Genetics and Ovarian Cancer June 16 2015 Ovarian












- Slides: 20

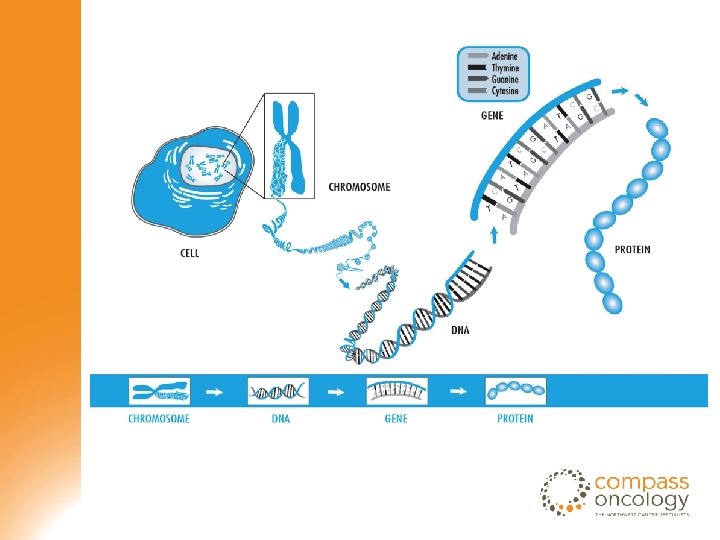
Genetics and Ovarian Cancer June 16, 2015 Ovarian Cancer Alliance of Oregon and SW Washington Becky Clark, MS, CGC Genetic Counselor

Risk for Ovarian cancer • ~20% of ovarian cancers are related to an inherited cancer syndrome • ~80% of ovarian cancers are sporadic Your relative with ovarian cancer Your risk None 1% Mother/Sister 4 -6% Grandmother/Aunt 1 -2%



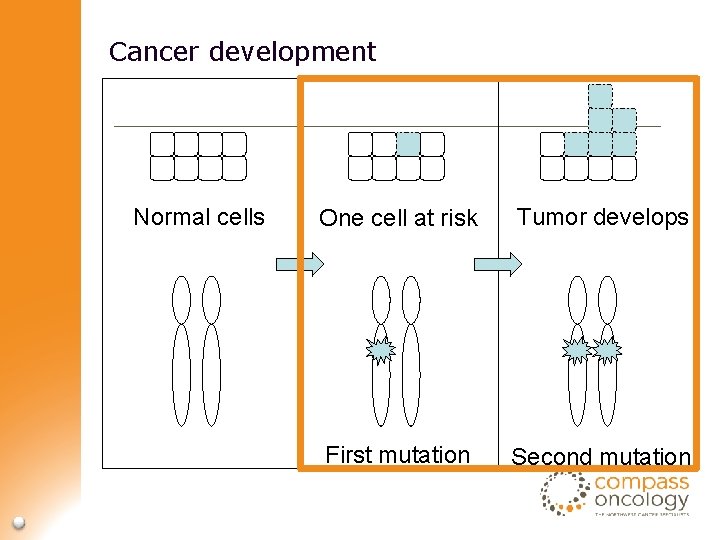
Cancer development Normal cells One cell at risk Tumor develops First mutation Second mutation

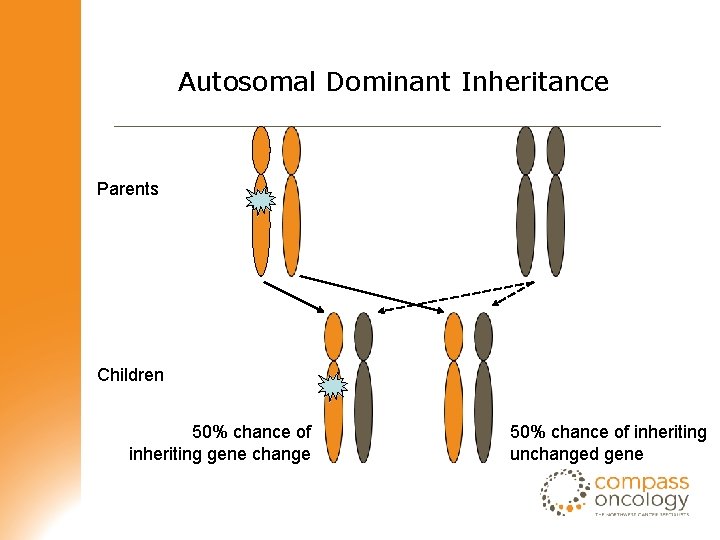
Autosomal Dominant Inheritance Parents Children 50% chance of inheriting gene change 50% chance of inheriting unchanged gene

