Feature Transudate Exudate Definition Ultra filtrate of plasma Edema of inflamed tissue Endothelial No changes Character endothelial permeability Non inflammatory Inflammatory edema
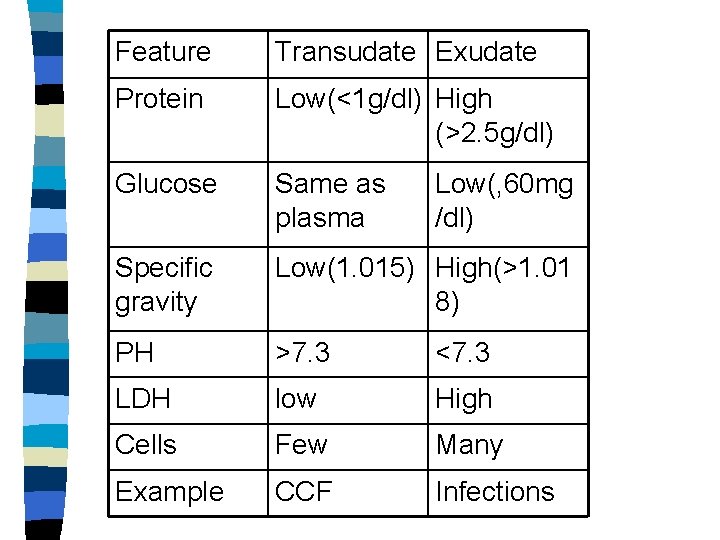
Feature Transudate Exudate Protein Low(<1 g/dl) High (>2. 5 g/dl) Glucose Same as plasma Specific gravity Low(1. 015) High(>1. 01 8) PH >7. 3 <7. 3 LDH low High Cells Few Many Example CCF Infections Low(, 60 mg /dl)


Renal edema Causes: 1. Nephorotic syndrome 2. Glomerulonephritis 3. Acute tubular injury
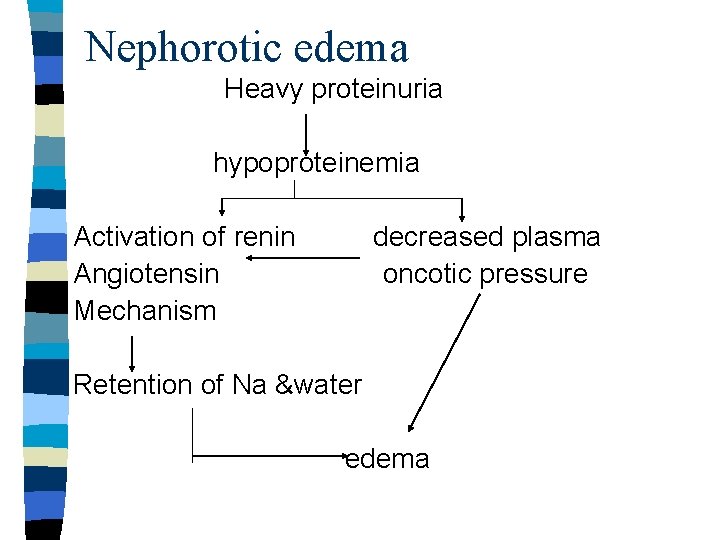
Nephorotic edema Heavy proteinuria hypoproteinemia Activation of renin Angiotensin Mechanism decreased plasma oncotic pressure Retention of Na &water edema

Nephritic edema Glomerulonephritis glomerular lesion I decreased filtration followed by increased absoption of Na & water by tubules Na & water retention edema

Acute tubular injury Toxins , drugs ATN Fails to excrete Na & water edema
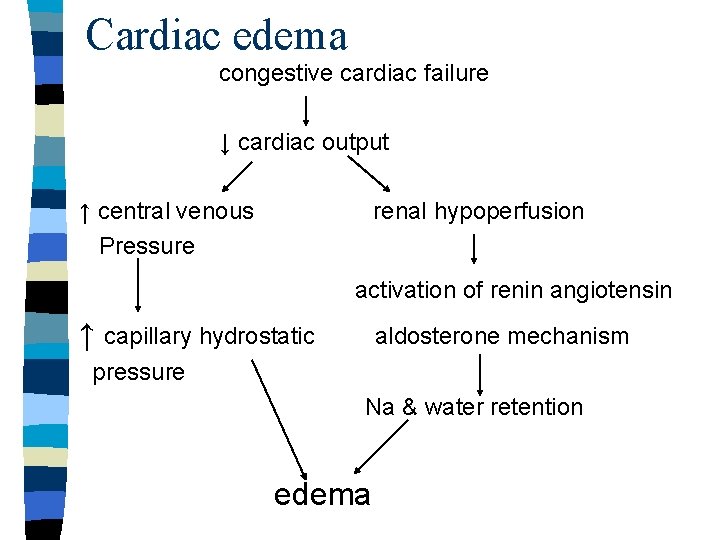
Cardiac edema congestive cardiac failure ↓ cardiac output ↑ central venous Pressure renal hypoperfusion activation of renin angiotensin ↑ capillary hydrostatic aldosterone mechanism pressure Na & water retention edema

