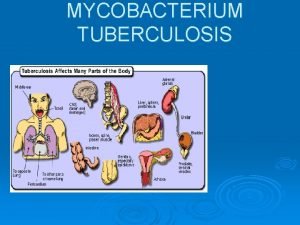
TUBERCULOSIS Diagnosis treatment Dr Fazli Wahab FCPSMed FCPSPulmonology


TUBERCULOSIS Diagnosis & treatment Dr. Fazli Wahab FCPS(Med), FCPS(Pulmonology) Assisstant Prof Peshawar Medical College

Diagnostic Tools �Microscopy ◦ AFB smear ◦ Histology �AFB Culture �Radiology �Tuberculin test skin �Serological Tests
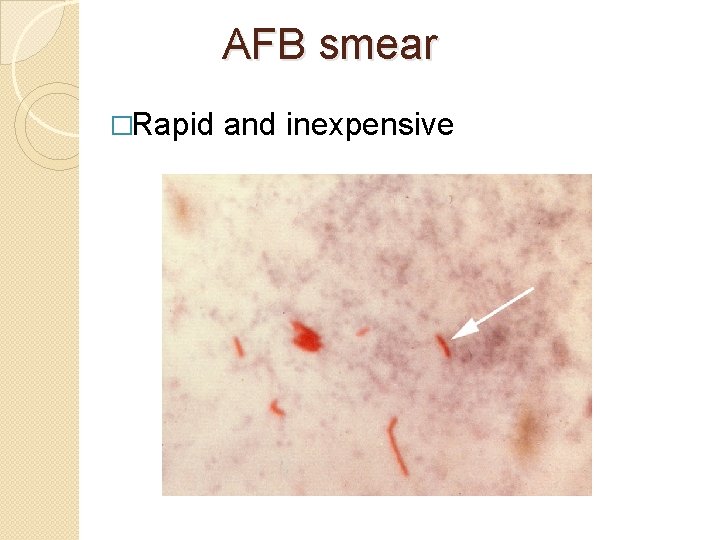
AFB smear �Rapid and inexpensive
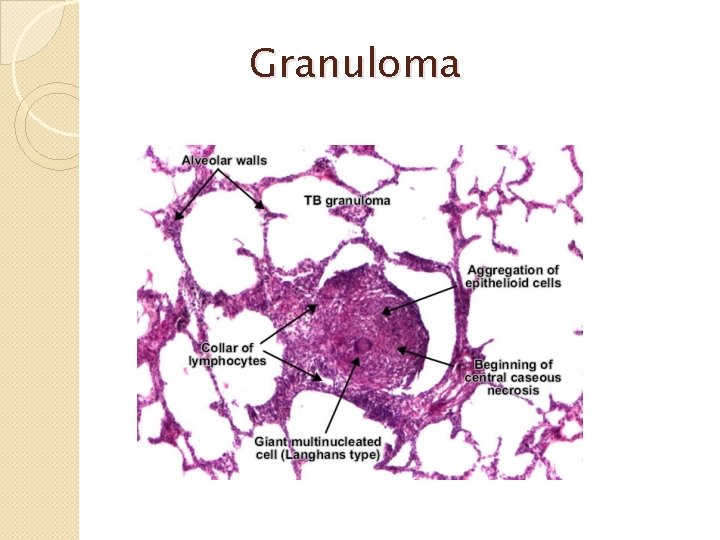
Granuloma
Mycobacterial Culture �Definitive �Growth diagnosis detected after 4– 8 weeks.

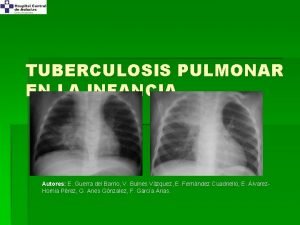
Radiographic Procedures �The "classic" picture is that of upperlobe disease with infiltrates and cavities,

X-ray chest appearance can be any of the following üInfiltration üCavitations üFibrosis with traction üEnlargement of hilar and mediastinal lymph node ü Pleural effusion/empyema üNodular/ Miliary shadows




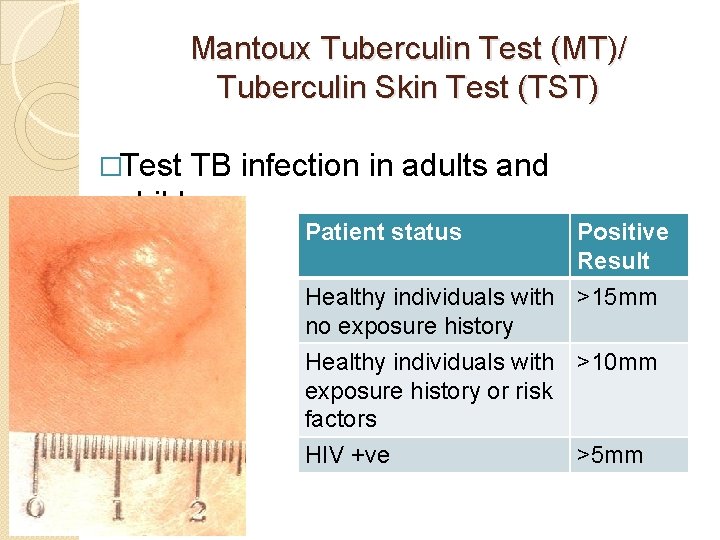
Mantoux Tuberculin Test (MT)/ Tuberculin Skin Test (TST) �Test TB infection in adults and children Patient status Positive Result Healthy individuals with >15 mm no exposure history Healthy individuals with >10 mm exposure history or risk factors HIV +ve >5 mm

