Prevention of Venous Thromboembolism in Nonorthopedic Surgical Patients

Prevention of Venous Thromboembolism in Nonorthopedic Surgical Patients ----Antithrombotic Therapy and Prevention of Thrombosis, 9 th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines Copyright: American College of Chest Physicians 2012 ©

Learning Objectives • Describe a formal methodology for the evidencebased development of clinical practice guidelines • Review select studies of venous thromboembolism (VTE) prevention in surgical patients, as well as the limitations of the studies • Summarize recommendations for VTE prevention in specific surgical populations

VTE • Thrombosis: the formation or presence of a blood clot within a blood vessel Merriam-Webster’s Medical Dictionary • Embolism: obstruction or occlusion of a vessel by a transported clot or vegetation, a mass of bacteria, or other … material Stedman’s Medical Dictionary
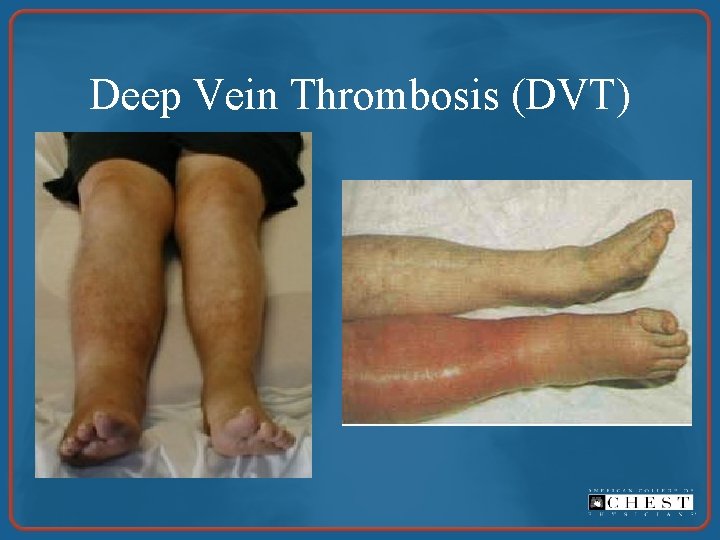
Deep Vein Thrombosis (DVT)
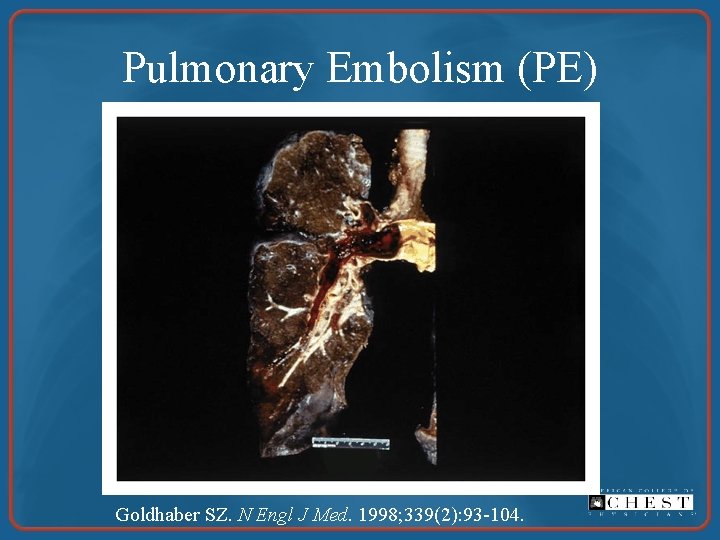
Pulmonary Embolism (PE) Goldhaber SZ. N Engl J Med. 1998; 339(2): 93 -104.
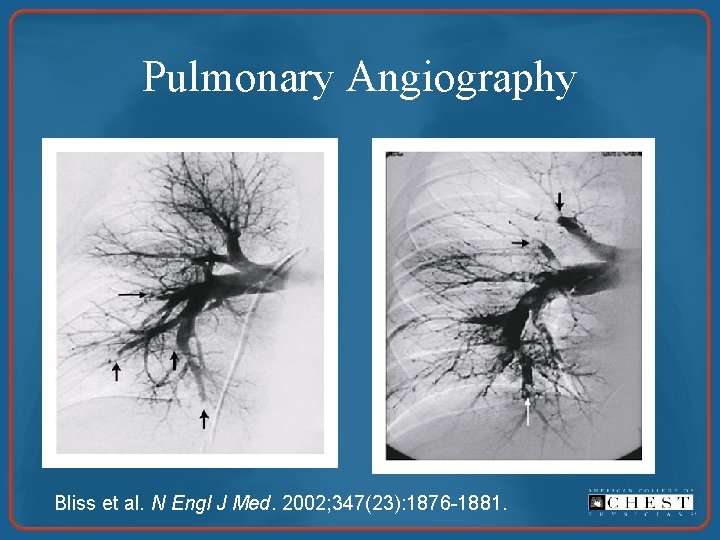
Pulmonary Angiography Bliss et al. N Engl J Med. 2002; 347(23): 1876 -1881.
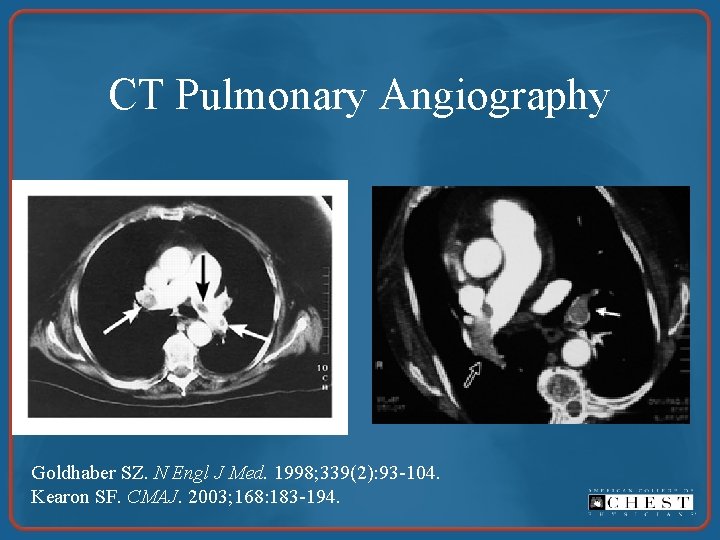
CT Pulmonary Angiography Goldhaber SZ. N Engl J Med. 1998; 339(2): 93 -104. Kearon SF. CMAJ. 2003; 168: 183 -194.

