Hospital Acquired Group A Streptococcal Infections What have



































- Slides: 57

Hospital Acquired Group A Streptococcal Infections What have we learned? Nov. 20, 2008 Nick Daneman Division of Infectious Diseases Sunnybrook Health Sciences Centre

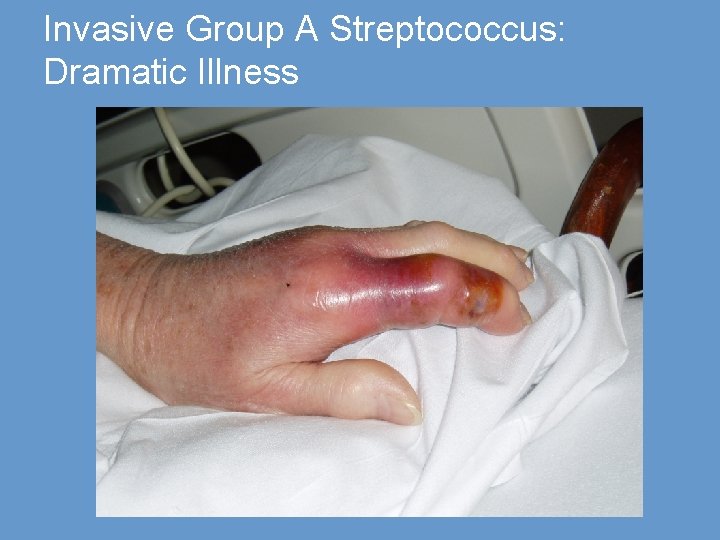
Invasive Group A Streptococcus: Dramatic Illness

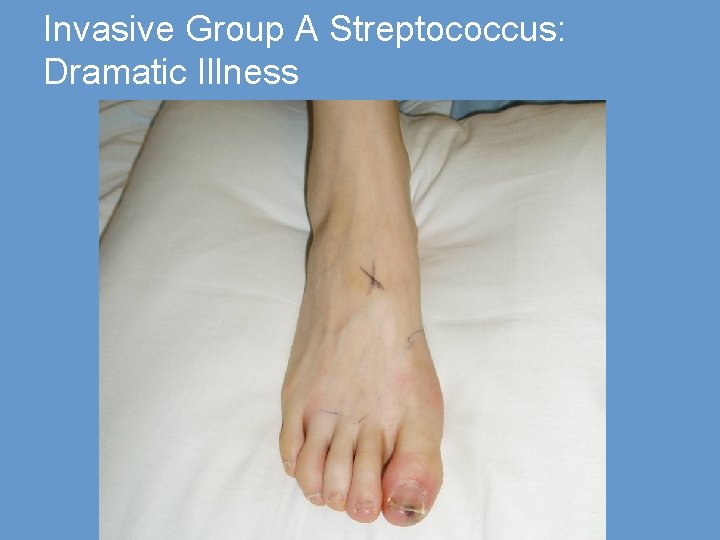
Invasive Group A Streptococcus: Dramatic Illness

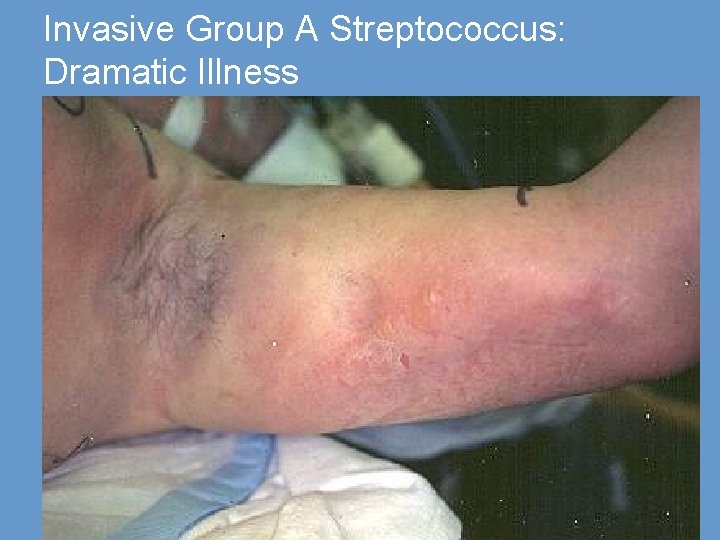
Invasive Group A Streptococcus: Dramatic Illness

