Family planning Wednesday 30 th March GP VTS






















![In summary… �LARC 23% of primary methods of contraception �LARC methods �intrauterine devices [IUDs] In summary… �LARC 23% of primary methods of contraception �LARC methods �intrauterine devices [IUDs]](https://slidetodoc.com/presentation_image_h/9f0d0bb220d30cead141e59a1b2a8176/image-23.jpg)











































- Slides: 67

Family planning Wednesday 30 th March GP VTS

Topics covered �What to consider with contraception �Pills �IUD/IUS �Implants and injection �Special circumstances �QOF �Case studies

Not covering �Surgical methods - no funding �Natural methods �Gillick (in too much detail) �Infertility

General intro �Common consultation �Increased choice �Benefits and risks �Unwanted pregnancy

Initial consultation �Personal preference �Lifestyle �Medical history �Family history �Risk of STI

Before starting �Confirm not pregnant �Previous methods �Current medical problems �BP �Migraine? �Smoker? �Family history of cancers

COCP �Vary by oestrogen content �Vary by progesterone type � 21 pills then break

Risk greater than benefit �Aged 35 y + smoker �>50 y �HTN �IHD/CVA/PVD �DM �VTE �Focal migraine

Risk greater than benefit �Female malignancy �Hormonal problems in pregnancy �Breast feeding �Acute hepatitis �Porphyria

Starter pills �Microgynon 30 �Ovranette � 150 mcg - levonorgesterol (progesterone) � 30 mcg – ethinylestradiol (oestrogen) �£ 2. 99 �£ 2. 29

Progesterone side effects �Acne �Headache �Depression �Weight gain �Breast symptoms �Decreased libido

Alternate options �Desogesterel – Marvelon �Gestodene – Femodene �Norgestimate – Cilest �Drospirenone - Yasmin �£ 6. 70 �£ 7. 18 �£ 11. 94 �£ 14. 70

Alternate options �Cyproterone acetate – Dianette �£ 3. 70 �Not licensed for contraception alone �Used in treatment of acne

Oestrogen side effects �Breast tenderness �Nausea �Weight gain �Bloating �Loestrin 20 – 20 mcg ethinylestradiol �£ 2. 70

Breakthrough bleeding �First few months �Exclude other cause �Compliance

Interactions �New advice on antibiotics �Enzyme inducers �Affect all hormonal contraception

Missed COC pills �Current advice �Take ASAP � 2 or less � 3 or more

POP �Older women �Smokers �VTE history �HTN, DM, Migraine �Breastfeeding <6 m post-partum

Types �Cerazette- desogesterel - £ 8. 85 �Micronor/Noriday – norethisterone - £ 2. 00 �Femulen – etynodiol - £ 3. 31 �Norgeston – levonorgesterel - £ 0. 98

Starting �Start on day 1 of cycle �Take every day – no breaks �Missed pill �D+V

Side effects �Higher failure rate �Irregular bleeding �Risk of ectopic

Long Acting Reversible Contraception (LARCs)
![In summary LARC 23 of primary methods of contraception LARC methods intrauterine devices IUDs In summary… �LARC 23% of primary methods of contraception �LARC methods �intrauterine devices [IUDs]](https://slidetodoc.com/presentation_image_h/9f0d0bb220d30cead141e59a1b2a8176/image-23.jpg)
In summary… �LARC 23% of primary methods of contraception �LARC methods �intrauterine devices [IUDs] �the intrauterine system [IUS] �injectable contraceptives �implants �all LARCs more cost effective than the COCP even at 1 year of use �IUDs, the IUS and implants are more cost effective than the injectable contraceptives (DMPA)

Who can use LARCs? All LARC methods are suitable for: �nulliparous women �breastfeeding �women who have had an abortion �BMI > 30 �women with HIV – encourage safer sex �women with diabetes �women with migraine with or without aura – all progestogen-only methods may be used �women with contraindication to oestrogen

Important points to discuss: �contraceptive efficacy �duration of use �risks and possible side effects �non-contraceptive benefits �initiation and removal/discontinuation �when to seek help while using the method.

