34 1 Reproductive Anatomy KEY CONCEPT Female and









- Slides: 31

34. 1 Reproductive Anatomy KEY CONCEPT Female and male reproductive organs fully develop during puberty.

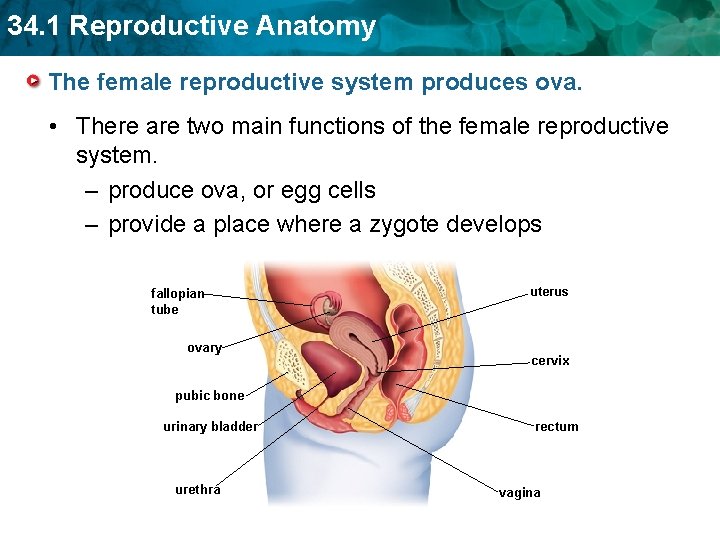
34. 1 Reproductive Anatomy The female reproductive system produces ova. • There are two main functions of the female reproductive system. – produce ova, or egg cells – provide a place where a zygote develops fallopian tube ovary uterus cervix pubic bone urinary bladder urethra rectum vagina

34. 1 Reproductive Anatomy • Estrogen has three main functions. – develop female sexual characteristics – develop eggs – prepare uterus for pregnancy

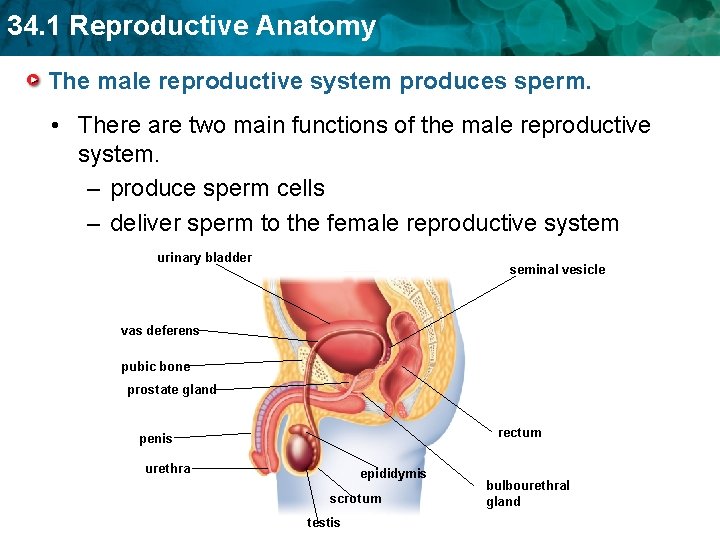
34. 1 Reproductive Anatomy The male reproductive system produces sperm. • There are two main functions of the male reproductive system. – produce sperm cells – deliver sperm to the female reproductive system urinary bladder seminal vesicle vas deferens pubic bone prostate gland rectum penis urethra epididymis scrotum testis bulbourethral gland

34. 1 Reproductive Anatomy • Testosterone has two main functions. – developing male sexual characteristics – producing sperm

34. 1 Reproductive Anatomy KEY CONCEPT 34. 2 Human reproductive processes depend on cycles of hormones.

