Joint Hospital Surgical Grand Round 17 January 2009






















- Slides: 36

Joint Hospital Surgical Grand Round 17 January 2009 Peptic Ulcer Rebleeding An Evidence-Based Management Dr Shirley Yuk-Wah Liu Department of Surgery Prince of Wales Hospital The Chinese University of Hong Kong

History of Peptic Ulcer Bleeding 1881 Theodor Billroth (1829 – 1894) Father of modern abdominal surgery First gastrectomy 1800 1950 -1980 s Introduction of endoscopy 2000 1983 Warren and Marshall Association of H pylori with peptic ulcer Warren et al. Lancet 1983 Marshall et al. Lancet 1983

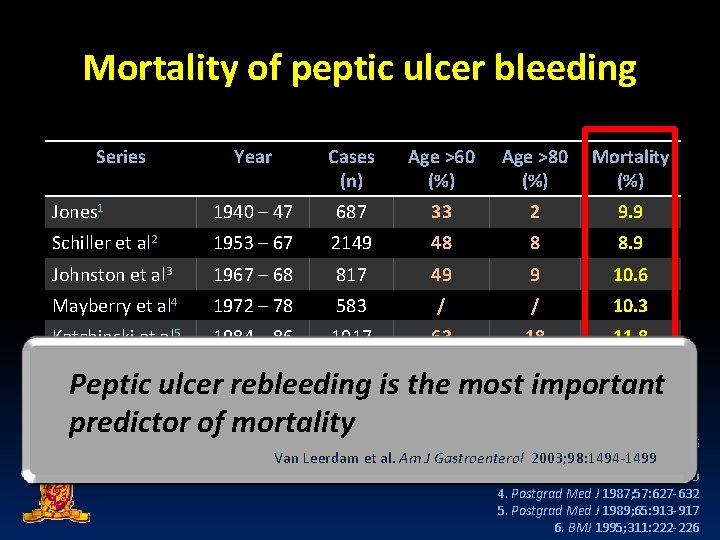
Mortality of peptic ulcer bleeding Series Year Cases (n) Age >60 (%) Age >80 (%) Mortality (%) Jones 1 1940 – 47 687 33 2 9. 9 Schiller et al 2 1953 – 67 2149 48 8 8. 9 Johnston et al 3 1967 – 68 817 49 9 10. 6 Mayberry et al 4 1972 – 78 583 / / 10. 3 Katchinski et al 5 1984 – 86 1017 63 18 11. 8 1993 4185 68 27 11. 0 Rockall et al 6 Peptic ulcer rebleeding is the most important predictor of mortality 1. BMJ 1947; 2: 441 -446 Van Leerdam et al. Am J Gastroenterol 2003; 98: 1494 -1499 2. BMJ 1970; 2: 7 -14 3. BMJ 1973; 3: 655 -660 4. Postgrad Med J 1987; 57: 627 -632 5. Postgrad Med J 1989; 65: 913 -917 6. BMJ 1995; 311: 222 -226

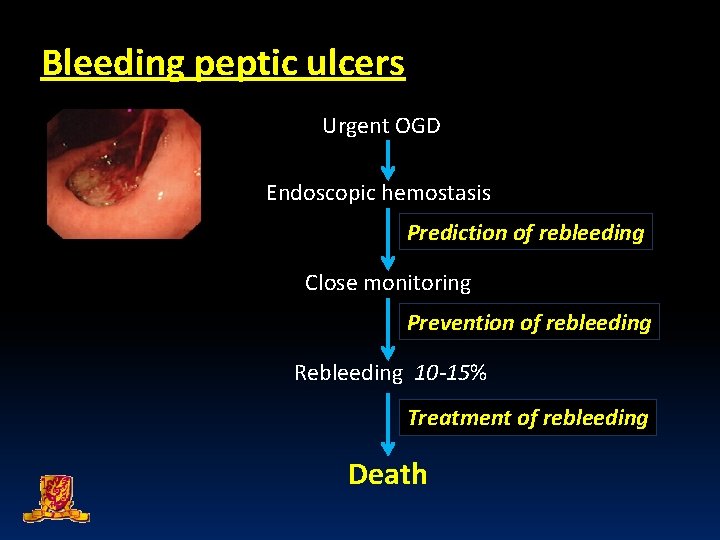
Bleeding peptic ulcers Urgent OGD Endoscopic hemostasis Prediction of rebleeding Close monitoring Prevention of rebleeding Rebleeding 10 -15% Treatment of rebleeding Death