Pulmonary edema causes : 1. Left heart failure 2. ARDS 3. Shock 4. Infections - pneumonia

left ventricular failure ↑ hydroastatic pressure ↑ pressure in pulmonary veins ↑ pressure in pulmonary capillaries interstitial edema pressure on alveolar wall &breaks alveolar linning alveolar edema

Hepatic Oedema hepatic pathology (e. g. cirrhosis) ↓ obstruction of portal venous system ↓ increased hydrostatic pressure & ↓albumin synthesis d. t. hepatocyte damge ↓ hypoproteinaemia ↓ transudate oedema (ascitis).
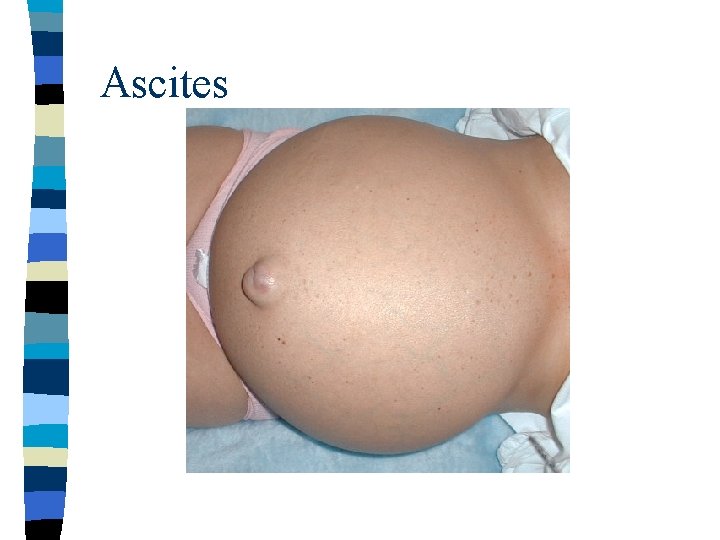
Ascites

Cerebral edema Causes: 1. Infection - encephalitis, meningitis 2. Brain infarct, hemorrhage 3. Trauma 4. Tumors

Localised Oedema: n acute inflammatory oedema - ↑ vascular permeability exudate - ↑ hydrostatic pressure of capillaries hyperaemia - ↑ osmotic pressure of interstitial fluid - ↑ fluidity of ground substance n allergic (hypersensitivity) oedema - histamine release ↑ vascular permeability exudate (e. g. allergic rhinitis)

Pitting & non pitting edema is clinical terms for subcutaneous edema of leg.

Pitting Oedema
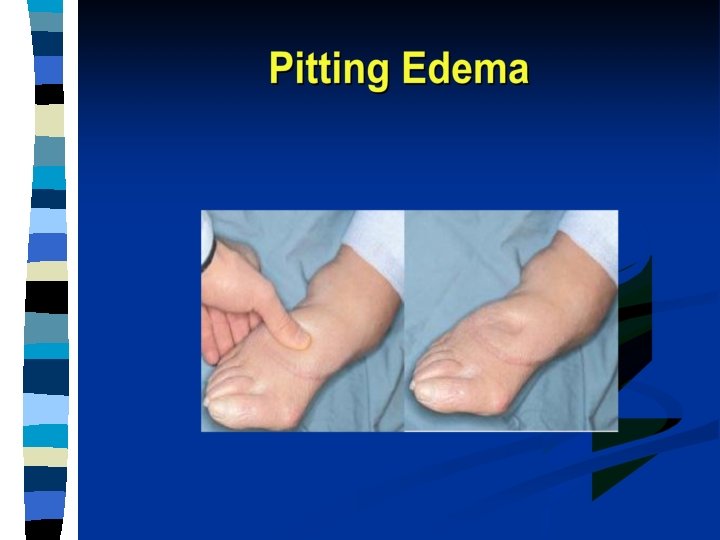


Clinical Features of Oedema n n n n Considerable quantities must accumulate before clinically apparent (oedema can be assessed by weighing the patient approx. 5 litres) Generalised Cardiac Oedema - gravitational distribution - pitting oedema holds depression for a few minutes Renal Oedema - fluid retention - generally distributed in C. T. puffy face/eyelids Serous Cavities - e. g. hydrothorax/ascites Brain Oedema - swollen; narrow sulci & flattened gyri Pulmonary Oedema - exudate - prone to infection e. g. bronchopneumonia - rales