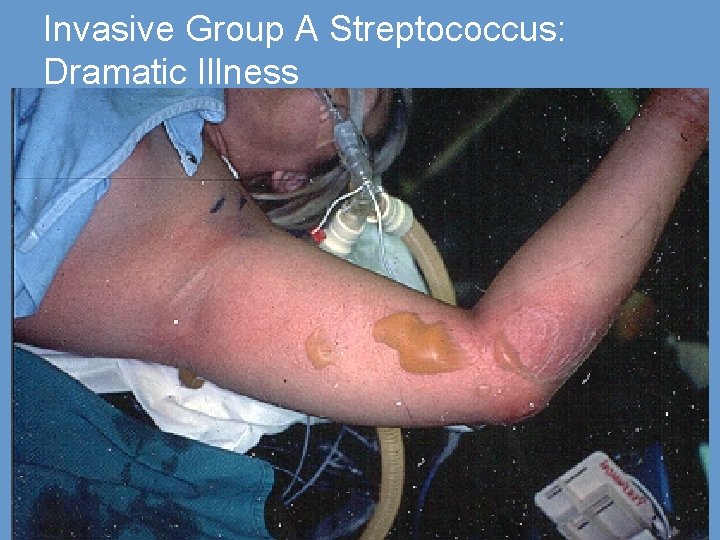
Invasive Group A Streptococcus: Dramatic Illness

Invasive Group A Streptococcus: Dramatic Illness

Invasive Group A Streptococcus: Dramatic Outbreaks 75 CASES, 10 DEATHS

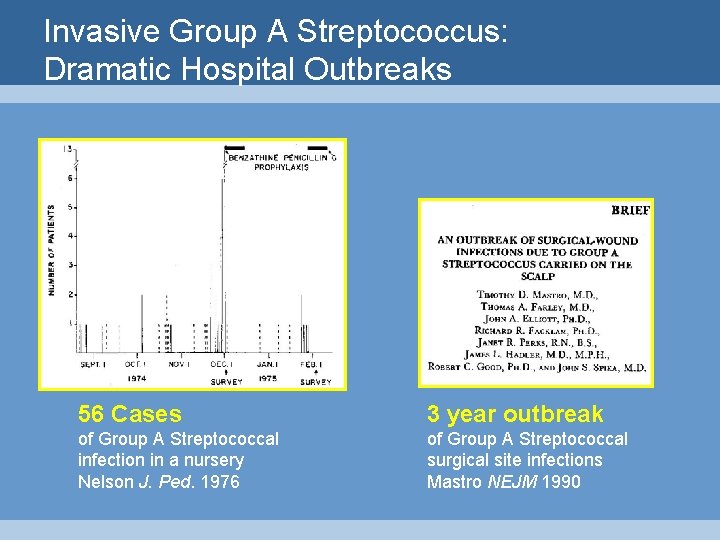
Invasive Group A Streptococcus: Dramatic Hospital Outbreaks 56 Cases 3 year outbreak of Group A Streptococcal infection in a nursery Nelson J. Ped. 1976 of Group A Streptococcal surgical site infections Mastro NEJM 1990

• 1 nosocomial case: – enhanced surveillance – isolate storage • 2 nosocomial cases within 6 months: – typing of isolates – if same strain: • epidemiologic investigation • culture health care workers CID 2002

• expert opinion • review of a handful of literature outbreaks CID 2002

Objectives • describe hospital acquired cases of invasive group A streptococcal infections in Ontario • describe hospital outbreaks of invasive group A streptococcal infections – in Ontario prospective surveillance – systematic review of the literature • provide evidence-based recommendations

Methods: Prospective Surveillance • • • Ontario Group A Strep Study Group population-based surveillance Ontario (population 11, 000) 1992 - 2000 all invasive isolates microbiology labs – all Ontario hospitals – largest outpatient microbiology lab

Methods: Definitions • invasive – group A streptococcus from a sterile site • hospital acquired – neither present nor incubating at admission • outbreak – > 2 cases of culture confirmed, symptomatic GAS infection – epidemiologically linked – caused by same M, T type – indistinguishable by PFGE

Methods: Literature Review • MEDLINE database, 1966 -2004 • search terms • “Streptococcus pyogenes” OR “group A streptococcus” OR “group A streptococcal” • nosocomial OR outbreak OR cross-transmission • review of reference lists • manuscripts reviewed by 2 investigators

