Hematologic Emergencies Tarek Elrafei D O HematologyMedical Oncology

















































- Slides: 54

Hematologic Emergencies Tarek Elrafei, D. O. Hematology/Medical Oncology

Hem/Onc Emergencies • Crises in sickle cell disease • Management of transfusion reactions • TTP • DIC • Cytopenia or Hyperleukocytosis – Febrile neutropenia – Acute leukemia with Hyperleukocytosis • Metabolic – Hypercalcemia – Tumor lysis syndrome • Compressive or Obstructive syndromes – – – Spinal Cord compression SVC syndrome Urologic Pericardial Central airway

Sickle Cell Disease • Which hemoglobin phenotype(s) are associated with ACS? • Are there any laboratory/diagnostic tests that can screen for ACS? • What is the best treatment modality for severe crises – simple vs exchange transfusion? Chest 2000 May; 117(5): 1386 -92 NEJM 2000; 342: 1855 -65

COMPLICATIONS IN SCD • • • Acute painful crises Acute chest syndrome (ACS) Renal complications Stroke Ostenecrosis of the head of the femur/humerus Sickle sequestration in the liver Sickle sequestration in the spleen Leg ulcers Priapism

PRESENTATION OF ACS • New infiltrate – pleural effusion (56%) AND… • Chest pain, cough, tachypnea, or wheezing OR • Fever > 38. 5 • Drop in Hb (< 2 g) and platelets (<175, 000) Vichinsky et al, NEJM: 342; 25. 1855 -1865

Differentiating Acute Chest Syndrome vs. Pneumonia in SCD • Low yield of bacterial diagnosis, even with broncoscopy and lavage. • Involvement of basal lobes and bilateral • Dramatic effect of exchange transfusion • In SCD, but not in other patients, sickle cells are trapped on the alveoli wall, become deoxygenated and incapable of exiting.

Other characteristics of ACS • Most common cause of death in SCD young adults in spite that it is treatable complication. • Second most common cause of hospitalization, . • Preceded or followed by acute painful crises. • After first ACS, repeat episodes are common • ACS can lead to pulmonary hypertension.

Etiology • Fat embolism Alveolar macrophages in 77% who had BAL • Viral: RSV, Parvo, Influenza, HSV, Echo, Rhino, CMV, EBV • Atypical bacteria: Mycoplasma, Atypical Mycoplasma, Chlamydia, Mycobacterium • Bacteria: Coag +Staph, Strep pneumonia, H Influenza, Legionella, pseudomonas, H Para-influenza, enterobacter, Klebsiella, Branhamella Catarrhalis, Serratia. • 23 -62% unknown

FAT EMBOLI PRESENTATION • The most severe form of ACS, with longer hospital stays and high mortality when misdiagnosed. – Lower mean oxygen saturation – Higher incidence of vaso-occlusive events • Fat emboli originate in marrow undergo infarct/necrosis with release of a combination of fat and hemopoietic precursors into the circulation. • Unique is the trapping of fat/cells in lung alveoli and sometimes the brain (confusion and ministrokes/hypoxia by imaging) • Frequently associated with sternal pain.

Is there a reliable screening test to predict impending ACS?

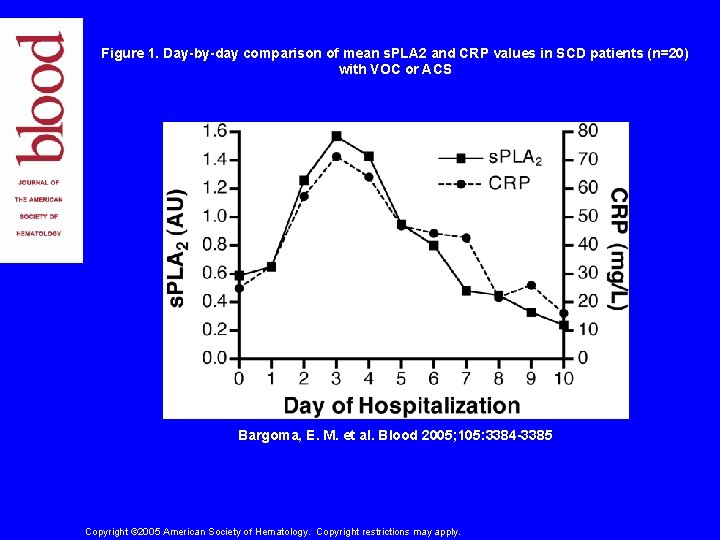
Secretory Phospholipase A 2 (s. PLA 2) • s. PLA 2 is a potent inflammatory mediator – s. PLA 2 hydrolysis of phospholipids acute lung injury – ACS patients have s. PLA 2 levels which correlate with severity of lung injury – SPLA 2 rise occurs 24 -48 hours prior to ACS – Transfusions rapidly lowers the plasma level of s. PLA 2 in ACS. • “Increased levels of s. PLA 2 are capable of predicting impending ACS, and qualify it as a screening tool. ” Styles et al. Blood. 1996; 87: 25732578