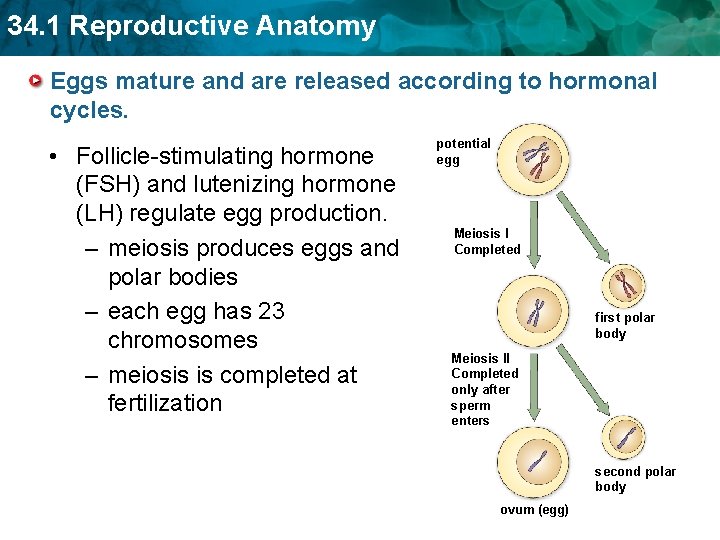
34. 1 Reproductive Anatomy Eggs mature and are released according to hormonal cycles. • Follicle-stimulating hormone (FSH) and lutenizing hormone (LH) regulate egg production. – meiosis produces eggs and polar bodies – each egg has 23 chromosomes – meiosis is completed at fertilization potential egg Meiosis I Completed first polar body Meiosis II Completed only after sperm enters second polar body ovum (egg)

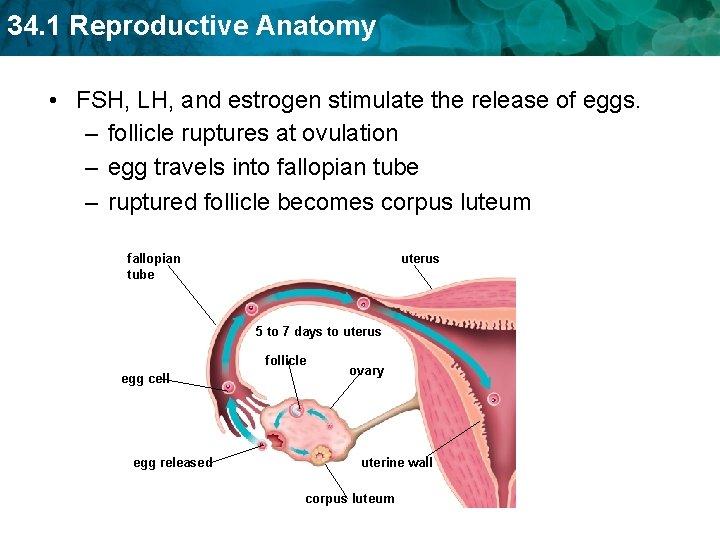
34. 1 Reproductive Anatomy • FSH, LH, and estrogen stimulate the release of eggs. – follicle ruptures at ovulation – egg travels into fallopian tube – ruptured follicle becomes corpus luteum fallopian tube uterus 5 to 7 days to uterus follicle egg cell egg released ovary uterine wall corpus luteum

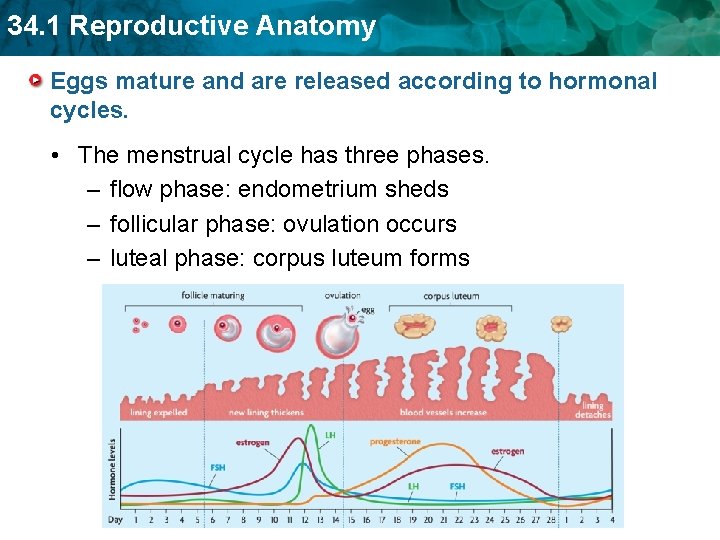
34. 1 Reproductive Anatomy Eggs mature and are released according to hormonal cycles. • The menstrual cycle has three phases. – flow phase: endometrium sheds – follicular phase: ovulation occurs – luteal phase: corpus luteum forms

