Evaluation of Microscopic Hematuria Alon Z Weizer MD





















- Slides: 32

Evaluation of Microscopic Hematuria Alon Z. Weizer, MD, MS Division of Urologic Oncology Department of Urology University of Michigan

Microscopic Hematuria (MH) • Objectives of Presentation – Appreciate the importance & possible etiologies of MH – Understand the proper determination of MH – Consider the steps in evaluation of MH – Articulate recommended follow-up in cases of MH with negative initial evaluation

Why Evaluate MH? • Gross hematuria is very often an indication of disease • Although less ominous, MH also can be an indication of disease • While many of these abnormalities are minor, some are significant and/or life-threatening

Possible Causes • Life-Threatening – Cancer • Renal parenchyma • Renal pelvic • Ureteral • Bladder • Prostatic • Urethral • Penile – AAA • Require Treatment – Calculi – Vesico-ureteral reflux – Infection – Ureteral obstruction – Symptomatic urethral obstruction – Renal parenchymal disease – Symptomatic BPH – Renal artery stenosis – Renal vein thrombosis

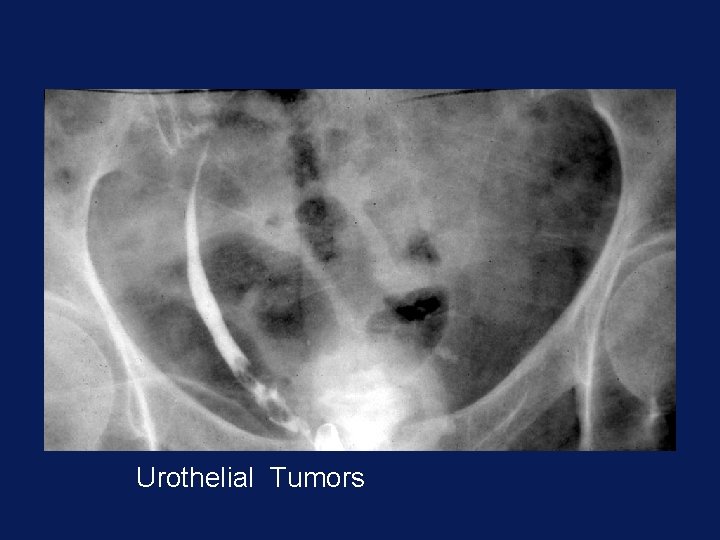
Urothelial Tumors

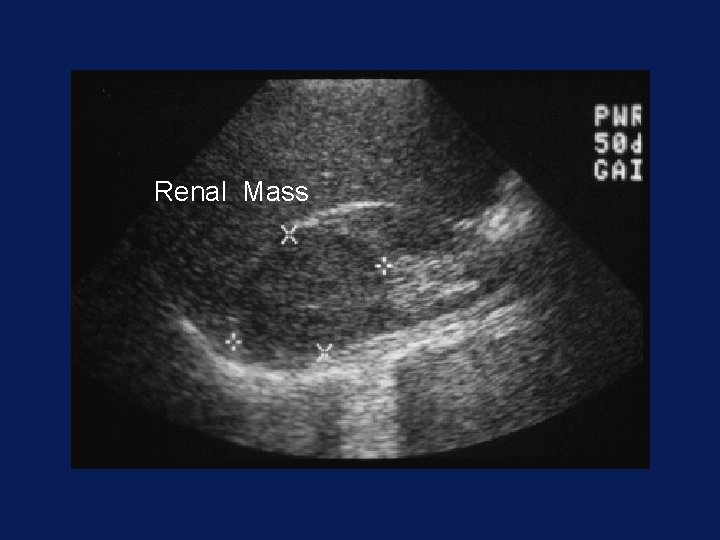
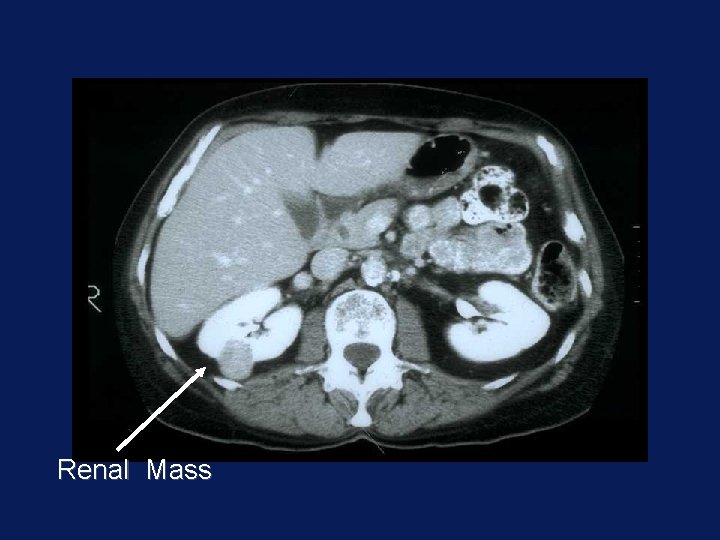
Renal Mass