Figure 1. Day-by-day comparison of mean s. PLA 2 and CRP values in SCD patients (n=20) with VOC or ACS Bargoma, E. M. et al. Blood 2005; 105: 3384 -3385 Copyright © 2005 American Society of Hematology. Copyright restrictions may apply.

Treatment of ACS • Treatment: – – Analgesics Broad-spectrum antibiotics Bronchodilator and incentive spirometry Simple or exchange transfusion • Simple: – when blood deoxygenation is not getting worse fast. • Exchange: – When O 2 sat is 87 or lower and falling within 6 hrs. – When patient is confused (fat emboli). – When sternal pain is present (fat emboli) • Bronchoscopy is recommended in patients with no response to initial therapy

Summary • Patients with any of the sickle cell disease Hgb phenotypes (SS, SC, S-ß thalassemia) can develop acute chest syndrome (ACS) • ACS is predominantly a clinical diagnosis – New pulmonary infiltrate accompanied by fever, chest pain or respiratory symptoms – usually preceded by VOC • RBC Exchange transfusion may be life saving in severe cases

Transfusion Reactions

Risk of Blood Transfusion • Infection • Transfusion related – – ABO Incompatible Acute Lung Injury (TRALI) Anaphylaxis Circulatory Overload • Total • 5: 10, 000 • 3: 10, 000 – – 1: 12, 000 1: 10, 000 1: 150, 000 1: 10, 000 • 8: 10, 000 U. S. Genreal Accounting Office, February 1997 Blood Supply; Transfusion-Associated Risks (GAO/PEMD – 97 -2)

Relative Risk of Transfusion Complications Occurrence • • • Death from transfusion Acute hemolytic reaction HBV via transfusion HCV HIV West Nile virus Anaphylaxis Annual risk of fatal accidents at home MVA Being murdered in Washington, D. C. Risk • • • 1: 100, 000 -200, 000 1: 20, 000 1: 50, 000 1: 100, 000 -300, 000 <1: 1 Million • • 1: 125, 000 1: 10, 000 1: 2, 155 Lee, Paling, Blajchman (1998) Transfusion, 37; 184

Acute Hemolytic Transfusion Reactions • Major AB in recipient plasma + Donor RBC with corresponding antigen • Minor Antigen on recipient RBC + Donor AB • Interdonor AB in donor X plasma + Antigen on donor Y RBC

Transfusion Reactions • Symptoms – Chest tightness – SOB – Chills – Back pain – Hypotension – Burning at I. V.

Other Transfusion Reactions • Allergic – Ig. A deficient individuals (1: 550) – Can result in anaphylaxis • Febrile – Bacterial contamination – Secondary to developing HLA Abs to contaminating (donor) leukocytes

Transfusion Reactions Management • Stop transfusion • Start IVF to avoid hypotension, shock, renal failure • If oliguric (late phase) then may need fluid restriction and lytes monitoring • Prevention – 50% are a result of clerical errors

Transfusion Reaction Investigations • Tbili & LDH – with hemolysis • Urine – Hemoglobinuria when free Hgb > 25 mg/d. L – Hemosiderinuria once plasma Hgb > 50 mg/d. L • Serum Haptoglobin with hemolysis because binds to free Hgb • Coombs test • Blood type