Joint Hospital Surgical Grand Round 17 Jan 2009 Peptic Ulcer Rebleeding: An Evidence-based Management P REDICTION OF ULCER REBLEEDING

Q Who are at risk of rebleeding? 10 studies published Evaluation on factors predicting rebleeding after endoscopic hemostasis

Predictive factors of rebleeding Meta-analysis Clinical Independent predictive factors for rebleeding: 1. hemodynamic instability 2. comorbid Endoscopic illness 3. active bleeding ulcers 4. large ulcer size 5. ulcers with difficult position Elmunzer et al. Am J Gastroenterol 2008; 103: 2625 -2632

Joint Hospital Surgical Grand Round 17 Jan 2009 Peptic Ulcer Rebleeding: An Evidence-based Management P REVENTION OF ULCER REBLEEDING

To prevent ulcer rebleeding Adjunctive Acid suppressants - Scheduled second-look endoscopy Is it useful? Type of drugs: H 2 -receptor antagonists or PPI Route of administration: IV or oral Dosage: high-dose or low-dose

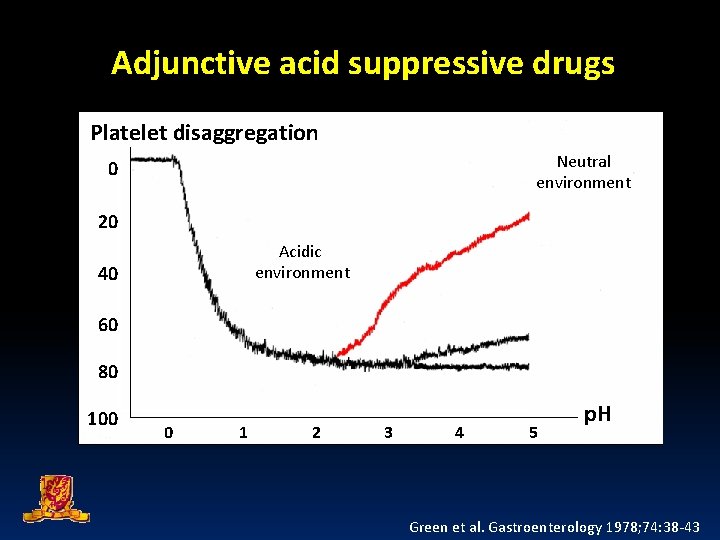
Adjunctive acid suppressive drugs Platelet disaggregation Neutral environment 0 20 Acidic environment 40 60 80 100 0 1 2 3 4 5 p. H Green et al. Gastroenterology 1978; 74: 38 -43

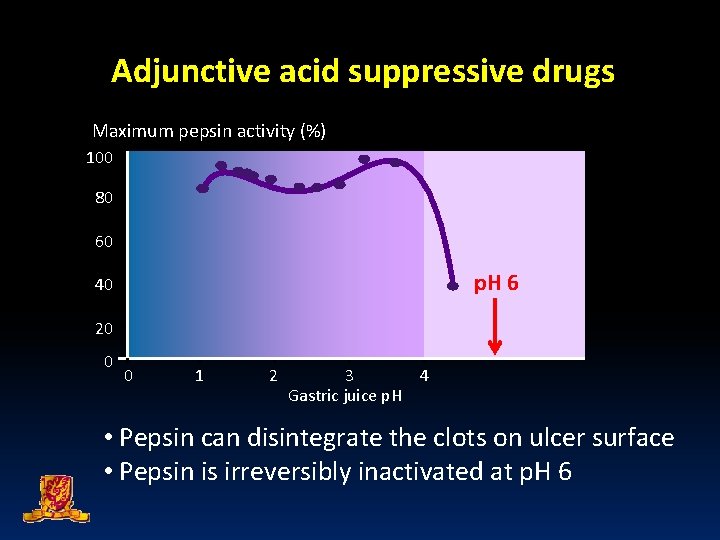
Adjunctive acid suppressive drugs Maximum pepsin activity (%) 100 80 60 p. H 6 40 20 0 0 1 2 3 4 Gastric juice p. H • Pepsin can disintegrate the clots on ulcer surface • Pepsin is irreversibly inactivated at p. H 6