Gene mutations increasing risk for ovarian cancer • Hereditary breast and ovarian cancer syndrome • BRCA 1, BRCA 2 • Lynch syndrome • MLH 1, MSH 2, MSH 6, PMS 2, EPCAM • • • • BARD 1 BRIP 1 CDH 1 CHEK 2 MRE 11 A MUTYH NBN PALB 2 RAD 50 RAD 51 C RAD 51 D STK 11 TP 53

Goals of genetic testing • Understand cause of cancer in family • Surveillance and prevention of other cancers • Allow unaffected family members to test • Surveillance • Prevention options • Family planning

Hereditary breast and ovarian cancer syndrome: BRCA 1 and BRCA 2 Prevalence in the general population: ~1 in 400 Prevalence in the Ashkenazi Jewish population: ~ 1 in 40 Consider when history includes one of the following: • Ovarian cancer at any age • Breast cancer at or before age 50 • Triple negative breast cancer at or before age 60 • Two primary breast cancers in the same person or on the same side of family • Breast and ovarian cancer in the same person • ≥ 3 relatives with breast, ovarian, pancreatic cancer and/or aggressive prostate cancer on the same side of family • Ashkenazi Jewish Ancestry and a personal or family history of breast, ovarian or pancreatic cancer • Male breast cancer

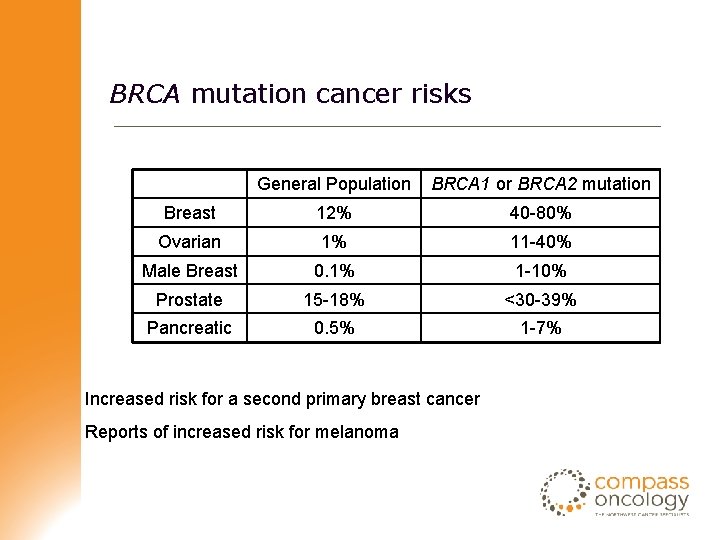
BRCA mutation cancer risks General Population BRCA 1 or BRCA 2 mutation Breast 12% 40 -80% Ovarian 1% 11 -40% Male Breast 0. 1% 1 -10% Prostate 15 -18% <30 -39% Pancreatic 0. 5% 1 -7% Increased risk for a second primary breast cancer Reports of increased risk for melanoma

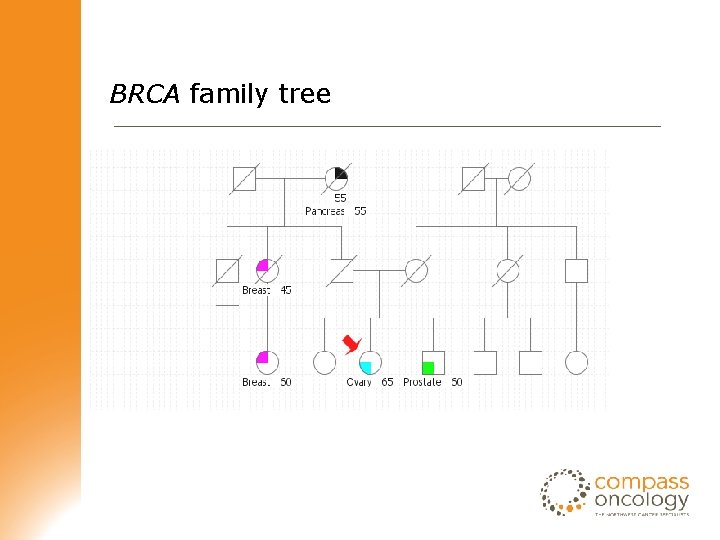
BRCA family tree

Lynch syndrome: MLH 1, MSH 2, MSH 6, PMS 2, EPCAM Consider when history includes one of the following: • Colon cancer before age 50 • Uterine cancer before age 50 • ≥ 2 Lynch cancers in the same person • ≥ 2 relatives with a Lynch cancer, one <50 years old • ≥ 3 relatives with a Lynch cancer at any age • Abnormal MSI and/or IHC tumor test result • Performed on colon and uterine tumors

