Epilepsy Awareness Epilepsy Nurse Specialists Learning Outcomes Demonstrate


















































- Slides: 52

Epilepsy Awareness Epilepsy Nurse Specialists

Learning Outcomes • Demonstrate an awareness of what Epilepsy is and recognition of different seizure types • Be able to support children/young person experiencing seizures, ensuring their safety and dignity • Demonstrate awareness of the importance in observing and recording seizure activity • Recognise possible trigger factors

Learning Outcomes • Demonstrate an understanding of the epilepsy/emergency management plan • Plan of action and emergency call sheet • Raise awareness of the impact of epilepsy on a child/young person’s life • Understand the need for balancing risk and achieving a quality of life • Raise awareness of the possible educational implications of the condition • Evaluation and close

What is Epilepsy? • Epilepsy has been defined as a tendency to have recurrent seizures, 'fits’ or ‘convulsions’ • These are caused by the chemical balance in the brain being upset and causing abnormal firing of nerve cells • One seizure does not constitute epilepsy • Common condition Affects 1: 242 School Age Children/young person (Epilepsy Action 2005) • More common in children/young people with learning disability with approx. 22% of people with learning disability being diagnosed with epilepsy

Important Points Never assume that all seizures are epileptic in nature ! • Common serious chronic condition • Approximately 40 different types of seizures • The type of seizure the child/young person experiences depends on which part of the brain it starts and how far or quickly it spreads • Can develop at any age, however it is usually diagnosed before the age of 20 • Very individual/specific to the child/young person

Prognosis of Epilepsy • 20% - 30% Excellent prognosis - Seizure free after AED withdrawal – cause no longer exists • 20% - 30% Good prognosis – remission with AED treatment but cause remains • 30% - 40% Seizures continue despite treatment, AED’s may only reduce frequency or severity (Kwan & Sander 2004)

What causes Epilepsy • 60 - 70% of cases the cause is unknown • Some known causes include: § § § § Birth injury Head injury Stroke Brain haemorrhage Brain Tumour Meningitis/encephalitis Drugs Alcohol

Potential Triggers • • Flickering lights/photosensitivity Lack of sleep/tiredness Stress Excitement Missed meals High Temperature Menstrual Missed or late medication

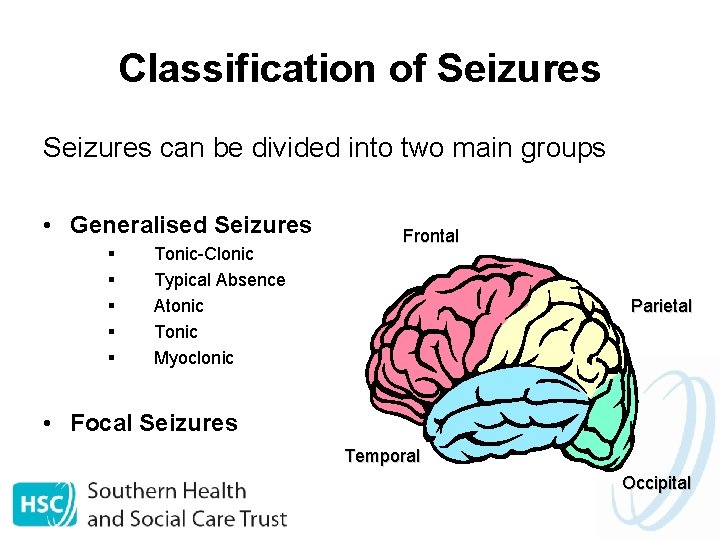
Classification of Seizures can be divided into two main groups • Generalised Seizures § § § Tonic-Clonic Typical Absence Atonic Tonic Myoclonic Frontal Parietal • Focal Seizures Temporal Occipital

Generalised Seizures • These occur when powerful centrally positioned nerve cells behave abnormally • The discharge spreads more or less simultaneously to all parts of the brain • There is loss of consciousness – can be brief or longer

Tonic -Clonic Seizures • Most common type of generalised seizure • The child/Young person may have an aura leading into the tonic/clonic seizure • May lose consciousness • Duration usually 1 -2 minutes • May follow on from a focal seizure

Tonic Phase • Muscles contract, body stiffens and child falls to the floor • The child may become pale • Their breathing may be irregular and around their lips may appear blue • Saliva may dribble from mouth and can be blood stained if tongue has been bitten • Incontinence may occur