Objectives • describe hospital acquired cases of invasive group A streptococcal infections in Ontario • describe hospital outbreaks of invasive group A streptococcal infections – in Ontario prospective surveillance – systematic review of the literature • evidence based recommendations

CID 2005

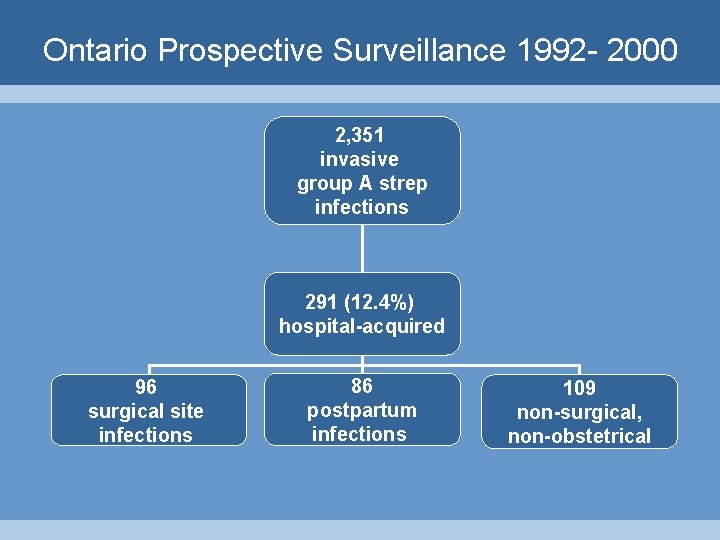
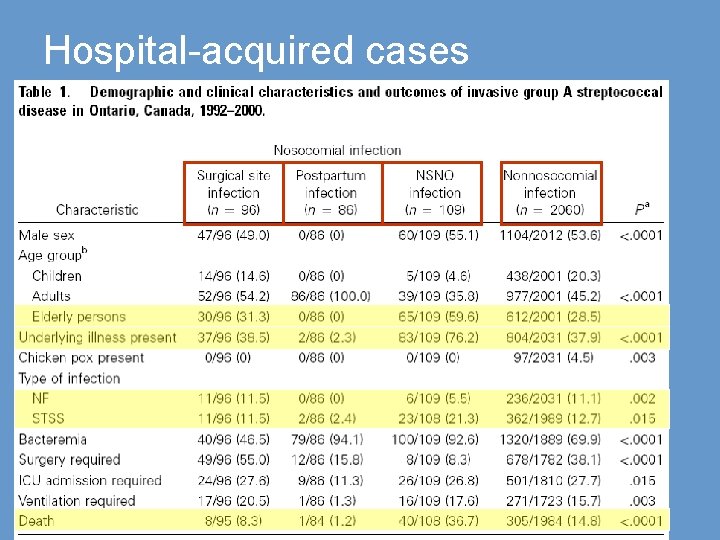
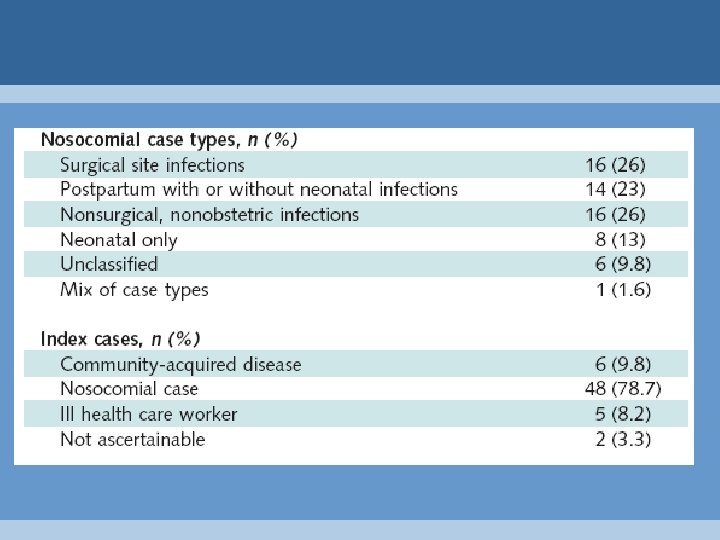
Ontario Prospective Surveillance 1992 - 2000 2, 351 invasive group A strep infections 291 (12. 4%) hospital-acquired 96 surgical site infections 86 postpartum infections 109 non-surgical, non-obstetrical