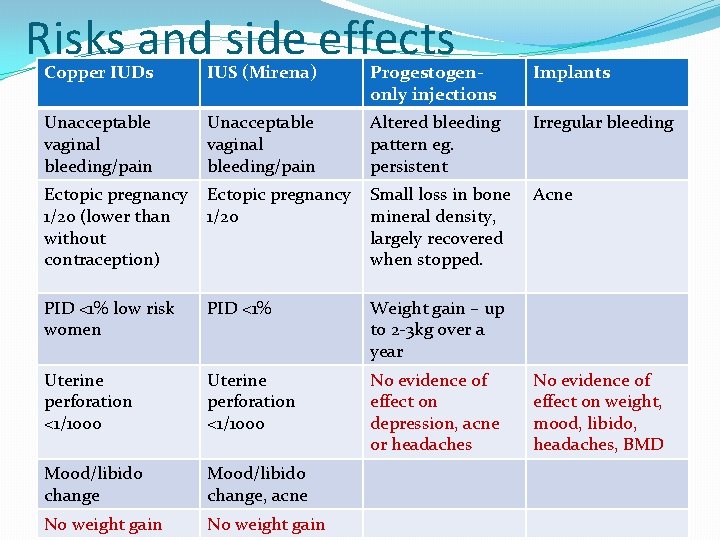
Risks and side effects Copper IUDs IUS (Mirena) Progestogenonly injections Implants Unacceptable vaginal bleeding/pain Altered bleeding pattern eg. persistent Irregular bleeding Ectopic pregnancy 1/20 (lower than without contraception) Ectopic pregnancy 1/20 Small loss in bone mineral density, largely recovered when stopped. Acne PID <1% low risk women PID <1% Weight gain – up to 2 -3 kg over a year Uterine perforation <1/1000 No evidence of effect on depression, acne or headaches Mood/libido change, acne No weight gain No evidence of effect on weight, mood, libido, headaches, BMD

Benefits – non contraceptive �Progestogen-only implants/DMPA may improve dysmenorrhoea and the symptoms of endometriosis. �Up to 20% of women using a progestogenonly implant will be amenorrhoeic �A RTC found a significant reduction in dysmenorrhoea and menorrhagia with the LNG-IUS (Mirena) when compared to a Cu. IUD.

Implants Implanon/Nexplanon

Implants - update �Nexplanon® is a progestogen-only subdermal implant (non palpable) - now replaced Implanon®. �Nexplanon and Implanon are bioequivalent (i. e. they both contain 68 mg etonogestrel and they have the same release rate and 3 -year duration of action). �Nexplanon is radio-opaque and has a different application device and insertion technique.

Implants When fitting: Check the woman is not pregnant! Nexplanon may be inserted: �at any time (but use barrier methods for first 7 days if the woman is amenorrhoeic or it is more than 5 days since menstrual bleeding started)

Implants �Prevention of ovulation. � 3 years �No delay � 20% of users - no bleeding � 50% will have infrequent, frequent or prolonged bleeding �Bleeding patterns are likely to remain irregular. �Not recommended for women taking enzymeinducing drugs eg. Anti-epileptics, St. Johns Wort. �Useful if high BMI

Intrauterine Devices and Intrauterine Systems Copper devices or Mirena coil.

Before inserting an IUD or IUS: �Test for: �Chlamydia trachomatis in women at risk of STIs �Neisseria gonorrhoeae in women at risk of STIs in areas where it is prevalent �For woman at increased risk of STIs, give prophylactic antibiotics before inserting an IUD or IUS if testing has not been completed.

�Like the implant - an IUD or IUS may be inserted: �at any time �If the woman has epilepsy, seizure risk may be increased at the time of fitting an IUD or IUS. �Women with a history of venous thromboembolism (VTE) may use the IUS.

�Pelvic infection risk - 20 days following insertion �risk same as non-IUD-using population thereafter �Irregular bleeding common in the first 6 months after insertion of the LNG-IUS but by 1 year amenorrhoea or light bleeding is usual.

IUDs �Previous endocarditis �Prosthetic heart valve �require intravenous antibiotic prophylaxis �Copper is toxic to ovum and sperm inhibiting fertilisation. �In addition, the endometrial inflammatory reaction has an antiimplantation effect and alterations in the copper content of cervical mucus inhibit sperm penetration.

IUDs �A Cu-IUD inserted when a woman >40 years can be retained until the menopause is confirmed. �>50 yrs - 1 year after the last menstrual period �<50 yrs - 2 years �Copper IUDs - 5 -10 years

IUS - Mirena �Prevents implantation. �Effects on cervical mucus reduce sperm penetration. �Inserted >45 years and amenorrhoeic - may retain the LNG-IUS until the menopause. �Randomised trials show that the LNG-IUS provides effective contraception for up to 7 years – licensed for 5 years.

After fitting: �At first follow-up visit (after the first menses, or 3– 6 weeks after insertion) �exclude infection, perforation or expulsion. �IUD only: For heavier and/or prolonged bleeding associated with use of an IUD: �– treat with NSAIDs and tranexamic acid �– or suggest changing to the IUS if the woman finds bleeding unacceptable.