Q 1. Is acid suppressive drugs useful? 24 RCT published Comparison of PPI to placebo in preventing rebleeding

First RCT on PPI vs placebo Daneshmend et al. Br Med J 1992; 304: 143 -147

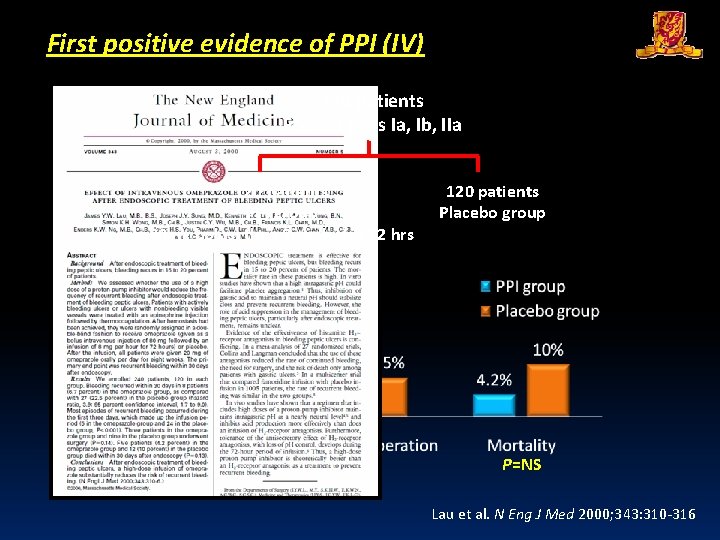
First positive evidence of PPI (IV) 240 patients Forrest class Ia, Ib, IIa 120 patients PPI group 80 mg bolus, then 8 mg/hr for 72 hrs P<0. 001 P=NS 120 patients Placebo group P=NS Lau et al. N Eng J Med 2000; 343: 310 -316

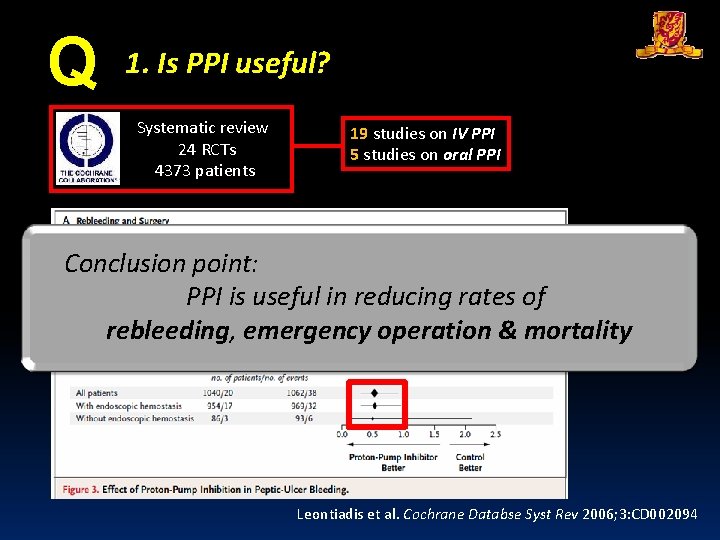
Q 1. Is PPI useful? Systematic review 24 RCTs 4373 patients 19 studies on IV PPI 5 studies on oral PPI Conclusion point: PPI is useful in reducing rates of rebleeding, emergency operation & mortality Leontiadis et al. Cochrane Databse Syst Rev 2006; 3: CD 002094

Q 2. Should we give PPI or H 2 R antagonists? 11 RCT published Comparison of PPI to H 2 R antagonists as adjunctive treatment to bleeding ulcers Meta-analysis 11 RCT PPI 681 patients H 2 R antagonist 671 patients Gisbert et al. Aliment Pharmacol Ther 2001; 15: 917 -926

