CHRONIC PAIN SYNDROME Chronic Pain define as Pain





















- Slides: 26

CHRONIC PAIN SYNDROME

Chronic Pain define as: Pain persists beyond either the course of an acute disease or reasonable time for an injury to heal Pain is associated with chronic pathological process Pain that recurs at interval of months or year

Chronic Pain Syndrome I Malignant Cancer pain syndrome II Non-Malignant Nociceptive Neuropathic Psychogenic Central pain

Nociceptive Low back pain Myofacial pain Visceral pain Headache and facial pain Neck and shoulder pain Neuropathic pain Sympathetically mediated pain Post herpetic neuralgia Trigeminal neuralgia Phantom pain

Modalities of Pain Management I Pharmacological II Anaesthesiologic III Special technique * Facet Blocks * Acupuncture (Gate control theory) * Cryolysis * Ablative technique * Radio frequency * Physical therapy

Contd. . . Pharmacological Analgesic Paracetamol NSAID Opioids Co-analgesics Anti-depressant Anti-convulsant

Anesthisiologic Central nerve blocks ○ Spinal ○ Epidural Peripheral nerve blocks ○ Femoral ○ ICN ○ Others Autonomic Nerve blocks ○ Stellete ganglion ○ Lumber Sympathectomy Contd. . .

Special Technique Contd. . . Facet block for back pain Cryolysis for nerve damage Radio frequency for facet joint / nerve damage Acupuncture 361 classical acupuncture points lie along specific pathway or meridians Ablative neuro-surgical procedure - interrupt sensory pathways to the brain or in the brain and brain stem.

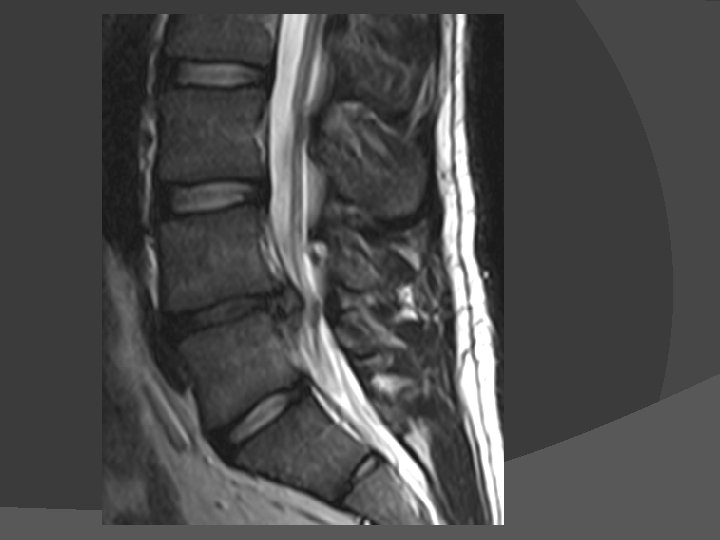
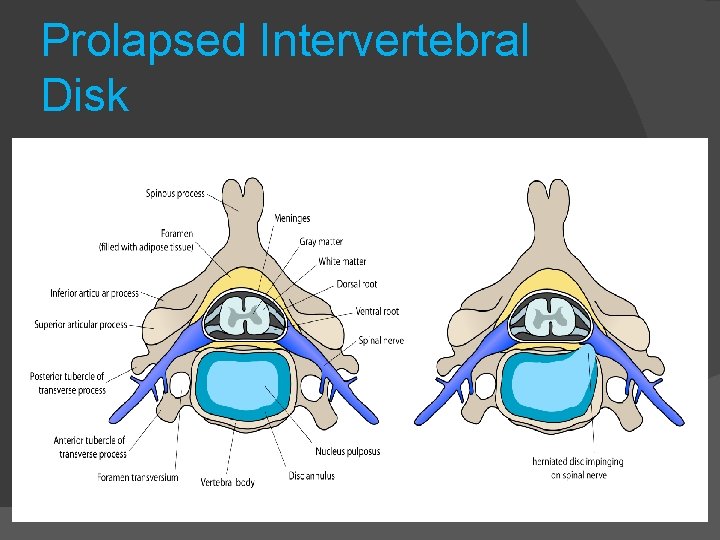
Low Back Pain Most common condition seen in the pain clinic Major causes: Prolapse inter-vertebral disc Facet joint degeneration Sacroiliac joint arthritis Musculoskeletal disorder Miscellaneous