Prevalence of MH • 0. 2% to 16% in population studies • 2. 5% to 21% in screening programs • 13% to 21% in men >60 years old • Likelihood of finding etiology of MH varies with risk – Low risk: Significant finding <5% – High risk: Significant finding >50%

Updated Clinical Guidelines • AUA Best Practices Panel: – Urology, Nephrology, Family Medicine, Radiology – Literature review & expert opinion – Critique of document by other physicians – Approval of AUA

Purpose of Recommendations • Resource for urologists & PCPs • Directed towards evaluation of asymptomatic MH in adults • Not meant to address: – Screening for hematuria – Gross hematuria – Symptomatic hematuria – Pediatric age group

Determination of MH • Freshly voided, clean-catch, midstream specimen • Dipstick for Hb is screening test only – 95% sensitive, but only ~80% specific – In population with 10% hematuria, PPV of Dipstick is only 35% • Positive Dipstick must be confirmed by microscopy (>3 RBC/hpf)


Determination of MH • >3 RBC/hpf is standard criterion – 1 to 2 RBC/hpf doesn’t require evaluation in most – However, it might if risk factors present • Just 1 specimen with hematuria should prompt evaluation – Old rule: 2 of 3 properly collected specimens was standard criterion

Why the Change? 1. There is substantial evidence that MH caused by a serious underlying condition can be highly intermittent 2. Studies that evaluated patients after 1 positive sample, rates of malignancy in most were over 2% 3. Non-life-threatening diagnoses that would benefit from active management or follow-up are frequently found

Risk Factors for Significant Disease • Smoking history • Occupational exposure to chemicals or dyes – Benzenes or aromatic amines • History of analgesic abuse • Age >40 years • Significant urological history – Previous gross hematuria – Irritative voiding symptoms – Urinary tract infection – Prior pelvic radiation

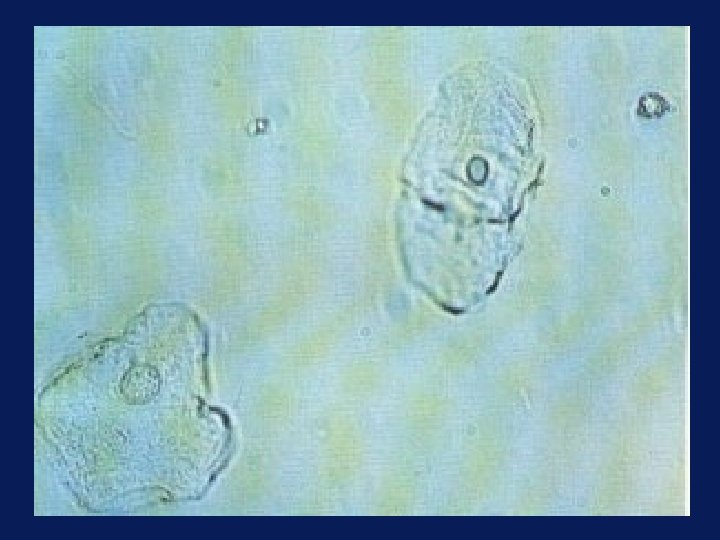
Determination of MH • Hematuria cannot be determined in presence of squamous epithelial cells • These cells may indicate contamination from source outside urinary tract – Frequent in women • Difficultly obtaining perfect clean-catch specimen – Occasionally in men • Phimosis (cells from foreskin) – Squamous cells may be present in bladder urine


Determination of MH • If there appears to be hematuria, but squamous cells are present, then get catheterized specimen – Most common reason for “unnecessary” hematuria referral = contaminated specimen – Conversely, urine w/o RBCs is adequate for determination, even if there are squamous cells