34. 1 Reproductive Anatomy • The menstrual cycle stops at menopause. – cycle continues until a woman’s mid-40’s or 50’s – decline in hormone levels make cycles irregular – eventually, cycle stops altogether

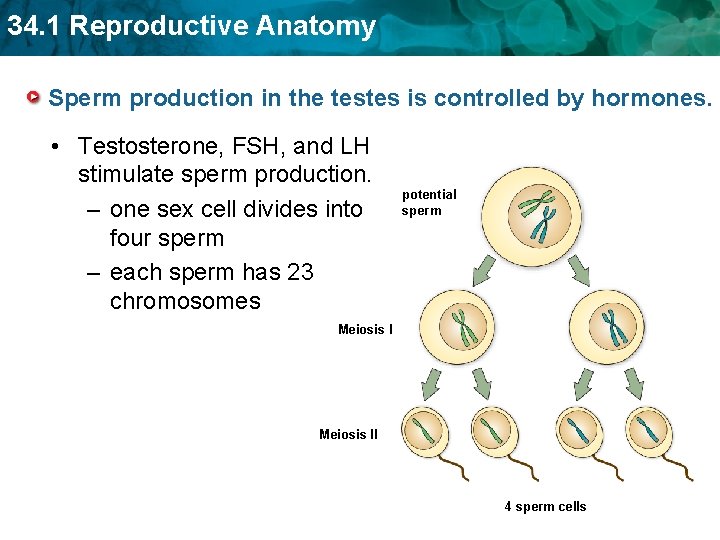
34. 1 Reproductive Anatomy Sperm production in the testes is controlled by hormones. • Testosterone, FSH, and LH stimulate sperm production. – one sex cell divides into four sperm – each sperm has 23 chromosomes potential sperm Meiosis II 4 sperm cells

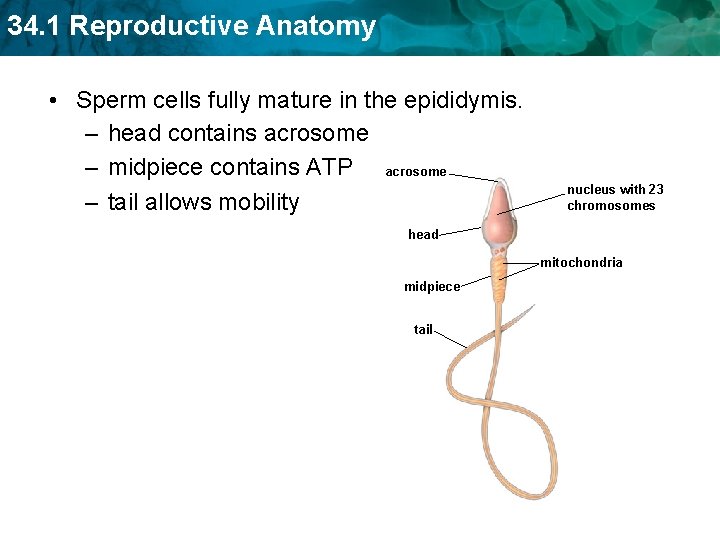
34. 1 Reproductive Anatomy • Sperm cells fully mature in the epididymis. – head contains acrosome – midpiece contains ATP acrosome – tail allows mobility nucleus with 23 chromosomes head mitochondria midpiece tail

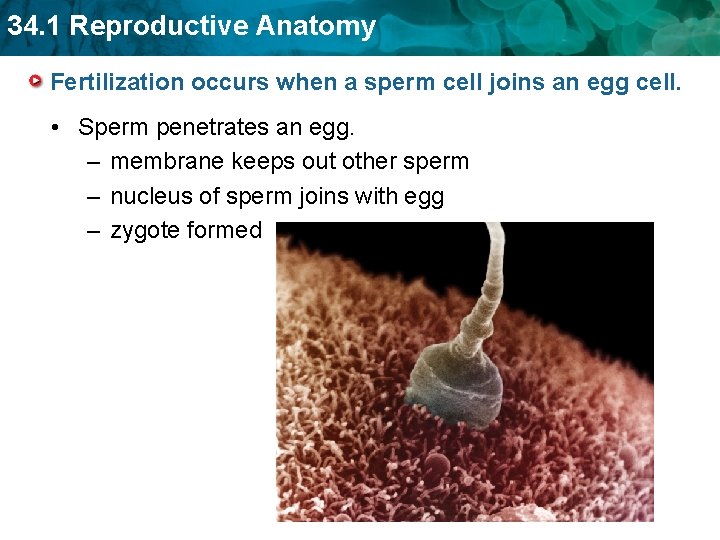
34. 1 Reproductive Anatomy Fertilization occurs when a sperm cell joins an egg cell. • Sperm penetrates an egg. – membrane keeps out other sperm – nucleus of sperm joins with egg – zygote formed

34. 1 Reproductive Anatomy • Multiple zygotes can result from fertilization. – identical twins from the same egg – fraternal twins from two separate eggs • Infertility makes reproduction difficult or impossible.

