The Trials and Tribulations of Code Capture in

The Trials and Tribulations of Code Capture in Radiation Oncology SROA 32 nd Meeting October 18, 2015 San Antonio 1

Disclosure • ROC © works with many cancer centers, societies, and physicians. • This presentation will address objectives that have been outlined in the next slide and will not address specific manufacturers. • Special Thank you to Kevin Ewalt, CEO of Radmax, LTD. – kevin. ewalt@radmaxonline. com/877. 839. 9517 2

Objectives To Compare and Contrast: • Technical Charge Capture • Professional Charge Capture • Split Billed Environment • Global Billed Environment 3

Technical Charge Capture • Hospital Settings: Split Billed Environments • Technical Component Only • Technical Component (TC) • Use of equipment and supplies • Employment of the RTT to administer treatments • Hospitals fall under different rules than Freestanding Centers 4

Professional Charge Capture • Hospital Settings: Split Billed Environments • Professional Component (26) Modifier • Services Provided by the Physician • Supervision of Staff • Documentation in Medical Record • Example 77280 -26 5

Technical Charge Capture • Hospital Settings: Split Billed Environments • Technical Component Only • Technical Component (TC) • Use of equipment and supplies • Employment of the RTT to administer treatments • Hospitals fall under different rules than Freestanding Centers • Example: 77280 TC (insurance only pays technical) 6

Split Billed Environment • Technical Billing is separated from the Professional Billing • Professional Billing Codes, that contain a technical component are differentiated with a 26 modifier • Technical Billing is captured in hospital departments and goes to the hospital billing system where the codes are “scrubbed” for CCI edits • Example 77280 TC and 77280 -26 7

GLOBAL Billed Environment • Technical Billing is combined the Professional Billing • Bill with one CPT code • Example: 77280 8

Radiation Oncology CPT 2015 Codes • Sixty three specific radiation oncology codes exist • Of these codes Hospitals or centers for radiation therapy may report 19 technical-only codes • The radiation oncologist has access to all 99000 series E /M Codes (18 commonly used) • The radiation oncologist may also utilize other specific codes from other specialties • The Physician is ALWAYS Responsible for every event that gets captured. 9

Hospital Technical Charge Capture • Radiation Oncology is a department of the hospital • Requires a different billing form- UB 04 • Follow the Medicare 72 hour rule • Charges are billed under hospitals’ Tax ID number • Follows policies and procedures • Bills Technical Component of Charges 10

Freestanding Center (compared to Hospital) • Separate Entity • Bill charges under own Tax ID • Separate Board of Directors • Has own policies and procedures • Usually bills Globally (combines technical and professional) 11

Freestanding (continued) • Can be owned by a hospital • Must run independently • Can be both technical facility based) and/or (UB 04) • Professional (Physician) charges (HCFA 1500) • May be combined (Global) • Depends on Ownership 12

HOSPITAL BILLING FORM (UB 04) UB 04 Billing Form used to bill hospitalbased outpatient radiation therapy technical charges. • American Hospital Association (AMA) and National Uniform Billing Committee controls UB 04. • Electronic Billing 837 I. 13

HOSPITAL BILLING FORM (UB 04) – Medicare requires electronic submission initially. – Unless the provider qualifies as exempt with the Administrative Simplification Compliance Act (ACSA). – No waiver request necessary if institution is less than 25 FTE’s. – Timely filing is required by most carriers. – Medicare requires claims be submitted within 12 months of date of service. – Line item ‘from’ date on claim form (single day). – Line item ‘through’ date on claim form (date span). 14

HOSPITAL BILLING FORM (UB 04) What can be billed on a UB 04 form? • Hospital technical charges only (Part A). • Hospitals can NEVER bill Globally • Physicians charges can NEVER be billed as Part A – NOTE: any hospital who employs a physician (or physician group) must still bill the professional component separately on a 1500 form using a -26 modifier. 15
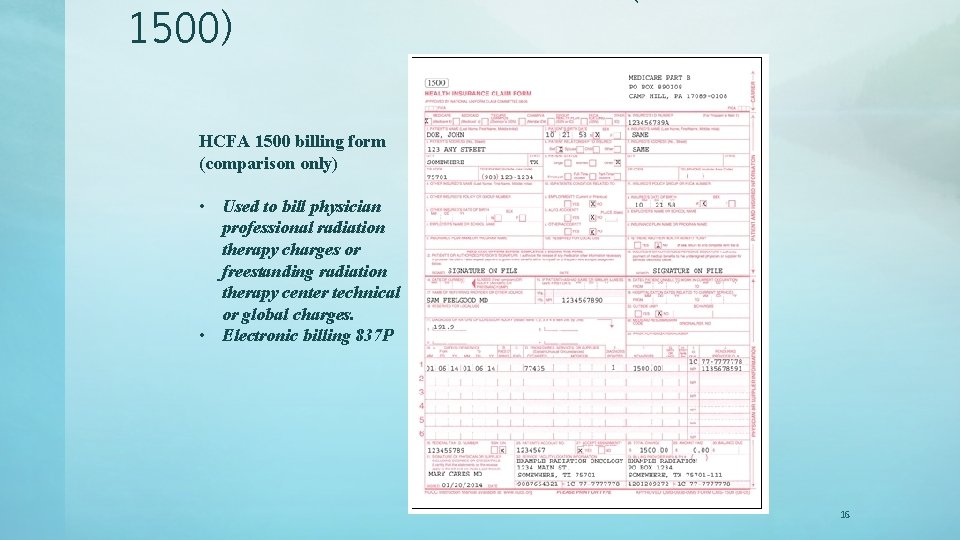

1500) HCFA 1500 billing form (comparison only) • Used to bill physician professional radiation therapy charges or freestanding radiation therapy center technical or global charges. • Electronic billing 837 P 16

PHYSICIAN BILLING FORM (HCFA 1500) • What can be billed on a 1500 HCFA form? – Physician PROFESSIONAL charges. – Does not matter whether they work in a hospital or are employed by a hospital. – Technical freestanding cancer facility charges are also paid as “fee for service. ” – Part B. – Global Billing (pro/tech). – Freestanding cancer center “if” the docs are either employed by the center or have ownership. – In many cases you see “split-billing” (pro-26/tech-TC) if the physician group is not employed by the facility or does not have ownership in that facility. 17

