ACUTE RESPIRATORY DISTRESS SYNDROME ARDS Oea Khairsyaf Acute

















- Slides: 23

ACUTE RESPIRATORY DISTRESS SYNDROME ( ARDS ) Oea Khairsyaf

Acute Respiratory Distress Syndrome Defenisi • “Non-cardiogenic Pulmonary Oedema” – Ashbaugh, Bigelow et al, 1967 • “Adult Respiratory Distress Syndrome” – Petty and Ashbaugh, 1971 • “Shock Lung” – Staub, 1974 • “Acute Respiratory Distress Syndrome” – American-European Consensus Committee, 1992

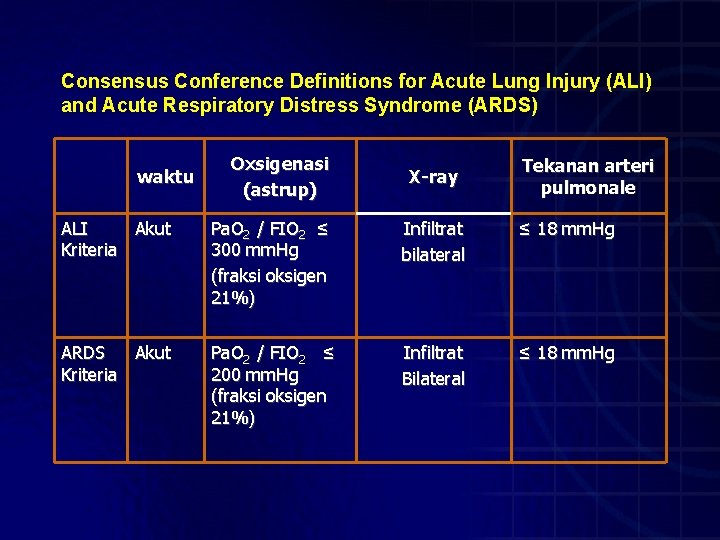
Consensus Conference Definitions for Acute Lung Injury (ALI) and Acute Respiratory Distress Syndrome (ARDS) waktu Oxsigenasi (astrup) X-ray Tekanan arteri pulmonale ALI Akut Kriteria Pa. O 2 / FIO 2 ≤ 300 mm. Hg (fraksi oksigen 21%) Infiltrat bilateral ≤ 18 mm. Hg ARDS Akut Kriteria Pa. O 2 / FIO 2 ≤ 200 mm. Hg (fraksi oksigen 21%) Infiltrat Bilateral ≤ 18 mm. Hg

ETIOLOGI ARDS SECARA LANGSUNG • • Asma bronkial PPOK Pneumonia Aspirasi makanan Pulmonary contusion Near-drowning Inhalational injury DLL TIDAK LANGSUNG • Sepsis • Severe trauma with shock • Drug overdose • Acute pancreatitis • Transfusion of blood products

Acute Respiratory Distress Syndrome Gambaran klinis: § Awal “shock” responsif terhadap resusitasi. § Periode latent : beberapa jam, biasanya beberapa hari (12 -48 jam). § Insidious tachypnoea, pasien jadi gelisah. § Paru tidal volume kecil, napas cepat, hipoksemia refrakter. § Mula-mula alkalosis respiratorik asidosis respiratorik § Ventilasi mekanis

Patogenesis 3 fase dari lung injury: 1. Fase exudatif ( edema and perdarahan ) 2. Fase inflammatory and repair 3. Fase fibrotic

Acute Respiratory Distress Syndrome Exudative Phase, 0 -5 hari. § Ruang alveoli terisi cairan, protein dan inflammatory cells. § Necrosis sel-sel pneumocyte type 1, fibrin, platelet thrombi. Inflammatory Phase, 5 -10 hari. § Proliferasi fibroblasts dan sel-sel pneumocyte type 2. § Squamous metaplasia dan pembentukan hyaline membranes. Fibroproliferative Phase, 10 hari sampai sembuh atau mati. § § § Fibrosis interstital dan intra-alveolar. Thrombosis dan obliterasi vaskuler. Collagen paru meningkat.

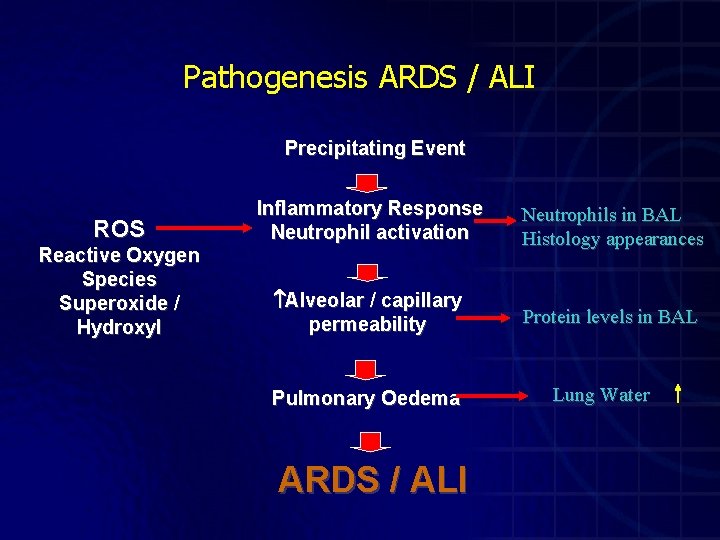
Pathogenesis ARDS / ALI Precipitating Event ROS Reactive Oxygen Species Superoxide / Hydroxyl Inflammatory Response Neutrophil activation Neutrophils in BAL Histology appearances Alveolar / capillary permeability Protein levels in BAL Pulmonary Oedema ARDS / ALI Lung Water