34. 1 Reproductive Anatomy Sexually transmitted diseases affect fertility and overall health. • Sexually transmitted diseases (STDs) are passed from one person to another during sexual contact. – bacterial STDs include chlamydia, syphilis, gonorrhea – viral STDs include hepatitis B, genital herpes, human papillomavirus, and HIV

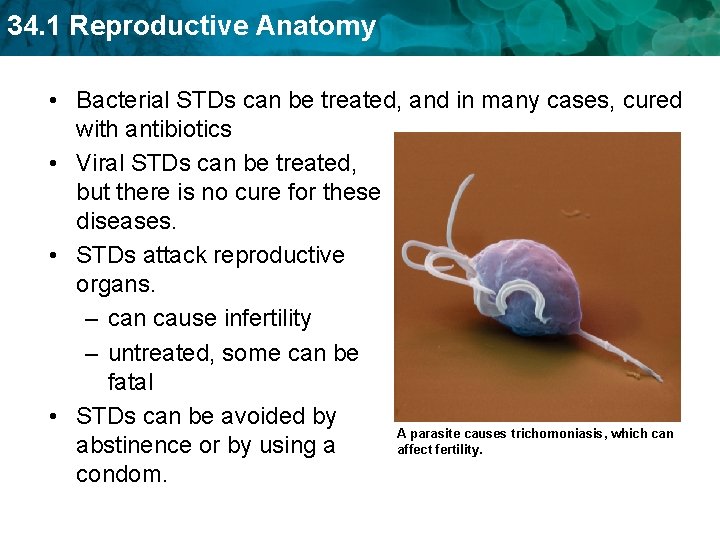
34. 1 Reproductive Anatomy • Bacterial STDs can be treated, and in many cases, cured with antibiotics • Viral STDs can be treated, but there is no cure for these diseases. • STDs attack reproductive organs. – can cause infertility – untreated, some can be fatal • STDs can be avoided by A parasite causes trichomoniasis, which can abstinence or by using a affect fertility. condom.

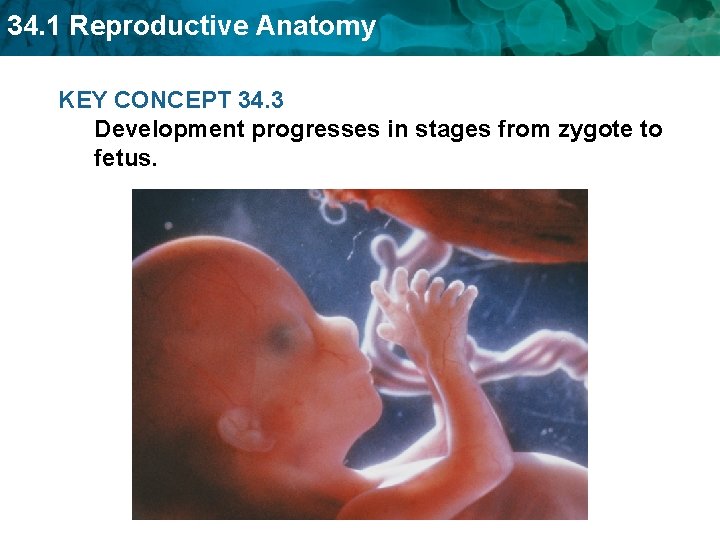
34. 1 Reproductive Anatomy KEY CONCEPT 34. 3 Development progresses in stages from zygote to fetus.