BILLING SCENARIOS – If you are billing charges for the technical hospital portion only, which form would you use? – UB 04 and billed “under” the hospital’s TAX ID number. – The only time this does not apply is if the hospital cancer center is a free-standing facility with its own Tax ID (different from the hospital). In that case hospital technical charges would be billed on a HCFA 1500 form using a TC modifier. – What about a physician(s) treating at a hospital but “not” employed by the hospital? – Either way you would bill professional charges separately on a HCFA 1500 form using a -26 modifier. – Can a hospital bill Globally (Pro/Tech together)? – NO (and NO) 18
![HOSPITAL BILLING TERMS • HOSPITAL OUTPATIENT PROSPECTIVE PAYMENT SYSTEM (HOPPS [or OPPS]) – System HOSPITAL BILLING TERMS • HOSPITAL OUTPATIENT PROSPECTIVE PAYMENT SYSTEM (HOPPS [or OPPS]) – System](http://slidetodoc.com/presentation_image/478cdaead2e634fd33bc66fe29976336/image-19.jpg)
HOSPITAL BILLING TERMS • HOSPITAL OUTPATIENT PROSPECTIVE PAYMENT SYSTEM (HOPPS [or OPPS]) – System was implemented August 1, 2000 by the Centers for Medicare and Medicaid Services (CMS) to reimburse hospital “outpatient” services. – Congress mandated that CMS develop a system to reduce beneficiary co-payments. – HOPPS bases payments on geometric mean costs. – Claims are matched to cost reporting data filed by individual hospitals. – NOTE: radiation therapy is paid per ‘line-item’ unlike most hospital out patient services. 19

HOSPITAL BILLING TERMS • OUTPATIENT QUALITY REPORTING (OQR) – HOPPS Conversion Factor: – Hospitals that meet the OQR requirement will see an increase in their 2014 conversion factor from $72. 672 to $74. 144 (or +2. 2%) in 2015. – Hospitals that fail to meet the reporting requirements for outpatient services will see a reduction in the conversion factor to $71. 661. 20

Hospital Billing Terms • PAYMENT TO COST RATIO (PCR) – For cancer hospitals CMS provides additional payments to offset other HOPPS hospitals. – Offsets losses in cancer centers that are spending greater than 1. 75 times the APC payment amount and the $2, 775 fixed-dollar threshold over the APC payment rate. – Payment = 50% of the amount that the hospital exceeds cost of services that exceed 1. 75 x’s the APC rate (when both the 1. 75 multiple threshold and the fixed dollar threshold are met) / Formula = (cost-(APC payment x 1. 75))/2. – NOTE: only eleven (11) cancer hospitals fall under this policy in the US. 21

Professional Billing Terms MEDICARE PHYSICIAN FEE SCHEDULE (MPFS) • Comparison Only: • Freestanding Centers our paid ‘FEE FOR SERVICE” PER PROCEDURE (CPT) • Medicare PART B pays for physician services based on PFS • Over 7, 400 unique covered services 22

Professional Billing Terms MEDICARE PHYSICIAN FEE SCHEDULE (MPFS) Payment rates for an individual service are based on the following: 1. Relative Value Units (RVU) including work RVU, Practice Expense (PE) RVU, and Malpractice (MP) RVU. 2. Conversion Factor (CF). 3. Geographic Practice Cost Indices (GPCI). 23

HOSPITAL BILLING TERMS • DIAGNOSIS RELATED GROUP (DRG) – Medicare Hospital Inpatient Payment Methodology – Established in the 1970’s and implemented in 1982 to encourage access to care, rewards efficiency, improves transparency, and improves fairness by paying similarly across hospitals for similar care. – Was initiated in much the same way as packaging to make hospitals contain their costs/spending and shorten patient length of stay (hospitalization). – Paid on a per diem rate per patient (per product) for highest level of complexity. 24

HOSPITAL BILLING TERMS • DIAGNOSIS RELATED GROUP (DRG) – Medicare Hospital Inpatient Payment Methodology – Established in the 1970’s and implemented in 1982 to encourage access to care, rewards efficiency, improves transparency, and improves fairness by paying similarly across hospitals for similar care. – Was initiated in much the same way as packaging to make hospitals contain their costs/spending and shorten patient length of stay (hospitalization). – Paid on a per diem rate per patient (per product) for highest level of complexity. 25

HOSPITAL BILLING TERMS • AMBULATORY PAYMENT CLASSIFICATIONS (APC) – APC’s are units of payment under the OPPS. – APC’s are a system of classification where CPT codes are concerted into APC groupings for reimbursement for hospital outpatient type services. – APC’s consolidate reimbursement for services that are similar in nature. – Example: 77280 (Simulation: Simple Confirmation) and 77336 (Physics Consultation) are both APC 0304 and pay the same reimbursement of $113. 12 (2015). – Note: most radiation therapy is still paid “per line item. ” 26

HOSPITAL BILLING TERMS • WHAT IS A COMPREHENSIVE APC? – A Comprehensive APC produces one single payment that includes the primary service and all supporting services (date spans included). – This could be an issue for hospitals in 2015 that may bill more frequently where the primary code and supporting code(s) may be billing on different claims on different days. – CMS finalizing the policy to establish 28 Comprehensive APC’s for 2015. 27
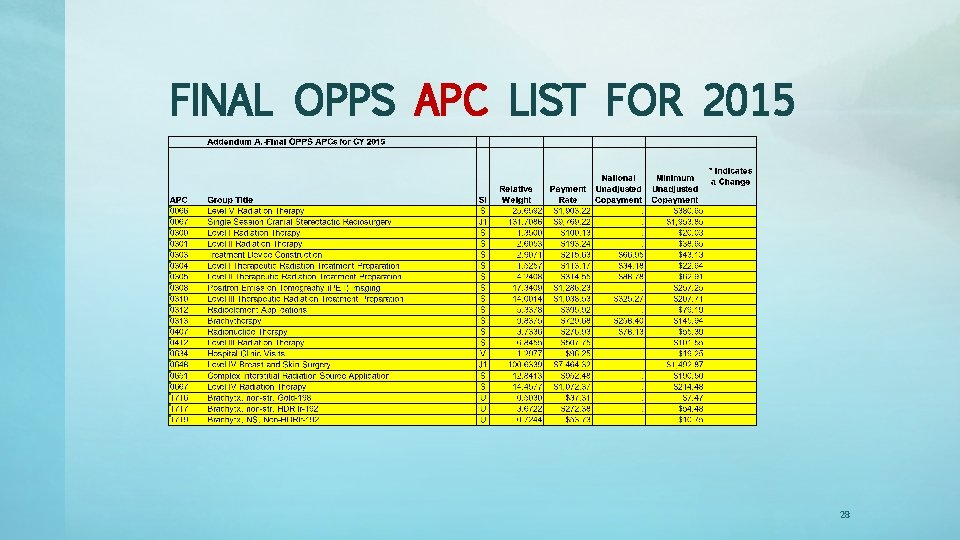
FINAL OPPS APC LIST FOR 2015 28