Hospital-acquired cases

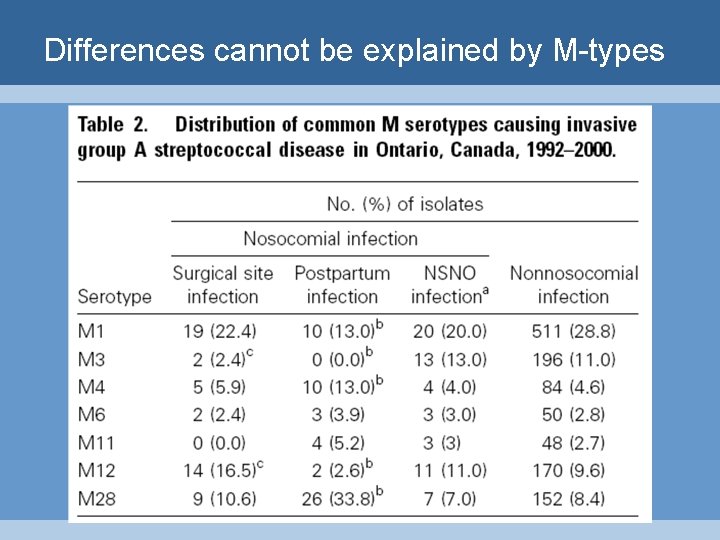
Differences cannot be explained by M-types

Group A Strep Surgical Site Infections • 96 cases • out of 9, 078, 030 surgical admissions • =1. 1 cases / 100, 000 surgical admissions • entire range of surgical procedures – – – – digestive tract 28% musculoskeletal 24% cardiovascular 9% nervous system 11% skin and soft tissue 9% urogyne 8% …

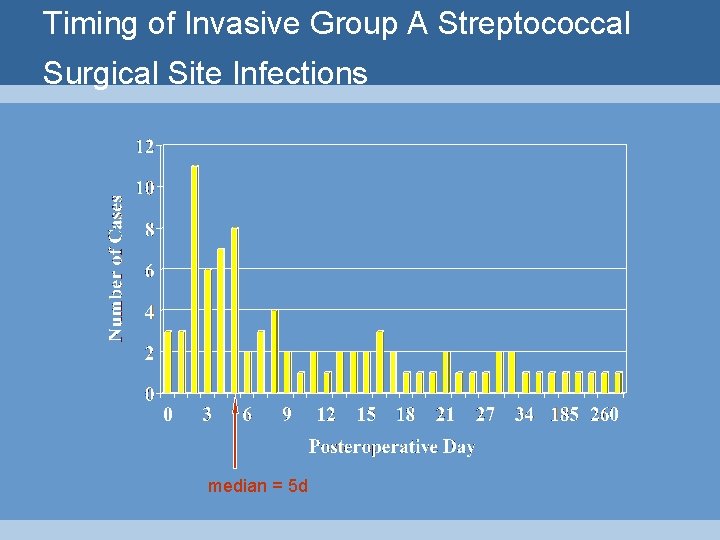
Timing of Invasive Group A Streptococcal Surgical Site Infections median = 5 d

Group A Strep Postpartum infections • 86 cases • out of 1, 269, 722 live births • =0. 7 cases / 10, 000 live births • ~ 1/10 as common as neonatal group B strep infections • but these were infections of mothers (only 2 newborn cases, both non-invasive)

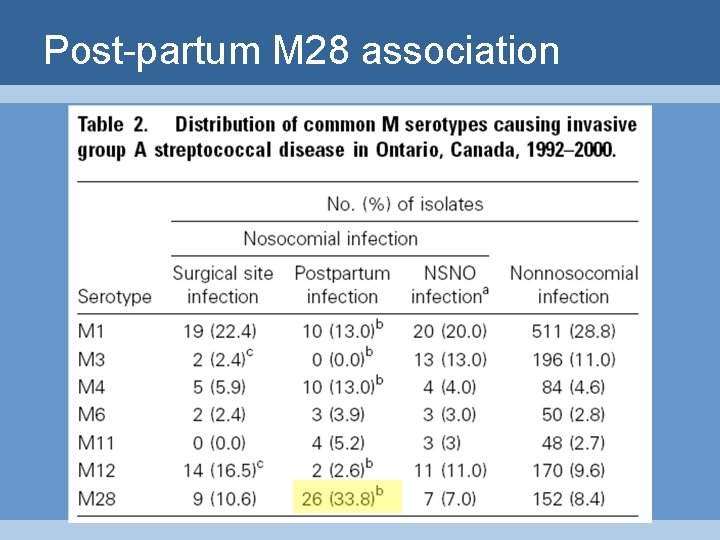
Post-partum M 28 association

Post-partum M 28 association • M 28 predominated in CDC postpartum surveillance 1 • also predominates in perineal infection in children 2 • express surface protein (R 28) related to cell-surface molecules in Group B Strep which enhance binding to cervical epithelium 1. Chuang CID 2002; 2. Mogielnicki Ped 2000; 3. Stalhammar MM 1990