Hemorrhage n Indicates extravasation of blood due to rupture of vessel.
Classification based on origin 1. Cardiac- penetrating wound rupture of ventricles in MI 2. Arterial – trauma rupture of aneurysm 3. Capillary – trauma, surgery 4. Venous – trauma, surgery

Petechiae, Pupura, Ecchymoses n Refers to the hemorrhage into the skin & mucosae. Petechiae- pinpoint hemorrhage ( < 1 mm) Purpura- 1 mm- 1 cm in diameter Echymoses- >1 cm

Petechiae

Purpura
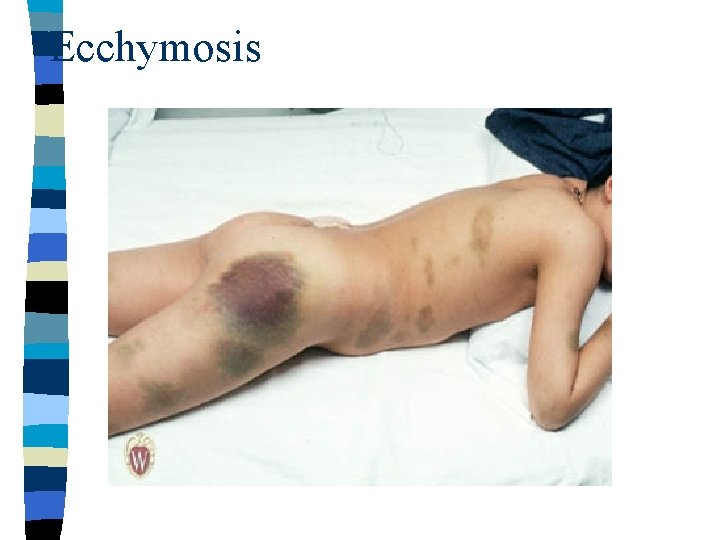
Ecchymosis

Hematoma n Is grossly visible accumulation of extravasted blood in tissue. n First it is red, then as the blood is deoxygenated it becomes dusky & bluish red.
Body cavity hemorrhage Hemothorax – accumulation of blood in pleural cavity Hemopericardium – in pericardial cavity Hemoperitonium – in peritonial cavity Hemoarthrosis – in intra – articular space Hematocephalus – in ventricles of brain
Hematuria Is appearance of blood in urine. 1. Microscopic – detectable by microscopic examination of urine. 2. Macroscopic – visible to naked eye n Hematuria signifies disease of kidney or urinary tract

Hematemesis n Is vomiting of blood. n Sign of esophageal & gastric hemorrhage like rupture of esophageal varices & peptic ulcer bleeding.

Hematochezia n Bleeding through rectem. n Sign of diseases in large intestine.

Melena n Black colored blood in stools. n Indicates bleeding in upper GIT. n Blood is partialy digested by HCLof gastric juice & transformed into a black pigment called hematein. This pigmentis not digested in the intestines & is passed in the feces.

Epistaxis & Hemoptysis n Epistaxis is bleeding from the nose. n Hemoptysis is bleeding from lungs.

Menorrhagia & Metrorrahagia n Menorrhagia is heavy menstrual bleeding. n Metrorrhagia occurs at any time & is not related to menstrual cycle.

