CRITICAL THINKING The Nursing Process Learning objectives 1


CRITICAL THINKING &The Nursing Process Learning objectives : . 1. Define critical thinking. 2. Discuss the skills and attitudes of critical thinking. 3. Describe the significance of developing critical thinking abilities in order to practice safe, effective, and professional nursing care. 4. Discuss the relationships among the nursing process, critical thinking, the problem-solving process, and the decision making process. 5. Explore ways of demonstrating critical thinking

critical thinking l critical thinking in nursing practice is a discipline specific, reflective reasoning process that guides a nurse in generating, implementing, and evaluating approaches for dealing with client care and professional concerns.

critical thinking Nurses use critical thinking skills in a variety of ways : l Nurses use knowledge from other subjects and fields. l Nurses deal with change in stressful environment. l Nurses make important decisions.

Components of Critical Thinking l Creativity is a major component of Critical Thinking l Creativity is thinking that results in the development of new ideas and products. l Creative thinkers must have: 1. Knowledge of the problem. 2. Assessed the present problem. 3. Be knowledgeable about the underlying facts and principles that apply.

Using creativity , nurses 1. Generate many ideas rapidly. 2. Are generally flexible and natural: that is , they are able to change view points or directions in thinking rapidly. 3. Create original solutions to problems. 4. Tend to be independent and selfconfident , even when under pressure. 5. Demonstrate individuality.

Critical Thinking Skills l 1. 2. 3. 4. 5. Critical Thinking Skills includes: Critical analysis. Inductive and deductive reasoning Making valid inferences. Differentiating facts from opinions. Evaluating the credibility of information sources. 6. Clarifying concepts. 7. Recognizing assumptions.

Characteristics of a Critical Thinker l Curiosity: The desire, not just to know, but to understand how and why, to apply knowledge. l Systemic Thinking: Uses an organized approach to problem solving, rather than knee-jerk responses l Analytical: Applies knowledge from various disciplines, approaches a problem by examining the parts ands seeing how they fit together

l Open-Minded: Willing to consider various alternatives l Self-confident: Sense of assurance that the problem solving process produces a good conclusion/plan l Maturity: Recognition that many variables are at work in patient situations, and sometimes the best plans do not work

l Truth-seeking: Eager to know, asking questions, seeking answers, reevaluates "common knowledge"

Applying critical thinking to nursing practice l The nursing process is the framework for providing professional, quality nursing care. It directs nursing activities for health promotion, health protection, and disease prevention and is used by nurses in every practice setting and specialty. “The nursing process provides the basis for critical thinking in nursing”

l Nursing process is a systematic, rational method of planning and providing individualized nursing care. l Nurse employs critical thinking when setting priorities for the day. l The nurse manager uses critical thinking attitudes and skills. l The nurse uses critical thinking in nursing practice when solving problems and making decisions.

Nursing process Is a series of scientific steps that assist the nurse in using theoretical knowledge to diagnose the strengths and nursing care needs of persons and to implement therapeutic actions for the purpose of attaining, maintaining, and promoting optimal biopsychosocial functioning.

l The Nursing Process The term “Nursing Process” came to the UK in the 1970’ s and came to be understood as: l A form of documentation l As a means of organizing work, that is patient allocation or primary nursing l As an educational tool to help achieve patient centered nursing l As a philosophy to help nursing attain professional status by offering an alternative to the medical model.
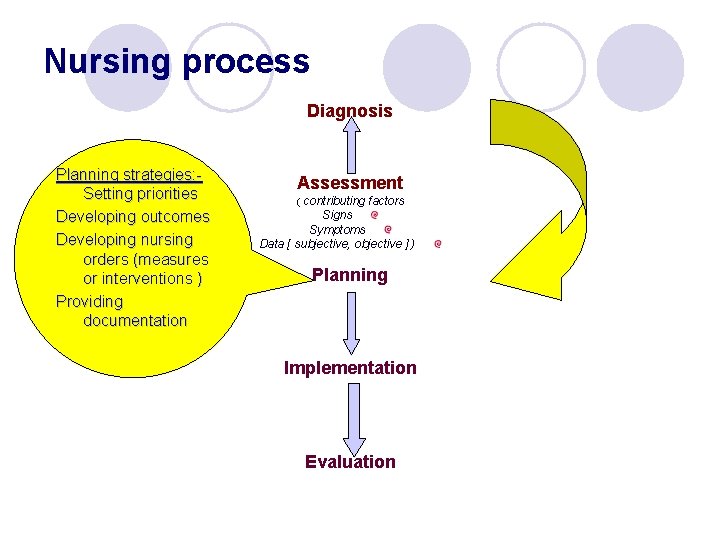
Nursing process Diagnosis Planning strategies: Setting priorities Developing outcomes Developing nursing orders (measures or interventions ) Providing documentation Assessment ( contributing factors Signs Symptoms Data [ subjective, objective ] ) Planning Implementation Evaluation
STEPS OF THE NURSING PROCESS ● l 1. Assessment l 2. Diagnosis l 3. Planning l 4. Implementation l 5. Evaluation

Assessment l Assessment is the first step in the nursing process and includes collection, verification, organization, interpretation, and documentation of data. l The completeness and correctness of the information obtained during assessment are directly related to the accuracy of the steps that follow.