HOSPITAL BILLING TERMS • WHAT IS PACKAGING? – Packaging is a combination of inter-related procedures (CPT codes) performed on a single day into one ‘daily’ payment. – Purpose/Design: to motivate hospital out-patient facilities to be more cost-effective when treating patients. – The fear is hospitals will simply delay patient treatment (or spread it out) to increase reimbursement. 29

HOSPITAL BILLING TERMS • PAYMENT STATUS INDICATORS (PSI) – PSI’s are another form of grouping for Medicare payments. – Important indicator codes: – Q 1 – packaged if billed on the same DOS as codes assigned to PSI “S”, “T”, or “V”. – Q 2 – packaged if billed on the same DOS as codes assigned to PSI “T”. – Q 3 - payment is packaged into a single payment for specific combinations of services. – S – not discounted when multiple. – T – multiple procedure reductions apply. – V – clinic or ER visit. 30

HOSPITAL BILLING TERMS • PSI Q 3 (Codes That May Be Paid Through a Composite APC): – Composite APC payment based on OPPS compositespecific payment criteria. – When services are completed in a single hospital encounter payment is made through a separate APC composite payment. Payment is packaged into a single payment for specific combinations of services. 31
![HOSPITAL BILLING TERMS • PSI “J 1” (Part B [Comprehensive APC]). – All Part HOSPITAL BILLING TERMS • PSI “J 1” (Part B [Comprehensive APC]). – All Part](http://slidetodoc.com/presentation_image/478cdaead2e634fd33bc66fe29976336/image-32.jpg)
HOSPITAL BILLING TERMS • PSI “J 1” (Part B [Comprehensive APC]). – All Part B services on the claim are packaged (one payment) with the primary "J 1" service. – Includes supporting procedures with PSI ‘N’, ‘Q 1’, and ‘Q 2’ (packaged codes). – Date spans included. – Exceptions: PSI ‘F’, ‘G’, ‘H’, ‘L’ and ‘U’ (Brachytherapy Sources). – – Ambulance services. Diagnostic and screening mammography. All preventive services. Certain Part B inpatient services. 32
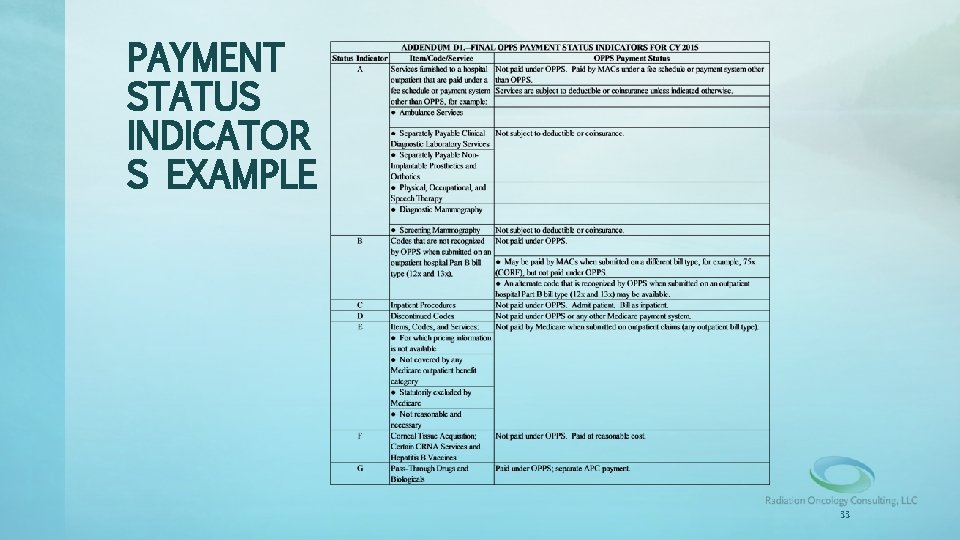