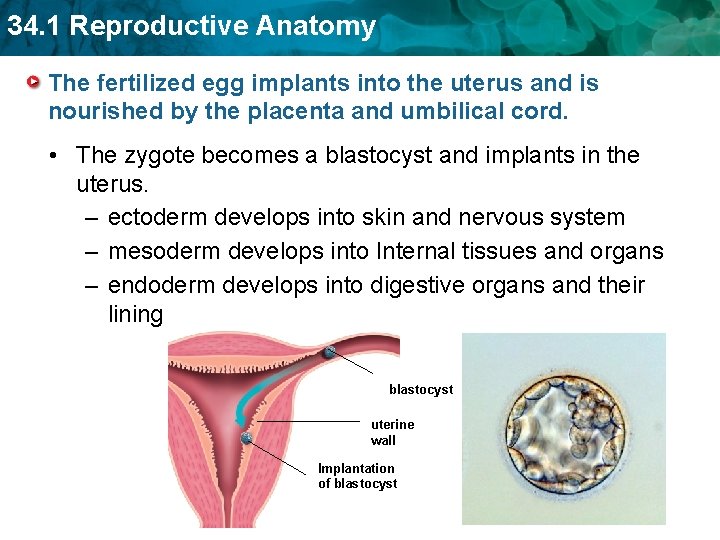
34. 1 Reproductive Anatomy The fertilized egg implants into the uterus and is nourished by the placenta and umbilical cord. • The zygote becomes a blastocyst and implants in the uterus. – ectoderm develops into skin and nervous system – mesoderm develops into Internal tissues and organs – endoderm develops into digestive organs and their lining blastocyst uterine wall Implantation of blastocyst

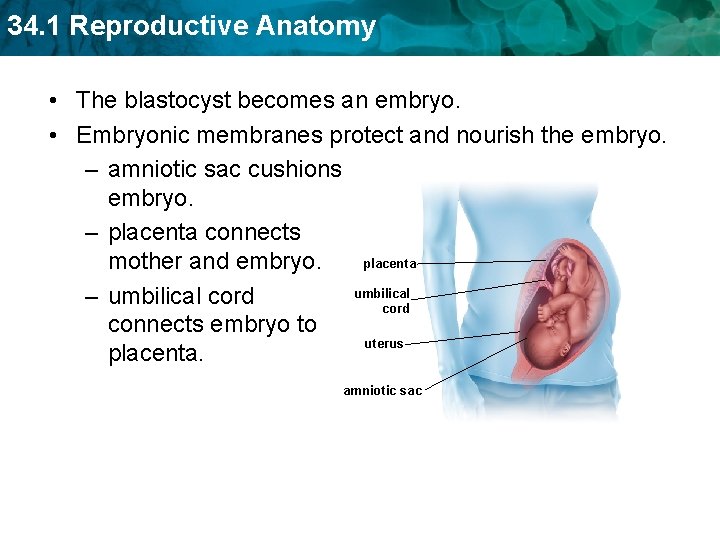
34. 1 Reproductive Anatomy • The blastocyst becomes an embryo. • Embryonic membranes protect and nourish the embryo. – amniotic sac cushions embryo. – placenta connects placenta mother and embryo. umbilical – umbilical cord connects embryo to uterus placenta. amniotic sac

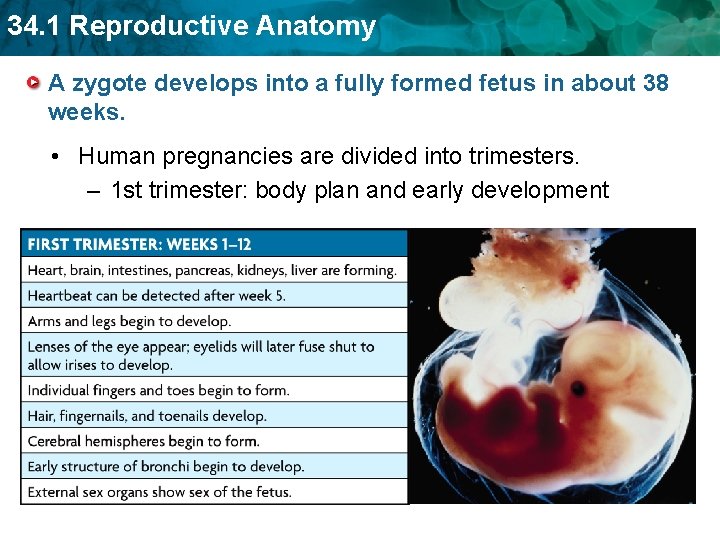
34. 1 Reproductive Anatomy A zygote develops into a fully formed fetus in about 38 weeks. • Human pregnancies are divided into trimesters. – 1 st trimester: body plan and early development