Group A Strep Non-surgical, non-obstetrical infections • 109 cases • 40% of all cases – (despite no mention in nosocomial group A strep guidelines) • time of onset: – median 10. 5 days – range 2 d to >1 year • ? community or nosocomial acquisition?

Group A Strep Non-surgical, non-obstetrical infections • most common syndromes – – primary bacteremia 33% non-necrotizing soft tissue infection 32% lower respiratory tract infection 21% necrotizing fasciitis 6% • 32 / 35 skin infections were associated with preexisting skin breakdown – IV lines (16), G-tubes /tracheostomy (6), chronic ulcers (5), trauma (2), burns (1), other lesions (2)

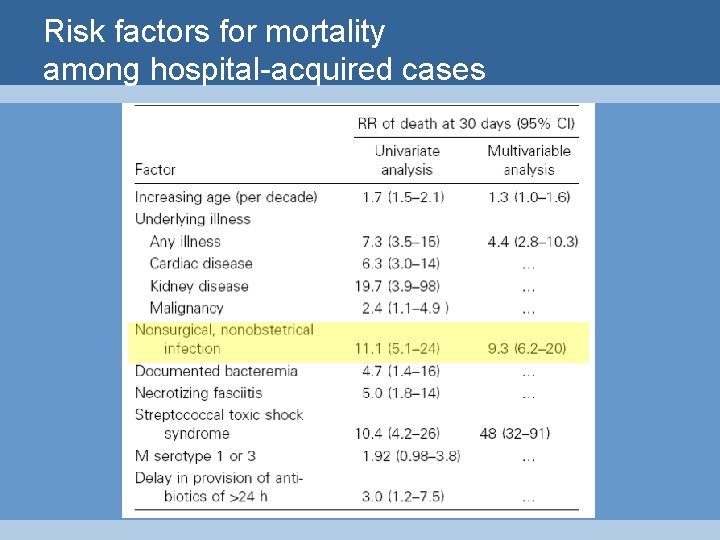
Risk factors for mortality among hospital-acquired cases

Objectives • describe hospital acquired cases of invasive group A streptococcal infections in Ontario • describe hospital outbreaks of invasive group A streptococcal infections – in Ontario prospective surveillance – systematic review of the literature • recommendations


Complementary methods Literature Review Publication bias Prospective Surveillance Hawthorne effects