Prolapsed Intervertebral Disk

Management of Low Back Pain alone may not justify decompression surgery like laminectomy or micro-discectomy

Treatment Options Drug therapy vs nerve block procedure drug therapy NSAID, week opioids & other support therapy Low morbidity out patient ○ Epidural steroid ○ Facet joint steroid injection ○ Sacroiliac steroid injection

Myofacial Pain Syndrome Pathogenesis The likely has a central mechanism, with peripheral clinical manifestations. Causes Abnormal stresses on the muscles from sudden stress on shortened muscles, leg-length discrepancies, or skeletal asymmetry Poor posture, static position for a prolonged period of time Chronic infections and sleep deprivation

Sympathetically Mediated Pain (SMP) Reflex sympathetic dystrophy (RSD) and causalgia RSD A group of condition associated with extremity pain and autonomic dysfunction Causalgia Specific syndrome of burning pain and autonomic dysfunction associated with major nerve trunk injury.

Treatment Options Drug therapy Antidepressant Anti convulsant Narcotic analgesic Oral nifedipine Adrenergic blocking agents Nerve Block Chemical sympathectomy Physical therapy

Post-herpetic neuralgia Pain in the distribution of a nerve It follows an acute herpetic attack Incidence: 3 -4 per 1000 Clinically: Burning pain constant deepache crawling or scratching pain stabbing or shooting

Management Drug therapy (main stay) Anticonvulsant Anti depressant Nerve block Little role

Trigeminal Neuralgia Conditions occur more often in Female middle aged Strictly unilateral, however in 2% it may be bilateral Pain in the face is characterized by sharp, severe (paroxysmal) and brief lasting no more then a few seconds.

Management of Trigeminal Neuralgia Drug Therapy Anti-convulsant Anti depressant Nerve block Cryo-analgesia Radio-frequency

Malignant Pain Syndrome Incidence 70% of cancer patients suffer from pain as a symptoms

Management Strategies Pharmacological methods Interventional pain management neurolytic blocks Intraspinal drug delivery system

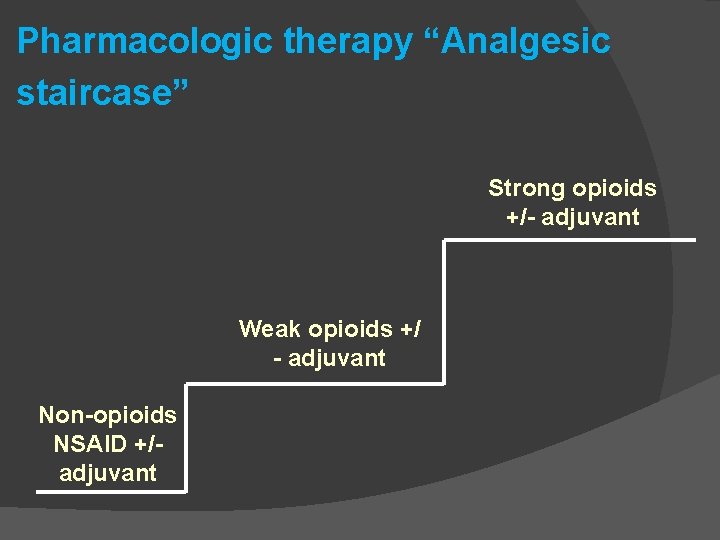
Pharmacologic therapy “Analgesic staircase” Strong opioids +/- adjuvant Weak opioids +/ - adjuvant Non-opioids NSAID +/adjuvant

Invasive Procedures When pain or side effects persist despite comprehensive trials of pharmacologic therapy I Neurolytic blocks ○ Coeliac plexus ○ Hypogastric plexus II Intra-spinal drug delivery ○ short terms – intrathecal or epidural infusion ○ long term – implants

CONCLUSION Control of pain in chronic pain syndrome can be achieved in most patients by the application of a carefully individualized, flexible programme of : analgesic drugs Interventional pain management