Risk Factors: Virchow’s Triad • Stasis – Immobility – Congestive heart failure • Injury – Surgery (especially major orthopedic and pelvic) – Trauma • Thrombophilia – Cancer – Oral contraceptives – Hereditary states (factor V Leiden, PT mutations)

VTE Epidemiology • Most common cause of preventable death in hospitalized patients • Risk of fatal perioperative PE ~0. 8% International Multicentre Trial. Lancet. 1975 • 150, 000 to 200, 000 deaths per year; ~1/3 in perioperative patients Horlander et al. Arch Intern Med. 2003; 163: 1711 -1717. • AHRQ: VTE prevention is number 1 priority to improve safety in hospitals

Many Surgical Patients At-Risk • 2003 Nationwide Inpatient Sample • Adult surgical patients, LOS ≥ 2 days • 7. 8 million surgical discharges • • 44% low risk 15% moderate risk 24% high risk 17% very high risk • 4. 4 million at risk for VTE Anderson et al. Am J Hematol. 2007; 82: 777 -782.

Million Women Study • Population-based, prospective cohort study • 947, 454 middle-aged women in U. K. enrolled between 1996 -2001 • Mean follow-up 6. 2 years • 239, 614 underwent surgery – 5, 419 readmitted for VTE within 12 weeks of inpatient surgery – 270 deaths from fatal PE Sweetland et al. BMJ. 2009; 339: b 4583.
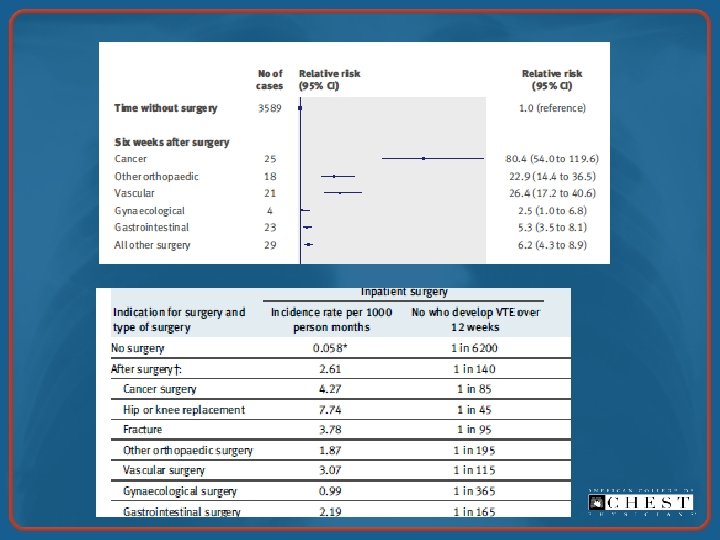

VTE Consequences • • Leg swelling, discomfort (DVT) Dyspnea, chest pain, hemoptysis, hypoxemia (PE) Extended hospital LOS Fatal PE (RV failure) ≥ 3 months of anticoagulant treatment Postphlebitic syndrome Chronic thromboembolic pulmonary HTN (~4%) Pengo et al. N Engl J Med. 2004; 350: 2257 -2264.
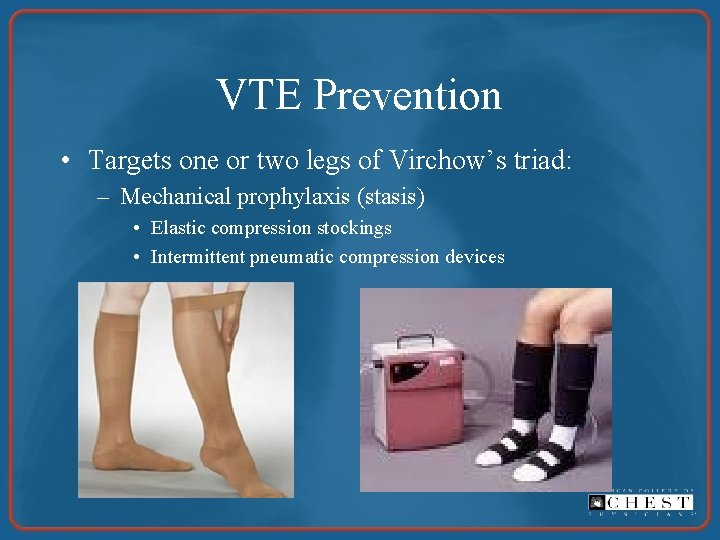
VTE Prevention • Targets one or two legs of Virchow’s triad: – Mechanical prophylaxis (stasis) • Elastic compression stockings • Intermittent pneumatic compression devices

VTE Prevention • Targets one or two legs of Virchow’s triad: – Mechanical prophylaxis (stasis) • Elastic compression stockings • Intermittent pneumatic compression devices – Pharmacological prophylaxis (hypercoagulability) • • Unfractionated heparin Low-molecular-weight heparins Fondaparinux Aspirin (? )

Guidelines Defined “Systematically developed statements to assist practitioners and patient decisions about appropriate health care for specific circumstances. ” Field MJ, Lohr KN (eds). Clinical Practice Guidelines: Directions for a New Program. Institute of Medicine, Washington, DC: National Academy Press, 1990.

Guidelines and Performance Measures • Public reporting – Cardiac surgery outcomes in New York State • Pay for performance – Reward “good” behavior – CMS: several VTE prevention P 4 P measures • Registries – Accreditation – Facilitate quality improvement

Case Scenario • 50 year-old woman scheduled to undergo elective laparoscopic cholecystectomy – – PMH notable for moderate emphysema No personal or family history of VTE Medications: Spiriva®, albuterol Stopped smoking 1 year ago • What should we recommend for perioperative VTE prophylaxis in this patient?

BMJ. 1999; 318: 593 -596.