Q 2. Should we give PPI or H 2 R antagonists? mortality operation Comparison on emergency rebleeding Conclusion point PPI is more superior to H 2 R antagonists in reducing the rates of rebleeding and emergency operation Gisbert et al. Aliment Pharmacol Ther 2001; 15: 917 -926

Q 3. What should be the best route of administration? 0 RCT published No RCT performed on direct comparison of oral versus IV PPI

Q 3. What should be the best route of administration? Oral PPI IV PPI 5 trials 658 patients 19 trials 3714 patients Meta-regression analysis: Evidence is still on inconclusive No difference - Rebleeding which route is better - Emergency operation - Mortality of Leontiadis et al. Cochrane Databse Syst Rev 2006; 3: CD 002094

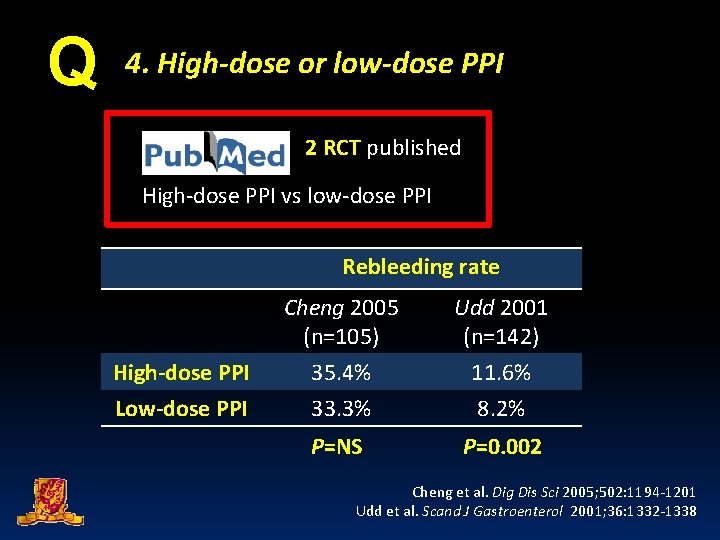
Q 4. High-dose or low-dose PPI 2 RCT published High-dose PPI vs low-dose PPI Rebleeding rate High-dose PPI Low-dose PPI Cheng 2005 (n=105) Udd 2001 (n=142) 35. 4% 33. 3% 11. 6% 8. 2% P=NS P=0. 002 Cheng et al. Dig Dis Sci 2005; 502: 1194 -1201 Udd et al. Scand J Gastroenterol 2001; 36: 1332 -1338

Q 4. High-dose or low-dose PPI High-dose PPI 80 mg IV bolus then 8 mg/hr infusion 6 trials 2320 patients Low-dose PPI Oral PPI or IV PPI dose <120 mg/day 18 trials 2052 patients Conclusion point: Emergency surgery Rebleeding High-dose PPI bereduced the recommended 36/1149 (3. 1%) 59/1171 (5. 0%) Both should significantly Only high-dose PPIbleeding significantly reduce the need dosage for peptic ulcer OR=0. 61, 95% C. I. 0. 40 -0. 93, P=0. 02 Leontiadis et al. Cochrane Databse Syst Rev 2004; 3: CD 002094

To prevent ulcer rebleeding Adjunctive Acid suppressants Scheduled second-look endoscopy Is it useful ?

Scheduled second-look endoscopy Rationale – To treat before clinical rebleeding occurs – To perform second-look OGD within 16 – 24 hours after primary endoscopic hemostasis Villanueva et al. Gastrointest Endosc 1994; 40: 34 -39 Saeed et al. Endoscopy 1996; 28: 288 -294 Rutgeerts et al. Lancet 1997; 350: 692 -696 Messmann et al. Endoscopy 1998; 30: 583 -589 Chiu et al. Gut 2003; 52: 1403 -1407