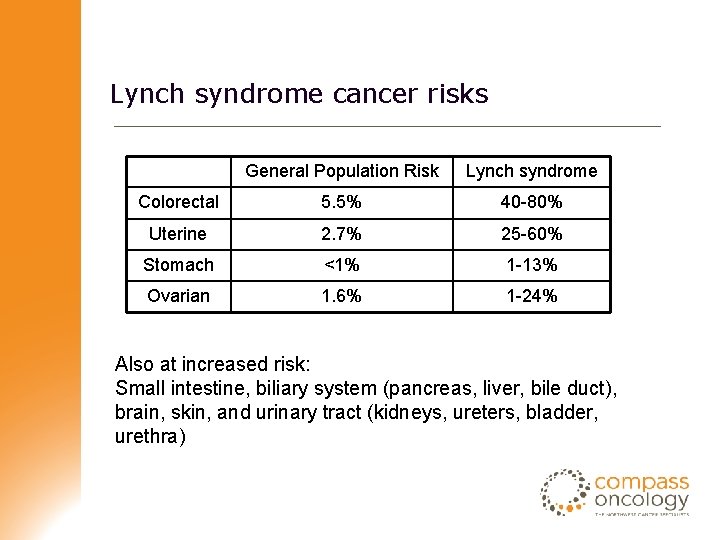
Lynch syndrome cancer risks General Population Risk Lynch syndrome Colorectal 5. 5% 40 -80% Uterine 2. 7% 25 -60% Stomach <1% 1 -13% Ovarian 1. 6% 1 -24% Also at increased risk: Small intestine, biliary system (pancreas, liver, bile duct), brain, skin, and urinary tract (kidneys, ureters, bladder, urethra)

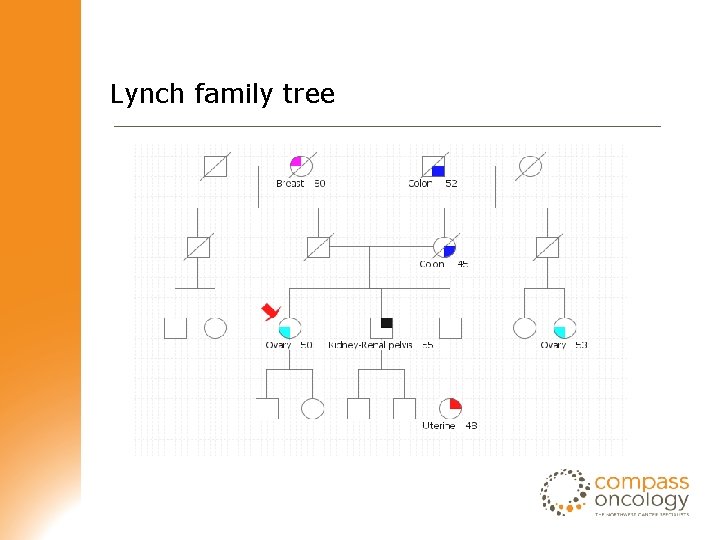
Lynch family tree

Genetic testing for ovarian cancer • Ashkenazi Jewish? Start with the three founder mutations in BRCA 1 and BRCA 2 • Testing to include BRCA 1, BRCA 2, and Lynch syndrome • Recent availability of panel tests: covers BRCA 1, BRCA 2, Lynch syndrome, and other more rare, lower risk genes • Single site testing for family members if relative tests positive

Insurance coverage • Covered benefit if medical criteria is met (NCCN criteria). Some insurance have their own criteria. • Always pre-authorized by the genetic testing lab • Out of pocket cost depends on your insurance plan • Discounted prices for those without insurance coverage

Laws that protect against genetic discrimination in health insurance and employment • HIPAA: Health Insurance Portability and Accountability Act • Federal law • GINA (Genetic Information Non-Discrimination Act) 2008 • Applies to family history and genetic test results • Does not cover life insurance, long-term disability • State laws • Oregon law DOES cover life insurance and long-term disability • Applies to genetic test results, not family history

Types of results from genetic testing • Negative: no mutation detected • Base cancer risks on family history • Positive: mutation detected that causes an increased risk for cancer • Follow management guidelines for care • Offer genetic testing to other family members • Variant of uncertain significance (VUS): • Change identified, but not enough evidence to determine if disease causing or benign • Identified in ~10% of tests • Cannot test family members. Exception: Family Studies Programs • VUS will be reclassified over time

Thinking about the future • DNA banking • Store DNA at a facility for future testing • Fertility preservation and family planning • Freezing eggs • Pre-implantation Genetic Diagnosis (PGD) • Prenatal testing (amniocentesis)

Contact Compass Oncology GREAT Program Genetic Risk Evaluation & Testing Lucy Langer, MD, MSHS Becky Clark, MS, CGC Lisa Clark, FNP, AOCNP, APNG Phone: 503 -297 -7403