PAYMENT STATUS INDICATOR S EXAMPLE 33
![HOSPITAL BILLING TERMS • WAGE INDEX (BASED ON LAST YEAR [2014]) – Wage Index HOSPITAL BILLING TERMS • WAGE INDEX (BASED ON LAST YEAR [2014]) – Wage Index](http://slidetodoc.com/presentation_image/478cdaead2e634fd33bc66fe29976336/image-34.jpg)
HOSPITAL BILLING TERMS • WAGE INDEX (BASED ON LAST YEAR [2014]) – Wage Index for urban and rural areas based on CBSA labor market. – The Social Security Act requires that, as part of the methodology for determining prospective payments to hospitals, the Secretary must adjust the standardized amounts “for area differences in hospital wage levels by a factor reflecting the relative hospital wage level in the geographic area of the hospital compared to the national average hospital wage level. ” 34
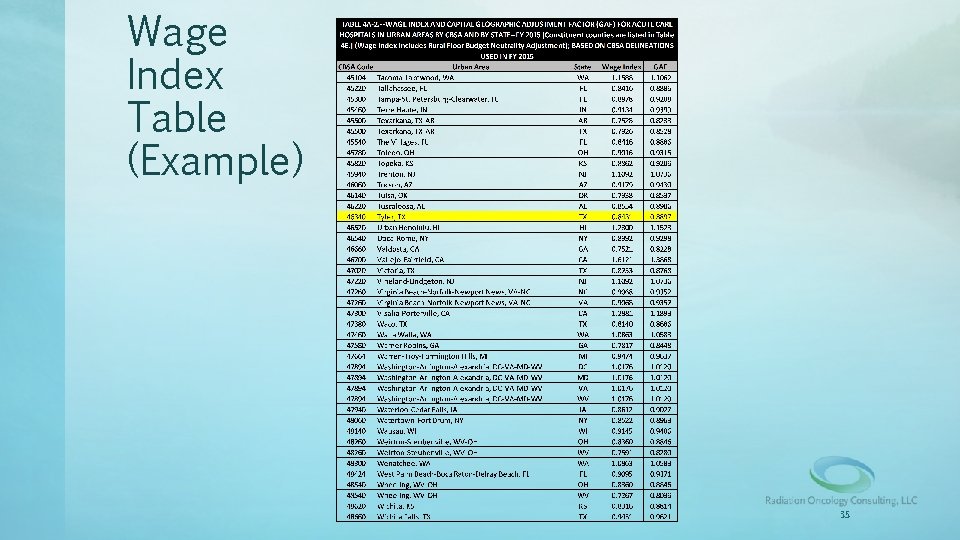
Wage Index Table (Example) 35

HOSPITAL BILLING TERMS • REVENUE CODES/COST CENTER – Describes the dollar amount charged for hospital services provided to a patient. – Tells an insurance company whether the procedure was performed in the emergency room, operating room or another department (i. e. radiation therapy). – Radiation therapy is 333 Revenue Code. – Groups similar charges onto one line in the billing form. – Example: a revenue code attached to a supply code identifies the equipment and whether the equipment was used in the hospital or taken home by a patient. 36

Revenue Codes (Example) 37

FINAL HCPCS CODES FOR 2015 • What is the calculation for determining your local Medicare reimbursement? – Most recent CF (Conversion Factor) X’s HCPCS Code RW (Relative Weight) = NR (National Reimbursement). – Take your NR X’s your local WI (Wage Index) to get your local Medicare reimbursement. – Example: – 77301 (Radiotherapy Dose Plan IMRT) RW (14. 0014) X’s CF (74. 144) = $1, 038. 12 (NR). – $1, 038. 12 (NR) X’s WI (Tyler, TX = 0. 8431) = $875. 24. 38
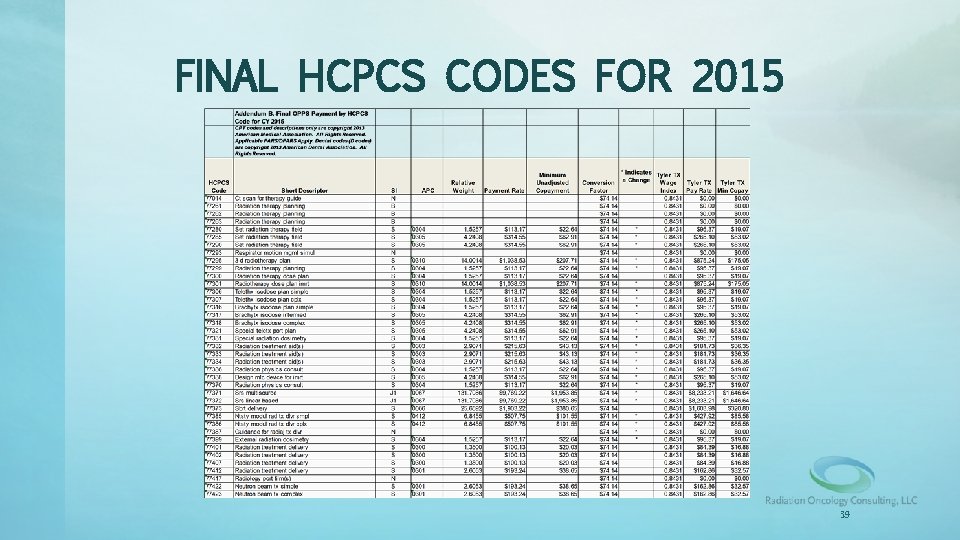
FINAL HCPCS CODES FOR 2015 39

HOSPITAL BILLING REVENUE • For those of you working in a radiation therapy hospital-based department, determining your bottom line (cash flow) can be next to impossible! Why is this? – Most hospital-based radiation therapy facilities are rolled up under another department like radiology. – Hospitals work on an accrual based accounting system. – “The bottom line for a hospital department is not based on actual cash-flow!” 40
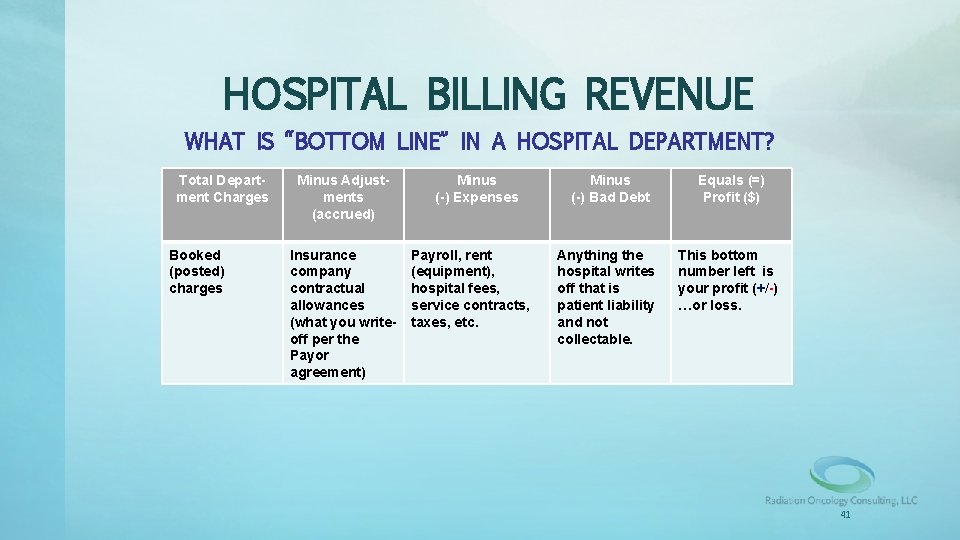
HOSPITAL BILLING REVENUE WHAT IS “BOTTOM LINE” IN A HOSPITAL DEPARTMENT? Total Department Charges Booked (posted) charges Minus Adjustments (accrued) Insurance company contractual allowances (what you writeoff per the Payor agreement) Minus (-) Expenses Payroll, rent (equipment), hospital fees, service contracts, taxes, etc. Minus (-) Bad Debt Anything the hospital writes off that is patient liability and not collectable. Equals (=) Profit ($) This bottom number left is your profit (+/-) …or loss. 41

