Joint Hospital Surgical Grand Round Accelerated partial breast

Joint Hospital Surgical Grand Round Accelerated partial breast irradiation: where should we go? Dr Ma Kwok Kuen Queen Mary Hospital

Background l Early Breast Cancer Trialist’s Collaborative Group meta-analysis: Whole breast radiotherapy (WBRT) after breast conserving surgery (BCS) l l 19% absolute risk reduction of ipsilateral breast recurrence in 5 years 5% absolute reduction in 15 -year risk of death Lancet 2005

Definitions l l l Conventional WBRT: 50 Gy over 25 fractions (5 weeks) Partial breast irradiation (PBI): irradiation of a limited volume of breast tissue around the tumor bed Accelerated partial breast irradiation (APBI): deliver a larger than standard dose of radiation with each treatment, shortening the overall treatment time

Rationale of APBI l The spatial pattern of relapse after BCS with or without WBRT: 76 -90% at “same site” l Five prospective randomized trials l l l NSABP B 06. Cancer 1986 Uppsala-Orebro. J Clin Oncol 1999 Ontario Clinical Oncology Group. J Natl Cancer Inst 1996 Milan III. Ann Oncol 2001 Swe. BCG 91 -RT. Eur J Cancer 2003

Rationale of APBI l WBRT may not protect against the development of new primary cancer in the irradiated breast l Milan I trial: comparing mastectomy with quadrantectomy and WBRT l l Similar rate of other quadrant breast recurrence and contralateral breast cancers (CLB) Yale group: at 15 years after BCT in 1152 patients, 13% incidence of other quadrant breast tumor compared with 10% incidence of CLB New Engl Med 2002 Int J Radiation Oncology Biol Phys 2000

Potential advantages of APBI l Reduction of treatment time l l l Convenient to patient Increase the use of BCS Shorten the waiting time Treatment costs Reduce normal tissue toxicity Cosmesis

Questions to be answered 1. 2. 3. Which patients are best served by APBI? What is the best technique? What is the long term result?

1. Which patients are best served by accelerated partial breast irradiation?
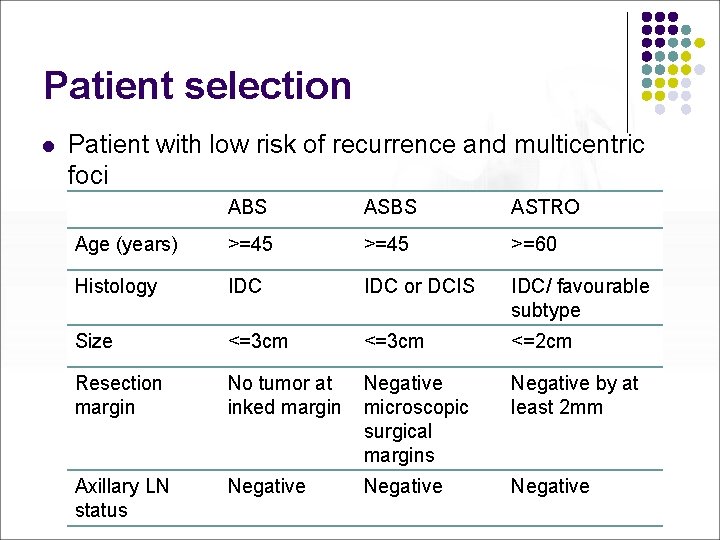
Patient selection l Patient with low risk of recurrence and multicentric foci ABS ASTRO Age (years) >=45 >=60 Histology IDC or DCIS IDC/ favourable subtype Size <=3 cm <=2 cm Resection margin No tumor at inked margin Negative microscopic surgical margins Negative by at least 2 mm Axillary LN status Negative