Effects of Hemorrhage n Site of hemorrhage – brain, pericardium, pleural spac n Rate of blood loss – acute • loss of > 20% of blood volume may cause hypotension or hypovolemic shock • hemoglobin concentration not altered – non-acute • volume loss compensated by shift of fluid from extravascular to intravascular compartment • hemoglobin concentration decreased

HYPEREMIA & CONGESTION n Is increase in volume of blood in a particular tissue. n Hyperemia is an “active process” , the increased blood influx results from arteriolar dilatation. n Congestion, also known as “passive hyperemia”, results due to stagnation of blood because of venous obstruction.
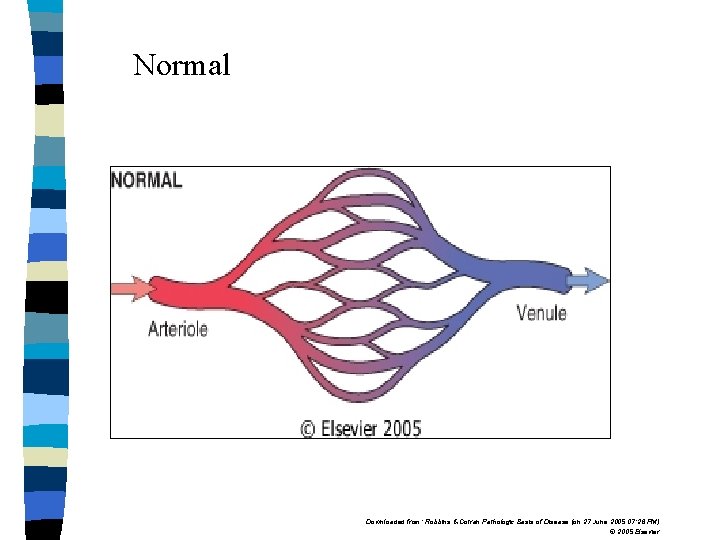
Normal Downloaded from: Robbins & Cotran Pathologic Basis of Disease (on 27 June 2005 07: 26 PM) © 2005 Elsevier
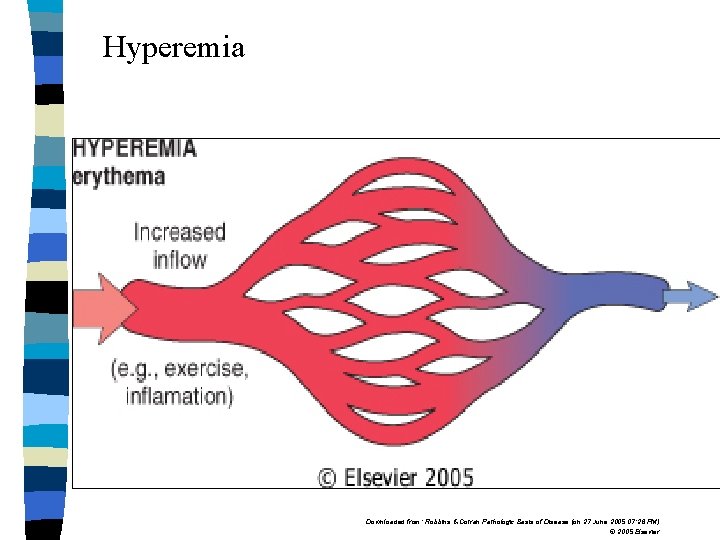
Hyperemia Downloaded from: Robbins & Cotran Pathologic Basis of Disease (on 27 June 2005 07: 26 PM) © 2005 Elsevier
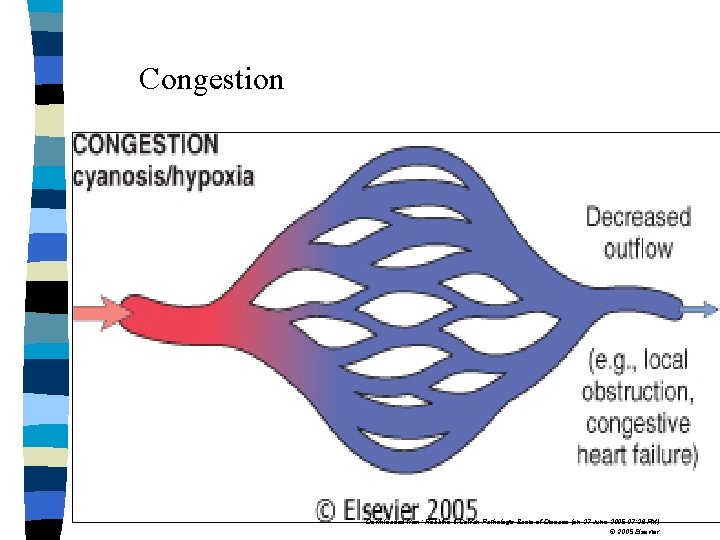
Congestion Downloaded from: Robbins & Cotran Pathologic Basis of Disease (on 27 June 2005 07: 26 PM) © 2005 Elsevier

Examples: Hyperemia: 1. Inflammation 2. Blushing – adrenergic stimulation 3. Exercise – incresed blood flow to the muscle. Congestion: Obstruction of veins due to thrombi or backward pressure due to heart failure.

