Chest Pain James Ignatius Nicole Qaqish 7192010 Classification





























- Slides: 32

Chest Pain James Ignatius Nicole Qaqish 7/19/2010

Classification • Cardiac Vs Non-Cardiac causes • Cardiac: Ischemic Vs Non-ischemic pathology • Ischemic: Angina, Myocardial Infarction • Non-Ischemic: Pericarditis • Non Cardiac: G. I (GERD, PUD), Pulmonary (PE, Pneumothorax, Pneumonia, Pleurisy, and Pul. HTN)

Chest Pain Questions • • “LIQUOR’D” mnemonic L = location, (retro, substernal… I Intensity (1 -10) Q Quality (Sharp, Pressure, dull…) U Upsetting/Aggravating Factors O Onset R Releiving factors + Radiation D Duration

Angina • Chest pain that occurs when the coronary arteries do not deliver an adequate amount of oxygen-rich blood to the heart • Categorized as stable, unstable, and Variant (Prinzmetal’s )

Stable Angina • • • Clinical findings of stable angina: Substernal , high pressure/heavy feeling Duration from 1 – 5 minutes Instigated by physical exertion Relieved with rest or nitrates

Unstable Angina • • Clinical findings of Unstable Angina: Occurs even at rest unexpected More severe and lasts longer than stable angina, maybe as long as 30 minutes • May not disappear with rest or use of nitrates

Variant Angina • Transient coronary vasospasm that is associated with a fixed atherosclerotic lesion (75%) • Pt tends to be younger and in seemingly good health • Occurs at rest and associated with ventrcular dysrhythmias • Nitrates and CCB’s are often effective

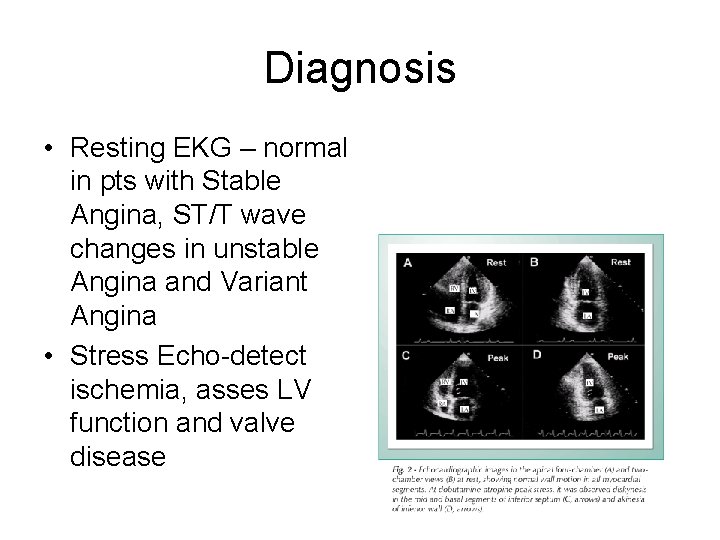
Diagnosis • Resting EKG – normal in pts with Stable Angina, ST/T wave changes in unstable Angina and Variant Angina • Stress Echo-detect ischemia, asses LV function and valve disease

Treatment • Lifestyle changes • Pharmacotherapy – Aspirin, Beta, Blockers, CCB, Nitrates • Revascularization (CABG)

Myocardial Infarction • Interruption of blood supply which causes necrosis of the myocardium. • Atheromatous plaque ruptures into lumen and thrombus forms on top of the lesion causing occlusion • MI has a 30% mortality rate.

Myocardial Infarction • Clinical Features: • Crushing substernal chest pain(usually >30 minutes) • Radiation to arms, neck, jaw, back (Left side) • Diaphoresis, Nausea, Vomiting, Dyspnea, Syncope

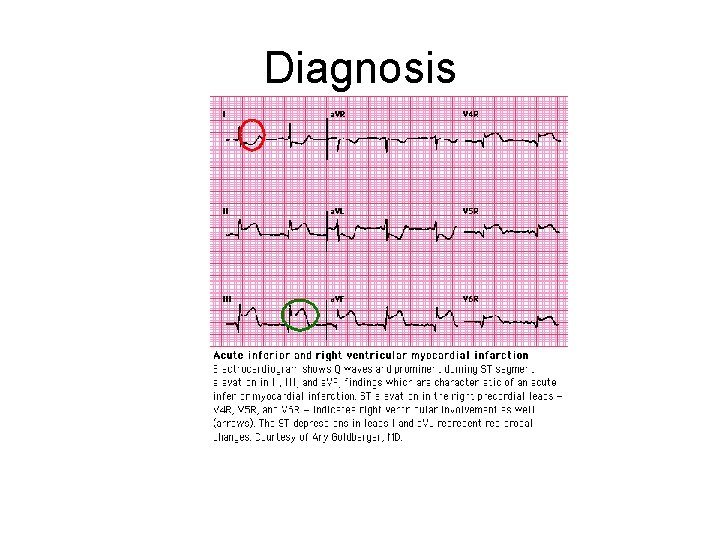
Diagnosis EKG changes: ST elevation – transmural injury and can be diagnostic of acute infarct ST depression – Sunbendocardial injury Q wave – evidence for necrosis, usually indicative of an old MI. Not seen acutely

Diagnosis

Diagnosis • Cardiac enzymes – Gold Standard. • 3 sets q 8 in 24 hours • CKMB – increases within 4 -8 hours, peaks at 24 hrs, and returns to normal 48 -72 hrs later • Trop I – More specific/sensitive than CKMB. • Trop. I falsely increased in Renal failure

