Aging of Cardiac Muscle and Cardiac Failure Dr



















- Slides: 25

Aging of Cardiac Muscle and Cardiac Failure Dr. Franco Navazio

Aging Heart in the Elderly In absence of specific disease the heart adjusts very well to advancing age.

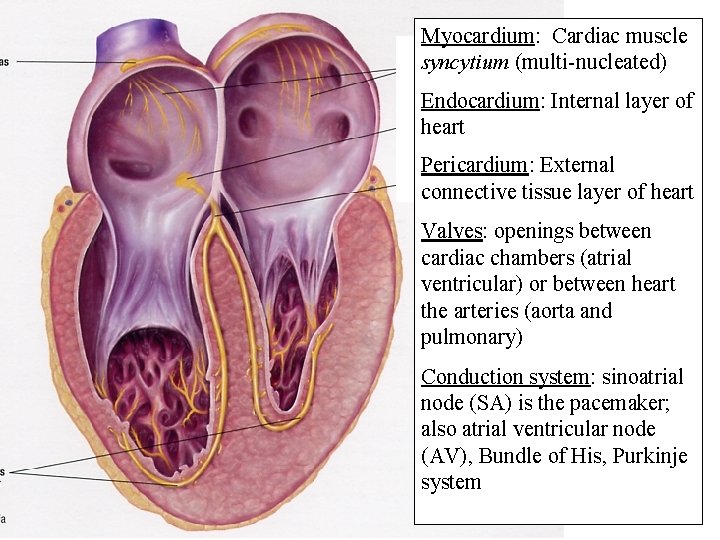
Myocardium: Cardiac muscle syncytium (multi-nucleated) Endocardium: Internal layer of heart Pericardium: External connective tissue layer of heart Valves: openings between cardiac chambers (atrial ventricular) or between heart the arteries (aorta and pulmonary) Conduction system: sinoatrial node (SA) is the pacemaker; also atrial ventricular node (AV), Bundle of His, Purkinje system

Aging Heart: Physiology Decline in the VO 2 Max with advancing age Minor decline in the cardiac output Important Variables: – physical conditions – dietary habits Conclusions: Physically fit elderly people have a cardiac physiology similar to younger individuals

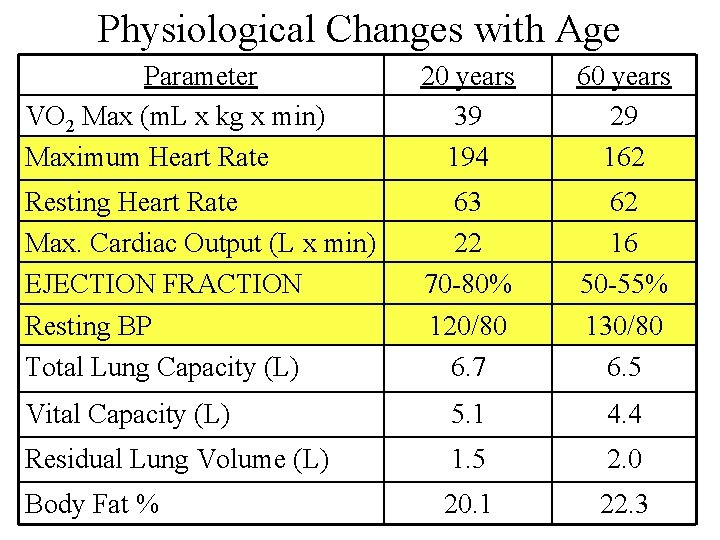
Physiological Changes with Age Parameter VO 2 Max (m. L x kg x min) Maximum Heart Rate 20 years 39 194 60 years 29 162 Resting Heart Rate Max. Cardiac Output (L x min) EJECTION FRACTION Resting BP Total Lung Capacity (L) 63 22 70 -80% 120/80 6. 7 62 16 50 -55% 130/80 6. 5 Vital Capacity (L) 5. 1 4. 4 Residual Lung Volume (L) 1. 5 2. 0 Body Fat % 20. 1 22. 3