Conceptual Framework • VTE pharmacoprophylaxis involves a tradeoff between preventing thrombosis and causing bleeding • When making tradeoffs, need to compare absolute risks of thrombosis and bleeding • In order to determine absolute risks (eg, number of symptomatic DVTs prevented), need to know the following: – Baseline risk in control/comparison group – Relative risk for intervention vs control • When making tradeoffs, also need to assign values to events being compared
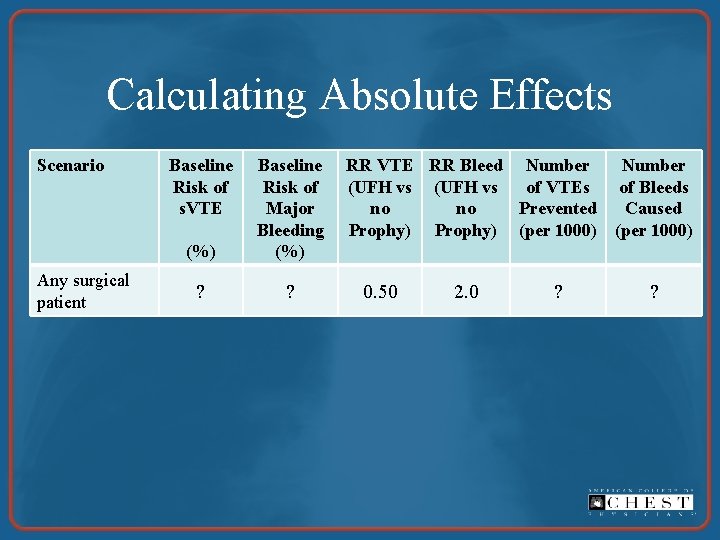
Calculating Absolute Effects Scenario Any surgical patient Baseline Risk of s. VTE (%) Baseline Risk of Major Bleeding (%) ? ? RR VTE RR Bleed Number (UFH vs of VTEs of Bleeds no no Prevented Caused Prophy) (per 1000) 0. 50 2. 0 ? ?
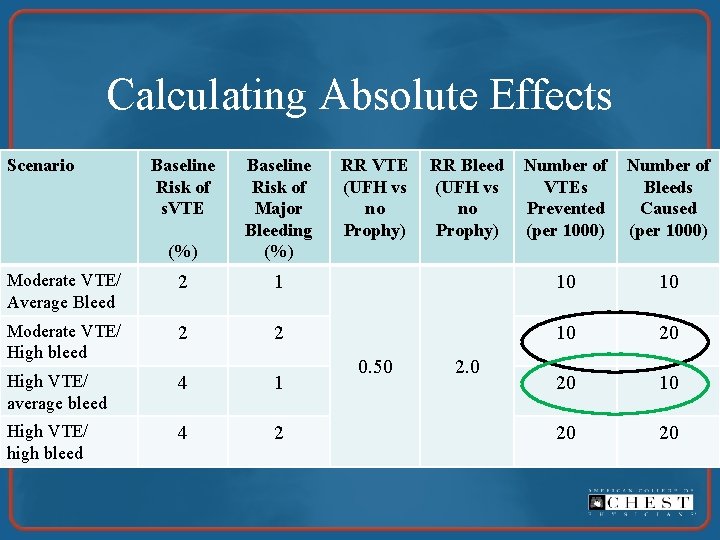
Calculating Absolute Effects Scenario Baseline Risk of s. VTE (%) Baseline Risk of Major Bleeding (%) RR VTE (UFH vs no Prophy) Moderate VTE/ Average Bleed 2 1 10 10 Moderate VTE/ High bleed 2 2 10 20 High VTE/ average bleed 4 1 20 10 High VTE/ high bleed 4 2 20 20 0. 50 RR Bleed (UFH vs no Prophy) 2. 0 Number of VTEs Prevented (per 1000) Number of Bleeds Caused (per 1000)

PICO Question • Among patients undergoing elective abdominal surgery, should LDUH vs no prophylaxis be used for VTE prevention? • Are we confident that the benefits of reducing fatal and nonfatal VTE exceed the harms of increasing fatal and nonfatal major bleeding?

Evidence Synthesis • Systematic Review for each PICO! – – Literature search Assessment for eligibility Assessment of study quality Data abstraction and synthesis • Expensive, time-consuming, and labor-intensive – AHRQ Evidence-Based Practice Centers

Assessment of Baseline Risk Ideal study Most studies • Large, population-based • Prospective (? ) • Few exclusions or losses to follow-up • Well-defined endpoints • • Single center Referral center bias Prospective Employ surveillance methods to identify asymptomatic DVT – Important to patients – Objectively confirmed • Short time horizon • Sufficiently long time horizon • No description or • No prophylaxis or controlled for adjustment for prophylaxis

Estimating Baseline Risk Ann Surg. 2010; 251: 344 -350.

Estimating Baseline Risk • Retrospective, observational study • Large sample (n=8, 216) of consecutively admitted “general” surgical inpatients • Tertiary center • Measured clinically suspected, objectively confirmed VTE over 30 days • Risk stratification according to patient-specific and procedure-specific characteristics • Prophylaxis nonuniform but reported
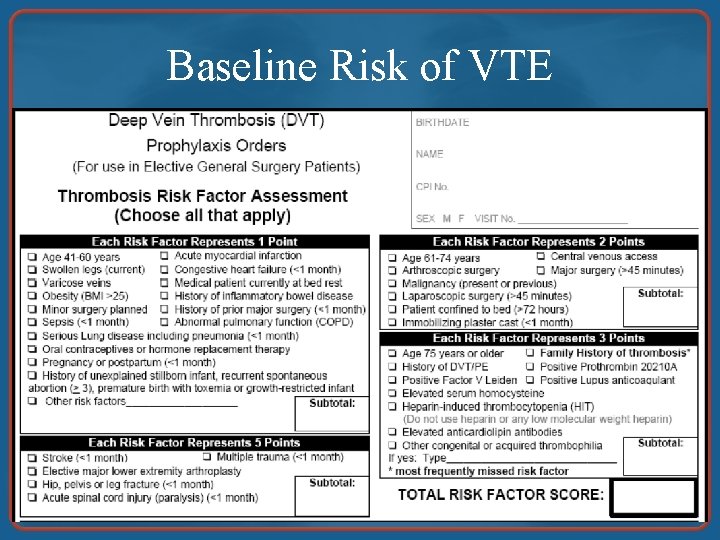

Baseline Risk of VTE

Case Scenario • 50 -year-old woman scheduled to undergo elective laparoscopic cholecystectomy – – PMH notable for moderate COPD No personal or family history of VTE Medications: Spiriva®, albuterol Stopped smoking 1 year ago • What should we recommend for perioperative VTE prophylaxis in this patient?
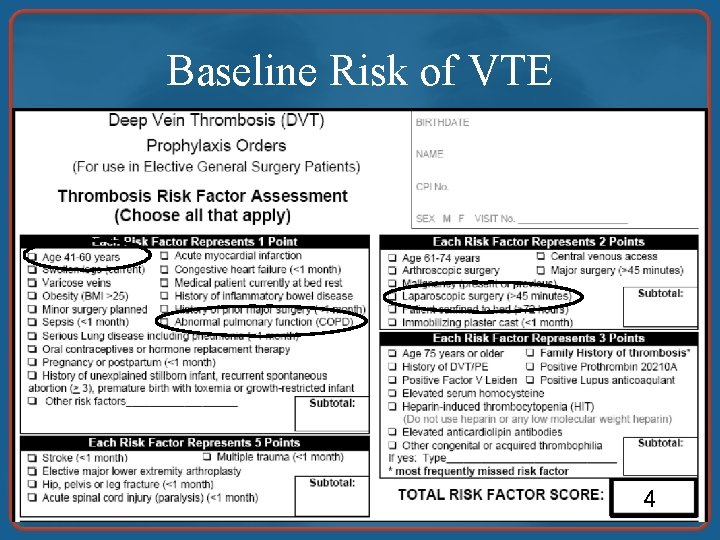