Serological Tests �Not routinely used �Polymerase �Interferon (IGRS) �Enzyme assays: ◦ ◦ Chain Reaction (PCR) Gamma release assays Assays & Chromatographic Unreliable & Ineffective methods No role in diagnosis in any form of TB Mycodot assay ICT TB

Treatment

�Two aims ◦ Interrupt transmission ◦ Prevent morbidity and death.

Anti-tuberculosis Drugs 1 ST LINE DRUGS: • Isoniazid (H) • Rifampicin (R) • Pyrazinamide (Z) • Ethambutol (E) • Streptomycin (S)
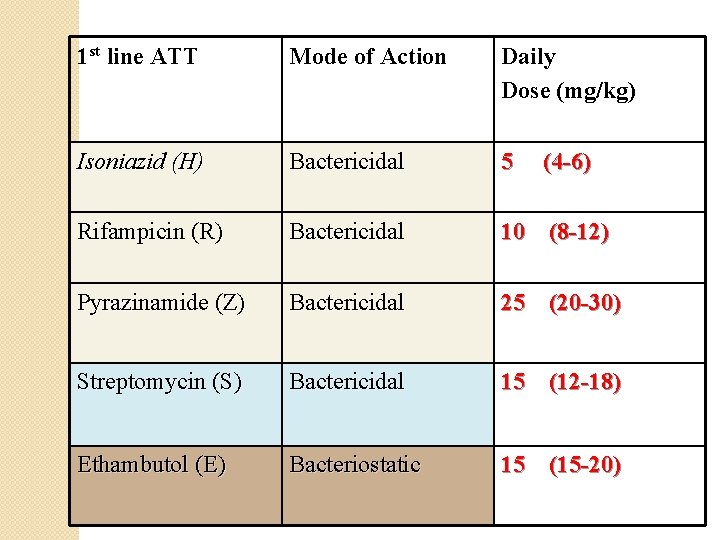
1 st line ATT Mode of Action Daily Dose (mg/kg) Isoniazid (H) Bactericidal 5 Rifampicin (R) Bactericidal 10 (8 -12) Pyrazinamide (Z) Bactericidal 25 (20 -30) Streptomycin (S) Bactericidal 15 (12 -18) Ethambutol (E) Bacteriostatic 15 (15 -20) (4 -6)

Regimens Standard short course regimens 6 -8 months. �An initial, intensive or bactericidal, phase and �A continuation, or sterilizing, phase.

DOTS � DOTS (directly observed treatment, short-course), the WHO-recommended TB control strategy.
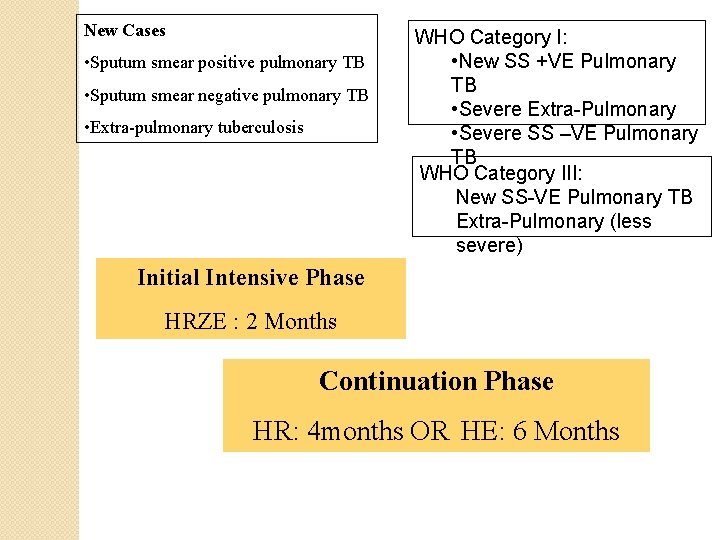
New Cases • Sputum smear positive pulmonary TB • Sputum smear negative pulmonary TB • Extra-pulmonary tuberculosis WHO Category I: • New SS +VE Pulmonary TB • Severe Extra-Pulmonary • Severe SS –VE Pulmonary TB WHO Category III: New SS-VE Pulmonary TB Extra-Pulmonary (less severe) Initial Intensive Phase HRZE : 2 Months Continuation Phase HR: 4 months OR HE: 6 Months