Assessment involves several steps: l Collecting data from a variety of sources l Validating the data l Organizing data l Categorizing or identifying patterns in the data l Making initial inferences or impressions l Recording or reporting data

l Collecting data: Data collection is the process of gathering information about a client’s health status. A data base is all the information about a client, it includes the nursing health history, physical assessment , , , ,

COMPARISON OF DATA BASE AND FOCUS ASSESSMENTS l DATA BASE ASSESSMENT l Obtained on admission l Consists of predetermined questions and systematic head-totoe examination l Performed once l Suggests possible problems l Findings documented on an admission assessment form l Time-consuming; may take 1 hour or more (about 15 minutes) l Supplies a broad, comprehensive volume of data l Provides breadth for future comparisons l Reflects the client’s condition on entering the health care system FOCUS ASSESSMENT Compiled throughout subsequent care Consists of unstructured questions and collection of physical assessments Repeated each shift or more often Rules out or confirms problems a checklist or in progress notes Completed in a brief amount of time Collects limited data Adds depth to the initial data base Provides comparative trends for evaluating the client’s response

Types of data l Subjective data are data from the client’s point of view and include feelings, perceptions, and concerns. l Subjective data consist of information that only the client feels and can describe, and are called symptoms. An example is pain.

Objective data are observable and measurable facts and are referred to as signs of a disorder. OBJECTIVE DATA l Weight l Temperature l Skin color l Blood cell count l Vomiting l Bleeding SUBJECTIVE DATA l Pain l Nausea l Depression l Fatigue l Anxiety l Loneliness

Sources of data collection l Client. l Support people. l Client records. l Health care professionals. l Literature.

Data collection methods 1. Observing 2. Interviewing ( approaches to interviewing, Types of interviewing, planning the interviewing& setting, and stages of an interviewing ) 3. Examining. 4. Organizing data. (Wellness model, Body system model, Maslow’s Hierarchy of needs ) 5. Validating data. 6. Documenting data.

Diagnosis Learning objectives : . 1. Differentiate various types of nursing diagnosis. 2. Identify the components of a nursing diagnosis. 3. Compare nursing diagnoses, medical diagnosis and collaborative problems.

4. Identify basic steps in the diagnostic process. 5. Describe various formats for writing nursing diagnoses. 6. Describe the characteristics of a nursing diagnosis. 7. List guidelines for writing a nursing diagnosis statement.

l Diagnosis, the second step in the nursing process, is the identification of health-related problems. Diagnosis results from analyzing the collected data and determining whether they suggest normal or abnormal findings.

Nursing Diagnoses Nurses analyze data to identify one or more nursing diagnoses. l A nursing diagnosis is a health issue that can be prevented, reduced, resolved, or enhanced through independent nursing measures. It is an exclusive nursing responsibility. Nursing diagnoses are categorized into five groups: actual, risk, possible, syndrome, and wellness

l TYPES OF NURSING DIAGNOSES TYPE EXPLANATION AND EXAMPLE l Actual diagnosis A problem that currently exists Impaired Physical Mobility related to pain as evidenced by limited range of motion, reluctance to move l Risk diagnosis A problem the client is uniquely at risk for developing Risk for Deficient Fluid Volume related to persistent vomiting l Possible diagnosis A problem may be present, but requires more data collection to rule out or confirm its existence Possible Parental Role Conflict related to impending divorce l Syndrome diagnosis Cluster of problems predicted to be present because of an event or situation Rape Trauma Syndrome and Disuse Syndrome l Wellness diagnosis A health-related problem with which a healthy person obtains nursing assistance to maintain or perform at a higher level Potential for Enhanced Breastfeeding

Components of a Nursing Diagnosis 1. The problem and its definition. (diagnostic label) 2. Etiology (related factors &risk factors) 3. Defining characteristics.