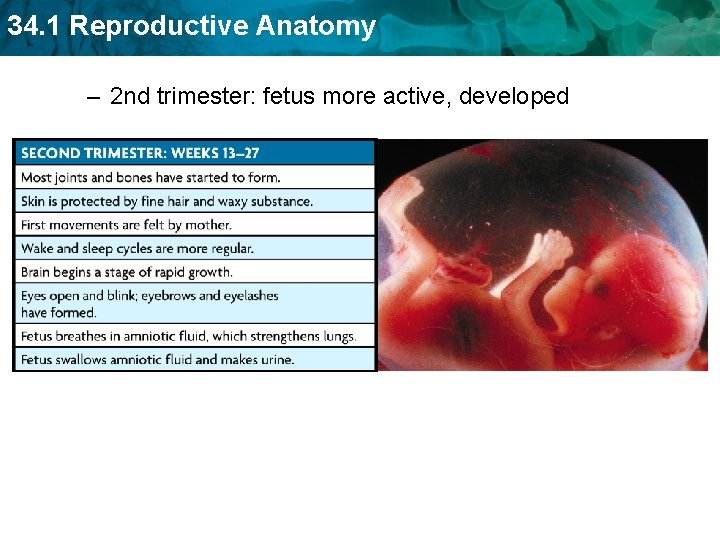
34. 1 Reproductive Anatomy – 2 nd trimester: fetus more active, developed

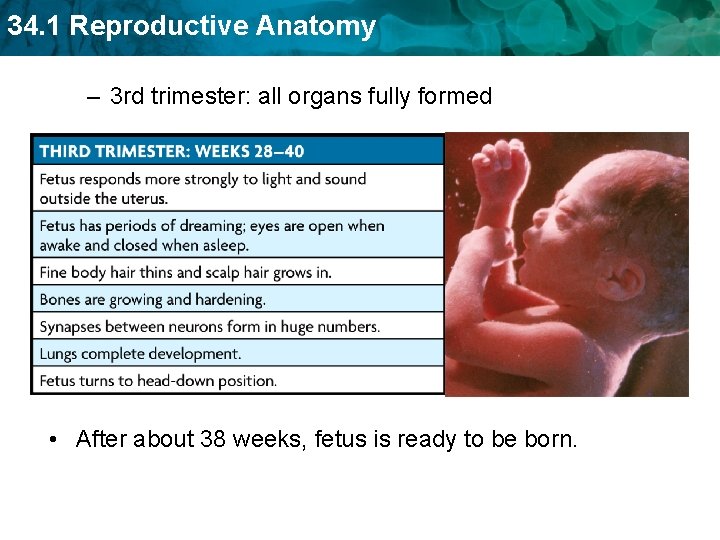
34. 1 Reproductive Anatomy – 3 rd trimester: all organs fully formed • After about 38 weeks, fetus is ready to be born.

34. 1 Reproductive Anatomy The mother affects the fetus, and pregnancy affects the mother. • The fetus depends on the mother for all its nutrition. – mother's diet must support fetal health – mother must avoid toxic chemicals

34. 1 Reproductive Anatomy • The mother’s health is affected by pregnancy in a number of ways. – increase in Calories and body weight – pregnancy hormones affecting homeostasis – regular medical checkups needed

34. 1 Reproductive Anatomy KEY CONCEPT 34. 4 Physical development continues through adolescence and declines with age.

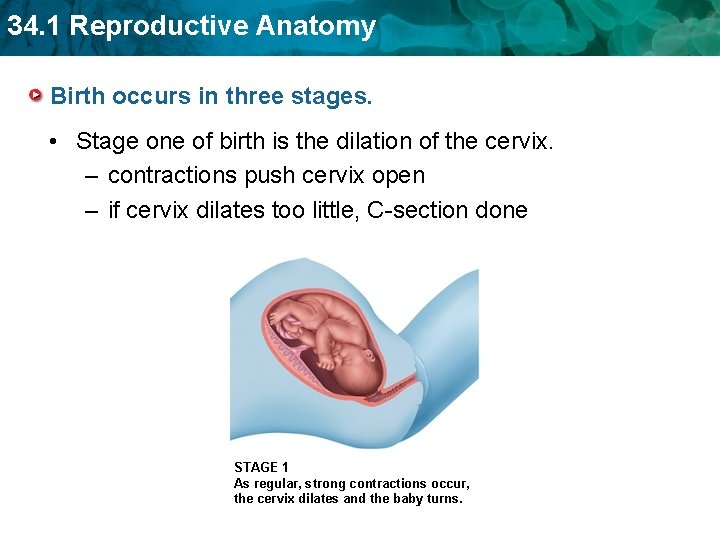
34. 1 Reproductive Anatomy Birth occurs in three stages. • Stage one of birth is the dilation of the cervix. – contractions push cervix open – if cervix dilates too little, C-section done STAGE 1 As regular, strong contractions occur, the cervix dilates and the baby turns.