RE-TREATMENT CASES/ WHOCategory II: • Relapse • Treatment Failures • Smear positive patients who have taken ATT for more than one month and defaulted INITIAL INTENSIVE PHASE (3 months) HRZES: 2 MONTHS Then HRZE: 1 Month CONTINUATION PHASE HRE: 5 Months

No Treatment is better than Poor Treatment � Drug-resistant TB is caused by: ◦ Inconsistent or partial treatment, when patients do not take all their medicines regularly for the required period. ◦ Doctors and health workers prescribe the wrong treatment regimens, or because ◦ The drug supply is unreliable.

�The ultimate result is the multidrugresistant TB (MDR-TB) or extensively-drug resistant TB (XDR-TB) �In MDR-TB the Mycobacterium Tuberculosis is resistant to Rifampacin and INH with or without resistance to other 1 st ATT. �Treatment is difficult and expensive.

Prevention �The best way to prevent tuberculosis is to Treat. �Additional strategies include ◦ BCG vaccination and ◦ Treatment of persons with latent tuberculosis infection who are at high risk of developing active disease.

ATT in Special situations �Pregnancy �Infants of T. B. mothers & Breast Feeding �Women �Renal on O. C. P Impairment �ATT Induced Hepatitis �HIV - Infected or AIDS

Pregnancy �H, R, Z, E : Safe �Streptomycin: Ototoxic �May cause deafness in babies �Contraindicated

Infants of T. B. mothers & Breast Feeding �Mothers must continue A. T. T during feeding �Child should not be separated �Mother should cover her mouth during cough particularly if smear +ve �INH prophylaxis : 5 mg/Kg 2 months

Infants of T. B. mothers & Breast Feeding �Do T. T: �If –ve ◦ Stop INH, give BCG �If +ve ◦ Continue INH 4 months ◦ Then BCG �Do not give BCG while on INH ◦ INH resistant BCG �Rifampicin + INH – 3 months

Women on O. C. P �Rifampicin: ◦ Hepatic enzyme inducer ◦ O. C. P may become ineffective

Renal Impairment �General principle: ◦ Standard chemotherapy ◦ Standard duration ◦ Dose interval modification �Rifampicin and INH ◦ Safe and use normal dose �Pyrazinamide ◦ Needs dose interval adjustment

Renal Impairment �Ethambutol ◦ Nephrotoxic , Renal excretion - 80% unchanged ◦ Ocular toxicity – dose dependent ◦ Serum monitoring required �Amino glycosides – Streptomycin ◦ Nephrotoxic, renal excretion- 80% unchanged ◦ Needs dose interval adjustment in all stages �New recomandations ◦ Avoid Aminoglycosides

ATT Induced Hepatitis �Usually present early but may present any time �Mild / transient derangement in LFTs is normal (15 – 20 %) �TYPES: ◦ Hepatocellular: ◦ Cholestatic ◦ Mixed

ATT Induced Hepatitis RISK FACTOR �Age >35 years �Female sex �Oriental race (EAST ASIAN) �Pre-existing liver disease �Extensive tuberculosis �High alcohol consumption �Malnutrition and hypo Albuminemia �Other hepatotoxic drugs �Slow Acetylator status �High dosage in relation to body weight

Management �↑ ALT/AST (< Twice normal) ◦ Continue ATT ◦ Check after 2 weeks �↑ ALT/AST (>Twice normal) ◦ Continue ATT ◦ Check LFTs weekly for 2 weeks ◦ Then every 2 weeks until normal

Management �↑ ALT/AST (>Thrice normal) + Symptoms �↑ ALT/AST (>5 time normal) OR ↑ Bilirubin � If patient is smear –ve / Clinically stable � If patient is smear +ve / Clinically unstable ◦ Anorexia, Nausea, Vomiting, Abdominal Pain , Jaundice ◦ STOP ATT ◦ Even If Patient Asymptomatic ◦ Stop ATT ◦ Wait until LFTs are normal ◦ No need for alternate drugs ◦ Start Ethambutol, Streptomycin and one of the reserve drugs until LFT‘s are normal ◦ Continue safe drugs until LFTs are normal

Management �When LFT’s are normal ◦ Reintroduce ATT to detect offending drugs ◦ Start with least hepatotoxic one by one �INH > RIF > PZA �If no reaction ◦ Continue ATT ◦ Stop alternate drugs �If reaction has developed ◦ Stop offending drug ◦ Continue remaining drugs �Ensure adequate regimen and duration

HIV - Infected or AIDS �Standard regimen – usually good response ◦ Drug reactions more common ◦ Thiacetazone should be avoided ◦ Prolonged treatment

Thanks
- Slides: 39