2. What is the optimal technique of administration of APBI?

Methods of APBI l Interstitial brachytherapy Balloon brachytherapy Intraoperative radiotherapy External beam radiotherapy l Promising Phase I/II trials l l l
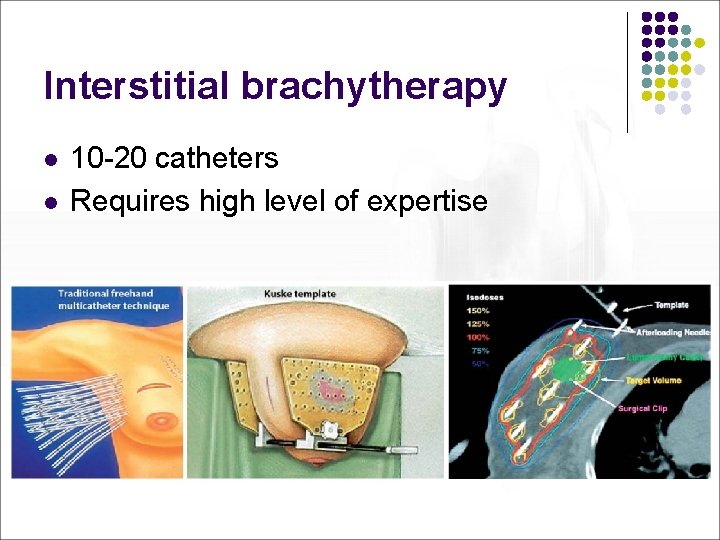
Interstitial brachytherapy l l 10 -20 catheters Requires high level of expertise
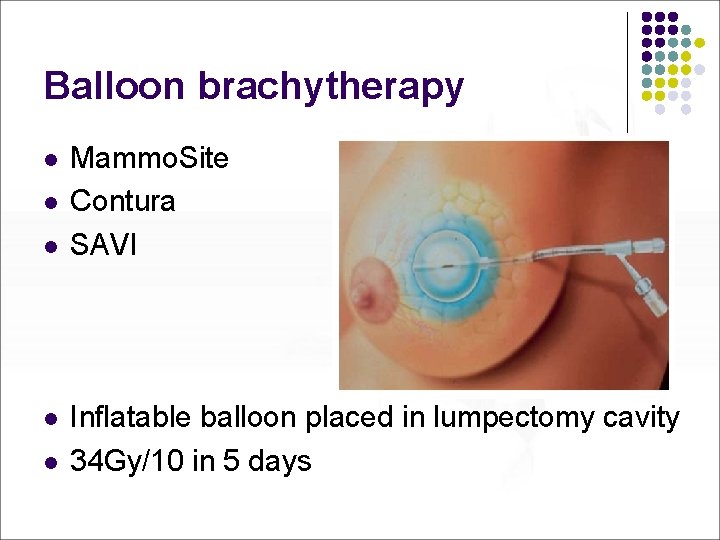
Balloon brachytherapy l l l Mammo. Site Contura SAVI Inflatable balloon placed in lumpectomy cavity 34 Gy/10 in 5 days
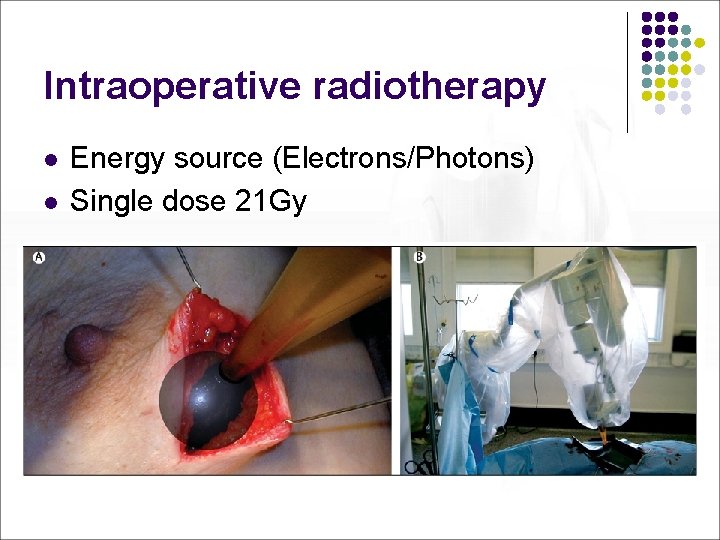
Intraoperative radiotherapy l l Energy source (Electrons/Photons) Single dose 21 Gy

External beam radiotherapy l l 3 D conformal Other methods (Intensity modulated radiotherapy (IMRT), tomotherapy)