HOSPITAL BILLING REVENUE • Your year-end numbers don’t necessarily reflect a true picture. – Final adjustments for things like bad debt and indigent may be adjusted. – Unlike a freestanding radiation therapy facility that takes contractual allowances (adjustments) at the time of payment (per the EOB), hospitals accrue adjustments (book in advance) based on the department’s prior history (say past six months). 42

HOSPITAL BILLING REVENUE • ACCRUAL ADJUSTMENT METHOD: – If you have a 70% write-off history on your Medicare charges, the hospital Finance Department will book (accrue) your Medicare adjustments based on that history at the time of billing. – Any discrepancies are checked (compared against real write-offs) at fiscal year-end. – You may have additional adjustments or credits depending on how accurate the accrual rate (budget) was! 43

HOSPITAL BILLING REVENUE • WHY DO HOSPITALS ACCRUE ADJUSTMENTS INSTEAD OF JUST WAITING FOR THE EOB? – Because hospitals want their contractual write-offs done as soon as possible and do not want to overstate (exaggerate) their bottom line (income). – Since most write-offs come at the time of payment (30 – 60 days out), this extends AR Days and inflates your Accounts Receivables. 44

HOSPITAL BILLING REVENUE • WHY DO HOSPITALS ACCRUE ADJUSTMENTS INSTEAD OF JUST WAITING FOR THE EOB? – If your AR is a million dollars and you only typically collect 38% of your gross charges (depends on how your charges are set), 62% of your AR is not real money! – Hospitals need to constantly estimate (predict) their “true” cash by having a much more “controllable” AR. 45

FREESTANDING BILLING REVENUE • NON HOSPITAL-BASED CANCER CENTERS (COMPARISON ONLY) – Typically a freestanding cancer center will adjust their insurance contractuals at the time of payment (not billing) and will write off bad debt based on approval. – This is typically referred to as “real-time” accounting – think check-book (money-in and money-out). – For Medicare (Government), Medicaid, and Champus some centers (freestanding) will pro-rate their payments and take the insurance contractual adjustment automatically at the time of billing. 46

HOSPITAL BILLING RULES • HOSPITAL 72 HOUR RULE – In effect since 1998 and updated July 1, 2012 with PD modifier. – Cancer hospitals are only subject to a one day payment window. – CAH’s (critical access hospitals) are exempt from this rule. 47

HOSPITAL BILLING RULES • HOSPITAL 72 HOUR RULE – Medicare’s 3 -day payment window applies to Medicare hospital outpatient Part B services and requires the hospital to bundle the technical component of all outpatient diagnostic services and related non-diagnostic services (i. e. radiation therapy) with the claim for an inpatient stay when services are furnished to a Medicare beneficiary in the 3 days preceding an inpatient admission. – Suggestion: hold charges for one week to ensure compliance with rule! 48

HOSPITAL BILLING RULES • When would a “freestanding” radiation therapy center fall under the 72 Hour Rule? – If the center is wholly owned or operated by a hospital or hospital system. – You must use a PD modifier on the UB claim form to report inclusive technical only radiation therapy services (just like a hospital-based radiation therapy department). – Professional component (physician) can still be billed and reimbursed separately. 49

HOSPITAL BILLING RULES • Definitions for the 3 Levels of Supervision – Direct: physicians/NPP must be immediately available to furnish assistance and direction throughout the performance of the procedure. – physicians or NPP is not required to be present in the room when the procedure is performed. – General: procedure is furnished under the physicians/NPP overall direction and control, but physicians/NPP presence is not required during the performance of the procedure. – Personal: physicians/NPP must be in the room during the procedure. 50

HOSPITAL BILLING RULES • RURAL OUTPATIENT SERVICES (HISTORY) – In 2012 the Advisory Panel on Hospital Outpatient Payment (HOP Panel) recommended that CMS adopt alternate supervision levels, including general supervision, for individual small and rural hospital outpatient therapeutic services. – Based on recommendations made by five hospitals who presented at the HOP Panel’s February and August 2012 meetings, CMS reduced the level of supervision for 49 outpatient therapeutic services from “direct” to “general” supervision. – American Hospital Association (AMA); 9/9/13 51

HOSPITAL BILLING RULES • 2014 CHANGED FOR RURAL HOSPITALS – Hospital outpatient radiation therapy procedure supervision rules require the physician to have “direct” supervision over patient treatment. – Critical Access Hospitals (CAH’s) and rural hospitals (< 100 beds) had been exempt from this rule prior to 2014. – There was a lot of confusion over this rule and it was mistakenly adopted by freestanding centers! 52

HOSPITAL BILLING RULES • 2014 CHANGED FOR RURAL HOSPITALS – In 2014 supervision requirements of all Critical Access Hospitals (CAH’s) and rural hospitals were enforced. – Presently radiation therapy can only be provided when there is a physician or non-physician practitioner immediately available who can provide assistance, direction, and orders. – Includes hospitals and freestanding centers! 53

HOSPITAL BILLING RULES • INCIDENT-TO SERVICES (INCLUDING CAH'S) – Must be performed by “qualified” individuals: – Example: physicists incident-to physician. – Example: therapist [RT] incident-to physician. – Has to be in compliance with the hospital’s particular State’s requirements. – Medicare had already required this. This was a regulatory change in 2014 that adopts existing requirements as a condition of getting paid and for the concern and safety of patients. 54