Patogenesis ARDS / ALI REDOX Balance Generation of Oxidant species ROS H 2 O 2 Superoxide (O 2. -) Hydroxyl radical (OH-) RNS Nitric oxide (NO) Peroxynitrite (ONOO-) Antioxidant Protection Normal Superoxide dismutase Catalase Glutathione Transferrin Ceruloplasmin Vit E Vit C Beta-carotene

Patogenesis ARDS / ALI Oxidative Stress Depletion of antioxidants ROS formation & Oxidative damage

The Pathogenesis of ARDS / ALI Predisposition? Inflammatory mediators signalling Precipitating Event Inflammatory Response (Respiratory Burst) ROS RNS Molecular Damage and Dysfunction Inflammatory mediators Alveolar / capillary permeability Pulmonary Oedema ARDS/ALI Ventilatory support Inhaled NO

Faktor-faktos seluler dan humoral pada ALI/ARDS • Neutrophils. – – ROS dan proteases. Resting, activated, primed and unresponsive. – – – TNF- , macrophages, monocytes, neutrophils. IL-1 , macrophages, endothelial cells GM-CSF, monocytes, macrophages, fibroblasts epithelial, endothelial dan smooth muscle cells. • Cytokines (polypeptides). • Chemokines (chemotactic cytokines). – IL-8. • Eicosanoids (prostaglandin, leucotrienes, thromboxanes), complement, endotoxins, adhesion molecules, PAF, endothelins, NO.

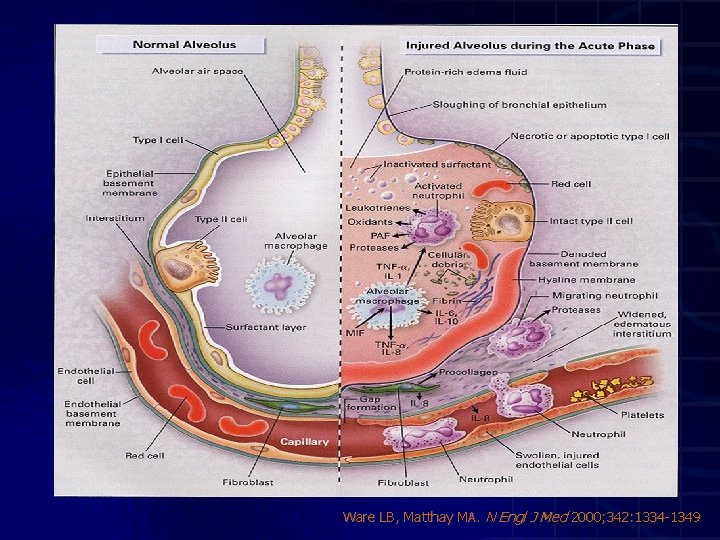
Pathogenesis • Influx cairan edema kaya protein alveoli (permeabilitas alveolar-capillary barrier ) • Kerusakan Type 2 cells gangguan epithelial fluid transport gangguan pengeluaran cairan dan produksi surfactant abnormal • Bila kerusakan hebat gangguan epithelial repair fibrosis • Neutrophils merupakan sel yang dominant • Cytokines dan proinflammatory compounds mengawali dan memperkuat respons inflammatory

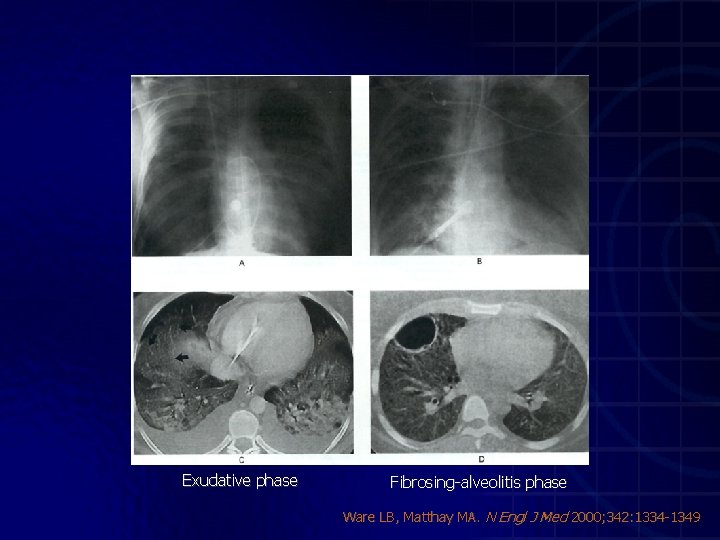
Ware LB, Matthay MA. N Engl J Med 2000; 342: 1334 -1349