Baseline Risk of VTE 4
Baseline Risk of VTE Bahl et al. Ann Surg. 2010; 251: 344 -350.
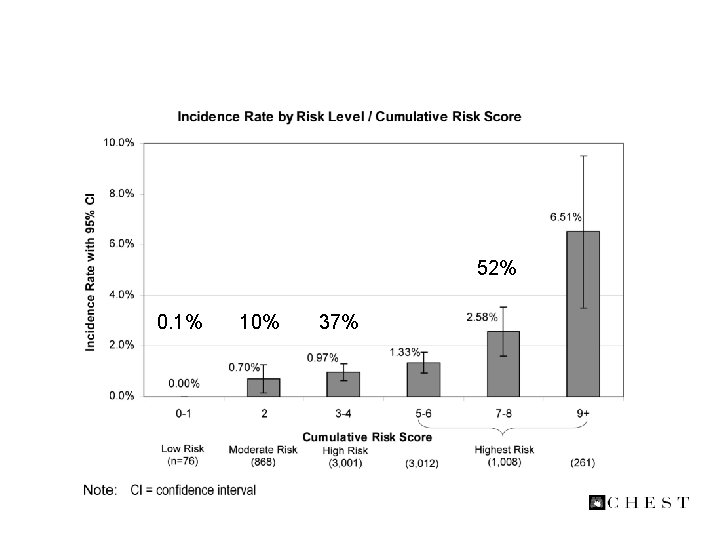
Baseline Risk of VTE 52% 0. 1% 10% 37% Bahl et al. Ann Surg. 2010; 251: 344 -350.
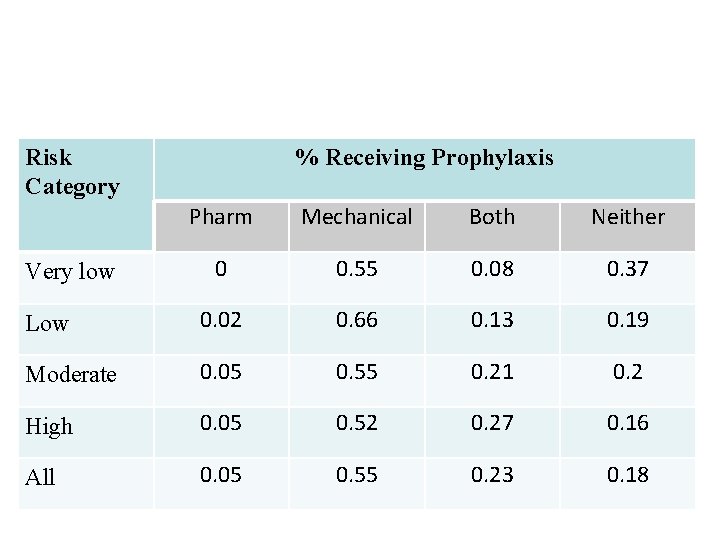
Prophylaxis Received Risk Category % Receiving Prophylaxis Pharm Mechanical Both Neither 0 0. 55 0. 08 0. 37 Low 0. 02 0. 66 0. 13 0. 19 Moderate 0. 05 0. 55 0. 21 0. 2 High 0. 05 0. 52 0. 27 0. 16 All 0. 05 0. 55 0. 23 0. 18 Very low
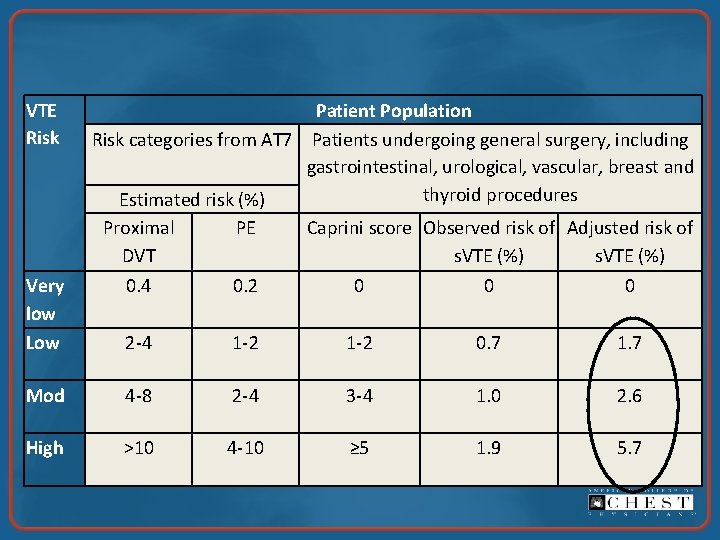
VTE Risk Patient Population Risk categories from AT 7 Patients undergoing general surgery, including gastrointestinal, urological, vascular, breast and thyroid procedures Estimated risk (%) Proximal PE Caprini score Observed risk of Adjusted risk of DVT s. VTE (%) Very low Low 0. 4 0. 2 0 0 0 2 -4 1 -2 0. 7 1. 7 Mod 4 -8 2 -4 3 -4 1. 0 2. 6 High >10 4 -10 ≥ 5 1. 9 5. 7

Estimated Baseline Risk • Caprini score = 4 • Unadjusted risk = 1. 0% • Crude adjusted risk = 2. 6% • Observed, unadjusted risk in observational study of 2, 274 discharges following lap chole in California, 1992 -1996 was 0. 9% White RH et al. Thromb Haemost. 2003; 90: 446 -455.
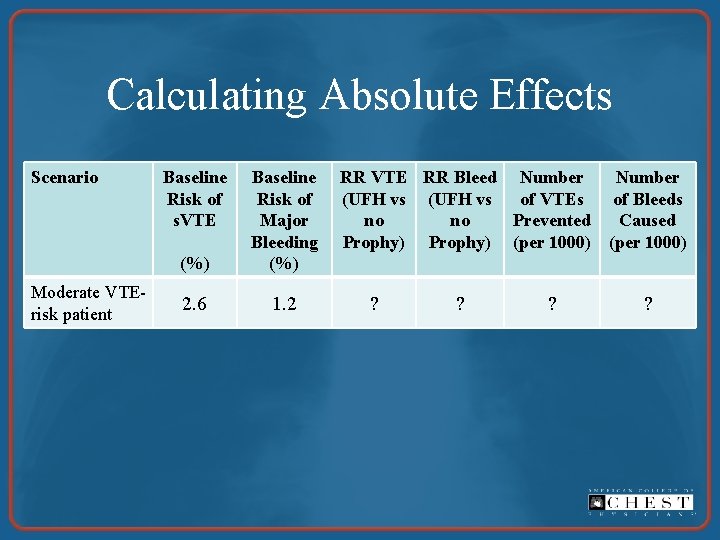
Calculating Absolute Effects Scenario Moderate VTErisk patient Baseline Risk of s. VTE (%) Baseline Risk of Major Bleeding (%) 2. 6 1. 2 RR VTE RR Bleed Number (UFH vs of VTEs of Bleeds no no Prevented Caused Prophy) (per 1000) ? ?