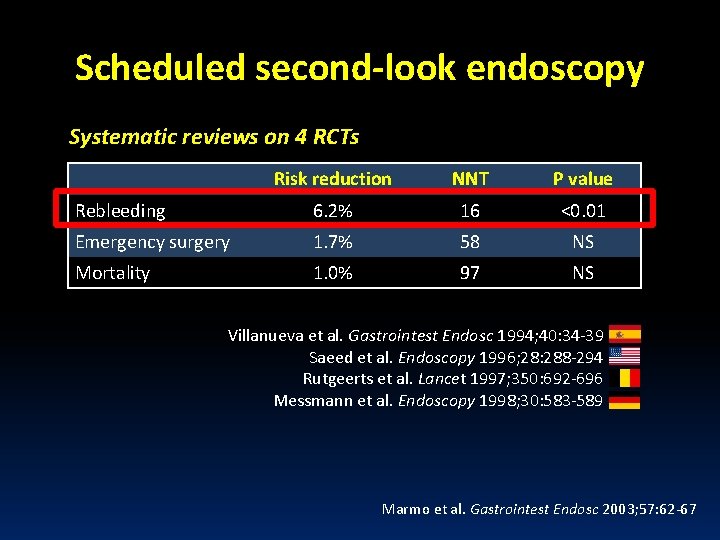
Scheduled second-look endoscopy Systematic reviews on 4 RCTs Risk reduction NNT P value Rebleeding 6. 2% 16 <0. 01 Emergency surgery 1. 7% 58 NS Mortality 1. 0% 97 NS Villanueva et al. Gastrointest Endosc 1994; 40: 34 -39 Saeed et al. Endoscopy 1996; 28: 288 -294 Rutgeerts et al. Lancet 1997; 350: 692 -696 Messmann et al. Endoscopy 1998; 30: 583 -589 Marmo et al. Gastrointest Endosc 2003; 57: 62 -67

Scheduled second look endoscopy Forrest class Ia to IIb bleeding ulcers Conclusion point: Second-look endoscopy can prevent rebleeding P=0. 03 P=0. 05 P=NS Chiu et al. Gut 2003; 52: 1403 -1407

Joint Hospital Surgical Grand Round 17 Jan 2009 Peptic Ulcer Rebleeding: An Evidence-based Management T REATMENT OF ULCER REBLEEDING

Q How to treat rebleeding? A. Endoscopic re-treatment B. Immediate surgery C. Angiographic embolization What is the best treatment option? What type of emergency operations to perform?

Q Surgery vs endoscopic re-treatment - 1169 patients with bleeding ulcers requiring endoscopic hemostasis - 92 patients (8. 7%) developed rebleeding 1 RCT published P=0. 03 P=0. 27 P=0. 59 P=0. 16 P=0. 37 Lau et al. N Eng J Med 1999; 340: 751 -756

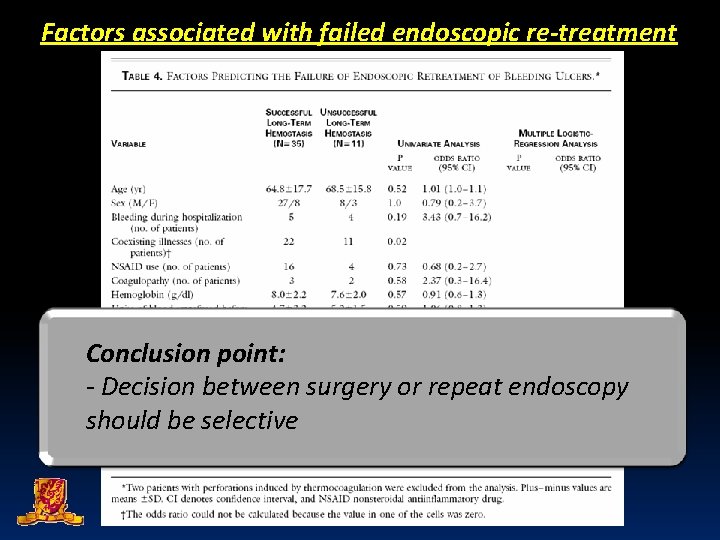
Factors associated with failed endoscopic re-treatment Conclusion point: - Decision between surgery or repeat endoscopy should be selective