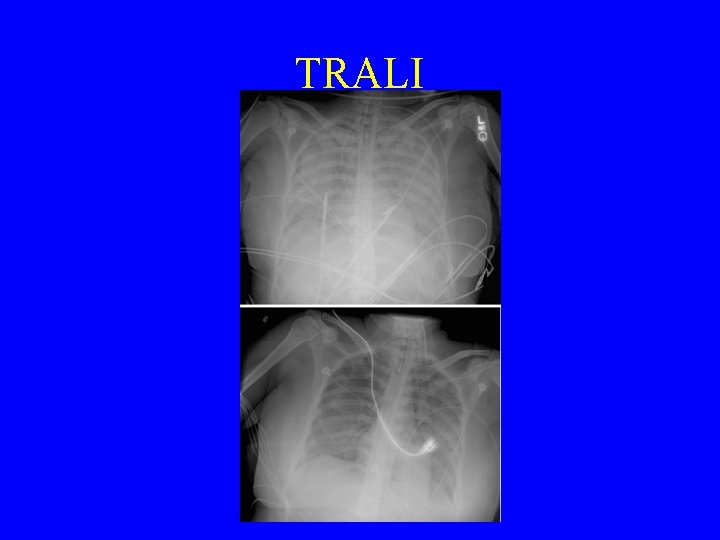
TRALI • Defined as noncardiogenic pulmonary edema temporally related to the transfusion of (plasma-containing) blood products • Mechanism: pulmonary leukoagglutinin reaction • Criteria for ALI * 1. Acute onset of lung injury (1 -6 hours after transfusion) 2. Measured PA occlusion pressure ≤ 18 mm Hg or a lack of clinical evidence of left atrial hypertension (ie, no circulatory overload) 3. Bilateral pulmonary infiltrates seen on frontal chest radiograph 4. Hypoxemia: Pa. O 2/FIO 2 <300 mm Hg, or O 2 saturation ≤ 90 percent on room air • Symptoms include dyspnea, cough, and fever – • • Onset Bilateral pulmonary infiltrates Risk factors are cardiac disease and hematologic malignancy or a predisposing inflammatory condition present in the OR or ICU *Transfusion 2004; 44: 1774. 5 -8% mortality

TRALI

TRALI Diagnostic Algorithm Chest. 2004 Jul; 126(1): 249 -58.

TRALI Treatment • Make the correct diagnosis • IV fluid administration • Supplemental oxygen/mechanical ventilation • Diuretics relatively contraindicated • Glucocorticoids? ?

Summary • Transfusion reactions may be due to incompatibility, Ig. A deficiency, allergy, or rarely bacterial contamination • Major hemolytic transfusion reactions may progress to hypotension and shock • Prevention should be aimed at minimizing unnecessary transfusions and eliminating clerical errors


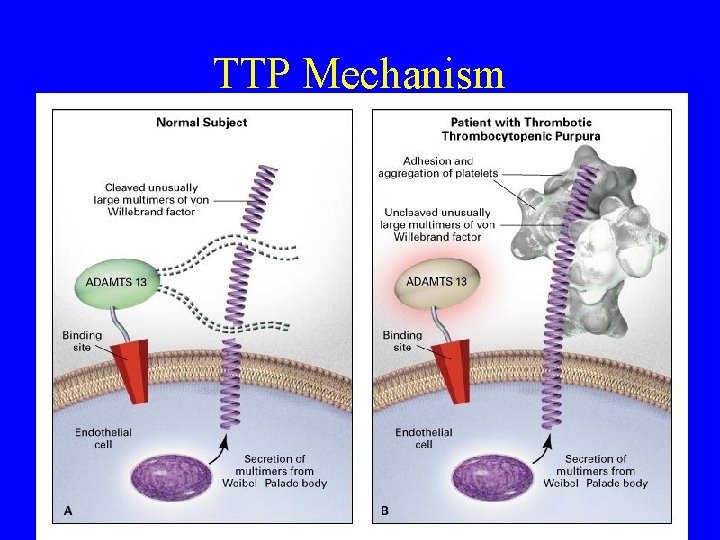
TTP • Is a syndrome of target-organ dysfunction caused by marked platelet aggregation in the microcirculation • Explained by an acquired or inherited absence of VWf cleaving protease resulting in ULVWf – The plasma metalloprotease ADAMTS 13 (A Disintegrin And Metalloprotease with Thrombo. Spondin type 1 motif 13)