Assessment of Safety/Effectiveness Ideal study Most studies • Large, multicenter RCT • Blinding of patients, treating physicians, adjudicators • Well-defined endpoints • • – Important to patients – Objectively confirmed • Few exclusions or losses to follow-up • Sufficiently long time horizon Small, single center Referral center bias Incomplete blinding Surrogate outcome, asymptomatic DVT • Large percent excluded from efficacy evaluation • Short time horizon

Effectiveness of LDUH: IMT

IMT Design • Unblinded, randomized, controlled trial • Patients: adults age > 40 years undergoing major elective surgery (GA, >30 min, LOS ≥ 7 days) at 28 centers in Europe, Australia and South Africa • Intervention: UFH 5, 000 units tid for 7 days, 1 st dose 2 hours pre-op • Comparator: no prophylaxis • Outcomes: fatal PE, fatal bleed, nonfatal PE, nonfatal bleed, clinical DVT, DVT by FUT

IMT Outcomes • PE: clinically suspected with confirmatory evidence recorded (chest radioraph and ECG) • Fatal PE: confirmed by autopsy • DVT: – Clinically suspected and confirmed by venography – Continuous surveillance by fibrinogen uptake test (10 centers) • Excessive operative bleeding (surgeon’s judgment) • Wound hematoma, transfusion, fall in Hgb
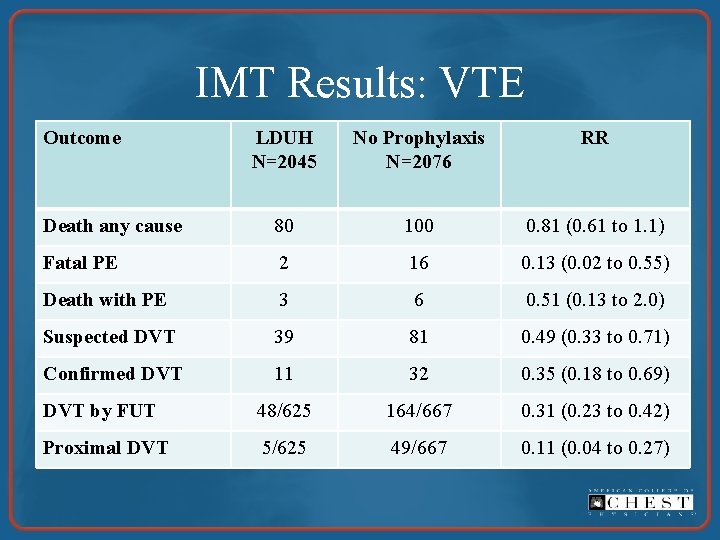
IMT Results: VTE Outcome LDUH N=2045 No Prophylaxis N=2076 RR Death any cause 80 100 0. 81 (0. 61 to 1. 1) Fatal PE 2 16 0. 13 (0. 02 to 0. 55) Death with PE 3 6 0. 51 (0. 13 to 2. 0) Suspected DVT 39 81 0. 49 (0. 33 to 0. 71) Confirmed DVT 11 32 0. 35 (0. 18 to 0. 69) DVT by FUT 48/625 164/667 0. 31 (0. 23 to 0. 42) Proximal DVT 5/625 49/667 0. 11 (0. 04 to 0. 27)
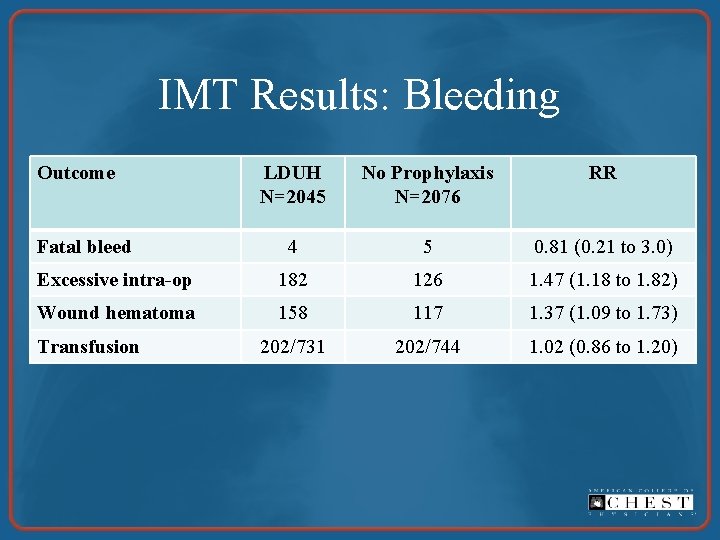
IMT Results: Bleeding Outcome LDUH N=2045 No Prophylaxis N=2076 RR 4 5 0. 81 (0. 21 to 3. 0) Excessive intra-op 182 126 1. 47 (1. 18 to 1. 82) Wound hematoma 158 117 1. 37 (1. 09 to 1. 73) 202/731 202/744 1. 02 (0. 86 to 1. 20) Fatal bleed Transfusion

Collins Meta-analysis N Engl J Med. 1988; 318: 1162 -1173.