Color of hyperemic & congested tissue: n Hyperemic tissue contains increased amounts of oxygenated blood & therefore the tissue appears bright red. n Congested tissue contains increased amounts of deoxygenated blood & appears blue. n Hyperemic tissue is warm, while congested blood is cold & clammy.

Chronic venous congestion (CVC): n In CVC there is long standing there is accumulation of deoxygenated blood & hence there is damage to the tissue.
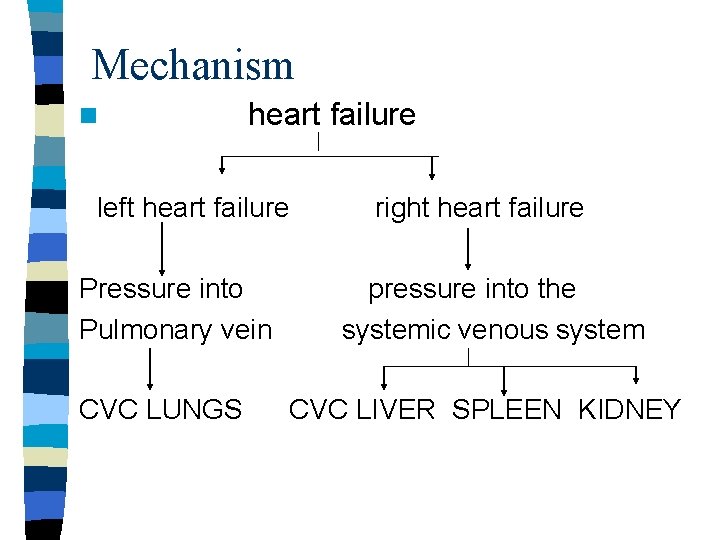
Mechanism n heart failure left heart failure Pressure into Pulmonary vein CVC LUNGS right heart failure pressure into the systemic venous system CVC LIVER SPLEEN KIDNEY

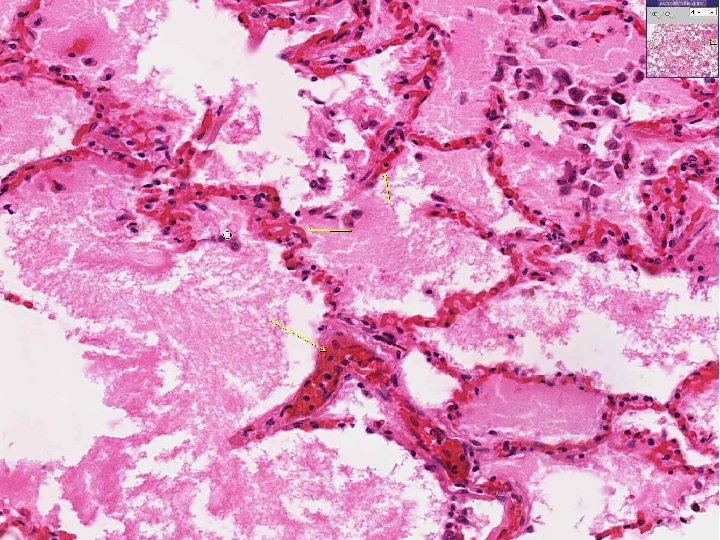
CVC Lung Causes: Left heart failure Gross : The lungs are heavy. Lungs appear brown - BROWN INDURATION OF LUNGS.

CVC Lungs Micro: Rupture of congested vessel results in edema & hemorrhage. Lysis of RBC’s releases hemosiderin pigment which is taken up by macrophages – HEART FAILURE CELLS.