TTP Mechanism

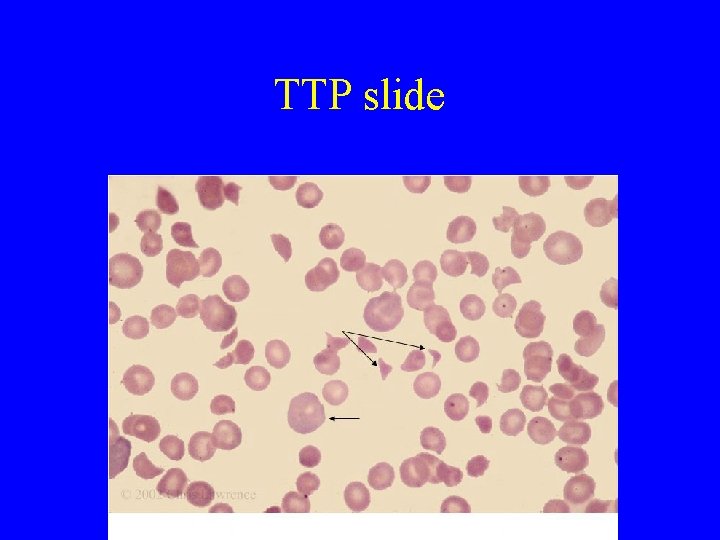
TTP slide

Red Cell Fragmentation • Traumatic Prosthetic Heart Valves March hemoglobinuria • Infections Clostridia sepsis Malaria • Microangiopathic

Microangiopathic Hemolytic Anemia • • Vasculitis Malignant hypertension Disseminated Intravascular Coagulation Thrombotic Microangiopathies – Hemolytic Uremic Syndrome – Eclampsia & HELLP Syndrome – Thrombotic Thrombocytopenic Purpura – Cancer-associated HUS

Treatment options for TTP • Plasma exchange Canadian Apheresis Study Group N Engl J Med. 1991 Aug 8; 325(6): 393 -7. • • • Plasma infusion NO platelet transfusion! Immunosuppresion with corticosteroids Antiplatelet drugs Splenectomy Rituximab

Apheresis in TTP • Probably acts to supply v. WF protease and remove its inhibitor • Procedures are done daily • FFP is the replacement fluid • Endpoint is a normal platelet count, LDH

Venous Access • Two large, durable peripheral veins • Central line with at least a dual lumen – Femoral versus subclavian • Femoral increases thrombosis and infection • JAMA. 2001 Aug 8

Complications of femoral and subclavian venous catheterization in critically ill patients Merrer, J. et al. JAMA 2001; 286: 700 -707. Copyright restrictions may apply.

Infectious complications of central venous access

Complications of plasma exchange in 71 consecutive patients treated for clinically suspected thrombotic thrombocytopenic purpura-hemolytic-uremic syndrome Transfusion 40 (8), 896– 901

Complications of Plasmapheresis related to central venous catheter access or plasma • Twenty-one patients (30%) had 27 major complications, which caused two deaths. • The major complications included 2 episodes of hemorrhage after subclavian line insertion (1 death), 1 pneumothorax requiring a chest tube, 12 systemic infections (1 death), – 7 episodes of catheter thrombosis requiring removal of the central venous catheter, 2 episodes of venous thrombosis requiring anticoagulant treatment, 2 episodes of hypoxemia and hypotension, and 1 episode of serum sickness. • Minor complications occurred in 22 additional patients (31%). • Twenty-eight patients (39%) had no complications.


DIC

Disseminated Intravascular Coagulation (DIC) • A heterogeneous group of clinicopathologic syndromes • Characterized by dysregulated generation of thrombin (pathologic thrombin formation) • Leading to intravascular fibrin formation, and • Secondary fibrinolysis (plasmin generation), • Often resulting in hemorrhage, thrombosis, and/or multi-organ system failure

Routine Laboratory Investigation • • CBC, peripheral smear PT/a. PTT Fibrinogen, thrombin clotting times FDPs, fibrin D-dimer

Tests for DIC D-dimer * FDP Platelet count Fibrinogen PT/INR a. PTT *more specific for DIC • Highest Sensitivity • Lowest Sensitivity