Collins Meta-analysis • 69 studies of LDUH prophylaxis – – • • General surgery (45) Urology (7) Elective orthopedic (12) Trauma (7) About half open label Most measured surrogate outcome for VTE Many used suboptimal test (FUT) Bleeding outcome: excessive intraoperative bleeding or need from transfusion
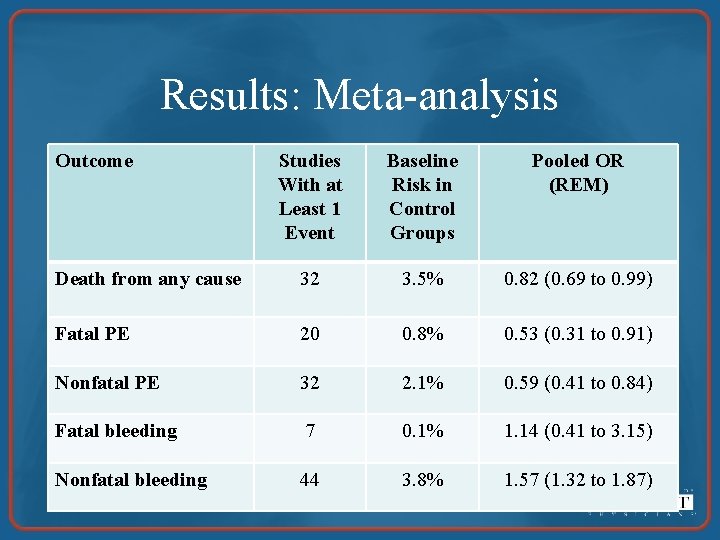
Results: Meta-analysis Outcome Studies With at Least 1 Event Baseline Risk in Control Groups Pooled OR (REM) Death from any cause 32 3. 5% 0. 82 (0. 69 to 0. 99) Fatal PE 20 0. 8% 0. 53 (0. 31 to 0. 91) Nonfatal PE 32 2. 1% 0. 59 (0. 41 to 0. 84) Fatal bleeding 7 0. 1% 1. 14 (0. 41 to 3. 15) Nonfatal bleeding 44 3. 8% 1. 57 (1. 32 to 1. 87)
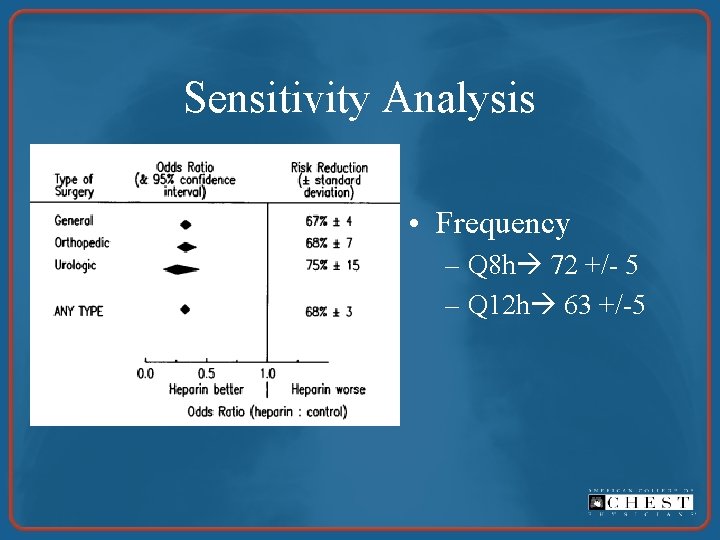
Sensitivity Analysis • Frequency – Q 8 h 72 +/- 5 – Q 12 h 63 +/-5
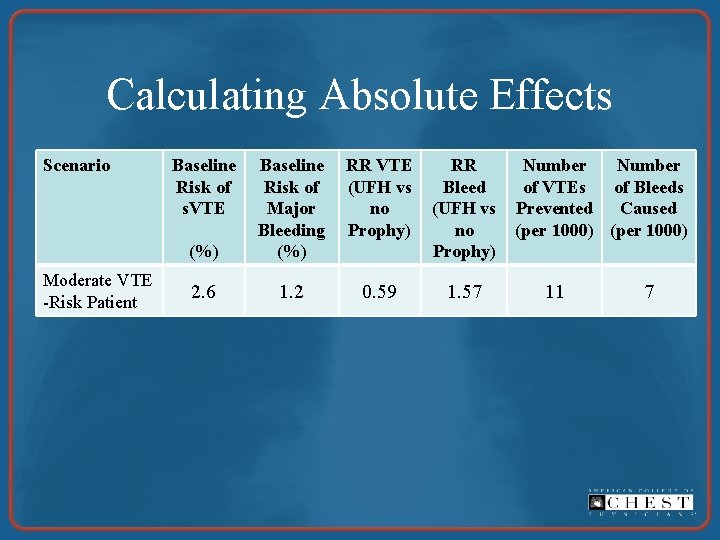
Calculating Absolute Effects Scenario Moderate VTE -Risk Patient Baseline Risk of s. VTE RR VTE (UFH vs no Prophy) (%) Baseline Risk of Major Bleeding (%) RR Bleed (UFH vs no Prophy) 2. 6 1. 2 0. 59 1. 57 Number of VTEs of Bleeds Prevented Caused (per 1000) 11 7

Evidence Synthesis: Tradeoffs between desirable and undesirable outcomes
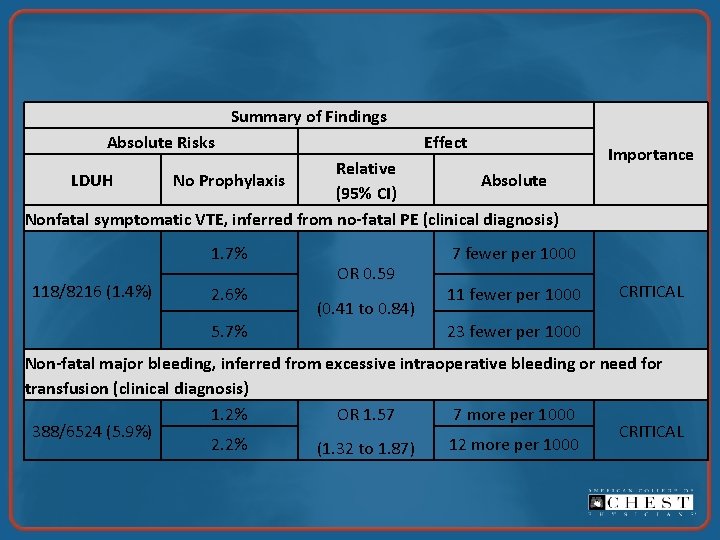
Summary of Findings Absolute Risks Effect Relative LDUH No Prophylaxis Absolute (95% CI) Nonfatal symptomatic VTE, inferred from no-fatal PE (clinical diagnosis) 1. 7% 118/8216 (1. 4%) 2. 6% 5. 7% OR 0. 59 (0. 41 to 0. 84) Importance 7 fewer per 1000 11 fewer per 1000 CRITICAL 23 fewer per 1000 Non-fatal major bleeding, inferred from excessive intraoperative bleeding or need for transfusion (clinical diagnosis) 1. 2% 7 more per 1000 OR 1. 57 388/6524 (5. 9%) CRITICAL 2. 2% 12 more per 1000 (1. 32 to 1. 87)
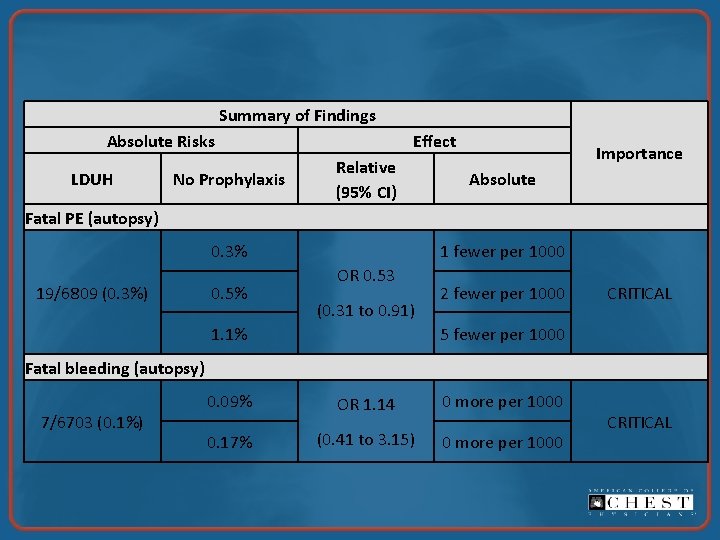
Summary of Findings Absolute Risks LDUH No Prophylaxis Effect Relative (95% CI) Importance Absolute Fatal PE (autopsy) 0. 3% 19/6809 (0. 3%) 0. 5% 1 fewer per 1000 OR 0. 53 (0. 31 to 0. 91) 1. 1% 2 fewer per 1000 CRITICAL 5 fewer per 1000 Fatal bleeding (autopsy) 7/6703 (0. 1%) 0. 09% OR 1. 14 0 more per 1000 0. 17% (0. 41 to 3. 15) 0 more per 1000 CRITICAL