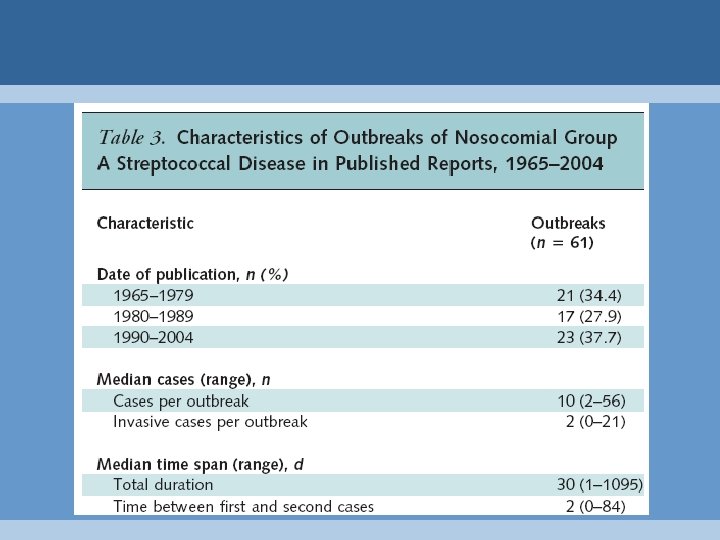
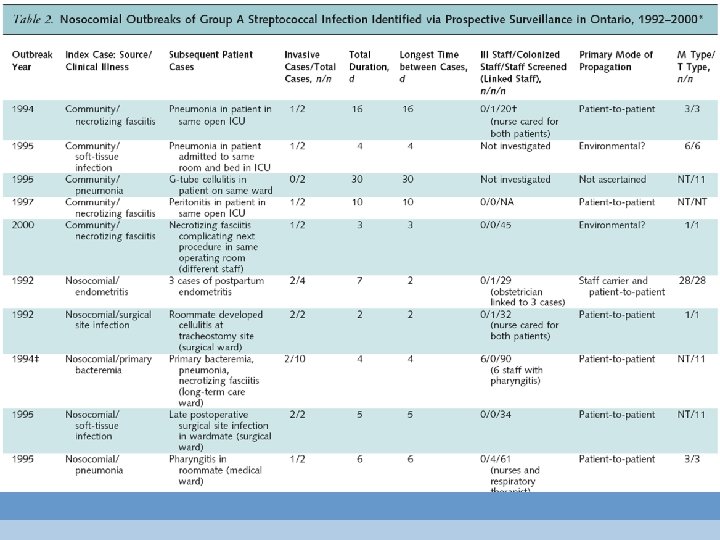
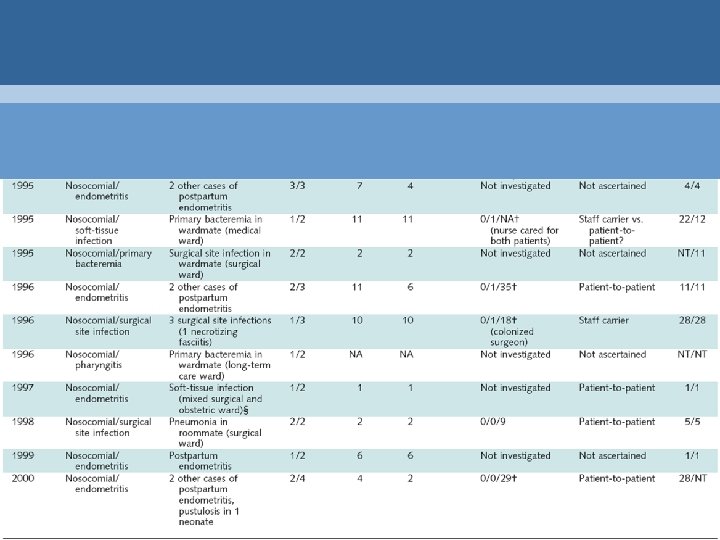
Number of Outbreaks Literature Surveillance 66 publications 2, 351 invasive cases 60 available 291 nosocomial 61 outbreaks 29 outbreak-linked (20 outbreaks)

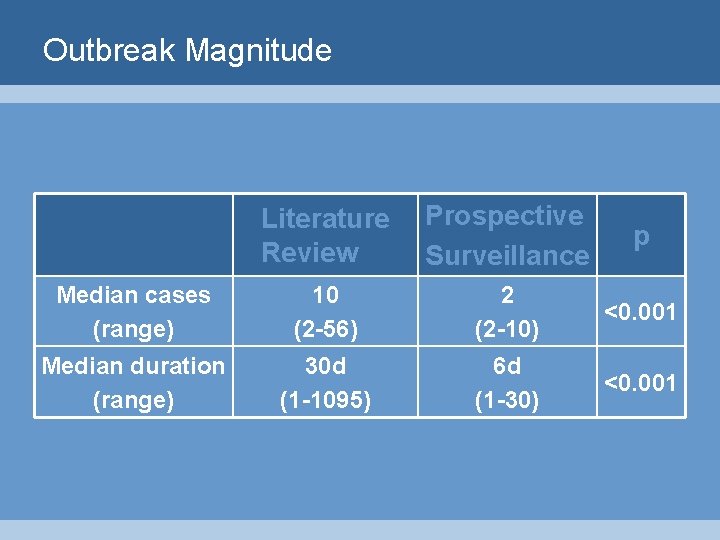
Outbreak Magnitude Literature Review Prospective Surveillance p Median cases (range) 10 (2 -56) 2 (2 -10) <0. 001 Median duration (range) 30 d (1 -1095) 6 d (1 -30) <0. 001