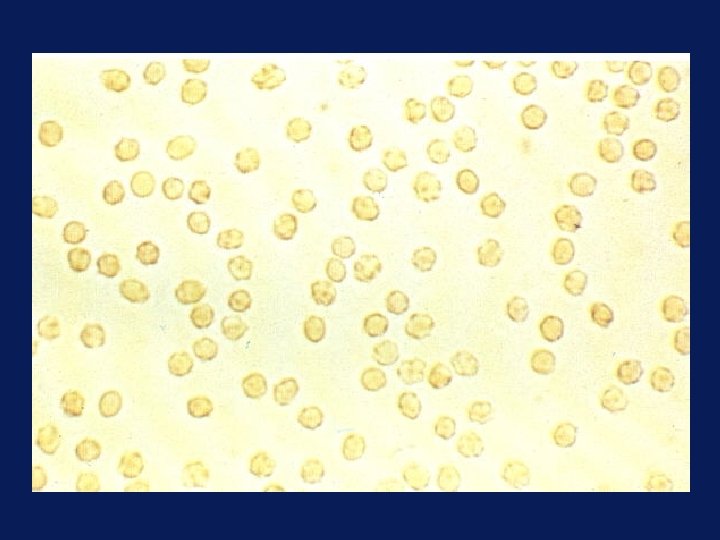
Glomerular Hematuria • Origin of blood from renal parenchymal disease can be suggested by UA – Dysmorphic RBCs (variable size & shape w/irregular outline) → sensitive – Plain microscopy, or may need inverted phasecontrast microscopy


Asymptomatic MH History and Physical Examination Rule Out Benign Causes: Menstruation Vigorous Exercise Sexual Activity Viral Illness Trauma Infection Resolved after Tx or delay No Evaluation Persistent Evaluation Required

Evaluation: H&P • Gross or microscopic? – Gross more often assoc w/significant disease • Initial, terminal or total? – Initial = urethra, terminal = bladder neck/prostate • Pain, dysuria, bladder irritability – Suspect infection or obstruction • Anti-coagulated – Still require evaluation

Evaluation: H&P • Sickle cell, diabetes • Family or personal history of calculi, PCKD, other GU/Neph diseases • Trauma, physical or sexual activity • Tobacco use, occupational exposure • Association with menses • Fever, palpable mass, atrial fibrillation, visible blood at meatus, CVAT

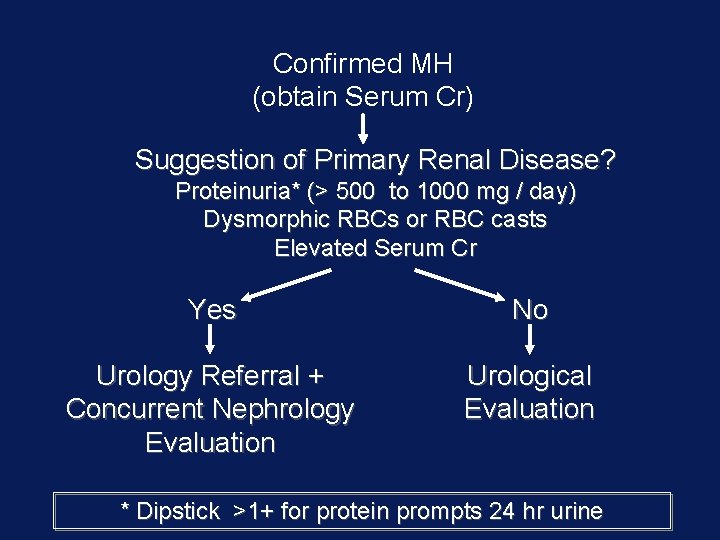
Confirmed MH (obtain Serum Cr) Suggestion of Primary Renal Disease? Proteinuria* (> 500 to 1000 mg / day) Dysmorphic RBCs or RBC casts Elevated Serum Cr Yes No Urology Referral + Concurrent Nephrology Evaluation Urological Evaluation * Dipstick >1+ for protein prompts 24 hr urine

Purpose of Urological Eval • Upper tract imaging – Diseases of the kidney & ureter – Most commonly &/or significantly: • • Calculi • Urothelial lesions • Obstruction • Renal masses Cystoscopy – Diseases of the bladder & urethra – Most commonly &/or significantly: • Bladder cancer • BPH • Urethral strictures