GRADE: Quality of Evidence Limitations Inconsistency Indirectness Imprecision Other Threats to validity, risk of bias: concealment of allocation sequence, blinding, losses to follow-up, selective reporting, early stopping Unexplained heterogeneity in results across studies Indirect evidence from different population, intervention, comparator or outcome Confidence interval around effect includes both no effect and either important benefit or important harm (or both) Potential for publication bias OR Indirect comparison: Use studies of A vs B and B vs C to compare A vs C
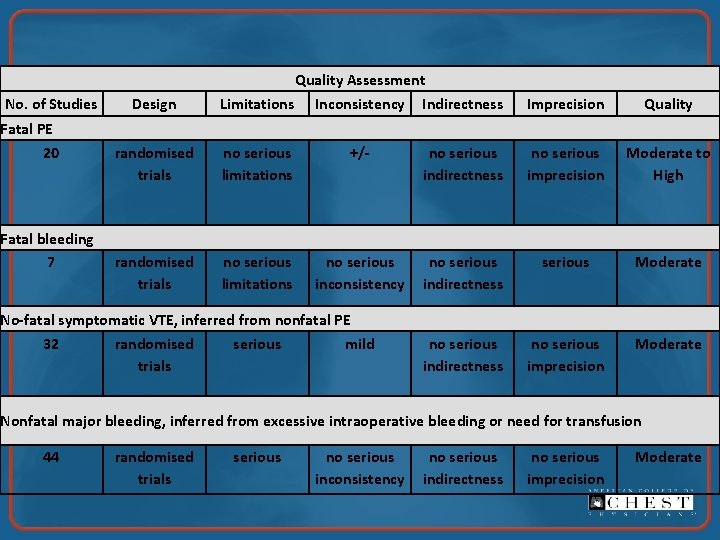
Quality Assessment No. of Studies Fatal PE 20 Fatal bleeding 7 Design Limitations Inconsistency Indirectness Imprecision Quality randomised trials no serious limitations +/- no serious indirectness no serious imprecision Moderate to High randomised trials no serious limitations no serious inconsistency no serious indirectness serious Moderate no serious indirectness no serious imprecision Moderate No-fatal symptomatic VTE, inferred from nonfatal PE 32 randomised serious mild trials Nonfatal major bleeding, inferred from excessive intraoperative bleeding or need for transfusion 44 randomised trials serious no serious inconsistency no serious indirectness no serious imprecision Moderate

Guyatt et al. BMJ. 2008; 336: 1049 -1051.

GRADE: Strength of Recommendation BMJ. 2008; 336: 1049 -1051.

Recommendation For general surgical patients at moderate risk for venous thromboembolism who are not at high risk for perioperative bleeding, we suggest low-dose unfractionated heparin (Grade 2 B) over no prophylaxis.

Recommendation For general surgical patients at high risk for venous thromboembolism who are not at high risk for perioperative bleeding, we recommend use of low-dose unfractionated heparin (Grade 1 B) over no prophylaxis.

Major Challenges • Multiple sources of heterogeneity • Indirectness – When should one apply indirect evidence from studies performed in a mixed (surgical) or different patient population? • Surrogate outcome: asymptomatic DVT • Poorly standardized outcome: major bleeding • Limited information about baseline risk of VTE in absence of prophylaxis

Biases Introduced by Surveillance for Asymptomatic DVT • Downward: identification and treatment of asymptomatic DVT prevents unknown number of events that would have become symptomatic • Upward: more likely to label a finding (eg, leg swelling) as a symptomatic if event is detected by surveillance • Difficult to estimate the ratio of asymptomatic to symptomatic events

Additional Challenges • Numerous comparisons – LDUH, LMWH, fondaparinux, low-dose ASA, high-dose ASA, ES and IPC vs no prophy – Mechanical vs pharmacologic – Add mechanical to pharmacologic – 16 unique evidence profiles and still counting! • Numerous surgical populations – – Abdomen and pelvis (vascular, bariatric) Neurosurgery (craniotomy, spine) Trauma (TBI, SCI, other major trauma) Cardiac, thoracic, other…

Patients Undergoing General, GI, Urologic, Gynecologic, Bariatric, Vascular, Plastic, or Reconstructive Surgery For general and abdominal-pelvic surgery patients at very low risk for VTE (< 0. 5%; Rogers score, < 7; Caprini score, 0), we recommend that no specific pharmacologic (Grade 1 B) or mechanical (Grade 2 C) prophylaxis be used other than early ambulation.

Patients Undergoing General, GI, Urologic, Gynecologic, Bariatric, Vascular, Plastic, or Reconstructive Surgery For general and abdominal-pelvic surgery patients at low risk for VTE (~ 1. 5%; Rogers score, 7 -10; Caprini score, 1 -2), we suggest mechanical prophylaxis, preferably with intermittent pneumatic compression (IPC), over no prophylaxis (Grade 2 C).

Patients Undergoing General, GI, Urologic, Gynecologic, Bariatric, Vascular, Plastic, or Reconstructive Surgery For general and abdominal-pelvic surgery patients at moderate risk for VTE (~ 3. 0%; Rogers score, > 10; Caprini score, 3 -4) who are not at high risk for major bleeding complications, we suggest LMWH (Grade 2 B), LDUH (Grade 2 B), or mechanical prophylaxis, preferably with IPC (Grade 2 C), over no prophylaxis. Remarks: Three of the seven authors favored a strong (Grade 1 B) recommendation in favor of LMWH or LDUH over no prophylaxis in this group.

Patients Undergoing General, GI, Urologic, Gynecologic, Bariatric, Vascular, Plastic, or Reconstructive Surgery For general and abdominal-pelvic surgery patients at moderate risk for VTE (3. 0%; Rogers score, > 10; Caprini score, 3 -4) who are at high risk for major bleeding complications or those in whom the consequences of bleeding are thought to be particularly severe, we suggest mechanical prophylaxis, preferably with IPC, over no prophylaxis (Grade 2 C).

Patients Undergoing General, GI, Urologic, Gynecologic, Bariatric, Vascular, Plastic, or Reconstructive Surgery For general and abdominal-pelvic surgery patients at high risk for VTE (~ 6. 0%; Caprini score, ≥ 5) who are not at high risk for major bleeding complications, we recommend pharmacologic prophylaxis with LMWH (Grade 1 B) or LDUH (Grade 1 B) over no prophylaxis. We suggest that mechanical prophylaxis with elastic stockings or IPC should be added to pharmacologic prophylaxis (Grade 2 C).