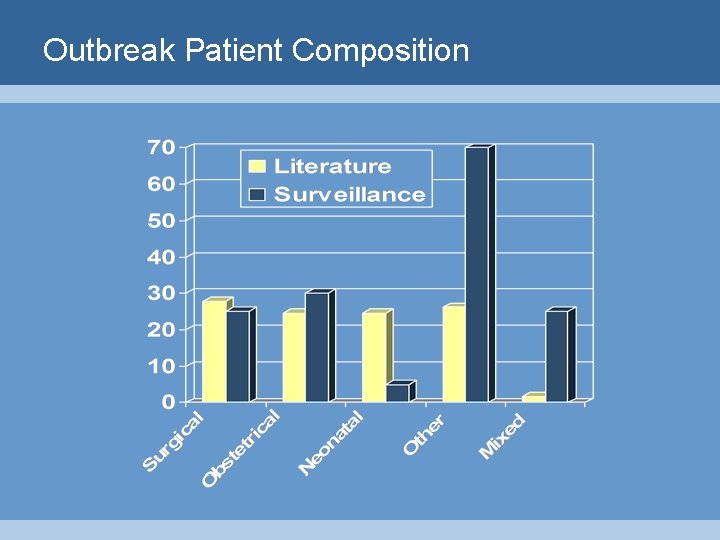
Outbreak Patient Composition

Outbreak Initiation: Index Cases • 3/4 of indexes cases = nosocomial cases • two other sources of outbreaks: – ill health care workers • 5 literature outbreaks* – community-acquired cases • 9 of 11 admitted to ICU • 5 of 9 necrotizing fasciitis† * Di. Persio 1996, Holloway 1967, Kakis 2002, Lannigan 1985, Nicolle 1986, Schwartz 1992 †Burnett 1990, Decker 1985, Ejlertsen 2001, Quinn 1965, Walter 1974

Outbreak Initiation: Rapid Tempo • median interval between first two cases – literature outbreaks: – surveillance outbreaks: 2. 0 d 4. 5 d • interval between first two cases <1 month in 80 of 81 outbreaks

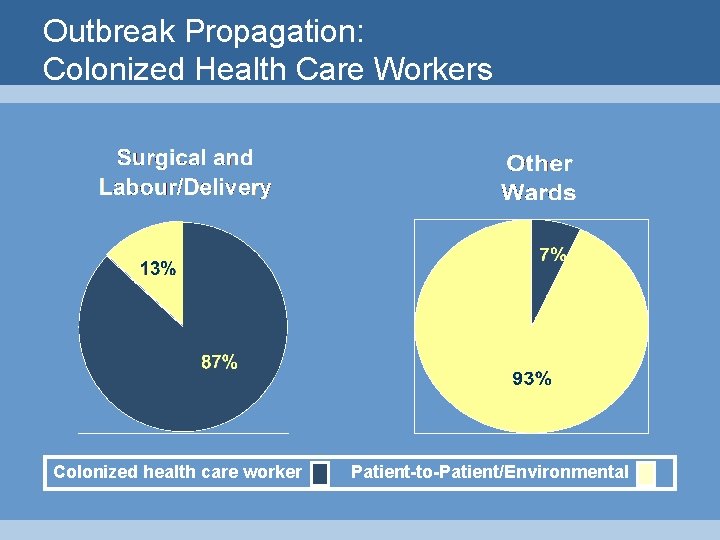
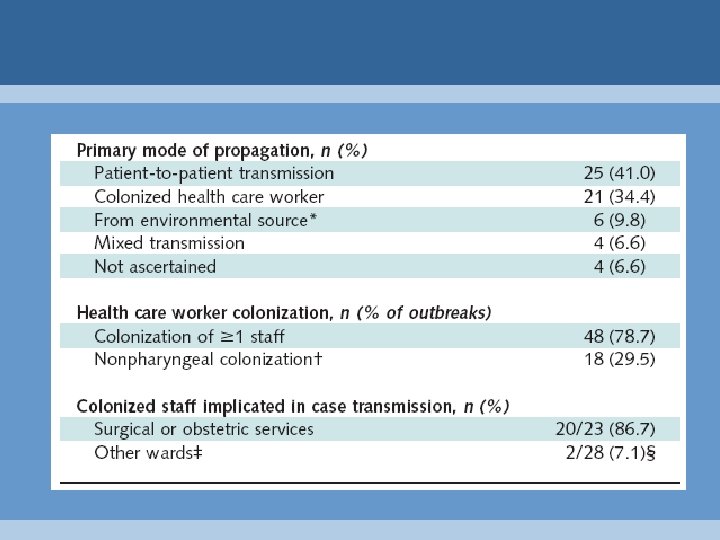
Outbreak Propagation • • • patient to patient colonized health care worker environmental mixed insufficient information 47% 27% 9% 6% 11%