Clonic Phase • Consists of short sharp rhythmic jerks caused by alternate contraction and relaxation of muscles in the trunk and limbs • Periods of relaxation become more frequent and prolonged • Muscles relax and the body goes limp. At this stage the child will still be unconscious • Slowly they will regain consciousness, but may be groggy and confused

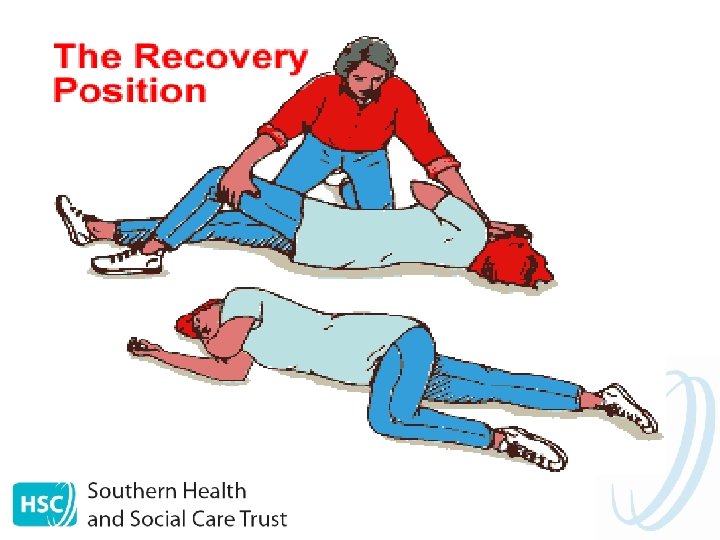
Management of Tonic-Clonic Seizures DO: • • • Stay calm Assess danger to child- move if in danger Protect their head Loosen tight clothing, remove glasses Time seizure/observe and record Once seizure has finished aid breathing by gently placing them in the recovery position • Stay with the child until recovery is complete • Reassure and re-orientate the child, tell them they have had a seizure • Allow the child a period of rest /sleep afterwards if required

Management of Tonic-Clonic Seizures DON’T: • Try to restrain or restrict the child's movements • Put anything into their mouth • Give the child anything to eat or drink until they are fully recovered

http: //learn. epilepsy. org. uk/first-aid-forseizures-in-schools/

Typical Absence Seizures • Generally a childhood disorder • Brief lasting only seconds- begins and ends abruptly • May look blank and stare, lasting a few seconds • Eye lid fluttering/blinking may occur • May have minor facial movements or head drop • Able to continue normal activity almost immediately

Management of Absence Seizures • Usually no help is needed • Record the time of day and frequency • Reassure if necessary • Repeat information that the child may have missed • If walking they may require guidance


Atonic Seizures (drop attack) • Sudden loss of muscle tone • Fall heavily to the ground • Lasts only a few seconds • Able to continue normal activity almost immediately

Tonic Seizures • Muscles contract • Body stiffens- trunk, facial muscles and limbs • Results in falls • Quick recovery

Management of Atonic and Tonic Seizures • Maintain the child/young persons safety and dignity • Over very quickly therefore little can be done during seizure • Check for injuries which may need medical attention • Stay with the child and reassure

Myoclonic Seizures • Quick muscle jerks usually of limbs however head and shoulders may jerk forward • May be one or both sided • Usually seen in specific childhood epilepsy syndromes • Frequent soon after waking • Short lived so difficult to tell if consciousness is impaired

Management of Myoclonic Seizures • Usually so short lived little can be done other than reassure when over. • May become unsteady so if they fall assist and check for injuries • Stay with the child until they recover • Reassure


Focal Seizures • Focal seizures have a starting point in a particular area of the brain. • The type of seizure activity seen is dependant on where the focus point is. • Focal seizures can spread to the rest of the brain resulting in a secondary generalised seizure

Focal Seizures • Symptoms can last from seconds to 1 – 3 minutes can present as: • Either mumbling or uncontrolled laughter • Sucking, chewing or swallowing movements • Plucking at or removing clothing • May wander around as if confused

Management of Focal Seizures DO: • Stay calm • Guide the child from danger • Stay with the child until recovery is complete • Reassure and explain anything they have missed

Management of Focal Seizures DON’T: • Restrain the child • Act in a way that could frighten them, such as making abrupt movements or shouting at them • Give the child anything to eat or drink until they are fully recovered