Patients Undergoing General, GI, Urologic, Gynecologic, Bariatric, Vascular, Plastic, or Reconstructive Surgery For high-VTE-risk patients undergoing abdominal or pelvic surgery for cancer who are not otherwise at high risk for major bleeding complications, we recommend extended-duration pharmacologic prophylaxis (4 weeks) with LMWH over limited-duration prophylaxis (Grade 1 B). Remarks: Patients who place a high value on minimizing out-ofpocket health-care costs might prefer limited-duration over extended-duration prophylaxis in settings where the cost of extended-duration prophylaxis is borne by the patient.

Patients Undergoing General, GI, Urologic, Gynecologic, Bariatric, Vascular, Plastic, or Reconstructive Surgery For high-VTE-risk general and abdominal-pelvic surgery patients who are at high risk for major bleeding complications or those in whom the consequences of bleeding are thought to be particularly severe, we suggest use of mechanical prophylaxis, preferably with IPC, over no prophylaxis until the risk of bleeding diminishes and pharmacologic prophylaxis may be initiated (Grade 2 C).

Patients Undergoing General, GI, Urologic, Gynecologic, Bariatric, Vascular, Plastic, or Reconstructive Surgery For general and abdominal-pelvic surgery patients at high risk for VTE (6%; Caprini score, ≥ 5) in whom both LMWH and unfractionated heparin are contraindicated or unavailable and who are not at high risk for major bleeding complications, we suggest low-dose aspirin (Grade 2 C), fondaparinux (Grade 2 C), or mechanical prophylaxis, preferably with IPC (Grade 2 C), over no prophylaxis.

Patients Undergoing General, GI, Urologic, Gynecologic, Bariatric, Vascular, Plastic, or Reconstructive Surgery For general and abdominal-pelvic surgery patients, we suggest that an inferior vena cava (IVC) filter should not be used for primary VTE prevention (Grade 2 C).

Patients Undergoing General, GI, Urologic, Gynecologic, Bariatric, Vascular, Plastic, or Reconstructive Surgery For general and abdominal-pelvic surgery patients, we suggest that periodic surveillance with venous compression ultrasound (VCU) should not be performed (Grade 2 C).

Patients Undergoing Cardiac Surgery For cardiac surgery patients with an uncomplicated postoperative course, we suggest use of mechanical prophylaxis, preferably with optimally applied IPC, over either no prophylaxis (Grade 2 C) or pharmacologic prophylaxis (Grade 2 C).

Patients Undergoing Cardiac Surgery For cardiac surgery patients whose hospital course is prolonged by one or more nonhemorrhagic surgical complications, we suggest adding pharmacologic prophylaxis with LDUH or LMWH to mechanical prophylaxis (Grade 2 C).

Patients Undergoing Thoracic Surgery For thoracic surgery patients at moderate risk for VTE who are not at high risk for perioperative bleeding, we suggest LDUH (Grade 2 B), LMWH (Grade 2 B), or mechanical prophylaxis with optimally applied IPC (Grade 2 C) over no prophylaxis. Remarks: Three of the seven authors favored a strong (Grade 1 B) recommendation in favor of LMWH or LDUH over no prophylaxis in this group.

Patients Undergoing Thoracic Surgery For thoracic surgery patients at high risk for VTE who are not at high risk for perioperative bleeding, we suggest LDUH (Grade 1 B) or LMWH (Grade 1 B) over no prophylaxis. In addition, we suggest that mechanical prophylaxis with ES or IPC should be added to pharmacologic prophylaxis (Grade 2 C).

Patients Undergoing Thoracic Surgery For thoracic surgery patients who are at high risk for major bleeding, we suggest use of mechanical prophylaxis, preferably with optimally applied IPC, over no prophylaxis until the risk of bleeding diminishes and pharmacologic prophylaxis may be initiated (Grade 2 C).

Patients Undergoing Craniotomy For craniotomy patients, we suggest that mechanical prophylaxis, preferably with IPC, be used over no prophylaxis (Grade 2 C) or pharmacologic prophylaxis (Grade 2 C).

Patients Undergoing Craniotomy For craniotomy patients at very high risk for VTE (eg, those undergoing craniotomy for malignant disease), we suggest adding pharmacologic prophylaxis to mechanical prophylaxis once adequate hemostasis is established and the risk of bleeding decreases (Grade 2 C).

Patients Undergoing Spinal Surgery For patients undergoing spinal surgery, we suggest mechanical prophylaxis, preferably with IPC, over no prophylaxis (Grade 2 C), unfractionated heparin (Grade 2 C), or LMWH (Grade 2 C).

Patients Undergoing Spinal Surgery For patients undergoing spinal surgery at high risk for VTE (including those with malignant disease or those undergoing surgery with a combined anterior-posterior approach), we suggest adding pharmacologic prophylaxis to mechanical prophylaxis once adequate hemostasis is established and the risk of bleeding decreases (Grade 2 C).

Major Trauma For major trauma patients, we suggest use of LDUH (Grade 2 C), LMWH (Grade 2 C), or mechanical prophylaxis, preferably with IPC (Grade 2 C), over no prophylaxis.

Major Trauma For major trauma patients in whom LMWH and LDUH are contraindicated, we suggest mechanical prophylaxis, preferably with IPC, over no prophylaxis (Grade 2 C) when not contraindicated by lower-extremity injury. We suggest adding pharmacologic prophylaxis with either LMWH or LDUH when the risk of bleeding diminishes or the contraindication to heparin resolves (Grade 2 C).

Major Trauma For major trauma patients, we suggest that an IVC filter should not be used for primary VTE prevention (Grade 2 C).

Patients With Major Trauma: Traumatic Brain Injury, Acute Spinal Injury, and Traumatic Spine Injury For major trauma patients at high risk for VTE (including those with acute spinal cord injury, traumatic brain injury, and spinal surgery for trauma), we suggest adding mechanical prophylaxis to pharmacologic prophylaxis (Grade 2 C) when not contraindicated by lower extremity injury.

Patients With Major Trauma: Traumatic Brain Injury, Acute Spinal Injury, and Traumatic Spine Injury For major trauma patients, we suggest that periodic surveillance with VCU should not be performed (Grade 2 C).

Endorsing Organizations This guideline has received the endorsement of the following organizations: • American Association for Clinical Chemistry • American College of Clinical Pharmacy • American Society of Health-System Pharmacists • American Society of Hematology • International Society of Thrombosis and Hemostasis

Acknowledgement of Support The ACCP appreciates the support of the following organizations for some part of the guideline development process: Bayer Schering Pharma AG National Heart, Lung, and Blood Institute (Grant No. R 13 HL 104758) With educational grants from Bristol-Myers Squibb and Pfizer, Inc. Canyon Pharmaceuticals, and sanofi-aventis U. S. Although these organizations supported some portion of the development of the guidelines, they did not participate in any manner with the scope, panel selection, evidence review, development, manuscript writing, recommendation drafting or grading, voting, or review. Supporters did not see the guidelines until they were published.
- Slides: 85