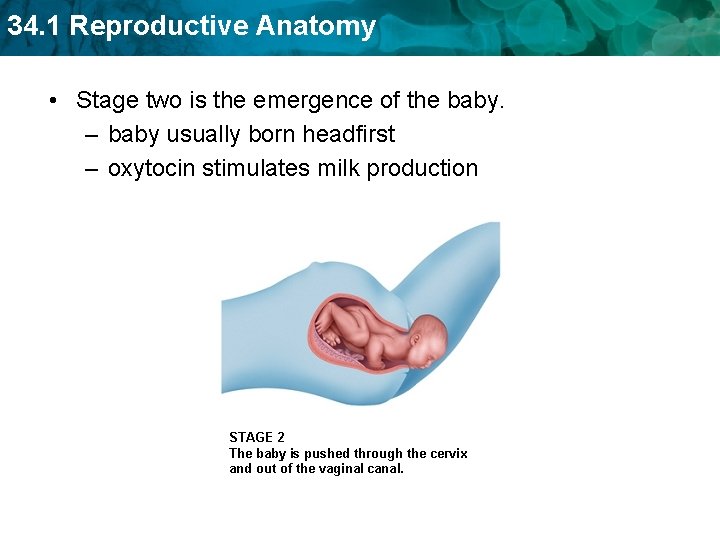
34. 1 Reproductive Anatomy • Stage two is the emergence of the baby. – baby usually born headfirst – oxytocin stimulates milk production STAGE 2 The baby is pushed through the cervix and out of the vaginal canal.

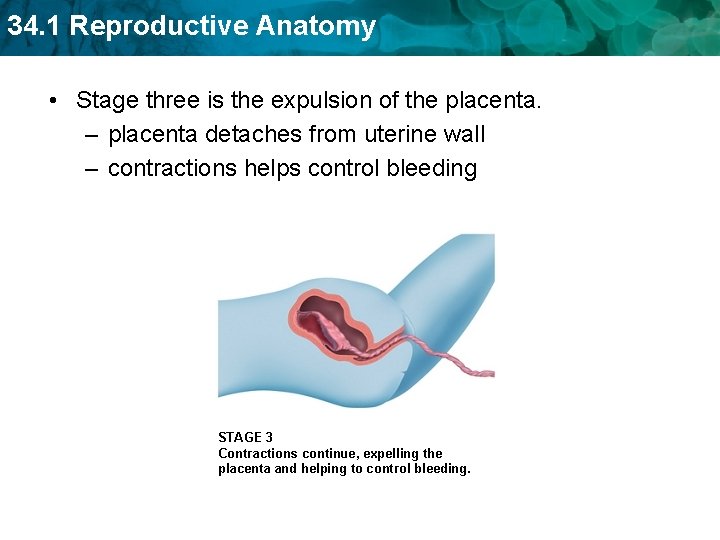
34. 1 Reproductive Anatomy • Stage three is the expulsion of the placenta. – placenta detaches from uterine wall – contractions helps control bleeding STAGE 3 Contractions continue, expelling the placenta and helping to control bleeding.

34. 1 Reproductive Anatomy Human growth and aging also occur in stages. • Genetics, hormones, lifestyle, environment affect all stages. – during infancy, growth is rapid – during childhood, motor and language skills develop

34. 1 Reproductive Anatomy • Genetics, hormones, lifestyle, environment affect all stages. – during puberty, sexually maturity begins – during adolescence, growth is rapid and the brain rewired – adulthood marks the peak of skills and independence

34. 1 Reproductive Anatomy • Aging is also affected by genetics, hormones, lifestyle, environment. • Effects of aging can be reduced with good diet, exercise, and continued learning. Jerry Peel at age 1 1/2 Jerry Peel at age 17 Jerry Peel at age 71