Treatment • Admit pt to CCU, Insert IV, , administer oxygen, nitrates, morphine • Aspirin, b-blockers, ACE Inhibitors reduce mortality • Lovenox can slow progression of thrombosis. • Cardiac Rehab- exercise + lifestyle changes post MI

Pericarditis • Inflammation of fibrous sac which covers the heart • Causes: Viral Infection (Coxsackie B, Echovirus, Hep. A/B) MI, Uremia, • Pts usually recover in 1 -3 weeks

Pericarditis • Clinical Features: • Pleuritic chest pain that is positional(worsened by lying down, inspiration). Pain is releived by sitting up + leaning forward • Friction Rub – scratching, high-pitched sound caused by rubbing of visceral and parietal pleura

Pericarditis • Diagnosis • EKG – ST elevation and PR depression , then ST returns to normal, Twave inverts, then returns to normal. • Treatment: Treat underlying cause and offer NSAIDS for pain

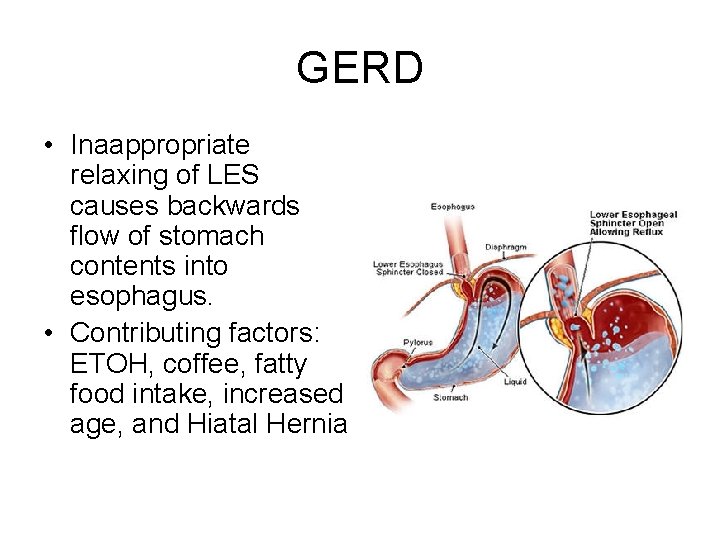
GERD • Inaappropriate relaxing of LES causes backwards flow of stomach contents into esophagus. • Contributing factors: ETOH, coffee, fatty food intake, increased age, and Hiatal Hernia

GERD • • • Clinical Features: Burning, retrosternal pain after meals Cough, nausea, vomiting Hoarseness , sore throat Reflex saliva hypersecretion

GERD • Diagnosis: • Endoscopy w/ Biopsy- Can detect cancer complication or GERD • 24 hr p. H monitoring of LE – Gold Standard. Highly specific/sensitive

GERD • • Treatment: Phase I- diet changes + antacids Phase II – Add H 2 blocker (Ranitidine) Phase III – Switch to PPI if symptoms don’t resolve • Phase IV – Add pro – GI motility Agent (bethanechol/metoclopramide) • Phase V – combo (H 2 or PPI) + BTH/MET

Peptic Ulcer Disease • A peptic ulcer is erosion in the lining of the duodenum. • Causes: H. pylori infection, NSAID, Zollinger-Ellison syndrome, Smoking, Stress • Clinical Features: • Epigastric pain that is achy • Nausea, vomiting, weight loss, Upper GI bleed

Diagnosis • Endoscopy is most accurate test • Histological evaluation of endoscope biopsy – Gold Standard for H. pylori infection • Urease Breath Test – Shows active infection, and efficacy of antibiotic therapy • Serum gastrin- specific test for ZE Syndrome

Treatment • Lifestyle mods(Reduce smoking, stress, ETOH, NSAID) No food before bedtime! • If H. pylori is present use Triple or Quadruple therapy • Triple ( PPI + 2 antibiotics) • Quadruple (PPI + Peptobismol + 2 Antibiotics)

Treatment • H 2 blockers help with ulcer healing • Surgical intervention need for complications of PUD like bleeding, perforation

Case Study • A 30 year old woman comes to the clinic complaining of chest pain. For the last 2 years, she has had intermittent nocturnal chest pain that lasts up to 10 minutes. The pain is substernal and radiates to her throat. It is 6/10 and wakes her up from sleeping. She has mild nausea and a clammy feeling. In the past, she has used antacids and PPI which did NOT help. Aerobic exercise sometimes instigates this pain.

Case Study • She reports being quite healthy except for having Raynauds phenomenon in winter and migraines treated with sumatriptan. Social history is remarkable for cocaine use. Vital signs and physical exam are unremarkable. Holter monitor study is arranged. What findings would be most likely evident during an episode of her chest pain?

Case Study • A) PR segment depression • B) Normal electrocardiographic tracing • C) Prolonged QT interval with increased duration at night • D) Transient St elevation in inferior Leads

Answer • D) This patient has a classic presentation of Variant Angina, which is caused by coronary vasospasm that induces transient ischemia and ST elevations. Patients are usually young women w/o classic CVS risk factors. It usually occurs at night and can be worsened by cocaine and serotonergic agents like sumatriptan.

Answer • Vasospams can occur in any distribution but tend to favor the right coronary artery which supplies the inferior portion of the heart • A = Pr depression is indicative of pericardits. Viral infection in Hx would have been a clue and leaning forward in bed would have produced relief.

Answer • B= ST elevations and T wave changes are associated with variant angina. EKG can not be normal • C= There is no reason to suspect QT interval prolongation. Pts who have syncopal episodes may have QT prolongation and it would not worsen at night.