Formulating Diagnostic Statements. 1. Basic two parts Diagnostic Statements 2. Basic three parts Diagnostic Statements 3. One part Diagnostic Statements

Formulating diagnostic statements l Table (12 -5) p. 201

Comparison of Nursing diagnosis, Medical diagnosis , and Collaborative problems l A nursing diagnosis is a health issue that can be prevented, reduced, resolved, or enhanced through independent nursing measures. l THE NANDA LIST. The ANA has designated the North American Nursing Diagnosis Association (NANDA) as the authoritative organization for developing and approving nursing diagnoses.
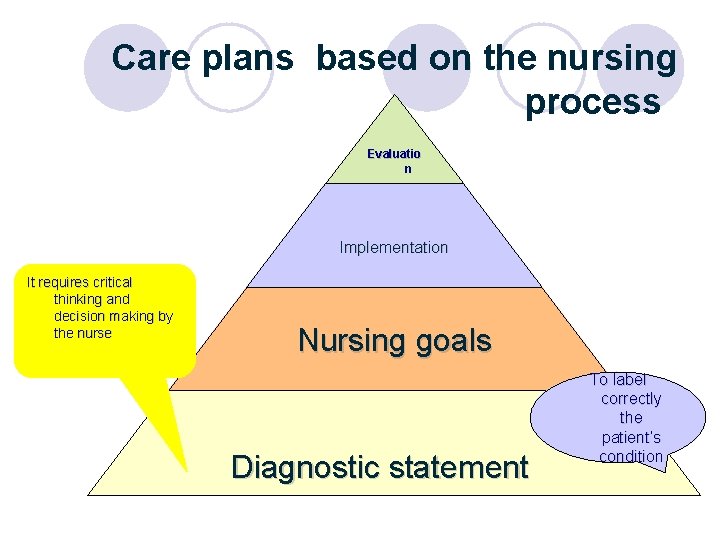
Care plans based on the nursing process Evaluatio n Implementation It requires critical thinking and decision making by the nurse Nursing goals Diagnostic statement To label correctly the patient’s condition

Nursing diagnosis It is a clinical judgment about an individual , a family or a community’s responses to actual and potential health problems/life process Nursing diagnostics refers to nursing diagnosis described as products and as process

DIAGNOSTIC STATEMENTS. l A nursing diagnostic statement contains one to three parts: l 1. Name of the health-related issue or problem as identified in the NANDA list l 2. Etiology (its cause) l 3. Signs and symptoms

l 1. Disturbed Sleep Pattern = problem l 2. Related to excessive intake of coffee = etiology l 3. As manifested by difficulty in falling asleep, feeling tired during the day, l and irritability with others = signs and symptoms

Planning Characteristics of planning l process of prioritizing nursing diagnoses and collaborative problems l identifying measurable goals or outcomes, l selecting appropriate interventions, and l documenting the plan of care. l Whenever possible, the nurse consults the client while developing and revising the plan.

l Setting Priorities Not all clients’ problems can be resolved in a brief time. Therefore, it is important to determine which problems require the most immediate attention. This is done by setting priorities. Prioritization involves ranking from those that are most serious or immediate to those of lesser importance.

l Establishing Goals 1. SHORT-TERM GOALS. Nurses use shortterm goals (outcomes achievable in a few days to 1 week) most often in acute care settings 2. LONG-TERM GOALS. Nurses generally identify long-term goals (desirable outcomes that take weeks or months to accomplish) for clients who have chronic health problems

PRIORITIZING NURSING DIAGNOSES HUMAN NEED EXAMPLES OF NURSING DIAGNOSES Physiologic Imbalanced Nutrition: Less than Body Requirements Ineffective Breathing Pattern Pain Impaired Swallowing Urinary Retention Safety and security Risk for Injury Impaired Verbal Communication Disturbed thought Processes Anxiety Fear

Love and belonging Social Isolation Impaired Social Interactions Interrupted Family Processes Parental Role Conflict Esteem and Disturbed Body Image self-esteem Powerlessness Caregiver Role Strain Ineffective Breastfeeding Self-actualization Delayed Growth and Development Spiritual Distress

l Selecting Nursing Interventions Planning the measures that the client and nurse will use to accomplish identified goals involves critical thinking. Nursing interventions are directed at eliminating the etiologies. The nurse selects strategies based on the knowledge that certain nursing actions produce desired effects.

Nursing interventions are nursing treatments based on clinical judgment and knowledge they are implemented by nurses to improve patient outcomes.

l Documenting the Plan of Care l Communicating the Plan of Care

Implementation l Implementation, the fourth step in the nursing process, means carrying out the plan of care. The nurse implements medical orders as well as nursing orders, which should complement each other.

Evaluation l Evaluation, the fifth and final step in the nursing process, l is the way by which nurses determine whether a client has reached a goal. Although this is considered the last step, the entire process is ongoing. By analyzing the client’s response, evaluation helps to determine the effectiveness of nursing care
- Slides: 47