Cardiovascular Changes with Age Hypertension: most common treatable cardiovascular change in the elderly Definition: values above 140/190 In young, if standing BP but in elderly it may to 20 mm. Hg Systolic mumur: 50% of elderly but of very short duration EXG (or ECG): only nonspecific changes due to aging in voltage and nonspecific RBBB Hypotension: diminished baro-reflex response in the elderly. With age, cerebral blood flow but autoregulation acts in a compensatory fashion; some patients maybe affected by symptomatic orthostatic hypotension Orthostatic hypotension: drop of 20 mm. Hg in the systolic and 10 or more in the diastolic BP on standing upright *MEMO as well as the post-prandial hypotension

Pathology of the Aging Heart Changes due to: • Normal Aging Processes • Superimposed Processes (i. e. endocarditis) • Residuals of other conditions (i. e. hypertension, bicuspid, aortic valve

Aging Heart • Size: can atrophy, remain unchanged or develop moderate hypertrophy. The normal aging heart demonstrates a modest in L ventricular wall thickness. Possible enlargement of the L atrium and L ventricular cavity. • Cardiac myocytes: in size, not numbers (some replaced with fibrous tissue). Cardiac myocytes effective in reentering the cell cycle & proliferating, partly offsetting cell loss due to necrosis or apoptosis. • Amyloid deposition: half of those +70 years have some amyloid deposits in the heart but mostly in small amount & confined to the atria. Amyloid is not present in all elderly persons, not even in centenarians.

Aging Heart • Vasculature (atherosclerosis) – Walls of large arteries thicken, vessels become dilated and elongated – Increase intimal thickness (due to cellular and matrix deposition) – Fragmentation of the internal elastic membrane • Cardiac output (L x min) – not decreased in healthy older men – slightly decreased in older women

Age Associated Changes in Cardiac Function 1. Overall in systolic BP due to arterial stiffening & in plus wave velocity. Reflects resetting of the baro-receptor reflex to a higher level in the elderly 2. Myocardial contractility: relaxation is prolonged in senescent cardiac muscle due the sarcoplasmic reticulum seugesters less Ca+2 3. Ejection Fraction (EF): no change in resting EF 4. Heart Rate (HR): supine HR does not change, in sitting and standing positions from 10 to 25%.

Aerobic Capacity & Cardiovascular Function During Exercise in the Elderly With age, peak exercise capacity & peak oxygen consumption slightly but inter-individual variation is substantial Aerobic capacity 50% between 20 years to 80 years: Maximal Cardiac Output (CO) 25% Peripheral O 2 utilization 25% (due to in muscle mass & strength) Although the stroke volume in older persons is maintained, age apparently blunts the Frank. Starling mechanism

Heart Failure: Cardiac Output (CO) insufficient to meet physiologic demands In the elderly, heart failure due to: • Mostly systemic arterial hypertension • Coronary artery & valvular diseases (due to impaired cardiac filling & chronic volume overload) • Combined right & left cardiac failure most common, but isolated occurrence of left or right also probable

Heart Failure in the Elderly • Symptoms: dyspnea, orthopnea, fatigue on exertion and dependent edema • Severity: classified according to the NY Heart Association Scale

The Cardiomyopathies: Myocardial disorders without a known underlying cause BUT where other heart diseases may coexist Dilated Cardiomyopathy Hyperthrophic Cardiomyopathy Restrictive Cardiomyopathy