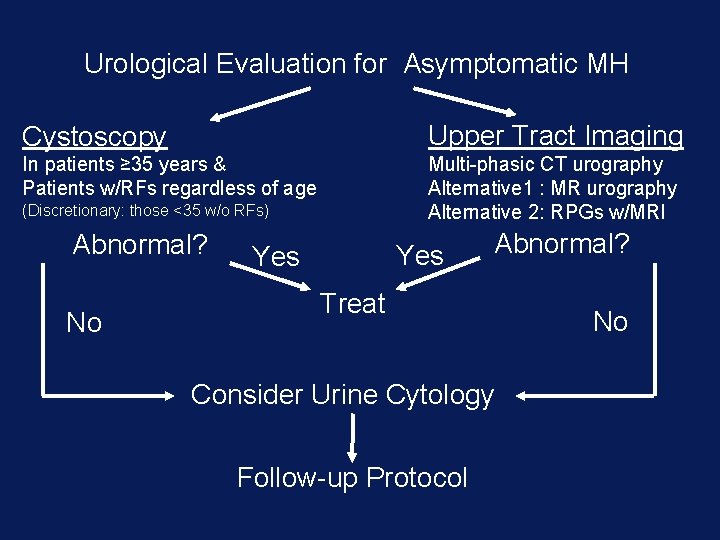
Urological Evaluation for Asymptomatic MH Cystoscopy Upper Tract Imaging In patients ≥ 35 years & Patients w/RFs regardless of age Multi-phasic CT urography Alternative 1 : MR urography Alternative 2: RPGs w/MRI (Discretionary: those <35 w/o RFs) Abnormal? No Yes Abnormal? Treat Consider Urine Cytology Follow-up Protocol No

Imaging Modalities • Computed Tomography – Best modality for characterization of small renal masses – More widely available & less expensive than MRI – Best modality for calculi, renal and perirenal infection & associated complications – Sensitivity for urothelial lesions not defined with certainty, but thought to be good with “urography” technique

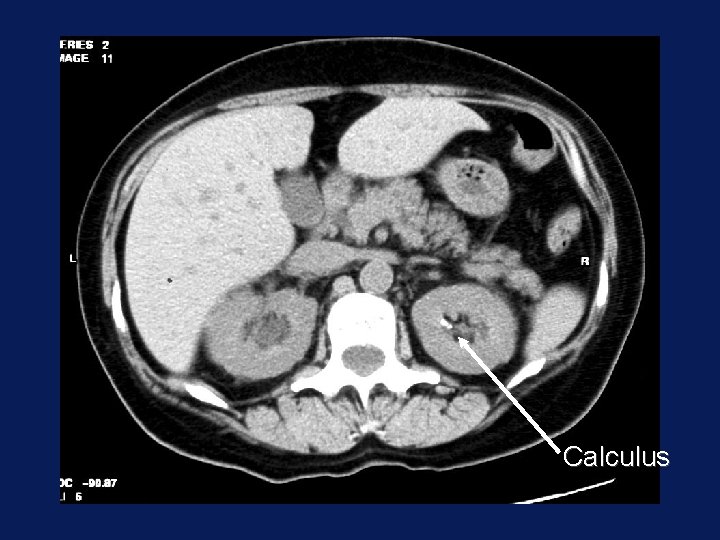
Calculus

Renal Mass

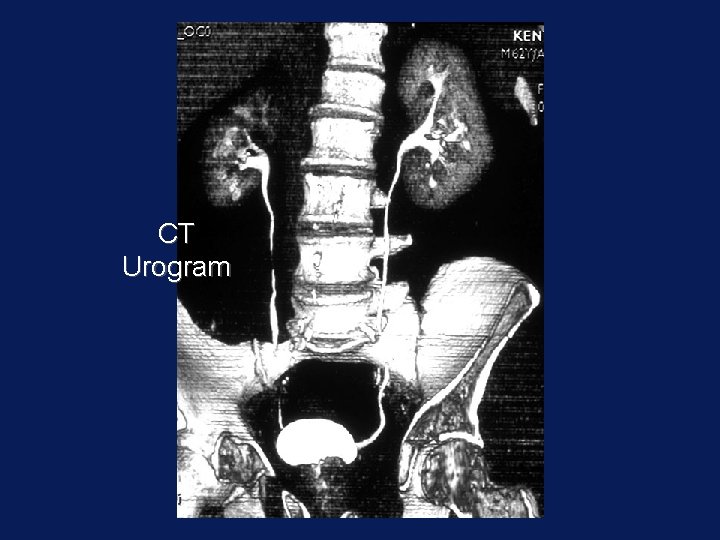
CT Urogram

Other Options • MR urography – Pregnancy, patients with iodinated contrast allergy – Risk of nephrogenic systemic fibrosis in patients with renal insufficiency • Retrograde pyelograms combined w/magnetic resonance imaging

Follow-Up Protocol • UA at 12 & 24 months – If negative for 2 consecutive years, then D/C • If persistent asympomatic MH, repeat urological evaluation w/in 3 – 5 years • If gross hematuria or new voiding sx, repeat urological evaluation

Before Urological Referral • Determine if this is real MH – >3 RBC/hpf – Catheterized urine if squamous cells • Exclude benign causes w/H&P • Likely glomerular → Refer to neph, too • Obtain serum Cr • Order imaging