Injectable contraceptives Depo Provera

Injectable contraceptives Depo Provera or Noristerat (short term use) Inhibits ovulation. Check not pregnant! Can give: �– up to 5 th day of the menstrual cycle without the need for additional contraceptives �– or use barrier contraception 7 days

�Every 12 weeks �Deep intramuscular injection �into the gluteal or deltoid muscle or the lateral thigh �Delay up to 1 year in the return of fertility BUT �…no evidence of reduced fertility long term

�Amenorrhoea (14. 4%) �Infrequent bleeding (24. 2%) �Spotting (27. 9%) �Prolonged bleeding (33. 5%) were all reported

�Small loss of BMD, which is usually recovered after discontinuation. �Women should be advised that there is no available evidence on the effect of DMPA on longterm fracture risk. �Use may continue to age 50 years.

Managing irregular bleeding �Can try: � 3 cycles of 20 -30 mcg COC, taken cyclically – can be repeated �If COC contraindicated: mefenamic acid 500 mg BD until bleeding settles… �Cerazette 1 tab daily for approx. 3 months

Managing problems with Depo Provera �Repeat injections may be given up to 2 weeks late. �DMPA use >2 years, review and discuss the balance of benefits and risks again eg. BMD �No evidence of congenital malformation to the fetus if pregnancy occurs during DMPA use. �Good choice if on enzyme-inducing drugs

Follow-up required for LARCs in summary:

Follow-up required acc. to NICE Routine follow-up IUD/IUS �At 3– 6 weeks �Return if problems or time for removal. Injectable contraceptives �Every 12 weeks; every 8 weeks for NET-EN Implants �No routine follow-up

SPECIAL CIRCUMSTANCES Under 16 s and post-partum

Providing contraception for those under 16 Fraser Guidelines and Gillick Competence

Under 16 s and providing contraception �Be aware of the law �Duty of care and a duty of confidentiality to all patients, including under 16 s. �> 25% of young people are sexually active <16 years. �Least likely to use contraception. �Confidentiality

�If considering any disclosure of information - weigh up a right to privacy against: �current or likely harm �what any such disclosure is intended to achieve �potential benefits to the young person’s well-being. �Except in the most exceptional of circumstances - consult the young person and offer to support a voluntary disclosure.

The Fraser Guidelines: �the young person understands the health professional’s advice; �cannot persuade the young person to inform his or her parents or allow the doctor to inform the parents that he or she is seeking contraceptive advice; �the young person is very likely to begin or continue having intercourse with or without contraceptive treatment; �unless he or she receives contraceptive advice or treatment, the young person’s physical or mental health or both are likely to suffer; �the young person’s best interests require the health professional to give contraceptive advice, treatment or both without parental consent.

The Sexual Offences Act 2003 The Act states that, a person is not guilty of aiding, abetting or counselling a sexual offence against a child where they are acting for the purpose of: �protecting a child from pregnancy or STIs �protecting the physical safety of a child, �promoting a child’s emotional well-being by the giving of advice.

Post partum contraception

Choices for women post-partum, including breastfeeding �IUD – copper: from 4 weeks after childbirth �IUS - Mirena: from 4 weeks after childbirth �DMPA injection: any time after childbirth, if >21 days need additional. �Implants - Nexplanon: any time after childbirth; if >21 days postpartum need additional

Abortion/miscarriage �Progestogen-only injectable contraception or implant is appropriate: �after surgical abortion �(second part of) medical abortion �miscarriage. �If DMPA or Nexplanon within 5 days �Ideally insert IUD or IUS within the first 48 hours or delay until 4 weeks postpartum.

Emergency contraception �Less than 72 hours – levenorgesterol - 1. 5 mg �Between 72 h and 120 h – Ella. One �Most effective is Copper IUD

Emergency contraception �Advise to return if abdominal pain or next period overdue �Advice on STI �Plan contraceptive follow up

TOP - practicalities �Less than 24 w �Reasons �Medical and surgical �Marie Stopes centres �http: //www. mariestopes. org. uk

QOF �LARC – offered and coded �Chlamydia testing – people under 25

Case study 1 � 17 y �Only current partner �BMI 22 �Non-smoker �Wants contraception

Case study 1 �Comes back 3 m later �Spots over face, some on back

Case study 2 � 42 y �Finished family �Wants something long term

Case study 3 � 24 y �New baby �Unplanned pregnancy

Case study 4 � 37 y �Heavy smoker �BMI 42 �Bed bound �Diabetic �Previous DVT �BP 172/104

Resources �Faculty of Family Planning �Oxford handbook of General Practice �BNF �Marie Stopes �Monkgate Clinic