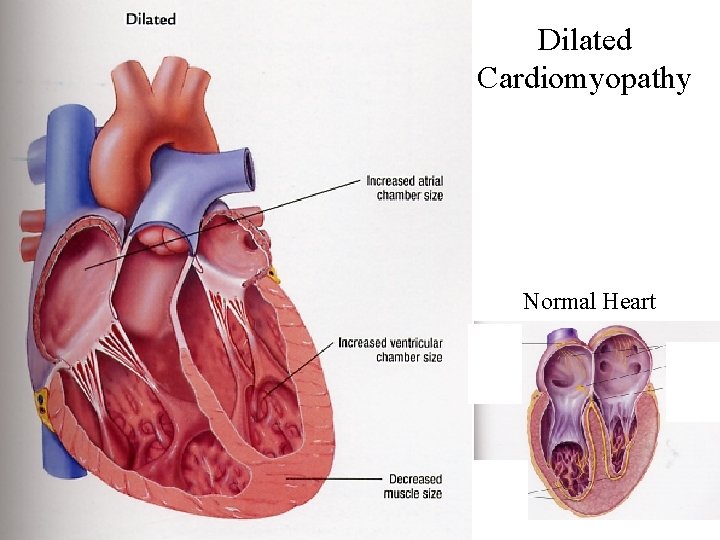
Dilated Cardiomyopathy Normal Heart

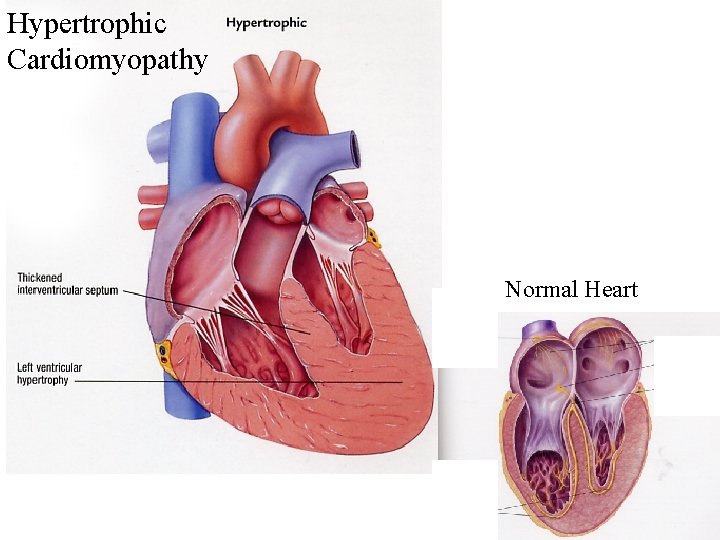
Hypertrophic Cardiomyopathy Normal Heart

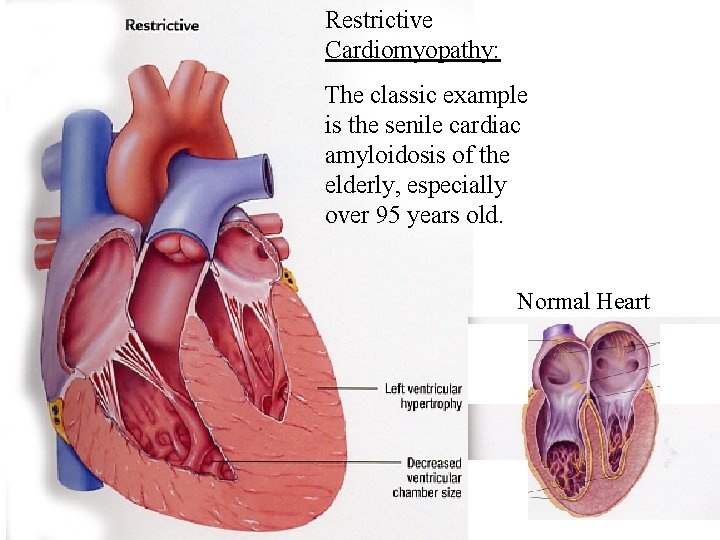
Restrictive Cardiomyopathy: The classic example is the senile cardiac amyloidosis of the elderly, especially over 95 years old. Normal Heart

Cardiomyopathy: Any heart muscle disorder not caused by coronary artery disease, hypertension or congenital valvular or pericardial diseases. Prevalence of heart failure: 25 -54 yrs: 1% 55 -65 yrs: 3% 65 -74 yrs: 4. 5% +75 yrs: 10% • > 75% of patients with heart failure +60 years of age • Primary reason is Coronary Heart Disease (CHD) • Secondary reason is Hypertension • Third reason is cardiomyopathy