HOSPITAL BILLING RULES • NURSING HOMES/HOSPICE – (Comparison) freestanding cancer centers are billed using POS (Place Of Service) code ‘ 11’. – POS code 11 falls under Fee for Service Billing. – Freestanding cancer centers are considered “Out-Patient” or Medicare Part B. – Nursing homes are considered “In-Patient” or Medicare Part A. – Cannot be billed simultaneously to Medicare. – Freestanding cancer centers must bill the nursing home/hospice direct for radiation oncology therapy services. – Suggestion – work out an arrangement with Nursing Home (contract) for radiation therapy services up-front! 55

HOSPITAL BILLING RULES • NURSING HOMES/HOSPICE – Hospital-based outpatient cancer centers and nursing homes can bill patient charges “separately” (simultaneously). – Both are considered Part A. – Radiation oncology falls under Medicare Consolidated Billing (carve-out). – NOTE: for SNF /Hospice and radiation therapy treatment located on campus (same Tax ID) billing falls under 72 Hour Rule. 56

HOSPITAL BILLING • SMOKING CESSATION COUNSELING – G 0375: > 3 minutes and < 10 minutes. – G 0376: > 10 minutes are used for 2 cessation attempts or up to 8 cessation counseling sessions per year. – Medicare will allow medically necessary E/M services to be billed on the same date as tobacco cessation counseling (clinically appropriate) with modifier 25. – You will need a separate report if > 3 minutes: face-to-face patient contact by a physician or "incident to" the services of a qualified practitioner with documentation showing the intent to counsel the patient in the hopes to get him/her to stop smoking or stop using tobacco products. 57

HOSPITAL BILLING • ONE OUTPATIENT ROOM CHARGE – All HCPCS codes (five levels for new patient/established patient) were reduced to one (1) code in 2014. – No Longer Used – 99201, 99202, 99203, 99204, and 99205. – No Longer Used – 99211, 99212, 99213, 99214, and 99215. – G 0463 (hospital outpatient clinic visit for assessment and management of a patient). – 2015 APC 0634 = $96. 25. 58

HOSPITAL BILLING • G 0463 Definition – Direct contact between the patient and the physician (or other authorized person by state law or hospital bylaws). – Must coincide with a separate patient visit (consult) by the treating physician billed under his/her NPI. – Should only be billed one time (1 X) per course of treatment! – Includes items like nursing, nutrition, social work, scheduling, etc. 59

HOSPITAL BILLING • G 0463 Billing Exceptions – Patient seen in different Hospital Department on same day (modifier 27). – Laryngoscopy (modifier 25). – [example: G 0463 -25, 31575] – What rules differ from before? 1. 2. 3. Whether the physician has a new consult or follow-up visit, the hospital always bills G 0463 can be reported and paid during the global 90 day period unlike physician [not payable]. You can bill G 0643 at the patient’s six (6) month check-up visit. 60

HOSPITAL BILLING • 77293 (Respiratory motion management simulation). – Must be billed in addition to primary procedure code 77295 (3 D Plan) or 77301 (IMRT Plan) on the “Same Claim” (together). – No assigned APC code. – PSI “N” – no separate payment. – Packaged to primary procedure. 61

HOSPITAL BILLING CHANGES • PACKAGING IN 2015 – CMS will continue the five categories of ancillary support items/services that are packaged into primary diagnostic or therapeutic services (payment). 1. 2. 3. 4. 5. Drugs, biologicals, and radiopharmaceuticals used in diagnostics and procedures (does not include pass through). Drugs and biologicals used as supplies in surgeries. Some clinical diagnostic lab tests. Add-on procedures. Removal of a device. – Example: HALO for stereotactic. 62

21 HOSPITAL BILLING CHANGES • IMAGE GUIDANCE – Deleted: – 76950 (ultrasound guidance for placement of radioelements applications). – 77421 (stereoscopic x-ray guidance for localization of target volume for the delivery of radiation therapy). – 0197 T (intra-fraction localization and tracking of target or patient motion during the delivery of radiation therapy). 63

HOSPITAL BILLING CHANGES • IMAGE GUIDANCE – 77014 (therapeutic radiology for placement of radiation fields) no longer reported with IGRT: – Replaced by 77387 (guidance for localization of target volume for delivery of radiation treatment delivery). – PSI ‘N’ - packaged into the primary IMRT procedures 77385/77386 (no separate payment). – NOTE: physicians will still report 77014 -26 and will be paid separately (77387 -26 starting 2016). 64

HOSPITAL BILLING CHANGES • RADIOSURGERY – 77371 (SRS single session cranial using multi-source cobalt 60 device). – 77372 (SRS single session cranial using linear accelerator). – APC 0067 (single session cranial stereotactic radiosurgery) = $ 9, 769. 22. – Comprehensive APC with PSI J 1 (payment will include “all” services performed within date span). – Planning, devices, calcs, treatment, etc. 65

HOSPITAL BILLING CHANGES • RADIOSURGERY (CONT. ) – 77373 (SBRT - per fraction to one or more lesion including image guidance - not to exceed 5 fractions). – APC 0066 (Level V Radiation Therapy) = $1, 903. 22. – PSI ‘S’ (not discounted when multiple). – Exclusive code for any fractionated SRS treatment to any part of the body including cranial. – Includes first fraction. – Do not charge 77371 or 77372 for first fraction. 66

HOSPITAL BILLING CHANGES • PROTON BEAM – 77520 (proton treatment simple w/o comp). – APC 0412 (Level III Radiation Therapy) = $507. 75. – APC 0664 (Level I Proton) deleted for 2015. – PSI ‘S” (procedure or service, not discounted when multiple). – 77522 (proton treatment simple w/comp). – 77523 (proton treatment intermediate). – 77525 (proton treatment complex). – APC 0667 (renamed: Level IV Radiation Therapy) = $1, 072. 37. – PSI ‘S” (procedure or service, not discounted when multiple). 67

HOSPITAL BILLING CHANGES • INTRAOPERATIVE – 77424 (IORT delivery, x-ray, single treatment session). – 77425 (IORT delivery, electrons, single treatment). – Assigned to Comprehensive APC 0648 (Level IV Breast and Skin Surgery) = $7, 464. 32. – PSI J 1 (comprehensive) – Intraoperative services no longer paid separately. All services will be “packaged” into a single payment. 1. Supplies 2. Surgical 3. Radiation therapy 68