3. What are the long-term effects on local control, survival and toxcity?
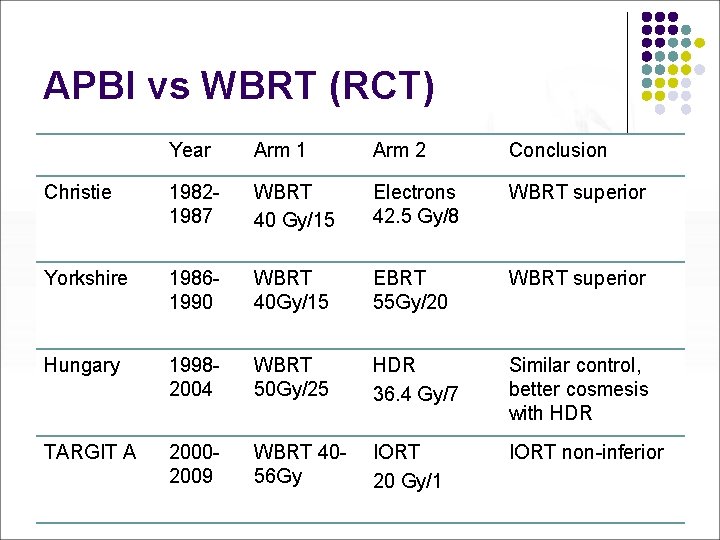
APBI vs WBRT (RCT) Year Arm 1 Arm 2 Conclusion Christie 19821987 WBRT 40 Gy/15 Electrons 42. 5 Gy/8 WBRT superior Yorkshire 19861990 WBRT 40 Gy/15 EBRT 55 Gy/20 WBRT superior Hungary 19982004 WBRT 50 Gy/25 HDR 36. 4 Gy/7 Similar control, better cosmesis with HDR TARGIT A 20002009 WBRT 4056 Gy IORT 20 Gy/1 IORT non-inferior

Hungary l l WBRT (130) vs PBI (128) using HDR multicatheter brachytherapy (69%) or EB (31%) No statistically significant difference in l l l 5 year local recurrence rate: 3. 4% in WBRT vs 4. 7% in PBI Overall survival: 91. 8% vs 96. 4% Cancer specific survival: 96% vs 98. 3% Disease free survival: 90. 3% vs 88. 3% Better cosmesis with HDR APBI Int. J. Radiation Oncology Biol. Phys. 2007
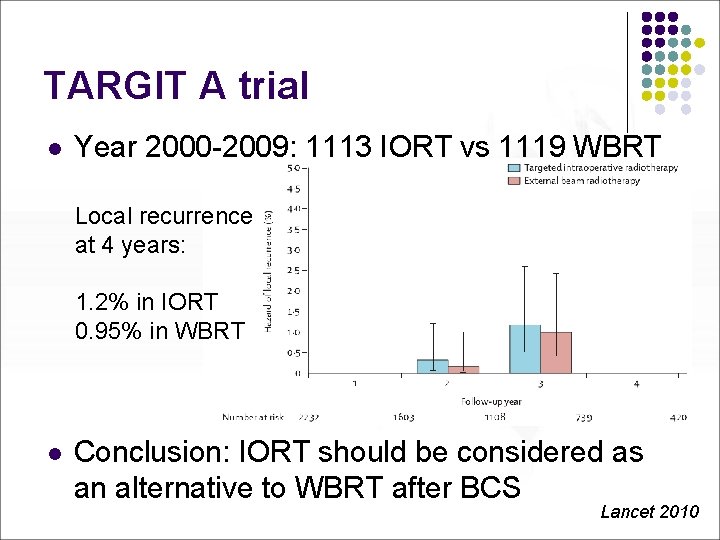
TARGIT A trial l Year 2000 -2009: 1113 IORT vs 1119 WBRT Local recurrence at 4 years: 1. 2% in IORT 0. 95% in WBRT l Conclusion: IORT should be considered as an alternative to WBRT after BCS Lancet 2010
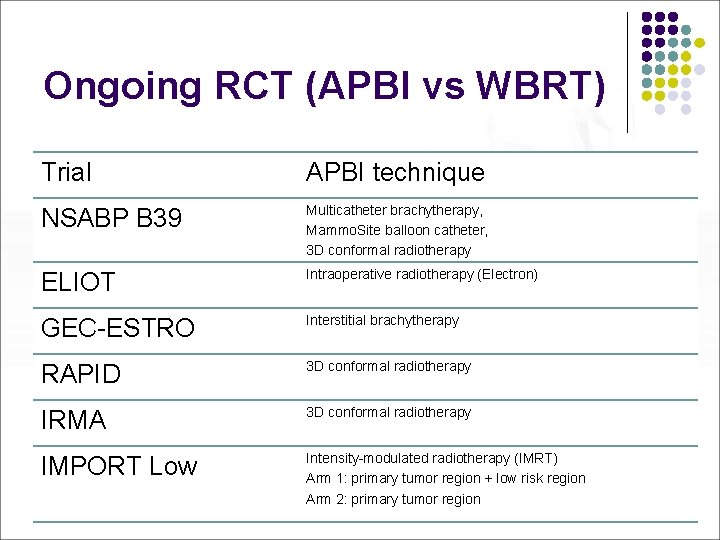
Ongoing RCT (APBI vs WBRT) Trial APBI technique NSABP B 39 Multicatheter brachytherapy, Mammo. Site balloon catheter, 3 D conformal radiotherapy ELIOT Intraoperative radiotherapy (Electron) GEC-ESTRO Interstitial brachytherapy RAPID 3 D conformal radiotherapy IRMA 3 D conformal radiotherapy IMPORT Low Intensity-modulated radiotherapy (IMRT) Arm 1: primary tumor region + low risk region Arm 2: primary tumor region