Outbreak Propagation: Colonized Health Care Workers Colonized health care worker Patient-to-Patient/Environmental

Outbreak Propagation: Colonized Health Care Workers • site of health care worker colonization – 31 pharyngeal only – 10 anal – 2 vaginal – 5 skin

Outbreak Propagation: Environmental sources • • • bidet hand shower vinyl sheet airflow mattress multidose vaccine vials (3) food borne outbreak (1) Claesson 1985, Decker 1976, Gordon 1994, Reid 1983, Rutihauser 1999, Decker 1985

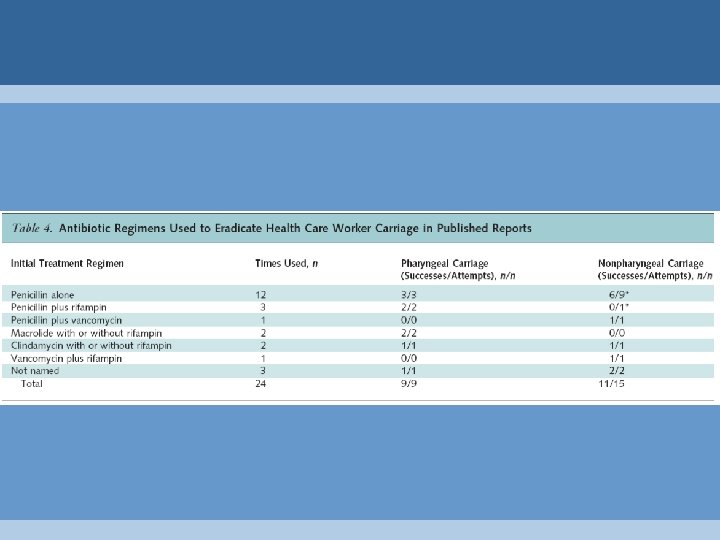
Outbreak Termination: Treatment of Colonized HCWs • data from 24 literature outbreaks • first regimen usually successful: – pharyngeal carriage only: – nonpharyngeal carriage: 9/9 (100%) 11/15 (73%) • 4 failures* – 2 ongoing transmission – 2 late relapses (4 mos and 15 mos) • all ultimately successfully eradicated * Berkelman 1982, Mc. Intyre 1968, Schaffner 1969, Viglionese 1991

Outbreak Termination: Patient to Patient Transmission • multifaceted control measures required • 1 st attempt usually unsuccessful (14/25) • most effective control measures – ward closure (86% success) – mass treatment/prophylaxis (69% success)

5 Recommendations

#1: Target all Nosocomial Cases Hospitalized CID 2002

#2: Isolation of Necrotizing Fasciitis • 11 community acquired index cases • majority due to necrotizing fasciitis admitted to intensive care unit • isolate necrotizing fasciitis on admission (pending cultures)

#3: immediate investigations • current guidelines for single case: – enhanced surveillance + isolate storage • short interval between first cases (2 -4 d) • will not prevent second case • majority of outbreaks only 2 cases • therefore, preemptive investigations

#4 One month ceiling • current guidelines for 2 cases in 6 months: – type isolates; if same strain: • epidemiologic investigations • culturing health care workers • virtually no outbreaks with initial interval >1 month • limit investigations to cases within 1 month

#5: Tailor Investigation by Ward Surgery/Labour & Delivery Miscellaneous Wards • health care worker carriers • patient and environmental reservoirs • broad epi search for linked staff • multifaceted infection control strategies • cultures – throat, anal, vaginal, skin • test of cure for nonpharyngeal carriers – – – isolation/cohorting disinfection sterilization ward closure mass treatment

Summary • 12% of invasive group A streptococcal infections are hospital-acquired • three groups with different characteristics and outcomes – surgical (1/100, 000 surgeries) – postpartum (0. 7/10, 000 births) – non-surgical/obstetrical (largest group)

Summary • 10% of hospital-acquired cases are associated with outbreaks – 90% of hospital-acquired cases are sporadic • when outbreaks do occur they are smaller and shorter than those in the literature

Summary • these complementary data sources lead to 5 recommendations: – 1: include all hospital cases in guidelines – 2: isolate necrotizing fasciitis – 3: immediate investigations after 1 case – 4: one month ceiling for linked cases – 5: tailor investigations & management to ward

Acknowledgements • • Dr. Allison Mc. Geer Dr. Donald Low Karen Green Ontario Group A Streptococcal Study Group