HOSPITAL BILLING CHANGES • LDR PROSTATE BRACHYTHERAPY – CPT codes 55875 (transperineal placement of needles/catheters) with PSI Q 3. – APC 0162 (Level III Cystourethroscopy and other Genitourinary Procedures). – CPT 77778 (interstitial radiation source application) with PSI Q 3. – APC 0651 (Complex Interstitial Radiation Source Application). 69

HOSPITAL BILLING CHANGES • LDR PROSTATE BRACHYTHERAPY – Composite APC 8001 (LDR Prostate Brachytherapy Composite). – PSI ‘T’ (Multiple Procedure Reduction Applies). – “Report APC 8001 when 55875 and 77778 are reported together. ” – Reimbursement = $3, 609. 85. – CMS bases the payment for composite APC 8001 (LDR prostate brachytherapy composite) on the geometric mean cost derived from claims for the same date of service that contain both CPT codes 55875 and 77778. 70

AMBULATORY SURGICAL CENTER (ASC) • CMS increased the payment rate by 1. 4% – Final conversion factor = $44. 071 (meet quality reporting requirements). – Final conversion factor = $43. 202 (does not meet quality reporting requirements). – LDR PROSTATE BRACHYTHERAPY – CMS provides a single payment for LDR prostate brachytherapy when CPT codes 55875 and 77778 are performed on the same DOS. – Report HCPCS Level II Code G 0458 for service (not CPT codes). 71

HOSPITAL BILLING CHANGES • BRACHYTHERAPY PLANNING CODES – CPT Codes Deleted: – 77326 (brachytherapy isodose plan; – 77327 (brachytherapy isodose plan; – 77328 (brachytherapy isodose plan; – CPT Codes Added: – 77316 (brachytherapy isodose plan: – 77317 (brachytherapy isodose plan; – 77318 (brachytherapy isodose plan; simple). intermediate. complex). simple). intermediate). complex). – Note: dose calculations included! 72

HOSPITAL BILLING CHANGES • BRACHYTHERAPY PLANNING CODES DEFINED – 77316 (brachytherapy isodose plan: simple). – 1 -4 sources; 1 channel. – Note: dose calculations included! – 77317 (brachytherapy isodose plan; intermediate). – 5 -10 sources; 2 -12 channels. – Note: dose calculations included! – 77318 (brachytherapy isodose plan; complex) – Over 10 sources; Over 12 channels. – Note: dose calculations included! 73

HOSPITAL BILLING CHANGES • BRACHYTHERAPY SOURCES PAYMENT RATES – CMS will continue to set the payment rates for brachytherapy sources using their established prospective payment methodology, which is based on geometric mean costs. – ASC’s and Hospitals included. 74

HOSPITAL BILLING CHANGES • RADIATION THERAPY TREATMENT DELIVERY – CPT Codes Deleted: – 77402, 77403, 77404, 77406 (radiation tx simple). – 77407, 77408, 77409, 77411 (radiation tx intermediate). – 77412, 77413, 77414, 77416 (radiation tx complex). – 0073 T (IMRT compensator tx). – 77418 (IMRT radiation tx). 75

HOSPITAL BILLING CHANGES • RADIATION THERAPY TREATMENT DELIVERY – CPT Codes New/Revised: – 77401 (radiation tx superficial/or ortho-voltage). – 77402 (radiation tx >1 MEV; simple). – 77407 (radiation tx >1 MEV; intermediate). – 77412 (radiation tx >1 MEV; complex). – 77385 (IMRT simple. – Used for breast, prostate, and compensator based IMRT. – 77386 (IMRT complex). – Used for all other IMRT treatment areas (non-compensator based). 76

HOSPITAL BILLING CHANGES • RADIATION THERAPY PLANNING CODES – CPT Codes Deleted: – 77305 (teletherapy isodose plan simple ). – 77310 (teletherapy isodose plan intermediate). – 77315 (teletherapy isodose plan complex). – CPT Codes New: – 77306 (teletherapy isodose plan simple). – 77307 (teletherapy isodose plan complex). – Note: dose calculations included! – CPT Codes Remaining: – 77295 (3 D planning). – 77301 (IMRT planning). 77

HOSPITAL BILLING CHANGES 2014 Codes Description 2015 Codes (Professional) 2015 Technical (Freestanding) 2015 Global (Freestanding) 2015 Codes OPPS (Hospital) 0073 T IMRT compensator tx (simple) N/A G 6016 77385 0197 T Intrafraction track motion N/A G 6017 Deleted 76950 Echo guidance radiotherapy G 6001 -26 G 6001 -TC G 6001 Deleted 77014 Ct scan for therapy guide 77014 -26 77014 -TC 77014 77387 77305 Teletherapy isodose plan simple 77306 -26 77306 -TC 77306 77310 Teletherapy isodose plan intermediate Deleted 77315 Teletherapy isodose plan complex 77307 -26 77307 -TC 77307 78