Specialized Tests • Coagulation factor levels • Natural anticoagulant levels: – Protein C, Protein S, antithrombin • ‘Paracoagulation’ assays (e. g. protamine sulfate paracoagulation test) • Molecular markers of: – Thrombin generation – Factor Xa generation – Thrombin action of fibrinogen • Fibrinolytic system – Plasminogen, -2 antipalsmin, PAI-1, etc – Molecular markers of plasmin activation: plasmin-antiplasmin complexes, fibrin Bbeta-42 peptide

Some Causes of DIC • Infections – Bacteremia – Rickettsial infections • Metabolic disorders – Hypotension – Hypoxia – Hyper/hypothermia • Obstetrical complications – – – Placental abruption Placenta previa Pregnancy-induced HTN Amniotic fluid embolism Retained dead fetus • Vascular abnormalities • Tumors – Adenocarcinoma – Tumor Lysis Syndrome – AML: M 3(APL), M 4 or M 5 • Trauma – Crush injuries – Head injuries • Toxins – Viper venom bites • Drugs – L-asparaginase – Prothrombin complex concentrates – Heparin (via HIT)

Pathogenesis of DIC 1. Depletion of hemostatic factors – Hypofibrinogenemia (e. g. , ‘defibrination’ syndrome, especially placental abruption and certain snakebites) – Thrombocytopenia – Generalized depletion of multiple coagulation factors 2. Depletion of inhibitors – Potential for bleeding • Depletion of 2 -antiplasmin (unchecked plasmin action) – Potential for thrombosis • • Depletion of antithrombin (unchecked thrombin action) Depletion of protein C/protein S (unchecked thrombin generation) 3. Heterogeneous ‘triggers’ of DIC

Pathogenesis of DIC: Heterogeneous triggers • Systemic activation of hemostasis – Tissue thromboplastin (released by tissue injury, placental abruption, tumors, etc. ) – Cytokines (septicemia, inflammatory states) – Direct activator of Factor X (adenocarcinoma) – Prothrombin activation (Ecchis carinatus snake venom) – Procoagulant platelet membranes (HIT) – Endothelial injury or activation (infections, HIT) • Localized activation of hemostasis – Abdominal Aortic Aneurysm – Giant hemangioma syndrome

Treatment of DIC: Special Situations • Prohemorrhagic patients – Placental abruption: obstetrical intervention, treat defibrination (cryoprecipitate) – Prostate CA with hyperfibrinolysis: Replace fibrinogen (cryoprecipitate), antifibrinolytic therapy (tranexamic acid, -aminocaproic acid) – Acute Promyelocytic Leukemia: All-trans-retinoic acid (ATRA)

Treatment of DIC: Special Situations • Prothrombotic patients – Adenocarcinoma (Trousseau’s syndrome): Heparin, avoid warfarin – Septicemia with acral gangrene (purpura fulminans): Vitamin K, heparin, FFP, recombinant activated protein C concentrates (Drotrecogin alfa) – Heparin-induced thrombocytopenia: Unusual DIC picture with increased thrombin generation without low fibrinogen, PT, a. PTT, THUS use agent that reduces thrombin generation (lepirudin, argatroban, danaproid)

Recombinant Human Activated Protein C N Engl J Med. 2001 Mar 8; 344(10): 699 -709. • 1960 patients – Known infection – > 3 signs of systemic inflammation AND sepsis -induced dysfuncion of one organ system • Drotrecogin alfa or placebo infusion • Relative risk reduction of death = 19. 4% (absolute reduction = 6. 1%) • 3. 5% vs 2% serious bleeding

Summary • In SCD crises RBC exchange transfusion can be life saving • Transfusion reactions – Hemolytic reactions can be due to incompatibility, Ig. A deficiency, allergy, or rarely bacterial contamination of blood product – The key to diagnosis and treatment of TRALI is a high clinical suspicion and the need to exclude cardiogenic pulmonary edema or volume overload

Summary • TTP – Is a disorder of marked platelet aggregation which can be worsened by platelet transfusion – Must differentiate from other causes of MAHA – Plasmapheresis is the treatment of choice • DIC – Can manifest as uncontrolled bleeding, excessive clotting, and/or multi-organ system failure – Treatment of underlying cause is of central importance. Select cases may benefit from APCC