Sudden Death • In young athletes (also in middle aged men), SUDDEN DEATH can occur in patients with congenital hypertrophic cardiomyopathy – Usually due to severe arrythmia (ventricular fibrillation) – If diagnosis is made a cardiac defibrillator should be implanted. • The SUDDEN DEATH of runners are usually limited to 1 case per 15, 000 runners per year-- hence, very rare. • MEMO: There is still the possibility of ANAPHYLACTIC SHOCK in runners or walkers, if stung by a bee.

Syncope in Elderly Definition: temporary suspension of conciousness due to cerebral ischemia Causes • Orthostatic Hypotension • Vaso-Vagal Reflex (? ) • Arrhythmias (brady- & tachyarrhythmias) • Drugs – Antihypertensives (vasodilators/diuretics) – Cardiac drugs: beta-blockers, digitalis, anti- arrhythmias, Ca+2 channel blockers, nitrates. – Recreational: alcohol, marijuana and cocaine. – Psychiatric: Antidepressants and phenothiazines

Contributory Causes to Heart Failure in the Elderly • • Hypertension (poor elasticity of arterial system) Alcohol, but only if in excess Viral infections Autoimmunity Heredity (specially for the cardiomyopathies) Senile amyloid Diabetes (due to the microvascular disease) Arrhythmias and especially the TACHYCARDIAS

Conduction System in Aged Heart • Sinoatrial Node: Increased fibrous tissue; seldom origin for arrythmias • Atrio-Ventricular Node: Slight increase in collagen fibers • Bundle of His: Increased fibrous tissue with higher frequency of First or Second degree heart block (the mobitz) • Also the possibility of: L or R BBB (Bundle Branch Block) -this is seldom a complete heart block. • In the conduction system fibrosis occurs: 40% – Coronary Artery Disease : 20% – Calcification : 10%

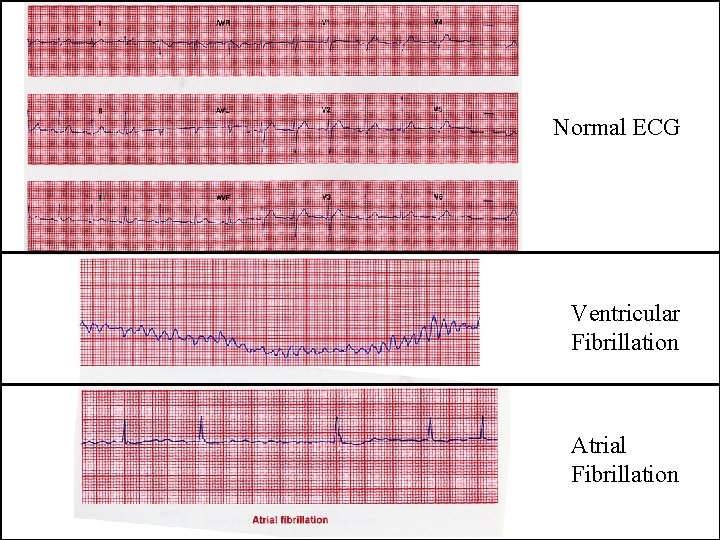
Normal ECG Ventricular Fibrillation Atrial Fibrillation

Aortic Stenosis: Narrowing of the aortic orifice of the heart or of the aorta itself A common condition due to: – Fatty alteration of collagen – Calcification – Rigidity and various degrees of aortic stenosis – Amyloid infiltration of the valves

Age Specific Lesion: The Valves • Fibrous thickening at sites of closure • Valvular sclerosis caused by collagen and elastic tissue, this is a true wear and tear phenomenon • Calcification of the mitral ring where fatty degeneration invites deposition of calcium – Calcifications is detected in 17 to 45% of patients over 90 years of age – Complications include: heart blocks, infections, embolic