HOSPITAL BILLING CHANGES 2014 Codes Description 2015 Codes (Professional) 2015 Technical (Freestanding) 2015 Global (Freestanding) 2015 Codes OPPS (Hospital) 77326 Brachytherapy isodose plan; simple 77316 -26 77316 -TC 77316 77327 Brachytherapy isodose plan; intermediate 77317 -26 77317 -TC 77317 77328 Brachytherapy isodose plan; complex 77318 -26 77318 -TC 77318 77402 Radiation tx >1 MEV; simple N/A G 6003 77402 77403 Radiation tx >1 MEV; simple N/A G 6004 77402 77404 Radiation tx >1 MEV; simple N/A G 6005 77402 77406 Radiation tx >1 MEV; simple N/A G 6006 77402 79
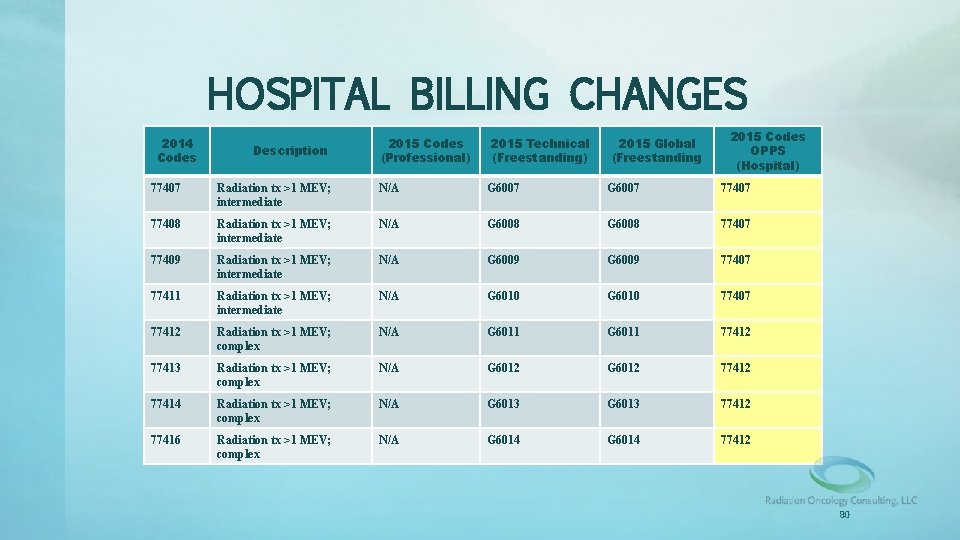
HOSPITAL BILLING CHANGES 2014 Codes Description 2015 Codes (Professional) 2015 Technical (Freestanding) 2015 Global (Freestanding 2015 Codes OPPS (Hospital) 77407 Radiation tx >1 MEV; intermediate N/A G 6007 77407 77408 Radiation tx >1 MEV; intermediate N/A G 6008 77407 77409 Radiation tx >1 MEV; intermediate N/A G 6009 77407 77411 Radiation tx >1 MEV; intermediate N/A G 6010 77407 77412 Radiation tx >1 MEV; complex N/A G 6011 77412 77413 Radiation tx >1 MEV; complex N/A G 6012 77412 77414 Radiation tx >1 MEV; complex N/A G 6013 77412 77416 Radiation tx >1 MEV; complex N/A G 6014 77412 80

HOSPITAL BILLING CHANGES 2014 Codes Description 2015 Codes (Professional) 2015 Technical (Freestanding) 2015 Global (Freestanding) 2015 Codes OPPS (Hospital) 77418 IMRT radiation tx (simple) N/A G 6015 77385 77418 IMRT radiation tx (complex) N/A G 6015 77386 77421 Stereoscopic x-ray guidance G 6002 -26 G 6002 -TC G 6002 Deleted 81

HOSPITAL BILLING CHANGES • Provider-Based outpatient Departments (PBD) – In response of rapid acquisition of physician practices by hospitals (off campus PBD), CMS started soliciting comments (2014) in regards to collecting data that would allow CMS to analyze the frequency, type, and payment for services. – Data shows that Medicare paid less for total services provided by the physician versus the same practice now owned by the hospital. 82

HOSPITAL BILLING CHANGES • HOSPITAL PBD REQUIREMENTS – Must report modifier with services performed in a hospital outpatient off-campus department. – Services, procedures, and/or surgeries provided at offcampus provider based hospital outpatient departments. – Use new HCPCS Level II Modifier (PO). – Does not include remote locations, satellite facilities, or ER departments. – NOTE: voluntary in 2015 – mandatory in 2016. 83

HOSPITAL BILLING CHANGES – New 2015 HCPCS Level II modifiers (Replaces ‘ 59’) – PO: Services, procedures, and/or surgeries provided at offcampus provider based outpatient departments. – XE: Separate encounter (a service that is distinct because it occurred during a separate encounter). – XP: Separate practitioner (a service that is distinct because it was performed by a different practitioner). – XS: Separate structure (a service that is distinct because it was performed on a separate organ/structure). – XU: Unusual non-overlapping service (the use of a service that is distinct because it does not overlap usual components of the main service). – NOTE: voluntary in 2015 – mandatory in 2016. 84

HOSPITAL CLINICAL TRIALS • CLINICAL TRIALS NUMBER NO LONGER OPTIONAL IN 2015 – In 2014 clinical trials hospitals must include a required eight (8) digit trial number on all claims that identifies services to the clinical trial patient. – After January 1, 2014 claims not containing this number will be returned and not processed. – ID number always proceeded by ‘NTC’ – https: //www. clinicaltrials. gov/ 85

2015 FINANCIAL CHANGES FOR HOSPITALS • THE BIG PICTURE ($) – Medicare payment adjustment for hospitals under HOPPS had an increase of 2. 2% in 2015. – Rural Sole Community Hospitals (SCH’s) or Essential Access Community Hospitals (EACH’s) will receive a 2. 4% payment increase in 2015 (most services). 86

REFERENCES 1. CMS Manual System; Department of Health & Human Services (DHHS); Pub 100 -04 Medicare Claims Processing; December 27, 2013 2. ASTRO online article (CY 2014 Hospital Outpatient Payment Rates Released): https: J/w. NN. astro. ag!Wf!Jb. . Ex: lusiws. JPrac: lice-M anagemant/CY-2014 -Hospitai-Outpaliert. Pa}ment-Rai. Bs-Released. aspx 3. DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services; Medicare Billing: 837 I and Form CMS-1450; ICN 006926 March 2013 4. DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services; Medicare Physician Fee Schedule; PAYMENT SYSTEM FACT SHEET SERIES; ICN 006814 April 2013 5. DEPARTMENT OF HEALTH AND HUMAN SERVICES Centers for Medicare & Medicaid Services; Hospital Outpatient Prospective Payment System; PAYMENT SYSTEM FACT SHEET SERIES; ICN 006820 December 2012 6. The Diagnosis Related Groups (DRGs) to Adjust Payment-Mechanisms for Health System Providers; Inter-American Conference on Social Security; November-2005; CISS/WP/05122 7. ASTRO 2015 Radiation Oncology Coding Resource 8. Bogardus Medical Systems (Bmsi) Principles of Coding, Billing, and Documentation in Radiation Therapy 87

Questions? susan@radoncconsulting. com 88
- Slides: 88