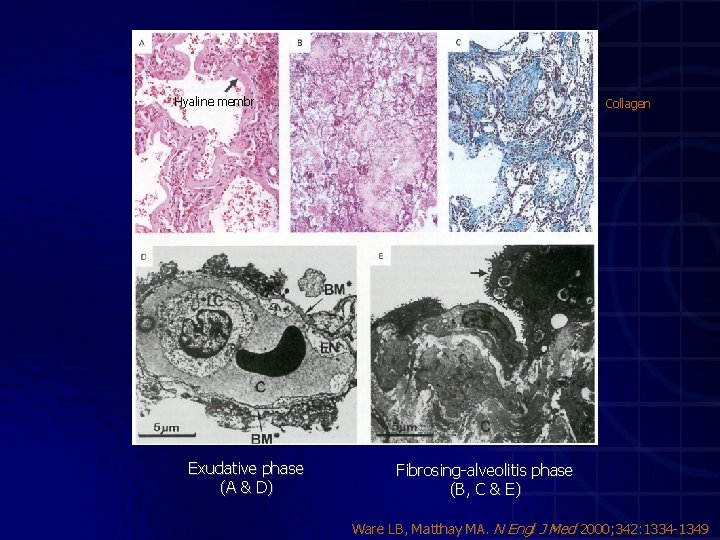
Hyaline membr Exudative phase (A & D) Collagen Fibrosing-alveolitis phase (B, C & E) Ware LB, Matthay MA. N Engl J Med 2000; 342: 1334 -1349

Exudative phase Fibrosing-alveolitis phase Ware LB, Matthay MA. N Engl J Med 2000; 342: 1334 -1349

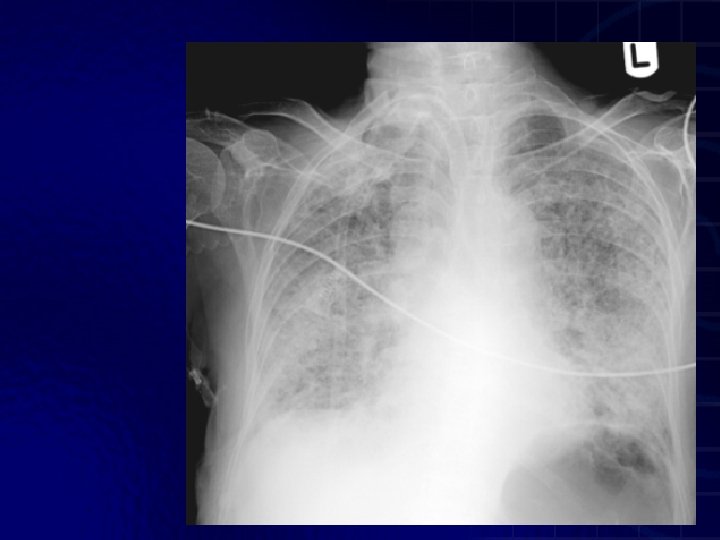
ARDS

PENATALAKSANAAN § Obati penyakit dasar § Antibiotika § Kortikosteroid § oksigenasi § Anti oksidan

Keluaran (outcome) • Tahun 1967 - 1979 – Asbaugh (1967) : survival 42% – Survival : 18 – 38% • Tahun 1980 - 1989 – Survival (< 1985) : 32 – 36% – Survival (> 1985) : 41 - 52% (European Collaborative Study 41%) • Tahun 1990 – 2000 – Survival : 41 – 60% – NIH ARDS study : mortality 40% vs 30% (penurunan 25%, antara VT 12 m. L/kg vs 6 m. L/kg)

Outcome Jangka Panjang pada Survivors (1 -1, 5 tahun pasca ARDS) Sequelae pulmoner Majoritas, fungsi paru kembali hampir normal Gangguan residual: • • • restrictive ventilatory defect (biasanya ringan), Hipertensi pulmoner (ringan), airflow limitation ( bronchial hyperactivity) Gangguan pada exercise testing lebih bermakna (setara pasien COPD berat) Derajat gangguan ~ umur, riwayat merokok, ventlasi mekanis berkepanjangan

Survival • 10 tahun terakhir, mortalitas turun 20% • Mortalitas: – Umur : 75% (≥ 60 th) vs 37% (< 60 th) – Faktor resiko : 64% (sepsis) vs 42% (trauma) – Penyulit : 86% (sepsis) vs 38% (tanpa sepsis) – Response thd PEEP : Pa. O 2/Fi. O 2 > 150 mm. Hg mortalitas 23%

TERIMA KASIH