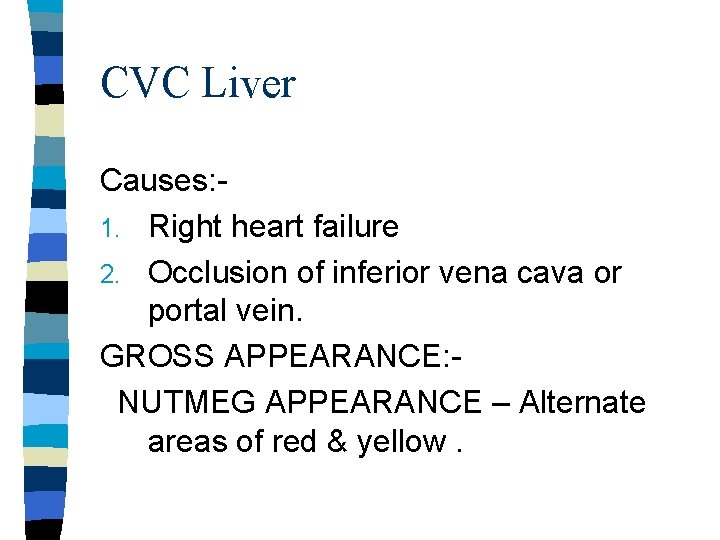
CVC Liver Causes: 1. Right heart failure 2. Occlusion of inferior vena cava or portal vein. GROSS APPEARANCE: NUTMEG APPEARANCE – Alternate areas of red & yellow.

CVC Liver Micro: - Periportal zone midzonal Centrilobular

CVC Liver (MICRO) Blood fills up the central vein & sinusoids around it. Followed by centrilobular hepatocytes necrosis. n In the long standing cases the necrotic area is replaced by fibrous tissue. n The areas with blood appears red & areas with fibrosis appears whitish yellow- NUTMEG APPEARANCE.


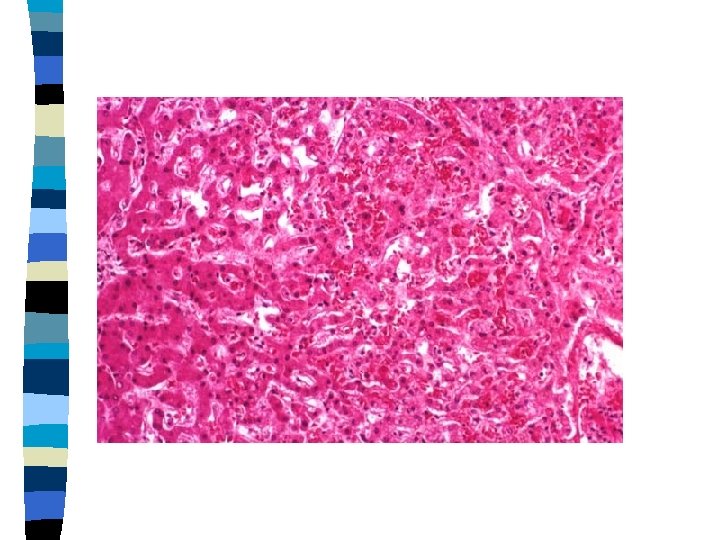

CVC Spleen Causes: 1. Right heart failure 2. Portal hypertension GROSS: Spleen is enlarged & congested.

CVC Spleen (micro) Red pulp appears congested. GAMMA GANDY BODIES OR SIDEROFIBROTIC NODULES: Deposits of hemosiderin & calcium salts on fibrous tissue.
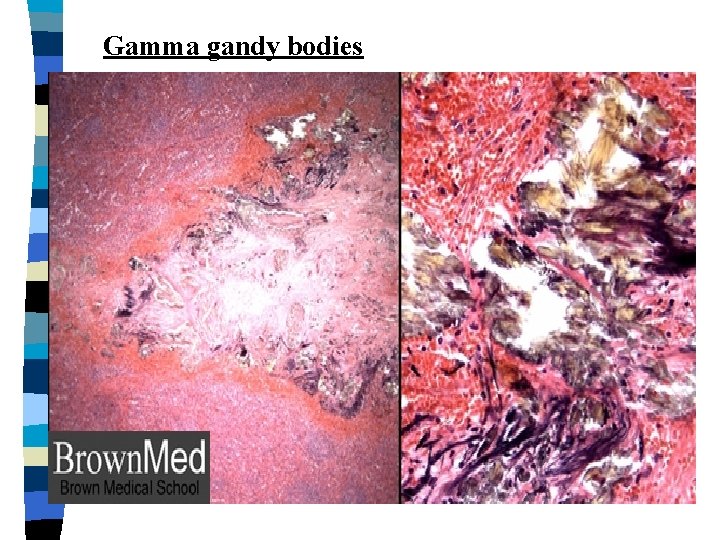
Gamma gandy bodies
CVC Kidney Cause: 1. Right heart failure 2. Obstruction of renal vein Gross: Kidney is congested.

CVC Kidney (micro) n Glomeruli – shows mesangial proliferation. n Tubules – shows degenerative changes (cloudy swelling).

- Slides: 77