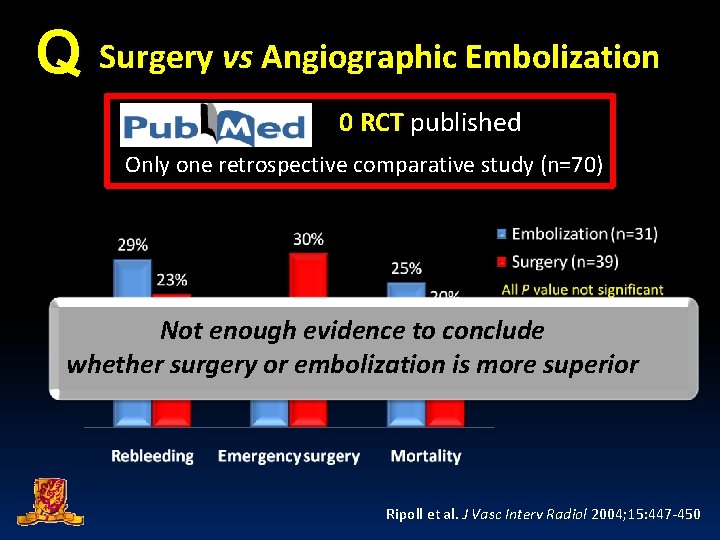
Q Surgery vs Angiographic Embolization 0 RCT published Only one retrospective comparative study (n=70) Not enough evidence to conclude whether surgery or embolization is more superior Ripoll et al. J Vasc Interv Radiol 2004; 15: 447 -450

Q Angiographic embolization vs endoscopic re-treatment 0 RCT published No RCT evidence to compare angiographic embolization to repeat endoscopy

Q What type of surgery to do? Conservative surgery Definitive surgery - Ulcer plication - Ulcer excision - Vagotomy +/- drainage - Partial gastrectomy Stop bleeding Prevent rebleeding 2 RCT published Lau et al. Best Pract Res Clin Gastroenterol 2000; 14: 505 -518

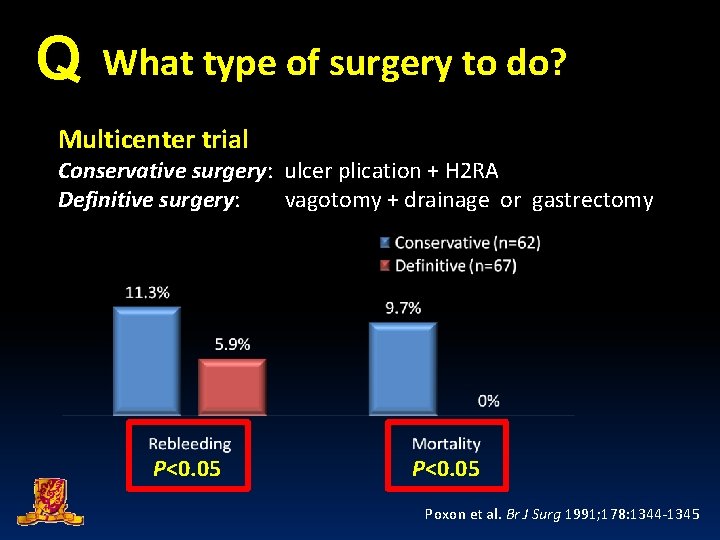
Q What type of surgery to do? Multicenter trial Conservative surgery: ulcer plication + H 2 RA Definitive surgery: vagotomy + drainage or gastrectomy P<0. 05 Poxon et al. Br J Surg 1991; 178: 1344 -1345

Q What type of surgery to do? French Association of Surgical Research trial [1978 -1988] Conservative surgery: ulcer plication + vagotomy Definitive surgery: gastrectomy Results before the era of PPI may not be reliable P<0. 05 Millat et al. World J Surg 1993; 17: 568 -573

Conclusion High-dose IV PPI infusion is useful in reducing rebleeding, emergency operation and mortality Second-look endoscopy is useful in preventing rebleeding in high-risk patients Both endoscopic re-treatment and surgery should be selectively applied to rebleeding patients The choice between conservative and definitive Surgery is still controversial

Department of Surgery The Chinese University of Hong Kong