Call an Ambulance if …… • You think the child needs urgent medical assistance • The child has any breathing difficulties following a seizure • It is a first seizure • The seizure continues for longer than normal • One seizure follows another without the child regaining consciousness

Following a Seizure After a seizure the child may be…. . § Confused § Have no memory of what has occurred § Subdued § Tired & sleepy § Have a headache § Concentration impaired § Hyperactivity

Care following a Seizure • Clear understanding of what has occurred • Observe: § Breathing & colour § Any injuries • Be aware of post-ictal state • Offer support and counselling as appropriate

SUDEP (sudden unexpected death in epilepsy) • Sudden death with no obvious cause • Can occur with/without evidence of a seizure • It is estimated that approx 1 per 1000 people with epilepsy in the UK die as a result.

Role of School Staff/Carer • Be aware of children with epilepsy • Have as much information as possible about specific seizures from parent/carer • Observe any unusual behaviour & liaise with parent/carer • School staff may be first to pick up on the seizures like Absences/day dreaming • Positive attitude to epilepsy • Try to avoid treating epilepsy as an illness

Role of School Staff/Carer contd. • Recognise/record changes in mood/behaviour/academic achievement/social interaction • Risk assess for particular activities • Promote communication with parents • Minimize embarrassment • Observe and record details of seizures

Description of Seizure Why? • Informs care staff of what is normal for child/young person • Assists with establishing a diagnosis • Observe changes in frequency and type of seizures • Helps monitor effects of treatment • Important to review recordings otherwise changes may go unnoticed.

Observation of Seizures – Before - During - After • How did the child/young person feel before the event? • In what environment/activity? • Time of day or night? • Anything ‘trigger’ the event? • Was there a warning? • What was the event like? § Standing / Sitting / Lying? § Was there a fall? § Parts of body effected/movements? § Eyes open/closed?

Observation of Seizures – Before - During – After contd. • • • Were they unconscious -fully or just had a vagueness If unconscious ? How long Behaviour after seizure Incontinence /tongue bite /excessive salvia Any injury or bruising Length of time in the seizure How were they after the event ? Recovery time Howe did the staff cope with the event ? Anxiety /debriefing

Seizure Management Plan • Seizure Management Plan should be in place & available agreed by: § Parent/carer § Children’s Epilepsy Nurse Specialist • Updated yearly or more often if required • Be aware of who is responsible for first aid • Parent/carer should be informed of seizure ASAP • Record seizure

Seizure Management Plan WILL PROVIDE: • Description of seizure • Triggers • Management of the seizures • What to do in an emergency • Any other relevant information applicable to the individual child

Emergency Seizure Management Plan This is only provided for children who are prescribed emergency medication WILL PROVIDE: • Description of seizure/duration • Indications for use of emergency medication • Initial dose of emergency medication • The child’s/young person’s response to emergency medication (if known) • Who is trained to administer the medication • Consent from the parents for this to be administered

Educational Implications A change in behaviour can be observed : May be caused by • Seizure activity • Side effects of medication BUT Behaviour can be independent of seizures/medication? Memory: Can experience some loss or difficulty retaining Information, depending on each individual child/young person.

Care of other Pupils • Reassure other pupils present • The type of seizure they witness will have a direct impact on how they cope so give them an opportunity to express their worries and fears. • Do not keep epilepsy a secret

Sport • Most children with epilepsy should be able to fully participate in most activities ensuring adequate supervision is provided • Each activity & each child should be considered individually • Special considerations & precautions should be discussed with the parent

Social Life The following can increase the risk of seizures: § Excess alcohol § Lack of sleep § Disturbed sleep patterns § Missing meals § Forgetting to take medication § Recreational drugs

Points to remember • Do I know about the child’s/young person’s epilepsy? • Is there a Seizure Management Plan in place? • Is the child/young person prescribed emergency medication? if so are relevant staff trained to administer? • Has the person’s epilepsy been reviewed recently? • Lifestyle and impact on Epilepsy • Are any Risk assessment required?

Points to Remember contd. • Are all relevant staff aware? • Normally seizures run their course and the child recovers without need for medical intervention. • Children should be given the opportunity to participate in the same activities as their peers promoting independence, confidence and self-esteem.

Further Information WEBSITES: • WWW. Young Epilepsy. org. uk • Epilepsy Action Northern Ireland