Is it a perfect solution?

Counterpoints l The spatial pattern of ipsilateral breast tumor relapse is not accurately defined l l Definition of “same site”: no generally accepted criteria (? index quadrant ? tumor bed ? surgical field ? scar area) Does not correspond closely to pathological findings l Pathological studies suggest multifocal/multicentric foci are relatively common (~45%) in patients with clinically unifocal tumors l Holland R et al. Cancer 1985 l Vaidya JS et al. Br J Cancer 1996

Counterpoints l The distinction between true recurrence and new primary tumor may not be reliable l l Vicini FA et al. Cancer 2007: Clinical and the clonality classifications only show 65% concordance 7 randomized breast conservation trials suggests that other quadrant ipsilateral breast relapse is reduced by whole breast radiotherapy

What is the likely impact of APBI trials?

Conclusions l l l ~16000 women Level I evidence for or against APBI in early breast cancer Identification of patient subgroups with the most and least to benefit from APBI technique comparison (NSABP B 39) Increase the understanding of ipsilateral breast tumor relapse and the impact of radiotherapy (IMPORT Low)

Supplementary

ELIOT trial l ELIOT (Electron Intraoperative Therapy) 2000 l l l 4 -12 Me. V external beam electron applicator 21 Gy single dose to 10 -30 mm around the applicator Milan III trial – testing the effect of WBRT after quadrantectomy, in which in the absence of radiotherapy, 85% of IBTR presented “in the scar area” Milan I trial – comparing quadrantectomy and mastectomy, in which patients treated with quadrantectomy suffered comparable rates of other quadrant IBTR and contralateral breast cancer Hypothesis – WBRT is not necessary, since most IBTRs occur in the vicinity of the primary tumor, and radiotherapy does not prevent other quadrant relapses which are mostly new primaries

TARGIT trial l TARGIT (TARGeted Intraoperative radio. Therapy) 2000 l l Low energy photons (50 k. V maximum) 20 Gy single dose to 2 mm beyond the surface of applicator Clinical and pathological observation l IBTR occurs in >90% of the patients at the site of the original primary tumor regardless of surgical excision margin and WBRT l A pathological study of 30 mastectomy specimens from women eligible for BCS revealed multiple tumor foci in 19 specimens, and in 15 of these, foci were located outside the index quadrant Hypothesis – Multicentric cancer foci remain dormant and are not generally responsible for IBTR

GEC-ESTRO trial l l European Brachytherapy Breast Cancer GEC -ESTRO Working Group trial 2004 High dose rate (HDR) [32 Gy/8 or 30. 3 Gy/7 BD] or pulsed dose rate (PDR) [50 Gy hourly fractions of 0. 6 -0. 8 Gy] brachytherapy Majority of IBTRs occur in close proximity to the tumor bed, and that other quadrant IBTR risk is low and unaffected by radiotherapy

NSABP B 39/RTOG 0413 trial l l 2005 Three APBI technique l l Multicatheter brachytherapy Mammo. Site balloon catheter 3 D conformal radiotherapy Rationals similar to ELIOT trial

RAPID and IRMA trials l l RAPID (Randomised Trial of Accelerated Partial Breast Irradiation) 2006 IRMA (Innovazioni nella Radioterapia della MAmmella) 2007 Compare WBRT and 3 D conformal radiotherapy Rationals similar to ELIOT trial

IMPORT Low trial l l IMPORT (Intensity Modulated and Partial Organ Radiotherapy) Low trial 2006 Fixed multisegmented tangential beams in all three arms l l Whole breast (40 Gy/15) Partial breast (40 Gy/15) + remainder of the whole breast (36 Gy/15) Testing l l WBRT vs PBI Direct measure of RT effect against other quadrant relapses
- Slides: 32